Back to Journals » ClinicoEconomics and Outcomes Research » Volume 13
Glycated Albumin for Glycemic Control in T2DM Population: A Multi-Dimensional Evaluation
Authors Ferrario L ![]() , Schettini F
, Schettini F ![]() , Avogaro A
, Avogaro A ![]() , Bellia C, Bertuzzi F, Bonetti G, Ceriello A
, Bellia C, Bertuzzi F, Bonetti G, Ceriello A ![]() , Ciaccio M, Corsi Romanelli M, Dozio E, Falqui L, Girelli A, Nicolucci A
, Ciaccio M, Corsi Romanelli M, Dozio E, Falqui L, Girelli A, Nicolucci A ![]() , Perseghin G
, Perseghin G ![]() , Plebani M
, Plebani M ![]() , Valentini U, Zaninotto M, Castaldi S
, Valentini U, Zaninotto M, Castaldi S ![]() , Foglia E
, Foglia E ![]()
Received 2 February 2021
Accepted for publication 23 April 2021
Published 27 May 2021 Volume 2021:13 Pages 453—464
DOI https://doi.org/10.2147/CEOR.S304868
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Giorgio Colombo
Lucrezia Ferrario,1 Fabrizio Schettini,1 Angelo Avogaro,2 Chiara Bellia,3 Federico Bertuzzi,4 Graziella Bonetti,5 Antonio Ceriello,6 Marcello Ciaccio,3,7 Massimiliano Corsi Romanelli,8,9 Elena Dozio,9 Luca Falqui,10 Angela Girelli,11 Antonio Nicolucci,12 Gianluca Perseghin,13,14 Mario Plebani,15 Umberto Valentini,11 Martina Zaninotto,15 Silvana Castaldi,9,16 Emanuela Foglia1
1Centre for Health Economics, Social and Health Care Management, Università Carlo Cattaneo - LIUC, Castellanza, Italy; 2Department of Medicine, University-Hospital of Padova, Padova, Italy; 3Section of Clinical Biochemistry and Clinical Molecular Medicine, Department of Biopathology and Medical Biotechnologies, University of Palermo, Palermo, Italy; 4Diabetology Unit, Grande Ospedale Metropolitano Niguarda Hospital, Milan, Italy; 5Department of Medicine Services, Valcamonica Hospital, Esine, Italy; 6Department of Cardiovascular and Metabolic Diseases, Multimedica Research Institute, Milan, Italy; 7Department of Laboratory Medicine, University-Hospital of Palermo, Palermo, Italy; 8Service of Laboratory Medicine 1-Clinical Pathology, Policlinico San Donato, Milan, Italy; 9Department of Biomedical Sciences for Health, Università degli Studi di Milano, Milan, Italy; 10Department of Medicine, Diabetes and Endocrinology, Multimedica Research Institute, Milan, Italy; 11Diabetes Care Unit, Spedali Civili Hospital, Brescia, Italy; 12Center for Outcomes Research and Clinical Epidemiology, Pescara, Italy; 13Department of Medicine and Surgery, Università degli Studi di Milano Bicocca, Milan, Italy; 14Department of Medicine and Rehabilitation, Unit of Metabolic Medicine, Policlinico di Monza, Monza, Italy; 15Department of Laboratory Medicine, University-Hospital of Padova, Padova, Italy; 16Fondazione Ca’ Granda Ospedale Maggiore Policlinico Research Institute of Milano, Milano, Italy
Correspondence: Lucrezia Ferrario
Centre for Health Economics, Social and Health Care Management, Università Carlo Cattaneo – LIUC, Corso Matteotti 22, Castellanza, 21053, VA, Italy
Tel +39 033 1572504
Fax +39 033 1572513
Email [email protected]
Purpose: To investigate the glycated albumin (GA) introduction implications, as an add-on strategy to traditional glycemic control (Hb1Ac and fasting plasma glucose – FPG) instruments, considering insulin-naïve individuals with type 2 diabetes mellitus (T2DM), treated with oral therapies.
Methods: A Health Technology Assessment was conducted in Italy, as a multi-dimensional approach useful to validate any innovative technology. The HTA dimensions, derived from the EUnetHTA Core Model, were deployed by means of literature evidence, health economics tools and qualitative questionnaires, filled-in by 15 professionals.
Results: Literature stated that the GA introduction could lead to a higher number of individuals achieving therapeutic success after 3 months of therapy (97.0% vs 71.6% without GA). From an economic point of view, considering a projection of 1,955,447 T2DM insulin-naïve individuals, potentially treated with oral therapy, GA introduction would imply fewer individuals requiring a therapy switch (− 89.44%), with a 1.06% in costs reduction, on annual basis, thus being also the preferable solution from a cost-effectiveness perspective (cost-effectiveness value: 237.74 vs 325.53). According to experts opinions, lower perceptions on GA emerged with regard to equity aspects (0.13 vs 0.72, p-value> 0.05), whereas it would improve both individuals (2.17 vs 1.33, p-value=0.000) and caregivers quality of life (1.50 vs 0.83, p-value=0.000). Even if in the short term, GA required additional investments in training courses (− 0.80 vs 0.10, p-value = 0.036), in the long run, GA could become the preferable technology (0.30 vs 0.01, p-value=0.018) from an organisational perspective.
Conclusion: Adding GA to traditional glycaemic control instruments could improve the clinical pathway of individuals with T2DM, leading to economic and organisational advantages for both hospitals and National Healthcare Systems.
Keywords: glycated albumin, type 2 diabetes mellitus, T2DM, Health Technology Assessment, economic evaluation, multidimensional approach
Introduction
Diabetes mellitus (DM) is a perfect example of a chronic disease that represents a significant burden on individuals and healthcare systems in the European Union and beyond, considering both insurance-based and National Healthcare Service (NHS)-based healthcare systems. According to the International Diabetes Federation, and considering type 2 diabetes mellitus (T2DM), in Europe almost 60 million people have T2DM and the number is projected to exceed 70 million by 2045, as more people live longer and grow heavier.1
The primary aim of T2DM individuals care, and consequently of antiglycemic oral therapies, is the achievement and the maintenance of glycemia in target, regulating blood glucose, and retaining glycaemia at (or below) the percentage of all haemoglobin that is glycated considering the target of 7% (53 mmol/mol). Strict glycaemic control in individuals with T2DM decreases the incidence of diabetic complications, which could determine the quality of life and prognosis of such chronic population.2,3
With regard to T2DM glycaemic control, traditionally, glycated haemoglobin (HbA1c), is an important indicator for long-term glucose monitoring, representing, together with fasting plasma glucose (FPG), the standard panel of in vitro diagnostics instruments for this specific setting.4–9 However, HbA1c may not be suitable for the evaluation of short-term variations of glycaemic control because of the long lifespan of erythrocyte.4,10,11
Over the last few years, an innovative glycaemic marker has emerged in clinical practice, which is useful for monitoring glycaemic control in T2DM individuals:6 glycated albumin (GA), to be implemented in addition to the above-mentioned traditional monitoring instruments (HbA1c and FPG), as an add-on strategy. GA, a ketoamine formed by non-enzymatic glycation of serum albumin, reflects short-term (2–3 weeks) mean glycaemic levels.12,13 Furthermore, GA values are not affected by changes in erythrocyte lifespan,14 and measurement of GA is not influenced by anaemia or other individuals’ clinical conditions or comorbidities (i.e. individuals with diabetes on dialysis), which could invalidate HbA1c measurements, in the diagnosis and monitoring of diabetes.15,16
Hence, this assay accurately reflects glycaemic control in T2DM individuals, whether their antihyperglycemic regimens are stable or being changed to improve control, thus also predicting future HbA1c levels, and consequently being helpful to clinicians wishing to evaluate early treatment responses or predict deteriorations in glycaemic control.17 Despite the importance of this innovative glycaemic marker, at present, its use in the Italian clinical practice is not yet standardized. Conversely, Asian Countries, such as Japan and China, have already utilized this innovative glycaemic marker in routine practice, with its inclusion in specific country-oriented guidelines and recommendations, as well as a consequent specific reimbursement tariff development.18–20
Therefore, an in-depth study is needed, particularly in the European setting, with a specific focus on Italy, since the Italian context represents the second In Vitro Diagnostic (IVD) market, after Germany, thus being the perfect location to evaluate the potential GA diffusion and impacts in both insurance-based and NHS-based healthcare systems.21 This is consistent with the European regulation on medical devices, reporting that once a product has proven its safety, efficacy and quality, it may need to go through an evaluation of its value compared with existing healthcare interventions, before being granted full access to markets.22 The governments, both at local and central level, would evaluate and consider only those innovations that were able to demonstrate their value-for money, and cost-effectiveness.23
Beyond these premises, the study aims at defining the potential benefits of GA introduction in the Italian clinical practice, as an add-on technology to the traditional glycaemic monitoring systems (Hb1Ac and FPG), thus creating consensus with regard to its routinely use in monitoring T2DM individuals, and answering to the following policy question:
Could GA be considered an appropriate and sustainable glycaemic marker to be implemented within the Italian NHS, for the adequate monitoring activity of T2DM insulin-naïve individuals?
This could support the decision-making process of all European and international Countries not yet using GA, by providing evidence-based information, with regard to its effectiveness, safety, efficiency and sustainability.
Methods
A Health Technology Assessment (HTA) was conducted in 2018–2019, considering the Italian NHS perspective and focusing on insulin-naïve individuals affected by T2DM diabetes, treated with oral therapies.
Due to the multi-dimensional and multi-disciplinary nature of an HTA, several aspects of the medical technologies were considered, as stated within the EUnetHTA Core Model.23 The following dimensions were analysed: i) relevance of the health problem; ii) technical description of the technologies under assessment; iii) safety; iv) efficacy and effectiveness; v) economic and financial impact; vi) equity; vii) legal aspects; viii) social and ethical impact; and ix) organisational impact.
A Focus on the Assessment of the Dimensions
The above dimensions were deployed considering the following methodological approaches.
a) A systematic literature review was conducted, to retrieve the safety and the efficacy profiles of both the traditional instruments and the GA add-on strategy potential impact, as well as to identify the target population eligible to GA use.
The PICO approach (Problem/population, Intervention, Comparator and Outcome) for literature retrieval was identified:24,25 i) P (population) - insulin-naïve individuals affected by T2DM, treated with oral therapies; ii) I (intervention) - introduction of GA to be implemented with Hb1Ac and FPG; iii) C (comparator) - traditional panel of instruments for glycaemic control (Hb1Ac and FPG); iv) O (outcome) - clinical effectiveness, in terms of rate of individuals achieving therapeutic success after 3 months of therapy.
Literature evidence came from a systematic search of literature databases (PubMed, Embase and Cochrane Library), from 2011 up to December 2020, considering the following search strategy: “glycosylated serum albumin”[Supplementary Concept] OR “glycosylated serum albumin”[All Fields] OR “glycated albumin”[All Fields]. Besides consistency with the search strategy, the defined inclusion criteria were the following: i) number of patients enrolled in the study (> 20); ii) journal impact-factor (> 1); iii) study design and clarity of the comparative claim. Once identified the papers to be included in the HTA, an independent validation of the scientific evidence available on the topic was performed, through the CASP (Critical Appraisal Skills Programme) checklist, with the support of 7 experts (3 methodological experts, 2 diabetologists and 2 laboratory experts).26
b) Health economics tools have been used for the economic evaluation of the clinical pathway and for budget impact analysis. The clinical pathway was defined in terms of standard procedures performed by T2DM individuals, according to structured interviews with 5 clinicians, referring to 5 Italian hospitals. A final approval and agreement from the clinicians of reference, in accordance with a Delphi approach,27 was retrieved, considering the following items that were mapped. i) Number and typology of blood/laboratory exams; ii) number and typology of diagnostic procedures; iii) number and typology of diabetic visits and other specialist visits; and iv) number and typology of self-monitoring of blood glucose. The standard clinical pathway, related to the implementation of only traditional instruments, was carried out and evaluated, comparing the clinical pathway of the individuals who have not experienced a therapy switch within a 12-month time horizon of treatment and monitoring, and the clinical pathway of the individuals who have experienced a therapy switch, during the 12-month time horizon of treatment and monitoring. It should be noted here that the therapeutic switch rate was hypothesized from scientific literature, in terms of diabetic individuals deemed to not have an effective response to the current oral therapy, since they did not achieve the glycemia in target.28 Furthermore, the innovative clinical pathway with GA introduction, was also hypothesised and accordingly valorised, starting from the traditional approach pathway analysis, thus defining possible changes in the number of blood exams specialist visits or diagnostic procedures. The above economic information was evaluated, in accordance with outpatients/hospital admission National Reimbursement Tariffs, already valid for years 2020–2021.29
The economic evaluation of the two clinical pathways was integrated with a cost-effectiveness analysis and a budget impact analysis. On one hand, the cost-effectiveness value indicator (CEV), in average terms, was determined in order to choose the technology that shows a better cost-effectiveness trade-off (calculated as cost per T2DM individual divided by the efficacy indicator, in terms of percentage of individuals achieving therapeutic success after 3 months of therapy), for both scenarios. On the other hand, the budget impact analysis compared the “AS IS” situation (use of only the traditional instruments), with the “TO BE” situation (introduction of the GA test in addition to the traditional panel of instruments), in order to define the economic sustainability of the innovative marker. A 100% replacement rate was assumed, for the introduction of the new technology, and the number of eligible T2DM individuals was determined, based on the Italian epidemiological T2DM prevalence rates available in the national evidence.29,30
c) Administration of qualitative questionnaires filled out by 15 healthcare T2DM diabetes experts (5 laboratory experts, 1 epidemiologist, 5 diabetes clinicians, 2 strategic directions, 2 representative of patients associations), representative of all the stakeholders across Italy (referring to both public and private hospitals) who have specific knowledge of the use of GA, because of their involvement in experimental studies on the topic.
The qualitative questionnaires were used for examining clinicians’ perceptions on equity, social, legal, and organisational aspects, considering a comparative approach of the two panels of technology being assessed, in accordance with a 7-item Likert scale ranging from – 3 to +3.31
All the items used for the deployment of each qualitative dimension, derived from the EUnetHTA Core Model issues,23 with specific integrations and modifications, in relation with the nature of the technology being assessed.
The above qualitative method was useful to collect a wide range of ideas and opinions that individuals carry out about issues and topics, as well as divulge viewpoint differences among stakeholders’ groups.32–34 Furthermore, for under discovered research areas, qualitative methods attempt to fill in gaps that are left unexposed by survey-based research, as well as literature evidence.35
A Focus on the Statistical Methods
Data were first synthetized, considering descriptive statistics. Statistically significant differences were analyzed, using parametric or not parametric tests, depending on the normal distribution of the variables investigated.
With regard to the economic dimension, a sensitivity analysis was conducted, by means of Bayesian methods, useful to provide a complete paradigm for both statistical inference and decision making under uncertainty.36,37 Gamma distributions were accordingly developed, in order to verify the robustness of the results, in presence of uncertainty factors (clinical pathway cost and CEV parameters were analyzed). The probability to have: i) any average cost value of the gamma distribution of the innovative panel of technology, lower with respect to the traditional one, and ii) any average CEV of the gamma distribution of the innovative panel of technology, lower with respect to the traditional one, was evaluated.
Results
Results from Literature Review
The search for Mesh terms resulted in 612 records. Out of them, only 50 were assessed for eligibility. In accordance with the above-mentioned search strategy, only 5 articles13,28,38–41 met the inclusion criteria defined in the methodology section, focusing on the specific use of GA for T2DM insulin-naïve individuals and comparing GA and HbA1c, as presented in the Prisma Flow Chart (Supplementary Figure 1). The other 45 articles had different aims, without focusing the attention on efficacy/safety data, but presenting sensibility and specificity information, concerning the presence of a strict correlation between GA and HbA1c.
Literature review stated that the introduction of GA as add-on strategy could improve both safety and the efficacy profiles, in comparison with the use of only traditional monitoring instruments.
From a safety point of view, GA could be a better relative risk predictor in the development of diabetes complications compared with using HbA1c alone, considering diabetic retinopathy, nephropathy, and cardiovascular events development.42–46
From an efficacy point of view, GA would increase the number of individuals achieving therapeutic success after three months of therapy (97.0% vs 71.6%), - in terms of individuals deemed to have effective response to oral therapy - with a consequent decrease in people with diabetes requiring a therapeutic switch.28 This would strengthen the consideration that GA is a useful marker for the monitoring activities of diabetes, thus being able to determine the effectiveness of treatment before initiating or changing medication for individuals with diabetes.12,47 Indeed, there may be no discernible reduction in the HbA1c level until several weeks after starting treatment, which may delay the determination of whether the specific therapeutic regimen is effective.28
Results from the Health Economics Evaluation
The economic evaluation of the “AS IS” and the “TO BE” scenario is detailed in Table 1, thus revealing a statistically significant difference between an individual who has not experienced a therapy switch within a 12-month time horizon and an individual who has experienced a therapy switch within a 12-month time horizon, in both scenarios (p-value = 0.000).
 |
Table 1 Economic Evaluation of the Diabetic Individual’s Clinical Pathway Derived from Delhi Approach Implementation |
In the comparison between the weighted average cost, considering the therapeutic switch occurrence rate,28 in terms of diabetic individuals not achieving an oral response therapy, no statistically significant differences emerged (€ 233.08 vs € 230.61, p-value > 0.05). However, sensitivity analysis reports that the innovative clinical pathway panel presented a probability to absorb lower economic resources equal to 74.53%, considering a 12-month time horizon (Figure 1).
 |
Figure 1 Gamma distributions for costs. |
Table 2 reports that the innovative panel of technology could be the preferable solution to be adopted from a cost-effectiveness point of view, thus always presenting the better trade-off between costs and effectiveness, with respects to the traditional instruments (Figure 2).
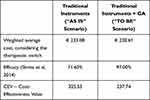 |
Table 2 Cost-Effectiveness Analysis |
 |
Figure 2 Gamma distributions for cost-effectiveness value. |
Whereas a CEA evaluates both costs and outcomes of alternative technologies over a specified time horizon, to estimate their economic efficiency, a budget impact analysis (BIA) is based on their affordability within a specific setting.
Based on the Italian population in 2018 and the diabetes prevalence rate, equal to 5.3%,30 3,205,651 Italian individuals suffer from T2DM diabetes. Out of them, 61% are being treated with oral therapies,31 thus resulting in 1,955,447 individuals, who could be potential users of the new GA glycaemic biomarker.
Given the economic evaluation previously mentioned, as well as the percentage of individuals experiencing a therapy switch, the GA test introduction would lead to fewer individuals requiring a therapy switch (−89.44%), with an economic advantage of 1.06% (in a 12-month time horizon). The Italian NHS could save € 4,835,985, through the proper clinical management of 1,955,447 type 2 diabetic insulin-naïve individuals, treated with oral therapy (Table 3).
 |
Table 3 Budget Impact Analysis |
Results from the Qualitative Assessment
The analysis of the qualitative perceptions of the healthcare professionals involved (Table 4) (as already explained, considering a 7-item Likert Scale, ranging from – 3 to + 3), reported that the traditional instruments could be considered the preferable technology (0.72 vs 0.13, p-value > 0.05), from an equity perspective. This consideration may be justified by limited accessibility to GA (−0.42 vs 1.83, p-value = 0.000), since the innovative technology has not yet been used and implemented in the Italian laboratories. In contrast, GA could be the preferable glycaemic marker, considering the professionals’ perception on the item “existence of factors limiting the use of the technology” (1.33 vs 0.67, p-value = 0.000), covering a larger population. In fact, GA is not influenced by erythrocyte lifespan, nor by anaemia, or other individuals’ clinical conditions, which invalidate HbA1c measurements, in the monitoring of diabetes.12,45,48–50
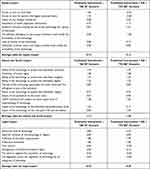 |
Table 4 Qualitative Assessment of the Equity, Ethical, Social and Legal Impacts |
The introduction of a GA test would improve the quality of life of both individuals with diabetes (1.33 vs 2.17, p-value = 0.000) and caregivers (0.83 vs 1.50, p-value = 0.000), since it is related to better glycaemic control monitoring and a lower relative risk of developing diabetes-related complications and adverse events.
An analysis of the legal implications reported that the two technologies under assessment could be considered super-imposable in their measurement (p-value > 0.05). Additional legal efforts are required regarding the regulation of GA acquisition.
Focusing on the organisational dimension (Table 5), in the short term (12 months), the GA test acquired a lower score than the comparator, since it needs additional investments in training courses for all those who are involved in the procedure (−0.80 vs 0.10, p-value = 0.036). A component that impacts significantly on the organisation appeared to be the acquisition of the new technology (−0.20 vs 0.00, p-value > 0.05), as well as the updating of laboratory equipment currently in use (−0.50 vs 0.00, p-value > 0.05), even if no statistically significant differences emerged. However, the implementation and the adoption of GA in clinical practice would allow an improvement in the diabetic individuals’ clinical pathway (0.90 vs 0.10, p-value = 0.015).
 |
Table 5 Organisational Impact |
Over a 36-month time-period from market penetration, there was a contraction in the above-mentioned drawbacks. The healthcare professionals, having become competent at using the innovative technology, no longer need to attend training courses. In this view, it emerges that the innovative technology may be considered the most preferred alternative from an organisational point of view, with an average value of 0.30 (p-value = 0.018).
Discussion
The results of the study generate an interesting scientific contribution, thus covering an important knowledge gap, regarding the implementation of GA test, in clinical practice, for glycaemic control in insulin-naïve individuals affected by T2DM. This is particularly important, because both early diagnosis of diabetes and strict glucose control are crucial for preventing or delaying the onset of serious, even life-threatening complications.51 In this view, the HTA results strengthen this consideration, showing that the introduction of GA in addition to the traditional instruments for glycaemic control may be considered a valid technological alternative, for the treatment of T2DM people with diabetes. As stated in literature evidence, the introduction of GA as an add-on technology presents advantages in both safety and efficacy profiles, with a consequent positive impact, concerning both the economic and the individual’s perspective.3,28,38–41
Results have demonstrated the feasibility and the sustainability of GA introduction into the clinical practice, revealing the need for less investment related to its acquisition. Additional advantages of GA over HbA1c are represented by its comparable costs, and by the possibility to process the GA test using conventional laboratory clinical chemistry analysers, without additional organisational effort and being consistent with literature evidence available on the topic.51 According to that, the budget impact analysis showed that the investment for GA routine implementation could be absorbed within the first year after its introduction, thus also leading to economic advantages related to the optimisation of the clinical pathway of T2DM insulin-naïve individuals, treated with oral therapies. This economic advantage could therefore be variable from a minimum of 1.06% to a maximum of 4.58%, strictly dependent on the number of people with diabetes requiring a therapeutic switch.
On the other hand, higher perceptions regarding the ethical and social profile of GA introduction emerged: it would improve the quality of life of both individuals with diabetes and the related caregivers, as it is related with better monitoring of blood glucose and a lower risk of complications. According to the above, a topic for further research could be represented by the integration of the HTA results, especially referring to the social dimensions, with specific patient-reported outcome measures (PROMs), thus investigating the level of diabetes distress perceived by people living with this chronic disease.
The main strength of the present study is that it provides a “real-life” picture of the potential implications of GA in the Italian clinical practice, thus giving an overview of the modification of the patient clinical pathway, with a consequent economic resources absorption estimation. It should be noted that, even though results could be influenced by Italian local issues, the clinical pathway is consistent with the International Guidelines on the topic, with regard to the exams and procedures devoted to people with diabetes, being, thus, generalizable. The only pattern that could change worldwide, is the economic evaluation of the single item of healthcare expenditure (in terms of tariffs and prices), even if the economic dimension, on the whole, could be replicable within both NHS-based and insurance-based Countries, as demonstrated in the sensitivity analysis, confirming the robustness of the results.
Although GA has been studied over the last few years, this in-vitro diagnostic test is not yet widely used in the European clinical laboratory routine, and few commercial products are yet available on the market for this test, thus requiring the need of a national and international consensus about clinical laboratory procedures and the clinical use of GA, and guaranteeing its inclusion in clinical laboratory routines. In particular, despite its proven clinical effectiveness, GA test is not included in any Italian clinical guideline and/or algorithm, thus requiring an in-depth evaluation as already performed in other Asian Countries.20
However, the results of the study, according to an HTA approach useful to validate the implementation of any innovative technology, with the integration of clinical and managerial information, make GA a promising marker to use for glycaemic control in people with T2DM, thus showing the strategic relevance of GA, in the improvement of the clinical pathway of individuals with diabetes, freeing-up NHS resources, for public and private sector, also ensuring a better equity and social profile for individuals with diabetes.
This could be consistent with scientific recommendation available on the topic, in fact both the American Diabetes Association (ADA) and the European Association Diabetes Study (EASD) suggests a “patient-centred” management of glycemic control in T2DM individuals, and the selection only of biomarkers, such as GA, that could be able to reflect the individual health status, maintaining the balance between risks and benefits.9
Abbreviations
BIA, budget impact analysis; CEA, cost-effectiveness analysis; CEV, cost-effectiveness value; DM, diabetes mellitus; Hb1Ac, glycated haemoglobin; HTA, Health Technology Assessment; IVD, In vitro diagnostic; GA, glycated albumin; FPG, fasting plasma glucose; NHS, National Health Service; T2, type 2; T2DM, type 2 diabetes mellitus.
Data Sharing Statement
Data will be available upon reasonable request.
Ethics Approval and Informed Consent
Not applicable, since the research activity investigated only the standard clinical pathway devoted to any T2DM individuals, without collecting human and sensible data. Furthermore, besides the process mapping approach used for the definition of the standard clinical practice, clinicians’ perceptions were collected according to a qualitative questionnaire. All the clinicians involved voluntary completed the questionnaire, whose perceptions were analyzed using aggregated methods, in accordance with the “EU Regulation n. 679 of 04.05.2016”.
Consent for Publication
All the clinicians involved were aware that the present research activity had as main aim the publication of the results, and they gave their consent in disseminating their perceptions, in an aggregated and anonymous manner, in accordance with the “EU Regulation n. 679 of 04.05.2016”.
Acknowledgments
The Authors would like to thank all the professionals involved, for their valuable support to complete the qualitative and quantitative questionnaires, leading to the success of the present research activity.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
There is no funding to report.
Disclosure
Dr Antonio Nicolucci reports grants from Astra Zeneca, grants from AlfaSigma, grants from Sanofi, grants from Medtronic, grants from Eli Lilly, grants from Novo Nordisk, grants from Pikdare, grants from Shionogi, grants from SOBI, outside the submitted work. Dr Emanuela Foglia reports non-financial support from Instrumentation Laboratories - Werfen, personal fees from Instrumentation Laboratories - Werfen, outside the submitted work. The authors declare that they have no other conflicts of interest in connection with the submitted article.
References
1. International Diabetes Federation. IDF diabetes atlas – 9th edition; 2019. Available from: https://www.diabetes.org.br/publico/images/Atlas-IDF-2019.pptx.pdf.
2. Rodríguez-Gutiérrez R, Montori VM. Glycemic control for patients with type 2 diabetes mellitus: our evolving faith in the face of evidence. Circ Cardiovasc Qual Outcomes. 2016;9(5):504–512. doi:10.1161/CIRCOUTCOMES.116.002901
3. Moodahadu LS, Dhall R, Zargar AH, Bangera S, Ramani L, Katipally R. Tight glycemic control and cardiovascular effects in type 2 diabetic patients. Heart Views. 2014;15(4):111–120. doi:10.4103/1995-705X.151084
4. Goldstein DE, Little RR, Lorenz RA, Malone JI, Nathan DM, Peterson CM; American Diabetes Association. Tests of glycemia in diabetes. Diabetes Care. 2003;26(Suppl 1):S106–8.
5. Sherwani SI, Khan HA, Ekhzaimy A, Masood A, Sakharkar MK. Significance of HbA1c test in diagnosis and prognosis of diabetic patients. Biomark Insights. 2016;11:95–104. doi:10.4137/BMI.S38440
6. Ohde S, Deshpande GA, Yokomichi H, et al. HbA1c monitoring interval in patients on treatment for stable type 2 diabetes. A ten-year retrospective, open cohort study. Diabetes Res Clin Pract. 2018;135:166–171. doi:10.1016/j.diabres.2017.11.013
7. World Health Organization. Use of glycated haemoglobin (HbA1c) in the diagnosis of diabetes mellitus abbreviated report of a WHO consultation. Geneva: World Health Organization; 2011.
8. Sacks DB. Hemoglobin A1c in diabetes: panacea or pointless? Diabetes. 2013;62(1):41–43. doi:10.2337/db12-1485
9. American Diabetes Association. Standards of medical care in diabetes. Diabetes Care. 2019;42(Supplement 1):S1–S2. doi:10.2337/dc19-Sint01
10. Weykamp C. HbA1c: a review of analytical and clinical aspects. Ann Lab Med. 2013;33:393–400. doi:10.3343/alm.2013.33.6.393
11. Krhač M, Vučić Lovrenčić M. Update on biomarkers of glycemic control. World J Diabetes. 2019;10(1):1–15. doi:10.4239/wjd.v10.i1.1
12. Furusyo N, Hayashi J. Glycated albumin and diabetes mellitus. Biochim Biophys Acta. 2013;1830(12):5509–5514. doi:10.1016/j.bbagen.2013.05.010
13. Koga M, Kasayama S. Clinical impact of glycated albumin as another glycemic control marker. Endocr J. 2010;57(9):751–762. doi:10.1507/endocrj.K10E-138
14. Kosecki SM, Rodgers PT, Adams MB. Glycemic monitoring in diabetics with sickle cell plus beta-thalassemia hemoglobinopathy. Ann Pharmacother. 2005;39(9):1557–1560. doi:10.1345/aph.1G010
15. Peacock TP, Shihabi ZK, Bleyer AJ, et al. Comparison of glycated albumin and hemoglobin A(1c) levels in diabetic subjects on hemodialysis. Kidney Int. 2008;73(9):1062–1068. doi:10.1038/ki.2008.25
16. Inaba M, Okuno S, Kumeda Y, et al.; Osaka CKD Expert Research Group. Glycated albumin is a better glycemic indicator than glycated hemoglobin values in hemodialysis patients with diabetes: effect of anemia and erythropoietin injection. J Am Soc Nephrol. 2007;18(3):896–903. doi:10.1681/ASN.2006070772
17. Desouza CV, Holcomb R, Rosentock J, et al. Results of a study comparing glycated albumin to other glycemic indices. J Clin Endocrinol Metab. 2020;105(3):677–687. doi:10.1210/clinem/dgz087
18. Araki T, Ishikawa Y, Okazaki H, et al. Introduction of glycated albumin measurement for all blood donors and the prevalence of a high glycated albumin level in Japan. J Diabetes Investig. 2012;3(6):492–497. doi:10.1111/j.2040-1124.2012.00224.x
19. Hsu P, Ai M, Kanda E, et al. A comparison of glycated albumin and glycosylated hemoglobin for the screening of diabetes mellitus in Taiwan. Atherosclerosis. 2015;242(1):327–333. doi:10.1016/j.atherosclerosis.2015.07.037
20. Nakao T, Inaba M, Abe M, et al. Best practice for diabetic patients on hemodialysis 2012. Ther Apher Dial. 2015;19:40–66. doi:10.1111/1744-9987.12299
21. MedTech Europe. European IVD Market statistics report; 2019. Available from: https://www.medtecheurope.org/wp-content/uploads/2019/12/2019_MTE_European-IVD-Market-Statistics.pdf.
22. Regulation (EU) 2017/746 of the European Parliament and of the Council of 5 April 2017 on in vitro diagnostic medical devices and repealing Directive 98/79/EC and Commission Decision 2010/227/EU. Available from: https://eur-lex.europa.eu/legal-content/EN/TXT/?uri=CELEX:02017R0746-20170505.
23. EUNetHTA. The HTA core model, version 3.0; January 2016. Available from: http://eunethta.eu/sites/5026.fedimbo.belgium.be/files/HTACoreModel3.0.pdf.
24. Huang X, Lin J, Demner-Fushman D. Evaluation of PICO as a knowledge representation for clinical questions. AMIA Ann Symp Proc. 2006;359–363.
25. Schardt C, Adams MB, Owens T, et al. Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med Inform Decis Mak. 2007;7:16. doi:10.1186/1472-6947-7-16
26. Critical Appraisal Skills Programme (CASP). Critical Appraisal Skills Programme (CASP); 2015. Available from: https://casp-uk.net/casp-tools-checklists/.
27. Quinn Patton M. Qualitative research & evaluation methods, third edition. Sage publications; 2002.
28. Shima K, Komatsu M, Noma Y, Miya K. Glycated albumin (ga) is more advantageous than hemoglobin a1c for evaluating the efficacy of sitagliptin in achieving glycemic control in patients with type 2 diabetes. Intern Med. 2014;53:829–835. doi:10.2169/internalmedicine.53.1364
29. Italian Ministry of Health. Outpatients/hospital admission National Reimbursement Tariffs. Available from: https://www.trovanorme.salute.gov.it/norme/renderPdf.spring?seriegu=SG&datagu=28/01/2013&redaz=13A00528&artp=3&art=1&subart=1&subart1=10&vers=1&prog=001.
30. Istituto Nazionale di Statistica. Il diabete in Italia; 2017. Available from: https://www.istat.it/it/files//2017/07/REPORT_DIABETE.pdf.
31. Associazione Medici Diabetologi. Le monografie degli Annali AMD. Diabete, Obesità e Malattia Cardiovascolare: lo scenario italiano; 2019. Available from: http://aemmedi.it/wp-content/uploads/2019/01/Annali-AMD-2018-password.pdf.
32. Mitton C, Dionne F, Damji R, Campbell D, Bryan S. Difficult decisions in times of constraint: criteria based resource allocation in the vancouver coastal health authority. BMC Health Serv Res. 2011;11(1):169. doi:10.1186/1472-6963-11-169
33. Berg B. Qualitative Research Methods for the Social Sciences. MA: Pearsons Education Inc.; 2009.
34. Kitzinger J. Qualitative research. Introducing focus groups. Br Med J. 1995;311(7000):299. doi:10.1136/bmj.311.7000.299
35. Jansen H. The logic of qualitative survey research and its position in the field of social research methods. 2010.
36. Mullen PD, Reynolds R. The potential of grounded theory for health education research: linking theory and practice. Health Educ Behav. 1978;6(3):280–294.
37. Spiegelhalter DJ, Myles JP, Abrams KR. Bayesian Approaches to Clinical Trials and Health-Care Evaluation. New York: Wiley N.Y; 2003.
38. Bernardo JM, Smith AFM. Bayesian Theory. West Sussex, England: John Wiley & Sons Ltd; 1994.
39. Won HK, Kim KJ, Lee BW, Kang ES, Cha BS, Lee HC. Reduction in glycated albumin can predict change in hba1c: comparison of oral hypoglycaemic agent and insulin treatments. Diabet Med. 2012;29:74–79. doi:10.1111/j.1464-5491.2011.03386.x
40. Koga M, Murai J, Saito H, Kasayama S. Prediction of near-future glycated hemoglobin levels using glycated albumin levels before and after treatment for diabetes. J Diabetes Investig. 2011;2:304–309. doi:10.1111/j.2040-1124.2011.00107.x
41. Lu JM, Ji LN, Li YF, et al. Glycated albumin is superior to glycated hemoglobin for glycemic control assessment at an early stage of diabetes treatment: a multicenter, prospective study. J Diabetes Complications. 2016;30:1609–1613. doi:10.1016/j.jdiacomp.2016.07.007
42. Li ZL, Liu JC, Liu SB, Li XQ, Yi DH, Zhao MG. Improvement of vascular function by acute and chronic treatment with the GPR30 agonist G1 in experimental diabetes mellitus. PLoS One. 2012;7(6).
43. Murea M, Moran T, Russell GB, et al. Glycated albumin, not hemoglobin A1c, predicts cardiovascular hospitalization and length of stay in diabetic patients on dialysis. Am J Nephrol. 2012;36(5):488–496. doi:10.1159/000343920
44. Song SO, Kim KJ, Lee BW, Kang ES, Cha BS, Lee HC. Serum glycated albumin predicts the progression of carotid arterial atherosclerosis. Atherosclerosis. 2012;225(2):450–455. doi:10.1016/j.atherosclerosis.2012.09.005
45. Xue Y, Sheng Y, Dai H, Cao H, Liu Z, Li Z. Risk of development of acute pancreatitis with pre-existing diabetes: a meta-analysis. Eur J Gastroenterol Hepatol. 2012;24(9):1092–1098. doi:10.1097/MEG.0b013e328355a487
46. Giglio RV, Lo Sasso B, Agnello L, et al. Recent updates and advances in the use of glycated albumin for the diagnosis and monitoring of diabetes and renal, cerebro- and cardio-metabolic diseases. J Clin Med. 2020;9:3634. doi:10.3390/jcm9113634
47. Patti AM, Rizvi AA, Giglio RV, Stoian AP, Ligi D, Mannello F. Impact of glucose-lowering medications on cardiovascular and metabolic risk in type 2 diabetes. J Clin Med. 2020;9:912. doi:10.3390/jcm9040912
48. Gram-Hansen P, Eriksen J, Mourits-Andersen T, Olesen L. Glycosylated haemoglobin (HbA1c) in iron- and vitamin B12 deficiency. J Intern Med. 1990;227(2):133–136. doi:10.1111/j.1365-2796.1990.tb00131.x
49. Coban E, Ozdogan M, Timuragaoglu A. Effect of iron deficiency anemia on the levels of hemoglobin A1c in nondiabetic patients. Acta Haematol. 2004;112(3):126–128. doi:10.1159/000079722
50. Church D, Simmons D. More evidence of the problems of using HbA1c for diagnosing diabetes? The known knowns, the known unknowns and the unknown unknowns. J Intern Med. 2014;276(2):171–173. doi:10.1111/joim.12200
51. Danese E, Montagnana M, Nouvenne A, Lippi G. Advantages and pitfalls of fructosamine and glycated albumin in the diagnosis and treatment of diabetes. J Diabetes Sci Technol. 2015;9(2):169–176. doi:10.1177/1932296814567227
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
