Back to Journals » OncoTargets and Therapy » Volume 13
Fibroblast Activation Protein-α Expressing Fibroblasts Promote Lymph Node Metastasis in Esophageal Squamous Cell Carcinoma
Authors Li F, Wu X , Sun Z, Cai P , Wu L, Li D
Received 15 April 2020
Accepted for publication 26 July 2020
Published 14 August 2020 Volume 2020:13 Pages 8141—8148
DOI https://doi.org/10.2147/OTT.S257529
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Sanjay Singh
Video abstract of "FAP-α expression promotes lymph node metastasis in ESCC" [ID 257529].
Views: 262
Feng Li,1,* Xia Wu,2,* Zhixiang Sun,3,* Peng Cai,1 Ligao Wu,2 Duojie Li1
1Department of Radiotherapy, First Affiliated Hospital of Bengbu Medical College, Bengbu 233000, People’s Republic of China; 2Department of Pathology, First Affiliated Hospital of Bengbu Medical College, Bengbu 233000, People’s Republic of China; 3Department of Neurosurgery, First Affiliated Hospital of Bengbu Medical College, Bengbu 233000, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Ligao Wu; Duojie Li Email [email protected]; [email protected]
Background and Objectives: Esophageal squamous cell carcinoma (ESCC) remains one of the most common malignancies in China and has a high metastasis rate and poor prognosis. Fibroblast activation protein-α (FAP-α) is a serine peptidase the expression of which in cancer-associated fibroblasts has been associated with a higher risk of metastases and poor survival. This study aimed to analyze the correlation of FAP-α expression with the lymph node metastasis and prognostic significance in ESCC.
Methods: FAP-α expression was examined in 121 resected ESCC specimens and 10 adjacent normal tissue using immunohistochemistry. FAP-α expression was scored in the stromal fibroblasts adjacent to neoplastic nests. A chi-square test was used to analyze the correlation between FAP-α expression in tumors stromal and lymph node metastasis of ESCC. The association between FAP-α expression and prognosis was evaluated using univariable and multivariable statistical modeling.
Results: FAP-α expression was absent in the benign controls. FAP-α expression was evident in the stromal 37% (45/121) of ESCC. Expression of FAP-α level is significantly associated with lymph node metastasis (p=0.023), but it is not correlated to age, gender, and tumor location in ESCC patients. Stromal FAP-α expression was significantly associated with poor survival in univariable (HR 2.009; 95% CI 1.259– 3.205; p=0.003) and multivariable analysis (HR 1.833; 95% CI 1.144– 2.937; p=0.012).
Conclusion: FAP-α may be an important regulator in lymph node metastasis of ESCC and may provide a novel therapeutic target in ESCC.
Keywords: esophageal squamous cell carcinoma, fibroblast activation protein-α, lymph node metastasis, prognosis, overall survival
Introduction
Esophageal cancer is one of the most common malignant tumors in humans, with the mortality ranking the 6th in the world.1 Squamous cell cancer is the most common histological subtype, accounting for approximately 95% of esophageal carcinoma cases in east Asian countries such as China and Japan.2 The 5-year overall survival rate is about 18%, with the poor prognosis for esophageal cancer.3 The high mortality is closely related to tumor invasion and metastasis. Lymph node metastasis (LNM) is the most common way of esophageal cancer metastasis, and it is also an important factor in evaluating the prognosis of esophageal cancer patients.4 Surgery is a cornerstone of the curatively intended treatment, and the selection of surgical methods for esophageal cancer or determining the extent of lymphadenectomy depends largely on whether the tumor is associated with LNM or not.5,6 Hence accurate identification of LNM status plays a crucial role in determining treatment strategies as well as prognostic outcomes. There is an urgent need to identify novel biomarkers that can help to select patients with a high risk of lymph node metastasis in esophageal squamous cell carcinoma. Such biomarkers could provide clinical clues that can be used for the individualization of treatment.
Tumor cells are disseminated throughout the body via the bloodstream, but only in the congenial microenvironment can metastases develop.7 Cancer-associated fibroblasts (CAFs) are one of the most common tumor stromal cells in the tumor microenvironment. By secreting cytokines, growth factors, chemokines, and extracellular matrix-degrading enzymes, it promotes inflammatory pathways, disrupts immune surveillance, rebuilds extracellular matrix, forms tumor niche, and promotes the growth and metastasis of tumor cells.8,9 FAP-α is an important surface marker of CAFs and belongs to the family of prolyl-specific serine proteases.10 It has been demonstrated to have pro-tumorigenic activity, and highly upregulated in a wide variety of cancers, but not detected in normal adult tissues.11 FAP-α was shown to predict survival, for example, high FAP-α being a marker for poor survival in oral squamous cell carcinoma, gastric cancer, and pancreatic ductal adenocarcinoma.12–14 Subsequently, another study investigated the role of epithelial FAP-α in distal cholangiocarcinoma and found that positive of this marker protein correlates with better survival.15
However, the relationship between FAP-α expression and lymph node metastasis and prognosis of esophageal squamous cell carcinoma remains unclear. This study aimed to assess the relation of stromal FAP-α expression to lymph node metastasis and overall survival in patients with ESCC.
Materials and Methods
The study was approved by the Research Ethics Committee of Bengbu Medical College. The need for informed consent was waived by the Research Ethics Committee because the study was retrospective and some patients had already been dead. Under the Declaration of Helsinki, patient data was maintained with confidentiality.
Operated Esophageal Specimens
All patients had undergone surgical resection for ESCC at First Affiliated Hospital of Bengbu Medical College from 2012 to 2016. For this study, the following criteria were required for inclusion: surgery with the radical operation, histopathologically confirmed ESCC, the pathological stage was T3N0–3M0, the degree of differentiation was G2, no history of neoadjuvant treatment, no early (30-d) postoperative mortality, complete clinical information, complete follow-up information, formalin-fixed paraffin-embedded tissue from primary resection available in the archives at the Department of Pathology, First Affiliated Hospital of Bengbu Medical College. Ten resected noncancerous esophageal specimens were obtained from the same batch of ESCC patients as controls. Tumor staging was based on the American Joint Committee on Cancer eighth edition. Follow-up data were obtained from clinical records and telephone interviews. Survival time was defined as the interval between time from surgery and death or the last visit to the outpatient clinic up to October 31, 2019.
Reagent
The neutralizing antibodies were as follows: Anti-fibroblast activation protein, alpha-antibody ab53066 was supplied from Abcam. Immunochromogenic reagent (EliVision plus rat/rabbit) was purchased from Fuzhou Maixin biotechnology development Co. LTD.
Immunohistochemistry
Fibroblast activating protein-α in ESCC tissue sections was stained with Ab53066 by immunohistochemistry. It was fixed with a 4% formalin solution, embedded in paraffin, sliced to 4um thickness continuously, baked slices, dewaxed in the corresponding solution and washed, and reduced the antigen in the buffer by heat-mediated. The samples were incubated with the primary antibody (1/50 in antibody dilution) at 21 °C for 30 minutes. Undiluted HRP-conjugated goat anti-rabbit IgG polyclonal antibody was used as the secondary antibody. The specific operation steps are carried out according to the kit instructions.
Evaluation of Immunoreactivity
Assessment of immunohistochemical staining was evaluated by two independent pathologists who were blinded to the clinicopathological parameters and clinical outcomes of the patients. The presence/absence of FAP-α was evaluated in the stromal fibroblasts adjacent to neoplastic nests. The number of FAP-α positive‐staining cells showing immunoreactivity in 5 microscopic fields (100 such cells for every 400×high-power visual field) was counted and the percentage of positive cells was calculated. The percentage scoring of immunoreactive tumor cells was as follows: 0 (0–5%), 1 (6–25%), 2 (26–50%), 3 (51–75%), and 4 (>75%). The staining intensity was visually scored and stratified as follows: 0 (negative), 1 (weak), 2(moderate), and 3 (strong). A final immunoreactivity score (IRS) was obtained for each case by multiplying the percentage and the intensity score. 0 was negative (-), 1–4 was weakly positive (+), 5–8 was moderate positive (++), and 9–12 was strongly positive (+++). The moderate positive and strong positive was used to define the high expression group and negative and weak positive was used to define low expression group.
Statistical Analysis
The software of SPSS version 23.0 for Windows was used for statistical analysis. Values are given as mean ± standard deviation. Chi-square test or Fisher’s exact test when appropriate for categorical variables. Patient survival and their differences were determined by Kaplan–Meier curves and Log rank tests. A Variable selection of covariables was performed using a forward elimination procedure (removal limit p<1). Variables considered as covariables were age, gender, tumor location, lymph node metastasis, chi-square test was used to analyze the correlation between FAP-α expression in tumors stromal, and lymph node metastasis of ESCC. Patient survival and their differences were determined by Kaplan–Meier curves and Log rank tests. Cox regression (proportional hazard model) was adopted for the multivariate analysis of prognostic factors. All tests were two-sided and a p-value of less than 0.05 was considered to be significant.
Results
Patient Characteristics
A total of 121 patients were included in the study. Until follow-up time, 73 patients (64%) had died of the disease. The median follow-up time was 49 months with a range between 2 and 91 months. Clinical and pathological data of the selected samples are summarized in (Table 1). Males predominated in the series (The cohort consisted of 95 males and 26 females). The age span ranged from 40 to 78 years with a mean age was 64±7.9years. All cases were middle differentiation (G2) and locally advanced (pT3N0–3 M0). None of the patients underwent preoperative chemotherapy, but 53 (43.8%) patients underwent postoperative chemotherapy or (and) radiotherapy. The median survival was 28 months.
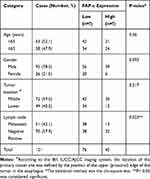 |
Table 1 Association of FAP-α Expression with Clinicopathological Factors in 121 ESCC Patients |
FAP-α Expression in ESCC Tissues
To understand the overall FAP-α expression in ESCC, 121resected ESCC specimens, and 10 adjacent normal tissue were analyzed by immunohistochemistry. The results demonstrated that no FAP-α expression was detected in adjacent normal tissue in resected ESCC tissues (Figure 1A). However, the expression of FAP-α was found predominantly in stromal cells and slightly in cancer cells in resected ESCC tissues. In the present study, we focused on stromal FAP-α expression in terms of the effect of stromal FAP-α expression on lymph node metastasis in esophageal squamous cell carcinoma. Stromal FAP-α expression was detected in 82.6% (100/121) of the specimens of ESCC, with the intensity being weak in 55 (Figure 1B), moderate in 40 (Figure 1C), and strong in 5 specimens (Figure 1D). In 17.4% (21/121) samples, FAP expression was negative (Figure 1E). The stromal FAP-α expression was classified as high in 45 (37.2%) and low in 76 (62.8%).
Association of FAP-α and Clinicopathologic Variables
A chi-square test revealed that high expression of FAP-α was significantly correlated with lymph node status. To analyze the correlation between FAP expression and the degree of lymph node metastasis, we obtained Spearman’s rho of 0.152 and P-value of 0.208 by Spearman’s rank correlation coefficients which showed that the correlation coefficient was not statistically significant and FAP expression was not correlated with the degree of lymph node metastasis. There was no statistically significant difference between high and low FAP-α expression in stromal concerning age, gender, tumor location (Table 1).
FAP-α Expression and Association with Survival
The correlation of FAP-α expression and survival was determined using a Cox proportional hazards model. Analyses by univariate Cox regression showed that among different clinicopathological variables, FAP-α expression and lymph node status were significant prognostic factors for 5-year overall survival and disease-free survival for ESCC (Table 2). Multivariate cox regression analyses showed that lymph node metastases and high expression of FAP-α remained independent prognostic factors for survival (Table 3). Compared with the FAP-α low expression group, the FAP-α high expression group has a higher risk of death with the hazard ratio (HR) was 1.833 (95% confidence interval (CI) 1.144 to 2.937; p=0.012). Lymph node metastasis was found to have an even higher predictive value for survival according to Cox regression analyses with the HR was 2.471 (95% CI 1.476 to 4.136; p=0.001).
 |
Table 2 Univariate Analysis of Risk Factors for Prognosis of 121 ESCC Patients |
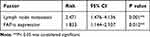 |
Table 3 Multivariate Cox Regression Analysis of Clinicopathological Factors for Risk Prediction in 121 ESCC Patients |
Kaplan–Meier analysis with associated Log rank test showed that the overall survival and disease-free survival of patients with FAP-α high expression group were significantly lower than that of FAP-α low expression group (mean survival time, 26.5 vs. 52.9 months, P =0.002) (Figure 2A and B). In the lymph node cancer-free case, stromal FAP-α expression is not a prognostic factor for overall survival and disease-free survival (Figure 2C and D). However, stromal FAP-α high expression as significant factors associated with poor overall survival and disease-free survival in lymph node metastasis group (Figure 2E and F).
Discussion
Esophageal cancer frequently shows a high degree of invasiveness and is associated with a high rate of lymph node metastasis. Lymphadenectomy includes a traditional two-field, improved two-field, and three-field lymph node dissection. Radiation therapy includes involved-field irradiation and Elective nodal irradiation. However, three-field lymph-node dissection or elective nodal irradiation had not improved the prognosis.16,17 Patients with esophageal squamous cell carcinoma still have a poor prognosis. There are no reasonable criteria for selecting patients who will benefit from more radical treatments. Continuous exploration of biomarkers that can predict lymph node metastasis and prognosis of esophageal cancer is a priority for medical researchers.
FAP-α is expressed in the reactive CAFs has been recognized as highly responsible for cancer growth and metastasis. FAP-α is a homodimer type II integral membrane prolyl-specific serine protease belonging to the dipeptidyl peptidase (DPP) family.18 The human FAP-α gene is located at 2q23 of chromosome 2 and encodes FAP-α.19 FAP-α features an eight-bladed β-propeller domain and an α/β hydrolase domain which characterized by the catalytic site sequence glycine-tryptophan-serine-tyrosine-glycine.20 FAP-α is most closely related to DPP IV, displaying around 50% homology in sequence and a 70% similarity in the catalytic region.21
FAP-α has post-proline exopeptidase activity and gelatinase activity that regulates tumor growth and invasiveness through mechanisms that are dependent and independent of its catalytic activity.22 For example, FAP-α may form a heterodimer complex with its homologous enzyme DPPIV, which allows fibroblasts to migrate and promotes the degradation of extracellular matrix (ECM), thereby promoting cancer cell invasion.20 FAP-α regulates tumor growth and invasiveness through increasing angiogenesis and by reducing the antitumor response of the immune system mediated by the signal transducer and activator of transcription 3 (STAT3)/C-C motif chemokine ligand 2 (CCL2) signaling pathway.23 FAP-α can mediate tumorigenic cell behaviors through phosphatase and tensin homolog (PTEN)/FAP-α signaling pathway.13 FAP-α has a role in cell–ECM interactions through classical integrin-signaling pathways and promotes adhesion and migration.24 At present, the mechanism of FAP-α promoting lymph node metastasis has not been revealed yet. Lymphatic metastasis occurs by permeation of tumor cells into intratumourous lymphatics, and subsequently reaching proximate lymph nodes, a process crucially depending on lymphangiogenesis. Chen et al demonstrated a positive association between FAP-α expression and lymphatic vessel density in squamous cell carcinoma of the lung.25 Cheng et al demonstrated that CAFs density in ESCC correlated significantly with increased tumoral lymphatic vessel density.26 VEGF-C and VEGF-D were also shown to be associated with tumor lymphangiogenesis and lymph node metastasis.27 Since CAFs could release VEGF to stimulate the formation of a vascular network, CAFs may induce lymphangiogenesis via the same mechanisms, then facilitate the dissemination of tumor cells into lymph nodes.
There are indications that high FAP-α expression is associated with higher tumor grade and poorer overall survival rate in most tumors. A meta-analysis including 9 kinds of solid tumors reported that high FAP-α expression is related to poor overall survival.11 In oral squamous cell carcinoma, high FAP-α expression correlated to lymph node metastasis and poor overall survival.13 In gastric cancer, high stromal FAP-α expression was reported to correlate with adverse clinic-pathological characteristics including higher grade, lymph node, and peritoneal invasion, advanced TNM stage, and worse overall survival.20,28 The intensity of stromal FAP-α expression was correlated to the high histological differentiation and reduced survival of pancreatic ductal adenocarcinoma.12 In ovarian cancer, high FAP-α was significantly associated with shorter disease-free survival.29 These results indicate that FAP-α plays a more critical role in disease progression and outcome.
Currently, research on FAP-α in esophageal squamous cell carcinoma is still limited. Higashino et al reported that FAP-α expression in the ESCC stroma is correlated with the depth of tumor invasion, lymph node metastasis, advanced pathological stage, and poor disease-free survival.30 However, Ha et al reported that FAP-α was not a significant prognostic factor for overall and disease-free survival in patients with ESCC.31 The reasons for this discrepancy are as follows:In addition to the differences in measurement methods, the two reports have different proportions of T stages and differentiation degrees, which may lead to different final results. Kashima et al demonstrated that FAP-α positive stromal cells correlate with lymph node metastasis and prognosis in ESCC.32 This conclusion is also consistent with Higashino N’s research.
The purpose of this study was to investigate the relationship between FAP-α expression and lymph node metastasis and prognosis of esophageal squamous cell carcinoma. To eliminate the effects of T stage and differentiation on FAP-α expression, all cases were middle differentiation (G2) and locally advanced (pT3N0–3 M0). Noteworthy, the cohort was not balanced for males and females. However, statistical analyses revealed that FAP-α expression did not depend on gender, and thus, no bias should be introduced. Among all investigated clinicopathological characteristics, the overexpression of FAP-α is significantly associated with a higher rate of lymph node metastasis. The univariate and multivariate analyses showed that among all investigated clinicopathological characteristics, only FAP-α density and lymph node status were potential independent survival predictors of ESCC. FAP-α abundance or lymph node metastasis negatively correlated with overall survival.
In this study, stromal FAP-α expression was evident in a majority of ESCC samples but was absent in adjacent normal tissue. The proportion of samples positive for stromal FAP-α expression was significantly higher in lymph node metastasis (N1–3) as compared to primary tumors (N0), suggesting that FAP-α expressing stroma might be essential during ESCC progression. The findings suggest that FAP-α may potentially be used as a biomarker for selecting treatment strategies.
FAP-α inhibition is often considered a potential therapeutic target for tumor diseases. FAP-α activity is inhibited by general serine-protease inhibitors and boronic acid peptides.33 Boronic acid derivatives are reversible covalent inhibitors of serine proteases, so most FAP-α inhibitors contain boric acid groups. PT-100 (talabostat, linagliptin) is the dual DPP IV/FAP-α inhibitor, which inhibits 90% of DPP IV-like exopeptidase activity, but only 20% of the FAP-α endopeptidase activity.34 PT-100 causes tumor regression in vivo, which involves tumor-specific cytotoxic T lymphocytes and produces cytokines and chemokines that promote T cell effector function.35 The combination of PT-100 and oxaliplatin can reduce tumor growth and improve survival enhance by enhancing the effect of chemotherapy and reducing CAF markers.36 Compared with treatment alone, linagliptin combined with anti-programmed cell death protein 1 was used for treating transplanted tumors of gastric cancer in murine, which improved survival, reduced tumor volume, reduced collagen accumulation and enhanced the ratio of CD8+ T cells to Tregs in tumor and lymph nodes.37 All these results have been encouraging in terms of clinical benefit. Jansen et al discovered that several structural components can produce highly specific FAP-α inhibitors with low toxicity in vivo, which may be good candidates for future preclinical studies.38 In consequence, designing highly specific FAP-α inhibitors is not impossible.
Conclusion
We found FAP-α to be upregulated in stromal of ESCC, as compared to absent in adjacent normal tissue. There was a significantly higher proportion of FAP-α expressing stroma present in lymph node metastasis. However, stromal FAP-α expression was associated with poor prognosis in both univariable and multivariable analyses. Further research is warranted to elucidate the functional role of FAP-α expression in ESCC stromal and validate the prognostic implication of stromal FAP-α expression identified in our cohort.
Acknowledgments
This work was supported by the Natural Science Foundation of Anhui Province (KJ2017A218) and Key Project of Translational Medicine in Bengbu Medical College (BYTM2019027).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin. 2019;69(1):7–34. doi:10.3322/caac.21551
2. Arnold M, Soerjomataram I, Ferlay J, Forman D. Global incidence of oesophageal cancer by histological subtype in 2012. Gut. 2015;64(3):381–387. doi:10.1136/gutjnl-2014-308124
3. Malhotra GK, Yanala U, Ravipati A, Follet M, Vijayakumar M, Are C. Global trends in esophageal cancer. J Surg Oncol. 2017;115(5):564–579. doi:10.1002/jso.24592
4. Wu N, Chen Z, Pang L, Ma Q, Chen G. Prognostic significance of lymph node characteristics on survival in esophageal squamous cell carcinomas. Wien Klin Wochenschr. 2013;125(1–2):26–33. doi:10.1007/s00508-012-0310-2
5. Mariette C, Markar SR, Dabakuyo-Yonli TS, et al. Hybrid minimally invasive esophagectomy for esophageal cancer. N Engl J Med. 2019;380(2):152–162. doi:10.1056/NEJMoa1805101
6. van der Schaaf M, Johar A, Wijnhoven B, Lagergren P, Lagergren J. Extent of lymph node removal during esophageal cancer surgery and survival. J Natl Cancer Inst. 2015;107(5):djv043.
7. Albini A, Bruno A, Gallo C, Pajardi G, Noonan DM, Dallaglio K. Cancer stem cells and the tumor microenvironment: interplay in tumor heterogeneity. Connect Tissue Res. 2015;56(5):414–425. doi:10.3109/03008207.2015.1066780
8. Quail DF, Joyce JA. Microenvironmental regulation of tumor progression and metastasis. Nat Med. 2013;19(11):1423–1437. doi:10.1038/nm.3394
9. Kalluri R, Zeisberg M. Fibroblasts in cancer. Nat Rev Cancer. 2006;6(5):392–401. doi:10.1038/nrc1877
10. Jacob M, Chang L, Puré E. Fibroblast activation protein in remodeling tissues. Curr Mol Med. 2012;12(10):1220–1243. doi:10.2174/156652412803833607
11. Liu F, Qi L, Liu B, et al. Fibroblast activation protein overexpression and clinical implications in solid tumors: a meta-analysis. PLoS One. 2015;10(3):e0116683. doi:10.1371/journal.pone.0116683
12. Kawase T, Yasui Y, Nishina S, et al. Fibroblast activation protein-α-expressing fibroblasts promote the progression of pancreatic ductal adenocarcinoma. BMC Gastroenterol. 2015;2(15):109. doi:10.1186/s12876-015-0340-0
13. Wang H, Wu Q, Liu Z, et al. Downregulation of FAP suppresses cell proliferation and metastasis through PTEN/PI3K/AKT and Ras-ERK signaling in oral squamous cell carcinoma. Cell Death Dis. 2014;10(5):e1155. doi:10.1038/cddis.2014.122
14. Lai D, Ma L, Wang F. Fibroblast activation protein regulates tumor-associated fibroblasts and epithelial ovarian cancer cells. Int J Oncol. 2012;41(2):541–550. doi:10.3892/ijo.2012.1475
15. Byrling J, Sasor A, Nilsson J, Said Hilmersson K, Andersson R, Andersson B. Expression of fibroblast activation protein and the clinicopathological relevance in distal cholangiocarcinoma. Scand J Gastroenterol. 2020;55(1):82–89. doi:10.1080/00365521.2019.1708449
16. Lagergren J, Mattsson F, Zylstra J, et al. Extent of lymphadenectomy and prognosis after esophageal cancer surgery. JAMA Surg. 2016;151(1):32–39. doi:10.1001/jamasurg.2015.2611
17. Li Q, Zhu S, Li S, Deng W. Elective nodal irradiation provides a superior therapeutic modality for lymph node positivity esophageal squamous cell carcinoma patients receiving definitive radiotherapy versus involved-field irradiation. Medicine. 2019;98(3):e14080. doi:10.1097/MD.0000000000014080
18. Goldstein LA, Ghersi G, Piñeiro-Sánchez ML, et al. Molecular cloning of seprase: a serine integral membrane protease from human melanoma. Biochim Biophys Acta. 1997;1361(1):11–19. doi:10.1016/S0925-4439(97)00032-X
19. Mathew S, Mathew S, Scanlan MJ, et al. The gene for fibroblast activation protein α (FAP), a putative cell surface-bound serine protease expressed in cancer stroma and wound healing, maps to chromosome band 2q23. Genomics. 1995;25(1):335–337. doi:10.1016/0888-7543(95)80157-H
20. Wang RF, Zhang LH, Shan LH, et al. Effects of the fibroblast activation protein on the invasion and migration of gastric cancer. Exp Mol Pathol. 2013;95(3):350–356. doi:10.1016/j.yexmp.2013.10.008
21. Scanlan MJ, Raj BK, Calvo B, et al. Molecular cloning of fibroblast activation protein alpha, a member of the serine protease family selectively expressed in stromal fibroblasts of epithelial cancers. Proc Natl Acad Sci USA. 1994;91(12):5657–5661. doi:10.1073/pnas.91.12.5657
22. Park JE, Lenter MC, Zimmermann RN, Garin-Chesa P, Old LJ, Rettig WJ. Fibroblast activation protein, a dual specificity serine protease expressed in reactive human tumor stromal fibroblasts. J Biol Chem. 1999;274(51):36505–36512. doi:10.1074/jbc.274.51.36505
23. Yang X, Lin Y, Shi Y, et al. FAP promotes immunosuppression by cancer-associated fibroblasts in the tumor microenvironment via STAT3-CCL2 signaling. Cancer Res. 2016;76(14):4124–4135. doi:10.1158/0008-5472.CAN-15-2973
24. Baird SK, Allan L, Renner C, Scott FE, Scott AM. Fibroblast activation protein increases metastatic potential of fibrosarcoma line HT1080 through upregulation of integrin-mediated signaling pathways. Clin Exp Metastasis. 2015;32(5):507–516. doi:10.1007/s10585-015-9723-4
25. Chen L, Chen M, Han ZL, et al. Clinical significance of FAP-α on microvessel and lymphatic vessel density in lung squamous cell carcinoma. J Clin Pathol. 2018;71(8):721–728. doi:10.1136/jclinpath-2017-204872
26. Cheng YF, Wang K, Ma W, et al. Cancer-associated fibroblasts are associated with poor prognosis in esophageal squamous cell carcinoma after surgery. Int J Clin Exp Med. 2015;8(2):1896–1903.
27. Krzystek-Korpacka M, Matusiewicz M, Diakowska D, et al. Up-regulation of VEGF-C secreted by cancer cells and not VEGF-A correlates with clinical evaluation of lymph node metastasis in esophageal squamous cell carcinoma (ESCC). Cancer Lett. 2007;249(2):171–177. doi:10.1016/j.canlet.2006.08.011
28. Liu J, Huang C, Peng C, et al. Stromal fibroblast activation protein alpha promotes gastric cancer progression via epithelial-mesenchymal transition through Wnt/ β-catenin pathway. BMC Cancer. 2018;18(1):1099–1108. doi:10.1186/s12885-018-5035-9
29. Zhang M, Xu L, Wang X, Sun B, Ding J. Expression levels of seprase/FAPα and DPPIV/CD26 in epithelial ovarian carcinoma. Oncol Lett. 2015;10(1):34–42. doi:10.3892/ol.2015.3151
30. Higashino N, Koma YI, Hosono M, et al. Fibroblast activation protein-positive fibroblasts promote tumor progression through secretion of CCL2 and interleukin-6 in esophageal squamous cell carcinoma. Lab Invest. 2019;99(6):777–792. doi:10.1038/s41374-018-0185-6
31. Ha SY, Yeo S-Y, Xuan Y-H, Kim S-H, Hoheisel JD. The prognostic significance of cancer-associated fibroblasts in esophageal squamous cell carcinoma. PLoS One. 2014;9(6):e99955. doi:10.1371/journal.pone.0099955
32. Kashima H, Noma K, Ohara T, et al. Cancer-associated fibroblasts (CAFs) promote the lymph node metastasis of esophageal squamous cell carcinoma. Int J Cancer. 2019;144(4):828–840. doi:10.1002/ijc.31953
33. Edosada CY, Quan C, Wiesmann C, et al. Selective inhibition of fibroblast activation protein protease based on dipeptide substrate specificity. J Biol Chem. 2006;281(11):7437–7444. doi:10.1074/jbc.M511112200
34. Narra K, Mullins SR, Lee H-O, et al. Phase II trial of single agent Val-boroPro (talabostat) inhibiting fibroblast activation protein in patients with metastatic colorectal cancer. Cancer Biol Ther. 2007;6(11):1691–1699. doi:10.4161/cbt.6.11.4874
35. Nemunaitis J, Vukelja SJ, Richards D, et al. Phase I trial of PT-100 (PT-100), a cytokine-inducing small molecule, following chemotherapy for solid tumor malignancy. Cancer Invest. 2006;24(6):553–561. doi:10.1080/07357900600894732
36. Li M, Li M, Yin T, et al. Targeting of cancer-associated fibroblasts enhances the efficacy of cancer chemotherapy by regulating the tumor microenvironment. Mol Med Rep. 2016;13(3):2476–2484. doi:10.3892/mmr.2016.4868
37. Wen X, He X, Jiao F, et al. Fibroblast activation protein-α-positive fibroblasts promote gastric cancer progression and resistance to immune checkpoint blockade. Oncol Res. 2017;25(4):629–640. doi:10.3727/096504016X14768383625385
38. Jansen K, Heirbaut L, Verkerk R, et al. Extended structure–activity relationship and pharmacokinetic investigation of (4-quinolinoyl) glycyl-2-cyanopyrrolidine inhibitors of fibroblast activation protein (FAP). J Med Chem. 2014;57(7):3053–3074. doi:10.1021/jm500031w
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


