Back to Journals » Journal of Multidisciplinary Healthcare » Volume 15
Effect of Daily Multidisciplinary Team Reflection in Ambulatory Care: A Qualitative Analysis
Authors Miyazaki K , Taguchi T, Takemura Y
Received 8 November 2021
Accepted for publication 2 February 2022
Published 22 February 2022 Volume 2022:15 Pages 323—331
DOI https://doi.org/10.2147/JMDH.S348423
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Kei Miyazaki,1 Tomohiro Taguchi,2 Yousuke Takemura3
1Department of Community Medicine NABARI, Mie University School of Medicine, Tsu City, Mie, Japan; 2Community Medicine, Fujita Health University School of Medicine, Toyoake City, Aichi, Japan; 3Department of General Medicine, Northern TAMA Medical Center (Tokyo Metropolitan Health and Hospitals Corporation), Higashimurayama City, Tokyo, Japan
Correspondence: Kei Miyazaki, Department of Community Medicine NABARI, Mie University School of Medicine, 2-174 Edobashi, Tsu City, Mie Prefecture, 514-8507, Japan, Tel +81 59 231 5290, Fax +81 59 231 5289, Email [email protected]
Purpose: Research suggests that daily previsit team huddling leads to improved teamwork, however there are no reports on the effect and mechanism of daily team reflection in primary care practice. To help healthcare professionals to integrate fragmented information and to enhance continuity, we previously developed and implemented a daily multidisciplinary team reflection (DMDTR) approach. The present study aimed to construct a conceptual diagram illustrating how participation in DMDTR influence medical care in an ambulatory clinic.
Participants and Methods: In this qualitative study, we analyzed data from semi-structured interviews (n = 12) conducted with physicians, nurses, and medical assistants who regularly participated in DMDTR. Modified grounded theory approach (M-GTA) was adopted as the analysis method, and structure-construction qualitative research method (SCQRM) was used as a meta-theory to determine the number of cases correlatively with the research objectives.
Results: Our conceptual diagram demonstrated that, through DMDTR, team members shared fragmented information to gain a more holistic view of the patient and discuss diverse points of view, a process that resulted in real-time problem solving through collaboration. This team approach showed benefit to each discipline and improves the care attributes of contextuality, coordination, accessibility, accountability, continuity, and comprehensiveness of care.
Conclusion: We generated a conceptual diagram showing that DMDTR embodies a team approach that leads to improved care attributes, which results in enhanced quality of primary care.
Keywords: interdisciplinary communication, patient care team, patient centered care, qualitative research
Introduction
Fragmentation seems to be at the root of the current global healthcare crisis, which is characterized by problems of unsustainable cost increases, poor quality, and inequalities.1 To reduce fragmentation and foster integration, generalists around the world have sought solutions, such as the introduction of the patient-centered medical home (PCMH) care model.2 As Berry-Millett et al have pointed out, ineffective team care is a barrier to PCMH.3 According to some studies, team huddles promote patient safety in hospitals, especially in the perioperative4 and inpatient settings.5–9 Some recent studies were also done in the primary care area/outpatient setting, but most were pre-visit team huddles and only described the benefits of the huddle, not the mechanism of how the daily wrap-up huddles would work.10–17 In addition, usefulness of the team huddle has been mentioned mostly from the papers from USA, Europe but not from Asia, including Japan.9
Background
Japan’s healthcare system has achieved one of the highest life expectancies in the world with universal health insurance. In the field of primary care in Japan, patients are free to choose and change doctors and medical institutions, making it difficult to maintain continuity and provide integrated care. Under these circumstances, there have been moves to promote team medicine and multi-professional collaboration and revisions to medical fees in Japan in the past 10 years.18 However, these system reforms have only promoted inter-facility cooperation between hospitals and clinics and multi-professional cooperation within hospitals, and have not led to a movement to promote integrated care within primary care facilities.18
Takachaya Clinic is a small primary care clinic with two full-time equivalent physicians and is located in a suburban area (Tsu city, Japan). As the clinic is affiliated to a neighboring community hospital (Tsu Cooperative Hospital), most of the physicians spend their working hours in the hospital rather than in the clinic. Furthermore, most of the nurses and medical assistants work part-time. As fragmented information and loss of continuity is a concern, we have developed a daily multidisciplinary team reflection (DMDTR) approach, which has been implemented since 2010. After every half-day clinic, all staff involved in patient care (physicians, nurses, and medical assistants) spend 10 to 30 minutes sharing information and discussing patient care.
The format of the DMDTR is as follows:
- SELECT: Team members SELECT the patients to be discussed. Selection criteria include patients that are medically unstable, have medically unresolved issues, have high social support needs, have family problems, have medical problems characterized by uncertainty, and are complex cases.
- SHARE: The team SHARE information about the patient.
- DISCUSS: The team DISCUSS patient management using the biopsychosocial approach.
- PLANS: The team generate follow-up PLANS using a checklist describing WHO, WHEN, and HOW.
- FOLLOW-UP: During the following morning huddle or the next DMDTR, the team share FOLLOW-UP results from the previous DMDTR.
The aim of this study was to construct a conceptual diagram illustrating how DMDTR participation influences medical care in an ambulatory clinic to promote the adoption of team huddles, DMDTR in primary care settings in Japan and around the world.
Materials and Methods
Setting
The study was conducted in one suburban family medicine clinic.
Theory and Participants
Modified grounded theory approach (M-GTA) was adopted as the analysis method, and SCQRM was used as a meta-theory to determine the number of cases correlatively with the research objectives.
SCQRM is a meta-research method that uses structural constructivism as a super-meta-theory (super-epistemology), with “interest correlation” as its core principle, and the number of cases can be determined correlatively with the research objective.19–22 SCQRM, developed by Saijo determines the number of cases or samples based on the research questions or interest of researchers, which preserve scientific validity and refutability with a small case study by structuring and showing the trajectory of construction of the model under study.
As an analytical method, we adopted the modified grounded theory approach (M-GTA), which allows the use of graphical representation for model building. In M-GTA based on SCQRM, saturation (purpose-correlated structural saturation) can be defined as the state in which the model created by completing the analysis worksheets for each concept can achieve the research objectives.
The number of participants (12) was defined as all the workers involved in patient care in the facility who agreed to participate in the study, based on the purpose of this study.
All physicians, nurses, and medical assistants who regularly participated in the DMDTR were invited to take part in the study. All three physicians, all three medical assistants, and six of the seven nurses agreed to participate. Overall, 92% of the requested members participated in our study.
Intervention
Semi-structured face-to-face interviews were conducted in a quiet room with no interruptions between February and April 2013. Interviews were conducted by KM, who is a full-time physician in Takachaya Clinic. Each interview lasted between 20 and 60 minutes. Using the following keywords, participants were asked how DMDTR influenced their patient care. All interviews were transcribed verbatim and to avoid any information distortion caused by the respondent’s poor state in the interview, we had the participants refer to the transcribed verbatim transcripts to confirm that there are no errors in the content.
After all the interviews were completed, a simple questionnaire consisting of the following questions was administered to store the missing information.
Do you think that there are times when the multidisciplinary review picks up things that were not covered or were overlooked in the medical treatment? If yes, please give specific examples.
Keywords
The five keywords, Accessibility, Comprehensiveness, Coordination, Continuity and Accountability were adopted from the Institute of Medicine report as the five attributes essential to the good practice of primary care.23,24 We also adopted the keywords, Access to Care, Continuity of Care, Comprehensive Care, Coordination of Care, and Contextual Care, which have been defined as fundamental principles of family medicine by Saultz.25 A final total of six key words were summarized in Table 1.
 |
Table 1 Six Keywords Used in Semi-Structured Interviews |
Analysis
A modified grounded theory approach (M-GTA) developed by Kinoshita was used.26 M-GTA is a qualitative study approach, in which concepts are generated one by one from the data and then several concepts are combined into broader categories using an analysis worksheet. M-GTA can be used to map relationships among the categories generated and to construct a conceptual model.
Transcribed sentences were examined by KM. Sentences or passages that had similar themes or patterns were grouped and variation within each category identified, with concrete examples. The category groups were then given concept names. One analysis worksheet was created for each concept. The worksheet recorded the concept name, its definition, concrete examples (quotations from participants), theoretical notes with opposite examples, and analysis perspectives. A sample analysis worksheet is shown in Table 2.
 |
Table 2 Analysis Worksheet (Sample) |
These concepts were combined to form a hypothesis, which was summarized in a conceptual diagram.
The actual work process consisted of creating an analysis worksheet from the verbatim transcripts of the interviews, conducting the next interview while constructing the overall conceptual diagram, and repeating the analysis worksheet to complete the interviews with all participants. When reconstructing the overall conceptual diagram from the analysis worksheets for each concept completed at that stage, we determined that there was missing information, so we conducted the aforementioned questionnaire. By combining the information obtained from the questionnaire, it was judged that information necessary to create the analysis worksheet and the overall conceptual diagram was satisfied, and that purpose-correlative structural saturation had been reached.
The content of generated thematic units and the conceptual diagram were reviewed by TT, a researcher experienced in qualitative approaches.
Results
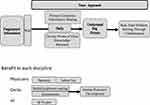
All thematic units were summarized into a conceptual diagram. Generated concepts are shown in gray rounded square boxes in the conceptual diagram (Figures 1 and 2).
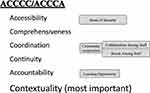 |
Figure 2 Conceptual diagram: 6 attributes of care and generated concepts. Generated concepts are described in gray rounded square boxes. |
Thematic units are described below. Derived concepts are shown in boldface type, and examples quotes are shown in italics.
Fragmented Information
Example quotes:
Since most of the information is obtained in the examination room, very little of the information obtained by other professionals is recorded in the medical record, as I mentioned earlier.
Each patient shows different attitudes to physicians, nurses, and medical assistants, which is described as fragmented information. As there is a dividing wall between the examination rooms and the reception (waiting) room, physicians and medical assistants do not know what is happening in other rooms. Nurses may pass back and forth beyond the wall, but are not necessarily aware of everything that happens.
Team Approach
Through DMDTR, team members share information gathered by each member during their own encounters with patients and also share diverse points of view, knowledge, and resources based on their own expertise.
Example quotes:
As a clerk, I see the patient’s condition outside the examination room and the family’s condition, but when someone from another profession comes in, I hear that nurses are different and so are doctors.
Being aware of privacy is very important, as patients may not necessarily agree to share information about themselves with other members of the team. Therefore, we termed this concept privacy-conscious information sharing. In this way, the team gains a holistic view of the patient and is able to solve problems through collaboration. Daily collaboration enables real-time problem solving, which we summarized as real-time problem solving through collaboration. This series of processes was termed the team approach.
Example quotes:
I think it would be better if the frequency is every half day. If we don’t do it in real time, we can’t do it all at once later. We can respond quickly to the patients, so I think it’s good to do it after the half-day is over.
Benefits to Each Discipline
Physicians are able to speed up their practice by prioritizing issues that needed to be addressed on the spot, such as accurate diagnosis and treatment, and leave the collection of background information related to long-term care such as family, environment, and care situation, for later DMDTR. Nurses and medical assistants are able to pick up things missed by physicians, a process described as a safety net.
Through DMDTR, medical assistants will become more familiar with the patient and are expected to proactively provide patient information. They will start to autonomously develop their own role, rather than to mechanically perform receptionist tasks. Medical assistants begin to act beyond the scope of their own disciplinary roles, a process described as multidisciplinary tasking. A good example is proactively triaging a seemingly ill patient in the waiting room. A more autonomous attitude is not only related to multidisciplinary tasking, but also to human resource development.
Finally, DMDTR is a good opportunity to generate new ideas for quality improvement projects.
Attributes of Care (ACCCC/ACCCA)
6 attributes of care and generated concepts are illustrated in Figure 2.
Accessibility
The participants interpreted the sharing of reflections as a way to ensure mental proximity and security. DMDTR enhances patients’ beliefs that the clinic staff know me well, which makes them feel more at home in the clinic and improves their sense of security.
Example quotes:
Reflecting together, for example, if you have a family member who is sick, it is possible to ask about him or her and talk to him or her in the waiting area, so they are more likely to be psychologically attached to the clinic.
Comprehensiveness
Participants described the concept as looking at the patient holistically, including prevention, mind and body, regardless of age, gender, or organ.
Example quotes:
You can learn about the history and the current situation, including the economic situation, so you can have a comprehensive view.
Coordination
There were many mentions of three concepts: collaboration with the Community, collaboration among staff, and bonds among staff.
Example quotes:
For example, (as a result of DMDTR) we frequently applied for nursing care insurance, contacted care managers, and we often approached other people and the environment surrounding the patient.
Continuity
Continuity was described as connecting fragmented care by being involved even when patients are not sick, or by continuing to follow them in outpatient, inpatient, and outpatient settings throughout their hospitalization.
Example quotes:
When we look back at the reason why the person was admitted to the hospital and the current situation, we pick up the hospitalized person’s chart, and the head nurse provides us with information, which we share with everyone.
Accountability
Accountability was described as monitoring the content of the medical care provided, studying it as necessary, improving it, and explaining it well to the patient. DMDTR often accompanies mini-lectures, which are good learning opportunities that help the participants to improve their ability to enhance accountability.
Example quotes:
I think there is a learning effect. The various staff members understand that the doctor has done this kind of assessment on the patient and that this is what they would like to see done.
Contextuality
Many of the participants recognized contextuality as most important among six attributes of care. Contextuality represents aspects such as the patient’s values, thoughts, wishes, clinical course, background, and family status.
Example quotes:
I think this is actually the most beneficial effect of reflection. It is difficult for patients to express their values, thoughts, and feelings are difficult to express in a short period of time in a doctor’s office, which makes it difficult for us to respect them, but gathering information from multiple professions has a very positive impact.
Discussion
Together with the previsit team huddle, which has been shown to improve teamwork, DMDTR further enhances a team approach by improving the quality of primary care. As many participants in our study pointed out, contextuality was the most important of the six attributes. By integrating fragmented patient information, the team is able to gain a holistic view of the patient, mainly through acquiring information related to the context of the patient. This approach can foster a healing relationship, which leads to trust, hope, and a sense of being known, as described by Scott et al.27
Reflection is a well-known tool to improve quality of care.28 This study demonstrated that the so-called 3Ds (Dedicated time, Diversity, Daily) are important factors. Dedicated time, or protected time to sit together and discuss the patient, is necessary for interprofessional collaboration.29 Goldman et al have suggested that prioritizing regular time periods for all employees to contribute to practice discussions allows a team to make positive changes in a practice and to sustain those changes over time.30 Diversity is another important keyword for a successful team. As shown in our conceptual diagram, the sharing of diverse points of view from individuals with different expertise is important, and this diversity of perspectives enhances group problem solving and creativity.29 Daily reflection is another important concept. Previous studies have shown that weekly staff meetings enhance the team approach.31 All our participants agreed that daily reflection was needed to resolve a range of issues in a timely manner. They also agreed that a period of up to 30 minutes for the daily meeting was an acceptable burden.
Although the findings suggest that dedicating protected time is important, this is one of the main inhibiting factors when newly introducing DMDTR. Xyrichis and Lowton reported that factors inhibiting or facilitating interprofessional teamworking in primary and community care settings include organizational support and team size. It is important for the team to physically sit together and have protected time in which to discuss patient care.32 Team members may be reluctant to newly allocate time for DMDTR, particularly in settings where a “we” paradigm has not yet been established. As described by Ghrob and Bodenheimer, the “we” paradigm involves reallocating responsibilities, not just tasks, so that all team members share responsibility for and contribute meaningfully to the health of their patient panel33 As we found in our practice, once DMDTR is implemented, a “we” paradigm will be fostered among team members and they will realize that spending 20–30 minutes for DMDTR is worth the time.
Limitations
This study was conducted in 2013, and since then, despite progress in advanced medicine and other areas, the most significant advancement in primary care settings has been the introduction of electronic medical records, and the importance of human interaction remains the same as before in Japan. In addition, as mentioned in the background, there has been a movement to promote team medicine and multi-professional cooperation in Japan over the past decade, but it has been limited to promoting cooperation among facilities and multidisciplinary cooperation within hospitals, and the current lack of multidisciplinary cooperation in primary care settings remains almost unchanged.18
The importance of further promoting multidisciplinary cooperation in primary care field, mainly clinics, is expected to be the same in other countries in 2022.
The model developed in this study shows how multidisciplinary reflections affect the quality of medical care in a relatively small clinic in Japan where multiple physicians work in shifts. It is presumed that this model can be applied to primary care clinics in similar settings in Japan, but whether it can be applied to large hospitals and other countries needs to be treated with caution.
Conclusion
We generated a conceptual diagram showing that DMDTR embodies a team approach, has benefit to each discipline, and enhances the six attributes of care.
Data Sharing Statement
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Ethics Approval and Informed Consent
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the research ethics committee at Mie Health CO-OP Tsu Cooperative Hospital (approval number TCH2013K001). Written informed consent was obtained from all individual participants included in the study.
Consent for Publication
Consent for publication was obtained from all individual participants included in the study.
Acknowledgments
The authors are extremely grateful to the Takachaya Clinic staff members who participated in this study. We thank Diane Williams, PhD, from Edanz Group for editing a draft of this manuscript.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This research was funded by the Fund for Establishing Centers for Fostering Medical Researcher of the Future Project, Ministry of Education, Culture, Sports, Science and Technology, Japan. The study sponsor had no involvement in the study design; in the collection, analysis, and interpretation of data; in writing the manuscript; or in the decision to submit the manuscript for publication.
Disclosure
None of the authors have any financial or intellectual conflicts of interest related to this study.
References
1. Stange KC. The problem of fragmentation and the need for integrative solutions. Ann Fam Med. 2009;7(2):100–103. doi:10.1370/afm.971
2. Academy of Family Physicians A. Joint principles of the patient-centered medical home; 2007. Available from: https://www.aafp.org/dam/AAFP/documents/practice_management/pcmh/initiatives/PCMHJoint.pdf.
3. Berry-Millett R, Bandara S, Bodenheimer T. The health care problem no one’s talking about. J Fam Pract. 2009;58(12):633–637.
4. Glymph DC, Olenick M, Barbera S, Brown EL, Prestianni LMC, Miller C. Healthcare utilizing deliberate discussion linking events (HUDDLE): a systematic review. AANA J. 2015;83(3):183–188.
5. Brady PW, Muething S, Kotagal U, et al. Improving situation awareness to reduce unrecognized clinical deterioration and serious safety events. Pediatrics. 2013;131(1):e298–e308.
6. Goldenhar LM, Brady PW, Sutcliffe KM, Muething SE. Huddling for high reliability and situation awareness. BMJ Qual Saf. 2013;22(11):899–906. doi:10.1136/bmjqs-2012-001467
7. Ryan S, Ward M, Vaughan D, et al. Do safety briefings improve patient safety in the acute hospital setting? A systematic review. J Adv Nurs. 2019;75(10):2085–2098. doi:10.1111/jan.13984
8. Franklin BJ, Gandhi TK, Bates DW, et al. Impact of multidisciplinary team huddles on patient safety: a systematic review and proposed taxonomy. BMJ Qual Saf. 2020;29(10):844–853. doi:10.1136/BMJQS-2019-009911
9. Pimentel CB, Snow AL, Carnes SL, et al. Huddles and their effectiveness at the frontlines of clinical care: a scoping review. J Gen Intern Med. 2021;36(9):2772–2783. doi:10.1007/s11606-021-06632-9
10. Rodriguez HP, Meredith LS, Hamilton AB, Yano EM, Rubenstein LV. Huddle up!: the adoption and use of structured team communication for VA medical home implementation. Health Care Manage Rev. 2015;40(4):286–299. doi:10.1097/HMR.0000000000000036
11. Stroebel CK, McDaniel RR, Crabtree BF, Miller WL, Nutting PA, Stange KC. How complexity science can inform a reflective process for improvement in primary care practices. Jt Comm J Qual patient Saf. 2005;31(8):438–446. doi:10.1016/s1553-7250(05)31057-9
12. Kellish AA, Smith-Miller C, Ashton K, Rodgers C. Team huddle implementation in a general pediatric clinic. J Nurses Prof Dev. 2015;31(6):324–327. doi:10.1097/NND.0000000000000220
13. Picciano A, Winter RO. Picciano & winter 2013. Fam Med. 2013;45(7):501–504.
14. Taliani CA, Bricker PL, Adelman AM, Cronholm PF, Gabbay RA. Implementing effective care management in the patient-centered medical home. Am J Manag Care. 2013;19(12):957–964.
15. Gale RC, Asch SM, Taylor T, et al. The most used and most helpful facilitators for patient-centered medical home implementation. Implement Sci. 2015;10(1):1–11. doi:10.1186/s13012-015-0246-9
16. Nagelkerk J, Thompson ME, Bouthillier M, et al. Improving outcomes in adults with diabetes through an interprofessional collaborative practice program. J Interprof Care. 2018;32(1):4–13. doi:10.1080/13561820.2017.1372395
17. Biernacki PJ, Champagne MT, Peng S, Maizel DR, Turner BS. Transformation of care: integrating the registered nurse care coordinator into the patient-centered medical home. Popul Health Manag. 2015;18(5):330–336. doi:10.1089/POP.2014.0131
18. Kato D, Ryu H, Matsumoto T, et al. Building primary care in Japan: literature review. J Gen Fam Med. 2019;20(5):170–179. doi:10.1002/jgf2.252
19. Saijo T. Live lecture series. what is qualitative research? (SCQRM basics) (In Japanese). Shin-yo-sha; 2007.
20. Saijo T. Live lecture series. What is qualitative research? (SCQRM advanced) (In Japanese). Shin-yo-sha; 2008.
21. Iwata K, Shirai C, Kimura K, et al. How were the high-fever consultation center perceived by the officers who provided it in Kobe City, during swine-origin influenza a (H1N1) outbreak? A qualitative study utilizing SCQRM. Kobe J Med Sci. 2010;56(5):195–203.
22. Kitaoka K. A qualitative analysis of films focusing on students’ L2 WTC, language anxiety, and learner autonomy. ATEM J. 2019;24:31–44.
23. Institute of Medicine. A Manpower Policy for Primary Health Care. Washington, D.C.: National Academies Press; 1978. doi:10.17226/9932
24. Institute of Medicine (US) Committee on the Future of Primary Care. Primary Care: America’s Health in a New Era. Donaldson MS, Yordy KD, Lohr KN, Vanselow NA, editors. Washington, D.C.: National Academies Press; 1996. doi:10.17226/5152
25. Saultz JW. Textbook of Family Medicine: Defining and Examining the Discipline. McGraw-Hill, Health Professions Division; 2000.
26. Kinoshita Y. Live lecture series. modified grounded theory approach. Practical qualitative research methods. (In Japanese). Kobundo; 2007.
27. Scott JG, Cohen D, DiCicco-Bloom B, Miller WL, Stange KC, Crabtree BF. Understanding healing relationships in primary care. Ann Fam Med. 2008;6(4):315–322. doi:10.1370/afm.860
28. Ménard L, Ratnapalan S. Teaching moment: reflection in medicine: models and application. Can Fam Physician. 2013;59(1):
29. Roth LM, Markova T. Essentials for great teams: trust, diversity, communication… and joy. J Am Board Fam Med. 2012;25(2):146–148. doi:10.3122/jabfm.2012.02.110330
30. Goldman J, Meuser J, Rogers J, Lawrie L, Reeves S. Interprofessional collaboration in family health teams: an Ontario-based study. Can Fam Physician. 2010;56(10):e368–e374.
31. Craigie FC, Hobbs RF. Exploring the organizational culture of exemplary community health center practices. Fam Med. 2004;36(10):733–738.
32. Xyrichis A, Lowton K. What fosters or prevents interprofessional teamworking in primary and community care? A literature review. Int J Nurs Stud. 2008;45(1):140–153. doi:10.1016/j.ijnurstu.2007.01.015
33. Ghorob A, Bodenheimer T. Share the CareTM: building teams in primary care practices. J Am Board Fam Med. 2012;25(2):143–145. doi:10.3122/jabfm.2012.02.120007
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.