Back to Journals » Psoriasis: Targets and Therapy » Volume 5
Disease burden and patient reported outcomes among patients with moderate to severe psoriasis: an ethnography study
Authors Narayanan S, Guyatt V, Franceschetti A, Hautamaki E
Received 25 September 2014
Accepted for publication 2 November 2014
Published 23 December 2014 Volume 2015:5 Pages 1—7
DOI https://doi.org/10.2147/PTT.S74906
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Prof. Dr. Uwe Wollina
Siva Narayanan,1 Victoria Guyatt,2 Alessandra Franceschetti,3 Emily L Hautamaki1
1Ipsos Healthcare, Columbia, MD, USA; 2Ipsos Ethnography Centre of Excellence (ECE), London, UK; 3Ipsos Healthcare, London, UK
Objectives: To assess the impact of psoriasis on health-related quality of life (HRQoL).
Methods: An ethnographic study of patients with moderate to severe psoriasis was conducted in the US, France, Germany, Italy, Spain, UK, Brazil, and Canada to explore patients' views on treatment and the impact of psoriasis on HRQoL. Anthropologists and ethnographers spent a minimum of 5.5 hours with each consented patient and filmed their behaviors in everyday situations. Visual data and notes were analyzed to identify HRQoL-related themes.
Results: The study included 50 adult patients. Patients described their appearance with disgust and self-loathing. Frustration was expressed due to a perceived lack of control of their lives. Prior to initiation of biologic treatment, daily rituals absorbed a good part of their day, including applying creams, checking one's appearance, and covering the body. Due to a lack of cultural discourse and patient's difficulty in articulating the impact of psoriasis, partners and family did not know how to react nor did they realize the full extent of the problem, and many patients experienced perceived social discrimination due to psoriasis, leaving them with feelings of isolation. Patients established on biologic treatment noticed a significant physical improvement and regained confidence, but psychosocial impacts, including social isolation, remained.
Conclusion: This ethnographic study vividly depicted the unarticulated and emotional impact of psoriasis on the everyday lives of patients and presents an effective method of assessing HRQoL in chronic diseases.
Keywords: psoriasis, health-related quality of life, ethnography, patient reported outcomes, conceptual model
Introduction
Psoriasis is a chronic, autoimmune disease of the skin, characterized by rapid turnover of skin cells, resulting in thick plaques of itchy, sore, inflamed skin, covered with silvery scales. Plaques can occur anywhere on the body. Some people with psoriasis develop painful joint inflammation, called psoriatic arthritis. Psoriasis can present at any age and occurs in men and women at equal rates.1 Psoriasis affects approximately 2% of the world’s population and is influenced by genetic and environmental factors.1,2 People with psoriasis may experience flares due to infections, stress, dry skin due to weather changes, certain medications, and trauma.1 Treatment aims to alleviate signs and symptoms and slow progression of the disease.3 Psoriasis is treated with a combination of topical treatments (corticosteroids, vitamin D analogs, retinoids, coal tar, and anthralin), ultraviolet light therapy, and systemic treatments, taken orally or via injection or infusion (methotrexate, retinoids, cyclosporine, and biologic response modifiers).1 Psoriasis does not affect survival.4
Psoriasis causes a substantial impact on health-related quality of life (HRQoL). The pain, itching, impact on physical appearance, and intensive medical care of psoriasis can interfere with the individual’s daily activities, choice of occupation and hobbies, and social and psychological well-being.1,4,5 Thus, disease-specific and generic HRQoL assessments are often included as secondary endpoints in clinical trials of psoriasis medications, including the Dermatology Life Quality Index (DLQI), the Self-Administered Psoriasis Area and Severity Index (SAPASI), Psoriasis Disability Index (PDI), the Short Form 36 Health Survey (SF-36), the EuroQol-5D (EQ-5D), the Health Assessment Questionnaire Disability Index (HAQ DI), and others.6–8 While such instruments may be useful to portray a quantitative snapshot of patient status and measure changes over time in the context of a clinical trial, qualitative methods offer advantages in the ability to uncover and describe subtle or less well-defined HRQoL concepts and highlight the voice of the patient and their perception of their disease. Rather than relying on patient report alone, ethnography observes the subject’s actual behaviors in their own environment over an extended period of time, and can reveal behaviors that may be subconscious, or that the individual may not consider relevant or interesting, and thus may not be reported by the patient via other methods. As such, an ethnographic methodology could be useful for informing quantitative patient reported outcomes (PRO) instrument development.
In this study, we employed ethnographic methods among a sample of patients with psoriasis in the US, Brazil, Canada, and Europe to gain a better understanding of patient burden in psoriasis, including differences among patients by exposure to biologic therapy, and to explore the suitability of ethnography for evaluating PRO.
Methods
Patient recruitment
The study was conducted among adult patients (at least 18 years of age) with moderate to severe psoriasis in the US, France, Germany, Italy, Spain, the UK, Brazil, and Canada. Patients must have been currently undergoing treatment. Given differences in treatment burden, a mix of patients was recruited in each country based on experience with biologic therapy for psoriasis, including patients who had never used biologic therapy, patients who had been on biologic therapy for less than 1 year, and patients who had been on biologic therapy for more than 1 year.
Patients were recruited via commercially available patient panels. A purposive sampling approach was taken to recruit patients with a range of demographic characteristics where possible. Written informed consent was obtained from all patients prior to enrollment in the study.
Data collection
Data collection consisted of a home visit by a specialist ethnographer who was a native speaker of the local language of the country. On the day of the home visit, patients underwent their planned activities for the day, inside and outside of the home, while researchers filmed the patients in their environment with a small hand-held video camera and took detailed field notes. Researchers had an unstructured discussion guide, but the interactions were driven by the patient. Researchers captured the patient’s environment, interactions, and daily activities, and observed the context in which patients made decisions. Researchers spent a minimum of 5.5 hours with each participant.
Analysis
Ethnographers and study researchers viewed the video footage and analyzed behavior and language using frameworks from anthropology and behavioral economics. An iterative process of analysis of the visual data led to the emergence of themes related to HRQoL.
Results
A total of 50 participants with moderate to severe psoriasis were enrolled in the study (n<15 in the US, n<5 in each other country). Participants were 21–67 years of age; 57% were female; 22% had never used biologic therapy (“Biologic-Naïve”), 43% had initiated biologic therapy within the past year (“Newly Initiated”), and 35% had initiated biologic therapy more than 1 year ago (“Established”).
A total of 250 hours of video footage was produced and analyzed alongside field notes to identify and describe common themes related to HRQoL. Major themes emerged during the interactions, including negative psychological effects, activity impairment, family relationship impairment, and social impairment. Each theme is described in detail below.
Negative psychological effects
Patients reported poor self-image. Patients described their appearance with a sense of disgust and self-loathing.
I’m very neurotic about not having the patches in public. It looks gross. Self-esteem has always been an issue. – Male, US, Newly Initiated
I hate looking in the mirror even now. I don’t think that will ever change. – Female, UK, Established
It doesn’t just affect your skin and things like that, but also your mind. It destroys you mentally. – Male, Italy, Established
Patients described attempting to hide their symptoms during flare-ups by wearing long-sleeved tops and full-length pants, or staying in the house to avoid being seen by others. They describe feeling “lucky” if their symptoms were confined to the trunk area or other areas of the body that cannot easily be seen. After becoming established on biologic treatment, patients described having fewer or no symptoms, but in rare cases physical scars from the disease remained that they attempted to cover up, and psychological effects remained.
Many patients considered stress to be a trigger of an exacerbation, and family members frequently described the psoriasis patients as being overly anxious or nervous. This was described as a “vicious circle”, as psoriasis itself was a source of stress, and the act of trying to control one’s stress level was in itself stressful, and the stress leads to more symptoms. Some patients perform relaxation techniques to control stress.
There were some things that happened in my life – some serious problems for me, and so it came back overnight covering my whole body – really. So I think stress is definitely a factor. – Female, US, Newly Initiated
I would have a modeling job coming up. And I would start to feel stressed that I would have a flare-up. Which would then mean I had a flare-up! I couldn’t win. – Female, Spain, Established
Patients also described feelings of frustration and hopelessness, due to a perceived lack of control over one’s life and uncertainty of when the next flare will occur. Some biologic-naïve patients have had to switch to a career that they found less stressful.
That’s how I used to look [points at picture on mantelpiece], it’s like I miss myself. Running things, being in charge, being in the office, being up in management and now I’m just like this now. – Female, US, Established
I had to give up nursing because of the symptoms on my feet and my hands – I have always been a nurse, so when I had to stop I almost [felt like I] died. – Female, Brazil, Established
I used to work as a waitress, and my boss told me I had to cover any patches on my arms. I eventually quit because it was so stressful. – Female, Spain, Established
Due to the embarrassment of the visible symptoms, patients tended to isolate themselves. Some preferred working from home to avoid being around others, a coping mechanism which may perpetuate feelings of isolation. The isolation and poor self-image may lead to depression. After biologic initiation, many patients regained confidence as a result of having fewer or no symptoms, though psychological scars remained, especially if the patient had a long delay between first experiencing psoriasis and initiating a biologic.
Physically, today, I can say that I am rid of it. But psychologically I think I am not rid of it. If I really started thinking about all of this, I think I’d fall into depression. I can’t say that today my psoriasis is in the past – even if it’s no longer visible. – Female, France, Established
I didn’t really want to socialize as much, and I know it sounds stupid, but [I don’t really want to] be around other people’s kids because my son was saying how disgusting it was. He didn’t like me touching him. He would be like “Gross, get off me, don’t touch me with your hands.” – Female, UK, Biologic-Naïve
With my dad [who also has psoriasis], we never talk about it. When I say never, I mean never. – Female, France, Biologic-Naïve
Activity impairment
Prior to biologic initiation, participants expressed that their daily rituals to control the disease absorbed a great part of the day. Participants described continuously cleaning the house to remove dead skin flakes from the carpet and surfaces, waking up early to check for new flares, going to work early to check one’s appearance and cover patches of dead skin, and covering one’s work surface every day in order not to leave traces of psoriasis. One patient noted using hair ties around her wrists to keep her shirt tight to her skin to prevent skin flakes from falling on the floor. Furthermore, patients felt discouraged from pursuing their passions (for example, dancing) because of the visibility of psoriasis.
Researchers observed bathrooms that were often filled with creams and treatments, both prescription topicals and over-the-counter moisturizers. Maintaining one’s physical appearance and hiding signs of psoriasis was a critical part of the patient’s morning routine.
I would get up early to apply creams, then get into work early so I could check myself in the toilets. I would check myself throughout the day, I became obsessive. – UK, Male, Newly Initiated
In the morning it’s first of all getting myself up so that I have time to moisturize and check there aren’t any flare-ups in the morning. I always have to check. It can take time. – Female, France, Biologic-Naïve
I would make sure I was in the restrooms at work at 6.30 am every morning just to make sure I could check my appearance. – Female, US, Established
After biologic initiation, many patients continued to follow their rituals of applying over-the-counter moisturizers, though the number of prescription topicals may be reduced. Patients described feeling liberated from years of obsession with cleaning and moisturizing.
Most patients acknowledged that medication was necessary to control their psoriasis, and that lifestyle changes, such as diet, exercise, or quitting smoking were not enough. Understanding one’s triggers can empower the patient, though some struggle with having to add more restrictions to their daily routine.
I try to exercise and eat well because, for me, a healthy body equals a healthy mind and a healthy mind will help to reduce my symptoms, as I will be less stressed. – Male, Brazil, Newly Initiated
Diet was half the battle because I know that I’m putting healthy things in my body – I now know that I have more control than I did before. – Male, US, Newly Initiated
Well, I have found that before you get depressed or such-like, you should do some physical exercise – so I go to the swimming pool. – Male, Germany, Established
Family relationship impairment
Due to the lack of awareness of psoriasis, partners described not knowing how to react to the diagnosis. Also, given the difficulty some people have in describing how psoriasis symptoms affect them psychologically, partners may not realize the full extent of the problem. Patients expressed the desire to be supported by their family, but found it difficult to get the type of psychological support that they needed, leaving them with feelings of resignation. Patients described feeling embarrassed when other members of the family helped to clean up their dead skin flakes around the home. Even when they are on biologics, despite their regained confidence, they still don’t discuss their condition with family and friends.
I don’t know what goes on in a partner’s head when they see that. Most likely they find it repulsive but they just don’t say. – Male, Germany, Established
I’m not sure what the emotional response is supposed to be. If you have cancer it triggers some sort of emotional response. When you say you have psoriasis people don’t know how to react to that. – Husband of participant, Female, US, Established
Social impairment
Stemming from the lack of awareness of psoriasis, patients described social impairment due to their friends’ and coworkers’ perceptions and judgments. Patients had experienced social discrimination; for example, someone refusing to shake the psoriasis patient’s hand. Patients described feeling “controlled” by their friends and colleagues, as their judgments forced them to change their routines and behaviors (such as wearing special clothes to cover flares).
When it was on my face – I would never go out unless I really had to … – Male, Canada, Established
Many patients were habitually secretive about their psoriasis, admitting to frequently lying about their chronic condition, and instead attributing it to an acute complaint like an insect bite or allergic rash.
I would say it was a burn or something like that. Just play it down. – Female, US, Newly Initiated
In some extreme cases, patients compared their social status to someone who was “plague-stricken”.
You do feel ugly, yes, that’s what it is – you don’t like to show yourself. You feel ostracized as if you were a monster. The only thing missing is pitch forks and torches. – Male, Germany, Biologic-Naïve
I had a breakout on my hands and this man wouldn’t even shake my hand. I felt like had leprosy. – Male, Italy, Established
Patients fear being stigmatized and fear that others will think the disease is contagious. Patients typically only tell close friends or partners about their psoriasis; the disease is kept hidden from colleagues as much as possible.
You do a lot so that people don’t see it, you get the impression that you have to do more, you cover your skin, even when it’s hot, you try to make up stories, you say you’re allergic to the sun so as not to say that you have psoriasis. – Female, France, Biologic-Naïve
Nobody at work knows. I’m very careful not to let them see. I don’t really know how to explain it so I don’t want to have that conversation. – Male, UK, Newly Initiated
Differences across treatment types
There were marked differences in the ways in which the three patient groups (“Biologic-Naïve,” “Newly Initiated,” and “Established”) discussed the disease, and primarily its psychological impacts.
“Biologic-Naïve” patients experienced higher levels of anxiety regarding perceptions of using needles and efficacy of biologics. They were also concerned about side effects, and in countries outside of France and the UK, were concerned about the affordability of biologics. This was the time at which feelings of self-loathing were felt most strongly and the primary concern for patients is that their symptoms improve and their skin “returns to normal.”
“Newly Initiated” patients were enthusiastic as symptoms began to improve, although a few patients had to change biologics to find one that worked for them. For these patients, there was a sense of disappointment that they did not improve as quickly or profoundly as first hoped. While their symptoms had improved, the psychological scarring remained and there was still fear that they may return to their prebiologic state.
“Established” patients were appreciative for the improvement of their symptoms and the impact this had on their everyday lives. Patients felt liberated from years of obsession with cleaning and moisturizing. However, there was still resignation over any unsolved areas of skin. Few worried about the side effects as the benefits far outweighed them, but there was fear over long-term efficacy.
Cultural differences
Across countries, the way in which patients articulated disease burden, engaged with health care providers, and sought information about their illness and disease differed. Patients in the US had very advanced knowledge of psoriasis, often referring to it as an autoimmune disease and listing out the names of medications and their manufacturers. Patients in the UK and France by comparison had very limited knowledge. Some patients in the France struggled to pronounce the word “psoriasis,” while patients in the UK referred to psoriasis as “severe eczema.” These variations in knowledge could come from the differing healthcare delivery systems within each country and the subsequent ways in which this directs patients’ behaviors and interactions with health care providers.
Furthermore, the expressions of the psychological effects of the disease varied greatly. In Germany patients did not want to speak about mental health and psychiatry. Patients in this sample preferred to talk about practical assistance rather than emotional assistance from a health professional. In the US, however, many patients spoke of the invaluable assistance that they had received from mental health professionals and the importance of acknowledging this element of disease burden.
Canadian patients were more likely to disengage from the disease completely, by not focusing on having the disease and hiding the symptoms. This meant that they were less likely to seek support (formal or informal). In contrast, in Brazil there was a lot of enthusiasm for patient support communities.
Patients in Spain and Italy were most likely to express the deep psychological impact of having visible symptoms of psoriasis. The importance of appearance and socializing in these cultures made the effects of psoriasis more isolating, as these patients attempted to avoid friends and family.
The culture surrounding psoriasis in France is rife with taboos. It is common for patients not to discuss their illness and their feelings towards their illness with families or friends. – Female, France, Biologic-Naïve
I miss living in New York, first of all because of the way people look at you – it’s completely different here, I think, when it comes to skin problems … I saw lots of people with psoriasis there, especially in Central Park playing sports, nobody gave them a second glance. Because in France – well it wouldn’t be allowed. It’s really very French – flaws cannot be visible. – Female, France, Biologic-Naïve
Discussion and conclusion
The present study is the first, to our knowledge, to use an ethnographic methodology to gain a unique insight into the daily life of the patient with psoriasis in their home environment. It shed light on patients’ self-isolation, relationships with their partner and family, self-consciousness and anxiety, and the extensive planning and daily routines that are required to cope with everyday life and avoid uncomfortable social situations. Advantages of using ethnography in this study include observing the patient in their own environment for a relatively long period of time, capturing interactions with partners/family, medication taking, daily rituals and routines, and nonverbal communication. Ethnography also exposed cultural differences in this study, including differing expression of emotional impacts and willingness to discuss psoriasis with others, which should be noted when developing and interpreting the results of PRO instruments in psoriasis. Ethnographic study could be a useful methodology for the cultural validation of PRO instruments, an element found to be lacking in many of the commonly used PRO instruments in psoriasis.9 A direct comparison of different qualitative methodologies could result in more conclusive recommendations. As is common in qualitative research, it should be noted that this study took a purposive sampling approach to obtain a diverse sample but the sample was not intended to be representative. In addition, patients who participated via the commercially available patient panels may differ from the general population of patients with psoriasis.
This study design could be used as a basis for future instrument development for quantitative research to address the limitations of existing PRO instruments. Based on the results, we developed a conceptual model depicting the impacts of psoriasis on HRQoL from the patient’s perspective (Figure 1). In the conceptual model, we show that symptom triggers, such as infection and stress, influence the presence and severity of the physical symptoms of psoriasis. In turn, experiencing physical symptoms, such as itching, flaking, and visible patches, results in psychological impacts (such as poor self-image, embarrassment, and stress), activity impairment (including the avoidance of hobbies, lengthy morning routines, and impact on work and career), social impacts (including stigma, secrecy, and social isolation), and family relationship impairment (stemming from perceived lack of understanding and support). In turn, psychological impacts lead patients to further avoid social activities and hobbies, which perpetuate the psychological distress, which may lead to further symptoms. Symptom modifiers, including effective treatment, avoidance of triggers, and relaxation techniques, may help prevent psoriasis symptoms, thereby improving the patient’s HRQoL and alleviating disease burden.
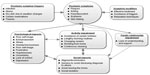  | Figure 1 The impact of psoriasis on health-related quality of life from the patient perspective: a conceptual model. |
This conceptual model includes a number of concepts that are missing or inadequately covered in existing instruments. Specifically, the existing psoriasis-specific quantitative instruments (the PDI, the Psoriasis Area and Severity Index [PASI], the Self-Administered PASI, and the Psoriasis Index of Quality of life [PSORIQoL]), and the commonly-used DLQI, do not address the domain of psychological impacts,6 which was found to be of paramount importance in the lives of the psoriasis patients in this study and related to symptom exacerbations. Furthermore, the DLQI and the PDI, the most widely used psoriasis-specific PRO instruments,8 have been shown to have some psychometric limitations.9 The new Reflective Evaluation of Psoriasis Efficacy of Treatment and Severity (REFLETS) instrument does have a psychological functioning subscale, but the items are general and do not address many of the specific concerns patients reported in this study.10 Concepts such as social stigma, daily regimen burden, secrecy, stress, and depression do not appear to be included in the existing psoriasis-specific PRO instruments. Generic instruments such as SF-36 are widely used in clinical trials, but are found to lack assessment of psychosocial effects and well-being of psoriatic patients, thereby necessitating its use in combination with a disease-specific instrument.9
In conclusion, this study confirms that patients with psoriasis have high disease burden. Ethnography could be a useful technique to assess HRQoL in chronic diseases such as psoriasis. Additional research may be warranted to ensure the commonly used PRO instruments in psoriasis are adequate for portraying burden in this patient population.
Author contributions
SN and ELH contributed to the analysis and interpretation of the data and the writing of the manuscript. VG and AF designed the study, conducted the fieldwork and analysis, and contributed to editing the results section the manuscript. All authors read and approved the final manuscript.
Disclosure
The authors are employees of Ipsos Healthcare, and the study was funded by Ipsos. The authors report no other conflicts of interest in this work.
References
National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), National Institutes of Health (NIH). Questions and answers about psoriasis. NIH Publication No 13-5040, October 2013. Available from: http://www.niams.nih.gov/Health_info/Psoriasis/. Accessed June 27, 2014. | |
Parisi R, Symmons DP, Griffiths CE, Ashcroft DM. Identification and Management of Psoriasis and Associated ComorbidiTy (IMPACT) project team. Global epidemiology of psoriasis: a systematic review of incidence and prevalence. J Invest Dermatol. 2013;133(2):377–385. Review. | |
World Health Organization (WHO). Psoriasis: Report by the Secretariat (EB133/5). Geneva: World Health Organization. EB133/5, April 5, 2013. Available from: http://apps.who.int/gb/ebwha/pdf_files/EB133/B133_5-en.pdf. Accessed July 10, 2014. | |
Langley RG, Krueger GG, Griffiths CE. Psoriasis: epidemiology, clinical features, and quality of life. Ann Rheum Dis. 2005;64(Suppl 2):ii18–ii23; discussion ii24–ii25. Review. | |
Bhosle MJ, Kulkarni A, Feldman SR, Balkrishnan R. Quality of life in patients with psoriasis. Health Qual Life Outcomes. 2006;4:35. | |
Tan X, Feldman SR, Balkrishnan R. Quality of life issues and measurement in patients with psoriasis. Psoriasis: Targets Ther. 2012;2:13–23. | |
Frankel EH, Strober BE, Crowley JJ, et al. Etanercept improves psoriatic arthritis patient-reported outcomes: results from EDUCATE. Cutis. 2007;79(4):322–326. | |
Otuki MF, Reis RC, Cabrini D, Prudente AS, Horinouchi CD, Correr CJ. Patient-reported outcomes in psoriasis research and practice. Br J Dermatol. 2011;165(6):1361–1362. | |
Bronsard V, Paul C, Prey S, et al. What are the best outcome measures for assessing quality of life in plaque type psoriasis? A systematic review of the literature. J Eur Acad Dermatol Venereol. 2010;24(Suppl 2):17–22. | |
Gilet H, de Climens AR, Arnould B, et al. Development and psychometric validation of the REFlective evaLuation of psoriasis Efficacy of Treatment and Severity (REFLETS) questionnaire: a common measure of plaque-type psoriasis severity and treatment efficacy for patients and clinicians. J Eur Acad Dermatol Venereol. Epub July 25, 2014. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
