Back to Journals » Infection and Drug Resistance » Volume 13
Increased Virological Failure and Determinants Among HIV Patients on Highly Active Retroviral Therapy in Adigrat General Hospital, Northern Ethiopia, 2019: Hospital-Based Cross-Sectional Study
Authors Negash H ![]() , Welay M, Legese H
, Welay M, Legese H ![]() , Adhanom G
, Adhanom G ![]() , Mardu F
, Mardu F ![]() , Tesfay K, Gebrewahd A, Berhe B
, Tesfay K, Gebrewahd A, Berhe B ![]()
Received 27 February 2020
Accepted for publication 12 June 2020
Published 18 June 2020 Volume 2020:13 Pages 1863—1872
DOI https://doi.org/10.2147/IDR.S251619
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Eric Nulens
Hadush Negash,1 Miglas Welay,2 Haftom Legese,1 Gebre Adhanom,1 Fitsum Mardu,3 Kebede Tesfay,3 Aderajew Gebrewahd,1 Brhane Berhe3
1Unit of Medical Microbiology, Department of Medical Laboratory Sciences, College of Medicine and Health Sciences, Adigrat University, Tigrai, Ethiopia; 2Department of Midwifery, College of Medicine and Health Sciences, Adigrat University, Tigrai, Ethiopia; 3Unit of Medical Parasitology, Department of Medical Laboratory Sciences, College of Medicine and Health Sciences, Adigrat University, Tigrai, Ethiopia
Correspondence: Hadush Negash Email [email protected]
Background: In Ethiopia, despite the integrated implementation of antiretroviral therapy since 2005, the human immunodeficiency virus remains a public health concern. Managing and detecting antiretroviral treatment response is important to monitor the effectiveness of the therapy for individuals who experience failed virological response. An increased viral load indicating drug resistance or rapid progression of viral replication needs early detection. Hence, we aimed to assess the prevalence and determinants of virological response among human immunodeficiency virus-infected patients on highly active antiretroviral therapy.
Methods: A hospital-based cross-sectional study was conducted in Adigrat General Hospital from September to December, 2019, on a total of 422 participants. An interviewer-based questionnaire was used for data collection. About 4 mL of venous blood was collected for viral load determination. Patient records were reviewed for the previous results of CD4+ T cell counts. STATA 14 software was used to analyze the data. Descriptive data were presented using tables and figures. Bivariate and multivariate analyses were performed. A p-value < 0.05 was considered a statistically significant association.
Results: The mean age of study participants was 39 years (SD ± 12.2 years), of which 66.7% of them were females. The overall prevalence of virological failure was 12.47% (49/393). Moreover, the prevalence of virological failure was observed to be higher among tuberculosis co-infected individuals (26%) compared with the mono-infected HIV patients (6.3%). The odds of virological failure were higher among obese and undernourished individuals, tuberculosis co-infected, and individuals with the failure of immune reconstitution.
Conclusion: There was a high rate of virological failure among the study participants. Tuberculosis infection increased the rate of failure. There should be consistent assessment of viral load testing to determine the status of virological response for appropriate drug switching to clients. HIV patients with virological failure are recommended for switching of the antiretroviral therapy.
Keywords: Ethiopia, prevalence, HAART, HIV, HIV/TB co-infection, virological failure
Introduction
Human immune-deficiency virus (HIV) continues to be one of the top public health priorities in Ethiopia.1 By the end of 2013, there were a total of 593,400 adults living with HIV of which only 298,512 were on highly active antiretroviral therapy (HAART). Moreover, an estimated 45,200 people died due to HIV-related conditions in 2013.2 HAART is a life-saving treatment for patients with HIV which is an important component of the overall treatment plan among HIV patients.3 Since the introduction of HAART, the impact of HIV infection has significantly decreased4 due to viral suppression, restoring and preserving immune function, improving quality of life, and reducing HIV related morbidity and mortality along the course of treatment.5–7
Globally, many reports revealed that HIV infected individuals are experiencing virological, clinical, and immunological treatment failures.7 Virological failure, which is more suggestive of treatment failure of HAART, is a common problem that an HIV infected individual faces after starting treatment. Current World Health Organization (WHO) guidelines recommend that virological failure should not exceed 10% RNA copies per mL of plasma from the initiation of HAART.8 Patients who have experienced virological failure were found to have an increased risk of clinical progression to acquired immune deficiency syndrome (AIDS) and mortality compared with patients with virological success.9 Previous studies reported various factors like baseline CD4+ T cell counts,5,9-11 being younger,12–14 longer duration on HAART,10,13,15 poor adherence to treatment12,13,16,17 and current lower CD4+ T cell counts15,18 as associated with virological failure.
The introduction of combination therapy19,20 has modified the natural history of HIV infection from an end of life event to a manageable chronic condition21 thereby changing the landscape of HIV related mortality. Despite the benefits of HAART, it is not without challenges. There are many adverse drug reactions (ADRs) associated with HAART treatment resulting in negative health outcomes22,23 and increased mortality.24 Treatment discontinuation and medication non-adherence associated with ADRs are significant risk factors to catalyze virological failure.25,26 HAART failure to first-line regimens resulting from ADRs creates the need for very expensive and difficult-to-implement second-line regimens. Second-line HAART regimens are often unaffordable and largely donor dependent in resource-limited settings.27
The United Nations program on HIV/AIDS (UNAIDS) is aimed at the “90-90-90 target” to maintain viral suppression in 90% of persons on HAART by 2020.28 An important strategy to achieve this target, apart from the promotion of treatment adherence, is the use of a safer HAART regimen to promote maximal viral suppression and immune reconstitution.29,30 Identifying and managing determinants of virological failure have an important role in achieving high treatment success, improving the quality of life, and increasing survival rate from treatment failure. However, there is limited evidence on the epidemiology of virological failure among HIV infected individuals on HAART in the study area. Thus, this study aimed to identify the prevalence and determinants of virological failure among HIV-infected individuals on HAART in Adigrat General Hospital, Northern Ethiopia.
Methods
Study Design, Area and Period
A hospital-based cross-sectional study was employed to assess the prevalence of virological failure and determinants among HIV infected individuals on highly active retroviral therapy in Adigrat General Hospital, Eastern Tigrai, Ethiopia from September to December 2019.
Adigrat General Hospital is one of the governmental Hospitals located in Adigrat Town and was established to serve people from 6 weredas (districts). The Hospital is currently providing teaching and referral services for a population of more than 1,000,000 with an average annual client flow of 131,125 people.31 The Hospital has about 120 beds with a total of 209 health care providers and 132 administrative staff. There are 10 health care providers in the HAART clinic of the Hospital with a total of 1582 HIV patients currently on HAART. There is also an integrated service of ART clinic, laboratory services and pharmacy department. CD4+ T cell and viral load determinations are being used to monitor the effectiveness of HAART therapy with additional laboratory tests like complete blood cells and chemistry tests.
Source Population
- All HIV infected individuals on HAART who were attending Adigrat General Hospital.
Study Population
- All HIV infected individuals on HAART who attended appointments at the HAART clinic in the hospital during the study period.
Sampling Technique and Sample Size
- A convenience sampling technique was used to enroll the study participants among HIV infected individuals on HAART.
- The sample size was calculated using a single population proportion and determined using the following assumptions 95% CI, 5% margin of error and considering 50% prevalence rate.
Then total sample size (n) = (Zα/2)2 (p) (1-p)/d2 = (1.96)2 (0.5) (0.5)/0.05 = 384
While (Zα/2 = 1.96), p is estimated prevalence (50%) and d is margin of error (5%) which Finally, after adding 10% non-response rate 422 study participants were enrolled.
Eligibility Criteria
Inclusion Criteria
- HIV infected individuals with at least 6 months of follow-up on HAART
- HIV infected individuals who have provided written informed consent for individuals greater than 18 years of age or those individuals less than 18 years who have informed consent from a parent/guardian.
Exclusion Criteria
- HIV patients who were critically ill and unconscious
- HIV infected individuals with incomplete charts
Dependent Variable
- Virological response
Independent Variables
- Age, sex, intake of modern contraceptives, residence, adherence to treatment, co-infection with tuberculosis, marital status, educational status, body mass index, functional status, baseline CD4+ T cell count, WHO stage, presence of opportunistic infections
Data Collection, Preparation, and Analysis
Data Collection
An interviewer-based semi-structured questionnaire was used to collect socio-demographic data (age, sex, modern contraceptive intake, BMI, and residence). Clinical data (duration of HAART, current adherence to HAART, TB co-infection, eligibility criteria, cotrimoxazole intake, functional status, WHO stage, TB status, and presence of opportunistic infections) and previous results of CD4+ T cell counts for each patient were collected from patients’ medical records and through the questionnaire.
Sample Collection, Transportation, and Viral Load Determination
About 4 mL of venous blood was collected from each patient by trained laboratory professionals using EDTA vacutainer tube. Plasma was separated by centrifugation at 1500 rpm for 10 minutes and transferred into a sterile screw-capped polypropylene (Cryo) tube. The plasma specimens were then frozen at −20 °C and transported to Tigrai Research and Health Institute (THRI) adhering to the cold chain processes within 3 days of collection for viral load determination. To ensure the safety of the plasma specimens we applied triple packaging and labelled with UN3373. In the THRI, HIV-1 RNA was extracted from each patient’s plasma using the Abbott m2000sp automated sample preparation system (Abbott Molecular™, USA). Further RNA quantitative determination was performed using Abbott m2000rt quantitative Real-Time HIV-1 assay (Abbott Molecular™, USA) with a detection level of 40 to 10 million RNA copies/mL.
Data Analysis
We used STATA Version 14 software for data entry and analysis. Descriptive statistics were performed. Data were summarized and organized using figures and frequency tables. Bi-variate and multi-variate regression analysis were employed to measure the association between dependent and independent variables using backward model analysis. Variables with p < 0.2 in the bivariate logistic regression were imported to multi-variate regression analysis to identify the factors that have statistical significance in relation to the dependent variable. In the multivariate analysis, multicollinearity was considered by performing variance inflation factor (VIF) to indicate the correlation of independent variables to each other. Additionally, Hosmer-Lemeshow goodness of fit statistic was considered for the logistic regression. A p-value of < 0.05 was considered statistically significant.
Quality Control
Quality of laboratory data was maintained by strictly following standard operational procedures (SOPs) during sample collection, handling, and transportation. Quality control reagents were included in each test to evaluate the run validity of the viral load determination. Furthermore, viral load reagents were checked for expiry date. Questionnaires were checked for completeness and consistency on a daily bases during data collection by the principal investigator. Patient records were managed for confidentiality.
Operational Definition
Treatment Adherence
Taking HAART medications properly on a consistent basis over time and not missing doses of the prescribed therapeutic agents.8
- Good adherence: When the average treatment adherence of HIV patients is greater than or equal to 95%.
- Average Adherence: The average treatment adherence by the patients is from 85% to 94%.
- Weak Adherence: The average treatment adherence by the patients is less than 85%.
Immune Reconstitution
The ability of the body to respond to HAART and recovery of CD4+ T cell counts.
- Failure in Immune Reconstitution: CD4+ T cell counts to baseline or below/CD4+ T cell counts below 100 cells/mm3 for consecutive tests during the course of HAART.8
- Success in immune reconstitution: CD4+ T cell counts greater than the baseline count after initiation of HAART.8
Virological Failure
When the viral load of the HIV infected individual is greater than 1000 copies/mL of plasma which is determined based on two consecutive viral load measurements with adherence support.32
Results
Socio-Demographic Characteristics of Patients
A total of 422 HIV infected individuals on HAART were enrolled in our study, yielding an overall response rate of 93.1% (393/422). Out of the total study participants, 262 (66.7%) were females. The mean age of the study participants was 39 years ranging from 5 to 78 years. The participant had been followed in the clinic from 6 to 180 months with a median of 121 months and IQR of 66 to 132. Nearly two-thirds (249/393) of the study participants were urban dwellers.
Baseline Clinical Characteristics of Patients
The majority of study participants, 80% (314), were linked to HAART due to clinical staging. One hundred twenty-three (31.3%) of the total study participants were observed to be co-infected with TB. Most of the study participants, 89.1% (350/393), were in WHO clinical stage I. The overall virological failure of HIV patients in our study was 12.5% (49/393) (Table 1). One-hundred ninety-four (49.4%) of the study participants had opportunistic infections, such as: intestinal parasitic infections [24.23%, 47/194], fungal infections [9.3%, 18/194], varicella-zoster [6.19%, 12/194], pneumonia [5.67%, 11/194], upper respiratory tract infection [4.12%, 8/194] and urinary tract infections [3.61%, 7/194].
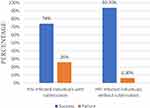
Comparison of Virological Failure Among Tuberculosis Co-Infected and Mono-Infected Clients
From this study, the prevalence of virological failure among HIV/TB co-infected patients was 26% (32/123) compared to 6.3% (17/270) amongst HIV mono-infected patients (Figure 1).
Prevalence and Determinants of Virological Failure of HAART Among HIV Patients
The overall prevalence of virological failure was 12.47% (49/393). Increased virological failure was observed among clients with overweight body mass index [AOR = 1.19, 95% CI: [0.290–1.717], p = 0.001], being malnourished [AOR = 2.1, 95% CI: [1.322–8.271], p = 0.001], individuals with tuberculosis infection [AOR = 6.1, 95% CI: 3.000,12.223, p < 0.001] and immunological treatment failure [AOR = 19.4, 95% CI: [0.019, 20.129], P = 0.049] (Table 1).
Discussion
In this current study, the overall virological failure of HAART treatment was 12.47% (49/393). This finding aligned with a number of studies previously conducted in Ethiopia such as: in Tigrai, 11.5%,33 Gondar, 11.8% and 14.7%,18,34 Bahir Dar, 10.7%35 and Addis Ababa 15%.36 Studies outside of Ethiopia showing similar rate of virological failure were found in Zambia 12.3%,37 Tanzania, 12.3%,38 Malawi, 9.2%,39 Nigeria, 13.7%,40 South Africa, 13.7%,41 Uganda, 9.9%, 11.3% and 14.15%,42–44 New Guinea, 13.7%,45 China, 13.4%,46 Thailand, 9.6%,47 Nepal, 9.9%,48 and Cambodia, 12.9%.49. The result of the current study was higher for virological failure than previously conducted research in Ethiopia (i.e., Jimma, 5.3%50 and Gondar, 4.1%51) and Burkina Faso at 7.5%.52 However; our finding was lower than the other studies done in Cameron, 23.2%53 and Kenya, 24%,54 Liberia, 47%,55 Zimbabwe, 30.6%,56 Tanzania 57.1%,57 32%,58 Cameroon, 20.6%,59 Ghana, 16.7%,60 Togo, 51.6%,61 Colombia, 20.9%,62 India, 69.6%63 and Peru, 24%.64 This variance might be attributed due to differences in cutoff values of viral RNA copies per mL of plasma to be considered as virological failure, the difference among study participants, duration of follow-up, study design, and variations on the treatment adherence of HAART. Moreover, protease inhibitors were used as the first-line HAART regimen52 and nutritional support given for the study participants50 which were different from our setting, difference in a geographical area, study design, and the virological failure cutoff points, in our study, was a plasma viral load ≥ 400 copies/mL,54,57,65 inclusion criteria used, study participants were clinically/immunologically failed,55,66 perinatally infected,61 lower mean age59 and shorter mean time on HAART.60
Two hundred eighty-five (72.5%) of our study participants had good adherence to treatment. Similar adherence trends were seen in previous studies across Ethiopia including Southern Ethiopia, 81.8%,36 Northwestern Ethiopia, 82.7%67 and Addis Ababa, Ethiopia, 78.5%.68 However, our study reported lower treatment adherence than select studies conducted in Addis Ababa, Ethiopia, 97.7%69 and Southwestern Ethiopia, 100%.50 These variations in patient adherence might be due to differences in psychosocial support of relatives or the society, stigma, and lack of commitment to take medications so that HIV patients might drop from the HAART treatment, after not feeling well (perceived it from the medication), fear of treatment side effects, and being busy (forgetting the HAART medication).8,34
Malnourished and overweight HIV infected individuals were 2.1 (p = 0.001) and 1.19 (p = 0.001) times high likely to experience virological failure than individuals with normal body mass index. This finding aligns with previous studies from Northwestern Ethiopia34 and Northwestern Uganda.70 It is evident that abnormal BMI is correlated significantly with the decrease in CD4+ T cell count and the increase in viral load by progressing into the advanced stage of the disease, and by exposing the patients not taking ART medication (poor adherence).71,72
This study revealed that virological failure was 6.1 times more likely to occur among TB co-infected individuals than the TB non-infect cohort (p < 0.001). This was similar to reports from Uganda,73 South Africa.74,75 It is possible for virological failure to lead to incident TB. The risk of virological non-suppression may also be increased by concurrent ART and TB treatment due to impaired treatment adherence and pharmacokinetics drug interactions. Patients on ART with active TB should be prioritized for viral load monitoring and adherence support. Strengthening interventions that prevent incident TB during ART, such as isoniazid prevent therapy and infection control at health facilities, is crucial. A possible explanation for this might be increased viral copies which may compromise immunity and negatively affect response to treatment by contributing to the double burden side effects of tuberculosis and HIV.76
Individuals with failure of immune reconstitution were observed to be at increased risk of experiencing immunological failure of HAART (p = 0.049). This finding was identified in previous studies from India,77 Northwestern Ethiopia78 and Brazil.79 The failure of immune reconstitution leads to the rapid progression of viral antigen replication.80 Failure in immune reconstitution should also be a surrogate marker for virological failure. Hence, detection and monitoring immunological response of CD4 + T cells for immune reconstitution should be intensified largely to prevent resistance to antiretroviral therapy.80,81
Strength and Limitation of the Study
The strength of the study is that both CD4+ T cell counts and viral load determination were assessed for each HIV infected individual on HAART to determine the response to immune reconstitution and virological failure. Despite this approach, the viral load to determine the virological response was performed only once. We should have performed two consecutive measurements to strengthen the findings.
Conclusion
The overall prevalence of virological failure among HIV patients on HAART was high. Factors such as being obese, malnourished, tuberculosis co-infected and failure in immune reconstitution were also associated with virological failure. The virological response should be regularly performed as per the WHO guideline in order to ensure early detection of drug resistance and to respond with the possibility of regimen switching. It is apparent that virological and immunological response in cases of suspected along with clinical failures should be performed simultaneously.
Abbreviations
ADRs, adverse drug reactions; AIDS, acquired immune deficiency syndrome; HAART, highly active antiretroviral therapy; HIV, human immunodeficiency virus; UNAIDS, United Nations on HIV/AIDS.
Data Sharing Statement
All datasets generated and/or analyzed during the current study are summarized in the manuscript.
Ethics Approval and Consent to Participate
Ethical clearance was obtained from the research and community service committee of Adigrat University with a reference number of Adigrat University/College of Medicine and Health Science/085/19. Official letters were obtained from Tigrai Regional Health Bureau, Tigrai Research and Health Institute, the Chief Executive Officer of Adigrat Hospital, Department of Patient Records, and Laboratory Head in Adigrat Hospital before the data collection. Written informed consent was sought from each study participant with parents or guardians consenting for participants aged less than 18 years. Data of every HIV patient on HAART were kept confidential. This study was conducted in accordance with the declaration of Helsinki.
Acknowledgments
We are thankful to Adigrat General Hospital laboratory, chief executive officer, staffs in the HAART clinic, data collectors and study participants for their valuable contribution to this study. We also want to extend our warmest appreciation to the Tigrai Health Bureau for giving official permission to conduct the research.
Author Contributions
All authors made substantial contributions to conception and design, acquisition of data, analysis and interpretation of data, drafting the manuscript, revising the manuscript critically, read and approve the final draft of the manuscript for submission, gave final approval of the manuscript version to be published and agreed to be accountable for every step of the work.
Funding
This study was funded by Adigrat University, Ethiopia. The funding organization had no role in the conceptualization and design of the study, data collection, enrollment of study participants, statistical analysis, data interpretation, and manuscript development.
Disclosure
The authors declared they have no competing interests.
References
1. Federal HIV/AIDS Prevention and Control Office. HIV/AIDS in Ethiopia. An Epidemiological Synthesis. Addis Ababa, Ethiopia: Federal HIV/AIDS Prevention and Control Office; 2014.
2. Federal Government Democratic Republic of Ethiopia. Country Progress Report on the HIV Response. Addis Ababa, Ethiopia: Federal Democratic Republic of Ethiopia; 2014.
3. UNHCR. Clinical Guidelines for Antiretroviral Therapy Management for Displaced Populations Southern Africa. Geneva, Switzerland: Southern African HIV Clinicians Society; 2007.
4. UNECA. HIV/AIDS Progress in 2014. Addis Ababa, Ethiopia: World Health Organization Ethiopia Country Office; 2015.
5. Churchill D, Waters L, Ahmed N, et al. British HIV association guidelines for the treatment of HIV-1-positive adults with antiretroviral therapy. Br HIV Assoc. 2015;17(4):2–104.
6. AIDS. Guidelines for the Use of Antiretroviral Agents in HIV-1-Infected Adults and Adolescents; 2016.
7. NACO. ART Guidelines for HIV-Infected Adults and Adolescents. Ministry of Health and Family Welfare Government of India; 2013.
8. WHO. Consolidated Guidelines on the Use of Antiretroviral Drugs for Treating and Preventing HIV Infection: Recommendations for a Public Health Approach.
9. Deeks SG. Determinants of virological response to antiretroviral therapy: implications for long-term strategies. Clin Infect Dis. 2000;30(2):177–184. doi:10.1086/313855
10. Liégeois F, Vella C, Eymard-Duvernay S, Eam KK. Virological failure rates and HIV-1 drug resistance patterns in patients on first-line antiretroviral treatment in semirural and rural Gabon. J Int AIDS Soc. 2012;15(2):s17985. doi:10.7448/IAS.15.2.17985
11. Grabar S, Pradier C, Corfec EL. Factors associated with clinical and virological failure in patients receiving a triple therapy including a protease inhibitor. AIDS. 2000;14(2):141–149. doi:10.1097/00002030-200001280-00009
12. Parienti JJ, Massari VR, Descamps D, et al. Predictors of virological failure and resistance in HIV-infected patients treated with nevirapine- or efavirenz-based antiretroviral therapy. Clin Infect Dis. 2004;38(9):1311–1316. doi:10.1086/383572
13. Rupérez M, Pou C, Maculuve S. Determinants of virological failure and antiretroviral drug resistance in Mozambique. J Antimicrob Chemother. 2015;70(9):2639–2647. doi:10.1093/jac/dkv143
14. Sang RK, Miruka FO. Factors associated with virological failure amongst adults on antiretroviral therapy in Nyanza Region, Kenya. IOSR J Dent Med Sci. 2016;15(7):108–121. doi:10.9790/0853-15076108121
15. Jobanputra K, Parker LA, Azih C, et al. Factors associated with virological failure and suppression after enhanced adherence counselling, in children, adolescents and adults on antiretroviral therapy for HIV in Swaziland. PLoS One. 2015;10(2):e0116144. doi:10.1371/journal.pone.0116144
16. Liang S, Shen Z, Yan J. Low virological failure and drug resistance among HIV-infected patients receiving hospital-based ART while care and outreach through community in Guangxi, China. Front Public Health. 2015;3:244. doi:10.3389/fpubh.2015.00244
17. Zuo Z, Liang S, Sun X. Drug resistance and virological failure among HIV-infected patients after a decade of antiretroviral treatment expansion in eight provinces of China. PLoS One. 2016;11(12):e0166661. doi:10.1371/journal.pone.0166661
18. Gizachew A, Belay T, Anteneh A, Getachew F, Gizachew Y. Prevalence and associated factors of treatment failure among HIV/AIDS patients on HAART attending University of Gondar Referral Hospital Northwest Ethiopia. BMC Immunol. 2018;19:37. doi:10.1186/s12865-018-0278-4
19. Dieffenbach CW, Fauci AS. Thirty years of HIV and AIDS: future challenges and opportunities. Ann Intern Med. 2011;154(11):766–771. doi:10.7326/0003-4819-154-11-201106070-00345
20. Tanser F, Bärnighausen T, Grapsa E, Zaidi J, Newell M-L. High coverage of ART associated with decline in risk of HIV acquisition in rural KwaZulu-Natal, South Africa. Science. 2013;339(6122):966–971. doi:10.1126/science.1228160
21. Deeks S, Lewin S, Havlir D. The end of AIDS: HIV infection as a chronic disease. Lancet Diabetes Endo. 2013;382:1525–1533.
22. Murphy RA, Sunpath H, Kuritzkes DR, Venter F, Gandhi RT. Antiretroviral therapy-associated toxicities in the resource-poor world: the challenge of a limited formulary. J Infect Dis. 2007;196(3):449–456. doi:10.1086/521112
23. Khan K, Khan AH, Sulaiman SA, Soo CT. Survival trend and impact of adverse drug reactions during haart on survival function in HIV/AIDS patients. Sex Transm Infect. 2015;91(s236):17–34. doi:10.1136/sextrans-2015-052270.612
24. Mouton JP, Mehta U, Parrish AG, et al. Mortality from adverse drug reactions in adult medical inpatients at four hospitals in South Africa: a cross-sectional survey. Br J Clin Pharmacol. 2015;80(4):818–826. doi:10.1111/bcp.12567
25. Prosperi MC, Fabbiani M, Fanti I, et al. Predictors of first-line antiretroviral therapy discontinuation due to drug-related adverse events in HIV-infected patients: a retrospective cohort study. BMC Infect Dis. 2012;12(1):296. doi:10.1186/1471-2334-12-296
26. Katz I, Kaplan R, Fitzmaurice G, et al. Treatment guidelines and early loss from care for people living with HIV in Cape Town, South Africa: a retrospective cohort study. PLoS Med. 2017;14(11):1–12. doi:10.1371/journal.pmed.1002434
27. Renaud-Théry F, Nguimfack BD, Vitoria M. Use of antiretroviral therapy in resource-limited countries in 2006: distribution and uptake of first- and second-line regimens. AIDS Behav. 2007;21(4):89–95. doi:10.1097/01.aids.0000279711.54922.f0
28. UNAIDS. Ending AIDS: Progress Towards the 90- 90-90targets; 2017.
29. Nachega JB, Sam-Agudu NA, Mofenson LM, Schechter M, Mellors JW. Achieving viral suppression in 90% of people living with human immunodeficiency virus on antiretroviral therapy in Low- and Middle-income Countries: progress, challenges, and opportunities. Clin Infect Dis. 2018;66(10):1487–1491. doi:10.1093/cid/ciy008
30. Trickey A, May MT, Vehreschild JJ, et al. Survival of HIV-positive patients starting antiretroviral therapy between 1996 and 2013: a collaborative analysis of cohort studies. Lancet HIV. 2017;4:349–356. doi:10.1016/S2352-3018(17)30066-8
31. Population. City Population. Adigrat: Adigrat City municipality.
32. WHO. World health organizaion. Available from: https://www.who.int/hiv/pub/guidelines/arv2013/art/WHO_CG_table_7.15.pdf.
33. Hailu GG, Hagos DG, Hagos AK, Wasihun AG, Dejene TA, Paraskevis D. Virological and immunological failure of HAART and associated risk factors among adults and adolescents in the Tigray region of Northern Ethiopia. PLoS One. 2018;13(5):e0196259. doi:10.1371/journal.pone.0196259
34. Mulu A, Maier M, Liebert UG. Low incidence of HIV-1C acquired drug resistance 10 years after the rollout of antiretroviral therapy in Ethiopia: a prospective cohort study. PLoS One. 2015;10(10):e0141318. doi:10.1371/journal.pone.0141318
35. Bokretsion G, Endalkachew N, Getachew K. HIV/AIDS treatment failure and its determinant factors among first line HAART patients at Felege-Hiwot referral hospital, Bahir Dar, Northwest Ethiopia. J AIDS Clin Res. 2017;8(11):4.
36. Yirdaw KD, Hattingh S, Paraskevis D. Prevalence and predictors of immunological failure among HIV patients on HAART in Southern Ethiopia. PLoS One. 2015;10(5):e0125826. doi:10.1371/journal.pone.0125826
37. ZAMPHIA. Zambia Population-Based HIV Impact Assessment, ZAMPHIA: 2015–2016. Summary Sheet: Preliminary Findings. New York: PHIA Project; 2016. Available from: https://phia.icap.columbia.edu/wp-content/uploads/2016/09/ZAMBIA-Factsheet.
38. Project PHIA. Tanzania HIV Impact Survey 2016–2017. New York: PHIA Project; 2017. Available from: https://phia.icap.columbia.edu/wpcontent/uploads/2017/11/Tanzania_SummarySheet_A4.
39. Government of Malawi. Malawi Population-Based HIV Impact Assessment, MPHIA: 2015–2016. Summary Sheet: Preliminary Findings. New York: PHIA Project; 2016. Availabele from: https://phia.icap.columbia.edu/wp-content/uploads/2016/09/MALAWI-Factsheet.
40. Rawizza HE, Chaplin B, Meloni ST, Eisen G, Rao T, Sankalé JL. Immunologic criteria are poor predictors of virologic outcome: implications for HIV treatment monitoring in resource-limited settings. Clin Infect Dis. 2011;53(12):1283–1290. doi:10.1093/cid/cir729
41. Mutevedzi PC, Lessells RJ, Rodger AJ, Newell M-L, Myer L. Association of age with mortality and virological and immunological response to antiretroviral therapy in rural south African adults. PLoS One. 2011;6(7):e21795. doi:10.1371/journal.pone.0021795
42. Reynolds SJ, Nakigozi G, Newell K, et al. Failure of immunologic criteria to appropriately identify antiretroviral treatment failure in Uganda. AIDS (London, England). 2009;23(6):697. doi:10.1097/QAD.0b013e3283262a78
43. Kamya M, Mayanja-Kizza H, Kambugu A, et al. Predictors of long-term viral failure among ugandan children and adults treated with antiretroviral therapy. JAIDS J Acquir Immune Defic Syndr. 2007;46(2):187–193. doi:10.1097/QAI.0b013e31814278c0
44. Von-Braun A, Sekaggya-Wiltshire C, Scherrer A, et al. Early virological failure and HIV drug resistance in Ugandan adults co-infected with tuberculosis. AIDS Res Ther. 2017;14:1–6. doi:10.1186/s12981-016-0128-5
45. Gare J, Kelly-Hanku A, Ryan CE, et al. Factors influencing antiretroviral adherence and virological outcomes in people living with HIV in the Highlands of Papua New Guinea. PLoS One. 2015;10(8):e0134918. doi:10.1371/journal.pone.0134918
46. Huang P, Tan J, Ma W, et al. Outcomes of antiretroviral treatment in HIV-infected adults: a dynamic and observational cohort study in Shenzhen, China, 2003–2014. BMJ Open. 2015;5(5):e007508. doi:10.1136/bmjopen-2014-007508
47. Khienprasit N, Chaiwarith R, Sirisanthana T, Supparatpinyo K. Incidence and risk factors of antiretroviral treatment failure in treatment-naïve HIV-infected patients at Chiang Mai University Hospital, Thailand. AIDS Res Ther. 2011;8:42. doi:10.1186/1742-6405-8-42
48. Ojha CR, Shakya G, Dumre SP. Virological and immunological status of the people living with HIV/AIDS Undergoing ART treatment in Nepal. Biomed Res Int. 2016;2016:6817325. doi:10.1155/2016/6817325
49. Barennes H, Guillet S, Limsreng S, et al. Virological failure and HIV-1 drug resistance mutations among naive and antiretroviral pre-treated patients entering the ESTHER program of Calmette Hospital in Cambodia. PLoS One. 2014;9(8):e105736. doi:10.1371/journal.pone.0105736
50. Abdissa A, Yilma D, Fonager J, et al. Drug resistance in HIV patients with virological failure or slow virological response to antiretroviral therapy in Ethiopia. BMC Infect Dis. 2014;14:181. doi:10.1186/1471-2334-14-181
51. Ayalew M, Kumilachew D, Belay A, et al. First-line antiretroviral treatment failure and associated factors in HIV patients at the University of Gondar Teaching Hospital, Gondar, Northwest Ethiopia. HIV/AIDS (Auckland, Nz). 2016;8:141.
52. Penot P, He’ma A, Bado G, et al. The vulnerability of men to virologic failure during antiretroviral therapy in a public routine clinic in Burkina Faso. JIAS. 2014;17:18646. doi:10.7448/IAS.17.1.18646
53. Meriki HD, Tufon KA, Afegenwi MH, et al. Immuno-haematologic and virologic responses and predictors of virologic failure in HIV-1 infected adults on first-line antiretroviral therapy in Cameroon. Infect Dis Poverty. 2014;3(1):5. doi:10.1186/2049-9957-3-5
54. Hassan AS, Nabwera HM, Mwaringa SM, et al. HIV-1 virologic failure and acquired drug resistance among first-line antiretroviral experienced adults at a rural HIV clinic in coastal Kenya: a cross-sectional study. AIDS Res Ther. 2014;11:9. doi:10.1186/1742-6405-11-9
55. Loubet P, Charpentier C, Visseaux B, et al. Prevalence of HIV-1 drug resistance among patients failing first-line ART in Monrovia, Liberia: a cross-sectional study. J Antimicrob Chemother. 2015;70(6):1881–1884. doi:10.1093/jac/dkv030
56. Makadzange AT, Higgins-Biddle M, Chimukangara B, et al. Clinical, virologic, immunologic outcomes and emerging HIV drug resistance patterns in children and adolescents in public ART care in Zimbabwe. PLoS One. 2015;10(12):e0144057. doi:10.1371/journal.pone.0144057
57. Mgelea EM, Kisenge R, Aboud S. Detecting virological failure in HIV-infected Tanzanian children. S Afr Med J. 2014;104(10):696–699. doi:10.7196/SAMJ.7807
58. Ramadhani HO, Thielman NM, Landman KZ, et al. Predictors of incomplete adherence, virologic failure, and antiviral drug resistance among HIV-infected adults receiving antiretroviral therapy in Tanzania. CID. 2007;45:1492–1498. doi:10.1086/522991
59. Nlend AE, Lyeb S, Moyo ST. A.N. M. Viral monitoring and prevalence of viral failure in HIV-1 infected children under first line antiretroviral therapy during the first 60 months of treatment in Yaoundé, Cameroon: a serial cross-sectional analysis. Open J Pediatr. 2016;6:69–74. doi:10.4236/ojped.2016.61012
60. Barry O, Powell J, Renner L, et al. Effectiveness of first-line antiretroviral therapy and correlates of longitudinal changes in CD4 and viral load among HIV-infected children in Ghana. BMC Infect Dis. 2013;13:476. doi:10.1186/1471-2334-13-476
61. Salou M, Dagnra AY, Butel C, et al. High rates of virological failure and drug resistance in perinatally HIV-1-infected children and adolescents receiving lifelong antiretroviral therapy in routine clinics in Togo. JIAS. 2016;19:20683. doi:10.7448/IAS.19.1.20683
62. De-la Hoz J, Bolaño L, Cárdenas O, et al. Charactrization of treatment failure in HIV positive patients in the Colombian Caribbean region. Colomb Med. 2014;45(4):s162–s167. doi:10.25100/cm.v45i4.1566
63. Raja K, Chandrasekar C, Krishnarajasekhar OR, et al. Predicting virological failure with immunological criteria in first line ART patients in a resource poor setting. World J AIDS. 2014;4:413–421. doi:10.4236/wja.2014.44049
64. Jorge AR, Jorge PB, Elsa GL, et al. Risk factors associated with virologic failure in HIV-infected patients receiving antiretroviral therapy at a public hospital in Perus. Rev Chilena Infectol. 2013;30(1):42–48. doi:10.4067/S0716-10182013000100006
65. Waruru A, Muttai H, Ng’ang’a L, et al. Positive predictive value of the WHO clinical and immunologic criteria to predict viral load failure among adults on first, or second-line antiretroviral therapy in Kenya. PLoS One. 2016;11(7):e0158881. doi:10.1371/journal.pone.0158881
66. Puthanakit T, Kerr S, Ananworanich J, Bunupuradah T, Boonrak P, Sirisanthana V. Pattern and predictors of immunologic recovery in human immunodeficiency virus-infected children receiving non-nucleoside reverse transcriptase inhibitor-based highly active antiretroviral therapy. Pediatr Infect Dis J Clin North Am. 2009;28(6):488–492. doi:10.1097/INF.0b013e318194eea6
67. Zeleke A. Prevalence of antiretroviral treatment failure and associated factors in HIV infected children on HAART at Gondar University Hospital, retrospective cohort study. Int J Med Med Sci. 2016;8(11):125–132. doi:10.5897/IJMMS2015.1164
68. Teshome W, Tefera A. Detection of immunological treatment failure among HIV infected patients in Ethiopia: a retrospective cohort study. BMC Immunol. 2015;16:55. doi:10.1186/s12865-015-0120-1
69. Teshome Y, Yalew A. Magnitude and predictors of antiretroviral treatment failure in private health facilities in Addis Ababa, Ethiopia. PLoS One. 2015;10(5):e0126026. doi:10.1371/journal.pone.0126026
70. Izudi J, Alioni S, Kerukadho E, Ndungutse D. Virological failure reduced with HIV- serostatus disclosure, extra baseline weight and rising CD4 cells among HIV-positive adults in northwestern Uganda. BMC Infect Dis. 2016;18(8). doi:10.1186/s12879-12016-11952-x
71. Duggal S, Chugh TD, Duggal AK. HIV and malnutrition: effects on immune system. Clin Dev Immunol. 2012;2012:1–8. doi:10.1155/2012/784740
72. Batterham M, Brown D, Garsia R. Nutritional management of HIV/AIDS in the era of highly active antiretroviral therapy: a review. Australian J Nut Diet. 2001;1:211–223.
73. Bulage L, Ssewanyana I, Nankabirwa V, et al. Factors associated with virological non-suppression among HIV-positive patients on antiretroviral therapy in Uganda, August 2014-July 2015. BMC Infect Dis. 2017;17(1):326. doi:10.1186/s12879-017-2428-3
74. Gupta A, Wood R, Kaplan R, Bekker L-G, Lawn SD, Polis MA. Prevalent and incident tuberculosis are independent risk factors for mortality among patients accessing antiretroviral therapy in South Africa. PLoS One. 2013;8(2):e55824. doi:10.1371/journal.pone.0055824
75. El-Khatib Z, Ekstrom AM, Ledwaba J, et al. Viremia and drug resistance among HIV-1 patients on antiretroviral treatment: a cross-sectional study in Soweto, South Africa. AIDS (London, England). 2010;24(11):1679–1687. doi:10.1097/QAD.0b013e32833a097b
76. Assemie MA, Alene M, Ketema DB, Mulatu S. Treatment failure and associated factors among first line patients on highly active antiretroviral therapy in Ethiopia: a systematic review and meta-analysis. Glob Health Res Policy. 2019;4:32. doi:10.1186/s41256-019-0120-4
77. Chakravarty J, Sundar S, Chourasia A, et al. Outcome of patients on second line antiretroviral therapy under programmatic condition in India. BMC Infect Dis. 2015;15(1):517. doi:10.1186/s12879-015-1270-8
78. Belete B, Amare T, Abera B, Yohannes A, Terefe D, Destaw F. Determinants of virological failure among patients on highly active antiretroviral therapy in University of Gondar Referral Hospital, Northwest Ethiopia: a case–control study. HIV AIDS. 2017;9:153–159. doi:10.2147/HIV.S139516
79. Mariana V, Ana R, Elisabeth C. Factors associated with early virological response in HIV-infected individuals starting antiretroviral therapy in Brazil (2014–2015): results from a large HIV surveillance cohort. J Acquir Immune Defic Syndr. 2018;78(4):19–28. doi:10.1097/QAI.0000000000001684
80. Negash H, Legese H, Tefera M, et al. The effect of tuberculosis on immune reconstitution among HIV patients on highly active antiretroviral therapy in Adigrat general hospital, eastern Tigrai, Ethiopia; 2019: a retrospective follow up study. BMC Immunol. 2019;20(1):45. doi:10.1186/s12865-019-0327-7
81. WHO. HIV Drug Resistance Fact Sheet. Geneva, Switzerland: WHO; 2011. Available from: https://www.who.int/hiv/facts/WHD2011-HIVdr-fs-final.pdf.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.