Back to Journals » Journal of Multidisciplinary Healthcare » Volume 15
Hospital Length of Stay and Related Factors for COVID-19 Inpatients Among the Four Southern Regions Under the Proposed Southern Business Unit of Saudi Arabia
Authors Alharbi AA , Alqumaizi KI, Bin Hussain I, AlHarbi NS , Alqahtani A, Alzawad W, Suhail HM, Alamir MI, Alharbi MA, Alzamanan H
Received 15 February 2022
Accepted for publication 6 April 2022
Published 20 April 2022 Volume 2022:15 Pages 825—836
DOI https://doi.org/10.2147/JMDH.S362625
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Abdullah A Alharbi,1 Khalid I Alqumaizi,2 Ibrahim Bin Hussain,3– 5 Nasser S AlHarbi,6 Abdulmalik Alqahtani,7 Wala Alzawad,8 Hussam M Suhail,9 Mohammed I Alamir,9 Mohammed A Alharbi,9 Hamad Alzamanan10
1Family and Community Medicine Department, Faculty of Medicine, Jazan University, Jazan City, Jazan, Saudi Arabia; 2Family Medicine Department, Faculty of Medicine, AlMaarefa University, Riyadh, Saudi Arabia; 3Department of Pediatrics, King Faisal Specialist Hospital & Research Centre, Riyadh, Saudi Arabia; 4Department of Pediatrics, College of Medicine, Al Faisal University, Riyadh, Saudi Arabia; 5Southern Business Unit, Health Holding Company Project, Healthcare Transformation, Vision Realization Office, Ministry of Health, Riyadh, Saudi Arabia; 6Department of Pediatrics, College of Medicine, King Saud University, Riyadh, Saudi Arabia; 7Ophthalmology Department, Prince Sultan Medical Military City, Riyadh, Saudi Arabia; 8Eastern Business Unit, Health Holding Company Project, Healthcare Transformation, Vision Realization Office, Ministry of Health, Khobar, Saudi Arabia; 9Faculty of Medicine, Jazan University, Jazan City, Saudi Arabia; 10The Vision Realization Office (VRO), Ministry of Health, Riyadh, Saudi Arabia
Correspondence: Abdullah A Alharbi, Family and Community Medicine Department, Faculty of Medicine, Jazan University, Jazan City, 45142, Jazan, Saudi Arabia, Tel +966556966880, Email [email protected]
Objective: To assess the length of stay (LoS) variation for COVID-19 inpatients among the four regions of the Southern Business Unit (SBU).
Methods: This is a comparative retrospective study of the LoS of COVID-19 inpatients in the four regions of the SBU in the KSA. Data was collected from the Ministry of Health (MoH) in all hospitals in the SBU. Participants were all patients admitted with confirmed COVID-19 between March 2020 and February 2021. Variables included region (variable of interest), demographics, comorbidities, and complications. Multilinear regression was performed to control for any factors that might have had an association with LoS.
Results: The mean LoS of the total sample was 10 days and Bisha (the reference) was 7 days. Compared to Bisha, LoS in Jazan was 34% longer, in Najran 62% longer, and Aseer 40% longer. We observed that other factors also had an association with LoS, compared to Bisha, compared to the references, Saudi patients had a 15% shorter stay; admission to ICU increased LoS by 57%; patients who died during hospitalization had a 39% shorter LoS; the complications from COVID-19 of acute kidney injury and ARDS increased LoS by 22% and 48% respectively.
Conclusion: After statistically controlling for confounders, this study reveals that LoS was significantly impacted by region in the SBU in the KSA. We recommend that further study be conducted to illuminate the underlying causes of this variation which may be organizational or structural to ensure high quality of care, access to care, and equity of resources throughout all regions of the SBU in accordance with the new Model of Care in Vision 2030.
Keywords: COVID-19, length of stay, Southern Business Unit, Health Holding Company, KSA
Introduction
The COVID-19 pandemic caused by the SARS CoV-2 coronavirus began in December 2019 in the city of Wuhan, China.1 This is the seventh coronavirus known to infect humans and it spread rapidly around the world, challenging most of the health systems of the world.2 By March 2020 the World Health Organization had declared COVID-19 a pandemic and the world is still in the grips of this pandemic more than two years later.3,4 Globally, according to the World Health Organization (WHO), as of July 13, 2021, confirmed cases of COVID-19 had exceeded 186 million with more than four million deaths while the Kingdom of Saudi Arabia (KSA) experienced confirmed cases of 503,734 with over 8000 deaths.5,6
The COVID-19 pandemic overwhelmed hospital systems globally as they reached maximum capacity and resources. The exponential growth in infection rates coupled with the need for many patients to stay in hospitals for prolonged periods, worsened the crisis in the face of shortages of everything from healthcare staff to ventilators.7,8 Financial costs rose as well, as healthcare systems struggled to deal with the rapid increase in the demand for care.9,10 Vekaria et al emphasized the need to measure LoS for the COVID-19 pandemic in order to plan for capacity needs for hospital beds in a test of three statistical models of LoS in the UK to avoid having the system be overwhelmed again in the future.11 Vision 2030 is a long-range plan proposed by the Saudi government to meet future demands for society. One of the strategies of this plan is the overhaul of the healthcare system which will collapse the present thirteen administrative healthcare regions into five BUs, among them, the Southern BU which will include the Jazan, Najran, Aseer, and Bisha regions. The goals of the new Model of Care (MoC) include several strategies that will close any gaps that exist in accessibility, quality, distribution of resources, prevention, workforce training, technology, primary care access, and efficiency for all Saudi citizens regardless of their region of residence.12 As the pandemic continues, we must have an accurate assessment of how the situation unfolded in healthcare by tracking LoS as well as costs to determine what circumstances should be addressed in light of the new MoC under vision 2030 to build a resilient healthcare system moving forward.
A great many studies of hospital LoS reporting a vast range of days from 4–53, depending on country and timing, have been conducted both internationally and domestically over the course of this pandemic.7–9,13,14 A study in the KSA of cases during a four-month period from mid-March to mid-July 2020 observed a mean LoS of 11.85 days with a range of 9.3–13.3 days depending on the region.15 Several factors have been identified as having an association with LoS. Comorbidities have an impact on LoS, ICU admission, and mortality; for example, several international studies observed increased LoS in patients with uncontrolled DM214,16–18 although one study in Iran did not find DM2 by itself to be statistically significant in affecting LoS.19 Comorbidities that have been linked to LoS by some investigators are hypertension (HTN), renal disease, chronic obstructive pulmonary disease (COPD), Type 2 diabetes mellitus (DM2), liver disease, fever on admission, congestive heart failure (CHF), coronary heart disease, several elevated blood chemistries, and others.14–16,18,20–22 Advanced age was particularly noted by many studies during the first year of the COVID-19 pandemic to be a major factor in LoS as were some other demographic characteristics such as sex and socio-economic status.13,17–19,21,22
Many investigators have observed clinical complications arising from COVID-19 infection as factors in LoS. These complications include acute respiratory distress syndrome (ARDS), multi-organ failure, severe pneumonia, sepsis, acute kidney or liver injury, and hyperglycemia.13,14,16,18,20,22 A study using LoS to compare how well the USA, Italy, and Germany handled the pandemic at the beginning showed that the number of days between diagnosis and death varied significantly between the three countries.23 Ours will be the first study to examine regional differences in factors related to hospital LoS in the SBU filling a crucial gap in knowledge needed to provide equitable high-quality healthcare across all four regions of the SBU.
The objective of this study was to assess whether there is any variation in LoS and related factors for COVID-19 inpatients among the four regions of the SBU. As the KSA is moving forward with Vision 2030 and its new MoC, the business units will become fully responsible to provide equity in the quality of medical care among all regions within the business unit. This is the first study to analyze the variation in LoS in the SBU. We hypothesized that our study would observe some degree of variation in LoS among the regions of the SBU. Understanding LoS as a quality indicator will aid policymakers as they continue the implementation of the new MoC.
Methodology
Design, Participants and Setting
We analyzed the MoH data of 1113 inpatients with confirmed COVID-19 in several public hospitals that had been designated to care for COVID-19 patients in the southern KSA. Participants were hospitalized patients with COVID-19 from several hospitals in the Bisha, Jazan, Najran, and Aseer regions of the SBU during the 12 months from March, 2020 to February, 2021. Participants were inpatients with COVID-19 from several hospitals in Bisha, Jazan, Najran, and Aseer regions of the SBU. The sample included all ages, however, there was very little data on inpatients under age 18 since it was rare for that age group to be hospitalized for COVID-19. The care of COVID-19 inpatients was universally provided free of charge for all persons in the KSA at Hospitals assigned by the MoH to treat COVID-19 patients. Patients were triaged at initial admission by severity as Stage A, B, or C. Stage A includes any patient who was either: (1) a suspicious case of COVID-19 with mild to moderate symptoms and a high-risk condition, or (2) a PCR confirmed case of COVID-19 and had mild to moderate symptoms. Stage B includes any patient who was a PCR confirmed case of COVID-19 and had severe symptoms. Stage C includes any patient who was a PCR confirmed case of COVID-19 and had critical symptoms.24
Data Source and Measures
The MoH collected data from all hospitals on inpatients with confirmed COVID-19 and our comparative retrospective study utilized only the data from the southern regions of KSA. Our study included 1113 randomly selected inpatients with confirmed COVID-19, from several hospitals in the SBU which includes Bisha, Aseer, Jazan, and Najran regions. The variables included socio-demographics, comorbidities, patient outcomes, and complications arising from COVID-19.
Statistical Analysis
Data were analyzed and tested in a multi-step process, applying standard statistical methods including, Chi-Square test, one-way ANOVA, independent sample t-test, and comparative and descriptive statistics. We first compared patient characteristics among the four regions using descriptive statistics and we then used linear regression to assess the variation in LoS. To meet the assumption of normal distribution by the statistical models, the LoS data were then subjected to natural log transformation. To measure the association of other variables with LoS, multivariable linear regression with forward stepwise selection was performed on demographics, comorbidities, and complications. The software used for all analyses was Stata version 14. Tests were two-sided and a p-value ≤ 0.05 was statistically significant. Finally, we tested sensitivity by running five models; the first of which was the entire sample, the second included all participants except ICU admissions, the third included all participants except those who died in hospital, the fourth included all participants except ICU admissions and died in hospital, and the fifth included all except transferred participants. The independent variable of interest was a region of the SBU which is a categorical variable reported as a percentage and is as follows: 0 = Bisha (Reference), 1 = Jazan, 2 = Najran, and 3 = Aseer. Binary variables included gender; nationality; comorbidities such as DM2, HTN, obesity, cardiac diseases, immunocompromised, and history of cancer; COVID-19 complications such as sepsis, bacterial pneumonia, ARDS, arrhythmia, acute kidney injury, hepatotoxicity, GIT perforation, and multi-organ failure; and inpatient outcomes including death, ICU admission, and referral to another facility. Continuous variables reported as means and standard deviation included age and length of stay. The Bisha region, having the most inpatients, was utilized as our reference for all variables.
Results
Table 1 presents the participant characteristics categorized by region in the SBU. The mean age of the total sample of 1113 was almost 60 years and compared to Bisha (59 yrs) (REF), it was significantly lower (56 yrs) in Jazan and significantly higher (63 yrs) in Najran while Aseer was the same as the reference (p <0.03). Males represented two-thirds of overall participants but were significantly higher at three fourths of participants in Jazan and Aseer (p <0.02). Participants were majority Saudi with statistically significant differences between regions (p =0.001). Pre-existing medical conditions showed statistically significant differences among regions with Najran and Aseer having significantly higher rates of DM2 (11% and 9%), HTN (12% and 8%), obesity (20 and 18 fold), cardiac diseases (20% and 2%), and immunocompromised conditions (2% and 1%) than Bisha (the reference). Jazan had statistically higher rates of obesity (7 fold), cardiac diseases (3%), and immunocompromised conditions (7%) as the reference but lower or equal rates of DM2 and HTN.
 |
Table 1 Demographic and Clinical Characteristics of COVID-19 Inpatients in the Four Regions of the SBU |
Table 2 presents complications of COVID-19 infection and clinical outcomes among the four regions of the SBU. Of the 1113 participants, at admission the majority (62%) presented as stage B, 27% were stage A and 11% were stage C. Compared to Bisha (REF) with 80% in Stage B and only 5% in Stage C, there were significant differences in the admission status among the other three regions. Of the total sample, almost two thirds were discharged to home while 22% died in hospital and 7% were referred to other facilities. We observed statistically significant differences between the regions in the discharge status, compared to the 86% discharge to home of the reference, Jazan experienced 68%, Najran only 45%, and Aseer only 58% (p <0.001). Compared to the reference’s 14% deaths in hospital, Jazan and Aseer had nearly double the rate at 26% and 27%, respectively, while Najran had nearly triple the rate at 39% (p <0.001). While the reference referred less than 1% to other facilities, other regions had significantly higher referral rates. Admission to ICU revealed significant statistical differences between regions in which just under half of the total sample were admitted to ICU. Compared to the reference at approximately 30%, admission to ICU was 10% higher in Jazan and more than double in Najran and Aseer (p <0.001). There were statistically significant differences among regions in regards to complications developing from COVID-19 infection. Overall occurrence of sepsis was less than one fifth, bacterial pneumonia was nearly three fourths, ARDS was just over one fourth, acute kidney injury and multiorgan failure were nearly one seventh, arrhythmia was only 4%, and hepatotoxicity and GIT perforation were only 1%. Compared to the reference, Najran had two and a half to six times the rate of all complications except bacterial pneumonia; Aseer had two and a half to five times the rate of complications except bacterial pneumonia, arrhythmia, hepatotoxicity, and GI perforation; and Jazan had approximately double the rate of ARDS, arrhythmia, and acute kidney injury; and four times the rate of hepatotoxicity but had lower or the same rates in all others.
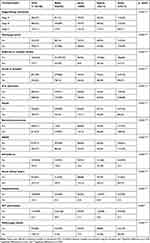 |
Table 2 Clinical Course, Outcomes, and Complications of COVID-19 Inpatients in the Four Regions of the SBU |
Table 3 presents the mean LoS delineated into four categories, total sample, transferred patients, ICU admissions, and in-hospital deaths. LoS for the total sample was slightly more than 10 days, for transferred patients just over 13, for ICU admissions just over 14, and for patients who died in hospital just over 15 making the LoS range for all categories of the total sample just over 10 to just over 15 days. One-way ANOVA applied to the sample revealed statistically significant differences in LoS among the regions of the SBU in all categories except LoS for transferred patients. Compared to the overall LoS in Bisha (reference), overall LoS in Jazan was three days longer, in Najran was nearly eight days longer, and in Aseer was nearly six days longer (p <0.0001). Compared to the ICU LoS in the reference region, ICU LoS in Jazan was one day longer, in Najran was more than five days longer, and in Aseer was almost four days longer (p <0.0001). Compared to the LoS for hospital deaths in the reference region, LoS in Jazan was more than one day shorter, in Najran was more than six days longer, and in Aseer was more than three days longer (p ≤0.0004).
 |
Table 3 Mean LoS for Inpatient Clinical Outcomes in the Four Regions in the SBU |
Table 4 presents results from the multiple linear regression analysis of the factors associated with the length of stay in the four regions of the SBU. Compared to patients admitted in Bisha, and controlling for chronic diseases and complications, the estimated average LoS for inpatients admitted in all three of the other regions are significantly longer; 34% in Jazan, 62% in Najran, and 40% in Aseer (p value ≤ 0.001). Other variables having a significant association with longer LoS (compared to reference) were nationality in which compared to Non-Saudi patients’ Saudi patients had a 15% shorter LoS, admission to ICU which had a 57% longer LoS (p value ≤ 0.005), and death during admission with a 39% shorter LoS (p <0.001). COVID-19 complications having a statistically significant association with LoS were Acute Kidney Injury with 22% longer LoS (p ≤0.01), and ARDS with a 48% longer LoS (p <0.0001).
 |
Table 4 Multiple Linear Regression Analysis of the Factors Associated with the Length of Stay in the Four Regions of the SBU |
Table 5 presents a sensitivity analysis to perform an in-depth investigation into the differentials in LoS in all four regions of the SBU. Compared to Bisha (reference), all other regions had significantly longer LoS (p-value ≤ (p <0.001) for all of the models). Because the results are similar, we can conclude that the patient subsets are unlikely to bias the results obtained from using the entire sample.
 |
Table 5 Sensitivity Analysis Models Predicting the COVID-19 Inpatient LoS in the Four Regions of the SBU |
Discussion
To our knowledge this is the first study of regional differences in COVID-19 LoS among the four regions of the SBU. This cross-sectional retrospective study investigated the LoS for 1113 inpatients with confirmed COVID-19 admitted to several hospitals within the four regions of the SBU over the one-year period of March, 2020 to February, 2021. We used parameters of demographics, comorbidities, and complications of COVID-19 as factors to assess whether there were differences in LoS among the four regions which includes Bisha, Jazan, Najran, and Aseer.
After adjusting for known demographic and disease severity characteristics that may have affected the LoS among patients with COVID-19 our study revealed a mean LoS for the total sample of just over 10 days which is shorter than that observed by most international studies,7,9,13 but similar to a recent study of all regions in the KSA.15 Linear regression analysis revealed a statistically significant association between region and LoS and compared to Bisha (reference) at just over seven days, Jazan had just over 10 days (34% longer), Najran had 15 days (62% longer) and Aseer had 13 days (40% longer) (Tables 3 and 4).
Overall LoS for ICU admissions was just over 14 days and Bisha (reference) had a shorter ICU LoS at just under 12 days, while compared to the reference, the remaining three regions had statistically significant prolonged ICU LoS with Jazan at almost 13 days, Najran at just over 17 days, and Aseer at just over 15 days (Table 3). Our findings for prolonged LoS in ICU admissions aligns with the findings of other scholars.15,18,22 We found statistically significant differences and prolonged LoS among patients who died in hospital with the overall sample experiencing just over 15 days and Bisha with almost 13 days (Table 3). Compared to the reference, hospital deaths in Jazan had a significantly shorter LoS at just over 11 days while Najran and Aseer had a significantly longer LoS at just under 20 and 17 days, respectively (Table 3).
Additionally, linear regression showed a statistically significant association between some other variables and LoS compared to the references including nationality with a 15% shorter LoS for Saudi patients compared to non-Saudi patients, admission to ICU had a 57% longer LoS (p value ≤ 0.005), and death during admission had a 39% shorter LoS, in spite of two regions being significantly longer. COVID-19 complications having a statistically significant association with LoS were Acute Kidney Injury with 22% prolonged LoS, and ARDS with a 48% prolonged LoS (Table 4). Comorbidities did not have a statistically significant relationship to LoS.
Our statistical model ruled out other factors that might potentially explain the LoS regional variation by controlling for the confounding variables of demographic and clinical characteristics of our participants. Our results confirm that the primary factor associated with SBU regional variations in LoS is the difference in each region’s quality of healthcare since the aforementioned confounders do not account for it statistically. Our findings are consistent with other studies that found variations in quality of care between and within many countries,15,24–26 however, a study of a young cohort in a Texas healthcare system did not find variation based on the patient’s location.27
Although controlling for other confounding factors leaves the region as the primary factor in LoS variation, a pattern has emerged of how these regional differences manifest. We observed several differences in the distribution of the known risk factors for the development of more serious COVID-19. Advanced age is a well-documented factor and we observed that the participants in Najran were significantly older than the other regions (Table 1).28,29 Our observation that Najran and Aseer had the most associated risk factors including sociodemographic, comorbidities, complications, and clinical outcomes for increased severity of COVID-19 while Bisha had the lowest may provide a partial explanation for Najran and Aseer having the longest LoS and Bisha having the shortest LoS consistent with studies showing an association between pre-existing conditions such as HTN, obesity, and DM2 and the severity of disease.15,24,30–37 National studies have also documented the association of complications of COVID-19 and severity of disease such as LoS and outcomes.15,24,30 Our study revealed that the complications of sepsis, ARDS, Arrhythmia, and acute kidney injury that led to prolonged LoS were highest in Najran and 2nd highest in Aseer, while the order was reversed in multiorgan failure (Table 2). By comparison, Bisha and Jazan were lower in overall complications. Likewise, clinical outcomes were observed to be significantly worse in Najran and Aseer. Mortality rates in descending order were Najran, Aseer, Jazan, and Bisha (Table 2); ICU admission rates in descending order were Aseer, Najran, Jazan, and Bisha. These factors that represent quality of care are linked to LoS and demonstrate the true impact of regional variations in quality of healthcare. There may be many other factors outside the scope of this study that impacted LoS in these regions such as a delay in seeking medical care, a delay in diagnosis, such as a study in Dakar which showed38 structural differences, or differences in peak infection times. Although the government of the KSA standardized protocols and provided resources to all of the KSA according to the recommendations of the WHO and the Centers for Disease Control in Atlanta, GA, USA; and also provided free care to all, there may still have been some lag in availability of resources depending on peak infection rates.
LoS is a quality indicator for utilization and outcome and is impacted by variables at many levels including patient, facility, and system.39 Further studies should be conducted to look more deeply into the reasons for increased comorbidities, complications, and worse outcomes in Najran and Aseer. Future studies should investigate other clinical and severity outcomes among regions such as variations in mortality rate, ICU admission rate, complication rate, and others among regions of the SBU and other business units. Studies are needed as well to examine structural, process, resource, and patient level variables affecting health care quality. Additional research is needed to ascertain methods to estimate LoS for planning purposes for future pandemics such as that undertaken in England for COVID-19 in which modeling of three methods explored the difference between the methods using both local and national data.11 Finally, based on our findings, we recommend that factors such as equitable resource distribution and other structural issues be strengthened to improve the quality of healthcare in all of the four regions of the SBU to meet the standards of the new MoC in Vision 2030.
Strengths
This retrospective study has a high degree of validity as it examines data from real inpatient cases for a period of one year which included the varying peak for each region. This was a multi-center study that included COVID-19 inpatients from eight hospitals making it relatively comprehensive and generalizable and will be a useful study for others to use to examine LoS in other settings. The sensitivity analyses for all models that we conducted provide strength to our observations as they all arrived at the same results. Our results are based on patient data rich confounders which we tested to verify the impact of these factors. All regions followed the same treatment protocols and guidelines, therefore, the difference in LoS must be explained by other factors between the regions such as care provision, resources, or infrastructure.
Limitations
We recognize that this study also contains some limitations including a cross-sectional design which admits the possibility of bias. Although we have many variables included in our study, there are many others outside our scope such as pre-existing infrastructural differences between the regions and other hospital circumstances we have not accounted for that may have impacted both the severity of COVID-19 and LoS. In spite of these limitations, we believe this is an important study to assess preparedness for transformation to the new MoC and to measure progress during this transformation.
Conclusions
This is the first study of LoS for COVID-19 inpatients in the four regions of the SBU that examined the data gathered over the entire first year of the pandemic. We found statistically significant variation among the regions using Bisha as a reference. Using linear regression and adjusting for demographic and clinical factors we observed that compared to Bisha (reference), LoS was 32% longer in Jazan, 64% longer in Najran, and 40% longer in Aseer (Table 4). Having controlled for them, other factors such as demographic characteristics, comorbidities, and complications did not explain these differences. Future studies should be directed at the level of clinical decision making and organizational protocols at the micro level as well as at regional structural factors and policies at the macro level to ascertain the underlying causes in these variations in LoS among the four regions of the SBU.
Abbreviations
LoS, length of stay; SBU, Southern Business Unit; KSA, Kingdom of Saudi Arabia; ICU, intensive care unit; CI, confidence interval; OR, odds ratio; HTN, hypertension; ARDS, acute respiratory distress syndrome; MoH, Ministry of Health; GIT, gastrointestinal tract.
Ethical Approval
Institutional Review Board Statement: Hospitals who reported the data to the MOH obtained, and the Clinical Excellence General Directorate of the MOH owned the data provided based on ethical approval from The Central Institutional Review Board of the MOH for providing the ethics review number IRB- log No: 20-163E. Informed Consent Statement: Data were taken from the Clinical Excellence General Directorate of the MOH Data Availability Statement: The data presented in this study are available on request from the corresponding author. Data were maintained in accordance with the Declaration of Helsinki.
Acknowledgments
The authors are grateful to the following for making this study possible. The King Abdulaziz City for Science and Technology (KACST) for supporting. The Clinical Excellence General Directorate of the MoH for making the data available. The Central Institutional Review Board and the General Administration for Research and Studies for providing the ethics review.
Funding
This study did not receive any specific grant from funding agencies in the public, Profit, or not-for-profit sectors.
Disclosure
The authors declare that they have no competing interests.
References
1. Wang C, Horby PW, Hayden FG, Gao GF. A novel coronavirus outbreak of global health concern. Lancet. 2020;395(10223):470–473. doi:10.1016/S0140-6736(20)30185-9
2. Ciotti M, Ciccozzi M, Terrinoni A, Jiang WC, Wang CB, Bernardini S. The COVID-19 pandemic. Crit Rev Clin Lab Sci. 2020;57(6):365–388. doi:10.1080/10408363.2020.1783198
3. McKay B, Calfas J, Ansari T. Coronavirus Declared Pandemic by World Health Organization. The Wall Street Journal; 2020.
4. Li X, Wang W, Zhao X, et al. Transmission dynamics and evolutionary history of 2019-nCoV. J Med Virol. 2020;92(5):501–511. doi:10.1002/jmv.25701
5. World Health Organization. COVID-19 weekly epidemiological update; 2021. Available from: https://www.who.int/publications/m/item/weekly-epidemiological-update-on-covid-19—13-july-2021.
6. Medicine JHU. COVID-19 case tracker; 2021. Available from: https://coronavirus.jhu.edu/.
7. Rees EM, Nightingale ES, Jafari Y, et al. COVID-19 length of hospital stay: a systematic review and data synthesis. BMC Med. 2020;18(1):270. doi:10.1186/s12916-020-01726-3
8. Liu X, Zhou H, Zhou Y, et al. Risk factors associated with disease severity and length of hospital stay in COVID-19 patients. J Infect. 2020;81(1):e95–e97. doi:10.1016/j.jinf.2020.04.008
9. Tsai Y, Vogt TM, Zhou F. Patient characteristics and costs associated with COVID-19–related medical care among Medicare fee-for-service beneficiaries. Ann Intern Med. 2021;174:1101–1109. doi:10.7326/M21-1102
10. Khan AA, AlRuthia Y, Balkhi B, et al. Survival and estimation of direct medical costs of hospitalized COVID-19 patients in the Kingdom of Saudi Arabia. Int J Environ Res Public Health. 2020;17(20):7458. doi:10.3390/ijerph17207458
11. Vekaria B, Overton C, Wiśniowski A, et al. Hospital length of stay for COVID-19 patients: data-driven methods for forward planning. BMC Infect Dis. 2021;21(1):1–15. doi:10.1186/s12879-021-06371-6
12. Health Mo. Healthcare transformation strategy. Updated 20 /February/ 2019; 2021. Available from: https://www.moh.gov.sa/en/Ministry/vro/Pages/Health-Transformation-Strategy.aspx.
13. Wu C, Chen X, Cai Y, et al. Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med. 2020;180(7):934–943. doi:10.1001/jamainternmed.2020.0994
14. Tee LY, Alhamid SM, Tan JL, et al. COVID-19 and undiagnosed pre-diabetes or diabetes mellitus among international migrant workers in Singapore. Front Public Health. 2020;8. doi:10.3389/fpubh.2020.584249
15. Alharbi AA, Alqassim AY, Alharbi AA, et al. Variations in length of stay of inpatients with COVID-19: a nationwide test of the new model of care under vision 2030 in Saudi Arabia. Saudi J Biol Sci. 2021;28:6631–6638. doi:10.1016/j.sjbs.2021.07.040
16. Bode B, Garrett V, Messler J, et al. Glycemic characteristics and clinical outcomes of COVID-19 patients hospitalized in the United States. J Diabetes Sci Technol. 2020;14(4):813–821. doi:10.1177/1932296820924469
17. Wang S, Ma P, Zhang S, et al. Fasting blood glucose at admission is an independent predictor for 28-day mortality in patients with COVID-19 without previous diagnosis of diabetes: a multi-centre retrospective study. Diabetologia. 2020;63(10):2102–2111. doi:10.1007/s00125-020-05209-1
18. Saand AR, Flores M, Kewan T, et al. Does inpatient hyperglycemia predict a worse outcome in COVID‐19 intensive care unit patients? J Diabetes. 2021;13(3):253–260. doi:10.1111/1753-0407.13137
19. Mansour A, Sajjadi-Jazi SM, Kasaeian A, et al. Clinical characteristics and outcomes of diabetics hospitalized for COVID-19 infection: a single-centered, retrospective, observational study. EXCLI J. 2020;19:1533. doi:10.17179/excli2020-2988
20. Guo A, Lu J, Tan H, et al. Risk factors on admission associated with hospital length of stay in patients with COVID-19: a retrospective cohort study. Sci Rep. 2021;11(1):1–7. doi:10.1038/s41598-020-79139-8
21. Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395(10229):1054–1062. doi:10.1016/S0140-6736(20)30566-3
22. Alwafi H, Naser AY, Qanash S, et al. Predictors of length of hospital stay, mortality, and outcomes among hospitalised COVID-19 patients in Saudi Arabia: a cross-sectional study. J Multidiscip Healthc. 2021;14:839. doi:10.2147/JMDH.S304788
23. Jamshidi B, Jamshidi Zargaran S, Bekrizadeh H, Rezaei M, Najafi F. Comparing length of hospital stay during COVID-19 pandemic in the USA, Italy and Germany. Int J Qual Health Care. 2021;33(1):mzab050. doi:10.1093/intqhc/mzab050
24. Alharbi AA, Alqassim AY, Gosadi IM, et al. Regional differences in COVID-19 ICU admission rates in the Kingdom of Saudi Arabia: a simulation of the new model of care under vision 2030. J Infect Public Health. 2021;14(6):717–723. doi:10.1016/j.jiph.2021.04.012
25. Corallo AN, Croxford R, Goodman DC, Bryan EL, Srivastava D, Stukel TA. A systematic review of medical practice variation in OECD countries. Health Policy. 2014;114(1):5–14. doi:10.1016/j.healthpol.2013.08.002
26. Du P, Li D, Wang A, Shen S, Ma Z, Li X. A systematic review and meta-analysis of risk factors associated with severity and death in COVID-19 patients. Can J Infect Dis Med Microbiol. 2021;2021:1–12. doi:10.1155/2021/6660930
27. Sandoval M, Nguyen DT, Vahidy FS, Graviss EA. Risk factors for severity of COVID-19 in hospital patients age 18–29 years. PLoS One. 2021;16(7):e0255544. doi:10.1371/journal.pone.0255544
28. Liu Y-C, Kuo R-L, Shih S-R. COVID-19: the first documented coronavirus pandemic in history. Biomed J. 2020;43(4):328–333. doi:10.1016/j.bj.2020.04.007
29. Abate SM, Ahmed Ali S, Mantfardo B, Basu B. Rate of Intensive Care Unit admission and outcomes among patients with coronavirus: a systematic review and meta-analysis. PLoS One. 2020;15(7):e0235653. doi:10.1371/journal.pone.0235653
30. Alharbi AA, Alqassim AY, Muaddi MA, Alghamdi SS. Regional differences in COVID-19 mortality rates in the Kingdom of Saudi Arabia: a simulation of the new model of care. Cureus. 2021;13(12):e20797.
31. Smith AA, Fridling J, Ibrahim D, Porter PS. Identifying patients at greatest risk of mortality due to COVID-19: a New England perspective. West J Emerg Med. 2020;21(4):785.
32. Elezkurtaj S, Greuel S, Ihlow J, et al. Causes of death and comorbidities in hospitalized patients with COVID-19. Sci Rep. 2021;11(1):1–9. doi:10.1038/s41598-021-82862-5
33. Chen L, Liu S, Tian J, et al. Disease progression patterns and risk factors associated with mortality in deceased patients with COVID‐19 in Hubei Province, China. Immun Inflamm Dis. 2020;8(4):584–594. doi:10.1002/iid3.343
34. Ciceri F, Castagna A, Rovere-Querini P, et al. Early predictors of clinical outcomes of COVID-19 outbreak in Milan, Italy. Clin Immunol. 2020;217:108509. doi:10.1016/j.clim.2020.108509
35. Soares CM, Mattos LR, Raposo LM. Risk factors for hospitalization and mortality due to COVID-19 in Espírito Santo State, Brazil. Am J Trop Med Hyg. 2020;103(3):1184. doi:10.4269/ajtmh.20-0483
36. Nikpouraghdam M, Farahani AJ, Alishiri G, et al. Epidemiological characteristics of coronavirus disease 2019 (COVID-19) patients in Iran: a single center study. J Clin Virol. 2020;127:104378. doi:10.1016/j.jcv.2020.104378
37. Salacup G, Lo KB, Gul F, et al. Characteristics and clinical outcomes of COVID‐19 patients in an underserved‐inner city population: a single tertiary center cohort. J Med Virol. 2021;93(1):416–423. doi:10.1002/jmv.26252
38. Diop M, Ba PS, Lo M, Essomba N, Fall B. Factors associated with severe COVID-19 in an Epidemic Treatment Center at Dakar. J Infect Dis Epidemiol. 2021;7(7). doi:10.23937/2474-3658/1510203
39. Setareh M, Alavi NM, Atoof F. Severity of illness affecting the length of stay and outcomes in patients admitted to intensive care units, Iran, 2019. J Educ Health Promot. 2021;10. doi:10.4103/jehp.jehp_780_20
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
