Back to Journals » Drug Design, Development and Therapy » Volume 11
Effects of intrathecal dexmedetomidine on shivering after spinal anesthesia for cesarean section: a double-blind randomized clinical trial
Authors Nasseri K , Ghadami N, Nouri B
Received 7 January 2017
Accepted for publication 21 February 2017
Published 3 April 2017 Volume 2017:11 Pages 1107—1113
DOI https://doi.org/10.2147/DDDT.S131866
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Manfred Ogris
Karim Nasseri,1,2 Negin Ghadami,1 Bijan Nouri2
1Department of Anesthesiology, Faculty of Medicine, Kurdistan University of Medical Sciences, Sanandaj, Iran; 2Social Determinants of Health Research Center, Kurdistan University of Medical Sciences, Sanandaj, Iran
Background: Shivering is among the common troublesome complications of spinal anesthesia (SA), and causes discomfort and discontentment in parturients undergoing cesarean sections (CSs). The aim of this study was to investigate the effects of intrathecal dexmedetomidine in the prevention of shivering in those who underwent CS under SA.
Subjects and methods: Fifty parturients planned for elective CSs under SA were enrolled in this prospective, double-blinded, controlled study and randomly divided into two equal groups. Spinal block was achieved with 12.5 mg 0.5% heavy bupivacaine plus 5 µg dexmedetomidine (BD group) or 0.5 mL 0.9% normal saline (BN group). The incidence and intensity of shivering, peripheral and core body temperature, hemodynamic parameters, and adverse events was recorded.
Results: The incidence of shivering was significantly higher in the BN group (52%) than the BD group (24%) (P=0.04). Likewise, the intensity of shivering was significantly higher in the BN group than the BD group (P=0.04). The incidence of adverse events, such as hypotension, nausea/vomiting, and bradycardia, was not significantly different between the two groups, although the grade of sedation was higher in the BD group than the BN group (P=0.004).
Conclusion: We conclude that intrathecal dexmedetomidine is effective in lowering the incidence and intensity of shivering in parturients undergoing CSs under SA without major adverse effects.
Keywords: dexmedetomidine, shivering, spinal anesthesia, cesarean sections, bupivacaine
Introduction
Shivering is one of the common troublesome complications involving regional anesthesia, and causes discomfort and dissatisfaction in parturients undergoing cesarean sections (CSs).1 A review of 21 studies showed that the median incidence of shivering after neuraxial anesthesia was 55%.2 Shivering can impair pulse oximetry and electrocardiogram monitoring. It can also increase demand for oxygen and production of CO2 about fourfold,3,4 and may also have a role in the intensification of wound pain, reduced wound healing, and delayed discharge from the recovery unit.5 Therefore, the prevention of shivering is rational and could result in better perioperative outcomes.
In previous studies, different pharmacological and nonpharmacological techniques have been attempted to prevent shivering, but a gold-standard method has not yet been determined.6 Dexmedetomidine has highly specific α2-adrenergic receptor-agonist properties, with strong impacts on the central nervous system without respiratory depression.3,7 It is postulated that intravenous dexmedetomidine could reduce shivering thresholds via its centrally mediated actions without any major adverse effects.8,9
In contrast to intravenous dexmedetomidine, the effect of intrathecal dexmedetomidine on shivering is not well known. We hypothesized that intrathecal dexmedetomidine could decrease the incidence and intensity of shivering. As such, we sought to examine the effect of intrathecal dexmedetomidine in the prevention of shivering during spinal anesthesia (SA) in patients who underwent CSs.
Subjects and methods
Registration
This study was registered in the Iranian Registry of Clinical Trials (IRCT201511301766N7) on January 12, 2016. We obtained the approval of the Kurdistan University of Medical Sciences review board before registration.
Design
This single-center, prospective, randomized, double-blinded, parallel, controlled study was undertaken at Besat Hospital, Sanandaj, Kurdistan, Iran (a university-affiliated tertiary referral hospital) from September 22, 2015 to June 21, 2016. Written informed consent was fulfilled by all participant in the study.
Eligibility criteria
Fifty American Society of Anesthesiologists physical status I or II patients aged 18–45 years scheduled for elective CSs under SA were enrolled for the study by the second author. Patients with a primary core body temperature of more than 37.5°C or lower than 36.5°C, body mass index >25, with contraindications for SA, cardiac disease, history of psychiatric disease, taking α-receptor antagonist drugs, hypertensives, or any antihypertensive drug, renal failure, hepatic failure, a history of allergy to the study drugs, excessive hemorrhage needing transfusion, or failure or incomplete spinal block were excluded from the study. After the beginning of the trial, the eligibility criteria and trial methods remained fixed.
Preanesthetic interventions
Upon patient arrival at the anesthesia room, two 18 G venous cannulae were inserted and fixed in the dorsum of the hand and the elbow of the left upper limb. Patients were then preloaded with lactated Ringer’s solution (10 mL/kg) and maintained with 8 mL/kg/h. Fluids were stored at room temperature. Before SA, basic monitoring, including noninvasive blood pressure, heart rate, electrocardiography, and pulse oximetry, was applied for all patients and basic values recorded. Patients were randomized using computer-generated numbers into two groups of 25 patients by the third author.
Study interventions
Using an aseptic technique, SA was performed with the patient in sitting position at the L3–L4 or L4–L5 interspaces with a 25 G spinal Quincke-tip needle. In the bupivacaine–dexmedetomidine (BD) group, 5 μg dexmedetomidine (Precedex; Hospira, Lake Forest, IL, USA) was added to 12.5 mg 0.5% heavy bupivacaine (AstraZeneca, London, UK). In the bupivacaine–normal saline (BN) group, 0.5 mL 0.9% normal saline was added to the same amount of bupivacaine. After completion of the SA, which was performed by the first author (who was not involved in data gathering), all patients were turned to the supine position immediately with left uterine displacement, while supplemental oxygen was administered at the rate of 5 L/min via a face mask. The study drugs were prepared by an anesthesia nurse, who had no prior knowledge of the study design, in equal volumes (3 mL) for both groups.
The temperature of the operating room and postanesthesia-care unit was kept at 22°C–26°C throughout the study. During the operation, the whole body of the patient, except the head, neck, and operation site, were covered with one layer of surgical drapes. In the postanesthesia-care unit, the patient’s body was covered with one cotton blanket.
Tools and measurements
The incidence and intensity of shivering, as well as core body temperature, which were the primary outcomes of the study, were evaluated by an anesthesiologist (second author), who had no prior knowledge of the administered drugs. The incidence of shivering was assessed by close observation of the patients during the operation and in the postanesthesia room. The intensity of shivering was classified by the method of Tsai and Chu: 0, no shivering; 1, piloerection or peripheral vasoconstriction, but no visible shivering; 2, muscular activity in only one muscle group; 3, muscular activity in more than one muscle group, but not generalized; and 4, shivering involving the whole body.9 The incidence, time interval from blocks to shivering occurrence, and intensity of shivering were recorded every 5 minutes during the surgery and in the recovery room.
Core body and peripheral temperatures were measured from the tympanic membrane and forehead-skin surface, once before SA and then at 15-minute intervals. Vital parameters, such as heart rate, systolic and diastolic blood pressure, and SPO2, were monitored continuously and recorded at intervals of 5 minutes for the first 30 minutes and then 15 minutes for the rest of the observation period. Anesthesia complications, such as sedation score, hypotension, bradycardia, and nausea/vomiting, were recorded and treated as follows. Sedation was graded using the 5-point sedation scale: 1, fully awake and oriented; 2, drowsy; 3, eyes closed, but open on command; 4, eyes closed, but open to mild physical stimulation; and 5, eyes closed and unresponsive to mild physical stimulation.10 Systolic blood pressure <30% from the primary value or <90 mmHg was determined as hypotension. Heart rate <50 beats/minute was specified as bradycardia. Nausea/vomiting was graded as none (no episode of nausea or vomiting), mild (one episode of nausea that was resolved without treatment), moderate (repeated episodes of nausea that were resolved with treatment), and severe (continues episodes of nausea or vomiting).
Rescue drugs for shivering (score ≥2), hypotension, bradycardia, and nausea/vomiting were intravenous meperidine (30 mg), ephedrine (5 mg) and then further infusion of crystalloid (250 mL) fluid as required, atropine (0.5 mg), and ondansetron (4 mg), respectively. The amount of rescue drugs in each group was recorded. After delivery, the neonates’ Apgar scores at 1 and 5 minutes were recorded.
Sample-size calculation
The median incidence of shivering following neuraxial anesthesia is 55%. To obtain a 20% reduction in the incidence of shivering in the study group with a power of 90% and α=0.9, a sample size of 25 patients in each group was required, so 50 patients were included in the study.
Statistical analysis
Data were analyzed using Stata version 12. Patients’ age, weight, duration of surgery, and gestational age were compared using the independent t-test. Shivering intensity in the two groups was compared using the Mann–Whitney U test. For comparing the incidence of shivering and adverse events between the groups, χ2 tests were used. Trends in changes in tympanic and forehead temperatures, blood pressure, and heart rate between the two groups were assessed using a repeated-measurement test. A P-value less than 0.05 was defined as statistically significant.
Results
From 73 participants who enrolled in the study, 54 met the inclusion criteria and were randomized by the third author, who had no role in outcome evaluation (Figure 1). There was no significant difference between the two groups with respect to patient age, weight, gestational age, or duration of surgery (Table 1).
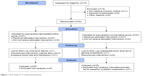  | Figure 1 Flow diagram of randomized patients. |
Shivering and core temperature
Time interval from blocks to shivering occurrence was not statistically significant different in the two groups (P=0.12). The difference in shivering incidence between the BD group (six patients [0.24%]) and the BN group (13 patients [52%]) was statistically significant (P=0.04). Also, shivering intensity was significantly greater in the BN group than the BD group (P=0.03) (Table 2). Trends in core and forehead temperatures showed no significant differences between the groups (Figure 2).
  | Figure 2 Core body temperatures were similar in the two groups. |
Hemodynamic indices
There were no differences in respect of trends of systolic and diastolic blood pressure or heart rate during operation and recovery time between the BD and BN groups (Figures 3 and 4).
  | Figure 3 Systolic blood pressure during the study showed no significant differences between two groups. |
  | Figure 4 Heart rate showed no significant differences between the two groups. |
Complications of the intervention
The sedation grade was higher in group BD than group BN (P=0.004). The incidence of nausea/vomiting (P=1), hypotension (P=0.51), and bradycardia (P=0.48) was not significantly different between the two groups (P=0.57, 0.55, and 0.26, respectively). There was no significant difference in escape doses of ephedrine, atropine, or ondansetron between the two groups. However, the escape dose of meperidine for treatment of high-grade shivering (≥2) was significantly higher in the BN group (P=0.04) (Table 3). Apgar scores of neonates within 1 and 5 minutes after delivery were not significantly different between the two groups.
  | Table 3 Adverse effects and drugs used as rescue treatment in the two study groups |
Discussion
The results of the current study showed that core body and forehead temperature trends intra- and postoperatively were not different between the two groups. However, the incidence and intensity of shivering was lower in the BD group. The incidence of shivering in the BN group was 52%, while 24% of patients in the BD group experienced shivering.
Intra- and postoperative shivering, with pain and postoperative nausea and vomiting, are distressing events for the patients. Various pharmacological methods have been examined for treatment or prevention of postoperative shivering; however, there is no gold-standard drug or method to prevent its occurrence.11
Numerous investigations regarding dexmedetomidine have shown it to have sedative, analgesic, perioperative sympatholytic, anesthetic-sparing, and hemodynamic-stabilizing properties.9,12,13 However, the antishivering effect of dexmedetomidine has not been adequately investigated.
Usta et al compared the effect of intravenous dexmedetomidine (1 μg/kg bolus followed by an infusion of 0.4 μg/kg/h) with normal saline on shivering in 60 patients during SA. Subarachnoid blockage was performed with 18 mg hyperbaric bupivacaine in all cases. They found that infusion of dexmedetomidine in the perioperative period significantly decreased the incidence and severity of shivering in patients during SA.9
Bajwa et al12 studied dexmedetomidine effectiveness in suppressing postanesthesia shivering in patients who had undergone laparoscopic surgery during general anesthesia. They administered intravenous dexmedetomidine 1 μg/kg during the perioperative period. They noted that the incidence of shivering was significantly lower in the dexmedetomidine group, and concluded that intravenous dexmedetomidine possesses antishivering properties and can reduce the occurrence of shivering.12
In the aforementioned studies, the antishivering effects of dexmedetomidine were via the systemic absorption of the drug, and it appears that intravenous dexmedetomidine decreases vasoconstriction and shivering thresholds, such that a higher degree of hypothermia is necessary to lead to shivering. Unlike systemic dexmedetomidine, information about the effects of intrathecal dexmedetomidine on shivering is limited. In a randomized, controlled trial, Moawad and Elawdy13 investigated the effect of subarachnoid dexmedetomidine in the reduction and prevention of shivering in 80 patients who received SA for transurethral resection of the prostate. Subarachnoid block was achieved by either 12.5 mg of hyperbaric bupivacaine plus 0.5 mL of isotonic saline or 12.5 mg of hyperbaric bupivacaine plus 10 μg dexmedetomidine in 0.5 mL of isotonic saline. The incidence of shivering was significantly lower (15%) in the dexmedetomidine group than the saline group (57%). They concluded that adding 10 μg dexmedetomidine to hyperbaric bupivacaine in the transurethral resection of the prostate procedure could reduce the incidence of shivering.
With regard to shivering, the results of Moawad and Elawdy’s13 study are in agreement with the current study. The lower incidence of shivering compared with our study may relate to the higher dose of dexmedetomidine (10 μg versus 5 μg). Qi et al14 compared the effects of 5 μg intrathecal dexmedetomidine with 100 μg morphine as supplements to 10 mg bupivacaine in 120 parturients undergoing elective CSs under SA. Only 7.7% of patients in the dexmedetomidine group had shivering, while 30% and 35.9% of patients in the morphine and bupivacaine groups experienced shivering, respectively. Although these results regarding lowering shivering are in agreement with our study, the incidence of shivering in that study was significantly lower than present study.
Abdelhamid and El-Lakany15 also reported a low incidence of shivering (2 in 31) following SA by heavy bupivacaine 0.5% plus 5 μg intrathecal dexmedetomidine for lower abdominal surgeries compared with 12 of 31 in the control group. The key factors that may contribute to these differences are those that could increase shivering during SA. These factors are aging, sensory-block levels, temperatures of the intrathecal local anesthetics, intravenous fluids, and operation room.9,16 In the current study, the age of patients in the two groups, ambient temperature of the operating and recovery rooms (22°C–26°C), temperatures of the intrathecal drugs, and intravenous solutions (room temperature) were comparable. It seems that none of these factors differed from the other studies; therefore, these variations in the results could be explained by the peculiar patient characteristics in the different studies. The antishivering effects of dexmedetomidine are mediated by binding to α2-receptors in the brain and spinal cord,12 which reduce central thermosensitivity via attenuating the conductance of neurons.17
The results of our study showed that the incidence of nausea/vomiting, hypotension, bradycardia, Apgar scores of neonates, and escape doses of rescue drugs for treatment of adverse events (except meperidine) were not significantly different between the two groups. However, the grade of mild sedation (grade 2 and 3) was higher in the BD group than the BN group. It seems that sedation in the absence of nausea and vomiting could provide more comfortable conditions in the potentially stressful environment of the operating room for patients, and thus could prove beneficial for the patient, surgeon, and anesthesia team.
Limitation
When we treat hypotension with further infusion of fluids, we must use stroke-volume variation as an appropriate hemodynamic monitoring, because it is a sensitive monitor of prediction of fluid responsiveness. This was a major limitation of the current study.
Conclusion
We concluded that adding 5 μg dexmedetomidine to heavy bupivacaine in SA can decrease the incidence and intensity of shivering, without any significant adverse effects.
Acknowledgment
Funding was received from Kurdistan University of Medical Sciences.
Disclosure
The authors report no conflicts of interest in this work.
References
Locks GF. Incidence of shivering after cesarean section under spinal anesthesia with or without intrathecal sufentanil: a randomized study. Rev Bras Anestesiol. 2012;62:676–684. | ||
Crowley LJ, Buggy DJ. Shivering and neuraxial anesthesia. Reg Anesth Pain Med. 2008;33:241–252. | ||
Bhattacharya PK, Bhattacharya L, Jain RK, Agarwal RC. Post anaesthesia shivering (PAS): a review. Indian J Anaesth. 2003;47:88–93. | ||
Kranke P, Eberhart LH, Roewer N, Tramèr MR. Pharmacological treatment of postoperative shivering: a quantitative systematic review of randomized controlled trials. Anesth Analg. 2002;453:60–94. | ||
Park SM, Mangat HS, Berger K, Rosengart AJ. Efficacy spectrum of antishivering medications: meta-analysis of randomized controlled trials. Crit Care Med. 2012;40:3070–3082. | ||
Alfonsi P. Postanaesthetic shivering: epidemiology, pathophysiology and approaches to prevention and management. Drugs. 2001;2193:205–261. | ||
Elvan EG, Oç B, Uzun S, Karabulut E, Coşkun F, Aypar U. Dexmedetomidine and postoperative shivering in patients undergoing elective abdominal hysterectomy. Eur J Anaesthesiol. 2008;255:357–364. | ||
Bansal P, Jain G. Control of shivering with clonidine, butorphanol, and tramadol under spinal anesthesia: a comparative study. Local Reg Anesth. 2011;4:29–34. | ||
Usta B, Gozdemir M, Demircioglu RI, Muslu B, Sert H, Yaldiz A. Dexmedetomidine for the prevention of shivering during spinal anesthesia. Clinics (Sao Paulo). 2011;66:1187–1191. | ||
Tsai YC, Chu KS. A comparison of tramadol, amitriptyline, and meperidine for postepidural anesthetic shivering in parturients. Anesth Analg. 2001;93:1288–1292. | ||
Kranke P, Eberhart LH, Roewer N, Tramer MR. Single dose parenteral pharmacological interventions for the prevention of postoperative shivering: a quantitative systematic review of randomized controlled trials. Anesth Analg. 2004;99:718–727. | ||
Bajwa SJ, Gupta S, Kaur J, Singh A, Parmar S. Reduction in the incidence of shivering with perioperative dexmedetomidine: a randomized prospective study. J Anaesthesiol Clin Pharmacol. 2012;28:86–91. | ||
Moawad HE, Elawdy M. Efficacy of intrathecal dexmedetomidine in prevention of shivering in patients undergoing transurethral prostatectomy: a randomized controlled trial. Egypt J Anaesth. 2015;31:181–187. | ||
Qi X, Chen D, Li G, et al. Comparison of intrathecal dexmedetomidine with morphine as adjuvants in cesarean sections. Biol Pharm Bull. 2016;39:1455–1460. | ||
Abdelhamid SA, El-Lakany MH. Intrathecal dexmedetomidine: useful or not? J Anesth Clin Res. 2013;4:1000351. | ||
Gozdemir M, Usta B, Demircioglu RI, Muslu B, Sert H, Karatas OF. Magnesium sulfate infusion prevents shivering during transurethral prostatectomy with spinal anesthesia: a randomized, double-blinded, controlled study. J Clin Anesth. 2010;184:9–22. | ||
Mittal G, Gupta K, Katyal S, Kaushal S. Randomised double-blind comparative study of dexmedetomidine and tramadol for post-spinal anaesthesia shivering. Indian J Anaesth. 2014;58:257–262. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


