Back to Journals » Infection and Drug Resistance » Volume 13
Direct-Acting Antiviral Drugs and Occurrence of Hepatocellular Carcinoma: Unjust or Oppressed
Authors Hassany SM , Hassan W, Abo-alam H, Khalaf M, Nafeh AM, Nasr-eldin E, Mostafa EF
Received 16 January 2020
Accepted for publication 13 May 2020
Published 18 June 2020 Volume 2020:13 Pages 1873—1880
DOI https://doi.org/10.2147/IDR.S241948
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Sahil Khanna
Sahar M Hassany,1 Wesam Hassan,2 Hany Abo-alam,2 Marwa Khalaf,2 Amany M Nafeh,3 Eman Nasr-eldin,4 Ehab F Mostafa1
1Tropical Medicine and Gastroenterology Department, Alrajhi University Hospital, Assiut University, Assiut, Egypt; 2Hepatology Centre, Ministry of Heath, Assiut, Egypt; 3Microbiology and Immunity Department, Assiut University, Assiut, Egypt; 4Clinical Pathology Department, Assiut University, Assiut, Egypt
Correspondence: Sahar M Hassany
Alrajhi University Hospital, Assiut University, Assiut, Egypt
Tel +201007314122
Fax +20882375308
Email [email protected]
Purpose: In interferon-free era, direct-acting antiviral agents (DAAs) have achieved high eradication rates with an excellent safety profile since revolutionized the management of hepatitis c virus (HCV) patients. Published papers have suggested a possible increased incidence of hepatocellular carcinoma (HCC) after successful DAAs treatment. Other papers have been published about the problem but without conclusive results. Because of this debate, we aim to evaluate the effects of antiviral therapy (Sofosbuvir plus Daclatasvir with or without Ribavirin) on the de novo occurrence of HCC in patients with liver cirrhosis (LC).
Patients and Methods: A prospective cohort study has included 350 patients who have visited our center for HCV treatment. Pretreatment history, examination, complete blood picture, liver function tests, kidney function tests, HA1C for diabetic patients, HCV PCR, HBsAg, alpha-fetoprotein (AFP), and abdominal ultrasound have been done, also Child-Pogh (CP) and Model for End-Stage Liver Disease (MELD) score before treatment. These investigations have been repeated for 3 months after the end of treatment. Abdominal ultrasound (US) has been done for 3 months after treatment and every 4 months for 2 years after the end of treatment to detect HCC occurrence.
Results: Patients age (58.11 ± 7.48), 55.4% of patients were males, 30.3% of patients were diabetic, 84.3% of them were treatment naïve and sustained virological response (SVR) occured in 94% of them. HCC occurrence after treatment was 6.7% in patients with SVR and 23.8% in patients with non-SVR (P value=0.016) during follow-up period. There is significant improvement of CP score. No significant changes in MELD score.
Conclusion: Treatment of HCV-related LC patients with sofosbuvir and daclatasvir with or without ribavirin for 3 or 6 months showed high SVR and significant improvement in CP score, but still at risk of HCC even if treated and should be followed up regularly according to screening programs with special meticulous attention to those with non-SVR.
Keywords: de-novo HCC occurrence, HCV treatment
Introduction
Hepatitis C virus (HCV) represents a major health problem in many countries; Egypt is considered one of the highest incidences of HCV as about 14.7% of the population is infected.1 However, more recent epidemiological studies have reported that the HCV disease estimates in Egypt are that about 7.3% of the population has been reported to have HCV viremia. This may be due to the mortality in the older age groups, who have the highest prevalence of infection.2 More recently in 2019, HCV disease burden in Egypt is suggested to be about 4.7% (100 Million Heath president program for Hcv treatment in Egypt).
About 70–80% of those who are infected with the HCV get chronic hepatitis, which may progress to cirrhosis in 20% of patients within 2–3 decades; a quarter of these patients will develop complications, such as hepatocellular carcinoma (HCC), portal hypertension, and liver decompensation, with an average 5-year survival rate of 50%.3
Hepatocellular carcinoma is the fifth most frequent form of cancer worldwide, and it holds the second cause of malignancy-related mortality.4,5 Incidence and death rates of HCC are steadily rising in most parts of the world (about 2–3% per year).
Liver cirrhosis (LC) is the major risk factor or HCC in patients with HCV where it occurs almost exclusively in those with cirrhosis. There is also suggestive experimental evidence that HCV infection itself can promote the development of HCC, where Mice that have been made transgenic for the HCV core gene have developed adenomas and subsequent carcinoma within the adenomas.6
In the last few years, a major progress towards the treatment of HCV had occurred with the introduction of all oral therapies. Direct-acting antiviral agents (DAAs) have achieved high eradication rates with an excellent safety profile since revolutionized the management of HCV patients.7
Interferon era teaches us that after cirrhosis has been established, eradication of HCV infection is not sufficient per se to prevent HCC development. It is not surprising to expect that some of them may develop HCC despite HCV eradication. That may be due to the possibility of treating patients with more advanced liver disease.8 This topic has become hot after the simultaneous publication of two papers from Spain and Italy suggesting a possible increased incidence of HCC after successful DAA treatment.9,10 Since Spain and Italy papers were publicated, more than 100 papers, letters or communications have been published about the problem, yet without conclusive results. Most of the debate attributed to the heterogeneity of the different studied population, the inclusion and exclusion criteria, the time points used to analyze the incidence rates, the length of follow-up, and finally the radiologic methods used for the diagnosis of HCC.8
The aim of this study is to evaluate the effect of antiviral therapy on the de novo occurrence of HCC in patients with liver cirrhosis who are treated by DAAs.
Materials and Methods
Study Design and Patients Selection
This prospective cohort study has been conducted from March 2016 till March 2019 in Assiut center for viral hepatitis mangment (one of the national established centers in every Egyptian Governorates) and Alrajhi University Hospital for Liver on 350 HCV-related liver cirrhosis patients who are seeking for HCV treatment by direct-acting antiviral drugs and have eligible criteria for treatment, after obtaining ethical approval from the University Hospital Ethics Committee (with Declaration of Helsinki) and an informed written consent from every included patient.
Patients with HBV co-infection, renal impairment, hepatocellular carcinoma have been excluded from the study.
A complete history taking and meticulous clinical examination have been done for all of the patients.
Baseline Laboratory Investigation
Investigations preliminary to antiviral therapy: Complete blood picture, liver and kidney function tests, HBA1c if diabetic, and serum alpha-fetoprotein (AFP). Child-Pugh (CP) and Model for End_Stage Liver Disease (MELD) scores have been calculated.
Quantitative assessment of HCV loads in the serum by real-time Quantitative PCR just before the study.
Abdominal Ultrasonography (US)
The patients have been evaluated by one expert hand hepatologist operator for assessment of the liver before the beginning of treatment.
Triple-Phase CT
An arterial phase, a portal venous phase, and a late washout phase have been done for patients with elevated AFP levels and patients with hepatic focal lesions on abdominal US.
Treatment Exposure and Outcome
Medications
The treated patients have been given sofosbuvir 400 mg plus daclatasvir 60 mg plus ribavirin daily for 3 months or sofosbuvir 400 mg plus daclatasvir 60 mg daily for 6 months in patients who are not eligible for ribavirin.
Monitoring
All the patients have regular monthly visits in the first 3 and 6 months where patients come to receive monthly drug and evaluation of any side effects.
Achievement of sustained virological response (SVR) defined as undetectable HCV RNA by real-time Quantitative PCR at 12 weeks after end of treatment.
Follow-up of the liver synthetic function, Child, and MELD scores has been done after 3 months by the end of treatment. Alpha-fetoprotein level also has been assessed 3 months after end of treatment and has been done for patients who are suspected to have hepatic focal lesions on follow-up.
Then, all patients come for follow-up every 4 months for 24 months. Patients’ evaluation in every visit includes a full history taking, clinical examination, routine laboratory investigations, and abdominal US examination by the same expert operator.
Triple-phase CT including an arterial phase, a portal venous phase, and a late washout phase has been done for patients with elevated AFP levels and patients with hepatic focal lesions on abdominal US to confirm the diagnosis of HCC.
Statistical Analysis
Our data are coded and verified prior to data entry. Computer program Statistical Package for Social Sciences (ver.21) (IBM Corporation, Armonk, NY, USA) is used for analyzing the collected data. Data are expressed as mean ± SD and numbers as percentage. Student’s t-test is used to determine the significance of the numeric variable. P-value is considered significant if P<0.05 and not significant if P>0.05.
Results
Baseline Characteristics of Patients
We have analyzed data from 350 consecutive patients with HCV-related liver cirrhosis who have been treated with direct-acting antivirals between March 2016 till March 2019 and the follow-up time after initiation of direct-acting antiviral treatment has been (12–30 months). Patient age (58.11 ± 7.48) and 55.4% of patients were males. As high as 30.3% had diabetes mellitus (D.M), and 84.3% of patients are naïve. PCR Median and range are 511,897 (52–815,000,000). A total of 283 (80.9%) patients are CP class A, 66 (18.9%) CP class B, and 1 (0.3%) CP class C at the start of the treatment and the median MELD score is 9 (6–18). At the initiation of therapy, mean bilirubin level is 1.18 ± 0.64 mg/dL, mean platelet count is 138.54 ± 63.01/mm3, and mean albumin level is 3.51 ± 0.56 mg/dL. Ascites is in 12.3% of patients and hepatic encephalopathy in 2.6% of patients. The baseline characteristics of the study population are shown in Tables 1 and 2.
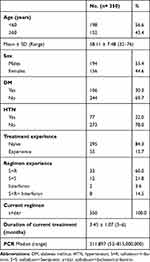 |
Table 1 Baseline Characteristics of Studied Patients |
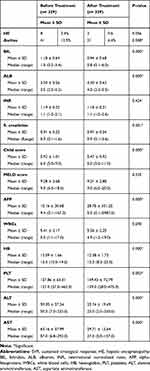 |
Table 2 Clinical and Biochemical Characteristics of SVR Patients Before and After Treatment |
Treatment Outcome
Three hundred and twenty-nine out of 350 patients (94%) have achieved SVR, while 21 (6%) of patients have not acheived SVR (Tables 2 and 3). No severe adverse effects can be detected apart from headache and fatigue in patients who responded to paracetamol treatment. Rather, few patients who have received Ribavirin have developed moderate anemia, which has later improved after lowering the dose of ribavirin.
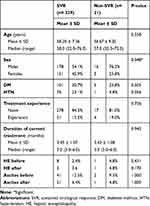 |
Table 3 Clinical Data of SVR and Non-SVR Patients Before and After Treatment |
Evolution of Liver Function
Significant improvement in liver enzymes (P value 0.000*), Bilirubin and Albumin levels (P value 0.000*), and Platelet count are noticed (P value 0.000*). Also, significant improvement in Child Score has occurred, where Child A patient is 88.6% and Child B is 10.9% (Table 2). One patient only has changed from Child B to Child C without valuable improvement in MELD Score.
Alfa-fetoprotein has increased after treatment in non-SVR patients compared to patients with SVR with (P value 0.014*), but this result may be due to wide median range with high value in one patient who has developed HCC later after treatment with median (5.0 (0.1–5987.0)), while the median before treatment is 8.1 (0.1–49.0).
There is no significant difference in both CP (P value =0.061) and MELD (P value=0.688) scores between both groups of patients with SVR and those with non-SVR.
Hepatocellular Carcinoma
Twenty-two (6.7%) patients with SVR have developed HCC and 5 (23.8%) patients with non-SVR have developed HCC, with significant difference between them. All HCC in patients with non-SVR has occurred in the first 10 months after end of treatment, while about 55% of HCC has occurred in patients with SVR in the first 12 months and about 45% of HCC has occurred in the 2nd year of follow-up. Nodule sizes were (1–4 cm) and 2 patients have developed multiple hepatic nodules. The Mean ± SE for the development of HCC is 22.89 ± 0.24 and with (22.42–23.36) 95% CI (Table 4, Figure 1). Characteristics of HCC patients were listed in table 5. Patients who are discovered to have HCC are referred to Hepatoma Board in Alrajhi Liver Hospital, Assiut University for further assessment and suitable line for management.
 |
Table 4 De-Novo Occurrence of HCC After Treatment in SVR and Non-SVR Patients |
 |
Table 5 Characteristics of HCC Patients with SVR and Non-SVR |
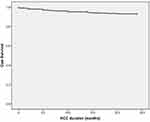 |
Figure 1 Kaplan–Meier curve for HCC occurrence after treatment. |
Discussion
The therapy of hepatitis C has dramatically changed since 2013. Direct-acting antivirals against HCV infection are new oral drugs, with potent antiviral activity, highly efficacious, relatively safe, and well tolerated, that can be used in for all patients with chronic HCV infection, including those with more advanced and complicated liver disease,11 which has been a major concern for hepatologists in the last few decades.12 Genotype 4 infections are seen in Africa and the Middle East, with a higher rate in Egypt, in particular.13 The response rate to DAAs in genotype 4 infections appears to be high in some real-world studies, regardless of cirrhosis status.14
Resolution of HCV infection in these patients leads to great expectations of possibility for preventing the most serious complications of liver cirrhosis, including the development of HCC.
Controversial data have emerged on HCC occurrence/recurrence after HCV eradication with DAAs. Most reports come from single-center, retrospective, observational studies, with differences in patients’ characteristics and duration of follow-up,2 while multiple large cohort studies have since demonstrated that DAA-induced SVR is associated with reduced risk of HCC occurrence.15–17 In other studies, an unexpected increased HCC recurrence and occurrence rate among HCV patients treated with DAAs combination has been reported, raising some concerns about a possible indirect role of the new antiviral drugs.10,18-20
Because of this debate, we tried in this current study to evaluate the impact of DAAs on patients with liver cirrhosis in our locality regarding the outcome and development of HCC.
In our study, SVR is in 94% of the included patient which in agreement with many studies, Calvaruso and his colleagues have reported that SVR is 95.2% in their liver cirrhosis patients,21 Also the ALLY-1 trial looks at the effects of Daclatasvir/Sofosbuvir with ribavirin on patients with advanced cirrhosis, including decompensated cirrhosis across 5 of the 6 major HCV genotypes, only genotype 5 is not represented. They have noted a high treatment response with Child-Pugh A or B cirrhosis (93%); SVR is 100% in genotype 4 patients.22
In our study, DM is in 30.3% of the studied patients; multiple studies throughout the world have shown an epidemiological association between HCV and type 2 diabetes mellitus (T2DM). The data from the National Health and Nutrition Examination Survey of nearly showed that10,000 patients from 1988 to 1994 had found that adults aged 40 years or older with HCV infection are nearly four times more likely to have concurrent diabetes than those without HCV infection.23 In a follow‐up case–control study of >1000 patients, Mehta and colleagues also have demonstrated that in patients with risk factors for metabolic syndrome, the presence of chronic HCV infection has increased the risk for development of T2DM by 11‐fold over a 9‐year follow‐up.24 In Italy, a study of 564 noncirrhotic HCV‐infected patients and control‐matched with noncirrhotic hepatitis B virus-infected patients has demonstrated an increased prevalence rate of T2DM of 12% versus 4.9% in controls (P = 0.008).25
In terms of the hepatic function, our study shows a significant improvement in the CP, without improvement in MELD scores, while Berge and his colleagues in their study have not shown a significant improvement in the CP and MELD scores, which may be because pre-treatment scores are already low.14 We have found that there is a statistically significant improvement in platelet counts and in albumin levels liked Berge study results .26
Patients who have achieved SVR have shown a significant reduction in the frequency of hepatic encephalopathy episodes, improvement in the management of ascites.
De-novo HCC has occurred in 22 out of 329 (6.7%) patients with SVR and in 5 out of 21 (23.8%) patients with non-SVR. All HCC in Patients with non-SVR has occurred in the first 10 months after end of treatment, while about 55% of HCC has occurred in patients with SVR in the first 12 months with 3.6% of the studied patients and about 45% of HCC has occurred in the 2nd year of follow-up. This result agrees with Conti and his colleagues who retrospectively have analyzed the occurrence of HCC in compensated patients who have achieved a SVR after IFN-free treatment with cirrhosis with no history of liver cancer and they have found that HCC occurrence rate is 3.1% within the first 6 months after treatment.19 Romano and his colleges in 2018 have studied a large sample of patients treated at several centers in Italy with a median follow-up of 17.4 months, ihe HCC occurrence rate during this period in the sub cohort of cirrhotic patients was the same as (or even lower than) expected without antiviral therapy. They have concluded that the incidence of HCC had significantly dropped after the first year and the reason for this is unclear, but it might relate to a greater reduction in intrahepatic inflammation in the longer term after stopping the antiviral therapy.27
In an analysis of data from a large prospective study of patients with hepatitis C virus–associated compensated or decompensated cirrhosis, Calvaruso et al have found that the SVR to DAA treatment has decreased the incidence of HCC over a mean follow-up of 14 months.21
This study results indicated that the occurrence of HCC is significantly higher in patients with non-SVR and the good response to treatment is protective and decreases HCC occurrence in the 2nd year of follow-up may be due to a greater reduction in intrahepatic inflammation in the longer term after stopping the antiviral therapy as Romano and his colleague have said.27
Conclusion
Treatment of HCV-related LC patients with sofosbuvir and daclatasvir with or without ribavirin for 3 or 6 months shows high SVR and significant improvement in CP score, but still at risk of HCC even if treated and should be followed up regularly according to screening programs with special meticulous attention to those with non-SVR.
Acknowledgments
We acknowledge all members of Assiut centre for liver and Alrajhi University Hospital for Liver.
Disclosure
The authors report no conflicts of interest in this work.
References
1. El-Zanaty F, Way A. Egypt Demographic and Health Survey 2008. Cairo, Egypt: Ministry of Health, El-Zanaty and Associates, and Macro International; 2009:431.
2. Waked I, Doss W, El-Sayed MH, et al. The current and future disease burden of chronic hepatitis C virus infection in Egypt. Arab J Gastroenterol. 2014;15(2):45–52. doi:10.1016/j.ajg.2014.04.003
3. Planas R, Ballesté B, Alvarez MA, et al. Natural history of decompensated hepatitis C virus-related cirrhosis. A study of 200 patients. J Hepatol. 2004;40(5):823–830. doi:10.1016/j.jhep.2004.01.005
4. Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61(2):69–90. doi:10.3322/caac.20107
5. Ryerson AB, Eheman CR, Altekruse SF, et al. Annual report to the Nation on the Status of Cancer, 1975–2012, featuring the increasing incidence of liver cancer. Cancer. 2016;122(9):1312–1337. doi:10.1002/cncr.29936
6. Moriya K, Fujie H, Shintani Y, et al. The core protein of hepatitis C virus induces hepatocellular carcinoma in transgenic mice. Nat Med. 1998;4(9):1065. doi:10.1038/2053
7. Burra P, Giannini EG, Caraceni P, et al. Specific issues concerning the management of patients on the waiting list and after liver transplantation. Liver Int. 2018;38(8):1338–1362. doi:10.1111/liv.13755
8. Buonfiglioli F, Brillanti S. Direct antiviral therapy for hepatitis C and hepatocellular carcinoma: facing the conundrum. Hepatoma Res. 2018;4:6. doi:10.20517/2394-5079.2017.42
9. Sangiovanni A, Prati GM, Fasani P, et al. The natural history of compensated cirrhosis due to hepatitis C virus: a 17-year cohort study of 214 patients. Hepatology. 2006;43(6):1303–1310. doi:10.1002/hep.21176
10. Reig M, Mariño Z, Perelló C, et al. Unexpected high rate of early tumor recurrence in patients with HCV-related HCC undergoing interferon-free therapy. J Hepatol. 2016;65:719–726.
11. Falade-Nwulia O, Suarez-Cuervo C, Nelson DR, Fried MW, Segal JB, Sulkowski MS. Oral direct-acting agent therapy for hepatitis C virus infection: a systematic review. Ann Intern Med. 2017;166(9):637–648. doi:10.7326/M16-2575
12. Zanetto A, Shalaby S, Ferrarese A, et al. Direct-acting antivirals and hepatocellular carcinoma occurrence and recurrence in hepatitis C virus-related liver cirrhosis: fact or fiction. Hepatoma Res. 2018;4:70. doi:10.20517/2394-5079.2018.102
13. Messina JP, Humphreys I, Flaxman A, et al. Global distribution and prevalence of hepatitis C virus genotypes. Hepatology. 2015;61(1):77–87. doi:10.1002/hep.27259
14. Gayam V, Khalid M, Mandal AK, et al. Direct-acting antivirals in chronic hepatitis C genotype 4 infection in community care setting. Gastroenterol Res. 2018;11(2):130. doi:10.14740/gr999w
15. Kanwal F, Kramer J, Asch SM, Chayanupatkul M, Cao Y, El-Serag HB. Risk of hepatocellular cancer in HCV patients treated with direct-acting antiviral agents. Gastroenterology. 2017;153(4):996–1005. doi:10.1053/j.gastro.2017.06.012
16. Li DK, Ren Y, Fierer DS, et al. The short-term incidence of hepatocellular carcinoma is not increased after hepatitis C treatment with direct-acting antivirals: an ERCHIVES study. Hepatology. 2018;67(6):2244–2253. doi:10.1002/hep.29707
17. Ioannou GN, Green PK, Berry K. HCV eradication induced by direct-acting antiviral agents reduces the risk of hepatocellular carcinoma. J Hepatol. 2017;
18. Rinaldi L, Di Francia R, Coppola N, et al. Hepatocellular carcinoma in HCV cirrhosis after viral clearance with direct acting antiviral therapy: preliminary evidence and possible meanings. WCRJ. 2016;3:e748.
19. Conti F, Buonfiglioli F, Scuteri A, et al. Early occurrence and recurrence of hepatocellular carcinoma in HCV-related cirrhosis treated with direct acting antivirals. J Hepatol. 2016;65:727–733. doi:10.1016/j.jhep.2016.06.015
20. Kozbial K, Moser S, Schwarzer R, et al. Unexpected high incidence of hepatocellular carcinoma in cirrhotic patients with sustained virologic response following interferon-free direct-acting antiviral treatment. J Hepatol. 2016;65(4):856–858. doi:10.1016/j.jhep.2016.06.009
21. Calvaruso V, Cabibbo G, Cacciola I, et al. Incidence of hepatocellular carcinoma in patients with HCV-associated cirrhosis treated with direct-acting antiviral agents. Gastroenterology. 2018;155(2):411–421. doi:10.1053/j.gastro.2018.04.008
22. Poordad F, Schiff ER, Vierling JM, et al. Daclatasvir with sofosbuvir and ribavirin for hepatitis C virus infection with advanced cirrhosis or post-liver transplantation recurrence. Hepatology. 2016;63(5):1493–1505. doi:10.1002/hep.28446
23. Mehta SH, Brancati FL, Sulkowski MS, et al. Prevalence of type 2 diabetes mellitus among persons with hepatitis C virus infection in the United States. Ann Intern Med. 2000;133:592–599. doi:10.7326/0003-4819-133-8-200010170-00009
24. Mehta SH, Brancati FL, Strathdee SA, et al. Hepatitis C virus infection and incident type 2 diabetes. Hepatology. 2003;38:50–56. doi:10.1053/jhep.2003.50291
25. Antonelli A, Ferri C, Fallahi P, et al. Hepatitis C virus infection: evidence for an association with type 2 diabetes. Diabetes Care. 2005;28(10):2548–2550. doi:10.2337/diacare.28.10.2548
26. Berge E, Arencibia A, Otón E, Cejas L, Acosta S, Pérez F. Clinical outcomes of direct-acting antiviral therapy in patients with compensated hepatitis C virus-related cirrhosis. Hepatoma Res. 2017;3(9):209–214. doi:10.20517/2394-5079.2017.28
27. Romano A, Angeli P, Piovesan S, et al. Newly diagnosed hepatocellular carcinoma in patients with advanced hepatitis C treated with DAAs: a prospective population study. J Hepatol. 2018;69(2):345–352. doi:10.1016/j.jhep.2018.03.009
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
