Back to Journals » International Journal of Chronic Obstructive Pulmonary Disease » Volume 15
Frustrated Caring: Family Members’ Experience of Motivating COPD Patients Towards Self-Management
Authors Sigurgeirsdottir J , Halldorsdottir S , Arnardottir RH , Gudmundsson G , Bjornsson EH
Received 25 July 2020
Accepted for publication 14 October 2020
Published 17 November 2020 Volume 2020:15 Pages 2953—2965
DOI https://doi.org/10.2147/COPD.S273903
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Richard Russell
Jonina Sigurgeirsdottir,1,2 Sigridur Halldorsdottir,3 Ragnheidur Harpa Arnardottir,3– 5 Gunnar Gudmundsson,1,6 Eythor Hreinn Bjornsson2
1University of Iceland, Medical Faculty, Reykjavik, Iceland; 2Reykjalundur Rehabilitation Center, Lung Department, Mosfellsbaer, Iceland; 3University of Akureyri, School of Health Sciences, Faculty of Graduate Studies, Akureyri, Iceland; 4Akureyri Hospital, Department of Rehabilitation, Akureyri, Iceland; 5Uppsala University, Department of Medical Sciences, Respiratory-, Allergy- and Sleep Research, Uppsala, Sweden; 6Landspitali University Hospital, Department of Respiratory Medicine, Reykjavik, Iceland
Correspondence: Jonina Sigurgeirsdottir
Reykjalundur Rehabilitation Center, Lung Department, Mosfellsbaer 270, Iceland
Tel +354 6261740
Email [email protected]
Aim: The aim of this phenomenological study was to explore principal family members’ experience of motivating patients with chronic obstructive pulmonary disease (COPD) towards self-management.
Methods: Interviews were conducted with 10 family members (spouses and adult children) of COPD patients. The interviews were audio recorded, transcribed and analyzed thematically.
Results: Being a principal family member of a COPD patient is characterized by frustrated caring; wanting the best for him/her and yet carrying a heavier burden than the person feels equipped for, lacking both knowledge about the disease progress and information about available healthcare resources. The situation demands much energy, due to COPD patients’ lack of stamina; family members’ fear of the patient’s possible breathlessness; willingness to help, though sometimes meeting with negative reactions from the patient; and feeling ignored by health professionals (HPs). Family members expressed a need for a formal connection between patient–family–HPs. The increasing burden experienced by patients’ family members is characterized by a sequential process in three phases of the patient’s declining self-management. In the early phase, family and patient are ignorant of COPD yet recognize the patient’s smoking as a risky lifestyle. In the intermediary phase, signs of COPD become evident to the family. The first turning point is when the family first observes the patient’s acute exacerbation. A second turning point is in the advanced phase, when family and patient recognize COPD as a progressive disease, possibly fatal. We also identified family members’ views on COPD patients’ needs, and their own roles, main frustrations and concerns.
Conclusion: Family members’ experience of motivating COPD patients towards self-management is a sequential process where the family experiences advancing caring burden and declining self-management by the patient. We propose the establishment of COPD patients’ teams consisting of patient–family–HP, aimed at the patients’ best possible self-management.
Keywords: chronic, obstructive, family’s needs, self-management, pulmonary rehabilitation, PR, qualitative research
Introduction
When a person develops chronic obstructive pulmonary disease (COPD), family members (spouses/adult children) assume the role of informal caregivers, providing practical help, psychological support and help with healthcare utilization.1 Family caregiving is important in COPD care and patients’ self-management support, yet reference to caregivers is largely absent, even in policy documents and research agendas, and little guidance is available on how caregivers can fulfil their role.1,2 Insufficient support from health professionals (HPs) has been observed,3–9 and families may experience a burden similar to suffering from chronic illness themselves.8 Researchers call for a comprehensive focus on caregivers’ role in motivating COPD patients towards self-management1,2,10–14 where the goal to optimize patients’ health, reduce symptoms and increase function, involves the establishment of alliances with HPs, family, friends and community.15
Early intervention and family involvement by HPs may reduce the burden and distress of the patient–caregiver dyad, and enhance their chance of developing practical skills, strategies for managing adverse events and anticipation of future events.11 Lack of efforts by HPs to involve families in arranging patients’ day-to-day disease management is noteworthy, since families are expected to intervene in case of patients’ acute exacerbations.8 A lack of definition of the family’s role in managing chronic illness, and HPs’ reluctance to recognize families’ existence, leads to some feeling unseen, neglected, and unsure when to intervene and seek help.6 On the other hand, being involved in decisions can give the feeling of being knowledgeable and participating in a team, and can facilitate an active role in decision-making and risk perception.7,16 Despite constantly witnessing patients’ limitations arising from COPD, families still lack organized education on COPD management, ranging from simple home care to complex drug management,1,14 how to understand and manage the symptoms, keep active, preserve quality of life, know what to expect and how to facilitate the patient’s resources on the illness journey.5,17
Some researchers warn that caregivers’ cognitive skills need to be evaluated and ethical and legal aspects addressed; but shared decision-making is recommended, including a formal agreement on responsibility between the patient, family and HPs where families can share their knowledge of patients’ situation without losing the confidence and cooperation of HPs.4,10,16 Looseness in current collaboration between some families and HPs indicates a need for more individualized practices regarding family involvement in patients’ support, symptom management and discussions concerning the patients’ therapy.4,13
Families may prioritize the patients’ needs while compromising their own health, a fact that receives little attention from HPs and social services.18 High levels of loneliness, stress and depression experienced by COPD patients and their families may be considerably mitigated by increased social support.19
Families’ uncertainty may be alleviated by implementing coordination of individual self-management and monitoring their needs.7,14 As the expected symptom profile in COPD may provide unique challenges in the relationship, such as coping with constant breathlessness, patients with advanced COPD and their families should be screened for psychological morbidities and unmet needs.20–22 Instead of focusing on the COPD patient only, the patient–caregiver dyad might be considered as the unit of care in COPD long-term management.18,23 As families’ responsibilities increase in parallel with patients’ disease trajectory, some may need more focused education and support to enhance their caregiving role.12
There is still a gap in the literature on the role of family members of a COPD patient and a study points out a certain reluctance by patients and family members to identify emerging symptoms as the beginning of an illness trajectory.24 The aim of the present study was to explore the experience of principal family members (spouses and adult children) of motivating COPD patients towards self-management.
Materials and Methods
The research approach was the Vancouver School of Doing Phenomenology (the Vancouver School). This is a unique blend of phenomenology, hermeneutics and constructivism, with its roots in the works of Spiegelberg25 (phenomenology), Ricoeur26 (hermeneutic phenomenology), and Schwandt27 (constructivism). The focus of the Vancouver School is on increasing knowledge and deepening understanding of human phenomena, aiming at exploring participants’ experiences in order to improve human services, such as healthcare services.28 The research process involves in-depth interviews with 5 to 15 participants.29 The research process has seven main cognitive aspects that are repeated throughout the research (Figure 1) and is implemented in 12 main research steps (Table 1) where each participant is seen as a case study. Figure 2 provides an example of the interview guide. The method thus involves analysis of individual cases (Steps 1–7) followed by inter-case analysis (Steps 8–12). Through text analysis methods, researchers communicate their understanding to others by means of abstract thought processes.29 Data collection and analysis is further described in Table 1. Eight participants were principal family members of patients from a waiting list for PR who participated in a previous study,2 two were principal family members of two other patients from the waiting list, six spouses and four adult children (Table 2). Data saturation was achieved when the data made it possible to answer the research question, in the judgment of the research team.
 |
Table 1 The 12 Research Steps of the Vancouver School of Doing Phenomenology and How Those Steps Were Followed in the Present Study |
 |
Table 2 Characteristics of Participants |
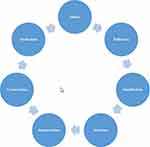 |
Figure 1 The repeated cycle of cognitive work in each of the 12 steps in the Vancouver School of Doing Phenomenology. |
 |
Figure 2 The main frame of the interview guide in the study. |
The participant informed consent included publication of anonymized responses, and this study was conducted in accordance with the Declaration of Helsinki. The Icelandic National Bioethics Committee gave ethical clearance for conducting the study (Reference number 17–120). The study was explained to the participants, in writing and orally, emphasizing that participation was voluntary and could be withdrawn at any time. All participants signed an informed consent which included a name and contact details of a person they could contact in case of emotional troubles caused by participation in the study. The study was funded by Oddur Olafsson scientific research fund at Reykjalundur Rehabilitation Institute, and the B-section of the Science Fund of the Icelandic Nurses’ Association.
Results
Frustrated caring was the essence of family members’ experience of motivating a COPD patient towards self-management. They wanted the best for the COPD patient but felt frustrated by the exacerbation of the disease, being aware of patients’ smoking relapses. They expressed a need for a formal connection between patient, family and a knowledgeable HP who could be their contact person within the healthcare system.
We identified three sequential phases in family members’ experience: early, intermediary and advanced phases (Figure 3), with two decisive turning points; the first when the family first witnessed the patient’s acute exacerbation, and the second, when they understood COPD as a disease trajectory, which created increased burden for the family and the patient, and might prove fatal. As patients’ self-management decreased, the families’ caring burden increased. We also identified families’ perspectives on COPD patients’ needs, roles of principal family members and their main frustrations (Table 3), and their perspectives on patient–family–HPs teamwork (Table 4).
 |
Table 3 The Family Members’ Perspectives on COPD Patients’ Needs, Roles of Family Members as Caregivers, and Their Main Frustrations |
 |
Table 4 Principal Family Members’ Perspectives on Patient–Family–HPs as a Team |
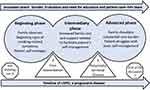 |
Figure 3 Principal family members’ perspective of the increasing caring burden caused by the progression of COPD, the need for education and a patient–family member–HPs team approach. |
Early Phase: Patient Self-Manages
Being a principal family member of a COPD patient may involve years of observing the developing disease, and even participating in smoking. While COPD slowly embedded in the patient’s lungs with only mild symptoms, they self-managed. The patient may have consulted a doctor because of beginning symptoms, but signs of COPD were not identified as such by family members, and no diagnosis had been presented to the family.
Physicians Warned the Patients About Smoking, but Some Persisted in the Habit
She started seeing a doctor and this [COPD] worsened gradually [...] and, she had a severe problem with smoking cessation [...] repeatedly admitted to the lung department, severely ill and, her oxygen saturation dropped down to 75[%]. (Husband/P5)
Discussions about smoking tended to become a sensitive subject between family members and smoking patients. Families observed patients’ struggle with smoking cessation, but any efforts to help were “just taken as criticism [...]. I understood she had to decide this for herself” (Husband/P1). Gradually increased breathlessness was identified with time:
I had sensed this [breathlessness] for several years, if we went out walking, [wife] would always be stopping, leaning against a handrail [...] She was stopping to get her breath back. At first I did not realize, but later I did.. (Husband/P2)
Being almost entirely ignorant of COPD, the families were reliant on the patients themselves to learn what could be done to relieve their symptoms. Some lacked time or willingness to follow up on patients’ COPD, experiencing themselves as “nagging” or being “nasty” around this “self-inflicted suffering”. Family members became irritated and frustrated when the patients spent their day in bed, reverted to smoking and/or refused to participate in domestic tasks.
I am certainly not asking him to sweep a whole community house, only our small home. (Wife/P3)
Intermediary Phase: Patient Self-Manages with Help from Family Members
The family members in the intermediary phase learned about COPD by experience, observing patients’ breathlessness, passivity, fatigue, even total exhaustion and reduced self-management, that led to reduced work participation, financial worries, and constraints on family and social life. Families’ ways of motivating patients towards self-management involved increased practical help, assisting with management of medication and, as time passed, adjusting participation in family and social life. Family members felt helpless in face of patients’ lack of energy to work, their giving up on life, but also frustrated, knowing they were even still sneaking out to smoke. This made the family members depressed, trying to be nice, but sometimes turning to tough love, saying “you can’t just think of yourself, you have a family” (Wife/P3).
Guilt, Shame and Blame
The family members experienced guilt, frustration and shame, due to patients’ smoking relapses and for failing to support them towards abstinence. Observing patients’ lack of stamina and reluctance to seek help made them irritated, and as one stated: “It’s far from good” [being a principal family member of a person that is addicted to smoking] (Daughter/P6), and another said: “This is kind of a surrender on his part, I think he never gave [PR] a chance” (Wife/P4).
Participants described how some patients tried to hide their COPD symptoms, and even the oxygen equipment they need.
She had this oxygen-concentrator [...] and cylinders, but her problem was that she was always hiding them [...]. If someone rang the doorbell, she rushed to get rid of the oxygen pipes, putting them away and shutting the door on them [...]. She wanted this [COPD] to be top secret, no one was to know. (Husband/P5)
Some participants also labelled COPD a shameful disease themselves, as described by a wife who had joined a support group for COPD patients’ families during PR:
Most of them sat there silent, definitely not willing to talk about their family member’s shameful disease. I want to declare that this disease provokes shame. The patient is unwilling to discuss it, he hides away, and [...] people make a fuss and say what, has he been smoking? And then of course I take the stance of defending him. (Wife/P9)
Experienced Restraints, Anxiety and Frustration
Gradually, the world of COPD patients and families shrunk, causing restraints in terms of keeping up with the grandchildren, visiting friends or travelling.
But some things that we so much wanted to do, like going hiking, taking the kids [...] showing them things [...] had to end. I didn’t have the heart to let him experience being put aside, [...] that we would go and leave him behind, alone. I wanted us to do things together. (Wife/P9)
Adjusting their pace made the families feel co-dependent, sometimes awkwardly telling white lies to “help” the patient, but still maintaining a clear focus on healthy lifestyle as recommended by HPs.
The summers were, very nice. We used to take the children to a cottage [...]. And, I had to take the load off him because he was unable to do many things. I remember him sometimes being totally exhausted. (Wife/P9)
Many participants could pinpoint their first terrifying experience of the patient’s acute COPD exacerbation:
He was 41 years old when he had pneumonia, ended in the ICU [...] He nearly died there, and after that he stopped smoking. (Wife/P9)
Observing the patient’s fear in face of breathing trouble and debilitating disease, the participants experienced insecurity, anxiety and: “fearing the uncertain future” (Daughter/P8). Fearing COPD as a progressive disease was expressed as
tiptoeing around the subject of illness – hush, hush – trying to be ready for something that might happen. (Daughter/P10)
Families tried to find an applicable approach to care for and motivate the patients while observing increased symptoms and not knowing how to help, which could lead to frustration and anxiety.
I was always asking what I should do. You don’t know how to respond when he has this labored breathing. (Wife/P4)
Need for More Knowledge and Patient–Family–HP’s Teamwork
Several participants mentioned the importance of being well informed about the disease. Some families lacked baseline knowledge about COPD and how to motivate patients towards self-management. Interdisciplinary PR, with specialized lung physicians, nurses and physical therapists, resulted in families’ increased knowledge and a sense of security. Families observed positive changes in patients who participated in PR, and in connection with PR the patients could invite them to group education with other families, but no personal questions were encouraged.
When you are diagnosed with COPD [...] you should receive an education with the family, because when you have teenagers and children, they need to be informed. (Wife/P9)
Family members facilitated re-evaluation of the patients’ medical therapy, contacting HPs regarding exacerbations of COPD, discussion of available therapeutic equipment or even medical tests. Even here, the need for more knowledge was evident.
If we had known better, we might not have let her wait [for a portable oxygen concentrator (POC)] but bought her one right away. Observing this difference, to have a POC, was unbelievable for me as a caregiver, because she was totally helpless with this oxygen-tank, totally locked-up [...]. Having proper equipment gave her quite a new life. (Daughter/P10)
Being invited to participate in COPD patients’ medical consultations gave participants a feeling of being regarded as important. Most often family members were welcome with the patients, but sometimes HPs were reluctant to respond to families’ concerns, such as thoughts about patients’ medical therapy.
He was repeatedly admitted to the emergency department [...] treated with steroid drugs and aerosol, discharged with several tablets to take home. After finishing the tablets, another acute exacerbation and, admission to the acute department. One week he was admitted twice [...]. They [HPs] ignored me initially. Then a nurse at the hospital arranged for the medical treatment to be customized. (Daughter/P6)
Some families wished for enhanced general healthcare follow-up for COPD patients at home, such as “suggesting patient support groups or offering to book the first time in smoking cessation therapy” (Daughter/P8). Re-evaluated medical therapy could lead to fewer acute exacerbations. Many participants mentioned how a professional follow-up reduced the uncertainty involved in the patient’s unstable health, never knowing how the next part of the day will be.
Having a contact person within the healthcare system gave families a sense of security. Knowing HPs meant being known by name and being allowed to make contact in case of emergency.
My sister found a lung specialist for him and now he is seeing him regularly. (Son/P7)
She [nurse] organizes the next appointment before he leaves [the office], making sure he knows the plan. He has her direct number and can call her if he gets worse or if he has some questions. This connection [feels] like a safety net. (Daughter/P6)
HPs did, however, not always invite family involvement.
I never experienced any action plan. Not that I was aware of at least, because I was not informed about how this [COPD] could evolve. Because they [HPs] were somehow always focusing on the present. (Wife/P9)
Advanced Phase: Patient Self-Management Decreases
The advanced phase was characterized by families’ fear of exacerbation of the patient’s illness, anxiety because of the unpredictable disease, uncertain future, and sometimes patients’ persistent smoking. Many family members voiced reasons for avoiding discussion of the illness: on one hand fear and anxiety in view of their awareness of the harm of smoking; and on the other, reluctance to become co-dependent regarding patients’ chronic disease.
COPD - A Progressive, Life-Threatening Disease
Some participants were burdened by the responsibility of supervision of their parents with advanced COPD who were alone at home: dropping in for a check early in the morning and in the afternoon, always being available by telephone, or to sleep overnight if needed.
I think about it, when she was having these severe coughs. What if she’s home alone? (Daughter/P10)
While coping with the progressing effects of COPD on their daily life, many families avoided thinking of the disease as fatal, as the patients regarded themselves as healthy between acute exacerbations.
For a long time, she managed to go out, if she was careful, like going to the mall, resting her shoulders on every rail, waiting to catch her breath. (Husband/P5)
However, some families needed answers:
I would rather [have a family meeting] without my mother attending, I would prefer she [mother] had another chance of such meeting with us. Because I want to be able to ask [...] difficult questions [...] about the progression of the disease. (Daughter/P10)
In the advanced phase, the families shouldered an increased caring burden to facilitate patients’ self-management:
There was always something, he was getting ill and stayed at home in bed, did not take any action and refused to contact a doctor. Then I took control and said, I’ve got time off from work, and we are going to see the doctor because this can’t go on like this [...] he said no, no. I will recover. I said, now you need to call [...]. Yes, he said. I will do that tomorrow, perhaps. (Wife/P9)
Then, I somehow take control. Because when the doctors and nurses are telling him things, he doesn’t remember or can’t even make sense of what they are saying. So, he takes me with him. (Daughter/P6)
Complicated Feelings
Family members needed to assume the role of a coordinator and take over from the patient regarding additional self-management and family duties. This involvement could deplete them of energy and make them depressed, especially when at the same time they were observing patients’ unhelpful coping strategies, such as smoking relapses or alcohol consumption.
On top of it all he smokes, and he’s using inhalation drugs. Ah, he has also this breathing machine [CPAP] which he uses regularly. But then he started drinking [alcohol], and drinking is not good [...]. Why is there nothing that can overcome his disease? It must be something deep inside [...] something uncontrollable. But I can’t see anything that would be helpful for me. This makes me depressed, becomes a burden for me [...]. It bothers me endlessly when he begins this strenuous breathing. (Wife/P4)
The family members expressed their pity and sad feelings for patients suffering a debilitating disease, leaning forward to struggle for breath in constant exhaustion.
He can’t do anything, that he wants to [...]. It makes him so irritated. (Daughter/P6)
[COPD] is [sadly] in my mind just, a slow way of dying. At such a relatively young age, 68 years – this is of course a self-inflicted suffering [...] having worked hard all her life [...] and finally, when she can retire, her health is gone. (Daughter/P10)
Discussion
Being a principal family member of a COPD patient was characterized by frustrated caring; wanting the best for the spouse or parent and yet carrying a heavier burden than participants felt equipped for, lacking both knowledge about the progress of the disease, and information about available healthcare resources. Three sequential and sometimes fluctuating phases were identified in family members’ experience: early, intermediary and advanced phase (Figure 3). We also identified families’ perspectives on COPD patients’ needs (Table 3) and patient–family–HP teamwork (Table 4).
In the early phase patients self-managed, were addicted to smoking, but reluctant to consult a doctor for signs of respiratory problems. From the viewpoint of participants, any consulted doctor has an excellent opportunity to encourage smoking cessation by educating smokers that their smoking can cause serious diseases, which affect the whole family and may lead to invalidity and death.
In the intermediary phase, the patients self-managed with help from family members. Patients’ signs of breathlessness were observed by family members and experienced as frightening and demoralizing, in light of patients’ smoking relapses, leaving the participants helpless and frustrated, as also described in other studies.1,24 Family members called for a formal contact HP, and a construction of a patient–family–HP team. The need for such a team became more prominent along patients’ disease trajectory, e.g. to ensure timely interventions in exacerbations, as mentioned in another study.11
The families in the intermediary phase adjusted their own social participation to the patient, tended to avoid discussing the illness, and some described patients’ gradually declining health like witnessing a slow death. Some felt guilty about patients’ COPD diagnosis, having even participated in smoking, but understood, however, that COPD was a reason to stop smoking.
Results revealed that patients’ breathlessness and exhaustion lead to their inactivity and shrinking lifeworld, greatly affecting their families as well. Observing patients’ acute exacerbation for the first time was a terrifying experience, and made the families feel helpless and scared, which is in line with other studies.11,30 Current study, however, identified the first observation of an acute exacerbation as a turning point, requiring the involvement of HPs, offering an educational opportunity, where HPs could invite the patient to include a principal family member in a patient–HP team. The patient’s will in this matter must be explored, and if the patient does not want a principal family member involvement, that must be respected; this is, however, an ethical issue that must be studied further as mentioned elsewhere.13 The results agree with others that families of COPD patients are often in a constant state of alertness and stress, with their social life modified, striving to maintain normalcy, while experiencing ambivalence in the relationship as their role changes from being a spouse or son/daughter into becoming a caregiver, but still willing to be involved.10,24 Facilitating families’ and patients’ understanding that COPD may in the future severely impair the patient’s self-management, is important.24 Ensuring families’ early understanding of the COPD trajectory might be enhanced by means of a teamwork–oriented attention to patients’ and family members’ concerns (Table 4) and needs special attention in patient/family education material, as previously suggested.30,31 Principal family members had, in the advanced phase, shouldered a substantial caring burden while the patient struggled to self-manage. Families’ unique position as a first-line help in patients’ acute exacerbations, made them call for HPs to explore the family’s insight into the COPD patients’ needs, the perceived roles of family members and their main frustrations (Table 3). The family members also expressed their need for patients’ advance care planning, as increasingly recommended by other researchers.9,32–34
Strengths of the study include that the research team is interprofessional and a mixture of experienced clinicians. The first author is an experienced rehabilitation nursing specialist and we have two professors and one associate professor. The two physicians are PhD pulmonary specialists, we have one professor who is specialized in qualitative methodology, and one specialist in pulmonary physiotherapy.
As the research subject is self-management of COPD patients we regard it as a strength to inform the study by asking the patients’ principal carers. We can identify it as a weakness that a patient who points out interviewees may act as a gatekeeper, however, the patient is the only person who can identify whom he/she relies on to facilitate his/her coping. Participants in this study were found through patients on a waiting list for PR and have thus already been introduced to the idea of rehabilitation, which may make them different from COPD patients’ principal carers who have never heard of PR. Qualitative studies are not constructed to generalize but can, however, inform where services could be improved.
Conclusion
We identified three phases in COPD patients’ gradually increasing need for external help from families and HPs, in order to be able to self-manage. Family members in this study were frustrated and called for a structured team orientation whereby HPs can evaluate the families’ need for early education on effective response to different manifestations of COPD. The family members wanted to urge HPs to seize the educational opportunities in different phases of patients’ COPD and their families’ caregiving burden, motivating the patients to involve a principal family member in his/her patient–self–management team.
Disclosure
The authors report no conflicts of interest for this work.
References
1. Nakken N, Janssen DJ, van den Bogaart EH, et al. Informal caregivers of patients with COPD: home sweet home? Eur Respir Rev. 2015;24(137):498–504. doi:10.1183/16000617.00010114
2. Sigurgeirsdottir J, Halldorsdottir S, Arnardottir RH, Gudmundsson G, Bjornsson EH. COPD patients’ experiences, self-reported needs, and needs-driven strategies to cope with self-management. Int J Chronic Obstr. 2019;14:1033–1043.
3. Mc Veigh C, Reid J, Larkin P, Porter S, Hudson P. The experience of palliative care service provision for people with non-malignant respiratory disease and their family carers: an all-Ireland qualitative study. J Adv Nurs. 2018;74(2):383–394. doi:10.1111/jan.13453
4. Aasbo G, Solbraekke KN, Kristvik E, Werner A. Between disruption and continuity: challenges in maintaining the ‘biographical we’ when caring for a partner with a severe, chronic illness. Sociol Health Ill. 2016;38(5):782–796. doi:10.1111/1467-9566.12396
5. Farquhar M, Penfold C, Benson J, et al. Six key topics informal carers of patients with breathlessness in advanced disease want to learn about and why: MRC phase I study to inform an educational intervention. PLoS One. 2017;12(5):e0177081. doi:10.1371/journal.pone.0177081
6. Knowles S, Combs R, Kirk S, Griffiths M, Patel N, Sanders C. Hidden caring, hidden carers? Exploring the experience of carers for people with long-term conditions. Health Soc Care Comm. 2016;24(2):203–213. doi:10.1111/hsc.12207
7. Lindqvist G, Heikkila K, Albin B, Hjelm K. Conceptions of daily life in men living with a woman suffering from chronic obstructive pulmonary disease. Prim Health Care Res. 2013;14(2):140–150. doi:10.1017/S1463423612000394
8. Hynes G, Stokes A, McCarron M. Informal care-giving in advanced chronic obstructive pulmonary disease: lay knowledge and experience. J Clin Nurs. 2012;21(7–8):1068–1077.
9. Caress A, Luker K, Chalmers K, Salmon M. A review of the information and support needs of family carers of patients with chronic obstructive pulmonary disease. J Clin Nurs. 2009;18(4):479–491. doi:10.1111/j.1365-2702.2008.02556.x
10. Bove DG, Zakrisson AB, Midtgaard J, Lomborg K, Overgaard D. Undefined and unpredictable responsibility: a focus group study of the experiences of informal caregiver spouses of patients with severe COPD. J Clin Nurs. 2016;25(3–4):483–493. doi:10.1111/jocn.13076
11. Bryant J, Mansfield E, Boyes AW, Waller A, Sanson-Fisher R, Regan T. Involvement of informal caregivers in supporting patients with COPD: a review of intervention studies. Int J Chronic Obstr. 2016;11:1587–1596.
12. Aloweni F, Doshi K, Fook-Chong S, Malhotra R, Ostbye T. The types of caregiving reactions experienced by the older spouse caregivers. J Clin Nurs. 2019;28(23–24):4538–4548. doi:10.1111/jocn.15044
13. Jonsdottir H, Ingadottir TS. Reluctance of patients with chronic obstructive pulmonary disease in its early stages and their families to participate in a partnership-based self-management trial: a search for explanation. Chron Respir Dis. 2018;15(3):315–322. doi:10.1177/1479972317743758
14. Whitehead L, Jacob E, Towell A, Abu-Qamar M, Cole-Heath A. The role of the family in supporting the self-management of chronic conditions: a qualitative systematic review. J Clin Nurs. 2018;27(1–2):22–30. doi:10.1111/jocn.13775
15. Effing TW, Vercoulen JH, Bourbeau J, et al. Definition of a COPD self-management intervention: international expert group consensus. Eur Respir J. 2016;48(1):46–54. doi:10.1183/13993003.00025-2016
16. Stacey D, Hill S, McCaffery K, Boland L, Lewis KB, Horvat L. Shared decision making interventions: theoretical and empirical evidence with implications for health literacy. St Health. 2017;240:263–283.
17. Micklewright K, Farquhar M. Does the carer support needs assessment tool cover the established support needs of carers of patients with chronic obstructive pulmonary disease? A systematic literature search and narrative review. Palliat Med. 2020;269216320939243.
18. Farquhar M, Penfold C, Walter FM, Kuhn I, Benson J. What are the key elements of educational interventions for lay carers of patients with advanced disease? A systematic literature search and narrative review of structural components, processes and modes of delivery. J Pain Symptom Manag. 2016;52(1):117–130.e127. doi:10.1016/j.jpainsymman.2015.12.341
19. Kara M, Mirici A. Loneliness, depression, and social support of Turkish patients with chronic obstructive pulmonary disease and their spouses. J Nurs Scholarship. 2004;36(4):331–336. doi:10.1111/j.1547-5069.2004.04060.x
20. Mi E, Mi E, Ewing G, et al. Do patients and carers agree on symptom burden in advanced COPD? Int J Chronic Obstr. 2018;13:969–977.
21. Miravitlles M, Pena-Longobardo LM, Oliva-Moreno J, Hidalgo-Vega A. Caregivers’ burden in patients with COPD. Int J Chronic Obstr. 2015;10:347–356.
22. Mansfield E, Bryant J, Regan T, Waller A, Boyes A, Sanson-Fisher R. Burden and unmet needs of caregivers of chronic obstructive pulmonary disease patients: a systematic review of the volume and focus of research output. COPD. 2016;13(5):662–667. doi:10.3109/15412555.2016.1151488
23. Ates G, Ebenau A, Busa C, et al. “Never at ease” - family carers within integrated palliative care: a multinational, mixed method study. BMC Palliat Care. 2018;17(1):39. doi:10.1186/s12904-018-0291-7
24. Pinnock H, Kendall M, Murray SA, et al. Living and dying with severe chronic obstructive pulmonary disease: multi-perspective longitudinal qualitative study. BMJ. 2011;342:d142. doi:10.1136/bmj.d142
25. Spiegelberg H. The Phenomenological Movement: A Historical Introduction by Herbert Spiegelberg.
26. Ricoeur P. Existence and hermeneutics. In: Bleicher J, editor. Contemporary Hermeneutics: Hermeneutics as Method, Philosophy and Critique. London: Routledge & Kegan Paul; 1980.
27. Schwandt T. Constructivist, interpretivist approaches to human inquiry. In: Denzin N, Lincoln Y, editors. Handbook of Qualitative Research. Thousand Oaks CA: Sage; 1994.
28. Ricoeur P. Hermeneutics and the Human Sciences: Essays on Language, Action and Interpretation. Cambridge: Cambridge University Press; 1990.
29. Halldorsdottir S. The Vancouver school of doing phenomenology. In: Fridlund B, Haldingh C, editors. Qualitative Research Methods in the Service of Health. Lund: Studentlitteratur; 2000:46–81.
30. Gysels MH, Higginson IJ. Caring for a person in advanced illness and suffering from breathlessness at home: threats and resources. Palliat Support Care. 2009;7(2):153–162. doi:10.1017/S1478951509000200
31. Andersen IC, Thomsen TG, Bruun P, Bodtger U, Hounsgaard L. Between hope and hopelessness: COPD patients’ and their family members’ experiences of interacting with healthcare providers - a qualitative longitudinal study. Scand J Caring Sci. 2018;32(3):1197–1206. doi:10.1111/scs.12565
32. Jowsey T, Strazdins L, Yen L. Worry and time: the unseen costs of informal care. Chronic Illn. 2016;12(4):249–260. doi:10.1177/1742395316647788
33. Pena-Longobardo L, Oliva-Moreno J, Hidalgo-Vega A, Miravitlles M. Economic valuation and determinants of informal care to disabled people with Chronic Obstructive Pulmonary Disease (COPD). BMC Health Serv Res. 2015;15:101.
34. Stefanacci R, Riddle A. Caring for caregivers. Geriatr Nurs. 2019;40(2):214–216. doi:10.1016/j.gerinurse.2019.03.003
35. Vogelmeier CF, Criner GJ, Martinez FJ, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 report. GOLD executive summary. Am J Respir Crit Care Med. 2017;195(5):557–582. doi:10.1164/rccm.201701-0150WS.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
