Back to Journals » Journal of Multidisciplinary Healthcare » Volume 13
Healthcare Worker’s Knowledge, Attitude, and Practice of Proper Face Mask Utilization, and Associated Factors in Police Health Facilities of Addis Ababa, Ethiopia
Authors Tadesse T , Tesfaye T , Alemu T , Haileselassie W
Received 8 September 2020
Accepted for publication 12 October 2020
Published 21 October 2020 Volume 2020:13 Pages 1203—1213
DOI https://doi.org/10.2147/JMDH.S277133
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Tirhas Tadesse,1 Tariku Tesfaye,2 Tadesse Alemu,3 Werissaw Haileselassie4
1Public Health Department, Yekatit12 Hospital Medical College, Addis Ababa, Ethiopia; 2Public Health Department, Ethiopian Police University College, Sendafa, Ethiopia; 3Public Health Department, Universal Medical and Business College, Addis Ababa, Ethiopia; 4School of Public Health, Addis Ababa University, Addis Ababa, Ethiopia
Correspondence: Tirhas Tadesse
Public Health Department, Yekatit12 Hospital Medical College, Addis Ababa, Ethiopia
Tel +251912053189
Email [email protected]
Background: Face masks were considered as an effective method of preventing respiratory infections like coronavirus infection. Identifying knowledge, attitude, and practice of healthcare workers regarding face mask utilization is very important to identify gaps and intervene immediately to control the spread of the infection. Hence, the main aim of this study was to determine the health worker’s knowledge, attitude, and practice of proper face mask utilization and associated factors at police health faculties in Addis Ababa, Ethiopia, 2020.
Methods: Across-sectional, quantitative approach study was conducted from June to July 2020. The study covered 408 health professionals of all categories working in the different police health facilities found in Addis Ababa, Ethiopia, during the study period. Data were collected using a pre-tested self-administered questionnaire adopted from different studies after getting consent from the study participants. After the data were collected, it was entered and analyzed using SPSS version 23 computer software. A logistic regression model was used to measure the association between the predictor and outcome variables. Statistical significance was declared at p-value< 0.05. Direction and strength of association were expressed using OR and 95% CI.
Results: The study showed that the overall knowledge, attitude, and practice of the healthcare provider towards proper face mask utilization were 98 (33.5%), 185 (45.3%), and 272 (33.3%) respectively. Factors associated with proper utilization of face mask were educational status (AOR = 10.4, 95% CI: 2.51, 43.32), police rank (AOR=0.2. CI: 0.05, 0.41), profession (AOR = 7.7, 95% CI: 2.63, 22.65), and knowledge about face mask use (AOR = 0.01, 95% CI: 0.003, 0.023).
Conclusion: In this study, the level of knowledge and attitude towards face mask utilization was relatively low, and the level of proper face mask utilization was quite low in comparison with some studies. Comprehensive training about a face mask that focuses on its proper use should be designed and given by the authorities to healthcare workers who are on the front-line in the fight against COVID-19.
Keywords: healthcare workers, knowledge, attitude, practices, proper face mask utilization, police health facilities
Introduction
Face masks and respirators were considered an effective method of preventing respiratory infections. Most participants described face masks/respirators as the “only” and the “best protection” method available to protect healthcare workers (HCWs) from respiratory infections.1
Preventing health professionals from infectious diseases/respiratory infections is crucial to promote the health and safety of staff and to maintain the performance and capability of the health workforce during outbreaks of emerging infections, such as pandemic COVID-19, influenza, Middle East Respiratory Syndrome Coronavirus (MERS-CoV), and Ebolavirus.2
In the context of the COVID-19 pandemic, healthcare workers (HCWs) protection from contamination is based on the wearing of personal protective equipment (PPE).3 Transmission routes of SARS-Cov-2 include direct transmission (droplet, eg cough, sneeze) and contact transmission (contact with oral, nasal, and eye mucous membranes).4 The existence of coronavirus (SARS-CoV-2) in the environment of patients with COVID-19 reinforces the belief that fomites play a role in the transmission of the virus; however, the relative significance of this route of transmission relative to direct exposure to respiratory droplets is still obscure.5
In developing countries, where the occurrence of communicable disease is high and the hospital environmental conditions are often poor, hospitals may rely mostly on PPE to protect their staffs.6 Face masks use (including medical and cloth masks) and respirators are strongly recommended by the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC) as a standard for transmission-based safety measures.7
The coronavirus disease, which is known as COVID-19 emerged in Wuhan, China at the end of 2019. Since then, it has spread to more than 200 countries; declared a global pandemic by the World Health Organization (WHO). To date, there are more than 6 million positive COVID-19 cases recorded with at least 450,000 deaths globally.1 The first case of COVID-19 in Ethiopia was detected in February 2020 involving one tourist from Japan.2
The number of cases highly increased after two months of the first case detected. As of 2 September 2020, Ethiopia has recorded 54,409 positive cases involving 846 deaths. A majority of these more 39,033 cases were from the capital city of the country, Addis Ababa.3
Healthcare workers are crucial to any healthcare system.9 During the ongoing COVID-19 pandemic, healthcare workers are at a substantially increased risk of becoming infected with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and could come to considerable harm as a result.10 Healthcare professionals are at greater risk of contracting COVID-19 because of the nature of their job. They could be exposed to atypical patients, infected family members, contacts, and colleagues, or live in communities of active transmission, as this type of work is very difficult to maintain social distancing. Due to this reason proper face mask as recommended by WHO guideline is needed for safe workforce reentry for people with elevated individual and occupational risk from COVID-19.11
According to the report of the Centers for Disease Control and Prevention (CDC) reports that healthcare workers account for at least 11% of reported SARSCoV-2 infections.12 A study conducted in a large public hospital in Spain reported that 11.6% of the employees tested positive for COVID-19.13
The Ethiopia Minister of health also enforced different prevention methods to reduce community spread of COVID-19, and the overburdening of the country’s health system which is already affected by infectious diseases. Unlike other community, the police force has no limited restriction on movement due to the nature of their work, which may increase the transmission of COVID-19 among police members, which in turn affects healthcare provider in the institution. In addition, police members are the turning agent for COVID-19 dissemination if we are equipped with the right information and skill. This study may also help the Ethiopian Federal Police Commission to take important prevention measures to limit the transmission of COVID-19 among police members of health professionals by developing a guideline on how to use the face mask as well as the development of ICC and BCC materials. It is also expected to help researchers use it as a base and/or source to do further and wider research exploration on this issue. Hence, this study was conducted to examine the knowledge, attitude, and practice of face mask utilization among healthcare providers at Federal Police Health Facilities in Addis Ababa, Ethiopia.
Methods and Materials
Study Area, Period, and Design
A health facility-based quantitative approach was conducted in federal police health facilities found in Addis Ababa from June to July/2020. Addis Ababa is the capital city of Ethiopia with a population of around 4.7million.7 The capital has ten administrative sub-cities and 99 Kebeles. There are a total of 38 hospitals (ten public and 28 NGO and private) in the study area.8 At the time of the study period, there were about 578 health professionals from the different departments working in all of the federal police health facilities in Addis Ababa.
Population
The source population was all health professionals who were working at federal police health facilities found in Addis Ababa. The study population for this study was all health professionals working at federal police health facilities in Addis Ababa during the study period and who fulfill the inclusion criteria were the study population. The inclusion criteria for this study were those health professionals who were willing to give informed consent and available at the time of the study. The total health professionals available during the study period were 578 and all of them were included in this study.
Data Collection Tool and Method
The questionnaire was developed by reviewing previous different literature on the proper use of surgical face mask and the guidelines of the Centre for Health Protection WHO and the CDC14–16 and in consultation with experts from different fields to check the relevance and make necessary changes according to the study requirements. The questions were modified according to the suggestions received from the expert panel and output from the pre-test. Guidelines for layout, question design, formatting, and pretesting testing were followed.
The self-administered questionnaire developed by the investigators contained the following 4 sections:1 basic demographic characteristics (age, gender, police rank, monthly income profession), and2 knowledge,3 attitude, and4 practices regarding the use of proper face mask utilization. The data were collected through a self-administered method by two trained data collectors.
Data Analysis
SPSS version 23 computer software package was used to analyze the data. Frequency, percent, and standard deviation of given data for each variable were calculated. Summary statistics of given data for each variable were calculated. A logistic regression model was used to measure the association between the outcome like Knowledge attitude and practice of proper face mask utilization and the associated factors. Statistical significance was declared at p-value<0.05. Direction and strength of association were expressed using OR and 95% CI.
Data Quality Assurance
A preliminary phase was conducted to assess the validity and reliability of the questionnaire before its use. Initially, three Ethiopian experts in the field of epidemiology and research in Ethiopian universities were asked to assess the degree to which items in the questionnaires are relevant and can correctly measure knowledge, attitude, and practice of proper face mask use in case of COVID-19 and then correction was made accordingly. Pretesting of the questionnaire was also done on 20 participants who were excluded later from the study sample. The data from the pre-test were used to assess internal consistency and reliability using Cronbach’s alpha. The results showed adequate internal consistency and reliability with Cronbach’s alpha= 0.78for attitude questions,0.67 for knowledge question, and 0.89 for practice question.
Ethical Considerations
Ethical approval was obtained from the Institutional Review Board of the Police College of Health Science, which was confirmed to the principles embodied in the Declaration of Helsinki. Official permission was also obtained from the principals of the health facilities before approaching the study participants. The objective and purpose of the study were clearly explained to the study subjects to obtain written informed consent before data collection. Participants were also informed that they can discontinue or decline to participate in the study at any time. Confidentiality of the information was maintained and the data were recorded anonymously throughout the study.
Operational Definition and Its Measurements
Knowledge About Face Mask and Its Use
For the convenience of analyses, each correct response in the knowledge category was scored 1, and each incorrect response was scored 0. The final score was calculated and then labeled based on score (out of 9). The correct response of >7 out of 9 questions (>80%) was considered as good knowledge and ≤7 (≤80%) was considered as poor knowledge.14
The Attitude of Face Mask Utilization
Respondents were asked nine questions (eg Face mask are very effective at preventing potentially infectious droplets from spreading) to describe their level of agreement in a five scale response format from “strongly disagree” to “strongly agree”. The 5-point Likert scale response options, scored from 1 to 5, were strongly disagree, disagree, neutral, agree, and strongly agree. Subscale scores were obtained by summing item scores and dividing by the total number of items. If it is above or equal to the average it was considered a positive attitude.14
Proper Practice of Face Mask Utilization
For the convenience of analyses, each correct response in the practice category was scored 1, and each incorrect response was scored 0. The correct response of >11 out of 14 questions (>80%) was considered as good practice and ≤11 (≤80%) was considered as poor practice.14
Result
Socio-Demographic Characteristics of the Respondents
A total of 408 health workers working in Police health facilities of Addis Ababa were included in this study. Around one-third of the study subjects, 127 (31.1%) were under the age group of 30years with a mean ± SD of 36.20 ± 9.05 years and ranges from 22 to 59 years old. The majority of the respondent 246 (60.3%) were males and more than half 258 (63.2%) of them were married. The majority 254 (62.3%) and 170 (41.7%) of them were degree holders by educational level and high level in rank, respectively. Most 178 (43.6%) of them were nurses in their profession. Concerning their experience, more than half 218 (53.4%) of the study participants had 10 and above years of experience (Table 1).
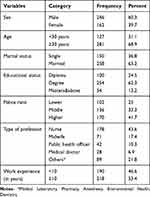 |
Table 1 Socio-Demographic Characteristics of the Police Health Professionals in Addis Ababa, Ethiopia, July 2020 |
Knowledge of the Respondents About Face Mask
Of the total of 408 respondents, 310 (76.5%) of them had poor knowledge about face mask (Figure 1).
 |
Figure 1 Level of knowledge of the respondents about face mask, police health professionals in Addis Ababa, Ethiopia, July 2020. |
Almost all 350 (85.8%) and 362 (89.7%) of the health professional know surgical mask can protect from COVID-19 and correct use of surgical face mask, respectively. Two hundred fifty-four (62.3%) and 230 (56.4%) of the participants know the lyres of the surgical mask and the layer which acts as a filter media, respectively. Concerning the type of mask, for protection against COVID-19, 276 (67.6) of the participants were responded to the correct answer. Less than half 196 (48%) of them know the duration of surgical mask use (Table 2).
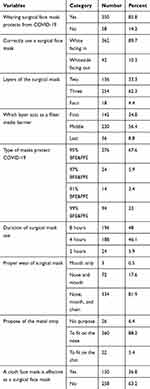 |
Table 2 Knowledge of the Police Health Professionals About Face Mask in Addis Ababa, Ethiopia, July 2020 |
Attitude of the Respondents Towards Face Mask Utilization
More than half 223 (54.7%) of the respondents had a negative attitude towards face mask utilization (Figure 2).
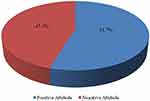 |
Figure 2 Attitude towards face mask utilization of the Respondents, police health professionals in Addis Ababa, Ethiopia, July 2020. |
This study identified most 332 (81.4%) and 327 (80.1%) of the health professionals were willing to know the correct steps of face mask wearing and believe that face mask should be carefully put-on and taken off, respectively. Regarding the effectiveness of face mask in preventing the spread of droplets, 326 (77.5%) of them believe it is effective while 86 (21%) of them disagreed. Half 220 (53.9%) of the professionals believe in changing face mask before going to another patient while 160 (39.2%) think it is not necessary to change face mask before going to another patient. Close to one-fourth of 92 (22.5%) disagreed it is not necessary to wear a face mask while in contact with patients and 174 (42.6%) said it is necessary to wear a face mask as am afraid of getting COVID-19. The large majority of 255 (62.5%) of the professionals believe that it is necessary to wear a face mask as infected with COVID-19 is the worst thing that could happen to me (Table 3).
 |
Table 3 Attitude Towards Face Mask Utilization of the Respondents, Police Health Professionals in Addis Ababa, Ethiopia, July 2020 |
Proper Practice of Face Mask Utilization of the Respondents
Of the total of 408 respondents, 272 (66.7%) of them had a poor practice of face mask utilization (Figure 3). Good practice of face mask use was higher among nurses (48.20%) and medical doctors (9.60%). The proportion of poor face mask use was higher among midwives (30.1%) and health offices (19.10%) (Figure 4).
 |
Figure 3 Summary of proper practice of face mask utilization of the Respondents, police health professionals in Addis Ababa, Ethiopia, July 2020. |
 |
Figure 4 Proper utilization of face mask by profession among police health professionals in Addis Ababa, Ethiopia, July 2020. |
More than half 243 (59.6%) of the professionals removed their face mask if there is a need to talk to the patient while 317 (77.7%) of the store using a mask in a bag for later use if not sick. One-third of 136 (33.3%) of the study participants do not wear face mask in public places and most 372 (91.3%) of them wore face masks in hospital premises. A significant number of 151 (37.0%) of health professionals do not clean their hands before wearing their face mask and more than half 233 (57.1%) of them check the inside and outside of the mask before wearing. Close to three-fourth 229 (71.6%) of them did not clean their hands after taking off the mask and 314 (77.0%) re-used a single-use mask (Table 4).
 |
Table 4 Proper Practice of Face Mask Utilization of the Respondents, Police Health Professionals in Addis Ababa, Ethiopia, July 2020 |
Factors Affecting Knowledge About Face Mask and Its Use
Sex, educational level, and profession were found to be significantly associated with knowledge about face mask used with a P-value < 0.05.
Male health professionals were 2.20 times less knowledgeable about face mask and its use compared to female professionals (AOR = 2.2, 95% CI: 1.25, 3.86). Similarly, nurses, midwives, and public health officers were less knowledgeable about face mask and its use compared to other professionals [(AOR = 2.6, 95% CI: 1.17, 5.65), (AOR = 3.3, 95% CI: 1.41, 7.89), (AOR = 9.30, 95% CI: 3.44, 25.02)], respectively (Table 5).
 |
Table 5 Factors Affecting Knowledge of the Respondents About Face Mask and Its Use, Police Health Professionals in Addis Ababa, Ethiopia, July 2020 |
Factors Affecting the Attitude Towards Face Mask Utilization
Attitude towards face mask use was significantly associated with the educational status, rank, profession, and knowledge about face mask and its use with a P-value < 0.05. Professionals with an educational level of diploma and degree were more likely to have a negative attitude about face mask use compared to professionals with an educational level of master and above professionals [(AOR = 5.0, 95% CI: 2.08, 12.20), (AOR = 2.4, 95% CI: 1.07, 5.47)], respectively.
Lower rank police professionals were less likely to have a negative attitude about face mask use than professionals with higher police rank (AOR = 0.3, 95% CI: 0.18, 0.64). Similarly, nurses and public health officers were less likely to have negative attitude than other professionals [(AOR = 0.5, 95% CI: 0.24, 0.84), (AOR = 0.3, 95% CI: 0.11, 0.79)]. Police health professionals with poor knowledge about face mask and its use were less likely to have a negative attitude about face mask use compared to police health professionals with good knowledge about face mask and its use (AOR = 0.1, 95% CI: 0.05,0.17) (Table 6).
 |
Table 6 Factors Affecting Attitude of the Respondents About Face Mask Use, Police Health Professionals in Addis Ababa, Ethiopia, July 2020 |
Factors Affecting the Proper Practice of Face Mask Utilization
Educational status, police rank, profession, and knowledge about face mask use were significantly associated with the proper practice of face mask use. Police health professionals with an educational status of degree were ten times (AOR = 10.4, 95% CI: 2.51, 43.32) more properly utilize face mask compared to master and above. Similarly, Midwives were approximately eight times (AOR = 7.7, 95% CI: 2.63, 22.65) compared to other professions.
Professionals with poor knowledge about face mask and its use were less likely to properly use face mask than professionals with good knowledge of face mask and its use (AOR = 0.01, 95% CI: 0.003,0.023) (Table 7).
 |
Table 7 Factors Affecting Proper Practice of Face Mask Use, Police Health Professionals in Addis Ababa, Ethiopia, July 2020 |
Discussion
Wearing a face mask will help prevent the spread of infection and prevent the individual from contracting any airborne infectious germs like COVID-19.16 So the main aim of this study was to determine the knowledge attitude, practice, and associated factors of proper face mask utilization practice at police health professionals in Addis Ababa Ethiopia.
A systematic review and meta-analysis conducted to assess the efficacy of face mask in preventing respiratory virus transmission were showed that the proper use of masks by healthcare workers and non-healthcare workers can reduce the risk of respiratory virus infection by 80%.17 But, in the current study, the magnitude of proper face mask utilization in the study area was 33.3%. This is almost in line with the study conducted at Dessie referral hospital, Northeast Ethiopia which was reported as 35.1% of the health professionals were wore a face mask when handling TB suspected patients only18 and with the study conducted in Pakistan which was 35.2 of the healthcare workers wear face mask correctly.6 Similarly, the current result was much lower compared to the study conducted in Malaysia which reported as 51.2% of the public had not used face mask.19 This difference might be due to the study’s aim difference the current study was focusing on the proper utilization of masks. But the current study was higher than with the study conducted in Hong Kong among adults in the community which was only 7.6 of the participants reported that they always wore face mask when taking care of family members with fever or respiratory infections.20
With regard attitude of health professionals towards face mask utilization, in the current study, less than half 45.3% of the respondents had a positive attitude towards proper face mask utilization. This was much lower compared to the study done in the DessieAmhara Region Ethiopia which accounted for 76.4% of the health workers had a favorable attitude18 This difference might be due to the difference in study area and tool, and similarly, it was lower compared to the study done in Malaysian public which accounted 83.1.19 These discrepancies might be explained by the qualitative study conducted among healthcare workers in Vietnam identified that as most of the discussants had a reservation on face mask protection against the respiratory disease as they did not have adequate data on the efficiency of face mask on the prevention of respiratory illness like COVID-19 and other discussants also raise the issue of face mask use might hurt the patient feelings.1
The current study identified that 24% of the health professionals had poor knowledge about face masks. The result was lower than the study conducted in Dessie, Ethiopia which in which 86.4% of them had good knowledge18 and with the study conducted in Public Malaysia which accounted for 80.5% of the public participants were knowledgeable.19 This difference might be contributed to the different study population sample size determination and operational definition.
Limitation
This study has some limitations. One of the limitations is bias occurred as a result of the study design (cross-sectional) since the study took the information at specified time-points and cause and effect association cannot be studied. Different mechanisms were used to reduce potential bias in the study. This study was also limited to a quantitative approach. In addition to this, a lack of sufficient similar study limited comparison to this study finding with other studies.
Conclusion
This study identified the knowledge, attitude, and practice of proper face mask utilization among police health professionals in Addis Ababa Ethiopia. This study concluded that the knowledge of face mask attitude towards proper face mask use and practice of proper face mask utilization of police health professionals extremely low. Educational status, police rank, profession, and knowledge about face mask use were significantly associated with the proper practice of face mask use. Comprehensive training about a face mask that focuses on its proper use should be designed and given by the authorities to healthcare workers who are on the front-line in the fight against COVID-19. Authorities should design policies and guidelines that address the different types of face mask, their use, and the importance of proper use of face mask use during this pandemic.
Permission for Publication
Consent to publish is not applicable for this manuscript because there are no individual data details like images or videos.
Accessibility of Data and Materials
The result of this research was extracted from the data gathered and analyzed based on the stated methods and materials. There are no supplementary files. The original data supporting this finding will be accessible at any time upon request.
Acknowledgments
Our heartfelt thanks go to Police University College for funding the study. The researchers also wish to express their gratitude to the study subjects and to all those who lent their hands for the successful completion of this research.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, have agreed on the journal to which the article will be submitted, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Funding
This research is funded by Police University College but they had no other role in the manuscript.
Disclosure
The authors affirm that there is no conflict of interest concerning the publication of this manuscript. The authors report no conflicts of interest for this work.
References
1. Chughtai AA, Seale H, Dung TC, Maher L, Nga PT, MacIntyre R. Current practices and barriers to the use of facemasks and respirators among hospital-based health care workers in Vietnam.Am. J Infect Control. 2015;43(1):72–77.
2. Alsubaie S, Temsah H, Al-Eyadhy AA, et al. Middle East Respiratory Syndrome Coronavirus epidemic impact on healthcare workers’ risk perceptions, work, and personal lives. J Infect DevCtries. 2019;13(10):920–926. doi:10.3855/jidc.11753
3. Bauchner H, Fontanarosa PB, Livingston EH. Conserving Supply of Personal Protective Equipment—A Call for Ideas. J Ame Med Assoc. 2020;323(19):1912–1914. doi:10.1001/jama.2020.4770
4. Peng X, Xu X, Li Y, et al. Transmission routes of 2019-nCoV and controls in dental practice. Int J Oral Sci. 2020;12(1):9. doi:10.1038/s41368-020-0075-9
5. Lepelletier D, Grandbastien B, Romano-Bertrand S, et al. For the French Society for Hospital Hygiene and the High Council for Public Health, What face mask for what use in the context of COVID-19 pandemic? J Hospital Infect. 2020;105(3):414–418. doi:10.1016/j.jhin.2020.04.036
6. Escombe AR, Ticona E, Chávez-Pérez V, Espinoza M, Moore D. Improving natural ventilation in hospital waiting and consulting rooms to reduce nosocomial tuberculosis transmission risk ina low resource setting. BMC Infect Dis. 2019;19:88. doi:10.1186/s12879-019-3717-9
7. World urbanization prospect. United Nation’s Population Estimate and Projections of Major Urban Agglomerations; 2018.
8. Lemecha G. Personal Communication. Addis Ababa; 2008.
9. Joseph B, Joseph M. The health of the healthcare workers. Indian J Occup Environ Med. 2016;20(2):71–72. doi:10.4103/0019-5278.197518
10. Bielicki JA, Duval X, Gobat N, et al. Monitoring approaches for health-care workers during the COVID-19 pandemic. Lancet Infect Dis. 2020;(20):30458. doi:10.1016/S1473-3099(20)30458-8
11. Larochelle MR. “Is It Safe for Me to Go to Work?” Risk Stratification for Workers during the Covid-19 Pandemic. N Engl J Med. 2020;383(5):e28. doi:10.1056/NEJMp2013413
12. Burrer SL, de Perio MA, Hughes MM; Center for Disease Control and Prevention (CDC)COVID-19 Response Team. Characteristics of health care personnel with COVID-19 — united States 2020. MMWR Morb Mortal Wkly Rep. 2020;69:477–481. doi:10.15585/mmwr.mm6915e6
13. Folgueira MD, Munoz-Ruiperez C, Alonso-Lopez MA, Delgado R. SARS-CoV-2 infection in health care workers in a large public hospital in Madrid, Spain, during March 2020. 2020 https://www.medrxiv.org/content/10.1101/2020.04.07.20055723v2.
14. Kumar J, Katto M. Knowledge, Attitude, and Practices of Healthcare Workers Regarding the Use of Face Mask to Limit the Spread of the New Coronavirus Disease (COVID19). Cureus. 2020;12(4):e7737. doi:10.7759/cureus.7737
15. Center for Disease Control and Prevention. CDC 24/7: saving lives, protecting people.Use of Masks to Help Slow the Spread of COVID-19 2020. Available at https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/diy-cloth-face-coverings.html.
16. World Health Organization. Advice on the Use of Masks in the Context of COVID-19. Interim guidance; 2020.
17. Liang M, Gao L, DO C Z. Efficacy of face mask in preventing respiratory virus transmission: a systematic review and meta-analysis. medRxiv Preprint. 2020. doi:10.1101/2020.04.03.20051649
18. Gezie H, Leta E, Admasu F, et al. Health care workers knowledge, attitude and practice towards hospital-acquired infection prevention at Dessie referral hospital, Northeast Ethiopia. Clin J Nurs Care Pract. 2019;3:059–063.
19. Azlan AA, Hamzah MR, Sern TJ, Ayub SH, Mohamad E. Public knowledge, attitudes and practices towards COVID-19: A cross-sectional study in Malaysia. medRxiv Preprint. 2020. doi:10.1101/2020.04.29.20085563
20. Lee LY, Lam EP, Chan C, et al. Practice and technique of using face mask amongst adults in the community: a cross-sectional descriptive study. BMC Public Health. 2020;20:948. doi:10.1186/s12889-020-09087
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
