Back to Journals » Clinical Epidemiology » Volume 10
High-potency statins but not all statins decrease the risk of new-onset osteoporotic fractures: a nationwide population-based longitudinal cohort study
Authors Lin TK, Liou YS, Lin CH, Chou P, Jong GP
Received 1 July 2017
Accepted for publication 14 December 2017
Published 18 January 2018 Volume 2018:10 Pages 159—165
DOI https://doi.org/10.2147/CLEP.S145311
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Irene Petersen
Tsung-Kun Lin,1,2 Yi-Sheng Liou,3,4 Ching-Heng Lin,5 Pesus Chou,2 Gwo-Ping Jong6
1Department of Pharmacy, Taoyuan Armed Forces General Hospital, Taoyuan, 2Institute of Public Health and Community Medicine Research Center, National Yang-Ming University, Taipei, 3Department of Family Medicine and Geriatrics, Taichung Veteran General Hospital, Taichung, 4School of Public Health, National Defense Medical Center, Taipei, 5Department of Medical Research, Taichung Veterans General Hospital, Taichung, 6Division of Internal Cardiology, Chung Shan Medical University Hospital, Chung Shan Medical University, Taichung, Taiwan, Republic of China
Background: Statins have been linked to new-onset osteoporotic fractures (NOFs), and different statins may alter the risk for the development of NOFs.
Aim: In this study, we investigated the association between different statins and the development of NOFs.
Patients and methods: This was a longitudinal cohort study performed using data from claim forms submitted to the Taiwan Bureau of National Health Insurance, including case patients with NOFs from January 2004 to December 2013 and non-NOF subjects. We estimated the hazard ratios (HRs) of NOFs associated with statin use. Nonuser subjects served as the reference group.
Results: A total of 44,405 patients with NOFs were identified from among 170,533 patients with hyperlipidemia during the study period. The risk of developing NOFs after adjusting for age, sex, comorbidities, and concurrent medication use was lower among users of atorvastatin (HR, 0.77; 95% CI, 0.71–0.84) and rosuvastatin (HR, 0.72; 95% CI, 0.64–0.81) than among simvastatin users. Lovastatin, pravastatin, fluvastatin, and pitavastatin were not associated with the risk of developing NOFs compared with simvastatin users.
Conclusion: This study supports previous reports regarding a beneficial effect of statin use and NOF risk, but not all statins. Patients taking atorvastatin or rosuvastatin were at lower risk of developing NOFs compared with simvastatin users during the 10-year follow-up. Other statins such as pravastatin, fluvastatin, lovastatin, and pitavastatin were not associated with NOFs. This study also highlighted that high-potency statin has a dose–response effect on lower NOF risk.
Keywords: statins, new-onset osteoporosis fracture, hyperlipidemia
Background
The incidence of osteoporotic fractures is increasing worldwide, especially in developed and developing countries.1,2 An estimated 9 million osteoporotic fractures were reported worldwide in 2000, and fractures of the hip and spine were found to be associated with an increased mortality rate of 10%–20%.3 Furthermore, recent reports estimate that the expected burden of osteoporotic fractures will increase by 20% by 2020 only in postmenopausal women.4,5 Concerns regarding the health care of osteoporotic fractures, particularly in terms of new-onset osteoporotic fractures (NOFs), have gradually increased worldwide.6,7 Moreover, osteoporotic fractures may result in significant health care costs8 because they have been shown to adversely affect the health-related quality of life, including limitation of ambulation, depression, loss of independence, and chronic pain and have become a major public health burden.9
Statins are effective agents to control hyperlipidemia and are widely used in the prevention of cardiovascular diseases.10,11 In particular, statins may influence bone metabolism by increasing bone formation.12 Recently, several randomized trials have led to a debate on whether the use of statins is associated with a lower risk of developing NOFs in hyperlipidemic patients undergoing treatment.13–18 However, the results of these studies are inconsistent, partly because of the inability to completely adjust for risk factors in baseline characteristics between statin users and nonusers or the short follow-up periods.19,20 It is also unclear whether different statins are associated with a lower risk of developing NOFs when compared with other statins in patients with hyperlipidemia during long-term follow-up. Therefore, the objective of this retrospective cohort study was to investigate the effect of different statins (simvastatin, pravastatin, lovastatin, fluvastatin, atorvastatin, rosuvastatin, and pitavastatin) on the risk of developing NOFs among hyperlipidemic patients in Taiwan.
Patients and methods
Study population
Data were collected from claim forms of the Taiwan National Health Insurance (NHI) that had been submitted to the Taiwan Bureau of National Health Insurance from 2002 to 2013. The Taiwan NHI program has been operating since 1995 and represents ~99% of Taiwan’s population. The claim forms contain inpatient and outpatient records. The information from the claim forms is stored in two tables, a visit table and a prescription table. Visit tables contain patient identification numbers, sex, age, three diagnostic codes, medical expenditures, and hospital and physician information. Prescription tables contain the quantity and expenditure of all drugs, surgeries, and treatments. Patients were included in the study if they had been diagnosed with hyperlipidemia and were statin users without osteoporotic fractures at baseline (January 1, 2004). Statin users were those patients who received at least a 180-day statin prescription during the period between January 1, 2004, and December 31, 2004. Nonusers were those patients who did not receive a statin prescription throughout the whole study period. We summarized the claim records of each patient into one record.
Study design
Participants were included in the study if they had been diagnosed with hyperlipidemia (International Classification of Diseases, Ninth Revision, Clinical Modification [ICD-9-CM] code 272) between January 1, 2004, and June 30, 2004. At least one of the following enrollment criteria had to be met for inclusion in the study: 1) two or more outpatient visits within a 6-month period, 2) all prescriptions of statins continuously administered to the patients for >6 months within a 10-year follow-up period, or 3) one or more inpatient admissions with a diagnosis of hyperlipidemia. The primary endpoint was the development of NOFs, which was defined by the time an osteoporotic fracture (ICD-9-CM codes 733.11 and 805–829) or a fracture-related surgery (ICD-9-CM codes 78.1, 78.4, 78.5, 78.9, 79, and 81) first appeared in the inpatient or outpatient claim records. Comorbidities related to osteoporotic fractures were defined according to the ICD-9-CM code and included coronary artery disease (ICD-9-CM code 410–415), hypertension (ICD-9-CM code 401–405), diabetes mellitus (ICD-9-CM code 250), alcohol-related disorders (ICD-9-CM codes 291, 303, 305, 571.0, 571.1, 571.2, 571.3, 790.3, and V11.3), chronic obstructive pulmonary disease (COPD) (ICD-9-CM codes 490–492 and 496), hyperthyroidism (ICD-9-CM code 242), liver cirrhosis (ICD-9-CM codes 571.5 and 571.6), stroke (ICD-9-CM code 430–438), and chronic kidney disease (ICD-9-CM code 585). Statins are available only by prescription in Taiwan. Patients using only one type of statins before the development of NOFs were categorized as single users based on the type of statin prescribed, including simvastatin, pravastatin, lovastatin, fluvastatin, atorvastatin, rosuvastatin, and pitavastatin. Patients who fulfilled any of the following criteria were excluded from the study: 1) had a prior history of an osteoporotic fracture or a fracture-related surgery before January 1, 2004, 2) patients taking calcium supplements, biphosphates, selective serotonin-specific reuptake inhibitors, serotonin–norepinephrine reuptake inhibitors, tricyclic antidepressants, estrogen, or calcitonin, and 3) patients suffering from other major medical problems, leaving those with a life expectancy of <6 months. Individuals in our nonuser statin group did not receive statin during the entire study period but were administered diet control, niacin, or fibrates for the treatment of hyperlipidemia. Initially, 177,151 outpatients fulfilled the inclusion criteria; however, 3,320 patients were excluded based on the diagnosis of an osteoporotic fracture before January 1, 2004. Therefore, a total of 173,831 patients were enrolled in the study at baseline (Figure 1). Furthermore, 2,045 patients who were lost to follow-up and 1,253 patients who died without the diagnosis of NOFs or NOF-related deaths were excluded. Finally, a total of 170,533 outpatients were included in this study. This study was approved by the ethics committee of Chung Shan Medical University Hospital (CS2-16086). Due to all patients’ records/information being de-identified, a patient consent to review their medical claim records was not required by the ethics committee of Chung Shan Medical University Hospital (CS2-15104).
  | Figure 1 Flowchart of selection of patients for the inclusion in this study. |
Statins are used to reduce the risk of cardiovascular events and are classified as high, moderate, or low intensity depending on the potency with which they reduce low-density lipoprotein cholesterol (LDL-cholesterol).21 High potency statin treatment was defined as at least 10 mg rosuvastatin and at least 20 mg atorvastatin; all other statin treatments were defined as having low to moderate potency. The toxic doses of statins were defined as >40 mg rosuvastatin, >80 mg atorvastatin, >80mg lovastatin, >80 mg fluvastatin, >80 mg pravastatin, >4 mg pitavastatin, and >40 mg simvastatin. Currently, in Taiwan, seven kinds of statins (high-potency atorvastatin and rosuvastatin and low- to moderate-potency fluvastatin, pravastatin, pitavastatin, and simvastatin) are used; however, the standard statin dose in Taiwan is lower than that in the American College of Cardiology/ American Heart Association guidelines.21
Statistical analysis
The basic information of the study cohort includes mean and standard deviation (SD) for age and duration of statin prescription, presented as number and percentage for sex, along with baseline comorbidity and medication. Student’s t-test and chi-square tests were used to evaluate whether there was a significant difference between statin-treated and statin nonusers. The NOF-free survival rates of the two groups were estimated by the Kaplan–Meier method using the log-rank test. This study aimed to examine the association between the use of certain types of statins and the risk of developing NOFs. The Cox proportional hazard regression model was used to compare the risk of NOF development between statin users and nonusers. The Cox proportional hazard regression model was also used to compare the risk of NOF development between different statins using simvastatin as reference group. Adjusted hazard ratios (HRs) and 95% confidence intervals (CIs) were calculated, adjusting for important risk factors for the development of osteoporotic fractures, including age, sex, comorbidities, and concurrent medication use. P-values <0.05 were considered to be statistically significant. All statistical calculations were performed using statistical analysis software, version 9.3 (SAS Institute Inc., Cary, NC, USA).
Results
Baseline characteristics of all patients
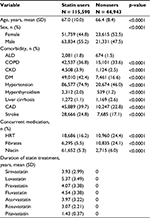
Baseline characteristics, comorbidities, and concurrent medication use among the overall study population are presented in Table 1. Among 170,533 eligible patients with defined hyperlipidemia, 44,405 (26.0%) developed NOFs from January 2004 to December 2013. There were more men than women in this study population. The mean age of patients with statin user group was 67.0 years and that of nonuser group was 66.4 years, which was statistically significantly different (p<0.0001).
Patients in the statin user group had more comorbidities, including alcohol-related disorders, COPD, chronic kidney disease, diabetes mellitus, hypertension, hyperthyroidism, liver cirrhosis, coronary artery disease, and stroke. There was a higher percentage of hormone replacement therapy, fibrates, and niacin users in the nonuser group than that in the statin user group. Regarding the duration of use of the statin subtype in this study, lovastatin was used for the longest duration and pitavastatin was used for the shortest duration.
Relative risk of NOF
Results of the Kaplan–Meier survival analysis are shown in Figure 2, which indicate that the risk of developing NOFs was significantly lower among statin users than that among the nonuser cohort (log-rank test; p<0.001).
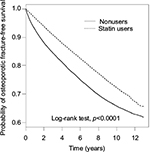  | Figure 2 Kaplan–Meier analysis comparing probabilities of osteoporotic fracture between statin users and nonusers. |
The analyses by defined daily doses (DDDs) indicated a tendency of decreasing risk for NOFs with increasing DDDs. The high DDDs (91–365 and ≥366) of statins showed a significantly lower risk for NOF development (crude HR, 0.37; 95% CI, 0.36–0.39; adjusted HR, 0.32; 95% CI, 0.31–0.34). Conversely, the low DDDs (<28) of statins revealed a significant association with the risk for NOF development (crude HR, 1.24; 95% CI, 1.18–1.30; adjusted HR, 1.07; 95% CI, 1.02–1.13).
The crude HR of developing NOFs was lower among nonusers (HR, 0.85; 95% CI, 0.80–0.91, Table 2) compared with simvastatin users. However, after adjusting for age, sex, comorbidities, and concurrent medication use, the risk for NOF development was not associated with the nonusers (HR, 0.99; 95% CI, 0.93–1.06, Table 2). Patients who took atorvastatin (crude HR, 0.76; 95% CI, 0.70–0.83; adjusted HR, 0.77; 95% CI, 0.71–0.84) and rosuvastatin (crude HR, 0.70; 95% CI, 0.62–0.79; adjusted HR, 0.72; 95% CI, 0.64–0.81) were at lower risk of developing NOFs compared to that of simvastatin users. Lovastatin, pravastatin, fluvastatin, and pitavastatin were not associated with the risk of developing NOFs compared with simvastatin users (p>0.05, Table 2). Finally, lipophilic and hydrophilic statins showed similar effects in patients with hyperlipidemia in terms of the risk of developing NOFs.
Discussion
This study indicated that the risk of developing NOFs was significantly lower among statin users than among nonusers, suggesting that using a statin continuously may have a potential impact of preventing the development of NOFs. This study also demonstrated that the use of atorvastatin and rosuvastatin was independently associated with a decreased risk of NOF development compared with simvastatin users in hyperlipidemic patients. Lovastatin, pravastatin, fluvastatin, and pitavastatin were not associated with the risk of NOF development compared to that of simvastatin users in patients with hyperlipidemia. Finally, the study also showed that statin has a dose–response effect on lower NOF risk.
In the current study, patients using high DDDs (91–365 or ≥366) of statin use were found to have a significantly protective effect against NOFs, whereas low DDDs of statin use were significantly associated with a higher risk of developing NOFs. It demonstrated that statin has a dose–response effect on lower NOF risk. To our knowledge, this is the first study to directly compare the incidence of osteoporotic fractures in patients treated with different statins. All the previous NOF studies were placebo-controlled or head-to-head comparison trials and had a short duration (2–5 years).13–18 These observational studies did not use a DDD for continuous prescription of statins. However, we are not certain whether our finding is consistent with those of observational studies. Additional studies using a DDD for continuous prescription of statins are required in the future.
In this study, pravastatin was not significantly associated with a decrease in the risk of NOF development compared with simvastatin users. This result is consistent with the results reported by Reid et al, who showed that the relative risk for NOF development in individuals taking pravastatin compared with those not taking statin was 0.94 (95% CI, 0.77–1.16).22 Similarly, Hippisley-Cox and Coupland also reported that pravastatin was not associated with a decreased risk of developing NOF (adjusted HR, 0.91; 95% CI, 0.75–1.11 in men; adjusted HR, 1.00; 95% CI, 0.73–1.36 in women) in hyperlipidemic patients.23 A potential explanation exists for ours and these two studies that the use of pravastatin may have little effect on bone in vivo.4
Lovastatin has been shown to accelerate ossification-related gene expressions in fracture healing in osteoporotic rats that were continuously administered lovastatin for >4 weeks.24 Our results contradicted this study, which may be because of not using a combination of tocotrienol or the use of lovastatin may have little effect on bone in vivo.25,26
The use of statins has been demonstrated to have a significant positive effect on osteoporotic fractures as reported by several observational studies.13–17 However, in our study comprising a 10-year follow-up period, no relationship was observed between the risk of developing NOF and the use of lovastatin, pravastatin, fluvastatin, and pitavastatin compared with that among simvastatin users. A similar finding has also been reported by several observational studies.4,19,27,28 For instance, Ward et al analyzed 46,249 patients in a Military Healthcare System and reported that there was no significant association between the risk of developing NOF and statin use.4
In vitro data show that statins have a catabolic effect on bones.12,24,29–31 Therefore, atorvastatin is generally considered to decrease the risk of developing NOFs.4,32 However, one study has indicated that atorvastatin is not associated with a decreased risk of developing NOFs compared with simvastatin.23 Our results showed a beneficial effect on the risk of developing NOFs, and this study is the first long-term longitudinal epidemiological investigation of the association between the use of atorvastatin and the risk of developing osteoporotic fractures with a follow-up period of 10 years.
In this study, rosuvastatin was associated with a decrease in the risk of NOF development compared with simvastatin users. This result is in contrast with the results reported by Hippisley-Cox and Coupland, who showed a nonstatistically significant decrease in the risk of developing NOFs (adjusted HR, 0.89; 95% CI, 0.65–1.21 in men; adjusted HR, 0.61; 95% CI, 0.36–1.03 in women).22 Our present study is also the first long-term longitudinal epidemiological investigation of the association between the use of rosuvastatin and the risk of developing osteoporotic fractures with a follow-up period of 10 years.
Some observational studies have recommended that lipophilic statins (lovastatin, simvastatin, and atorvastatin) were independently associated with a decreased risk of NOF development in patients with hyperlipidemia, whereas hydrophilic statins (pravastatin, fluvastatin, and rosuvastatin) were not.16,27,33 However, in our study that included a 10-year follow-up period, the association with NOF risk reduction was similar between lipophilic and hydrophilic statins. Similarly, our result is consistent with that reported by Ward et al, who enrolled 6,967 pairs of statin users and nonusers with hyperlipidemia and did show a reduction in the risk of developing femoral neck fractures in statin users compared to that in statin nonusers.4 In particular, a risk reduction among the users of high-potency statins (atorvastatin and rosuvastatin) and dose–response effect on NOF risk were observed in our study. The reason for these findings in our study is unclear, but it may be attributable to the statin dose (high vs low) and duration (10 vs 2–5 years).13,15,16,27 These findings emphasize the need for further investigation of the mechanistic links between these high-potency statins and the risk of developing NOFs.
Some limitations of this study need to be emphasized. First, this was a descriptive retrospective study conducted in Taiwan over a period of 10 years. Moreover, we excluded irregularly treated hyperlipidemic patients from the analyses. Therefore, caution must be exercised in interpreting our data. Second, all cases in this study were collected from claimed data sets of the Taiwan NHI that the diagnoses were based on physician reports only; therefore, it is unclear how our findings can be generalized to patients in different areas of the world. Third, the process of osteoporosis in patients who developed NOF in this study would have started many years before the diagnoses, and NOF may have coexisted with the process of hyperlipidemia for which statins were used. Thus, the cause-and-effect relationships between NOF and statins cannot be determined in this study.
Conclusion
In conclusion, our results show that hyperlipidemic patients who use atovastatins and rosuvastatins were independently associated with a decreased risk of NOF compared with simvastatin users. Other statins such as lovastatin, pravastatin, fluvastatin, and pitavastatin were not associated with NOFs. Our findings may provide some support for the hypothesis that there are differences in the risk of developing NOF with the use of different types of statins in hyperlipidemic patients. It also highlighted the lower risk of NOF associated with more commonly prescribed high-potency statins. These findings emphasize the need for further investigation of the mechanistic links between these high potency statins and NOFs.
Disclosure
The authors report no conflicts of interest in this work.
References
Center JR, Nguyen TV, Schneider D, Sambrook PN, Eisman JA. Mortality after all major types of osteoporotic fracture in men and women: an observational study. Lancet. 1999;353(9156):878–882. | ||
Holroyd C, Cooper C, Dennison E. Epidemiology of osteoporosis. Best Pract Res Clin Endocrinol Metab. 2008;22(6):671–685. | ||
Ioannidis G, Papaioannou A, Hopman WM, et al. Relation between fractures and mortality: results from the Canadian Multicentre Osteoporosis Study. CMAJ. 2009;181(5):265–271. | ||
Ward IM, Mortensen EM, Battafarano DF, Frei CR, Mansi I. Association of statins and risk of fractures in a military health system: a propensity score-matched analysis. Ann Pharmacother. 2014;48(11):1406–1414. | ||
Cawston H, Maravic M, Fardellone P, et al. Epidemiological burden of postmenopausal osteoporosis in France from 2010 to 2020: estimations from a disease model. Arch Osteoporos. 2012;7(1–2):237–246. | ||
Johnell O, Kanis JA. An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int. 2006;17(12):1726–1733. | ||
Hsiao PC, Chen TJ, Li CY, et al. Risk factors and incidence of repeat osteoporotic fractures among the elderly in Taiwan: a population-based cohort study. Medicine. 2015;94:e532. | ||
Gauthier A, Kanis JA, Jiang Y, et al. Epidemiological burden of postmenopausal osteoporosis in the UK from 2010 to 2021: estimations from a disease model. Arch Osteoporos. 2011;6(1–2):179–188. | ||
Adachi JD, Adami S, Gehlbach S, et al; GLOW Investigators. Impact of prevalent fractures on quality of life: baseline results from the global longitudinal study of osteoporosis in women. Mayo Clin Proc. 2010;85(9):806–813. | ||
Naci H, Brugts J, Ades T. Comparative tolerability and harms of individual statins: a study-level network meta-analysis of 246 955 participants from 135 randomized, controlled trials. Circ Cardiovasc Qual Outcomes. 2013;6(4):390–399. | ||
Taylor F, Huffman MD, Macedo AF, et al. Statins for the primary prevention of cardiovascular disease. Cochrane Database Syst Rev. 2013;1:CD004816. | ||
Mundy G, Garrett R, Harris S, et al. Stimulation of bone formation in vitro and in rodents by statins. Science. 1999;286(5446):1946–1949. | ||
Chan KA, Andrade SE, Boles M, et al. Inhibitors of hydroxymethylglutaryl-coenzyme A reductase and risk of fracture among older women. Lancet. 2000;355(9222):2185–2188. | ||
Ray WA, Daugherty JR, Griffin MR. Lipid-lowering agents and the risk of hip fracture in a Medicaid population. Inj Prev. 2002;8(4):276–279. | ||
Scranton RE, Young M, Lawler E, Solomon D, Gagnon D, Gaziano JM. Statin use and fracture risk: study of a US veterans population. Arch Intern Med. 2005;165(17):2007–2012. | ||
Rejnmark L, Vestergaard P, Mosekilde L. Statin but not nonstatin lipid-lowering drugs decrease fracture risk: a nationwide case-control study. Calcif Tissue Int. 2006;79(1):27–36. | ||
Helin-Salmivaara A, Korhonen MJ, Lehenkari P, et al. Statins and hip fracture prevention: a population based cohort study in women. PLoS One. 2012;7(10):e48095. | ||
McCandless, Lawrence C. Statin use and fracture risk: can we quantify the healthy-user effect? Epidemiology. 2013;24(5):743–752. | ||
van Staa TP, Wegman S, de Vries F, Leufkens B, Cooper C. Use of statins and risk of fractures. JAMA. 2001;285(14):1850–1855. | ||
20.LaCroix AZ, Cauley JA, Pettinger M, et al. Statin use, clinical fracture, and bone density in postmenopausal women: results from the Women’s Health Initiative Observational Study. Ann Intern Med. 2003;139(2):97–104. | ||
Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;63(25):2889–2934. | ||
Reid IR, Hague W, Emberson J, et al. Effect of pravastatin on frequency of fracture in the LIPID study: secondary analysis of a randomised controlled trial. Long-term Intervention with Pravastatin in Ischaemic Disease. Lancet. 2001;357(9255):509–512. | ||
Hippisley-Cox J, Coupland C. Unintended effects of statins in men and women in England and Wales: population based cohort study using the QResearch database. BMJ. 2010;340:c2197. | ||
Ibrahim N’, Mohamed N, Soelaiman IN, Shuid AN. The effects of targeted deliveries of lovastatin and tocotrienol on ossification-related gene expressions in fracture healing in an osteoporosis rat model. Int J Environ Res Public Health. 2015;12(10):12958–12976. | ||
Ibrahim N’, Khamis MF, Mod Yunoh MF, Abdullah S, Mohamed N, Shuid AN. Targeted delivery of lovastatin and tocotrienol to fracture site promotes fracture healing in osteoporosis model: micro-computed tomography and biomechanical evaluation. PLoS One. 2014;9(12):e115595. | ||
Klontzas ME, Kenanidis EI, MacFarlane RJ, et al. Investigational drugs for fracture healing: preclinical & clinical data. Expert Opin Investig Drugs. 2016;25(5):585–596. | ||
Rejnmark L, Olsen ML, Johnsen SP, Vestergaard P, Sorensen HT, Mosekilde L. Hip fracture risk in statin users: a population-based Danish case-control study. Osteoporos Int. 2004;15(6):452–458. | ||
Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet. 2002;360(9326):7–22. | ||
Tan J, Fu X, Sun CG, et al. A single CT-guided percutaneous intraosseous injection of thermosensitive simvastatin/poloxamer 407 hydrogel enhances vertebral bone formation in ovariectomized minipigs. Osteoporos Int. 2016;27(2):757–767. | ||
Kaji H, Kanatani M, Sugimoto T, Chihara K. Statins modulate the levels of osteoprotegerin/receptor activator of NFkappaB ligand mRNA in mouse bone-cell cultures. Horm Metab Res. 2005;37(10):589–592. | ||
Issa JP, Ingraci de Lucia C, Dos Santos Kotake BG, et al. The effect of simvastatin treatment on bone repair of femoral fracture in animal model. Growth Factors. 2015;33(2):139–148. | ||
Bauer DC, Mundy GR, Jamal SA, et al. Use of statins and fracture: results of 4 prospective studies and cumulative meta-analysis of observational studies and controlled trials. Arch Intern Med. 2004;164(2):146–152. | ||
Luisetto G, Camozzi V. Statins, fracture risk, and bone remodeling. J Endocrinol Invest. 2009;32(4 Suppl):32–37. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.