Back to Journals » Clinical Epidemiology » Volume 9
Effect modification, interaction and mediation: an overview of theoretical insights for clinical investigators
Authors Corraini P , Olsen M, Pedersen L, Dekkers OM , Vandenbroucke JP
Received 8 December 2016
Accepted for publication 28 April 2017
Published 8 June 2017 Volume 2017:9 Pages 331—338
DOI https://doi.org/10.2147/CLEP.S129728
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Irene Petersen
Priscila Corraini,1 Morten Olsen,1 Lars Pedersen,1 Olaf M Dekkers,1,2 Jan P Vandenbroucke1–3
1Department of Clinical Epidemiology, Institute of Clinical Medicine, Aarhus University Hospital, Aarhus, Denmark; 2Leiden University Medical Center, Leiden, the Netherlands; 3Department of Epidemiology and Population Health, London School of Hygiene and Tropical Medicine, London, UK
Abstract: We revisited the three interrelated epidemiological concepts of effect modification, interaction and mediation for clinical investigators and examined their applicability when using research databases. The standard methods that are available to assess interaction, effect modification and mediation are explained and exemplified. For each concept, we first give a simple “best-case” example from a randomized controlled trial, followed by a structurally similar example from an observational study using research databases. Our explanation of the examples is based on recent theoretical developments and insights in the context of large health care databases. Terminology is sometimes ambiguous for what constitutes effect modification and interaction. The strong assumptions underlying the assessment of interaction, and particularly mediation, require clinicians and epidemiologists to take extra care when conducting observational studies in the context of health care databases. These strong assumptions may limit the applicability of interaction and mediation assessments, at least until the biases and limitations of these assessments when using large research databases are clarified.
Keywords: methods, epidemiology, effect modifiers, stratified analyses, health care administrative claims
Corrigendum for this paper has been published
Further corrigendum has been published
Introduction
The concepts of effect modification, interaction and mediation have long existed in epidemiology to help understand different aspects of diseases or conditions, their treatments and risk factors.1–4 Yet, literature on these notions has rarely been adapted to facilitate the understanding of the clinical reader.5 In this article, we revisited the notions of effect modification, interaction and mediation for clinical investigators. In addition, we examined the applicability of these notions for clinical research in the context of observational investigations using health care databases.
Research efforts using epidemiological tools to solve clinical problems are often aimed to study preventive or therapeutic interventions. As such, we illustrate the application of the three epidemiological concepts with simple representations of their use in optimal clinical experiments, i.e., randomized controlled trials (RCTs). In RCTs, interventions are clearly stated. Due to the randomized study design, potential known and unknown confounding have been accounted for.6,7
On the other hand, routinely collected health care data are an increasingly relevant source for clinical epidemiological research.8 The use of such observational data may fill important research gaps left by clinical experiments.9,10 However, inherent limitations of health care databases may hamper their use, highlighting the need to assess feasibility and validity of studies that use this type of data.8,11 Therefore, for each concept, we transpose our “best-case scenario” RCT example to an example from an observational experiment and discuss the realities of observational designs when using health care research databases.
Terminology and motivation to assess effect modification, interaction and mediation
The notions of effect modification, interaction and mediation represent conceptually different, although potentially interdependent notions. These subtle different notions address different research aims, which are related to different aspects of an exposure–outcome relationship (Box 1).
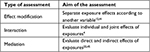  | Box 1 Main motivation for the assessment of effect modification, interaction and mediation. |
Effect modification
The clinical motivation behind the assessment of effect modification is to identify whether the effect of a treatment (or exposure) is different in groups of patients with different characteristics. If the effects are the same, the treatment (or exposure) effect is called homogeneous; if the effects are different, they are called heterogeneous.12
For example, one may be interested in whether the adverse effect of a new anti-inflammatory drug, e.g., gastrointestinal bleeding, is heterogeneous between men and women or between old and young. Researchers may use the age and sex of a patient to select those at high risk or to identify subgroups that would benefit the least or the most from a therapy.13
Assessing effect modification may also help to identify a subset of patients who would not benefit from an intervention at all. For example, when assessing the effect of topiramate treatment for alcohol dependence, researchers identified effect modification by a genetic marker: only carriers of the CC allele of the rs2832407 genotype would benefit from the topiramate treatment (Figure 1).
  | Figure 1 Mean (95% CI) heavy drinking days per week by topiramate (green circle) or placebo (red square) intervention group. Notes: (A) Main analysis; (B) analysis in three different alleles of the rs2832407 genotype. Adapted from Kranzler et al14 with permission from the American Journal of Psychiatry (Copyright ©2014). American Psychiatric Association. All Rights Reserved. |
In general, if one were to plan an RCT to test a hypothesis of effect modification, a single intervention suffices. The abovementioned example was an RCT on the effectiveness of topiramate vs placebo.14 In this RCT, the effect of the intervention was assessed in patients with three different alleles of the rs2832407 genotype (CC, AC and AA; Figure 1). As illustrated in Figure 1A, compared with placebo, topiramate resulted in a higher decrease in the average number of heavy drinking days per week. This effect of the intervention was observed in patients with the CC allele, but not in patients with the AC or AA alleles (Figure 1B). Thus, the main effect was heterogeneous and modified by the rs2832407 genotype.
With regard to effect modification in investigations based on observational data, the same principle from the RCT can be applied. For example, the Million Women Study was a cohort study including about one of every four women aged 50–64 years in the United Kingdom during 1996–2001. This study included 716,738 postmenopausal women with information on hormone replacement therapy (HRT).15 In this study, the use of continuous, combined HRT with progestogen and estrogen decreased the risk of endometrial cancer compared with never HRT use (relative risk = 0.71, 95% CI: 0.56–0.90).15 To assess effect modification by body mass index (BMI) at study entry, the effect of combined HRT was assessed in three subgroups of different BMI (<25, 25–29, and ≥30).
The result of the assessment of effect modification by BMI in a stratified analysis is represented in Table 1. Hereby, the main effect was consistent only in the subgroup of women with BMI ≥ 30 kg/m2 at study entry. Thus, only women with BMI ≥ 30 kg/m2 seem to have their risk of endometrial cancer reduced by HRT. More details on the assessment of effect modification using stratification are provided in the Supplementary materials.
  | Table 1 Relative risk of endometrial cancer in postmenopausal women continuously using combined hormone replacement therapy (HRT), and the effect modification by body mass index (BMI) Note: Data from the Million Women Study.15 |
Interaction
Interaction is of interest when researchers want to obtain the joint effect of two (or more) exposures on a disease or outcome.4 To be considered a synergistic interaction, the joint effect has to be higher than the effect expected by the sum of their individual effects. Conversely, there is an antagonistic interaction between exposures, when the joint effect is less than the sum of their individual effects. This is in contrast to effect modification, where the effect of an exposure on an outcome is assessed in different strata of a third variable, but a joint effect is not assessed.
From a clinical perspective, to assess interaction is particularly important when a disease can be treated by a combination of two or more treatments. For example, the use of combined antithrombotic therapy has increased since the introduction of new anticoagulants. Researchers may be interested in whether combining antithrombotic drugs decreases the risk of heart disease as a joint effect from the therapy, over and beyond the separate effect of each, single drug.
For an RCT to examine interaction, a single intervention does not suffice: two or more interventions should be studied, leading to a factorial design.16 For example, the Thrombosis Prevention Trial examined the joint effect of low-dose aspirin and warfarin for the prevention of ischemic heart disease.17 The trial included 5,499 men aged between 45 and 69 years in the United Kingdom. The investigators examined whether the combined effect of the two therapies was over and beyond the separate effect of each, single therapy. To address interaction between antithrombotic therapies in this RCT, the incidence of ischemic heart disease was assessed in four experimental groups, viz. a four-arm intervention trial. The four interventions consisted of treatment with aspirin alone, warfarin alone, aspirin plus warfarin or double placebo (Table 2).
  | Table 2 Incidence rate of ischemic heart disease after the use of single or combined antithrombotic therapy with low-dose aspirin and warfarin Note: Data from the Medical Research Council’s General Practice Research Framework.17 |
To assess interaction, the incidence rates provided in Table 2 give an interaction contrast of 1.5 per 1,000 person-years. The interaction contrast is calculated as the reduction in heart disease rate due to aspirin among those receiving warfarin (10.3–8.7 = 3.1) minus the rate reduction due to aspirin among those not receiving warfarin (13.3–10.2 = 1.6). As the interaction contrast exceeded zero, synergy between the two therapies can be concluded. For each year, an additional reduction of 1.5 new heart disease patients for every 1,000 treated individuals may be achieved by combining warfarin and aspirin to prevent ischemic heart disease. This was the surplus of the expected summed effects of each, single therapy. Thus, combining warfarin and aspirin was more effective in reducing ischemic heart disease than either agent on its own.17 The assessment of interaction using incidence rates or risks, as defined by the interaction contrast, is described in the Supplementary materials.
In observational investigations using health care research databases, the same principle can be applied (Table 3). Using administrative databases from Denmark between 2000 and 2004, Hallas et al18 addressed another interaction hypothesis about antithrombotic therapies. The authors hypothesized that the combination of aspirin and clopidogrel increases the risk of bleeding, as an adverse effect of the therapy, over and beyond the separate effect of each single therapy. To assess interaction, they performed a case–control study. Three types of effects were obtained by regression analysis: the effect of aspirin use alone, the effect of clopidogrel use alone and the joint effect of aspirin and clopidogrel use, in relation to no antithrombotic use at all (Table 3).19
  | Table 3 Use of single and combined antithrombotic therapy and risk of serious upper gastrointestinal bleeding in a case–control study using research databases in Denmark, 2000–2004 Note: Data from Hallas et al.18 |
The odds ratios (ORs) provided in Table 3 can be used to obtain another interaction measure, namely the relative risk due to interaction. In this example, the relative risk due to interaction can be computed by subtracting the effect among the double-exposed group by the effects of the two single-exposed groups, added by one, i.e., (12.6) − (3.1) − (2.4) + 1 = 8.1. By obtaining this relative risk due to interaction, the likelihood of serious upper gastrointestinal bleeding from the combined use of aspirin and clopidogrel was eight times higher than the likelihood expected by the addition of the two drugs. The assessment of interaction using the relative risk due to interaction and other standard methods, as well as a discussion on the key role of different effect measures in interaction assessment, is given in the Supplementary materials.
For clarity, we relate the description of interaction to the previous description of effect modification to show how they are conceptually different. These conceptual differences have implications for their assessments. For instance, as a thought experiment using the same example of combined antithrombotic therapy, let us assume that we want to assess effect modification and not interaction. Using the effect modification terminology, one would hypothesize that the effect of aspirin is heterogeneous between those using and not using clopidogrel. Therefore, only one effect (e.g., aspirin use) is of interest, and it is compared over two or more subgroups. The effect of the variable defining the subgroups is not measured (e.g., clopidogrel use).
Mediation
Mediation assessment is motivated by a wish to understand the pathways, whereby an exposure leads to an outcome.3 To be a mediator, or an intermediate,20 a variable may be a step in the chain of events, or pathways, between the exposure and the outcome (Figure 2). This means that the intermediate may partially, or entirely, account for the association between the exposure and the outcome.21
  | Figure 2 Relation between the exposure – the intermediate or mediator – and the outcome. |
In practical terms, a researcher will be interested in examining mediation to know in which pathways one might interfere to lessen the risk for a disease, or to ameliorate an outcome. In this framework, mediation assessment may help to identify different potential targets to intervene on a disease.22,23
For example, fibromyalgia patients can be treated with pregabalin, 600 mg/day, to restore patient sleep. Doctors are interested in whether the therapy works on restorative sleep not only by reducing insomnia but also by reducing pain. In this example, treatment with pregabalin is the exposure; pain reduction is referred to as the intermediate or mediator, and restorative sleep is the outcome (Figure 2).
As represented in Figure 2, the idea behind the assessment of mediation involves disentangling the total effect of the exposure on the outcome (irrespective of any intermediate), in two (or more) effects: the effect that acts through the intermediate, and the effect that is not explained by the intermediate.3,24,25 The effect that acts through the intermediate is called the indirect effect, sometimes referred to as the mediated effect.23 In turn, the effect that is unexplained by the intermediate is called the direct effect. As the total effect intuitively represents the sum of the direct and the indirect effects,24 one can examine mediation by obtaining the total effect, and either the direct or indirect effect.
This type of mediation assessment was performed using the results of an RCT on the effect of pregabalin (vs. placebo) among fibromyalgia patients.26 The mediation hypothesis was that pregabalin improves restorative sleep via pain reduction. To examine mediation, two effects were estimated: the total effect of pregabalin on restorative sleep, and the indirect effect acting through an intermediate variable that quantified pain. The intermediate variable was measured post randomization.27
Using the results provided in Table 4, from the total pregabalin effect of −1.295, an indirect effect of −0.718 was attributed to pain reduction. The magnitude of the indirect corresponded to 55% of the total pregabalin effect on restorative sleep. Thus, pain reduction might mediate the effect of pregabalin on restorative sleep in fibromyalgia patients. This information could be useful, for example, to test new therapies to improve restorative sleep in fibromyalgia. If restorative sleep is improved by pain reduction, other treatments affecting pain may also improve restorative sleep.
  | Table 4 Total effect of fibromyalgia treatment (pregabalin vs placebo) on restorative sleep improvement (measured using the Sleep Quality Daily Diary score), and indirect effect via pain scale reduction Note: Data from the randomized controlled trial (RCT) published by Mease et al26 and analyzed by Russell et al.27 |
In observational studies using health care research databases, the same principle from the RCT design can be applied. Using data from the case–control Leiden Thrombophilia Study,28 Le Cessie et al29 investigated the association between a genetic exposure (the presence of blood O type) and the occurrence of deep venous thrombosis. The researchers were particularly interested in whether the association could be mediated by clotting factor VIII.
In Table 5, two types of effects are given. The total effect was first measured as the OR for deep venous thrombosis among non-O blood type individuals. This effect could occur via several mechanisms, irrespective of clotting factor VIII. The direct effect of non-O blood type was then measured as the effect not occurring via the potential intermediate by adjusting the initial analysis for clotting factor VIII. The total effect was attenuated from 2.0 to 1.5. As mentioned earlier, the total effect intuitively represents the sum of the direct and indirect effects,24 and here, the direct effect was inferior to the total effect. Thus, there was an indirect effect, and factor VIII may mediate the association between non-O blood type and deep venous thrombosis. The estimation of mediation using those direct, indirect and total effects by standard methods is summarized in the Supplementary materials, and described in detail by MacKinnon.30
  | Table 5 Total effect of blood group (non-O vs O) on the occurrence of deep venous thrombosis, and the direct effect of blood group on the occurrence of deep venous thrombosis, from the case–control Leiden Thrombophilia study Note: Data from Le Cessie et al.29 |
Challenges and opportunities when assessing effect modification, interaction and mediation using research databases
The assessment of effect modification, as well as newer, complex analysis techniques that address interaction and mediation, seems very attractive when using research databases. Most of these analyses need large sample sizes, and often research databases can provide large numbers of study participants.10 However, there are intricacies of the newer techniques that even large data availability might not solve. In particular, because the right type of data might be lacking.
In comparison with the best-case scenario RCT experiment, some common problems in observational studies can affect the validity of estimations of effect modification, mediation and interaction using large databases. Indeed, these estimations are demanding in terms of the confounding and independency assumptions that needs to be fulfilled, and may even be more sensitive to selection bias31 and measurement error.
Confounding
A central problem affecting the interpretation of all three assessments is confounding. General issues about confounding were explained in an intuitive way for the clinical reader by Freemantle et al.32
Very few associations between an exposure and outcome, e.g., those involving genetic exposures, may be exempted from confounding in observational investigations. On the other hand, exposure–outcome relations from which lifestyle factors may be associated with both the exposure and the outcome are more subject to confounding in observational studies using research databases. In Danish databases, for instance, information on potential confounders such as smoking and lifestyle factors is frequently missing or incomplete.33,34 This may improve with optimization of clinical information contained in national databases, with the inclusion of information stemming from general practitioners, and integration to more specialized, clinical databases for a part of the population.35,36 More promising is the implementation of electronic medical records for research. Using electronic medical records in association with database research, more detailed knowledge about potential confounders could be obtained for a much larger proportion of the population. However, a widespread use of such detailed electronic patient data through health care databases for research is still a scenario for the future.
Assumptions about “no confounding” that are needed to assess interaction, and in particular mediation, are stricter than those needed to assess a direct exposure–outcome relation. To examine interaction, researchers need to control for confounding of the exposure and outcome relations for all the exposures that constitute the joint effect.23,37 Confounders of at least one of these relations could explain synergy or antagonisms between exposures when there is none.38 Confounding assumptions to assess interaction may be less strict in public health scenarios where only one of the interacting exposures is intended to be modified by intervention.37,39,40 In this scenario, only unmeasured confounding between the main exposure and the outcome may be a concern. Such examples can be found in the work by VanderWeele and Knol37 and VanderWeele and Robins.41
Using standard mediation analysis, it is possible but not sufficient to control for confounding of the exposure and outcome relationship. Mediation assessment has the additional assumption of no confounding in the relation between the intermediate and the outcome. While sensitivity analyses or more advanced analyses approaches may circumvent this problem, it is not possible to control or adjust for confounding between the intermediate and the outcome directly from the simpler, standard analysis approaches.22,24,42
Independency
The second main difficulty faced when assessing interaction using research databases is that the planned exposures to examine joint effects need to be considered independent from each other.2,43 Logically, a joint effect cannot represent the sum of its separated effects, if the effects cannot be separated. This separation has been claimed rather unrealistic outside RCTs, because interacting exposures such as environmental factors or behaviors may often be associated with one another.44
Mediation assessments presuppose no interaction between the exposure and the intermediate.45 However, as clinical questions posed in mediation presuppose a relation among exposure, the intermediate and the outcome, the effect of the exposure on the outcome could work via the intermediate, irrespective of the intermediate, or both. Standard approaches to assess mediation do not allow to accommodate a possible mediator–exposure interaction.45 Nonstandard, newer approaches are conceptually complicated, and as yet not completely settled.24,46 As such, researchers have to assume no mediator–exposure interaction (or relax this assumption).
Measurement error
The last main problem is measurement error.29 In interaction assessments, types of measurement error that would only affect sample size requirements in an exposure–outcome relation might affect estimates of effect modification and interaction, even by producing appearance of interaction where there is none.47,48 In special circumstances, that is, under independence between joint exposures and less prone exposure misclassification (e.g., genes), interaction results have been claimed more robust to measurement error.23
Particularly, in mediation analysis, measurement error of the mediator may limit the validity of the mediation inferences. In a real-life situation, Le Cessie et al29 indicated that, in most cases, either measurement error of the mediator or random variation of the mediator over time may lead to an underestimation of the direct effect. Using the results from the case–control Leiden Thrombophilia Study (Table 5), correction for random variation of the mediator over time resulted in an attenuation of the direct effect (OR) of blood group in the likelihood of thrombosis from 1.5 (95% CI: 1.0–2.1) to 1.1 (95% CI: 0.75–1.7).29
Conclusion
There are different motivations behind the assessment of effect modification, interaction and mediation. A researcher might be interested in effect modification to know in which type of patients a therapy (or other exposure) has most effect. Interaction is of interest when one wants to know whether two or more treatments (or exposures) have a joint effect over and beyond their separate effects. Finally, the motivation behind assessing mediation will be to understand the pathway, whereby a treatment (or exposure) exerts its effect. These three types of assessment have their particular main advantages and pitfalls. While the basic principles of these three concepts have been explained by simple examples, newer theories claim that the estimations are very sensitive to confounding, lack of independency, measurement error or their combinations. However, these potential problems have been shown mostly by rather extreme and often theoretical examples.24,38,49,50 Therefore, it is as yet uncertain whether in less extreme circumstances, problems would be equally severe. We need to study urgently in which real-life situations the assessment of effect modification, interaction and mediation is severely hampered by confounding, lack of independency and measurement error. Until we know more, the current strong assumption requirements will generally limit the applicability of interaction and mediation assessments in observational studies using large research databases.
Acknowledgments
We want to acknowledge Kenneth J Rothman for his suggestions on an earlier draft of this manuscript. This article was funded by the Program for Clinical Research Infrastructure (PROCRIN) established by the Lundbeck Foundation and the Novo Nordisk Foundation and administered by the Danish Regions.
Disclosure
The authors report no conflicts of interest in this work.
References
Miettinen O. Confounding and effect-modification. Am J Epidemiol. 1974;100(5):350–353. | ||
Rothman KJ. The estimation of synergy or antagonism. Am J Epidemiol. 1976;103:506–511. | ||
Judd CM, Kenny DA. Process analysis. Estimating mediation in treatment evaluations. Eval Rev. 1981;5:602–619. | ||
Rothman KJ. Synergy and antagonism in cause-effect relationships. Am J Epidemiol. 1974;99(6):385–388. | ||
Fletcher RH, Fletcher SW. Clinical Epidemiology: The Essentials. 4th ed. Baltimore: Lippincott Williams & Wilkins; 2005. | ||
Greenland S. Randomization, statistics, and causal inference. Epidemiology. 1990;1:421–429. | ||
Rubin DB. The design versus the analysis of observational studies for causal effects: parallels with the design of randomized trials. Stat Med. 2007;26(1):20–36. | ||
Nicholls SG, Langan SM, Sorensen HT, Petersen I, Benchimol EI. The RECORD reporting guidelines: meeting the methodological and ethical demands of transparency in research using routinely-collected health data. Clin Epidemiol. 2016;8:389–392. | ||
Sorensen HT, Lash TL, Rothman KJ. Beyond randomized controlled trials: a critical comparison of trials with nonrandomized studies. Hepatology. 2006;44(5):1075–1082. | ||
Harpe SE. Using secondary data sources for pharmacoepidemiology and outcomes research. Pharmacotherapy. 2009;29(2):138–153. | ||
van Staa TP, Goldacre B, Buchan I, Smeeth L. Big health data: the need to earn public trust. BMJ. 2016;354:i3636. | ||
Rothman KJ, Greenland S, Lash TL. Modern Epidemiology. 3rd ed. Philadelphia: Lippincott Williams & Wilkins; 2008. | ||
Hernan MA, Robins JM. Causal Inference. Boca Raton: Chapman & Hall/CRC; 2016. | ||
Kranzler HR, Covault J, Feinn R, et al. Topiramate treatment for heavy drinkers: moderation by a GRIK1 polymorphism. Am J Psychiatry. 2014;171(4):445–452. | ||
Beral V, Bull D, Reeves G, Collaborators MWS. Endometrial cancer and hormone-replacement therapy in the Million Women Study. Lancet. 2005;365(9470):1543–1551. | ||
McAlister FA, Straus SE, Sackett DL, Altman DG. Analysis and reporting of factorial trials. A systematic review. JAMA. 2003;289(19):2545–2553. | ||
The Medical Research Council’s General Practice Research Framework. Thrombosis prevention trial: randomised trial of low-intensity oral anticoagulation with warfarin and low-dose aspirin in the primary prevention of ischaemic heart disease in men at increased risk. Lancet. 1998;351(9098):233–241. | ||
Hallas J, Dall M, Andries A, et al. Use of single and combined antithrombotic therapy and risk of serious upper gastrointestinal bleeding: population based case-control study. BMJ. 2006;333(7571):726. | ||
Knol MJ, Egger M, Scott P, Geerlings MI, Vandenbroucke JP. When one depends on the other: reporting of interaction in case-control and cohort studies. Epidemiology. 2009;20(2):161–166. | ||
Porta M. A Dictionary of Epidemiology. 5th ed. Oxford: Oxford University Press; 2008. | ||
Greenland S, Neutra R. Control of confounding in the assessment of medical technology. Int J Epidemiol. 1980;9(4):361–367. | ||
Hafeman DM, Schwartz S. Opening the Black Box: a motivation for the assessment of mediation. Int J Epidemiol. 2009;38(3):838–845. | ||
VanderWeele TJ. Explanation in Causal Inference: Methods for Mediation and Interaction. New York: Oxford University Press; 2015. | ||
Richiardi L, Bellocco R, Zugna D. Mediation analysis in epidemiology: methods, interpretation and bias. Int J Epidemiol. 2013;42(5):1511–1519. | ||
Baron RM, Kenny DA. The moderator-mediator variable distinction in social psychology research: conceptual, strategic, and statistical considerations. J Pers Soc Psychol. 1986;51(6):1173–1182. | ||
Mease PJ, Russell IJ, Arnold LM, et al. A randomized, double-blind, placebo-controlled, phase III trial of pregabalin in the treatment of patients with fibromyalgia. J Rheumatol. 2008;35(3):502–514. | ||
Russell IJ, Crofford LJ, Leon T, et al. The effects of pregabalin on sleep disturbance symptoms among individuals with fibromyalgia syndrome. Sleep Med. 2009;10(6):604–610. | ||
Koster T, Blann AD, Briet E, Vandenbroucke JP, Rosendaal FR. Role of clotting factor VIII in effect of von Willebrand factor on occurrence of deep-vein thrombosis. Lancet. 1995;345(8943):152–155. | ||
Le Cessie S, Debeij J, Rosendaal FR, Cannegieter SC, Vandenbroucke JP. Quantification of bias in direct effects estimates due to different types of measurement error in the mediator. Epidemiology. 2012;23(4):551–560. | ||
MacKinnon DP. Introduction to Statistical Mediation Analysis. New York, NY: Taylor & Francis; 2008. | ||
Skrondal A. Interaction as departure from additivity in case-control studies: a cautionary note. Am J Epidemiol. 2003;158(3):251–258. | ||
Freemantle N, Marston L, Walters K, Wood J, Reynolds MR, Petersen I. Making inferences on treatment effects from real world data: propensity scores, confounding by indication, and other perils for the unwary in observational research. BMJ. 2013;347:f6409. | ||
Sogaard M, Heide-Jorgensen U, Norgaard M, Johnsen SP, Thomsen RW. Evidence for the low recording of weight status and lifestyle risk factors in the Danish National Registry of Patients, 1999-2012. BMC Public Health. 2015;15:1320. | ||
Haldorsen T, Martinsen JI, Kjaerheim K, Grimsrud TK. Adjustment for tobacco smoking and alcohol consumption by simultaneous analysis of several types of cancer. Cancer Causes Control. 2017;28(2):155–165. | ||
Green A. Danish clinical databases: an overview. Scand J Public Health. 2011;39(7 suppl):68–71. | ||
Sorensen HT, Pedersen L, Jorgensen J, Ehrenstein V. Danish clinical quality databases – an important and untapped resource for clinical research. Clin Epidemiol. 2016;8:425–427. | ||
VanderWeele TJ, Knol MJ. A tutorial on interaction. Epidemiol Methods. 2014;3:33–72. | ||
Vanderweele TJ, Ko YA, Mukherjee B. Environmental confounding in gene-environment interaction studies. Am J Epidemiol. 2013;178(1):144–152. | ||
Greenland S. Interactions in epidemiology: relevance, identification, and estimation. Epidemiology. 2009;20(1):14–17. | ||
Saracci R. Interaction and synergism. Am J Epidemiol. 1980;112:465–466. | ||
VanderWeele TJ, Robins JM. Four types of effect modification: a classification based on directed acyclic graphs. Epidemiology. 2007;18(5):561–568. | ||
Cole SR, Hernan MA. Fallibility in estimating direct effects. Int J Epidemiol. 2002;31(1):163–165. | ||
Pearce N. Analytical implications of epidemiological concepts of interaction. Int J Epidemiol. 1989;18(4):976–980. | ||
Skrondal A. Commentary: much ado about interactions. Epidemiology. 2014;25(5):723–726. | ||
Robins JM, Greenland S. Identifiability and exchangeability for direct and indirect effects. Epidemiology. 1992;3(2):143–155. | ||
Nguyen TT, Tchetgen Tchetgen EJ, Kawachi I, Gilman SE, Walter S, Glymour MM. Comparing alternative effect decomposition methods: the role of literacy in mediating educational effects on mortality. Epidemiology. 2016;27(5):670–676. | ||
Greenland S. The effect of misclassification in the presence of covariates. Am J Epidemiol. 1980;112(4):564–569. | ||
Greenland S. Basic problems in interaction assessment. Environ Health Perspect. 1993;101:59–66. | ||
Blakely T. Commentary: estimating direct and indirect effects – fallible in theory, but in the real world? Int J Epidemiol. 2002;31(1):166–167. | ||
VanderWeele TJ, Hernan MA. Results on differential and dependent measurement error of the exposure and the outcome using signed directed acyclic graphs. Am J Epidemiol. 2012;175(12):1303–1310. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
