Back to Journals » Drug Design, Development and Therapy » Volume 13
Efficacy of a fixed dose combination of irbesartan and atorvastatin (Rovelito®) in Korean adults with hypertension and hypercholesterolemia
Authors Ihm SH , Shin J , Park CG, Kim CH
Received 24 October 2018
Accepted for publication 4 January 2019
Published 13 February 2019 Volume 2019:13 Pages 633—645
DOI https://doi.org/10.2147/DDDT.S191973
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Tuo Deng
Sang-Hyun Ihm,1 Jinho Shin,2 Chang-Gyu Park,3 Cheol-Ho Kim4
1Division of Cardiology, Department of Internal Medicine, College of Medicine, The Catholic University of Korea, Seoul, South Korea; 2Department of Internal Medicine, Hanyang University College of Medicine, Seoul, South Korea; 3Cardiology Division, Korea University Guro Hospital, Seoul, South Korea; 4Department of Internal Medicine, College of Medicine, Seoul National University, Seoul National University Bundang Hospital, Seongnam-si, South Korea
Purpose: Coexistence of hypertension (HTN) and hypercholesterolemia is a major synergistic and modifiable risk factor for cardiovascular disease (CVD). Thus, a fixed-dose combination (FDC) of anti-HTN drugs and statins may be useful for treating CVD. This study evaluated the efficacy of an FDC of irbesartan and atorvastatin (Rovelito®) in Korean patients.
Patients and methods: Patients with HTN and hypercholesterolemia were screened for this prospective, observational, descriptive, multi-center, phase IV study. Eligible patients were administered with Rovelito for 3 months. Dose adjustment was allowed based on the physician’s discretion. Blood pressure (BP) goal was <140/90 mmHg, and blood lipid goal was based on Adult Treatment Panel III. Compliance with therapeutic lifestyle modification and safety of the study drugs were evaluated.
Results: Of the 2,777 patients enrolled in this study, 931 were analyzed for clinical efficacy. BP and low-density lipoprotein cholesterol (LDL-C) goals were achieved in 801 (86.04%) and 797 (85.61%) patients, respectively. For the BP goal, higher baseline BP and higher body mass index were risk factors for treatment failure. For LDL-C goal, baseline LDL-C level, number of concomitant drugs, smoking status, and alcohol consumption were risk factors for treatment failure. Of the 931 participants, 694 (74.54%) achieved the treatment goals for both BP and LDL-C. Smoking status, alcohol consumption, number of concomitant drugs, and higher baseline LDL-C and BP levels were risk factors for treatment failure in both BP and LDL-C goals. Adherence with Rovelito was 97.90%±5.79%, and incidence of adverse events was 4.19% (116).
Conclusion: FDC of irbesartan and atorvastatin (Rovelito) could be extremely helpful in treating patients with both HTN and hypercholesterolemia. Poor metabolic profiles were risk factors for poor treatment response and the reason for choosing Rovelito. Therapeutic lifestyle modification should still be underscored despite the 75% treatment success rate with Rovelito for both conditions.
Keywords: hypertension, hypercholesterolemia, fixed-dose combination, irbesartan, atorvastatin
Introduction
Cardiovascular diseases (CVD) have become one of the most important health issues worldwide. Hypertension (HTN) and dyslipidemia are the two major contributing and modifiable risk factors for CVD.1,2 The co-existence of the two risk factors has additive effects on the blood vessels, which results in enhanced atherosclerosis, and thereby leads to CVD and coronary heart disease (CHD).3,4 A recent large epidemiological study with a long follow-up demonstrated a remarkable positive association between blood pressure (BP) and the risk of CHD death in patients with higher total cholesterol levels.5 Furthermore, co-existence of HTN and hypercholesterolemia substantially increases the risk of CVD events compared with the presence of only one of these risk factors.6
Previous epidemiological studies in the United States have shown that the prevalence of HTN and hypercholesterolemia is 15%–31%.7,8 A large-scale retrospective study demonstrated that the prevalence of HTN (17.6%) is greater than that of dyslipidemia (12.3%), with HTN and dyslipidemia comorbidities found in 8.0% of the population.9 Moreover, among hypertensive patients, 45.2% had dyslipidemia and 64.9% of dyslipidemia patients had comorbid HTN.9 Additionally, 36% of hypertensive patients and 20% of dyslipidemia patients received pharmacologic treatment for their conditions, while 65% and 61% of patients with comorbidities received pharmacologic treatment only for HTN and dyslipidemia, respectively.
Despite the relatively higher treatment rate, the control rate of dyslipidemia or HTN was low. The control rates of patients with dyslipidemia only, HTN only, and both diseases were 7%, 15%, and 17%, respectively.9 Recent guidelines for HTN favor the use of a combination of two or more antihypertensive drugs at fixed doses in a single tablet because reducing the number of pills administered daily improves adherence, which in turn increases the rate of BP control.10,11 Such rationale could also be applied to patients with HTN with concomitant dyslipidemia, diabetes mellitus, CVD, and obesity. After the development of a single-pill combination of amlodipine and atorvastatin, this combination therapy became available and was shown to be efficacious and well-tolerated for the simultaneous treatment of HTN and hypercholesterolemia in clinical practice.12 Several fixed dose combinations (FDCs) of antihypertensive drugs and statins have been developed and prescribed. Renin–angiotensin system (RAS) blockers are effective in preventing CVD and angiotensin receptor blockers (ARB) are more advantageous for Asians patients as dry cough, an adverse effect of angiotensin converting enzyme (ACE) inhibitors was not observed in these patients.13 In addition, treating patients with type 2 DM, HTN, and overt nephropathy using irbesartan was both a cost-effective and life-saving strategy compared to the use of amlodipine and standard antihypertensive treatment.14 Hence, an FDC of irbesartan and atorvastatin (Rovelito®, Hanmi Pharmaceutical Co., Ltd., Seoul, Korea) could be useful for preventing CVD. A previous retrospective study9 demonstrated that several baseline characteristics, such as age, DM, smoking, CVDs, and family history of CHD affect treatment and control rates of HTN and dyslipidemia comorbidities.9 Most importantly, poor compliance should be overcome to improve the control rate in patients with both HTN and dyslipidemia. An FDC of ARBs and statins can be a useful option to improve compliance. Moreover, there are only a few studies showing the efficacy of FDC of ARB plus statins and evaluating risk factors affecting the control rate of patients with both HTN and dyslipidemia.6,8,12,15
Thus, this prospective observational study aimed to evaluate the efficacy of the FDC drug Rovelito in real-world clinical practice and identify how the overall clinical factors including medication status influenced the achievement of BP and/or low-density lipoprotein cholesterol (LDL-C) goal among Korean patients with both HTN and hypercholesterolemia.
Patients and methods
Study design and patient recruitment
This prospective, observational, descriptive, multi-center, phase IV study was conducted in 74 centers (56 hospitals and 11 clinics) in Korea from February 2014 to May 2016. Patients with both HTN and hypercholesterolemia and aged ≥19 years were eligible. Exclusion criteria were acute liver disease or hepatic dysfunction (aspartate aminotransferase or alanine aminotransferase levels ≥3 times the normal upper limit); elevated serum creatinine level (≥2.5 mg/dL); creatinine phosphokinase level >2 times the normal upper limit; elevated serum triglycerides (≥500 mg/dL); hypersensitivity to hydroxymethylglutaryl coenzyme A reductase inhibitors; uncontrolled HTN (SBP ≥180 mmHg or DBP ≥110 mmHg measured at rest, with antihypertensive medication); uncontrolled DM; current treatment with any type of lipid-lowering drugs; diagnosis or risk of myopathy (renal impairment or previous renal dysfunction, hypothyroidism, genetic defects or family history of myopathy, experienced muscle toxicity with statins or fibrates, prior liver disease, or high alcohol consumption); pregnant and breastfeeding women; adequate methods of contraception not being used by women (including those of childbearing potential); contraindications for participant; legal reasons for not participating or inability to participate based on the investigator’s decision; and concomitant drug therapy that could interact with the study drug.
Patients who underwent baseline evaluation and met the eligibility criteria were enrolled. The enrolled patients were treated with Rovelito and followed-up by normal clinical practice. The dosage was varied from 150/10 mg to 150/20, 300/10, and 300/20 mg (irbesartan/atorvastatin) according to the physician’s discretion.
The study protocol was approved by the institutional review boards at each participating center, and all study participants provided written informed consent (Table S1). This study was conducted according to the Declaration of Helsinki and Good Clinical Practice guidelines.
Patient data collection
Data on demographic characteristics, lifestyle habits, personal and familial medical history, and concomitant medications received during consultations were obtained. The participants also underwent physical examination, and their vital signs (BP and heart rate) were measured. Laboratory tests were conducted to evaluate lipid profiles. These tests were performed at baseline and the last visit. Furthermore, information on adverse events (AEs) from the baseline onwards was collected. Data on medication compliance were also obtained during the follow-up visits by evaluating the proportion of days covered.
Definition of measurements and questionnaire
Family history of premature CAD was defined as any occurrence of myocardial infarction or sudden death among same sex, first-degree relatives: parent or siblings (men <55 years old or women <65 years old).
Physical activity was described based on the number of episode of moderate or heavy exercise performed for >10 minutes. Moderate-intensity exercise induces a heart rate 60%–75% of the maximum heart rate (220-age), which one feels “a little tiring” and is equivalent to walking fast at 4.8–6.4 km/h (3–4 mph).
A dietary assessment questionnaire including 10 items of the mini dietary assessment index was administered at every visit, and compliance with the dietary assessment was classified as follows: poor adherence (total dietary score decreased compared with baseline and the items that scored ≤3 points at baseline for the main items [4, 5, 6, 7, 9] did not change after 3 months), average adherence (if one of the main items [4, 5, 6, 7, 9] improved and the total score increased compared with baseline), and good adherence (if two or more of the main items [4, 5, 6, 7, 9] improved compared with baseline or four or more of the main items scored 5 points [4, 5, 6, 7, 9]).
Whether the patients achieved moderate alcohol consumption and smoking cessation were investigated. The criteria for achieving moderation in alcohol consumption were 30 g/day in men, 15 g/day in women.
Efficacy and safety assessment
Treatment success was evaluated at the visit after 3 months of treatment based on target BP goal <140/90 mmHg for patients aged ≤80 years and LDL goals according to the Adult Treatment Panel III15 for HTN and hypercholesterolemia, respectively. Therefore, LDL goals were <100 mg/dL for cases with CHD or CHD risk equivalents, <130 mg/dL for cases with two or more risk factors, and <160 mg/dL for cases with no or one risk factor. This study also evaluated the clinical variables that affect the achievement of BP and/or LDL-C goals to determine treatment efficacy. Adherence to treatment with Rovelito and compliance with therapeutic lifestyle modification were also assessed, and AEs were measured. AEs were described using the Medical Dictionary for Regulatory Activities Terminology and/or based on actual observations.
Statistical analyses
Continuous variables are expressed as mean ± SD, or median with minimum, and maximum values. Categorical variables are expressed as frequency and percentage with 95% CIs.
Differences in demographic and other baseline characteristics by fulfillment/failure of the treatment goals were tested by independent t-test, chi-squared test, or Fisher’s exact test. Paired t-test or Wilcoxon signed-rank test was used to compare the baseline BP or LDL-C values and the values after 3 months.
Multiple logistic regression analysis was used to identify factors associated with failure to achieve the treatment goals for BP and LDL-C at 3 months after therapy. In model 1, the target variable was the achievement of treatment goals for BP. In model 2, target variable was the achievement of treatment goals for LDL-C. In model 3, target variable was the achievement of treatment goals for both BP and LDL-C.
A P-value <0.05 was considered statistically significant. All statistical analyses were performed using SAS statistical software version 9.3.
Results
Patient disposition, demographic characteristics, and baseline variables
A total of 2,777 patients were enrolled in this study, and 2,770 (99.75%) patients were included in the safety analysis. Of the 2,770 study participants who received irbesartan/atorvastatin (Rovelito), 2,545 (91.88%) completed the clinical study. The results of 931 patients were included in the final clinical progress analysis (Figure 1).
  | Figure 1 Study flowchart. |
The mean dose of irbesartan/atorvastatin at the end of study period was 160.1/12.4 mg. The average SBP of the 931 patients in the clinical progress analysis was 130.89±14.85 mmHg, while the average DBP was 79.94±11.31 mmHg. The average LDL level was 102.69±38.36 mg/dL (Table 1). Of 931 patients, 694 (74.5%) had controlled BP and 661 (70.9%) had controlled LDL-C after 3 months of treatment with Rovelito. At baseline, both BP and LDL-C goals were controlled in 504 participants (54.1%). With regard to the comorbidities, 405 had DM (43.50%) and 70 had chronic kidney disease (7.52%). Data on other demographic characteristics are presented in Table 1.
The number of medications for hypercholesterolemia and HTN in study participants at baseline was 1.4 and 2.4, respectively. The most commonly prescribed antihypertensive drugs were RAS blocker (70.5%; ARB [65.1%] or ACE inhibitors [7.4%]), followed by calcium channel blockers (29.9%), beta-blockers (15.7%), and diuretics (4.9%).
The number of medications other than Rovelito reported in study participants was 3.6 in 2,047 patients (73.9%). Other commonly reported concurrent medications were anti-thrombotic agents (48.3%) followed by antidiabetic drugs (25.7%).
Primary efficacy evaluation
Of the 931 participants who had all the variables needed for the analyses, 801 (86.04%) and 797 (85.61%) achieved the HTN and hypercholesterolemia treatment goals, respectively (Figure 2A and B).
The results of multiple logistic regression analyses showed that body mass index (BMI) ≥25 kg/m2 and BP levels, such as stage 1 and stage 2 HTN, were risk factors for failure to achieve treatment goals for BP (Table 2); and that smoking status, number of concomitant drugs, and severity of hypercholesterolemia severity were the significant factors for failure to achieve treatment goals for LDL-C level (Table 3). On the other hand, patient who failed to achieve moderate alcohol consumption had reduced failure to achieve the treatment goal for LDL-C (P=0.047).
Secondary efficacy evaluation
Achievement rate of both BP and LDL-C goals
Of 931 participants, 694 (74.54%) achieved the treatment goals for both HTN and hypercholesterolemia after 3 months of treatment (Figure 2C). The number of concurrent medications of participants who achieved the treatment goals for both HTN and hypercholesterolemia was 2.50±2.76, whereas that of those who failed to achieve the treatment goals for both was 3.56±2.68. In multiple logistic regression analyses for failure to achieve both BP and LDL-C goals, smoking, alcohol consumption, number of concomitant drugs, and severity of hypercholesterolemia and HTN were the significant risk factors (Table 4).
BP and LDL-C changes
In patients who achieved the BP goal (n=801), reductions in SBP and DBP at 3 months after treatment were −7.03±14.82 mmHg (−4.5%) and −4.40±10.09 mmHg (−4.4%), respectively (P<0.0001; Figure 3). In those who failed to achieve the BP goal (n=130), the SBP and DBP increased by 10.76±18.12 and 5.14±10.30 mmHg, respectively (P<0.0001; Figure 3).
  | Figure 3 Changes in SBP (A) DBP (B) from baseline to 3 months according to BP treatment goal attainment. |
In patients who achieved the LDL-C goal (n=797), LDL-C reduced by −15.56±33.53 mg/dL (−5%) (P<0.0001) at 3 months after treatment, whereas in those who failed to achieve the LDL-C goal (n=134), LDL-C reduced by −2.21±36.84 mg/dL only (Figure 4).
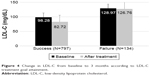  | Figure 4 Change in LDL-C from baseline to 3 months according to LDL-C treatment goal attainment. |
Therapeutic lifestyle modification
Drug adherence was 97.90%±5.79%. Patients with DM showed a significantly lower level of adherence compared to those without DM (P=0.0174). The drug adherence of the study participants with an alcohol consumption habit was significantly lower at baseline (P=0.0098).
Duration of physical exercise, which is a part of therapeutic lifestyle modification in the 931 participants, was 134.15±235.67 minute at the first visit and decreased to 129.42±216.54 minute, although the change was not significant.
Of the 931 participants, 89.04% achieved the moderate alcohol consumption goal. However, with a baseline value of 83.84% in the 2,770 study participants, the change was not remarkable. Male (P<0.0001) and smokers (P<0.0001) were less likely to meet the recommended moderate alcohol consumption goal. Participants aged ≥65 years (P=0.0148), with more concomitant medications (P=0.0074), and with normal BP level were more likely to meet the moderate alcohol consumption goal (P=0.0072).
Smoking cessation rate was not significantly changed (85.3 vs 89.0%). Male (P<0.0001), study participants with three or more visits (P=0.2305), those with more medications for hypercholesterolemia (P=0.0188), and those with a family history of CHD (P=0.0938) were less likely to quit smoking. Patients aged ≥65 years (P=0.0016), with more concomitant drugs used (P=0.0244) and with normal (P=0.0054) or prehypertension (P=0.0147) BP levels were more likely to quit smoking.
For dietary therapy, patients with three or more visits and those with “borderline high” were less adherent to the dietary therapy compared to those with two or less visits (P<0.0001) and those in the “very high” LDL-C category (P=0.0061), respectively. Those with more concomitant drugs used (P=0.0004) or DM (P<0.0001) were more adherent to dietary therapy.
Hence, while the study participants with both HTN and hypercholesterolemia showed a higher level of drug adherence, adherence to lifestyle change was not significantly different after the study.
Safety evaluation
One hundred sixteen (4.19%) participants who took Rovelito showed 155 AEs. The system organ class (SOC) with the highest number of AEs was nervous system disorders (45 study participants, 1.62%, 50 AEs). As per the preferred term (PT), dizziness had the highest occurrence with 25 instances (24 study participants, 0.87%). Thirteen participants had 14 severe AEs (0.47%) and 19 AEs resulted in study dropout by 17 participants (0.61%).
In addition, 31 participants (1.12%) showed 37 adverse drug reactions (ADR). The SOC with the highest number of ADRs was nervous system disorders (17 study participants, 0.61%, 19 cases). As per the PT, dizziness had the highest occurrence with nine instances (nine study participants, 0.32%). A serious adverse drug reaction to the medication (ie, aneurysm) occurred in one patient; however, no clear causal relationship between the drug and aneurysm was found (Table 5).
Discussion
Overall efficacy
In the clinical improvement evaluation group (n=931), BP and LDL-C goals were achieved in 801 (86.04%) and 797 (85.61%) patients, respectively, after 3 months of treatment with Rovelito, and 694 (74.54%) participants achieved both their BP and LDL-C treatment goals. Initially, regardless of baseline levels or control status, BP goal was set to <140/90 mmHg and LDL-C goals were set according to the baseline cardiovascular risk profiles. A previous study evaluated the efficacy of an FDC of amlodipine and atorvastatin using similar BP and LDL-C goals and showed a goal achievement rate for BP, LDL-C, and both of 65.0%, 75.7%, and 57.7%, respectively, at 12 weeks. Thus, the efficacy of Rovelito in our study appears comparable to that of an FDC of amlodipine and atorvastatin.16 Nevertheless, the difference in the efficacy could be attributed to the characteristics of the study population. A large proportion of the patients in our study had received medications for HTN and hypercholesterolemia before enrollment; ~88.7% participants had received antihypertensive drugs for HTN and 86.25% of them received statins for hypercholesterolemia prior to enrollment. Furthermore, this study did not exclude participants who had controlled BP and LDL-C at baseline. Thus, the overall efficacy of the FDC drug in relation to the BP goal could be higher in our study than that in a previous study.16 Moreover, participants achieved both BP and LDL-C goals more frequently after 3 months of treatment with Rovelito. Previous studies excluded participants who achieved both BP and LDL-C goals at baseline; by contrast, our study did not. Therefore, a number of participants had switched from previous antihypertensive drugs or statins to Rovelito, showing that Rovelito may be effective in the switching as well as the naïve groups.
In addition, we analyzed the achievement rate of treatment goals (for BP, LDL-C, and both BP and LDL-C) with each dose of Rovelito, but there were no significant differences among them (Table S2).
Factors related to efficacy
In our study, high baseline BP and high BMI were the factors for poor treatment success rate of the BP goal. Baseline LDL-C level, number of concomitant drugs, smoking, and alcohol consumption status were risk factors for poor treatment success rate of the LDL-C goal. Smoking, alcohol consumption status, number of concomitant drugs, and high baseline LDL-C and BP levels were risk factors for poor treatment success rate of both BP and LDL-C goals.
Adherence and its influence on efficacy
Adherence to Rovelito was 97.90%±5.79%. In this study, the incidence rate of AEs was 4.19%, and one patient had a serious ADR (aneurysm); however, no death was reported. In our study, therapeutic lifestyle modification was not effective in the treatment of hypercholesterolemia and HTN. The means to enhance adherence to therapeutic lifestyle modification, such as exercise prescription, dietary prescription, and advice on quitting smoking and moderate alcohol consumption, did not have a significant relationship with the achievement of treatment goals for HTN or hypercholesterolemia. The underlying reasons were that the study period was short and participants did not actively participate in therapeutic lifestyle modification. Although intensive lifestyle change was emphasized to patients with hypercholesterolemia and HTN, it may not have been performed properly and a more systematic approach might be needed.
In addition, smoking (OR [95% CI]: 1.81 [1.05–3.09], P<0.05), ≥3 concomitant drugs (OR [95% CI]: 1.77 [1.21–2.58], P<0.01), and high baseline LDL-C and BP levels were factors for poor treatment success rates of both BP and LDL-C goals (Table 4). This could be attributed to the fact that patients with a comorbid disease, such as CVD and DM, need more medications. Thus, improving drug adherence rate and achieving target treatment goals may be difficult. In our study, participants who failed to achieve moderate alcohol consumption were significantly more likely to achieve LDL-C goals than those who did not consume alcohol (non-drinking). Previous studies showed that alcohol consumption increases HDL-C levels slightly and tends to decrease LDL-C levels.17 However, the effect of moderate alcohol consumption on LDL-C levels appears difficult to establish as the study period was short and our study was based on participants’ self-filled questionnaires.
The BP-lowering effect of the combination drug (ie, antihypertensive drugs and statins) in patients who were already on antihypertensive medications was not statistically significant, whereas the LDL-C-lowering effect of the combination drug in patients on statins was statistically significant. Hence, this combination drug for HTN and hypercholesterolemia could also be an alternative drug to achieve LDL-C-lowering effects.
For hypercholesterolemia, there was a significant relationship between lower drug adherence rate and higher cardiovascular mortality and morbidity rates.18 In this study, adherence to Rovelito was high, which may be attributed to the fact that this was a prospective study.19 In addition, the short duration of the study (3 months) could have influenced the high compliance rate. Adherence to medications, according to previous studies, could be affected by various factors, such as the CAD, age, and other baseline characteristics.20,21
Regression analysis showed that participants with DM had a significantly lower rate of compliance with Rovelito compared to participants without DM. In addition, FDCs enhance compliance compared to free drug combination regimens.10,22 Hence, we suggested that requirement of FDCs may be higher in patients with comorbidities or more serious underlying diseases than in patients with simple HTN or hypercholesterolemia.
Therapeutic lifestyle modifications, such as exercise, dietary therapy, abstinence, or quitting smoking, showed no significant difference after the study. For physical activities, 80% cases had only consultation and recommendations; for dietary therapy, 82% received advice on dietary regimens. Based on these results, a more effective means of therapeutic lifestyle modification may be necessary.
Limitations
This study has some limitations. This observational study included various comorbidities or concurrent medications. Thus, limitations exist to the analysis of study findings due to the inability to control concomitant medications for HTN and hypercholesterolemia. In addition, a large proportion of participants in this study received treatments for both diseases before enrollment, thereby affecting the analysis. The study duration was only 3 months, which was rather short for judging the study drug’s protective effects on the cardiovascular system. Previous open label, non-comparative studies that evaluated the efficacy and safety of an FDC of amlodipine and atorvastatin for the treatment of patients with HTN and hypercholesterolemia, were conducted for 12–14 weeks.16,23 Furthermore, a previous placebo-controlled study showed that an FDC of irbesartan and atorvastatin provided effective, safe treatment to which patients with HTN and hypercholesterolemia showed good adherence, as the treatment duration was only 8 weeks.24 Therefore, we chose 3 months of treatment according to previous studies. The open-label, non-comparative design was a potential limitation; nonetheless, this study presents the effects of the study drug on both diseases in a real clinical setting. Furthermore, the only available observational study using an FDC of an anti-HTN drug and statin was the one using amlodipine and atorvastatin, which was the first observational study that used ARB and atorvastatin. Recent studies reported that RAS blockers are more effective in preventing CVD than calcium channel blockers, and among RAS blockers, ARB is more advantageous for Asians patients as it does not cause dry cough.13,14 In addition, irbesartan is extremely useful in preventing diabetic nephropathy. Considering these factors, Rovelito could be an extremely helpful drug for clinical practice as it prevents CVDs and improves drug compliance among Korean patients.
Conclusion
FDCs of ARBs and statins, such as Rovelito, could be extremely useful for the treatment of patients with both HTN and hypercholesterolemia as these can be comorbidities due to their mechanisms or epidemiology. Thus, using a single drug could enhance compliance. Therefore, our study’s findings could be used for management of the aforementioned diseases and for enhancing the compliance and lifestyle modifications of patients with HTN and hypercholesterolemia.
Moreover, the FDC of irbesartan and atorvastatin (Rovelito) is associated with the achievement of BP and LDL-C goals and higher adherence. Poor metabolic profiles are risk factors for poor treatment success rate. Despite the 75% treatment success rate for both HTN and hypercholesterolemia, therapeutic lifestyle modification should still be underscored in the treatment.
Acknowledgments
This study was supported by research grants from Hanmi Pharmaceutical Co., Ltd.
Disclosure
The authors report no conflicts of interest in this work.
References
Perk J, De Backer G, Gohlke H, et al. European guidelines on cardiovascular disease prevention in clinical practice (version 2012). The Fifth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of nine societies and by invited experts). Eur Heart J. 2012;33(13):1635–1701. | ||
National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Third report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation. 2002;106(25):3143–3421. | ||
Hurtubise J, McLellan K, Durr K, Onasanya O, Nwabuko D, Ndisang JF. The different facets of dyslipidemia and hypertension in atherosclerosis. Curr Atheroscler Rep. 2016;18(12):82. | ||
Thomas F, Bean K, Guize L, Quentzel S, Argyriadis P, Benetos A. Combined effects of systolic blood pressure and serum cholesterol on cardiovascular mortality in young (<55 years) men and women. Eur Heart J. 2002;23(7):528–535. | ||
Satoh M, Ohkubo T, Asayama K, et al. Combined effect of blood pressure and total cholesterol levels on long-term risks of subtypes of cardiovascular death: evidence for cardiovascular prevention from observational cohorts in Japan. Hypertension. 2015;65(3):517–524. | ||
Wong ND, Lopez V, Tang S, Williams GR, Prevalence WGR. Prevalence, treatment, and control of combined hypertension and hypercholesterolemia in the United States. Am J Cardiol. 2006;98(2):204–208. | ||
Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA. 2003;289(19):2560–2572. | ||
Wong ND, Lopez VA, L’Italien G, Chen R, Kline SE, Franklin SS. Inadequate control of hypertension in US adults with cardiovascular disease comorbidities in 2003–2004. Arch Intern Med. 2007;167(22):2431–2436. | ||
Petrella RJ, Merikle E. A retrospective analysis of the prevalence and treatment of hypertension and dyslipidemia in southwestern Ontario, Canada. Clin Ther. 2008;30(6):1145–1154. | ||
Bangalore S, Kamalakkannan G, Parkar S, Messerli FH. Fixed-dose combinations improve medication compliance: a meta-analysis. Am J Med. 2007;120(8):713–719. | ||
Mancia G, Fagard R, Narkiewicz K. 2013 ESH/ESC guidelines for the management of arterial hypertension: the task Force for the management of arterial hypertension of the European Society of hypertension (ESH) and of the European Society of cardiology (ESC). J Hypertens. 2013;31(7):1281–1357. | ||
Neutel JM, Bestermann WH, Dyess EM, et al. The use of a single-pill calcium channel blocker/statin combination in the management of hypertension and dyslipidemia: a randomized, placebo-controlled, multicenter study. J Clin Hypertens. 2009;11(1):22–30. | ||
Matchar DB, McCrory DC, Orlando LA, et al. Systematic review: comparative effectiveness of angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers for treating essential hypertension. Ann Intern Med. 2008;148(1):16–29. | ||
Borghi C, Cicero AF. The role of irbesartan in the treatment of patients with hypertension: a comprehensive and practical review. High Blood Press Cardiovasc Prev. 2012;19(1):19–31. | ||
Hyre AD, Muntner P, Menke A, Raggi P, He J. Trends in ATP-III-defined high blood cholesterol prevalence, awareness, treatment and control among U.S. adults. Ann Epidemiol. 2007;17(7):548–555. | ||
Blank R, Lasalle J, Reeves R, Maroni J, Tarasenko L, Sun F. Single-pill therapy in the treatment of concomitant hypertension and dyslipidemia (the amlodipine/atorvastatin GEMINI study). J Clin Hypertens. 2005;7(5):264–273. | ||
Brinton EA. Effects of ethanol intake on lipoproteins. Curr Atheroscler Rep. 2012;14(2):108–114. | ||
The West of Scotland Coronary Prevention Study Group. Compliance and adverse event withdrawal: their impact on the West of Scotland Coronary Prevention study. Eur Heart J. 1997;18(11):1718–1724. | ||
Halpern MT, Khan ZM, Schmier JK, et al. Recommendations for evaluating compliance and persistence with hypertension therapy using retrospective data. Hypertension. 2006;47(6):1039–1048. | ||
Jackevicius CA, Mamdani M, Tu JV. Adherence with statin therapy in elderly patients with and without acute coronary syndromes. JAMA. 2002;288(4):462–467. | ||
Ma J, Vaillancourt R, Bennett C. Adherence to lipid-lowering drug therapy among members of the Canadian forces. Mil Med. 2008;173(7):666–670. | ||
Dresser GK, Nelson SA, Mahon JL, et al. Simplified therapeutic intervention to control hypertension and hypercholesterolemia: a cluster randomized controlled trial (STITCH2). J Hypertens. 2013;31(8):1702–1713. | ||
Fedacko J, Pella D, Jarcuska P, et al. Slovak trial on cardiovascular risk reduction following national guidelines with CaDUET® (the strong duet study). Adv Ther. 2013;30(1):60–70. | ||
Kim SH, Jo SH, Lee SC, et al. Blood pressure and cholesterol-lowering efficacy of a fixed-dose combination with irbesartan and atorvastatin in patients with hypertension and hypercholesterolemia: a randomized, double-blind, factorial, multicenter phase III study. Clin Ther. 2016;38(10):2171–2184. |
Supplementary materials
  | Table S1 The name of all participating centers with institutional review boards, which provided approval |
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.







