Back to Journals » Cancer Management and Research » Volume 12
Diagnosis and Surgical Treatment and Pathological Findings of Solid Pseudopapillary Tumor of the Pancreas: A Single-Institution Experience
Authors Guo T, Wang L, Xie P, Zhang Z, Yu Y
Received 17 November 2019
Accepted for publication 14 January 2020
Published 23 January 2020 Volume 2020:12 Pages 581—588
DOI https://doi.org/10.2147/CMAR.S238527
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Antonella D'Anneo
Tong Guo, Lu Wang, Peng Xie, Zhiwei Zhang, Yahong Yu
Department of Biliary-Pancreatic Surgery, Affiliated Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, Hubei, People’s Republic of China
Correspondence: Yahong Yu
Department of Biliary-Pancreatic Surgery, Affiliated Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology, 1095 Jiefang Avenue, Wuhan 430030, Hubei, People’s Republic of China
Tel +86 13907190038
Email [email protected]
Purpose: To investigate the diagnosis, surgical treatment, and pathology of solid pseudopapillary tumors of the pancreas in our institution.
Patients and Methods: We retrospectively analyzed the demographic details, clinical features, imaging findings, and pathological findings of 87 patients with a confirmed diagnosis of solid pseudopapillary tumors of the pancreas (SPTP) and underwent surgery in Tongji Hospital of Tongji Medical College, over a period of 8 years from 2011 to 2018.
Results: Our study involved a total of 87 patients (16 males and 71 females) with a mean age of 31.3± 13.1 years (range: 10– 61 years). The main compliant was abdominal pain or discomfort (n=49) and the median tumor size was 58.6± 31.7 mm (range: 16– 156mm). Tumors were located in the head (27 patients, 31%), the neck (13 patients, 15%), and the body and tail (47 patients, 54%). There were no significant differences between the patients in terms of sex, age, or tumor location. Partial pancreatectomy was performed in 79 patients, enucleation in six patients, and total pancreatectomy in two patients. R0 resection was achieved in 86 patients. The postoperative morbidity was 36.8%, and the main complication was pancreatic fistula. Pathological examination and immunohistochemical markers were used to provide a final diagnosis. The main follow-up period was 46 months (range: 13– 97 months). At the end of the follow-up period, 86 patients were alive and had not experienced recurrence; one patient was lost to follow-up.
Conclusion: The accurate diagnosis of SPTP is vital. Our data showed that surgical resection is safe and associated with low morbidity and mortality rates. Pathological findings can play an important role in diagnosis and long-term survival.
Keywords: solid pseudopapillary tumor, pancreas, diagnosis, surgical strategy
Introduction
The first description of the disease was published by Frantz in 1959.1 These tumors were subsequently reclassified as solid pseudopapillary tumors (SPTs) by the World Health Organization in 1996,2 and then as solid pseudopapillary neoplasms (SPNS) in 2010.3 The precise origin of this form of tumor remains unclear, although some previous studies have suggested that they originate from cells related to the genital ridge.4 Previous studies have reported that SPTP represents only 1–2% of the pancreatic neoplasms and are associated with low-grade malignancies.5 However, as preoperative examination methods have improved, and increasing number of patients are being identified as having SPTP and those patients may be diagnosed with cystadenoma of pancreas or pancreatic neuroendocrine tumors without the improved examination methods. Surgery remains the first choice of treatment for this form of tumor and represents the only curative option. However, a range of surgical procedures have been reported, including local excisions, radical resections, and debulking procedures.6 There is a clear need to develop more effective methods for the diagnosis and treatment of SPTP and thus improve patient prognosis. We therefore carried out a retrospective analysis of clinical data including clinical features, surgical strategies, pathology features and immunohistochemistry results from 87 patients who had been diagnosed with SPTP and treated in Tongji Hospital of Tongji Medical College between January 2011 and December 2018.
Materials and Methods
We collected and analyzed a range of clinical data from 87 patients who had been diagnosed and treated for SPTP in Tongji Hospital of Tongji Medical College between January 2011 and December 2018, including demographic data, clinical presentation, pathological features, and surgical strategy.
The indications for surgery included the clinical manifestations and imaging diagnosis of SPTP, or a lesion, in the pancreas that had been prompted by endoscopic ultrasound-guided fine-needle aspiration cytology (FNAC). All patients underwent surgery by the same team of pancreatic surgeons in our pancreas center. R0 resection was the primary aim, although the specific location and size of the tumor were used to select the appropriate surgical method, including total pancreatectomy, distal pancreatectomy (LDP, ODP), distal pancreatectomy spleen-preserving, pancreaticoduodenectomy (LPD, OPD), middle pancreatectomy (MP), and enucleation. Total pancreatectomy, vascular resection, and metastasectomy resection were performed whenever deemed appropriate to achieve complete resection.
There were a range of postoperative complications, including wound infection, abdominal pain, abdominal infection, delayed gastric emptying (DGE), pancreatitis, pancreatic fistulae (PF), hemorrhage, and mortality. DGE was defined and graded according to the International Study Group for Pancreatic Surgery7 while PF was defined and graded according to the International Study Group on Pancreatic Fistula (ISGPF).8
In all patients, the diagnosis of SPTP was confirmed pathologically by histological and immunohistochemical findings. We determined the expression of PCK, CyclinD1, Syn, PR, Cga, Vim, EMA, E-cadherin, CD10, CD56, CK8/18, β-catenin, and KI67 and classified the relative expression as no expression (-), weak expression (±) and high expression (+). The tumor was defined as being malignant if we detected metastasis in the liver, or other organs, or invasion of the peripheral nerves or vessels, or the involvement of lymph nodes.
Patients were followed up every 3 months in the first year, every 6 months over the next 2 years, and annually thereafter. Follow-up examinations included clinical manifestations, a physical examination, blood tests, and an abdominal ultrasound scan. If any of these tests were positive, we carried out a total abdomen computed tomography (CT) scan to rule out recurrence. During follow-up, we directly telephone interview the patients and acquired data from electronic medical records.
All statistical analyses were performed using Statistical Product and Service Solutions (SPSS) software, version 21.0, for Windows. Continuous data are expressed as means ± standard deviation (SD). The independent t test was used to analyze continuous data while the Chi-square test, or Fisher’s exact test, was used for categorical variables. The level of statistical significance was set at p<0.05.
All patients provided written informed consent prior to the retrospective data retrieval from medical records. This study was examined and approved by the medical ethics committee of Tongji hospital of Tongji Medical College of Huazhong University of Science and Technology. The study was conducted according to the principles expressed in the Declaration of Helsinki.
Results
Patients Characteristics
Between January 2011 and December 2018, 87 patients were diagnosed with SPTP and underwent surgery in Tongji Hospital of Tongji Medical College. Of these, 16 were male and 71 were female. The median patient age was 31.3±13.1 years (range: 10–61 years) and the median tumor size was 58.6±31.7mm (range: 16–156mm). The clinical features were non-specific, including abdominal pain or discomfort (n=49, 56.3%), nausea (n=4, 4.6%), abdominal mass (n=5, 5.7%), although some patients were asymptomatic (n=29, 33.3%). Tumors were located in the head (27 patients, 31%), neck (13 patients, 15%), body and tail (47 patients, 54%). Patient characteristics are given in Table 1.
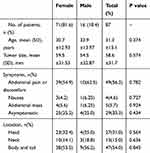 |
Table 1 The Clinical Features of the Patients Involved in This Study |
Preoperative Examinations
We tested the serum levels of serum carcinoembryonic antigen (CEA) and carbohydrate antigen 19–9 (CA19-9) in all patients. All patients were scanned by CT prior to surgery. In four patients, endoscopic ultrasound-guided fine-needle aspiration cytology (FNAC) was carried out in order to obtain an accurate diagnosis.
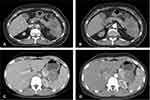
The typical CT appearance of an SPTP was a sharply defined tumor containing cystic areas of hemorrhage and necrotic changes; these characteristics were evident in 33 patients. Our analysis showed that of the 87 tumors examined, 14 were completely cystic, 63 were solid-cystic, and 10 were completely solid. Calcification was observed in 14 cases. One patient had liver metastases and two others showed invasion of the superior mesenteric vein and portal vein. Data acquired from blood tests and imaging studies are shown in Table 2. Figure 1 shows the CT images of SPTP.
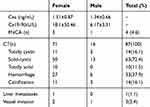 |
Table 2 Preoperative Examination Results |
Surgical Strategy and Complications
Data relating to the location and size of the tumor were used to select a suitable surgical method. In total, 51 patients with lesions in the body and/or tail underwent a distal pancreatectomy (26 LDP and 25 ODP), including six spleen-preserving resections. Twenty-four patients underwent pancreaticoduodenectomy (7 LPD and 17 OPD), four patients underwent middle pancreatectomy, and six patients underwent enucleation. Two patients underwent pancreatectomy, one underwent partial superior mesenteric vein resection, one underwent partial portal vein resection, and one received partial liver resection in order to achieve complete resection.
There were no surgical mortalities. The main complication was pancreatic fistula, which occurred in 21 patients (19 patients were classified as Grade A, and two patients were classified as Grade B); none were classified as Grade C. A range of other complications were observed, including wound infection (n=1), abdominal pain (n=3), abdominal infection (n=2), delayed gastric emptying (n=1), and pancreatitis (n=3). Hemorrhage was the most serious postoperative complication, and occurred in one patient. All complications were cured following prompt treatment and none of the patients required another round of surgery. Surgical strategies and complications are described in Tables 3 and 4.
 |
Table 3 Surgical Strategies |
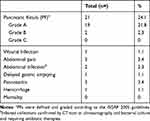 |
Table 4 Complications Noted During Our Study |
Macroscopic and Microscopic Features
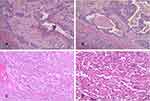
Our primary goal was R0 resection. All surgical specimens were assessed pathologically by two experienced pathologists. Analysis showed that we achieved a clear margin in 86 patients, and an involved margin in one patient. Three patients showed pancreatic parenchymal invasion, one patient showed perineural invasion, and two showed local regional invasion when examined under the microscope. These data are shown in Table 5. Figure 2 shows the pathologic image results.
 |
Table 5 Pathological Features |
Immunohistochemistry Results
In addition to pathological examination, all of the surgical specimens were also assessed immunohistochemically. Our results showed that SPTPs expressed a range of proteins, including pan cytokeratin (n=40), vimentin (n=83), β-catenin (n=86), cyclinD1 (n=75), synaptophysin (n=65), progesterone receptor (n=54), chromogranin A (n=5), epithelial membrane antigen (n=0), E-cadherin (n=1), CK8/18 (n=13), CD10 (n=82), CD56 (n=86), and Ki-67 (n=3). Immunohistochemical data are shown in Table 6.
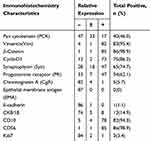 |
Table 6 Immunohistochemistry Results |
Follow-Up
During follow-up, patients were assessed for clinical manifestations, and underwent a physical examination, blood tests and an abdominal ultrasound scan and CT, if necessary. There are no patients suffered recurrence with a median follow-up period of 46 months (range: 13–97). One patient was lost to follow-up.
Discussion
Solid pseudopapillary tumors of the pancreas (SPTPs) are a rare form of neoplasm with low malignant potential and account for 1–2% of all pancreatic neoplasms.5 SPTPs often occur in young women in the second or third decade of life; this suggests the potential involvement of sex hormones, although there is no direct evidence for this at the present time.9 Several previous studies have indicated that males presenting with SPTP are older,10 so as to our study (males 33.9±13.97 vs females 30.7±12.93), but we found no difference between the males and females with regards to clinicopathological characteristics.
There are no specific clinical features associated with SPTP, although 70–90% of the patients present with symptoms.11 In our study, we found that 58 patients (66.7%) had clinical symptoms and 29 patients (33.3%) were asymptomatic. These symptoms included abdominal pain, discomfort, nausea, and abdominal masses. Recent studies have also shown an increasing trend for asymptomatic patients, thus concurring with our present study.
We found that the mean tumor size in our patients was 58.6±31.7 mm (range: 16–156mm), and also found that the tumors were smaller in males than females (54.5±32.87 vs 59.5±31.53mm); this is consistent with previous studies, but was not statistically significant.12 We also found that the body and tail were more commonly involved both in males and females; this was consistent with the previous findings of Lee et al, who reported that 69.4% of SPTPs were located in the pancreatic body or tail.13 Yu et al further reported that the size and location of a tumor could not predict malignancy,14 although Kim et al considered that a tumor that was larger than 5 cm represented a risk factor for malignancy.15 Our experience indicates that tumor size and location are not factors that are associated with malignancy.
Due to its sensitivity and specificity, CT is the first choice for diagnosing SPTP.16 In addition, MRI can also identify the cystic, solid-cystic, and hemorrhagic areas of SPTP.17 Most of our patients were diagnosed incidentally by imaging examinations (such as US, CT, MRI, PET) without particular clinical symptoms. The accuracy of EUS with FNA for the diagnosis of SPTs ranges from 41.2% to 69%,6,18 and is becoming increasingly accepted by surgeons, especially for patients who are difficult to diagnose.19 However, some authors have argued that EUS with FNA should not be the first choice due to the uncertain potential for malignancy and the high risk of false negatives.20 Consequently, it is necessary to use a combination of techniques when examining patients.
Surgical resection is the only curative treatment for SPTP whenever metastasis, local invasion, or lymph invasion is evident. At our institution, our primary goal is R0 resection. Our aim is to use surgery to preserve the pancreas in all patients, if at all possible. The location and size of a tumor is used to select the appropriate surgical approach. Distal pancreatectomy, with or without splenectomy, was used for tumors in the pancreatic body and/or tail, while pancreatoduodenectomy was used for tumors in the pancreatic head. Enucleation was performed when tumors were smaller than 3 cm and had been confirmed not to be associated with the common bile duct and the main pancreatic duct. Enhanced CT was also used to assess how resectable a tumor was, along with vascular involvement and metastasis.21 SMV/PV resection was planned when there was evidence of vessel wall involvement according to the CT scan or the MRI results and two patients received SMV/PV resection and reconstruction due to SMV/PV involvement. One patient underwent partial hepatectomy in order to resect liver metastasis. Two other patients received total pancreatectomy due to atrophy of the pancreas caused by tumor compression. Overall, we achieved R0 resection in 86 patients. No extensive lymphatic dissection was required because we only found one patient with lymph node metastasis in our study (the patient was suspected to pancreatic cancer so the lymph nodes (NO.10,11,18) around the body and tail of the pancreas were dissected)this concurs with the previous findings of Suzuki et al.22 The role of neo-adjuvant or adjuvant chemotherapy, and radiotherapy, in the treatment of SPT is limited,23,24 but Brunetti et al find an interesting result that a patient diagnosed to SPTP with malignant transformation treated with adjuvant chemotherapy achieved a long-duration.25
In the present study, we found that pancreatic fistulas were the predominant complication (n=21 patients); grade A fistulas were found in 19 patients, while grade B fistulas were found in two patients; we did not identify any grade C fistulas. Postoperative bleeding was the most dangerous complication and one of the patients who underwent vascular resections suffered hemorrhage post operation and was cured by conservative treatment such as drainage and hemostatic.
Previous studies have reported that 10% of the patients experience recurrence after resection22 and that lymphadenectomy and microscopic margins are not strong prognostic factors for disease recurrence.26 We found no recurrence in patients undergoing liver metastasis resection or SMV/PV resection; these findings concurred with those of previous studies,27,28 showing that radical resection is safe and effective. At a mean follow-up of 46 months, 86 patients were disease-free (even one patient has positive margin in the stump of the pancreas), showed an excellent prognosis. These excellent long-term outcomes may be due to the fact that the surgeries were performed by experienced surgeons. We did lose one patient to follow-up; however, this should be taken into consideration when interpreting our outcomes.
An SPTP contains a mixture of solid, cystic, and pseudopapillary patterns in a variety of proportions,9 and is composed of small, uniform tumor cells with round nuclei and an eosinophilic cytoplasm.22,29 Biopsy and hematoxylin and eosin staining may not be able to differentiate SPTP from acinar cell carcinomas and pancreatic neuroendocrine tumors. Thus, immunohistochemical tests should be used to clarify the diagnosis.30 Our immunohistochemical assays showed that β-catenin was the most characteristic feature of SPTPs, and was detected in all of our patients. SPTPs can also express a range of proteins that are not specific for the tumor.31,32 Previous work has shown that SPT is typically positive for vimentin (Vim), and neuron-specific enolase (NSE);33 our present findings were consistent with this previous data. We also found high levels of CD56, although a recent study reported that the unique immunohistochemical features of CD56 expression were unclear.34 SPTP cells are also known to express synaptophysin (Syn), chromogranin A, CD10, cytokeratin (CK), and the progesterone receptor (PR); consequently, all of these proteins could be used to distinguish SPTPs from other tumors, particularly neuroendocrine tumors. However, none of these pathological factors can accurately predict the outcome of SPTP. We therefore tested Ki-67, which is known to be able to predict poor outcome in SPTP patients.26,31 In our study, we found that one in three patients with malignant tumors was positive for Ki-67, but we found no recurrence of the patient.
There are several limitations to our study that need to be considered. For example, we had a short follow-up time, and our dataset was limited due to the retrospective nature of our study. Further studies should be carried out using larger datasets.
In conclusion, SPTP is a low-grade malignant tumor that generally occurs in young women without significant symptoms. Surgical resection is the only curative procedure and is associated with low morbidity and mortality rates, even in patients with metastases and vascular invasion. Following surgery, patients can achieve excellent long-term survival rates. Pathological and immunohistochemical examination can help to make a definite diagnosis. Accurate diagnoses and follow-up are vital in order to increase the prognosis of the patients affected.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Yang J, Cong X, Ren M, et al. Circular RNA hsa_circRNA_0007334 is predicted to promote MMP7 and COL1A1 expression by functioning as a miRNA sponge in pancreatic ductal adenocarcinoma. J Oncol. 2019;2019:7630894. doi:10.1155/2019/7630894
2. Kloppel G, Heitz PU, Capella C, Solcia E. Pathology and nomenclature of human gastrointestinal neuroendocrine (carcinoid) tumors and related lesions. World J Surg. 1996;20(2):132–141. doi:10.1007/s002689900021
3. Dai G, Huang L, Du Y, Yang L, Yu P. Solid pseudopapillary neoplasms of the pancreas: clinical analysis of 45 cases. Int J Clin Exp Pathol. 2015;8(9):11400–11406.
4. Estrella JS, Li L, Rashid A, et al. Solid pseudopapillary neoplasm of the pancreas: clinicopathologic and survival analyses of 64 cases from a single institution. Am J Surg Pathol. 2014;38(2):147–157. doi:10.1097/PAS.0000000000000141
5. Hackeng WM, Hruban RH, Offerhaus GJ, Brosens LA. Surgical and molecular pathology of pancreatic neoplasms. Diagn Pathol. 2016;11(1):47. doi:10.1186/s13000-016-0497-z
6. Law JK, Ahmed A, Singh VK, et al. A systematic review of solid-pseudopapillary neoplasms: are these rare lesions? Pancreas. 2014;43(3):331–337. doi:10.1097/MPA.0000000000000061
7. Wente MN, Bassi C, Dervenis C, et al. Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery. 2007;142(5):761–768. doi:10.1016/j.surg.2007.05.005
8. Bassi C, Dervenis C, Butturini G, et al. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005;138(1):8–13. doi:10.1016/j.surg.2005.05.001
9. Yu PF, Hu ZH, Wang XB, et al. Solid pseudopapillary tumor of the pancreas: a review of 553 cases in Chinese literature. World J Gastroenterol. 2010;16(10):1209–1214. doi:10.3748/wjg.v16.i10.1209
10. Hirabayashi K, Kurokawa S, Maruno A, et al. Sex differences in immunohistochemical expression and capillary density in pancreatic solid pseudopapillary neoplasm. Ann Diagn Pathol. 2015;19(2):45–49. doi:10.1016/j.anndiagpath.2015.02.002
11. Reddy S, Cameron JL, Scudiere J, et al. Surgical management of solid-pseudopapillary neoplasms of the pancreas (Franz or Hamoudi tumors): a large single-institutional series. J Am Coll Surg. 2009;208(5):
12. Xu Y, Zhao G, Pu N, et al. One hundred twenty-one resected solid pseudopapillary tumors of the pancreas: an 8-year single-institution experience at Zhongshan Hospital, Shanghai, China. Pancreas. 2017;46(8):1023–1028. doi:10.1097/MPA.0000000000000885
13. Lee SE, Jang JY, Hwang DW, Park KW, Kim SW. Clinical features and outcome of solid pseudopapillary neoplasm: differences between adults and children. Arch Surg. 2008;143(12):1218–1221. doi:10.1001/archsurg.143.12.1218
14. Yu P, Cheng X, Du Y, et al. Solid pseudopapillary neoplasms of the pancreas: a 19-year multicenter experience in China. J Gastrointest Surg. 2015;19(8):1433–1440. doi:10.1007/s11605-015-2862-8
15. Kim MJ, Choi DW, Choi SH, Heo JS, Sung JY. Surgical treatment of solid pseudopapillary neoplasms of the pancreas and risk factors for malignancy. Br J Surg. 2014;101(10):1266–1271. doi:10.1002/bjs.9577
16. Patil TB, Shrikhande SV, Kanhere HA, Saoji RR, Ramadwar MR, Shukla PJ. Solid pseudopapillary neoplasm of the pancreas: a single institution experience of 14 cases. HPB (Oxford). 2006;8(2):148–150. doi:10.1080/13651820510035721
17. Yao X, Ji Y, Zeng M, Rao S, Yang B. Solid pseudopapillary tumor of the pancreas: cross-sectional imaging and pathologic correlation. Pancreas. 2010;39(4):486–491. doi:10.1097/MPA.0b013e3181bd6839
18. Law JK, Stoita A, Wever W, et al. Endoscopic ultrasound-guided fine needle aspiration improves the pre-operative diagnostic yield of solid-pseudopapillary neoplasm of the pancreas: an international multicenter case series (with video). Surg Endosc. 2014;28(9):2592–2598. doi:10.1007/s00464-014-3508-8
19. Chhadi TS, Deshpande AH, Chhadi SA, Kumbhalkar DT, Raut WK. A solid pseudopapillary tumour of the head of pancreas: a rare case report diagnosed by fine needle aspiration cytology. J Clin Diagn Res. 2016;10(6):Ed06–Ed08. doi:10.7860/JCDR/2016/19456.7929
20. Papavramidis T, Papavramidis S. Solid pseudopapillary tumors of the pancreas: review of 718 patients reported in English literature. J Am Coll Surg. 2005;200(6):965–972. doi:10.1016/j.jamcollsurg.2005.02.011
21. Shrikhande SV, Barreto SG, Goel M, Arya S. Multimodality imaging of pancreatic ductal adenocarcinoma: a review of the literature. HPB (Oxford). 2012;14(10):658–668. doi:10.1111/j.1477-2574.2012.00508.x
22. Suzuki S, Hatori T, Furukawa T, Shiratori K, Yamamoto M. Clinical and pathological features of solid pseudopapillary neoplasms of the pancreas at a single institution. Dig Surg. 2014;31(2):143–150. doi:10.1159/000363420
23. Ji S, Xu J, Zhang B, et al. Management of a malignant case of solid pseudopapillary tumor of pancreas: a case report and literature review. Pancreas. 2012;41(8):1336–1340. doi:10.1097/MPA.0b013e31824d52c7
24. Kumar NAN, Bhandare MS, Chaudhari V, Sasi SP, Shrikhande SV. Analysis of 50 cases of solid pseudopapillary tumor of pancreas: aggressive surgical resection provides excellent outcomes. Eur J Surg Oncol. 2019;45(2):187–191. doi:10.1016/j.ejso.2018.08.027
25. Brunetti O, Aprile G, Marchetti P, et al. Systemic chemotherapy for advanced rare pancreatic histotype tumors: a retrospective multicenter analysis. Pancreas. 2018;47(6):759–771. doi:10.1097/MPA.0000000000001063
26. Butte JM, Brennan MF, Gonen M, et al. Solid pseudopapillary tumors of the pancreas. Clinical features, surgical outcomes, and long-term survival in 45 consecutive patients from a single center. J Gastrointest Surg. 2011;15(2):350–357. doi:10.1007/s11605-010-1337-1
27. Martin RC, Klimstra DS, Brennan MF, Conlon KC. Solid-pseudopapillary tumor of the pancreas: a surgical enigma? Ann Surg Oncol. 2002;9(1):35–40. doi:10.1245/aso.2002.9.1.35
28. Sperti C, Berselli M, Pasquali C, Pastorelli D, Pedrazzoli S. Aggressive behaviour of solid-pseudopapillary tumor of the pancreas in adults: a case report and review of the literature. World J Gastroenterol. 2008;14(6):960–965. doi:10.3748/wjg.14.960
29. Cai H, Zhou M, Hu Y, et al. Solid-pseudopapillary neoplasms of the pancreas: clinical and pathological features of 33 cases. Surg Today. 2013;43(2):148–154. doi:10.1007/s00595-012-0260-3
30. Wang P, Wei J, Wu J, et al. Diagnosis and treatment of solid-pseudopapillary tumors of the pancreas: a single institution experience with 97 cases. Pancreatology. 2018;18(4):415–419. doi:10.1016/j.pan.2017.12.012
31. Guo N, Zhou QB, Chen RF, et al. Diagnosis and surgical treatment of solid pseudopapillary neoplasm of the pancreas: analysis of 24 cases. Can J Surg. 2011;54(6):368–374. doi:10.1503/cjs.011810
32. Ud Din N, Arshad H, Ahmad Z. Solid pseudopapilllary neoplasm of the pancreas. A clinicopathologic study of 25 cases from Pakistan and review of Literature. Ann Diagn Pathol. 2014;18(6):358–362. doi:10.1016/j.anndiagpath.2014.10.001
33. Kosmahl M, Seada LS, Janig U, Harms D, Kloppel G. Solid-pseudopapillary tumor of the pancreas: its origin revisited. Virchows Arch. 2000;436(5):473–480. doi:10.1007/s004280050475
34. Geers C, Moulin P, Gigot JF, et al. Solid and pseudopapillary tumor of the pancreas–review and new insights into pathogenesis. Am J Surg Pathol. 2006;30(10):1243–1249. doi:10.1097/01.pas.0000213311.28682.b2
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.