Back to Journals » Infection and Drug Resistance » Volume 14
Efficacy and Safety of Giant Condyloma Acuminatum with Monotherapy of Topical Traditional Chinese Medicine: Report of Eight Cases
Received 28 January 2021
Accepted for publication 13 March 2021
Published 9 April 2021 Volume 2021:14 Pages 1375—1379
DOI https://doi.org/10.2147/IDR.S302195
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Suresh Antony
Mei-fang Wang, Li Lin, Lin-feng Li
Department of Dermatology, Beijing Friendship Hospital, Capital Medical University, Beijing, 100050, People’s Republic of China
Correspondence: Lin-feng Li
Department of Dermatology, Beijing Friendship Hospital, Capital Medical University, Beijing, 100050, People’s Republic of China
Tel +8613693620186
Email [email protected]
Background: Giant condyloma acuminatum (GCA), also called Buschke–Löwenstein tumor, presents as a verrucous infiltrating lesion and is caused by sexual transmission of human papilloma virus. The optimal treatment is controversial and there are no standard guidelines because of its rarity and frequent recurrence. It has a relatively high local recurrence rate.
Objective: We here report eight patients (six men and two women) with GCA whose lesions were successfully treated topically with traditional Chinese medicine (TCM) preparations, paiteling.
Methods and Materials: We administered topical TCM preparations to eight patients diagnosed with GCA who had refused surgery. The treatment process included three stages, their durations depending on the speed of resolution of the lesions and the results of visual inspection with acetic acid.
Results: No significant complications occurred in any patient. The functional and esthetic outcomes were satisfactory. No recurrences were detected during follow-up.
Conclusion: Topical treatment with TCM preparations may be a good alternative to surgery or other traditional methods for the treatment of GCA. This treatment has the advantages of being non-invasive, painless, and having a low risk of recurrence, and may be a useful adjunct to mainstream medical treatments.
Keywords: giant condyloma acuminatum, GCA, traditional Chinese medicine, TCM, treatment, dermatosis symptoms, paiteling
Introduction
Giant condyloma acuminatum (GCA), also known as Buschke–Lowenstein tumor, is a type of cutaneous and mucosal infection caused by sexual transmission of the human papilloma virus (HPV). It is rare, the reported incidence being 0.1% in the general population.1 GCA can present as a cauliflower-like lesion2 with broad-based papillomas up to several centimeters in diameter or as large confluent plaques. These lesions mostly occur in the perineum, vulva, vagina, perianal region and rectum,3 rarely developing in extragenital areas.4 Because these lesions frequently recur, being benign but contagious, lack a definitive form of treatment, and their treatment is expensive,5 they can adversely affect patients’ functioning and psychological health. This condition is, therefore, a serious public health concern and poses a significant medical burden.
Treatment strategies for condyloma acuminatum (CA) include topical chemotherapy, cryotherapy, electrocautery, carbon dioxide laser therapy, surgical excision, and photodynamic therapy. There are no standard guidelines for the treatment of GCA because of its rarity and relatively high local recurrence rate.6 Radical surgery alone or combined with other treatment modalities such as chemotherapy or photodynamic therapy6–8 has been recommended; however, this can have undesirable sequelae, such as scarring and poor functional and esthetic outcomes.1 Some recently published studies have reported satisfactory outcomes after topical use of drugs, such as imiquimod, interferon, and the traditional Chinese medicine (TCM) preparation, paiteling.1,9–11
TCM preparations may be effective adjuncts to, or replacements for, mainstream medicines for GCA because they contain numerous ingredients and therefore probably have multiple mechanisms of action. Chinese researchers have reported that paiteling is effective in eradicating lesions, achieving better cosmetic outcomes, and improving quality of life. Paiteling irrigation of the vaginal stump can reportedly play a role in the positive-to-negative conversion of high-risk HPV infection after total hysterectomy.12 In this report, we present a series of eight patients with GCA who were successfully treated with the TCM preparations, paiteling.
Case Descriptions
We here present eight patients with GCA, six men and two women aged from 19 to 75 years (Table 1), who were treated in the clinics of the HPV Technology Service Center of the Beijing Patborn Biotechnology Development Company (Beijing, China) in the past 2 years. The time from the onset of symptoms to diagnosis varied between 2 weeks and 1.5 years, with a mean of 7.5 weeks.
 |
Table 1 Characteristics of Patients, Lesions, and Treatment |
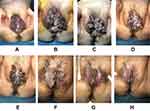
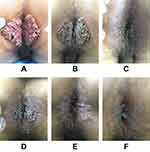
All patients presented with massive clustered or discrete cauliflower-like or mushroom-shaped lesions measuring from 4 cm × 3 cm to 15 cm × 10 cm (Table 1, Figures 1 and 2). The most commonly involved sites were the vulva, penis, vagina, perianal region, and rectum. No enlarged inguinal lymph nodes were found on physical examination. Two patients had a history of diabetes mellitus and two had hypertension. Laboratory tests showed no evidence of hematological disorders or other sexually transmitted diseases, including syphilis and HIV. Samples from five patients were subjected to HPV DNA analysis with a consensus polymerase chain reaction technique (Table 1). In all cases, biopsies confirmed the clinical diagnosis of CA and showed no evidence of malignant disease. Some of the patients had previously been treated with conservative therapies without significant improvement and some had refused the suggestions of further surgical treatment by their primary care doctors.
All eight patients were treated with paiteling (Beijing Patborn Biotechnology Development Company). The treatment process includes up to three stages, depending on whether the lesions have resolved and the results of visual inspection with acetic acid (VIA). In the first stage, local wet packing with a solution of paiteling was applied by professional medical staff for fifteen minutes once a day for three consecutive days per week. The patient could apply sea buckthorn oil topically to promote the wound healing for the remaining four days of each week. The above treatment course was repeated for one to eighteen weeks until the lesions were no longer visible on gross inspection. Photos were taken after the third day’s treatment each week. In the second stage, which lasted three to six weeks, the same procedure was followed until VIA was negative. In the third stage, dressings wetted with a 2% dilution of paiteling were applied for ten minutes once a day for the first month, then every other day for the following two months. This treatment was stopped when no lesions were visible and VIA was negative at the three-month follow-up visit. All patients reported during a 6-month telephone follow-up that they had no recurrences. We have provided representative photos at different stages of treatment in chronological order (Figures 1 and 2). No serious adverse reactions, including swelling, pain, or scarring, were detected, and none of the treatments had to be discontinued.
Discussion
Treatment of GCA is problematic because the lesions are massive, it has a high recurrence rate, and its rarity prevents adequate assessment of treatment options.6 Complete surgical excision with histologically clear margins is currently the mainstay of treatment.1,6,13 Considering oncological principles, cosmetic and functional outcomes, and the patient’s physical and mental health, the selection of the optimal surgical procedure is challenging.1,5,13 Some patients refuse surgery because of their general health, immunologic status, fear, or for other reasons. Many mainstream therapies, including podophyllin, 5-fluorouracil, bleomycin, methotrexate and imiquimod, are administered to complement surgery or to patients in poor health.1,5,6,14 Imiquimod alone reportedly has a beneficial effect; however, the evidence for this is based only on case reports, and no large, evidence-based studies have confirmed it.1,9 Topical therapy for GCA has the advantages of being free of intraoperative complications and leaving no scarring.
The eight patients in this series were successfully treated with TCM paiteling alone. Chinese specialists have reached a consensus on recommending paiteling for treatment of CA and it is widely used for this purpose in much of China. TCM has been used for the prevention, treatment, and cure of many disorders for centuries15 and is a treasure of Chinese civilization that is gaining increasing international interest.16 Paiteling, a mixture of more than ten TCM components, was developed by the Chinese Academy of Sciences approved by the ministry of Chinese health in 1996. Its components include Lonicera japonica, Folium isatidis, Sophora flavescens, Fructus cnidii, Oldenlandia diffusa, Nidus vespae, Java brucea, and other traditionally-used herbs. These herbs have anti-inflammatory, antiviral, detoxifying, relief of swelling, analgesic, blood circulation-stimulating, and wound-healing effects and are used to treat warts and tumors caused by HPV infection. It has been shown that paiteling can achieve resolution of HPV infection and regression of related cervical lesions.17 The first stage of the treatment process for GCA is aimed at resolution of the visible mass, the second at suppressing possible subclinical (latent) HPV infection as revealed by VIA-positivity, and the third stage at consolidating the clinical efficacy and HPV clearance to minimize recurrence.10,12
In our series, the duration of the first stage of treatment varied from 1 to 18 weeks, depending on the diameter and thickness of the initially massive lesions. The bigger the verrucae, the greater the degree of keratinization, and the longer the required course of treatment. Thinner lesions of finer texture tend to absorb paiteling better; this contributes to shortening the required duration of treatment. The second stage varied from 3 to 6 weeks depending on the anatomical region of the primary lesions and the duration of the first stage. The third stage lasted for 3 months, which is similar to the duration of follow-up treatment required for most HPV-associated lesions.5,18 Because of its strong ability to permeate, paiteling can pass quickly through the epidermal cells to reach the basal layer of the epidermis without damaging the dermis and the subcutaneous tissues,17 in the process promoting exfoliation of vigorously metabolizing epidermal cells. Of note, there were no serious adverse reactions during treatment and no subsequent scarring or relapse in any of our eight patients. Compared with other modalities, paiteling has the advantages of being non-invasive, painless, and achieving significant improvement in patients’ quality of life. It is regrettable that HPV DNA analysis was not performed in all patients at the time of initial treatment and after completion of therapy.
In summary, we have here presented eight patients with GCA treated with topical TCM preparations only, all of whom recovered completely with satisfactory functional and esthetic outcomes. This treatment is an effective alternative to surgery and other traditional means of treating GCA, and may be a useful adjunct to mainstream medical treatment. However, more clinical evidence and further research on molecular mechanisms are warranted to clarify the effects of this therapy.
Statement of Ethics
This study was conducted in accordance with the Declaration of Helsinki. And the study protocol was approved by the Beijing Friendship Hospital Ethics Committee for Human Research (2021-P2-048-01). A written informed consent has been provided by the eight patients to have the case details and the accompanying images published.
Disclosure
The authors declare that they have no conflicts of interest.
References
1. Combaud V, Verhaeghe C, Hachem H, et al. Giant condyloma acuminatum of the vulva: successful management with imiquimod. JAAD Case Rep. 2018;4(7):692–694. doi:10.1016/j.jdcr.2018.04.007
2. Park IU, Introcaso C, Dunne EF. Human papillomavirus and genital warts: a review of the evidence for the 2015 centers for disease control and prevention sexually transmitted diseases treatment guidelines. Clin Infect Dis. 2015;61(Suppl 8):S849–S855. doi:10.1093/cid/civ813
3. Cui T, Huang J, Lv B, et al. Giant condyloma acuminatum in pregnancy: a case report. Dermatol Ther. 2019;32(4):e12972. doi:10.1111/dth.12972
4. Lee CN, Hsu CK, Lee JY. Recalcitrant extragenital giant condyloma acuminatum: a need for combination therapy. Dermatol Ther. 2019;32(3):e12867. doi:10.1111/dth.12867
5. Mehmet S, Ali Murat C, Nevgun S, et al. HPV infection in urology practice. Int Urol Nephrol. 2020;52(1):1–8. doi:10.1007/s11255-019-02302-2
6. Spinu D, Rădulescu A, Bratu O, et al. Giant condyloma acuminatum - Buschke-Lowenstein disease - a literature review. Chirurgia (Bucur). 2014;109(4):445–450.
7. Jorgaqi E, Jafferany M. Giant condyloma acuminatum (Buschke-Lowenstein tumor): combined treatment with surgery and chemotherapy. Dermatol Ther. 2020;33(1):e13193. doi:10.1111/dth.13193
8. Chen X, Zhou Y, Tan Y. Successful management of giant condyloma acuminatum of vulva with the combination of surgery and photodynamic therapy: report of two cases. Photodiagnosis Photodyn Ther. 2020;31:101847. doi:10.1016/j.pdpdt.2020.101847
9. Marino F. Complete healing of perianal giant condyloma (buschke-lowenstein tumor) with imiquimod 5% cream alone. Tech Coloproctol. 2020;24(12):1313–1314. doi:10.1007/s10151-020-02280-z
10. Hui-Ling S, Bei Y, Chang-Qiang L. Treatment of giant condyloma acuminatum with paiteling: a case report. Dermatol Ther. 2020;33(6):e13936.
11. Tian YP, Yao L, Malla P, et al. Successful treatment of giant condyloma acuminatum with combination retinoid and interferon-γ therapy. Int J STD AIDS. 2012;23(6):445–447. doi:10.1258/ijsa.2011.011331
12. Lee CN, Hsu CK, Lee JY. Clinical efficacy of paiteling in the treatment of condyloma acuminatum infected with different subtypes of HPV. Dermatol Ther. 2019;32(5):e13065.
13. Niazy F, Rostami K, Motabar AR. Giant condyloma acuminatum of vulva frustrating treatment challenge. World J Plastic Surg. 2015;4(2):159–162.
14. Tripoli M, Cordova A, Maggì F, Moschella F. Giant condylomata (Buschke-Lowenstein tumours): our case load in surgical treatment and review of the current therapies. Eur Rev Med Pharmacol Sci. 2012;16(6):747–751.
15. Liu SH, Chuang WC, Lam W, et al. Safety surveillance of traditional Chinese medicine: current and future. Drug Saf. 2015;38(2):117–128. doi:10.1007/s40264-014-0250-z
16. Xu Q, Bauer R, Hendry BM. The quest for modernisation of traditional Chinese medicine. BMC Complement Altern Med. 2013;13:132. doi:10.1186/1472-6882-13-132
17. Tao P, Zheng W, Meng X. Effect of paiteling on human papillomavirus infection of the cervix. Mol Clin Oncol. 2017;7(6):957–964. doi:10.3892/mco.2017.1454
18. Gross GE, Werner RN, Becker JC. S2k guideline: HPV-associated lesions of the external genital region and the anus – anogenital warts and precancerous lesions of the vulva, the penis, and the peri- and intra-anal skin (short version). J Dtsch Dermatol Ges. 2018;16(2):242–255. doi:10.1111/ddg.13441
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.