Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 12
Empowerment of patients with type 2 diabetes: current perspectives
Authors Gómez-Velasco DV, Almeda-Valdes P , Martagón AJ , Galán-Ramírez GA, Aguilar-Salinas CA
Received 16 February 2019
Accepted for publication 25 June 2019
Published 6 August 2019 Volume 2019:12 Pages 1311—1321
DOI https://doi.org/10.2147/DMSO.S174910
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Steven F. Abcouwer
Donají V Gómez-Velasco,1 Paloma Almeda-Valdes,1,2 Alexandro J Martagón,1,3 Gabriela A Galán-Ramírez,1 Carlos A Aguilar-Salinas1–3
1Unidad de Investigación de Enfermedades Metabólicas, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Mexico City, Mexico; 2Departamento de Endocrinología y Metabolismo, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Mexico City, Mexico; 3Tecnológico de Monterrey, Escuela de Medicina y Ciencias de la Salud, Mexico City, Mexico
Abstract: Patient empowerment is a continuous process in which knowledge, motivation, and capacity to take control of their disease are built within a person. This concept is not always well understood and applied. This review describes the strategies to induce empowerment in patients with diabetes. In addition, the most common scales used to evaluate empowerment in diabetes is described. Furthermore, the effectiveness of the empowerment-based interventions for improving metabolic control and diabetes knowledge are described. Finally, we discuss opportunities for empowerment implementation in clinical practice and current needs on research that can be translated into public policies.
Keywords: empowerment, motivation, self-care, Diabetes Empowerment Scale, depression
Introduction
The patients’ involvement in their own care is a cornerstone of diabetes care and the health care providers’ role is to stimulate and support patients’ self-management and problem-solving skills.1,2 Self-management behaviors are needed for the successful implementation of every intervention that improves metabolic control in patients with diabetes or delays the onset of chronic complications. According to the American Diabetes Association (ADA), all people with diabetes should participate in diabetes self-management education to acquire the knowledge, skills, and abilities necessary for diabetes self-care.3 Therefore, diabetes care programs should include a diabetes self-management education and support (DSMES) module, in which knowledge, skills, and motivation to care are developed for the patient and close relatives.4
In this article, we review the importance of empowerment in patients with diabetes, tools for empowering patients and for evaluating empowerment and its impact in metabolic outcomes. Also, we propose an algorithm for health care providers to implement it. Finally, some challenges and opportunity areas are discussed.
We searched on PubMed for relevant publications with the terms empowerment and self-management and diabetes, obtaining a total of 393 results. All titles were reviewed; the ones considered pertinent were included within the references. We also reviewed references from key papers to identify additional relevant bibliography.
Definition of empowerment
The concept of empowerment has its beginnings in the 1970s during the civil rights movements where it was initially applied to women. The main idea was to transfer power from those who were aware of it to those who did not have any. Empowerment is a construct shared by various contexts and disciplines, including psychology, education, economics, social science, public health, among others.5
Empowerment was applied, for the first time in health issues, as part of health promotion programs. It was accepted that powerlessness is a risk factor for having an adverse outcome for almost every disease; therefore, empowerment arises as a health-enhancing strategy.6 Later, it was used to increase the autonomy and participation of patients in the adoption of a healthy lifestyle.7 In recent years, empowerment is the strategy used for the management of chronic diseases, such as diabetes, in which patients participate and take responsibility for their care to improve health outcomes, and secondarily to reduce health costs.8
The WHO defines empowerment as “a process through which people gain control over decisions and actions affecting health” and it should be considered as both an individual and a community process.9 Funnell et al define empowerment as the discovery and development of one’s inherent capacity to be responsible for one’s own life. People are empowered when they have adequate knowledge to make rational decisions, resources to implement their decisions, and sufficient experience to evaluate the effectiveness of their decisions.10 Empowerment is more than an intervention or strategy to help people make behavior changes to adhere to a treatment plan. Fundamentally, patient’s outcomes can be potentially and positively influenced through empowerment, to achieve better compliance with their program of treatment.11 Patients are empowered when they have knowledge, skills, attitudes, and the self-awareness necessary to influence their own behavior and that of others, in order to improve the quality of their lives.12 Orem considers health empowerment when a person develops the ability for self-care, critical thinking, attitude, and autonomy to make decisions regarding health.13
The three main pillars of empowerment in diabetes are:12
- Diabetes is a patient-managed disease
- Patients should be capable to make decisions based on the information provided by the health team
- Patients should identify and implement their own treatment goals, which have a real impact on their lives
Empowerment clearly represents a shift in attitude for both patients and health care professionals.14 The empowerment approach does not involve convincing, persuading, or changing people minds.7 Empowerment requires the facilitation and support for patients to reflect on their own experience of living with diabetes. Promoting an environment characterized by psychological safety, warmth, collaboration, and respect will enhance a self-reflection process. Those requirements are essential for building a self-directed positive change in behavior, emotions, and/or attitudes.7 Despite of the latter, a common scenario is that patients may have diabetes knowledge, but are not empowered.15 This could be secondary to several different circumstances, such as psychosocial aspects (eg, denial), lack of skills, interference with daily life activities, and a lack of an organized strategy to implement self-care behaviors.
Implementation of an empowerment program in diabetes management
There is not a unique accepted model or standardized technique for behavioral change in diabetes management. Some behavioral change models are described in Table 1. In practice, empowerment programs incorporate several theories in their conceptual model. Assessment of the motivation stages (considered in cognitive programs) is critical to select the approach to share information and create a competence (as proposed in the perceived self-efficacy programs or in the locus of control theory). Programs should be adapted to the target population characteristics; health professionals should be capable of adapting the interventions based on the patient’s profile.
 |
Table 1 Behavior change models |
Empowerment programs are composed of a core intervention supplemented with a set of reinforcement tools. The main outcomes, self-care behaviors, knowledge, skills, etc., are achieved during individual or group sessions.16 In order to achieve a long-term effect, several tools should be implemented to induce adherence.14,17,18
Supporting tools: booklets or manuals
Printed and/or digital education materials (eg, manuals, books and infographics) are the most frequently used source of information since this approach has the greatest likelihood to reach a large number of individuals at a low cost. As an example, the National Diabetes Education Program created the “Four steps to manage your diabetes for life” booklet. It contains simple recommendations that help patients to understand the disease, to do self-monitoring and to make correct decisions in a timely manner. Language is understandable for individuals with basic education. Colors, images, and graphics are used to help improve the acceptance of the booklet.18
The effectiveness of the booklets-based interventions has been measured in several settings and populations. For example, a group from New Zealand analyzed the impact of the Diabetes Passport booklet and concluded that the use of this resource leads to an improvement of HbA1c levels. However, no change in diabetes knowledge was achieved. This group suggested the use of this material in combination with other tools.18–20 Wallace et al used consultations and the Living with Diabetes guide. The intervention increased patient participation and improved behaviors and knowledge.18,21
Cell phone calls
The advantage of the use of cell phones is the direct communication with patients using either short text messages or direct calls at any time and any place. Topics include glucose monitoring, medication use, nutritional guidance, or physical exercise. Evidence has shown that this technology helps improve HbA1c levels.22 In 2008, a systematic review evaluated the use of phone calls in patients with diabetes and obesity. Care, support, and guidance via phone calls and/or text messages improved health outcomes related to diabetes by promoting self-efficacy and self-care behaviors.17
Websites
Massive health information providers, such as Google Health or Microsoft HealthVault, are used through the internet to actively involve patients in their self-care. Patients prefer these services since they provide a safe and free place to organize their personal records.17 Also, both servers contain links to other online health services to get extra support for patients or their relatives. Several websites have been developed for patients with diabetes. Some examples are: ADA (diabetes.org), ASweetLife.org, BehavioralDiabetesInstitute.org, ChildrenwithDiabetes.com, DiabetesDad.org, DiabetesMine.com, Diatribe.org, dLife.com, Fit4D.com, Insulindependence.org, JDRF.org, Joslin.org, MayoClinic.com, Mendosa.com, QuantiaMD.com, WebMD.com, Social Communities, DiabetesSisters.org (female-specific), DiabeticConnect.com, DiabetesDaily.com, EstuDiabetes (Spanish) SocialDiabetes (insulin users, Spanish), MyGlu.org (type 1 diabetes-specific), Juvenation.org (type 1 diabetes-specific), PatientsLikeMe.com (various disease states), TypeOneNation.org (type 1 diabetes-specific), and TuDiabetes.org among others. In addition, a growing number of blogs and forums are available worldwide.
Software
Nightscout Project is a software targeting patients with type 1 diabetes, which was created by a father of a 4-year-old boy who was newly diagnosed. This patient required a continuous glucose monitoring system (CGMS) that would provide interstitial glucose readings every 5 mins. The challenge was to monitor him while he was at school; therefore, his father developed a computer code that would enable him access to the blood glucose readings from the CGMS receiver to the computing cloud through a smartphone. This tool has received positive feedback when patients and their families get involved, as they provide initiatives, create tools, and provide relevant information about their daily issues and concerns.23 This software is relevant since: 1) reflects the autonomy of patients and their caregivers to design and create their own technologies for self-care; 2) reveals an opportunity area for the creation of products or tools through the use of technology and; and 3) reflects the importance of teamwork through patients who provide their knowledge about their daily problems and time to improve the software virtually.23
Mobile apps
Approximately, 77% of adults in the US have access to a smartphone, and more than 50% of smartphone owners use their device to obtain health information. Chavez et al used the Mobile App Rating Scale to evaluate which mobile apps were most adequate for self-care in diabetes. They evaluated four parameters (engagement, functionality, aesthetics, and information), and included the number of diabetes management tasks incorporated in each app. Unfortunately, the score that each app received did not reflect the impact on behavioral changes. This suggests that a clinical evaluation of apps for self-care in diabetes could be an area of opportunity to explore.24
Telemedicine
Telemedicine is another important resource. In the US, the Informatics for Diabetes Education and Telemedicine (IDEATel) Project installed telemedicine units in cultural diverse centers and nursing homes to offer videoconferences focused on various aspects of diabetes. The aim was helping participants to establish a self-care plan and setting goals. They obtained positive results in increasing self-care and improving glycemic control, but not in blood pressure and lipid levels.25
Integration of techniques and tools in empowerment programs
There is a worldwide consensus that the best practice for reducing the frequency of diabetes complications is through self-care.22 Specific tasks (as proposed by the ADA) should be developed for diabetes knowledge (ie, the nutritional plan, physical activity, medication, self-monitoring, actions in sickness days and feelings or stage of behavioral change, among others). All these actions are directed to reach active participation of patients in their glucose control, promoting lifestyle changes for a better quality of life. Although goals are similar worldwide, major differences exist between programs due to the population’s profile and available resources. In the following lines, some examples of empowerment programs are described.
In Chile, a group of researchers assessed the efficacy of an education program for patients with type 2 diabetes in a primary setting. This program had a duration of 12 months and included the cognitive, emotional, and life aspects, organized in six basic units plus two complementary sections. The program was applied in 90-min group sessions, once a week, with eight participants per session, supervised by a trained educator. They compared the intervention with a control group receiving standard of care. All participants had a baseline assessment with follow-up visits every 4 months (including body mass index, blood pressure, HbA1c, and lipid profile). The intervention resulted in a greater HbA1c decrement compared to the reference group.26
In Mexico, the “Integral Diabetes Management by Stages” Program (MIDE) developed by the Instituto de Seguridad y Servicios Sociales de los Trabajadores del Estado (ISSSTE) was launched in 2007. It focuses on the development of cognitive-behavioral skills and training, promoting the active participation of patients, their families and a multidisciplinary health team (including staff and institutions). The MIDE program was designed to operate in primary care units. It is based on three strategies: 1) innovation and improvement of primary care; 2) promote empowerment; and 3) provide training to health professionals. The MIDE program has shown that patients with diabetes who participated improved their glucose, HbA1c, total cholesterol, and triglyceride levels.27
The Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán developed the “Center for Integrated Attention for Patients with Diabetes – CAIPaDi”. It is composed by nine structured interventions implemented in a single visit by a multidisciplinary team. Patients free of chronic complications, with a time since diagnoses lower than 5 years, were selected as the target population of the program. Empowerment was considered as a prime goal of the CAIPaDi program. Standardized protocols focused in self-efficacy and co-responsibility were applied. The program also includes elements of the chronic disease care model, such as the use of procedure manuals and treatment algorithms based on available resources, use of an electronic registry system, and evaluation of quality indicators of medical care.28 The program consists of two phases. The first phase consists of four monthly visits. In each visit, 10 health care providers treat patients following specific protocols. All interventions take place in a single shift of 7 hrs. The nine interventions are: medical care, diabetes education, diet, physical activity, psychological evaluation, psychiatric assessment, eye exam, foot care, and dental care. The interventions are delivered by one nurse, two endocrinologists, one diabetes educator, one nutritionist, one ophthalmologist, one psychologist, a psychiatrist, a physical activity instructor, and a dentist. Each intervention was implemented using a procedure manual; every session has a specific goal, a self-management strategy and pre-specified indicators. Each session is 30–60 mins long; some of them are group meetings in which a pre-designed dynamic is executed. The second phase of the CAIPaDi program is composed byannual visits in which all interventions of the initial phase are reinforced. During the annual visits, pre-specified outcomes are measured. A continuous at-distance support system was implemented to maintain communication with the patients using emails, phone calls, text messages, and a webpage (http://innsz.mx/opencms/contenido/departamentos/CAIPaDi/). More than 1000 patients have participated in this program, reflecting a remarkable impact on metabolic outcomes, empowerment, anxiety, depression, and quality of life.29
Measurement of empowerment
According to the ADA, there are four critical times to evaluate the need for diabetes self-management education and support: at diagnosis, annually, when complicating factors arise, and when transitions in care occur. Clinical outcomes, health status, and quality of life are key goals of diabetes self-management education and support that should be measured as part of routine care.3 Commonly used empowerment evaluation strategies are the Diabetes Empowerment Scale (DES) instrument and the Problem Areas in Diabetes (PAID) Scale.19 The DES scale is one of the surveys developed by the Michigan Diabetes Research Center, which has contributed with several survey instruments for diabetes patients and health professionals. Both of these instruments evaluate specific aspects of empowerment, being useful for guiding patients, although they do not evaluate empowerment as a whole, covering knowledge, skills, critical thinking, autonomy, aptitudes, and attitudes.
The DES was developed in 2000 to measure the psychosocial self-efficacy of people with diabetes. Originally it consisted of 37 items representing eight conceptual dimensions. The current questionnaire was reduced to 28 items using factor analyses (DES alpha=0.96 of reliability). It comprises three subscales: 1) managing the psychosocial aspects of diabetes; 2) assessing dissatisfactions and readiness to change; and 3) setting and achieving goals. A short version of the DES (DES-SF) is also available with a reliability of alpha=0.85 using the original dataset. The content of the DES-SF was validated in a study performed by Anderson et al, showing that both DES-SF scores and HbA1c levels changed in a positive direction after 229 subjects completed a 6-week problem-based patient education program. These data provided preliminary evidence about the DES-SF as a valid and reliable measure of overall diabetes-related psychosocial self-efficacy.30,31
There are sensitive instruments for specific disease symptoms and complications such as the PAID Scale. The PAID Scale was developed by the Joslin Diabetes Center in Boston. This scale has been specifically developed to evaluate patient’s perspectives on the current emotional burden of diabetes and its treatment. The PAID, developed in 199532 is a self-report questionnaire that contains 20 items that describe negative emotions related to diabetes (eg, fear, anger, frustration), commonly experienced by patients with diabetes. Completion takes approximately 5 mins (https://www.huskyhealthct.org/providers/provider_postings/diabetes/PAID_problem_areas_in_diabetes_questionnaire.pdf). The questionnaire is valuable as a clinical tool, as an outcome measurement to identify diabetes-related emotional distress, and to assess psychological adjustment to diabetes.33 In a meta-analysis by Aquino et al, PAID was the second most frequently used scale (36.4%).19
To determine the validity of the surveys used, some parameters such as knowledge about the disease, quality of life, and biochemical variables (HbA1c, cholesterol) have been evaluated. Generally, the most common parameter is the HbA1c reduction after follow-up.19
Studies evaluating empowerment interventions
Multiple studies have measured the short- and long-term effect of empowerment-based interventions in patients with diabetes. A summary of the outcomes modified by empowerment programs is presented in Table 2. Ebrahimi et al, in a randomized clinical trial, evaluated the effect of an empowerment program in metabolic control of patients with type 2 diabetes (n=106). The empowerment program included the recommendations of the ADA for diet, exercise, medications, and foot care. The program was implemented by two nurses in collaboration with an endocrinologist and a nutritionist in groups of 10 patients in 5–7 weekly meetings. In each session, patients’ knowledge was evaluated by two questions regarding the theme learned in the previous session. At the beginning of the study, the mean HbA1c was 8.1% and 3 months after the intervention patients in the program demonstrated the improvement of metabolic variables, including HbA1c (mean difference 0.86%), glucose, triglycerides, cholesterol, and HDL when compared with the control group.34
 |
Table 2 Outcomes positively impacted by self-management interventions based on empowerment |
In another study, two diabetes self-management interventions (extended and compressed) designed for Mexican Americans were evaluated in 216 individuals with type 2 diabetes. The extended intervention consisted of 1 year series of 12-weekly sessions regarding nutrition, glucose monitoring, physical activity, among other topics, followed by 14 support group sessions to promote behavioral change through problem-solving and goal setting. The compressed intervention involved 8 weekly educational sessions followed by support sessions at 3, 6, and 12 months. Both interventions demonstrated being effective in reducing HbA1c (1-year change −0.6% and –1.7% in the compressed and extended group, respectively) for those who attended ≥50% of the sessions. Attendance to the sessions was associated with greater knowledge levels at 12 months and knowledge was positively related to the number of hours of attendance.35
In a systematic review including 72 randomized, controlled clinical trials, the effectiveness of self-management training in patients with type 2 diabetes was demonstrated in a large proportion of the studies. The majority of the studies showed improvement in diabetes knowledge; regular reinforcement improved marks obtained in the pre-specified variables. Many of the studies documented an increased frequency of blood glucose self-monitoring in patients receiving self-management interventions. Studies that examined interventions focusing on foot lesions showed mixed results with a decrease in foot ulcers and amputations in some of them. Most studies that examined changes in diet reported a positive change in different aspects, except for two studies that did not show any improvement. Change in physical activity did not show a consistent effect of education interventions. Regarding other outcomes, 13 studies showed an effect in decreasing weight (average 2 kg, range from 1.3 to 3.1). Some studies evaluating total cholesterol levels, LDL cholesterol, and HDL cholesterol showed an improvement associated with the intervention. However, this effect was not consistent. Studies exploring blood pressure also showed mixed results with some of them demonstrating a decrease in systolic and diastolic blood pressure. Finally, only a couple of studies explored cardiovascular events or mortality; none of them demonstrated an effect of the interventions. Educational interventions that involve patient collaboration may be more effective than didactic interventions in improving glycemic control, weight, and lipid profiles.36
A meta-analysis specifically explored the effect of DSME in HbA1c. Authors classified educational approach as didactic when the patient did not interact in the sessions or collaborative when the patient has an active participation (group discussions, empowerment, and goal-setting). The collaborative interventions decreased HbA1c by 0.76% (95% CI 0.34–1.18) at immediate follow-up, 0.26% (0.21% increase to 0.73% decrease) at 1–3 months of follow-up and 0.26 (0.05–0.48) at ≥4 months of follow-up. Duration of contact time between educator and patient was the only significant predictor of the effect.37 Small, non-significant effects were observed in the studies in which a didactic approach was applied.
In another meta-analysis including 26 randomized clinical controlled trials (n=2833), the effect of group-based DSME compared to routine treatment was assessed in patients with type 2 diabetes. The length of the trials was 6 months for 8 of the trials, 12 months for 11, and 2 years for 2. Authors concluded that group-based DSME results in improvements in clinical, lifestyle, and psychosocial outcomes. At baseline, the average HbA1c in the intervention and control groups were similar (8.31±1.83 and 8.16±1.76, respectively). In 13 studies (n=1827) after 6 months of the intervention, the HbA1c was reduced 0.44% (95% CI −0.69 to –0.19, p=0.00006). In 11 studies (n=1503) with a follow-up of 12 months, the HbA1c was reduced by 0.46% (95% CI –0.74 to –0.18, p=0.001). Three studies (n=397) demonstrated a reduction of 0.87% (95% CI 1.25 to –0.49, p<0.0000) in HbA1c at 2 years in patients assigned to DSME. One study included in the meta-analysis also evaluated HbA1c at 4 and 5 years of follow-up finding also a significant reduction of –1.6% and –1.7%, respectively.
Regarding diabetes knowledge (n=768, six studies) the intervention resulted in improvement at 6 months (standardized mean difference [SMD] 0.83, 95% CI 0.67–0.99, p<0.00001). In two studies (n=333), diabetes knowledge improved at 12 months (SMD 1.03, 95% CI 0.8–1.26, p<0.00001). Two studies (n=355) showed significant better knowledge in the intervention group at 2 years (SMD 2.31, 95% CI 1.99–2.64, p<0.00001 and SMD 0.86, 95% CI 0.47–1.24, p=0.0001, respectively). Finally, one study that evaluated diabetes knowledge at 4 and 5 years found that the improvement persisted in patients allocated to the DSME.
Self-management skills also improved at 6 months (SMD 0.29, 95% CI 0.11–0.46, P=0.002). Only one study explored the effect on diabetes complications (diabetic retinopathy and foot ulcers) and found that diabetic retinopathy progressed slower in participants assigned to DSME (P<0.009). In a sub-analysis, the interventions delivered by a single educator, in <10 months, with more than 12 hrs and between 6 and 10 sessions were associated with better results.38
Unmet needs in empowerment of patients with diabetes
Despite the well-recognized prominent role of empowerment in diabetes care, it is not routinely implemented in many centers. In addition, in some instances, the implementation process is not standardized and it depends on the experience and enthusiasm of the health team. The process is rarely started by the patient’s request, because there is a limited understanding of the complexity of the disease in many societies. On the other hand, surveillance of the performance of health systems does not include indicators of the empowerment process; if available, data is limited to quantitative information (eg, number of participants).
There is a need for having simple and comprehensive indicators to measure the implementation of empowerment process and its long-term effect on self-care behaviors. The lack of widely accepted indicators has several adverse consequences. The impact of empowerment is not considered in cost-effectiveness analyses; as a result, health systems do not have evidence to fund the empowerment programs. In the long term, methodologic issues limit the ability of researchers to identify the diabetes-related outcomes (ie, amputations, severe hypoglycemia, among others) that could be modified by empowerment programs. Conflicting results and paradoxical conclusions (ie, higher cost of care without changes in attainment of treatment goals) are other potential consequences of the imprecise assessment of the empowerment process.
On the other hand, health professionals should identify the potential barriers that may interfere with the induction of empowerment. As stated by Ahola and Groop,39 there are individual- and environmental-related aspects that interfere with patient’s empowerment and their own management of diabetes. They will face challenges, including advanced age, memory loss, depression, and anxiety.39 Also, the environment will limit their ability to accomplish self-care practices. Factors to be explored are limitations in the access to health care, social and family support, cultural and socioeconomic factors. There is a need for having tools and algorithms that help health professionals to identify and solve potential barriers before the empowerment process is attempted.
In addition, empowerment is a continuous process that requires periodic reinforcement. Despite there are many tools and approaches to support it, there is a need for randomized studies designed to identify the best strategies to be applied, considering cost, affordability, and simplicity. Since this process is time-consuming, it is unlikely that it could be developed during a regular visit at a primary care clinic. On the side of the health care providers, optimization of medical visits to improve quality and focus in the patient needs must be addressed. Furthermore, effective communication must be encouraged.40
In order to achieve a better comprehension of the disease and to enroll the patient in their own care, public health policies must be revised and updated. In many countries, health systems continue using a model of care for type 2 diabetes that was developed in the 1940s (adequate for acute infectious diseases).40 To date, there are still important information gaps that must be addressed. More and better research must be performed worldwide. To date, no studies have demonstrated the effectiveness of self-management training on cardiovascular disease-related events or mortality; no economic analyses included indirect costs and few studies examined health care utilization.19,41,42 Also, it is uncertain if the inclusion of a close relative in the sessions has a positive effect on the empowerment process.
Opportunity areas for empowerment implementation
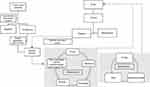
Based on the above, an algorithm for patient empowerment is proposed in Figure 1. The initial step is to assess the patient’s profile and the current motivation stage (pre-contemplation, contemplation, preparation, action, or maintenance). If the target subject is not prepared to take action, the participation of a potential ally (among close relatives or friends) and/or exchange of experiences with other cases that already have diabetes-related outcomes may be considered. The help of psychologist or a therapist must be considered. Potential barriers should be identified and solved (as much as possible) before the empowerment program is started. The systematic use of questionnaires (ie, PAID or DES) may be helpful to standardize the initial assessment. If a positive attitude is achieved and the major barriers are identified, patients could be included in the DSMES module. Otherwise, the participation of the patient should be reconsidered; they should receive information about the self-care activities that are needed and how they could contribute to achieve the best possible care of their disease. The implementation of the DSMES module should be in accordance with a procedure manual; every session should have predefined goals and activities. Attitudes, beliefs, and knowledge should be measured as many times as needed to assess the impact of the intervention. A multidisciplinary team along with the social partners of the patient should participate in this process. A reinforcement plan should be added, as soon as the main self-care behaviors are incorporated in the patient daily routine. Because relapse is common, health professionals should explore in every visit the quality and quantity of the self-care activities.
Factors affecting adherence differ between populations and patient’s profiles.43 Therefore, it is essential to consider individual characteristics to tailor knowledge and empowerment strategies.44 There are several factors influencing adherence that must be considered when implementing empowering strategies in patients with diabetes. Variables that correlate with adherence behaviors in diabetes can be organized into four clusters:2
- Treatment and disease characteristics, including treatment complexity, duration of the disease, and delivery of care
- Intra-personal factors: age, gender, self-esteem, self-efficacy, stress, depression, and alcohol abuse
- Inter-personal factors: quality of relationships between patients and providers, and social support
- Environmental factors: high-risk situations and environmental factors
Physicians should be catalysts in the empowerment process. However, they should be aware of the multiple challenges that they will face. They are responsible for prescribing the optimal medications, completing necessary tests and procedures, and providing guidance in relevant treatment areas. But in real life, patients are responsible for implementing the often-complicated treatment recommendations over a sustained period of time (“self-management”) (Table 3).45 Trained nurses, diabetes educators, empowered patients, and family members can also support empowerment.46 First, contact is always a unique opportunity to engage the patient. Every interaction between patients and health professionals is an opportunity to empower. Hospital stays are unique opportunities to provide information and incorporate it in the daily life. Also, the waiting room (with the use of videos, posters, or audios) may be a place to start the process.47
 |
Table 3 Health professional and patient roles |
Communication skills should be developed by health professionals in order to be effective.48 Health care professionals who aim to use empowerment should continuously reflect about these questions:46
- Do I help patients to identify and address their primary diabetes concerns?
- Do I encourage them to talk about the emotional aspects of having diabetes?
- Do I help them identify and choose goals that are relevant and important for them?
- Do I respect their right to make decisions with which I disagree?
A single intervention is not enough to manage diabetes effectively for a lifetime or to sustain the gains made through education. Ongoing self-management education support, including problem-solving and shared decision-making skills development is a continuous process.49
Conclusion
Diabetes is a complex and burdensome disease that requires the individual with diabetes to make numerous daily decisions regarding food, physical activity, and medications. It also requires patient’s proficiency in a number of self-management skills.50 Patient empowerment is a continuous process in which knowledge, motivation, and capacity to take control of their disease are built within a person. Health professionals should be aware of the skills and tools that they should have in order to induce and support empowerment. There is no standardized method to help patients become empowered; implementation should consider the target population profile. The process will face multiple obstacles that should be foreseen. In the same manner, there are no tools to evaluate empowerment outcomes as a whole, but different resources are available to evaluate specific components of empowerment separately, such as the psychosocial aspects.51 If health care professionals are aware and knowledgeable about empowerment techniques, they will be able to apply them adequately, personalize their attention (eg, according to their socioeconomic situation), and begin a change within the model of attention. Health systems should consider its inclusion in every effort to improve the quality of care.
Disclosure
The authors report no conflicts of interest in this work.
References
1. McAllister M, Dunn G, Payne K, Davies L, Todd C. Patient empowerment: the need to consider it as a measurable patient-reported outcome for chronic conditions. BMC Health Serv Res. 2012;12:157. doi:10.1186/1472-6963-12-157
2. Adherence to Long-term Theraphies. Evidence for Action. World Health Organization; Geneva:2003.
3. Powers MA, Bardsley J, Cypress M, et al. Diabetes self-management education and support in type 2 diabetes: a joint position statement of the American Diabetes Association, the American Association of Diabetes Educators, and the academy of nutrition and dietetics. Clin Diabetes. 2016;34(2):70–80. doi:10.2337/diaclin.34.2.70
4. American Diabetes A. 5. Lifestyle management: standards of medical care in diabetes-2019. Diabetes Care. 2019;42(Suppl 1):S46–S60. doi:10.2337/dc19-S005
5. Page N. Empowerment: what is it?. J Extension. 1999;37(5):1–5.
6. Wallerstein N. Powerlessness, empowerment, and health: implications for health promotion programs. Am J Health Promot. 1992;6(3):197–205. doi:10.4278/0890-1171-6.3.197
7. Anderson RM, Funnell MM. Patient empowerment: myths and misconceptions. Patient Educ Couns. 2010;79(3):277–282. doi:10.1016/j.pec.2009.07.025
8. Scambler S, Newton P, Asimakopoulou K. The context of empowerment and self-care within the field of diabetes. Health (London). 2014;18(6):545–560. doi:10.1177/1363459314524801
9. Health Promotion Glossary. World Health Organization; Geneva:1998.
10. Funnell MM, Anderson RM, Arnold MS, et al. Empowerment: an idea whose time has come in diabetes education. Diabetes Educ. 1991;17(1):37–41. doi:10.1177/014572179101700108
11. Powers TL, Bendall D. Improving health outcomes through patient empowerment. J Hosp Mark Public Relations. 2003;15(1):45–59.
12. Luczynski W, Glowinska-Olszewska B, Bossowski A. Empowerment in the treatment of diabetes and obesity. J Diabetes Res. 2016;2016:1–9. 5671492. doi:10.1155/2016/5671492
13. El Autocuidado En Las Personas Con Enfermedad Crónica. 2015.
14. Meetoo Danny HG. Empowerment: giving power to people with diabetes. J Diabetes Nurs. 2005;9(1):28–32.
15. Funnell MM, Brown TL, Childs BP, et al. National standards for diabetes self-management education. Diabetes Care. 2011;34(Suppl 1):S89–S96. doi:10.2337/dc11-S089
16. Driscoll KA, Young-Hyman D. Use of technology when assessing adherence to diabetes self-management behaviors. Curr Diab Rep. 2014;14(9):521. doi:10.1007/s11892-014-0475-3
17. Jacob S, Serrano-Gil M. Engaging and empowering patients to manage their type 2 diabetes, Part II: initiatives for success. Adv Ther. 2010;27(10):665–680. doi:10.1007/s12325-010-0071-0
18. Devchand R, Nicols C, Gallivan JM, et al. Assessment of a National Diabetes Education Program diabetes management booklet: the GRADE experience. J Am Assoc Nurse Pract. 2017;29(5):255–263. doi:10.1002/2327-6924.12445
19. Aquino JA, Baldoni NR, Flor CR, et al. Effectiveness of individual strategies for the empowerment of patients with diabetes mellitus: a systematic review with meta-analysis. Prim Care Diabetes. 2018;12(2):97–110. doi:10.1016/j.pcd.2017.10.004
20. Simmons D, Gamble GD, Foote S, Cole DR, Coster G, New Zealand Diabetes Passport S. The New Zealand Diabetes Passport Study: a randomized controlled trial of the impact of a diabetes passport on risk factors for diabetes-related complications. Diabet Med. 2004;21(3):214–217.
21. Wallace AS, Seligman HK, Davis TC, et al. Literacy-appropriate educational materials and brief counseling improve diabetes self-management. Patient Educ Couns. 2009;75(3):328–333. doi:10.1016/j.pec.2008.12.017
22. Liang X, Wang Q, Yang X, et al. Effect of mobile phone intervention for diabetes on glycaemic control: a meta-analysis. Diabet Med. 2011;28(4):455–463. doi:10.1111/j.1464-5491.2010.03180.x
23. Lee JM, Hirschfeld E, Wedding J. A patient-designed do-it-yourself mobile technology system for diabetes: promise and challenges for a new era in medicine. JAMA. 2016;315(14):1447–1448. doi:10.1001/jama.2016.1903
24. Chavez S, Fedele D, Guo Y, et al. Mobile apps for the management of diabetes. Diabetes Care. 2017;40(10):e145–e146. doi:10.2337/dc17-0853
25. Starren J, Hripcsak G, Sengupta S, et al. Columbia University’s Informatics for Diabetes Education and Telemedicine (IDEATel) project: technical implementation. J Am Med Inform Assoc. 2002;9(1):25–36. doi:10.1136/jamia.2002.0090025
26. Bachler R, Mujica V, Orellana C, et al. Effectiveness of a structured educative program in Chilean diabetic patients. Rev Med Chil. 2017;145(2):181–187. doi:10.4067/S0034-98872017000200005
27. Blanco-Cornejo M. New model for diabetes primary health care based on patient empowerment and the right to preventive health: the MIDE program. Rev Panam Salud Publica. 2017;41:e128.
28. Hernandez-Jimenez S, Garcia-Ulloa C, Mehta R, Aguilar-Salinas CA, Kershenobich-Stalnikowitz D. Innovative models for the empowerment of patients with type 2 diabetes: the CAIPaDi program. Recent Pat Endocr Metab Immune Drug Discov. 2014;8(3):202–209.
29. Hernandez-Jimenez S, Garcia-Ulloa AC, Bello-Chavolla OY, Aguilar-Salinas CA, Kershenobich-Stalnikowitz D; Group of Study C. Long-term effectiveness of a type 2 diabetes comprehensive care program. The CAIPaDi model. Diabetes Res Clin Pract. 2019;151:128–137. doi:10.1016/j.diabres.2019.04.009
30. Tools for Health Professionals. Available from: http://diabetesresearch.med.umich.edu/Tools_SurveyInstruments.php#des.
31. Anderson RM, Funnell MM, Fitzgerald JT, Marrero DG. The Diabetes Empowerment Scale: a measure of psychosocial self-efficacy. Diabetes Care. 2000;23(6):739–743. doi:10.2337/diacare.23.6.739
32. Polonsky WH, Anderson BJ, Lohrer PA, et al. Assessment of diabetes-related distress. Diabetes Care. 1995;18(6):754–760. doi:10.2337/diacare.18.6.754
33. Papathanasiou A, Koutsovasilis A, Shea S, et al. The Problem Areas in Diabetes (PAID) scale: psychometric evaluation survey in a Greek sample with type 2 diabetes. J Psychiatr Ment Health Nurs. 2014;21(4):345–353. doi:10.1111/j.1365-2850.2012.01875.x
34. Ebrahimi H, Sadeghi M, Amanpour F, Vahedi H. Evaluation of empowerment model on indicators of metabolic control in patients with type 2 diabetes, a randomized clinical trial study. Prim Care Diabetes. 2016;10(2):129–135. doi:10.1016/j.pcd.2015.09.003
35. Brown SA, Blozis SA, Kouzekanani K, Garcia AA, Winchell M, Hanis CL. Dosage effects of diabetes self-management education for Mexican Americans: the starr county border health initiative. Diabetes Care. 2005;28(3):527–532. doi:10.2337/diacare.28.3.527
36. Norris SL, Engelgau MM, Narayan KM. Effectiveness of self-management training in type 2 diabetes: a systematic review of randomized controlled trials. Diabetes Care. 2001;24(3):561–587. doi:10.2337/diacare.24.3.561
37. Norris SL, Lau J, Smith SJ, Schmid CH, Engelgau MM. Self-management education for adults with type 2 diabetes: a meta-analysis of the effect on glycemic control. Diabetes Care. 2002;25(7):1159–1171. doi:10.2337/diacare.25.7.1159
38. Steinsbekk A, Rygg LO, Lisulo M, Rise MB, Fretheim A. Group based diabetes self-management education compared to routine treatment for people with type 2 diabetes mellitus. A systematic review with meta-analysis. BMC Health Serv Res. 2012;12:213. doi:10.1186/1472-6963-12-213
39. Ahola AJ, Groop PH. Barriers to self-management of diabetes. Diabet Med. 2013;30(4):413–420. doi:10.1111/dme.12105
40. Arredondo A. Type 2 diabetes and health care costs in Latin America: exploring the need for greater preventive medicine. BMC Med. 2014;12:136. doi:10.1186/s12916-014-0141-2
41. Barcelo A, Arredondo A, Gordillo-Tobar A, Segovia J, Qiang A. The cost of diabetes in Latin America and the Caribbean in 2015: evidence for decision and policy makers. J Glob Health. 2017;7(2):020410. doi:10.7189/jogh.07.020410
42. Cusi K, Ocampo GL. Unmet needs in Hispanic/Latino patients with type 2 diabetes mellitus. Am J Med. 2011;124(10 Suppl):S2-9. doi:10.1016/j.amjmed.2011.07.017
43. Polonsky WH, Henry RR. Poor medication adherence in type 2 diabetes: recognizing the scope of the problem and its key contributors. Patient Prefer Adherence. 2016;10:1299–1307. doi:10.2147/PPA.S106821
44. Chen J, Mullins CD, Novak P, Thomas SB. Personalized strategies to activate and empower patients in health care and reduce health disparities. Health Educ Behav. 2016;43(1):25–34. doi:10.1177/1090198115579415
45. Heisler M. Actively engaging patients in treatment decision making and monitoring as a strategy to improve hypertension outcomes in diabetes mellitus. Circulation. 2008;117(11):1355–1357. doi:10.1161/CIRCULATIONAHA.108.764514
46. Patient Empowerment-Living with Chronic Disease.
47. Brown MT, Bussell JK. Medication adherence: WHO cares? Mayo Clin Proc. 2011;86(4):304–314. doi:10.4065/mcp.2010.0575
48. An inquiry into patient centred care in the 21st century. 2014.
49. Beebe CA. Engaging patients in education for self-management in an accountable care environment. Clin Diabetes. 2011;29(3):123–126. doi:10.2337/diaclin.29.3.123
50. Haas L, Maryniuk M, Beck J, et al. National standards for diabetes self-management education and support. Diabetes Care. 2012;35(11):2393–2401. doi:10.2337/dc12-1707
51. Sigurdardottir AK, Jonsdottir H. Empowerment in diabetes care: towards measuring empowerment. Scand J Caring Sci. 2008;22(2):284–291. doi:10.1111/j.1471-6712.2007.00506.x
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.