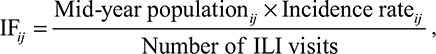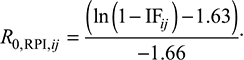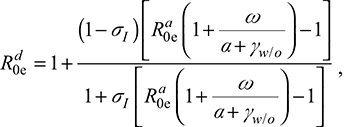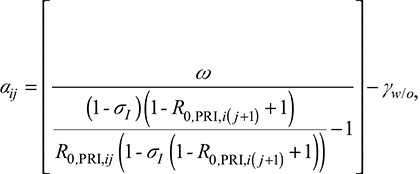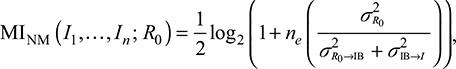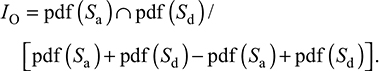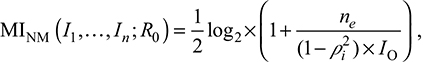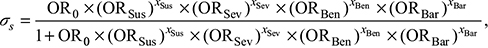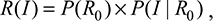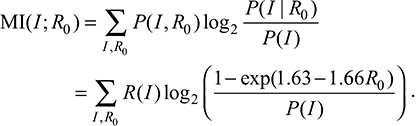Back to Journals » Infection and Drug Resistance » Volume 11
Health-seeking behavior and transmission dynamics in the control of influenza infection among different age groups
Authors You SH , Chen SC , Liao CM
Received 11 October 2017
Accepted for publication 23 January 2018
Published 6 March 2018 Volume 2018:11 Pages 331—343
DOI https://doi.org/10.2147/IDR.S153797
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Sahil Khanna
Shu-Han You,1 Szu-Chieh Chen,2,3 Chung-Min Liao4
1Institute of Food Safety and Risk Management, National Taiwan Ocean University, Taiwan, Republic of China; 2Department of Public Health, Chung Shan Medical University, Taichung, Taiwan, Republic of China; 3Department of Family and Community Medicine, Chung Shan Medical University Hospital, Taichung, Taiwan, Republic of China; 4Department of Bioenvironmental Systems Engineering, National Taiwan University, Taipei, Taiwan, Republic of China
Background: It has been found that health-seeking behavior has a certain impact on influenza infection. However, behaviors with/without risk perception on the control of influenza transmission among age groups have not been well quantified.
Objectives: The purpose of this study was to assess to what extent, under scenarios of with/without control and preventive/protective behaviors, the age-specific network-driven risk perception influences influenza infection.
Materials and methods: A behavior-influenza model was used to estimate the spread rate of age-specific risk perception in response to an influenza outbreak. A network-based information model was used to assess the effect of network-driven risk perception information transmission on influenza infection. A probabilistic risk model was used to assess the infection risk effect of risk perception with a health behavior change.
Results: The age-specific overlapping percentage was estimated to be 40%–43%, 55%–60%, and 19%–35% for child, teenage and adult, and elderly age groups, respectively. Individuals perceive the preventive behavior to improve risk perception information transmission among teenage and adult and elderly age groups, but not in the child age group. The population with perceived health behaviors could not effectively decrease the percentage of infection risk in the child age group, whereas for the elderly age group, the percentage of decrease in infection risk was more significant, with a 97.5th percentile estimate of 97%.
Conclusion: The present integrated behavior-infection model can help health authorities in communicating health messages for an intertwined belief network in which health-seeking behavior plays a key role in controlling influenza infection.
Keywords: health-seeking behavior, influenza, infection, network-based information model, probabilistic risk model
Introduction
It has been found that health-seeking behavior has a certain impact on influenza infection.1 Therefore, to facilitate public health decisions about intervention and management in controlling the spread of infectious diseases, it is crucial to assess to what extent, under scenarios of with/without control and preventive/protective behaviors, the age-specific network-driven risk perception influences influenza infection.2 To control respiratory infectious diseases, the development of vaccination, contact tracing, isolation, and the promotion of protective behaviors are the important measures. Indeed, the effectiveness of control measures fundamentally depends greatly on human beliefs on public infection awareness and risk perception for driving the change in self-behavior.3
Risk perception can be referred to as an awareness or belief about the potential hazard and/or harm, which plays an important role in shaping health-related behaviors to reducing susceptibility and infectivity.4 Generally, risk perception is affected by social factors such as media release by health authorities, observation or interaction with relation-specific groups, past experiences of similar hazards, habits, and culture.5 These factors result in variation in risk perception among individuals.
Epidemiological studies have found that variances in risk perception can be observed by examining the behavioral responses among different age groups. SteelFisher et al6 indicated that 60% of the adult population said that they did not intend to acquire the H1N1 vaccine for themselves. In addition, perception of vaccine safety and personal vulnerability were the major reasons for vaccine acceptance. Allison et al7 indicated that children could use accurate protective behavior; for example, they could use hand gel for preventing influenza. On the other hand, childhood vaccination is more likely to depend on parental decision making. Moreover, researchers have suggested assessment of the risk perception and behavior across different age groups.8,9
A social network could be an important social structure in which people could exchange information about risk-related events to spur the health behavior change.10 Scherer and Cho11 suggested that individual perceptions could be affected by self-perception in the social network. Researchers have explored the interactions between epidemic spreading and risk perception in the network.12,13 However, the influence of risk perception on the risk of infectious disease is controversial, because the perceptual capacity of individuals may both create and reduce the disease risks. Therefore, the behavior–disease dynamics in the social network structure may result in amplification or attenuation of the disease outbreak.
Most epidemic modeling techniques have used a simple epidemic model such as the susceptible–infected–recovered (SIR) model for describing a homogeneous disease network. Moreover, the effects the network with human responses to disease spreading were studied extensively and attracted substantial attention. Funk et al12 used SIR-based perceptual-influenza model for examining the effects of risk perception on behavioral change and susceptibility reduction. They also indicated that the effects within a disease network can induce health behavioral changes in the population. In turn, the influence of risk perception could result in a feedback signal to alter the progress of the disease dynamics.12,14
Recently, information theoretical approaches have been applied to infer the relations in diseases or social networks.15,16 Zhao et al15 developed a model to quantify the effects of a dynamic network, indicating that the behavior responses correspond to the entropy derived from different information content of the dynamic social network. Greenbaum et al17 proposed an information theoretic model to assess pandemic risk. They indicated that mutual information was a key determinant in minimizing risk of the pandemic threats.
We have previously incorporated the information-theoretic framework into a behavior-influenza (BI) transmission dynamic system to understand the effect of individual behavioral change on influenza epidemics.18,19 Here we assess that if, how, and to what extent, under different scenarios of with/without control and preventive/protective behaviors, the age-specific network-driven risk perception influences influenza infection.
Materials and methods
Influenza-like illness (ILI)-related emergency admission rates
In this study, we analyzed the emergency admission rates from the weekly ILI visits, which were obtained from Taiwan Centers for Disease Control (TCDC) by sentinel primary care physicians. The ILI cases were detected through the real-time outbreak and Taiwan National Infectious Disease Statistics System.21 The definition of an ILI case must meet three criteria: 1) fever (ear temperature ≥37.8°C) and respiratory tract symptoms (including rhinorrhea, nasal congestion, sneezing, sore throat, cough, and dyspnea), 2) one of the symptoms of muscle ache, headache, and extreme fatigue; and 3) exclusion of simple running nose, tonsillitis, and bronchitis.
Data on emergency admission rates for six influenza seasons in the period from week 8 of 2007 to week 13 of 2013 were adopted to test how health-seeking behavior influences the influenza infection dynamics. Influenza season was defined from July 1 (week 26) to June 30 (week 25) of the following year in Taiwan. The ILI-related emergency admission rates were detected by using the ICD-9-CM codes for influenza and pneumonia (480–487).
We also estimated the age-specific admission infection fraction (IF) for each age group, including child (0–14 years), teenage and adult (15–64 years), and elderly (65+ years), for different human behaviors or influenza risk perceptions. We multiplied the annual mid-year population estimates20 by the incidence rate for severe complicated influenza cases per 100,000 and then divided the result by the number of ILI visits to estimate IF, which is given as21
|
|
where i is the different age groups (child, teenage and adult, and elderly) and j is the yearly based time period in the period of 2007–2013.
BI model
The concept of the BI model developed in our previous studies18,19 mainly incorporated the SIR-based perception model12 into an information-theoretic framework, which was used to simulate the information flow of risk perception in response to an influenza outbreak. Briefly, the BI model uses six compartments to represent the disease states of susceptible, infected, and recovered by dividing the population into a with/without perception structure.12 The description of input parameters for the BI model is given in Table 1.
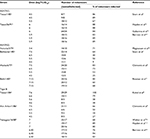
  | Table 1 Symbols, definition, and input values varied in different age groups with respect to the parameters used in the present BI model Notes: aMean (SD). bLN distribution with a gm and a gsd. cEstimated from this study. dData modified from Funk et al.12. eN distribution with mean and standard deviation. Abbreviations: BI, behavior-influenza; ILI, influenza-like illness; LN, lognormal; OR, odds ratio; SD, standard deviation; gm, geometric mean; gsd, geometric standard deviation; N, normal. |
Basic reproduction number (R0) can be used to quantify disease infection severity, defined as the average number of secondary cases produced successfully by an infected individual in a totally susceptible population.22 Therefore, based on the BI model, we can also estimate R0 with the perception state (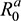 ) and without perception state (
) and without perception state (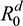 ). It can be described as input source information with perception Sa =
). It can be described as input source information with perception Sa =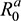 = α/λ, where α is the rate of perception spread and λ is the rate of perception loss. On the other hand, input source information can be described without perception Sd =
= α/λ, where α is the rate of perception spread and λ is the rate of perception loss. On the other hand, input source information can be described without perception Sd = 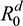 = β/γ where β is the infection rate describing contact between infected and susceptible populations and γ is the recovery rate from infected to recovered populations.19
= β/γ where β is the infection rate describing contact between infected and susceptible populations and γ is the recovery rate from infected to recovered populations.19
We assumed that R0 can be treated as the basic reproduction number resulting from individuals with risk perception information (R0,RPI) for each age group in the period of 2007–2013. Thus, R0,RPI can be estimated as:19
|
|
Furthermore, to better characterize perception spread rate for different age groups during each year (aij) on the BI transmission dynamics, we adopted aij from an epidemic equilibrium structure.12 The equilibrium information flow of risk perception from population without perception 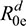 can be expressed as;12
can be expressed as;12
|
|
where 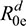 is the basic reproduction number at equilibrium with information flow of risk perception from population without perception, σI is the reduced infectivity factor from infected with perception to susceptible without perception, ω is the rate of infected becoming with perception, α is the perception spread rate, and γw/o is the recovery rate of infected without perception.
is the basic reproduction number at equilibrium with information flow of risk perception from population without perception, σI is the reduced infectivity factor from infected with perception to susceptible without perception, ω is the rate of infected becoming with perception, α is the perception spread rate, and γw/o is the recovery rate of infected without perception.
Moreover, we assumed that people may make the decision to change behavior based on R0,RPI in the previous year. Based on Equation 3, a can then be rewritten as;
|
|
where R0,PRI,ij and R0,PRI,i( j+1) are the basic reproduction numbers with/without risk perception, respectively, for each age group in the period of 2007–2013.
Network-based information model
To assess the effect of network-driven risk perception information transmission on influenza infection, we applied an information theoretic model referred to as the multiple access channel (MAC) that is used to capture a signal R0 transmitting through multiple channels to the responses I1, I2, …, In. We considered the network-driven risk perception information model (NM) with information bottleneck (IB).19 The maximum mutual risk perception information (MImax) resulting from the NM can be estimated as;23
|
|
where ne is the effective information from contact numbers of individuals, 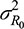 is the variance of the R0 signal distribution,
is the variance of the R0 signal distribution, 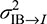 is the variance introduced in each access channel through the IB to response I, and the
is the variance introduced in each access channel through the IB to response I, and the 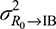 is the variance introduced to the IB. The ratio
is the variance introduced to the IB. The ratio 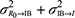 is the signal-to-noise ratio.23
is the signal-to-noise ratio.23
On the other hand, the NM model with a negative feedback was considered to explore the effect of perceived different health behaviors on reducing susceptibility.19 Here, we used the correlation coefficient (r) and the overlapping percentage (IO) to associate R0 and I from the published data (Table S1) to calculate 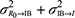 in Equation 5. We estimated the r based on the relationship between viral titer-based I and viral tier-based R0 corresponding to with/without perceived different health behaviors. Briefly, we selected published papers (Table S1) where health behaviors treated with vaccinations and antiviral drugs for different subtypes of influenza were included. Two protective behaviors (i.e., perceived of carrying the disease to vaccine and antiviral taking) were adopted in a state of greater alert. The value of r can be used to associate the amount of observed variability that is attributable to the overall biological variability and experimental noise.
in Equation 5. We estimated the r based on the relationship between viral titer-based I and viral tier-based R0 corresponding to with/without perceived different health behaviors. Briefly, we selected published papers (Table S1) where health behaviors treated with vaccinations and antiviral drugs for different subtypes of influenza were included. Two protective behaviors (i.e., perceived of carrying the disease to vaccine and antiviral taking) were adopted in a state of greater alert. The value of r can be used to associate the amount of observed variability that is attributable to the overall biological variability and experimental noise.
On the other hand, IO describes the age-specific overlapping percentage between the infected population with/without perception adjusted by the fractions of initial infected population with perceptual state over those without perceptual state. Here, we used three perceptual scenarios to assess our model with the initial infected population ratios of <1, =1, and >1. The IO can then be estimated as algebraic manipulation of probability density functions (pdfs) of Sa and Sd as;19
|
|
Thus, followed by the information-theoretic theorem with known values of ρ, IO, and 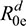 , the (
, the (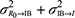 ) can be computed as
) can be computed as  .23 Therefore, the NM model with a negative feedback in Equation 5 can be rewritten as;
.23 Therefore, the NM model with a negative feedback in Equation 5 can be rewritten as;
|
|
where i represents the individuals perceived with/without health behaviors.
We further incorporated the estimated probability distributions of the model parameter with age-specific initial population sizes in the period of 2007–2013 (Table 2) and α into the BI model, to estimate the age-specific overlapping percentages.
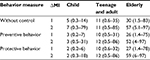  | Table 2 Percentage of decrease in infection risk at incremental maximum mutual risk perception information (∆MI) Notes: Values are presented as mean (minimum–maximum). |
Behavior change modeling
To parameterize the reduced susceptibility factor with regard to adopting preventive behaviors, including using masks, avoiding visiting crowded places, and hand washing24 (σS,pre), and protective behaviors of vaccination26 (σS,pro), we applied a standard logistic regression-based equation for mathematically expressing the components of the health-behavior model (HBM). The HBM-based health behavior with the standard logistic regression-based equation has been applied to estimate with/without preventive/protective health behaviors in respiratory infectious diseases such as severe acute respiratory syndrome (SARS), influenza,24–26 and other diseases.27–29 The estimates are equivalent to the decisions of rational individuals with influenza knowledge.
Here, σs can be expressed in terms of odds ratios (ORs) depending on health behaviors perceived to be associated with each HBM variable.26 σs is represented as a function of measured states, which are based on the HBM by using the standard logistic regression-based equation. σs can also be regarded as a predictor of behavior decision on the course of the epidemic.
σs can be rewritten as;26
|
|
where σs is the probability of the HBM-based health behaviors (such as preventive behavior, σs,pre, and protective behavior, σs,pro) and x is a binary variable with a value of 1 indicating a “high” state and a value of 0 indicating a “low” state. OR0 is a calibration factor when all HBM variables are in a “low” state. σs represents that an individual engages in a particular behavior, and it could be calculated from Equation 8. σs ≥0.5 indicates that an individual engages in a specific health behavior.
R0 perception-based probabilistic risk assessment
To develop a probabilistic risk model, a dose–response model describing the relationship between transmission potential quantified by signal R0 and the total proportion of the infected population (I) has to be constructed. In a previous study,18 we have successfully employed the joint probability distribution to assess the risk profile. It can be expressed mathematically as;
|
|
where R(I) is the cumulative distribution function describing the probabilistic infection risk in a susceptible population at specific R0 signal, P(R0) is the probability distribution of R0 signal (the prior probability), and P(I|R0) is the conditional response distribution describing the dose–response relationship between I and R0. The exceedance risk profile can be obtained by 1 - R(I).
In view of Equation 2, we can relate P(I, R0) to R(I) in Equation 9. Thus, the mutual information in R0-I risk perception model can be written as;18
|
|
These interdependences between belief of risk perception and infection risk can then be expressed as a mechanism of interpersonal influence described in Equation 10.
Results
Data description and parameterization
In Table 1, the numbers of ILI visits were 2.4 × 104± 1 × 104 (mean ± standard deviation [SD]), 2.8 × 104 ± 1.1 × 104, and 8.4 × 103 ± 1.7 × 103 per month for child, teenage and adult, and elderly age groups, respectively. Figure 1 shows the ILI-related emergency admission rates and IF among the three age groups, child (0–14 years), teenage and adult (15–64 years), and elderly (65+ years), in Taiwan. During the study period (2007–2013), the ILI-related emergency admission rates were estimated to be 16.8 ± 7.3 (mean ± SD), 1.2 ± 0.8, and 3.5 ± 1.3 per 10,000 population for child, teenage and adult, and elderly age groups, respectively. Overall, the ILI-related emergency admission rate was the highest in the child age group (6.4–67.3 per 10,000 population, minimum–maximum), whereas the lowest one was observed in the teenage and adult age group (0.4–8.8 per 10,000 population; Figure 1A). On the other hand, the highest ILI-related emergency admission IF was in the child age group (0.7 ± 0.1%), followed by teenage and adult (0.2 ± 0.1%) and elderly (0.03 ± 0.01%) age groups (Figure 1B).
Perception spread rate and overlapping responses
To model the BI model, the age-specific perception spread rate (α) has to be determined (Equation 4). We first calculated age-specific R0,PRI based on the age-specific ILI-related admission IF. Our results indicated that lognormal (LN) distribution with a geometric mean (gm) and a geometric standard deviation (gsd), LN (gm, gsd), was the most suitable fitted model for R0,PRI distributions of LN (1.78, 1.08), LN (1.14, 1.04), and LN (1.00, 1.01) for child, teenage and adult, and elderly, age groups, respectively (Table 1).
Figure 2 demonstrates age-specific overlapping percentage (IO) between infected population with/without perception adjusted by fractions of initial infected population with perceptual state over those without perceptual state. We used three different scenarios of initial infected population fraction: I+/I- < 1 (Figure 2A–C), I+/I- = 1 (Figure 2D–F), and I+/I- > 1 (Figure 2G–I). We showed that I+/I- > 1 results in the lowest estimates of IO in child and elderly age groups (Figure 2G and I), whereas for teenage and adult age groups, the estimate was the highest in the case of I+/I- = 1 (Figure 2E). Generally, IO estimates range from 40% to 43%, 55% to 60%, and 19% to 35% for child, teenage and adult, and elderly age groups, respectively (Figure 2). Thus, we used IO based on justified initial infected population fraction to further examine the MImax among each age group.
Estimates of mutual risk perception information
Generally, the individual with risk perceptual status is more likely to have the communicable belief among the population. In the case of effective information from contact numbers of individuals (ne = 1; Figure 3A), when I+/I- < 1 and I+/I- = 1, the MImax was <1 bit. On the other hand, when I+/I- > 1, as the perceptual information increased in the population, MImax was >1 bit, indicating that the network-based information reflected cooperativity.
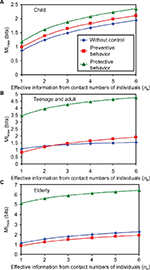
Our results showed that MImax–ne profile featured a smooth shape (Figure 3B). In the elderly group, as the strength of ne increased, MImax–ne profile experienced a nearly smooth curve. On the other hand, in the child and elderly groups, when ne was >6, MImax was >1 bit. Our results indicated that MImax ranged from 0.4 to 1.2 bits, 0.5 to 1.4 bits, and 1.2 to 2.4 bits for child, teenage and adult, and elderly age groups, respectively, given ne ranging from 1 to 6 (Figure 3B).
To explore the impact of ne-varying perceived health behavior information on MImax, we estimated correlation coefficient (r) based on the relationship between viral titer-based I and viral tier-based R0 corresponding to, with and without, perceived different health behaviors. The resulting estimates were rw = 0.7 and rw/o = 0.4 (Figure S1).
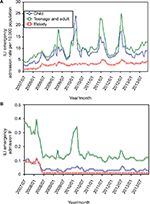
We further used Equation 7 to calculate MImax based on overlapping percentage (IO) and r affected by ne. The results indicated that MImax ranged from 0.9 to 1.9 bits, 1.0 to 2.1 bits, and 1.2 to 2.4 bits for without control, and preventive, and protective behaviors in the child age group, respectively (Figure 4A). For the teenage and adult age group, MImax ranged from 1.1 to 1.5 bits, 0.8 to 1.9 bits, and 3.5 to 4.8 bits for without control, and preventive, and protective behaviors, respectively (Figure 4B). Our results showed that individuals perceived the health behaviors to increase MImax among child, and teenage and adult, age groups (Figure 4A and B, respectively). Our results also revealed that individuals perceived the preventive behavior to improve risk perception information transmission among the teenage and adult age group (Figure 4B), and the elderly age group (Figure 4C), but not in the child age group.
Infection risk and change assessment
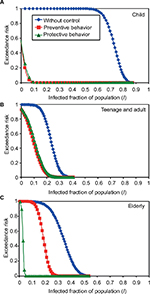
Our results indicated that there was 50% probability for exceeding the infected fraction of population (I); 0.73, 0.23, and 0.34 for child (Figure 5A), teenage and adult (Figure 5B), and elderly (Figure 5C) age groups, respectively, in the condition of without perceived health behaviors. However, there was a 50% probability for reducing the infected fraction of population within the ranges of 0.004–0.20 for preventive behavior and 0.007–0.10 for protective behavior (Figure 5).
The age-specific ∆MI with respect to with/without health behaviors was estimated based on Equations 7 and 10. We found that, for instance, without any control information released, the median percentages of decrease in infection risk with ∆MIs = 1 and 2 for elderly were 30 (1.5–83) and 57 (5.1–97), respectively, whereas the child age group had the lowest estimates of 5 (0.3–14) and 7 (0.3–79), respectively (Figure 6A).
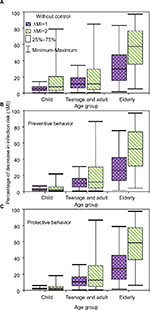  | Figure 6 Age-specific percentage of decrease in infection risk (∆MI) depending on (A) without control behavior, (B) preventive behavior, and (C) protective behavior, respectively. |
On the other hand, ∆MI estimates at incremental MI changes with perceived health behaviors were 2%–3%, 10%–12%, and 26%–59% for child, teenage and adult, and elderly age groups, respectively (Figure 6B and C). The population with perceived health behaviors could not effectively decrease the percentage of infection risk in the child group, whereas for the elderly age group, the percentage of infection risk decreased more significantly with a 97.5th percentile estimate of 97% (Figure 6B and C).
Discussion
Our results indicated that children may be preferable to adopt the protective behaviors. Allison et al7 indicated that the use of hand gel for hygiene was a feasible strategy in elementary schools to prevent influenza spread. Our results implicate that children could use the accurate knowledge about the protective behavior to prevent influenza infection effectively.
Our results found that the perceived protective behaviors enhanced the MImax in adults, whereas the perceived vaccination behavior might not. A meta-analysis of eligible studies also confirmed that raising risk perception from low to high would have a potential effect on vaccination behavior of adults.30 We suggest that future studies should detect the differences among the health behaviors in adults.
Schneeberg et al31 indicated that the vaccination rate for seasonal influenza was consistently low among the elderly population in Canada. Walter et al32 indicated that the elderly population failed to obtain information about vaccine perception from the Internet directly. It was also found that face mask wearing was easily performed by older adults in Hong Kong.25 Elderly people also appeared to be more active in conducting preventive measures.33
In this article, we incorporated the probability-based HBM with regard to specific health behaviors into an SIR-based epidemiological model. The HBM was used to examine individual’s perceptual dimensions such as perceived susceptibility, severity, benefits, and barriers. However, the HBM has led to somewhat controversial issues in exploring the health behaviors such as for vaccination programs.34,35 The HBM presents a rational point of view that assumes the perceiver to be uninfluenced by the emotion, on describing the human response to an epidemic.9,26 Our study, however, establishes a more robust mechanistic framework on modeling the influence of network-driven risk perception on influenza infection.
To our knowledge, we have conducted the first step on exploring the effects of risk perception in a population, on the spread of epidemics. We believe that our present methodology provides an innovative approach that integrates an epidemiology model with the information theory. We examined three scenarios for describing different age-specific populations to overcome susceptibility risk due to less accurate knowledge of influenza. We found that noise effect, which reflects as overlapping percentages about the uncertainty of accurate knowledge of influenza, can reduce risk perception information transfer on the network through the epidemic transmission. For example, previous studies found that participants had misconceptions between seasonal vaccine and pandemic strain.36,37
The effect of overlapping response may have resulted from the public health campaigns. For example, people were recommended to acquire the seasonal vaccine in pandemics. This may lead to a feedback mechanism between behavior change and disease dynamics. Future work should carefully consider the effects of this noise on specific age groups. Moreover, each intervention should be carefully investigated to the extent possible during an epidemic.
This study has several limitations. The estimation of information flow of risk perception in age groups depended on the ILI data. Indeed, the human response to influenza varied with time and hence is not possible to detect in real-time situations. Moreover, perceptual states in specific age groups may be affected by the severity levels of disease, the amount of accurate information about influenza, and other health-related leaflets. Therefore, we suggest that the health authorities could reinforce health monitoring by using information technology and then linking it to the real-time epidemiological surveillance systems.
A further limitation of our study is that we did not consider the influential factors on risk perception in an epidemic model. Hence, future research should explicitly consider a number of additional influential factors on risk perception within an epidemic modeling, including disease prevalence, network effects, and government and media health messages.
The findings of our study have an implication for public health. Risk communication might be more effective if health authorities focus on a variety of information communication channels for conveying health behavior messages. Moreover, our findings concerning perception of different health behaviors show substantial differences among age groups. We found that perceived protective behaviors (e.g., covering mouth, coughing hand washing) could reduce the infection risk for all age groups. This suggests that such crucial information for control measures would allow for targeting resources to designing and implementing the education plans concerning perception of healthy behaviors that are least perceived in the health behaviors.
Conclusion
We developed an integrated mathematical model by incorporating the epidemiological transmission dynamics, the information flow of human responses, and an information theoretic model to assess the effects of network-driven risk perception on influenza infection risk. The simulated human responses with perceived health behaviors could decrease the risk of infection among different age groups. We demonstrated that the risk perception among populations changed with the effective information varying with the contact numbers of individual. We conclude that the present integrated BI model can help public health authorities on communicating health messages for an intertwined belief network in which health-seeking behavior plays a key role in controlling influenza infection.
Acknowledgment
The authors acknowledge the financial support of the Ministry of Science and Technology, Republic of China, under Grant MOST 104-2221-E-002-030-MY3.
Author contributions
All authors contributed toward data analysis, drafting, and critically revising the paper and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Coelho FC, Codeço CT. Dynamic modeling of vaccinating behavior as a function of individual beliefs. PLoS Comput Biol. 2009;5(7):e1000425. | ||
Salathé M, Khandelwal S. Assessing vaccination sentiments with online social media: implications for infectious disease dynamics and control. PLoS Comput Biol. 2011;7(10):e1002199. | ||
Leppin A, Aro AR. Risk perceptions related to SARS and Avian Influenza: theoretical foundations of current empirical research. Int J Behav Med. 2009;16(1):7–29. | ||
Slovic P. The Perception of Risk. London: Routledge; 2000. | ||
Jacobs J, Taylor M, Agho K, Stevens G, Barr M, Raphael B. Factors associated with increased risk perception of pandemic influenza in Australia. Influenza Res Treat. 2010;2010:947906. | ||
SteelFisher GK, Blendon RJ, Bekheit MM, Lubell K. The public’s response to the 2009 H1N1 influenza pandemic. N Engl J Med. 2010;362(22):e65. | ||
Allison MA, Guest-Warnick G, Nelson D, et al. Feasibility of elementary school children’s use of hand gel and facemasks during influenza season. Influenza Other Respir Viruses. 2010;4(4):223–229. | ||
Kamate SK, Agrawal A, Chaudhary H, Singh K, Mishra P, Asawa K. Public knowledge, attitude and behavioural changes in an Indian population during the Influenza A (H1N1) outbreak. J Infect Dev Ctries. 2009;4(1):7–14. | ||
Bults M, Beaujean DJ, de Zwart O, et al. Perceived risk, anxiety, and behavioural responses of the general public during the early phase of the influenza A (H1N1) pandemic in the Netherlands: results of three consecutive online surveys. BMC Public Health. 2011;11:2. | ||
Muter BA, Gore ML, Riley SJ. Social contagion of risk perceptions in environmental management networks. Risk Anal. 2013;33(8):1489–1499. | ||
Scherer CW, Cho H. A social network contagion theory of risk perception. Risk Anal. 2003;23(2):261–267. | ||
Funk S, Gilad E, Jansen VA. Endemic disease, awareness, and local behavioral response. J Theor Biol. 2010;264(2):501–509. | ||
Bagnoli F, Massaro E. Epidemic spreading and risk perception in multiplex networks: a self-organized percolation method. Phys Rev E Stat Nonlin Soft Matter Phys. 2014;90(5–1):052817. | ||
Moussaïd M, Kämmer JE, Analytis PP, Neth H. Social influence and the collective dynamics of opinion formation. PLoS One. 2013;8(11):e78433. | ||
Zhao K, Karsai M, Bianconi G. Entropy of dynamical social networks. PLoS One. 2011;6(12):e28116. | ||
Stopczynski A, Sekara V, Sapiezynski P, et al. Measuring large-scale social networks with high resolution. PLoS One. 2014;9(4):e95978. | ||
Greenbaum BD, Li OTW, Poon LLM, Levine AJ, Rabadan R. Viral reassortment as an information exchange between viral segments. Proc Natl Acad Sci U S A. 2012;109(9):3341–3346. | ||
Liao CM, You SH. Assessing risk perception and behavioral responses to influenza epidemics: linking information theory to probabilistic risk modeling. Stoch Environ Res Risk Assess. 2014;28(2):189–200. | ||
Liao CM, You SH, Cheng YH. Network information analysis reveals risk perception transmission in a behaviour-influenza dynamics system. Epidemiol Infect. 2015;143(1):23–36. | ||
Department of Statics of Ministry of the interior in Taiwan [database on the Internet]. Statistical Yearbook of Interior. 2013. Available from: http://sowf.moi.gov.tw/stat/year/list.htm. Accessed September 19, 2017. | ||
Taiwan Centers for Disease Control (TCDC) [webpage on the Internet]. Taiwan National Infectious Disease Statistics System. 2013. Available from: https://nidss.cdc.gov.tw/en/EVNOSCHOOL_query_page.aspx?dc=INF&dt=4&disease=2&position=5. Accessed September 19, 2017. | ||
Anderson RM, May RM. Infectious Disease of Humans: Dynamics and Control. Oxford: Oxford University Press; 1991. | ||
Cover TM, Thomas JA. Elements of Information Theory. 2nd ed. Hoboken: Wiley-Interscience; 2006. | ||
Lau JTF, Yang XL, Tsui HY, Pang E. SARS related preventive and risk behaviours practised by Hong Kong-mainland China cross border travellers during the outbreak of the SARS epidemic in Hong Kong. J Epidemiol Community Health. 2004;58(12):988–996. | ||
Tang CSK, Wong CY. Psychosocial factors influencing the practice of preventive behaviors against the severe acute respiratory syndrome among older Chinese in Hong Kong. J Aging Health. 2005;17(4):490–506. | ||
Durham DP, Casman EA. Incorporating individual health-protective decisions into disease transmission models: a mathematical framework. J R Soc Interface. 2012;9(68):562–570. | ||
Shanks LC, Moore SM, Zeller RA. Predictors of cardiac rehabilitation initiation. Rehabil Nurs. 2007;32(4):152–157. | ||
Regan R, Morisky DE. Perceptions about HIV and condoms and consistent condom use among male clients of commercial sex workers in the Philippines. Health Educ Behav. 2013;40(2):216–222. | ||
Chen YW, Liu CC, Perng DS. Perceptions about preventing hepatocellular carcinoma among patients with chronic hepatitis in Taiwan. World J Gastroenterol. 2013;19(22):3459–3465. | ||
Brewer NT, Chapman GB, Gibbons FX, Gerrard M, McCaul KD, Weinstein ND. Meta-analysis of the relationship between risk perception and health behavior: the example of vaccination. Health Psychol. 2007;26(2):136–145. | ||
Schneeberg A, Bettinger JA, McNell S, et al. Knowledge, attitudes, beliefs and behaviours of older adults about pneumococcal immunization, a Public Health Agency of Canada/Canadian Institutes of Health Research Influenza Research Network (PCIRN) investigation. BMC Public Health. 2014;14(1):442. | ||
Walter D, Böhmer MM, Reiter S, Krause G, Wichmann O. Risk perception and information-seeking behaviour during the 2009/10 influenza A (H1N1)pdm09 pandemic in Germany. Euro Surveill. 2012;17(13):9–16. | ||
de Zwart O, Veldhuijzen IK, Richardus JH, Brug J. Monitoring of risk perceptions and correlates of precautionary behaviour related to human avian influenza during 2006–2007 in the Netherlands: results of seven consecutive surveys. BMC Infect Dis. 2010;10(1):114. | ||
Liao QY, Cowling BJ, Lam WWT, Fielding R. Factors affecting intention to receive and self-reported receipt of 2009 pandemic (H1N1) vaccine in Hong Kong: a longitudinal study. PLoS One. 2011;6(3):e17713. | ||
Murele B, Vaz R, Gasasira A, Mkanda P, Erbeto T, Okeibunor J. Vaccine perception among acceptors and non-acceptors in Sokoto State, Nigeria. Vaccine. 2014;32(26):3323–3327. | ||
Hilton S, Smith E. Public views of the UK media and government reaction to the 2009 swine flu pandemic. BMC Public Health. 2010;10(1):697. | ||
Jhummon-Mahadnac ND, Knott J, Marshall C. A cross-sectional study of pandemic influenza health literacy and the effect of a public health campaign. BMC Res Notes. 2012;5(1):377. |
Supplementary materials
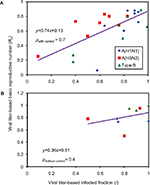  | Figure S1 Relationship between viral titer-based I and viral tier-based R0 corresponding to (A) with and (B) without perceived different health behaviors. |
References
Sears SD, Clements ML, Betts RF, Maassab HF, Murphy BR, Snyder MH. Comparison of live, attenuated H1N1 and H3N2 cold-adapted and avian-human influenza A reassortant viruses and inactivated virus vaccine in adults. J Infect Dis. 1998;158(6):1209–1219. | ||
Hayden FG, Atmar RL, Schilling M, et al. Use of the selective oral neuraminidase inhibitor oseltamivir to prevent influenza. N Engl J Med. 1999;341(18):1336–1343. | ||
Gubareva LV, Kaiser L, Matrosovich MN, Soo-Hoo Y, Hayden FG. Selection of influenza virus mutants in experimentally infected volunteers treated with oseltamivir. J Infect Dis. 2001;183(4):523–531. | ||
Barroso L, Treanor J, Gubareva L, Hayden FG. Efficacy and tolerability of the oral neuraminidase inhibitor peramivir in experimental human influenza: randomized, controlled trials for prophylaxis and treatment. Antivir Ther. 2005;10(8):901–910. | ||
Magnussen CR, Douglas RG, Betts RF, Roth FK, Meagher MP. Double-blind evaluation of oral ribavirin (Virazole) in experimental influenza A virus infection in volunteers. Antimicrob Agents Chemother. 1977;12(4):498–502. | ||
Clements ML, O’donnell S, Levine MM, Chanock RM, Murphy BR. Dose response of A/Alaska/6/77 (H3N2) cold-adapted reassortant vaccine virus in adult volunteers: role of local antibody in resistance to infection with vaccine virus. Infect Immun. 1983;40(3):1044–1051. | ||
Reuman PD, Bernstein DI, Keefer MC, Young EC, Sherwood JR, Schiff GM. Efficacy and safety of low dosage amantadine hydrochloride as prophylaxis for influenza A. Antiviral Res. 1989;11(1):27–40. | ||
Keitel WA, Couch RB, Cate TR, Six HR, Baxter BD. Cold recombinant influenza B/Texas/1/84 vaccine virus (CRB 87): attenuation, immunogenicity, and efficacy against homotypic challenge. J Infect Dis. 1990;161(1):22–26. | ||
Clements ML, Snyder MH, Sears SD, Maassab HF, Murphy BR. Evaluation of the infectivity, immunogenicity, and efficacy of live cold-adapted influenza B/Ann Arbor/1/86 reassortant virus vaccine in adult volunteers. J Infect Dis. 1990;161(5):869–877. | ||
Walker JB, Hussey EK, Treanor JJ, Montalvo A, Hayden FG. Effects of the neuraminidase inhibitor zanamivir on otologic manifestations of experimental human influenza. J Infect Dis. 1997;176(6):1417–1422. | ||
Hayden FG, Jennings L, Robson R, et al. Oral oseltamivir in human experimental influenza B infection. Antivir Ther. 2000;5(3):205–213. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.