Back to Journals » International Journal of Chronic Obstructive Pulmonary Disease » Volume 17
Evaluation of a Digital COPD Education Program for Healthcare Professionals in Long-Term Care – A Mixed Methods Study
Authors Nyberg A , Lundell S , Pesola UM , Audulv , Wadell K
Received 16 December 2021
Accepted for publication 28 March 2022
Published 23 April 2022 Volume 2022:17 Pages 905—918
DOI https://doi.org/10.2147/COPD.S353187
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Min Zhang
André Nyberg,1,* Sara Lundell,1,* Ulla-Maija Pesola,1 Åsa Audulv,2 Karin Wadell1,3
1Department of Community Medicine and Rehabilitation, Physiotherapy, Umeå University, Umeå, Sweden; 2Department of Nursing, Umeå University, Umeå, Sweden; 3Department of Public Health and Clinical Medicine, Division of Medicine, Umeå University, Umeå, Sweden
*These authors contributed equally to this work
Correspondence: André Nyberg, Department of Community Medicine and Rehabilitation, Physiotherapy, Umeå University, Umeå, 901 87, Sweden, Tel +46 90 786 66 39, Email [email protected]
Background: Lack of routines and competence among healthcare professionals have been reported as barriers to COPD management in long-term care. Online education could be used as a strategy to make COPD education more accessible.
Purpose: The aim of this study was to evaluate a digital COPD education program for healthcare professionals in long-term care regarding feasibility, knowledge and working procedures.
Methods: A randomized controlled feasibility trial with a convergent mixed methods design was conducted. Two municipalities in Sweden were randomized to intervention (n=20) or control (n=17). The intervention was a digital COPD education program accessible for three months. Data was collected through questionnaires on COPD-specific knowledge, conceptual knowledge, feasibility and usage of the COPD Web platform. Repeated individual interviews using a semi-structured interview guide was also performed. Quantitative and qualitative findings were merged using a mixed methods design.
Results: The digital COPD education program appears feasible based on the expressed satisfaction of the healthcare workers and their reports that it supported them in their work. Across questionnaires, objective COPD-specific knowledge increased by 14 to 16 percentage points in the intervention group compared to 0 to 6 percentage points in the control group (p=0.001). The objective increase in COPD-specific knowledge was also captured in the interviews, where a perceived increase in knowledge led to increased security and focus on COPD management. Few changes in working procedures were expressed, but participants felt that attention was raised regarding COPD and the importance of preventive healthcare services. In addition, increased knowledge of healthcare services provided by other involved professions was emphasized, leading to discussions with other professions in relation to COPD management.
Conclusion: A digital COPD education program is feasible and can increase the COPD-specific knowledge of healthcare professionals in long-term care, leading to increased focus on COPD-related issues. More comprehensive measures, including organizational changes, might be needed to change working procedures.
Keywords: e-health, feasibility, work task, qualitative longitudinal research, questionnaire
Introduction
People with chronic obstructive pulmonary disease (COPD), who are no longer able to live independently, often need long-term care. Such care can be provided in private residential homes or nursing homes.1 Several insufficiencies have however been found in the management of people with COPD in long-term care. Some of the barriers to providing sufficient care include a lack of routines and competence among the healthcare professionals.1–4 In an official policy statement from the American Thoracic and European Respiratory Societies in 2015, it was recommended that healthcare professionals should receive additional education in evidence-based guidelines to improve standards.5 Education programs are therefore considered crucial in increasing the competence of healthcare professionals and the organization of their working procedures in long-term care to improve COPD management.
Education programs are rarely prioritized by the management for healthcare professionals in long-term care.2 This is despite evidence that such programs have been shown to increase knowledge and self-efficacy of nurses in primary and hospital care involved with COPD management.6,7 Electronic health (eHealth) offers an opportunity to facilitate the accessibility of education for healthcare professionals.8 A digital COPD education program for healthcare professionals in primary care was found to increase knowledge and attitudes related to COPD management.9
The effects of education programs on healthcare professionals in long-term care, their routines and working procedures are however unknown. Increased understanding of how their knowledge and working procedures are influenced by online education programs about COPD is specifically warranted.9
The aim of this study was therefore to evaluate the feasibility of a digital COPD education program for healthcare professionals in long-term care, its influence on the COPD-specific knowledge and experience of the affiliated healthcare professionals and their working procedures.
Specific research questions were:
- How do healthcare professionals use, and experience the use of, a digital COPD education program?
- Does a digital COPD education program influence the objective and subjective COPD-specific knowledge and experiences of the affiliated healthcare professionals?
- Do healthcare professionals experience any changes in their working procedures and COPD-related healthcare services after a digital COPD education program?
Materials and Methods
Study Design
A randomized controlled trial with a convergent mixed methods design10 was used to evaluate a digital COPD education program among healthcare professionals working in long-term care. Quantitative and qualitative data was collected over time and analyzed separately, but in a parallel process. Quantitative data was collected using questionnaires and user data. Qualitative data was collected using repeated individual interviews.
Reporting procedures were in accordance with guidelines for reporting randomized controlled trials, qualitative research, qualitative longitudinal research and mixed methods studies.11–14
Setting
This study was conducted in two municipalities in the two most northern county councils in Sweden, both with between 70,000–80,000 inhabitants. The municipalities were selected through convenience sampling. In these municipalities 82 vs 90% of the inhabitants live in the city, while 18 vs 10% live in more rural areas.15 In Sweden, healthcare services are publicly funded. The municipalities are responsible for providing long-term care for the oldest and frailest people in the population, who need healthcare provided at home. Municipal healthcare includes care for people both in private residential housing and in nursing homes. Healthcare professionals within municipal healthcare includes nurses, physical therapists, occupational therapists, and sometimes dieticians. Physicians who prescribe medical treatment are however employed in primary care, but collaborate with healthcare professionals in long-term care, and is organized through the county councils. In addition, within long-term care, “care staff” are responsible for the daily care of people included in municipal healthcare, and they can be employed by home care services, at nursing homes, or in short-term residential care. They can be assistant nurses, which requires one-year of upper secondary education, or care assistants with no education requirements.2
Recruitment and Sample
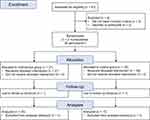
Registered healthcare professionals working in the two included municipalities were recruited for the study. Unit managers provided names and email addresses of registered healthcare professionals working in the municipalities. To detect a mean difference in COPD-specific knowledge on the primary outcome measure, the Bristol COPD Knowledge Questionnaire (BCKQ), of 8.3 ± 8.3 points as seen in a previous study conducted in a primary care setting,16 using a two-tailed test of significance with statistical power of 80% and alpha of 0.05, the required sample size of healthcare professionals was estimated to be 16. With an estimated dropout rate of 20%, we aimed to include a total of 20 healthcare professionals in each group. Potential participants were contacted via email by the researchers and asked if they could think of any additional colleagues interested in participating. Of the 43 invited healthcare professionals, 39 agreed to participate in the study and completed baseline assessment. Prior to the baseline measurements, the two municipalities were randomized to the intervention group or the control group by flipping a coin by a third party not involved in the recruitment. Twenty-one participants were subsequently included in the intervention group and 18 in the control group. All 39 individuals received intended interventions, but one participant in each group dropped out before follow-up tests and thus 37 individuals were analyzed for the primary outcome (Figure 1). Measurement data were collected before and after the intervention period. In addition, 13 participants from the intervention group were invited to participate in individual interviews before and after the intervention period using a semi structured interview guide (Appendices 1 and 2) One participant ended their employment in the municipality during the intervention period and one declined the second interview, resulting in eleven participants completing both interviews.
Intervention
The intervention was a digital COPD education program adapted for healthcare professionals in municipal healthcare, delivered through the interactive web-based platform the COPD Web. The digital COPD education program builds on current national and international COPD treatment guidelines.17,18 The COPD web is an interactive website intended for healthcare professionals and people with COPD.19 The website was first developed in a co-creative process which included people with COPD and healthcare professionals in primary care and the content is based on research evidence and national treatment guidelines.20 The content on the website was later restructured and packaged into a digital COPD education program based on the needs expressed in interviews with healthcare professionals in municipal healthcare,2 national guidelines17 and the BCKQ. The digital program consisted of six modules with different themes (Table 1) and a set of questions about their content. As an introduction to the digital COPD education program, the participants received an email containing information about the content of the modules, that the modules were expected to take approximately 20–30 minutes to complete and some practical information. They also received a computer tablet with internet access up to 10 GB per month. The digital program was available to the intervention group for 12 weeks and the participants received email reminders to take part every two weeks.
 |
Table 1 Content of the Online COPD Education Program as Provided on the COPD Web |
Control
The control group did not receive any intervention but they were informed that they would receive access to the digital COPD education program after the end of the intervention period.
Data Collection
The data collection lasted from January 2018 to May 2018. Data for the quantitative component was collected using questionnaires. The questionnaires were distributed to the participants at baseline and after the 12-week intervention.
COPD-specific knowledge was measured using the BCKQ, which includes 65 items divided into 13 topics.21 For this study, 25 items divided into five topics (Appendix 1) were added to the BCKQ. These items covered recommendations from the national treatment guidelines provided by the Swedish National Board of Health and Welfare in 2015.17 The BCKQ was translated to Swedish by one of the authors, and was – together with the new items – tested for face validity by two COPD nurses in specialty care.
The questionnaire Conceptual knowledge use, previously used by healthcare professionals in Swedish primary care,22 was also used in this study to assess attitudes, knowledge and whether it was considered part of their role to deliver evidence-based healthcare services to people with COPD.
Data on usage of the platform was collected through a standardized questionnaire in which participants noted the time spent on each module in minutes. In addition, the importance of the six modules in their work with people with COPD were ranked from 1–6 (1 = most important).
Ten statements from the questionnaire Task-technology measures23 were used to assess the feasibility of the COPD web and how it could support the participants in their work tasks. The statements were adapted to fit the context of the study. Statements related to “information” were used to assess if the COPD web supported the participants in their work tasks, while statements related to “assessing feasibility” focused on detecting possible issues related to access and learnability of the website. The participants rated their concurrence with the statements on a Likert scale from 1 to 7.
A qualitative longitudinal approach was used to evaluate and better understand the intervention. Qualitative longitudinal research is particularly useful in contributing to trial development, evaluation and implementation granting possibilities to investigate changes and processes.24,25 Individual interviews were performed with participants from the intervention group at baseline and after the 12-week intervention. All participants in the intervention group was asked to participate in individual interviews, 11 healthcare professionals accepted an interview at both baseline and the 12 months follow up.
All the interviews at baseline (n = 11) were conducted face-to-face by UMP and the interviews after the intervention were conducted face-to-face (n = 8) or by telephone (n = 3) by AN and KW. The interviewers had no earlier relationship with the participants and no additional persons were present during the interviews. The participants were aware that the interviewers were involved in the project. The interview guide was partly based on the interview guide in a previous study22 and covered questions about their knowledge of COPD and COPD-related healthcare services (eg How do you experience your knowledge about COPD?) and their COPD-related working procedures (eg What healthcare services do you provide based on your professional role?). The second interview also addressed the use and feasibility of the COPD web (eg How did you experience the use of the COPD web and this education program?), as well as perceived changes in knowledge and working procedures (eg Do you experience any change in your knowledge about COPD?). The interviews took place at the participants’ workplaces. The first interviews lasted 18–60 (median 38) minutes and the second 24–39 (median 29) minutes. All interviews were audio recorded and transcribed verbatim by a professional transcriber.
Data Analysis
The quantitative data analyses were per-protocol. First, the assumption of normality was assessed using the Shapiro–Wilk test. Then, between-group differences were assessed using independent sample T-tests or Mann–Whitney U-tests depending on data distribution. In addition, Pearson correlation coefficients were used to analyze the correlation between change in COPD knowledge and baseline COPD knowledge. The strengths of the correlation coefficients were categorized as 0.1–0.3 small, 0.3–0.5 moderate, 0.5–0.7 large, 0.7–0.9 very large and 0.9–1.0 extremely large.26 No additional analyses were performed. AN performed the majority of quantitative analysis. The software Jamovi version 1.6.7 (Jamovi, Sydney, Australia) was used for data management and statistical analysis, and a P-value of <0.05 was considered statistically significant.
The qualitative data were analyzed using qualitative content analysis27 in a diachronic manner (all data were analyzed after the data collection was completed).25 First, transcripts were read through and the interview text was divided into three domains: 1) feasibility of the digital COPD education program, 2) knowledge and experience, and 3) working procedures. The three domains were then analyzed separately, the text associated with each domain was divided in meaning units and coded. The texts and codes of each participant were then compared over time.24,25 In this stage, matrices with codes and interview text were constructed to visualize changes between the first and second interviews for each participant and domain.28,29 Finally, the within-participant changes were compared across the participants, thus enabling an interpretation of any potential changes in the domains over time. The first interview in each domain was coded collaboratively by SL and ÅA. SL performed the qualitative analysis, but had repeated discussions with ÅA during the emerging analysis. The participants were not asked to comment on the transcription or the analysis. The software MAXQDA 2020 was used for the coding procedure.
A mixed methods merging of the quantitative and qualitative components for each domain was conducted when preliminary quantitative and qualitative analyses were completed,10,30 using a weaving approach on a domain-by-domain basis.30 First, the preliminary quantitative and qualitative analyses were divided into the three domains, compared and discussed by SL, AN, ÅA and KW. Second, based on the discussions, SL wrote a first draft for the result section for each domain, where the quantitative and qualitative findings were described and compared to each other. The draft was discussed with AN and ÅA and further analyses were made. Finally, SL wrote the result section in close collaboration with AN. They presented and discussed the results with ÅA and KW and adjusted the analyses and text until agreement.
Results
The results of the study, where the quantitative and qualitative findings are intertwine, are presented in the three domains: 1) Feasibility of the digital COPD education program, 2) Knowledge and experience, and 3) Working procedures. Characteristics of the participants are presented in Table 2.
 |
Table 2 Characteristics of the Participants at Baseline |
Feasibility of the Digital COPD Education Program
Figure 2 shows the intervention group’s rated experience of the support received from the COPD web. The web was generally experienced as good support. In their first interviews, the participants expressed positive expectations and after the digital COPD education program they particularly stated that the structure of the program was good. However, participants also wanted more movies, pictures and recorded lectures to be combined with the text. They also described a few technical problems.
 |
Figure 2 Experiences of how the COPD web can support participants’ work tasks. Abbreviation: COPD, chronic obstructive pulmonary disease. Note: Data is mean (SD). |
The participants estimated that they had spent on average 26–31 minutes for each module (Table 3). However, in the interviews the described time and frequency for using the digital COPD education program varied. The digital program was completed on a computer and/or tablet, but it was perceived difficult to prioritize the program during the working day because of time constraints. Several participants consequently described completing the program at home in their spare time.
And there’s not been that much [time] because I’ve actually sat down [with the education program] when I’ve been on the bus and, like, in my spare time. It’s been a hindrance that you should try and prioritize [the program] during your work hours and it’s really difficult when you have lots of other things to do. (nurse, after intervention)
 |
Table 3 Estimated Time for Usage and Order of Importance for Each Module |
The two modules about COPD and common problems were rated as the most important modules (Table 3) and this was confirmed in the interviews. The module “COPD and follow-ups” was rated as the least important (Table 3). Participants did however state that all modules were important in order to acquire knowledge about the roles and healthcare services for all the different professions.
And there were even parts which were maybe more intended for, like, occupational therapists and physical therapists and such, but it’s good anyway that we get to see which part of the work that’s theirs and what they’re going to do and how they … it’s really good, so that you have, like, more understanding for what everyone does. If there’s anything that you wonder about, that you know that this is maybe your task. And then it becomes easier to work together. (nurse, after intervention)
The participants were generally satisfied with the information in the digital COPD education program. However, both occupational therapists and dieticians wanted more information related to their professions.
I think that it [the program] was missing a part about occupational therapy and daily activities. That could have been included as a part of the COPD web too … I mean however ill you are you have to be able to cope with daily, personal care. (occupational therapist, after intervention)
Each module concluded with 4–24 questions related to their content. The questions were described by the participants as good learning opportunities. The digital COPD education program had given the participants a desire to learn more, complete further COPD courses and they wanted more colleagues to complete the program. In the future, they wanted to continue using the COPD web to update their knowledge, but also for patient education and peer education.
The in-home healthcare staff are very interested in going on courses too. And then I thought, you can actually use [the COPD web] if you want to explain [COPD-related information]. (nurse, after intervention)
Knowledge and Experience
A significant increase in objective COPD-related knowledge in the intervention group compared to the control group was shown as measured by the BCKQ (14 vs 6 percentage points, p=0.007). Similarly, the additional questions (based on the Swedish national guidelines for COPD management) were significantly different between groups in favor of the intervention group (16 vs 0 percentage points, p=0.002), as well as when all the questions were analyzed together (15 vs 4 percentage points, p=0.001) (Table 4). The participants described in the interviews that the digital program increased their knowledge. Some stated that they learned about new aspects of COPD, while other participants said that it confirmed existing knowledge and gave them the possibility to update their knowledge. The experience of increased knowledge led to a feeling of increased security and attention to COPD.
And then this is something that I haven’t mentioned which has been important for me, infections and which signs you can think about … I’ll be quicker to realize if they get flu symptoms and quicker to act … that’s probably one of the most important things I think that I am more aware of now. (nurse, after intervention)
 |
Table 4 Objective COPD-Specific Knowledge Measured with BCKQ and Questions Based on the Swedish National Guidelines for COPD Management |
For the intervention group, there was a significant correlation between their objectively measured knowledge (BCKQ including the added questions) before the intervention and their increase in knowledge (r = −0.835, p <0.001). Namely, participants with a lower BCKQ score before the intervention showed a greater increase in knowledge, which was also confirmed by how the participants described their experiences in the interviews. Participants who experienced or described a relatively good knowledge in their first interview perceived that the digital COPD education program became a confirmation of already existing knowledge and only gave certain elements of increased knowledge.
… most of this that was in the program is stuff which I have learned before and stuff which I’ve heard, but when you’ve heard it again it’s like … you can take in other stuff. It’s like … oh yeah, it was like this, kind of thing. (nurse, after intervention)
On the other hand, participants who expressed a lack of knowledge in their first interview generally experienced that the digital education program had given increased knowledge.
… I realize that I have … what I can contribute with … I would like to do so much more, but I feel that I don’t have that knowledge.
… I have a better understanding now … I feel that I have more knowledge today than what I had then. (physical therapist, before vs after intervention)
Results from the BCKQ showed that the intervention group had significantly increased their specific knowledge about epidemiology, breathlessness, aetiology and follow-ups and tests (Table 4). Further, compared to the control group, a significant increase in percentage of participants with self-reported sufficient knowledge in providing COPD-related self-management, health promotion healthcare services, and disease-specific education was seen in the intervention group (Table 5). Although not shown in the knowledge questionnaire, participants also mentioned several areas of increased knowledge in the interviews, such as breathing techniques, physical activity, signs of exacerbations, weight loss/nutrition, and diagnostics. Increased knowledge about the areas of other professions was especially emphasized. As an example, in the first interview a nurse mainly mentioned healthcare services such as breathing exercises, pharmacological treatment and treating exacerbations. In the second interview, the same nurse also raised physical activity/exercise and nutrition as important healthcare services. Consequently, there was an increased focus on the importance of interprofessional collaboration in the second interviews.
On the other hand, I can kind of think more today about … yes but is this someone who can breathe against resistance in a bottle [PEP] or is anyone thinking about their work of breathing? Is the physical therapist involved? Like more that which is really not part of my profession but … I think that I’ve got a different view of … yes ok, I’m not going to do the physical therapist’s job or someone else’s job, but anyway check … have you included several professions? (dietician, after intervention)
 |
Table 5 Subjective Report of Sufficient Knowledge of COPD-Related Healthcare Services from the Conceptual Knowledge Use Questionnaire |
Working Procedures
Working procedures related to COPD management was subjectively evaluated in both the intervention group and the control group.
After the intervention, neither the intervention group nor the control group showed any changes from baseline regarding the estimated number of patients with COPD per week or their opinion of healthcare services that were part of their work tasks. In the interviews, participants stated that only a few of their patients had COPD and that even for those with COPD, COPD-related issues were rarely the reason for their initial contact. The participants also reported that they were not always informed about their patients’ COPD diagnosis. The National Treatment Guidelines for COPD were not implemented in their practice, but guidelines for some other diseases were. After the digital COPD education program, participants mainly experienced that their working procedures had not changed, but that their attention to patients with COPD and COPD-related healthcare services was raised. Furthermore, the digital program had also contributed to an increased confidence in talking about the disease.
In the conceptual knowledge use questionnaires, both the intervention group and control group reported health promotion healthcare services to people with COPD as important (INT mean 1.5–2.1, CON mean 1.5–2.7), with no change over time. In the interviews, working procedures were described where the patients’ needs directed the healthcare services, while the diagnosis itself was often ignored. This led to late healthcare services where the participants were “putting out fires” rather than working preventively and there was a lack of resources for health promotion healthcare services. After the intervention, the participants emphasized the importance of health promotion healthcare services and expressed a wish for earlier healthcare services to prevent exacerbations.
But then as I said, they’re so late in the process, so it feels like we’re more fixing what’s already there than we are improving their health. It feels like that so much earlier.
As physical therapists … we maybe work more when they are most ill, but it should maybe be the opposite. It maybe should be that you have more time before. (physical therapist, before vs after intervention)
In the interviews, some changes in working procedures were presented within their own professional area, such as starting to instruct pursed lip breathing, providing specific advice for physical activity and increased support for smoking cessation. In addition, the digital COPD education program led to an increased attention to healthcare services provided by other professions, interprofessional discussions with other professions and a desire for more interprofessional collaboration.
I’ve felt motivated to … yes this will be good. Yes, that I’ve like got confirmation that you’re thinking correctly when you’re trying to collaborate with others. (nurse, after intervention)
Finally, the participants expressed their wishes for changes in their working procedures to give them greater opportunities to use their increased knowledge.
Discussion
The present study is, to our knowledge, the first to evaluate a digital COPD education program for healthcare professionals in long-term care. The feasibility of the program was expressed as satisfactory concerning the content and structure. It was also experienced as supporting the participants’ work through increased COPD-specific knowledge, security and attention to COPD.
Previous research has shown that healthcare professionals in long-term and primary care in Sweden report that they have insufficient knowledge about COPD management. They also experience a huge gap between treatment guidelines and the healthcare services provided to people with COPD.2,22 In the present study, baseline COPD-specific knowledge of our participants was measured using the BCKQ. The percentage of correct answers for the intervention and control groups was 69% and 60% respectively, which can be compared to previous studies showing 51–59% for non-respiratory nurses and 60–61% for respiratory nurses.6,31,32 The healthcare professionals included in the present study thus had a similar, or slightly higher, level of COPD-specific knowledge compared those of previous studies. In a previous study, an intensive and interactive two-hour face-to-face education session increased the COPD-specific knowledge of nurses in different healthcare settings by 19 percentage points.6 That increase was five percentage points more than the increase seen for the intervention group in the present study who had a total education time of about three hours. However, the nurses in the aforementioned study had lower knowledge at baseline6 compared to the healthcare professionals in the present study, indicating greater potential for improvement in that group. Nevertheless, these findings suggest that a digital COPD education program can be as effective at increasing knowledge as a face-to-face education program. In support of this, a previous COPD education program consisting of six video lessons was found to increase the knowledge of healthcare professionals in primary care.33 A previous study further found that a COPD education program for nurses in primary care increased their sense of security and their confidence in their competence,34 which was also shown in the present study. Both nurses in primary care and the healthcare professionals in the present study described how the education programs had taught them about the value of contributions from other professions in COPD management and facilitated interprofessional collaboration.34 Thus, increased knowledge from a digital COPD education program can lead to a greater sense of security and increased focus on COPD-related issues, which in turn can facilitate COPD-related discussions with other healthcare professionals.
Despite the increase in COPD-specific knowledge, especially concerning epidemiology, breathlessness, aetiology, and follow-ups and tests, the healthcare professionals in the present study did not express any change in their working procedures. This is perhaps not surprising considering the relatively short time for the digital COPD education program to enable such a change. The present study also indicates that there might be organizational barriers to changes in working procedures. The integrated-Promoting Action on Research Implementation of Health Services (i-PARIHS) framework35 can be used to understand which factors are needed to achieve a successful implementation of evidence-based COPD management in long-term care. With the digital COPD education program, the knowledge of the recipients,35 ie the healthcare professionals, was improved. A previous study also showed that an education program can increase the self-efficacy of healthcare professionals.7 According to i-PARIHS, innovation, context and facilitation are crucial for implementation.35 Innovation focuses on the evidence for COPD management and how it will fit in the long-term care setting.35 There is substantial evidence for the effects of COPD management and the healthcare services are recommended in national and international guidelines,17,18 which the digital COPD education program is based on. Healthcare professionals in long-term care have however expressed that the national guidelines need to be adapted to fit the long-term care setting.2 Padilha, Sousa, Pereira36 concluded that it was important to develop specific guidelines and support for decision-making for the clinical practice of that particular profession. In addition, the healthcare professionals’ perceptions of digital services can influence the implementation of a digital education program.37 Including healthcare professionals as stakeholders in the development and implementation of such education programs is important to provide support adapted to their needs.38 Context includes the immediate work environment of the recipients and the organization.35 The participants expressed that they had little time to participate in the digital COPD education program, something which has also previously been reported as an organizational barrier.2,22 Another study in Swedish long-term care further found that interprofessional collaboration regarding COPD was rare.2 Time constraints and lack of collaborations thus likely negatively influence the potential to change working procedures. Finally, facilitation is an important factor and an active ingredient in i-PARIHS, and requires someone to take on the role of facilitator.35 In the present study, no person had the official role of facilitator. Healthcare professionals thus probably need more support for change than only a digital education program. Padilha, Sousa, Pereira36 suggested the need for a person who serves as an agent of change, stimulates reflection, and supports achieving the change. The support should also be directed at stimulating a change of working procedures in the whole working group, not only for individuals, to stimulate interprofessional collaboration. Further research is needed to explore which additional interventions are needed to change working procedures in long-term care.
Methodological Considerations
A major strength of the present study is the use of a mixed methods design and the longitudinal approach in the qualitative component. Using both quantitative and qualitative methods provides a more comprehensive picture and the two approaches strengthen each other.10 As an example, by using both quantitative and qualitative methods to evaluate COPD-specific knowledge, we found both objectively measured and experiences of increased knowledge, but also experiences that the increased knowledge led to more security and focus on COPD. The use of a mixed methods design also showed that, in addition to the 14% increase in objectively measured COPD-specific knowledge seen on a group level (Table 4), more than a third of the intervention group (36%) reported increased self-reported sufficient knowledge in providing targeted healthcare services for people with COPD, compared with only 4% in the control group (Table 5). The recurrent interviews enabled comparisons between participants’ experiences and attitudes before and after the intervention. The interviews followed a semi-structured interview guide so all interviews would have the same focus. However, had the interviewer also reviewed the first interviews before conducting the second interviews, the second interviews could had been adapted to follow up on aspects relevant to each participant and thus better capture change among individuals.28
For this study, we added 25 items to the original version of BCKQ. The original version of BCKQ21 consists of 13 topics with five items for each topic, where five of the topics are about pharmacological treatment. We wanted get a broader understanding of the participants’ knowledge, since it is mainly the nurses of the included participants who are involved in pharmacological treatment. Consequently, we compared the original version with the updated Swedish national treatment guidelines17 and added topics that were underrepresented to better fit the new guidelines. In the analysis we have, however, presented the results from the original version separately to facilitate comparisons with other studies.
The question about which healthcare services that were part of their role was answered quite differently by the intervention group and the control group. This may reflect the skewed distribution of professions between the groups and/or potential differences in work organization and attitudes across the two municipalities. The intervention group consisted for the most part of nurses, while the control group largely consisted of occupational therapists and physical therapists. This skewed distribution of professions could have influenced the generalizability of the results. However, the baseline knowledge of the two groups was rather similar, thus suggesting that the skewed distribution of healthcare professionals between intervention and control groups did not impact our between-group comparisons. Furthermore, the skewed distribution of professions is merely a reflection of the organizational structure of long-term care in Sweden, indicating that there are regional differences in access and availability of different health professionals within long-term care. Notably, the content of the digital COPD education program was not specifically designed for healthcare professionals in long-term care, it was designed based on international and national COPD treatment guidelines17,18 and could thus be used for healthcare professionals also in other settings than long-term care.
A possible limitation of the study design is that the researchers who conducted the interviews after the intervention period were part of the team that developed the COPD web and the digital COPD education program, which could have influenced the answers of the participants. However, it is not clear if the participants were aware of the interviewers’ involvement in the development and the recorded interviews and the transcripts did not reveal any obvious influence on the participants. Furthermore, all analyses of the interviews were made by a third party not involved in any of the interviews or the design of the current study.
Conclusions
The digital COPD education program was feasible to use among healthcare professionals in long-term care, with satisfaction regarding content, structure and support. The digital program also increased the COPD-specific knowledge of the healthcare professionals who received this intervention. Increased knowledge lead to increased experiences of security, increased focus on COPD-related issues and discussions about COPD with other healthcare professionals. More comprehensive measures might be needed to change working procedures, such as allocated time and opportunities for interprofessional collaboration, as well as a facilitator who can support the implementation of changing working procedures. Further research is needed to explore how such comprehensive measures should be designed.
Abbreviations
BCKQ, Bristol COPD Knowledge Questionnaire; CON, Control group; COPD, Chronic obstructive pulmonary disease; eHealth, Electronic health; i-PARIHS, integrated-Promoting Action on Research Implementation of Health Services; INT, Intervention group; NS, Non-significant; SD, Standard deviation.
Ethics Approval and Informed Consent
This study received ethical approval from the Regional Ethical Review Board in Umeå, Sweden (Dnr 2016/503-31). All participants were informed about the purpose of the study, and the informed consent included publication of anonymised responses. All included participants gave their written consent. We have ensured confidentiality for the individual participants through the whole process, from the analyses to the presentation of findings.
Acknowledgments
We would like to acknowledge all participants that have informed this study with their valuable time and knowledge.
Author Contributions
All authors made a significant contribution to the work reported. AN, KW and UMP in the conception, study design, execution, and acquisition of data. AN, SL and ÅA in the analysis and interpretation, SL drafted the manuscript in collaboration with AN while all authors took part in revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This study was funded by the Swedish Heart and Lung Foundation (Dnr: 20160505), SFO-V (Strategic research area Care Science), King Gustaf V’s and Queen Victoria’s Freemason Foundation, and the Swedish Heart and Lung patient association (Dnr: E-120-16). The sponsors were not involved in the research process or presentation of the findings.
Disclosure
The abstract of this paper was presented at the European Respiratory Society Annual Conference 2021 as a poster presentation with interim findings. The poster’s abstract was published in “Poster Abstracts” in European Respiratory Journal 2021 58: PA758; DOI: 10.1183/13993003.congress-2021.PA758. Sara Lundell and Karin Wadell report grants from the Swedish Heart and Lung Foundation, SFO-V (Strategic research area Care Science), King Gustaf V’s and Queen Victoria’s Freemason Foundation, and the Swedish Heart and Lung patient association, during the conduct of the study. The authors report no other conflicts of interest in this work.
References
1. Suarez-Barcelo M, Micca JL, Clackum S, Ferguson GT. Chronic obstructive pulmonary disease in the long-term care setting: current practices, challenges, and unmet needs. Curr Opin Pulm Med. 2017;23(Suppl 1):S1–S28. doi:10.1097/MCP.0000000000000416
2. Lundell S, Pesola UM, Nyberg A, Wadell K. Groping around in the dark for adequate COPD management: a qualitative study on experiences in long-term care. BMC Health Serv Res. 2020;20(1):1025. doi:10.1186/s12913-020-05875-2
3. Patel M, Steinberg K, Suarez-Barcelo M, Saffel D, Foley R, Worz C. Chronic obstructive pulmonary disease in post-acute/Long-term care settings: seizing opportunities to individualize treatment and device selection. J Am Med Dir Assoc. 2017;18(6):
4. Mousing CA, Timm H, Lomborg K, Kirkevold M. Barriers to palliative care in people with chronic obstructive pulmonary disease in home care: a qualitative study of the perspective of professional caregivers. J Clin Nurs. 2018;27(3–4):650–660. doi:10.1111/jocn.13973
5. Rochester CL, Vogiatzis I, Holland AE, et al. An official American Thoracic Society/European respiratory society policy statement: enhancing implementation, use, and delivery of pulmonary rehabilitation. Am J Respir Crit Care Med. 2015;192(11):1373–1386. doi:10.1164/rccm.201510-1966ST
6. Staiou M, Gourgoulianis K, Kotrotsiou E, Raftopoulos V. Closing the gap: the effect of an evidence-based intervention in increasing COPD nurses’ knowledge. Nurs Forum 2021;56:30–36.
7. Genuino MJ. Effects of simulation-based educational program in improving the nurses’ self-efficacy in caring for patients’ with COPD and CHF in a post-acute care (PACU) setting. Appl Nurs Res. 2018;39:53–57. doi:10.1016/j.apnr.2017.10.012
8. Shaw T, McGregor D, Brunner M, Keep M, Janssen A, Barnet S. What is eHealth (6)? Development of a conceptual model for ehealth: qualitative study with key informants. J Med Internet Res. 2017;19(10):e324. doi:10.2196/jmir.8106
9. Moreo K, Greene L, Sapir T. Improving interprofessional and coproductive outcomes of care for patients with chronic obstructive pulmonary disease. BMJ Qual Improv Rep. 2016;5(1):
10. Meissner H, Creswell J, Klassen AC, Plano V, Smith KC. Best practices for mixed methods research in the health sciences. Methods. 2011;29:1–39.
11. Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–357. doi:10.1093/intqhc/mzm042
12. O’Cathain A, Murphy E, Nicholl J. The quality of mixed methods studies in health services research. J Health Serv Res Policy. 2008;13(2):92–98. doi:10.1258/jhsrp.2007.007074
13. Moher D, Hopewell S, Schulz KF, et al. CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. J Clin Epidemiol. 2010;63(8):e1–37. doi:10.1016/j.jclinepi.2010.03.004
14. SmithBattle L, Lorenz R, Reangsing C, Palmer JL, Pitroff G. A methodological review of qualitative longitudinal research in nursing. Nurs Inq. 2018;25(4):e12248. doi:10.1111/nin.12248
15. Statistics Sweden. Kommuner i siffror [Municipalities in numbers]. Available from: https://kommunsiffror.scb.se/.
16. Hill K, Mangovski-Alzamora S, Blouin M, et al. Disease-specific education in the primary care setting increases the knowledge of people with chronic obstructive pulmonary disease: a randomized controlled trial. Patient Educ Couns. 2010;81(1):14–18. doi:10.1016/j.pec.2009.09.035
17. Socialstyrelsen (The National Board of Health and Welfare). Nationella riktlinjer. Vård vid astma och KOL. (National guidelines. Treatment of asthma and COPD); 2015. Available from: https://www.socialstyrelsen.se/kunskapsstod-och-regler/regler-och-riktlinjer/nationella-riktlinjer/riktlinjer-och-utvarderingar/astma-och-kol/.
18. Vogelmeier CF, Criner GJ, Martinez FJ, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 report. GOLD executive summary. Am J Respir Crit Care Med. 2017;195(5):557–582. doi:10.1164/rccm.201701-0218PP
19. Nyberg A, Tistad M, Wadell K. Can the COPD web be used to promote self-management in patients with COPD in Swedish primary care: a controlled pragmatic pilot trial with 3 month- and 12 month follow-up. Scand J Prim Health Care. 2019;37(1):69–82. doi:10.1080/02813432.2019.1569415
20. Tistad M, Lundell S, Wiklund M, Nyberg A, Holmner A, Wadell K. Usefulness and relevance of an ehealth tool in supporting the self-management of chronic obstructive pulmonary disease: explorative qualitative study of a cocreative process. JMIR Hum Factors. 2018;5(4):e10801. doi:10.2196/10801
21. White R, Walker P, Roberts S, Kalisky S, White P. Bristol COPD Knowledge Questionnaire (BCKQ): testing what we teach patients about COPD. Chron Respir Dis. 2006;3(3):123–131. doi:10.1191/1479972306cd117oa
22. Lundell S, Tistad M, Rehn B, Wiklund M, Holmner Å, Wadell K. Building COPD care on shaky ground: a mixed methods study from Swedish primary care professional perspective. BMC Health Serv Res. 2017;17(1):467. doi:10.1186/s12913-017-2393-y
23. Goodhue DL, Thompson RL. Task-Technology Fit and individual performance. MIS Q. 1995;19(2):213–236. doi:10.2307/249689
24. Calman L, Brunton L, Molassiotis A. Developing longitudinal qualitative designs: lessons learned and recommendations for health services research. BMC Med Res Methodol. 2013;13(1):14. doi:10.1186/1471-2288-13-14
25. Tuthill EL, Maltby AE, DiClemente K, Pellowski JA. Longitudinal qualitative methods in health behavior and nursing research: assumptions, design, analysis and lessons learned. Int J Qual Methods. 2020;19:1609406920965799. doi:10.1177/1609406920965799
26. Hopkins WG, Marshall SW, Batterham AM, Hanin J. Progressive statistics for studies in sports medicine and exercise science. Med Sci Sports Exerc. 2009;41(1):3–13. doi:10.1249/MSS.0b013e31818cb278
27. Graneheim UH, Lundman B. Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Educ Today. 2004;24(2):105–112. doi:10.1016/j.nedt.2003.10.001
28. Kneck Å, Audulv Å. Analyzing variations in changes over time: development of the pattern-oriented longitudinal analysis approach. Nurs Inq. 2019;26(3):e12288. doi:10.1111/nin.12288
29. Grossoehme D, Lipstein E. Analyzing longitudinal qualitative data: the application of trajectory and recurrent cross-sectional approaches. BMC Res Notes. 2016;9(1):136. doi:10.1186/s13104-016-1954-1
30. Fetters MD, Curry LA, Creswell JW. Achieving integration in mixed methods designs-principles and practices. Health Serv Res. 2013;48(6 Pt 2):2134–2156. doi:10.1111/1475-6773.12117
31. Ma Y, Peng Y, Chen P, Nie N, Chen Y. Assessment of COPD-related knowledge among internal medicine nurses: a cross-sectional study. Int J Chron Obstruct Pulmon Dis. 2019;14:2917–2925. doi:10.2147/COPD.S232055
32. Guo SE, Shen HC, Okoli C, et al. Generalist versus specialist nurses’ knowledge, attitudes, and behavioral intentions toward promoting pulmonary rehabilitation for patients with chronic obstructive pulmonary disease: a cross-sectional correlational study. Medicine. 2018;97(43):e12975. doi:10.1097/MD.0000000000012975
33. Alcântara EC, Corrêa KS, Jardim JR, Rabahi MF. Multidisciplinary education with a focus on COPD in primary health care. J Bras Pneumol. 2019;45(6):e20180230. doi:10.1590/1806-3713/e2018-0230
34. Berland A, Bentsen SB. Patients with chronic obstructive pulmonary disease in safe hands: an education programme for nurses in primary care in Norway. Nurse Educ Pract. 2015;15(4):271–276. doi:10.1016/j.nepr.2015.03.003
35. Harvey G, Kitson AL. Implementing Evidence-Based Practice in Healthcare: A Facilitation Guide. Oxon, UK: Routledge; 2015.
36. Padilha JM, Sousa PAF, Pereira FMS. Nursing clinical practice changes to improve self-management in chronic obstructive pulmonary disease. Int Nurs Rev. 2018;65(1):122–130. doi:10.1111/inr.12366
37. Gaveikaite V, Grundstrom C, Lourida K, et al. Developing a strategic understanding of telehealth service adoption for COPD care management: a causal loop analysis of healthcare professionals. PLoS One. 2020;15(3):e0229619. doi:10.1371/journal.pone.0229619
38. Leask CF, Sandlund M, Skelton DA, et al. Framework, principles and recommendations for utilising participatory methodologies in the co-creation and evaluation of public health interventions. Res. Involv Engagem. 2019;5(1):2. doi:10.1186/s40900-018-0136-9
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.