Back to Journals » Journal of Multidisciplinary Healthcare » Volume 15
Demographic Characteristics and Digital Platforms for Physical Activity Among the Chinese Residents During the COVID-19 Pandemic: A Mediating Analysis
Authors Fang P, Shi S, Menhas R , Laar RA , Saeed MM
Received 29 December 2021
Accepted for publication 25 February 2022
Published 16 March 2022 Volume 2022:15 Pages 515—529
DOI https://doi.org/10.2147/JMDH.S354984
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Ping Fang,1 Shusheng Shi,1 Rashid Menhas,2 Rizwan Ahmed Laar,3 Muhammad Muddasar Saeed4
1School of Sports Science and Physical Education, Nanjing Normal University, Nanjing, Jiangsu Province, People’s Republic of China; 2Research Center of Sports Social Sciences, School of Physical Education and Sports, Soochow University, Suzhou, Jiangsu Province, People’s Republic of China; 3College of Physical Education, Hubei Normal University, Huangshi, Hubei Province, People’s Republic of China; 4International Education College Chinese and Western Medicine Clinic, Dalian Medical University, Dalian, Liaoning, People’s Republic of China
Correspondence: Rashid Menhas, Research Center of Sports Social Sciences, School of Physical Education and Sports, Soochow University, Suzhou, Jiangsu Province, People’s Republic of China, Email [email protected] Rizwan Ahmed Laar, College of Physical Education, Hubei Normal University, Huangshi, Hubei Province, People’s Republic of China, Email [email protected]
Background: E-health apps play a vital role in the era of the COVID-19 pandemic. More people across the globe have started to use fitness and health apps to mitigate the COVID-19 negative impacts on the health-related quality of life. E-health treatments are becoming more common these days.
Aim: The present research aim was to explore the mediating role of digital platforms for physical activity and fitness with demographic characteristics among Chinese people during the pandemic.
Methods: The primary data was collected through an online survey across China under the snowball sampling technique. A total of 5351 respondents took part in the online questionnaire survey. After quantification and quality check of the data, a total of 5000 respondents’ responses were added in the final analysis. The collected data were analyzed by using SPSS-25 and SmartPLS 3.0 software.
Results: The structural equation model analysis H1 (β = 0.227, t = 18.725, p = < 0.000), H2 (β = 0.225, t = 17.892, p = < 0.000), H3 (β = 0.229, t = 17.845, p = < 0.000), H4 (β = 0.54, t = 60.928, p= < 0.000), H5 (β = 0.553, t = 57.291, p = < 0.000), H6 (β = 0.559, t = 56.956, p = < 0.000), H7 (β = 0.358, t = 24.779, p = < 0.000), H8 (β = 0.259, t = 19.617, p = < 0.000) and H9 (β = 0.288, t = 19.92, p = < 0.000) results confirm the proposed hypothesis of the study.
Conclusion: E-health apps are playing a vital role in maintaining an active lifestyle through physical activity. Fitness and health apps can promote physical activity and improve health-related quality of life. Results of the current study concluded that E-health apps are promising to promote physical activity and fitness during the COVID-19 preventive measures.
Keywords: COVID-19, digital platforms, demographic characteristics, physical activity, Chinese people
Introduction
A global lockdown has been imposed due to the daily increase in COVID-19 cases and deaths. Lockdown imposed by the government is said to be a successful COVID-19 prevention strategy.1 Most governments throughout the world have imposed movement restrictions to stem the spread of the COVID-19 virus. Examples include travel prohibitions between and within countries, commercial and public space closures, and long domestic isolation.2 Due to the closing of gyms, sports fields, and parks, as well as severe limitations on outdoor mobility, millions of individuals have been driven to adopt an exceptionally sedentary lifestyle. The forced physical inactivity, together with the documented advent of unhealthy neurotic tendencies such as smoking, drinking, and appetite, pose a significant threat to the affected population’s fitness and wellbeing. Human physical activities have been shown to impact our daily lives substantially. Exercise regularly helps avoid diseases like cognitive decline, maintain a healthy weight, and alleviate sadness and anxiety symptoms.3 Our living environments and lives are continually changing as a result of technological advancements. Self-administered physical activity surveys are used to monitor the health of local (eg, fitness bands) that tracked physical activity and recorded and computed motion capture patterns for study. Modern electronic devices, such as activity trackers, gyroscopes, and monitoring devices, give physical activity parameters such as estimated distance, time spent in various intensity levels of physical activity, steps, heart rate, and energy expenditure.4
Healthcare workers could significantly impact how new technology is selected and used. Due to sharing this information, scholars and healthcare practitioners will be better equipped to incorporate rising technologies into physical activity and health. We can now use our smartphones to connect with others over the phone, via email, and SMS and track our health and physical activity habits using a variety of health-related apps.5 In truth, existing electronic devices appeal to healthcare providers because they make creative use of developing technology like mobile device apps, the global positioning system (GPS) units, and health wearable’s to improve ease of use, accuracy, and scope (ie, data from various sources from one device). Knowing where, when, and how physical activity occurs using this information helps better understand physical activity patterns and, as a result, more successful physical activity behavioral modifications. Rapid technological improvements have led to the inclusion of accelerometers capable of measuring physical activity and sedentary behavior in smartphones and global positioning system devices. While technological improvements enable the general public to engage in daytime sleepiness, the introduction of motion sensors into an increasing number of electronic devices allows specialists to objectively analyze physical activity and sedentary behavior to address various health conditions.6 The current research explores the mediating role of digital platforms for physical activity and fitness related to demographic characteristics among Chinese residents during the pandemic.
Theoretical Framework
According to studies based on the self-determination theory, the strength of enthusiasm predicts people’s physical activity levels. A person with greater autonomous motivation is more likely to engage in regular physical activity than those with externally controlled causes, such as guilt and shame for not being active or peer pressure.7 Motivational regulation is directed by goals distinct from the behavior but in line with the individual’s identity and values (ie, intrinsic motivation).8 Motivational regulations are directed by goals that differ from the behavior but align with the individual’s characters and values (ie, recognized or integrated parameter). Diverse intervention techniques may be required to promote these various forms of autonomous motivation. People are more likely to engage in effective self-regulation when their desire for physical activity is independent.9,10 The cognition theory explained how people’s emotional and behavioral behaviors are influenced by their perceptions of situations. Physical exercise has been demonstrated to be beneficial for both physical and psychological health.11,12 Health, technology, data tracking of health behaviors, and the importance of health behavior theory and behavior change strategies are all important topics to learn more about, especially as innovation is becoming more pervasive in daily life. For many things, the Theory of Planned Behavior (TPB)13 is an acceptable theory to utilize to understand the internet and health habits. For starters, there is a TPB and activity survey validated.14
Perceptions and beliefs have been shown to impact health and wellbeing significantly and very well. Several studies have shown that having good health ideas and advantages regarding fitness improves one’s health.15 Social isolation has profoundly altered the world population’s behavior in all patterns, such as job, household managing, and daily fitness.16 The protection motivation theory (PMT), which exposes people’s perception of risk and explores the ability to adopt safety precautions heavily affected by high levels of perceived risk, is among the essential health behavior theories for affecting behavior. According to the hypothesis, people’s perceptions of the severity and vulnerability of a health hazard influence their risk perception of the disease. Rogers created and improved the PMT.17,18 It has been frequently employed in recent years as a framework for explaining why people want to engage in protective actions when faced with a health risk.19 PMT is a health promotion theory that has been effectively utilized to link younger people’s perceptions of health risks with their engagement in preventive practices. The role of cognitive abilities in health-related decision-making is emphasized in social-cognitive models of health behavior, which have been beneficial in uncovering psychological variables behind the desire to engage in healthy activities, for example, physical activity.20
Hypotheses Development
To prevent COVID-19 transmission, various measures have been implemented, including social distance, the closure of non-essential services, meeting limitations, and travel restrictions. Due to the closure of gyms, parks, and restrictions on recreational activities, these measures have a severe influence on all individuals’ physical health and quality of life.21 Increased physical activity and exercise in one’s daily routine may assist in mitigating the effects of muscle atrophy owing to inactivity, insufficient respiratory capacity, frailty risk, and poor mental health. Furthermore, COVID-19 may overstimulate the immune system, resulting in an overabundance of immune cells and cytokines, targeting the person’s cells, causing tissue damage.22 Domestic isolation negatively impacts the physical activity level of the masses. Screen time is enlarged, which further negatively impacts physical and psychological wellbeing. Individuals can stay active by using smartphone fitness apps that offer home-based workouts.23 More and more people’s daily activities have shifted from offline to online - from indoor sports using online resources to forming and sustaining relationships using apps. People experimented with numerous methods of exercising at home. One option was to employ fitness apps like Keep, a popular Chinese mobile fitness community with over 150 million subscribers. It encouraged users to continue their home exercise and preserve good mental health through bodily exercises during the epidemic.24 Our study hypotheses related to COVID-19 preventive measures and physical activity are;
Hypothesis 1 (H1): COVID-19 preventive measures (CPM) positively influence to use of fitness and health apps (F&HA)
Hypothesis 2 (H2): COVID-19 preventive measures (CPM) positively impact the use of live streaming workout classes (LSWC)
Hypothesis 3 (H3): COVID-19 preventive measures (CPM) positively influence the use of virtual reality fitness (VRF)
Mobile applications are a promising tool for increasing at-home adherence to physical exercise because they allow people to access health information and guidance at any time. In the fields of Educational techniques and physical health, information and communication technology are widely utilized. Technology-based therapies that encourage physical activity are a viable alternative to traditional health care.25 As the internet and mobile phones have advanced in recent years, physical activity has increased due to mobile phone fitness apps.26 In China, such as Gu Dong, KEEP, and Yue Dongguan, mobile fitness apps assist people in physical activity participation. Fitness and running apps are the two types of physical activity apps. Physical activity applications are not well-represented in health behavior change theories and evidence-based content.27 On the one hand, several emerging technologies (for example, sedentary video games) have aided in the epidemic of sluggish behavior and physical lack of activity. On the other hand, various revolutionary technologies are increasingly being employed to promote physical exercise and wellness.28,29 Our study hypotheses related to mobile applications and online platforms for physical activity are;
Hypothesis (H4): Demographic information (DI) has a significant favorable influence on the used fitness and health apps (F&HA)
Hypothesis 5 (H5): Demographic information (DI) has a significant-good effect on using the live streaming workout classes (LSWC)
Hypothesis 6 (H6): Demographic information (DI) has a significant positive influence on the use the virtual reality fitness (VRF)
E-health (or telemedicine) is a novel concept that takes advantage of the ubiquitous availability of mobile phones to ensure effective communication between patients and healthcare organizations, provide medical services, and encourage healthy habits.21 According to the World Health Organization’s global evaluation, mobile technologies are employed in several ways in health communication. These innovations are used to enhance (1) communication between individuals and health providers (eg, medical helplines or contact Centers); (2) interaction between healthcare personnel and clients (eg, Text message alerts for consultations, treatment adherence, or details to make people aware); (3) mobile medical counseling; and (4) interaction between many health care’s services in an emergency.21 Apps allow users to set fitness goals, log their actions, get workout ideas, and share their achievements on social media. Users of fitness apps desire features like a user-friendly interface, automatic tracking, and security.22 Our study hypotheses related to mobile applications and online platforms for physical activity are;
Hypothesis 7 (H7): During the COVID-19 preventive measures, the usage of fitness and health applications (F&HA) has a beneficial impact on physical activity (PA).
Hypothesis 8 (H8): During the COVID-19 preventive measures, the utilization of live streaming exercise classes (LSWC) has a positive impact on physical activity (PA).
Hypothesis 9 (H9): During the COVID-19 preventive measures, the usage of virtual reality fitness (VRF) has a positive impact on physical activity (PA).
Materials and Methods
The present study is based upon a nationwide survey in China. The survey was conducted online from March 10 to December 20, 2020. The survey participants were told of the study’s goal, and informed consent was obtained before conducting the study. It was guaranteed that the information gathered would only be utilized for research motives. The ethical committee of Soochow University approved the study and followed the Helsinki World Medical Declaration standards.
Sampling and Study Participants
The study population consisted of Chinese residents who utilized E-health apps for physical activity and health wellbeing during the epidemic. Study participants were recruited through snowball sampling technique under nonprobability sampling method. According to the study objectives, 5550 individuals were recruited to acquire primary data.
Questionnaire Survey
The primary data was gathered via a well-designed questionnaire. The questionnaire was validated on 75 individuals across China before conducting the final survey. After validation, certain questions were changed to achieve the optimum response rate. The accessibility to respondents was opened due to social applications such as (Social apps). The final questionnaire was included a total of 29 items (5-points Likert Scale) were related to 6 constructs (Demographic Information; DI, COVID-19 preventive measures; CPM, fitness and health apps; FHA, live streaming workout classes; LSWC, physical activity; PA, and virtual reality fitness; VRF). An online questionnaire was sent to all recruited study participants, and 5351 respondents returned the questionnaire after completion (See Table 1). Among the 5000 participants, men and women were 2454 (49.1%) and 2546 (50.9%), respectively.
 |
Table 1 Questionnaire Distribution |
Study Constructs Operationalization
- Demographic profile information played a vital role in the understanding of the social phenomena’s.30 Demographic variables were based upon the demographic profile information (DPI) of the survey participants, which includes gender (male, female); age (18–19, 20–29, 30–39, 40–49, 50–59, 60+); education (primary school, middle School, high school, technical and vocational college, graduate, university graduate, others); occupation (government employee, private employee, self-employed, retired, student, no occupation, others); and marital status (married, unmarried, others).
- The COVID-19 preventive measures include wearing masks, washing hands, quarantine, monitoring health, washing hands, maintaining social distance, and avoiding crowded places introduced by the WHO after the COVID-19 declared pandemic.31 In the current study, the COVID-19 preventive measures were mapped by asking the Likert scale questions related to the preventive measures which the study participants adopted during the early days of the pandemic. The questions were about staying at home, social distancing, wearing a face mask, social distancing, carrying out self-declaration, personal hygiene, staying physically active at home, avoiding public gatherings, and quarantine. These simple preventive measures play a significantly important role in preventing the COVID-19 pandemic.32
- Technology has become part and parcel of every segment of life. E-health technologies are very effective for motivation and promotion of the physical activity. Individuals can use technology to track, analyze, and instruct their physical activity performance.33 The study participant’s opinions were measured by asking questions about fitness and health apps, live streaming workout classes, and virtual reality fitness. The global smartphone fitness application industry is rapidly expanding. Consumers and providers of mental health care can benefit from new smartphone technology apps that offer a variety of capabilities and benefits. Diet, exercise, weight loss, nutritional benefits, and vegetarian options are just a few of the topics covered by these apps.34
- According to the WHO, adults should get at 150 minutes of average workout, 4 hours of intense workout, or even an extensive list of average moderate to vigorous strength physical activity each week; youth aged 5 to 17 years should get at least 60 minutes of workout daily. Adults should undertake muscular exercises (MSEs) at least twice per week, while teens should do them 2–3 times a week.35 The physical activity of the study participants was assessed by asking questions related to the use of digital platforms for exercise during the lockdown period; the use of fitness and health apps for physical activity is helpful to have an excellent motivation for physical activity because of using fitness apps, virtual reality fitness, and live streaming workout classes, during the lockdown period, your physical activity level increase by using fitness and health apps and fitness apps, virtual reality fitness, and live streaming workout classes help you to achieve the fitness goal.36
Statistical Analysis
After quantification and quality check of the data, a total of 5000 respondents’ responses were added in the final analysis. The demographic data were presented using SPSS-25 statistical software, which was also used to clean and prepare the data for testing all assumptions. The proposed research framework was examined using the structural equation modeling (SEM) approach for this work, and the SEM approach was employed through SmartPLS 3.0 software. SEM technique using partial least squares (PLS) was chosen in preferences for constructs and indicators.37 The SEM technique is used to measure the model assessment through convergent and discriminant validity and calculate average variance extracted values for each construct using factor loadings. Therefore, it is a multivariate analysis method to analyze the multiple relationships between variables of the conceptual model.
Results
Univariate Analysis
The demographic characteristics of the study sample are shown in Table 2. Age distribution shows that 2140 (42.8%) to 20–29, 1241 (24.82%) to 30–39, 533 (10.66%) to 18–19, 506 (10.12%) to 40–49, 424 (8.48%) to 50–59 and 156 (3.12%) to 60+ were belonged. The Educational context shows that University graduate (30.4%), technical and vocational College graduate (26.46%), high school (23.78%), middle school (9.48%), primary school (4.92%), and others (4.96%) were study participants. Occupation statistics reveal that private employee (41.08%), students (20.12%), self-employed (17.48%), government employee (12.28%), other (7.3%), no occupation (0.96%) and were retired (0.78%). The majority of the study participants were married (62.72%), unmarried (34.94%), and others were (2.34%) according to their marital status statistics.
 |
Table 2 Survey Participant’s Demographic Information (N-5000) |
Conceptual Measurement of the Study Model
Cronbach alpha values were used to assess the reliability of the online survey’s included components and items. The Cronbach alpha values were 0.938, 0.775, 0.938, 0.926, 0.928, and 0.935, respectively. (See Table 3 for further information). The standardized value of Cronbach alpha for assessing reliability is more than 0.70.38 The Cronbach alpha of each factor is declared reliable according to the standard. Discriminant and convergent validity of the study model was determined by using confirmatory factor analysis. The multitrait-multimethod matrix was used to analyze convergent techniques. It is the foundation for construct validity. The standard range value of composite reliability is more than 0.70. And 0.948, 0.848, 0.956, 0.948, 0.949, and 0.954 were calculated as the composite reliability values for each construct. In this study, factor loading values were consistently higher than the 0.60 criteria. The average variance extracted has a standard range of 0.50. This work’s average variance extracted values are 0.697, 0.531, 0.844, 0.819, 0.823, and 0.837. All of the average variances extracted values are greater than the typical range. Discriminant validity was utilized to assess and define constructs that were not theoretically connected.
 |
Table 3 Display the Convergent Validity Measurement of the Study Model (N-5000) |
In addition, the evidence of all measures concerning dissimilarity of all factors is also provided through discriminant validation. Discriminant validity necessitates a statistical test of components that are not significantly linked to other factors when calculating the correspondence of measures. DV can be calculated by relating a factor’s Square Root of AVE values with the correlation between constructs. The square root of AVE values should be less significant than correlations. All square roots of AVEs are higher than correlation coefficients in the DV analysis (see Table 4), indicating a good evaluation. The variation influence factor (VIF) value was also used to analyze the multicollinearity of all elements. VIF must be less than 10, and a value of 5 is regarded well. VIF values of less than 5 were found in all formative constructs in this research, showing that multicollinearity was not an impediment.
 |
Table 4 Display Discriminant Validity Analysis (N-5000) |
Multivariate Analysis
Structural Equation Model
The current study used the structural equation modeling approach to examine all proposed hypotheses using the smart-PLS 3.3.0 package. The standardized-root-mean-square-residual, chi-square, and normed fit indices were used for this study’s model fitness. Model fitness is determined using the SRMR value, a standardized-residuals index by comparing observed covariance and hypothesized matrices. A range of standardized root-mean-square-residual values of 0.08 or less can be utilized. The estimated standardized root-mean-square-residual value is 0.036 due to the findings, which is considered a satisfactory model fit. As indicated in (Table 5), the normed fit indices value is 0.951, and the chi-square value is 5578.217.
 |
Table 5 Model Fit Summary (N-5000) |
The standard beta was used to calculate the significance level of the hypotheses provided. The standardized beta (β) value shows how different factors may differ from each other. Each β value was calculated using the projected research framework (see Table 6). If the β values are large and significant, the principal effects of endogenous latent variables will be considered highly valued.
 |
Table 6 Final Results for Standard Beta, T-Statistics, and P-values (N-5000) |
The relevance of the beta value for each path was also confirmed using the T-statistics approach. To acquire the β value, the bootstrapping technique was utilized to assess and evaluate the significance degree of postulated associations—Table 6 and Figure 1 show this work’s proposed structural model relationships and β statistics. The link between smartPLS-bootstrapping T-values and observed variables is shown in Figure 2. COVID-19 preventive measures have a strong favorable influence on health and fitness apps, according to the statistics for H1 (β = 0.227, t = 18.725, p = < 0.000). H2 (β = 0.225, t = 17.892, p = < 0.000) statistically shows that on live streaming workout classes positively impacted by CPM.
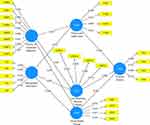 |
Figure 1 SmartPLS SEM results. |
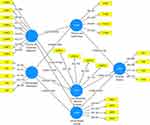 |
Figure 2 PLS-bootstrapping T-values. |
The results for H3 (β = 0.229, t = 17.845, p = < 0.000) statistically positions positive association between COVID-19 preventive measures and virtual reality fitness. Similarly H4 (β = 0.54, t = 60.928, p = < 0.000) results narrates the positive relationship between demographic information’s and fitness and health apps. H5 results (β = 0.553, t = 57.291, p = < 0.000) absolutely defines that the demographic information has a significant positive impact on live streaming workout classes. H6 statistics (β = 0.559, t = 56.956, p = < 0.000) show a positive association between demographic information and virtual reality fitness. Fitness & health related apps positively influence the physical activity according to the H7 (β = 0.358, t = 24.779, p = < 0.000) statistics. The statistics (β = 0.259, t = 19.617, p = < 0.000) confirmed the H8 and state that live streaming workout classes reveal a significant positive impact on physical activity. Similarly, H9 (β = 0.288, t = 19.92, p = < 0.000) proved positive correlation between virtual reality fitness and physical activity.
Discussion
According to our insights, it’s the first exploratory study to explore E-health applications’ role in physical activity and fitness among the Chinese people during the epidemic. Digital technologies have significantly impacted social life, sports, and health practices throughout the last decade. Apps and wearable’s track and compare physical activity, allowing users to track themselves and connect them to online networks.8 Physical inactivity is a potential risk during the COVID-19 due to the closure of public spaces for exercise and sports.39
COVID-19 and E-Health Apps
There seems to be no evidence on how prior users used e-Health for exercise and physical activity while in confinement during the pandemic and its effects on their motives and processes for behavioral change in terms of actual physical performance.40 Our results depicted that the COVID-19 preventive measures (CPM) positively influence the use of E-health apps. Online platforms promote health and fitness information while also emphasizing lifestyle sports and fitness trends. Likewise, internet fitness clubs and influencers allow their members to exercise virtually anywhere at any time.41 E-health apps using trends increased during the COVID-19 pandemic across the globe. Our study results align with several studies that reported that E-health apps provide health surveillance and maintenance information and keep the users up to date regarding the COVID-19 exposure and recommend the COVID-19 preventive measures such as physical activity social distancing.42–44 Study participants use E-health apps because of CPM. Public parks, gymnasiums, and other publicly accessible venues were closed. Many regular fitness studios and sports users adopt home-based, individualized, and most likely digital sports alternatives. People should be active throughout the pandemic by using digital tools for home-based physical activity.45 Digital health (DH) apps play a significant role in combating COVID-19 and providing information remotely to maintain people’s active living.46 A study was conducted in China’s Hubei province regarding the COVID-19 pandemic and the use of E-health. The study results show that 79.52% used E-health apps to avoid going out and minimize the risk of the COVID-19 infection.47 China’s health code is a unique E-health app used for contact tracing and monitoring under the instructions of the state council’s joint prevention and control mechanism (JPCMSC).48
The Demographic Profile Information (DPI) and E-Health Apps
Many types of research have explored the relationship between health app use, demographics, and prevalence of active living. For example, a US study reported that about (58%) Hispanics/Latinos with higher education and income downloaded a health app for health wellbeing.49 Our study results show that the demographic profile information of the study participants has significant positive impacts on fitness and health apps, live streaming workout classes, and virtual reality fitness. The correlation among the study variables is in line with various previous studies which focused on demographic association with the E-health apps impact on health well-being.50 Applications delivering healthier lifestyle advice, curative and rehabilitative content, and apps measuring/recording vital signs were more likely to be used by higher social classes.51 E-health apps (fitness and health combined apps) acceptance behavior is associated with urban residence, education, higher income, and age.52 The majority of the study participants agreed that E-health apps effectively reduce physical inactivity and improve health outcomes during the COVID-19 preventive measures. Health and fitness apps intervention significantly impacts health-related quality of life (HRQOL).53,54 China’s robust telecommunication infrastructure plays a vital role in national healthcare reform initiatives like government-sponsored Internet hospitals and eHealth interventions.55 A significant digital divide related to E-health behaviors among the Chinese residents is predicted based on socio-economic status.56 According to the findings of our study, the majority of the females used digital platforms for active living during the epidemic. Similar results are reported in a study conducted in China that female users are more likely to use health and medical reminder applications. Parenting could be a reason why women utilized health apps more than men, in addition to gender disparities in views toward healthy living.50 According to the study statistics, health disparities and digital health divide are projected by residence, ethnicity, age, education, and income. Previous research has focused on overall health app use rather than the demographic correlates of each type of health app (eg, healthy living information, diagnosis assistance, health, and medical reminders). The socio-economic status enables an individual to attain mobile technologies for a healthy lifestyle.57
E-Health Apps and Physical Activity
E-health treatments are becoming more common in public health. Virtual reality is one of the most interesting new advances in the medical paradigm.58 Many studies have shown that fitness technology can effectively engage inactive people in workout programs. According to a systematic review (web-based technology, mobile phones, and accelerometers), several investigations that used mixed technology-based physical activity interventions had good outcomes in sedentary people, including weight loss and decreased health risk behavior (according to a systematic review (web-based technology, mobile phones, and accelerometers)).59
Wearable technology firms like Garmin’s data also give a fascinating picture of the types of physical activities people engage in during these times. On the other hand, this data is from people who use wearable technology like smartwatches and fitness trackers, rather than being representative or cross-sectional. It’s worth noting that throughout the month of March 2020, there was a global decrease in the daily average number of steps taken, indicating that people’s movements were restricted. In March, virtual cycling grew in the nations of Italy and Spain during the tight lockdown regulations. In other nations where outdoor exercise is permitted, such as the United Kingdom and Sweden, there has been a significant increase in outdoor cycling activities compared to the same period in 2019.60 Our research confirmed that health and fitness applications positively affect physical exercise. Active lifestyle through physical activity prevents various non-communicable diseases. Obesity, dyslipidemia, and metabolic syndrome are only a few cardiovascular risk factors that can be reduced by regular physical activity.61 Another study found that pedometer users reported about a (27%) increase in physical activity levels. Walking programs using pedometers were also linked to significant reductions in BMI, body weight, and systolic blood pressure.62 Knowing that exercise can help with health recovery and protect COVID-19, it’s critical to stick to the physical activity guidelines for middle-aged adults, which include moderate-intensity aerobic activity, cardiorespiratory exercise, and two sessions of muscle strength work each week.63 During the COVID-19 lockdown period, most study participants used the KEEP app for physical activity. With over 10 million subscribers, KEEP is one of China’s most popular fitness apps.64 E-health physical activity-related apps (e-tools) positively impact the quality of life (QOL) during the social isolation period.65 The trend of using health and fitness apps during the early CPM was increased due to health consciousness. Several studies confirmed our results that physical activity levels increase due to E-health and fitness apps during the COVID-19 pandemic.66
Conclusion
The current study demonstrates the relevance and importance of digital platforms for physical activity during the epidemic. Digital technology has created a revolution in the health sector and changed the health monitoring and maintenance trend. E-health apps are gaining popularity among people because of health consciousness. The statistics of our study reveal that the E-health apps were widely used for fitness and health wellbeing during the COVID-19 home confinement. Health consciousness leads people to use various. E-health platforms such as health and fitness apps, live streaming workout classes, and virtual reality fitness (VRF) for physical activity during the epidemic home confinement. E-health assists in promoting physical activity and maintaining wellbeing during any critical situation. E-health apps positively modify their users’ behavior and attitude towards physical activity. Chinese urban residents are utilizing mobile fitness apps in their everyday exercise routine. E-health platforms such as health and fitness apps live streaming workout classes and VRF for physical activity during the epidemic home confinement. E-health assists in promoting physical activity and maintaining wellbeing during any critical situation. Physical inactivity level was increased in the early days of the pandemic due to the closure of public places for physical activity. Chinese urban residents are utilizing mobile fitness apps in their everyday exercise routine.
Limitations of the Study
The population for the current study was Chinese residents (+18 years old) across China who was in home isolation during the first wave of the pandemic in China and used digital platforms for physical activity (DPPA). The snowball sampling approach was used for data collecting under the non-probability sampling (NPS) strategy. A self-administered survey was used to collect the primary data, and the snowball sampling results cannot be generalized to the whole population. Cross-sectional studies mostly fail to specify a definite reason behind a correlation. This restriction might avoid a deep understanding of the essence of the causal relationship between study variables.
Future Scope of the Study
The Chinese government has launched the “Internet plus Exercise” program for active life and wellbeing. In addition, psychologically, three cognitive factors may be involved in an activity: (i) beliefs about the activity, (ii) motivation for the activity, and (iii) the sense of reward obtained from the activity. Our study focus is on the use of digital platforms for physical activity. A more interesting future study can be conducted on the influence of the Chinese government policy “Internet plus Exercise” in using digital platforms for physical activity and the relationship of digital platforms with those mentioned above three cognitive factors related to physical activity under the psychological paradigm.
Acknowledgments
We thank the participants for participating in this research and making this study possible. Rashid Menhas is the Principal investigator.
Funding
The current study belongs to the following given projects; The Key Project of Philosophy and Social Science Research in Colleges in Jiangsu Province study on comprehensive prevention and control of adolescent myopia based on multiple management (2020SJZDA128). The National Social Science Funds of China research on the intervention mechanism of sports promoting adolescent physical health outside school from the perspective of national social Science evidence-based governance (21BTY024).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Atalan A. Is the lockdown important to prevent the COVID-19 pandemic? effects on psychology, environment and economy-perspective. Ann Med Surg. 2020;56:38–42. doi:10.1016/j.amsu.2020.06.010
2. Fifield A, Sun LH. Travel ban goes into effect in Chinese city of Wuhan as authorities try to stop coronavirus spread. The Washington Post; 2020. Available from: https://www.washingtonpost.com/world/asia_pacific/nine-dead-as-chinese-coronavirus-spreads-despite-efforts-to-containit/2020/01/22/1eaade72-3c6d-11ea-afe2-090eb37b60b1_story.html.
3. O’Donovan G, Lee I-M, Hamer M, Stamatakis E. Association of “Weekend warrior” and other leisure time physical activity patterns with risks for all-cause, cardiovascular disease, and cancer mortality. JAMA Intern Med. 2017;177(3):335. doi:10.1001/jamainternmed.2016.8014
4. Gao Z, Lee AM, Solmon MA, et al. Validating pedometer-based physical activity time against accelerometer in middle school physical education. ICHPER. 2010;5(1):20–25.
5. Bort-Roig J, Gilson ND, Puig-Ribera A, Contreras RS, Trost SG. Measuring and influencing physical activity with smartphone technology: a systematic review. Sports Med. 2014;44(5):671–686. doi:10.1007/s40279-014-0142-5
6. Pope Z, Gao Z. Global positioning systems and geographic information systems and physical activity. In: Technology in Physical Activity and Health Promotion. Routledge; 2017:129–147. doi:10.4324/9781315526171-7
7. Deci EL, Ryan RM. The “what” and “why” of goal pursuits: human needs and the self-determination of behavior. Psychol Inq. 2000;11(4):227–268. doi:10.1207/s15327965pli1104_01
8. Ng JY, Ntoumanis N, Thøgersen-Ntoumani C, et al. Self-determination theory applied to health contexts. Perspect Psychol Sci. 2012;7(4):325–340. doi:10.1177/1745691612447309
9. Li K, Iannotti RJ, Haynie DL, Perlus JG, Simons-Morton BG. Motivation and planning as mediators of the relation between social support and physical activity among U.S. adolescents: a nationally representative study. IntJ Behav Nutr Physical Activity. 2014;11(1):42. doi:10.1186/1479-5868-11-42
10. Nurmi J, Hagger MS, Haukkala A, Araújo-Soares V, Hankonen N. Relations between autonomous motivation and leisure-time physical activity participation: the mediating role of self-regulation techniques. J Sport Exerc Psychol. 2016;38(2):128–137. doi:10.1123/jsep.2015-0222
11. Beck AT. Depression: Clinical, Experimental, and Theoretical Aspects. London: Staples Press; 1969.
12. Diamond R, Waite F. Physical activity in a pandemic: a new treatment target for psychological therapy. Psychol Psychother. 2020;94(2):357–364. doi:10.1111/papt.12294
13. Ajzen I. Perceived behavioral control, self-efficacy, locus of control, and the theory of planned behavior. J Appl Soc Psychol. 2002;32(4):665–683. doi:10.1111/j.1559-1816.2002.tb00236.x
14. Rhodes RE, Courneya KS, Jones LW. Translating exercise intentions into behavior: personality and social cognitive correlates. J Health Psychol. 2003;8(4):447–458. doi:10.1177/13591053030084004
15. Shephard RJ, Bouchard C. Population Evaluations of health related fitness from perceptions of physical activity and fitness. Can J Appl Physiol. 1994;19(2):151–173. doi:10.1139/h94-012
16. De Oliveira Neto L, Elsangedy HM, Tavares VD, et al. #traininginhome - home-based training during COVID-19 (SARS-COV2) pandemic: physical exercise and behavior-based approach. Revista Brasileira de Fisiologia do Exercício. 2020;19(2):9. doi:10.33233/rbfe.v19i2.4006
17. Rogers RW. A protection motivation theory of fear appeals and attitude change. J Psychol. 1975;91(1):93–114. doi:10.1080/00223980.1975.9915803
18. Rogers RW. Cognitive and psychological processes in fear appeals and attitude change: a revised theory of protection motivation. In: Social Psychophysiology: A Sourcebook. Guilford Press; 1983:153–176.
19. Milne S, Sheeran P, Orbell S. Prediction and intervention in health-related behavior: a meta-analytic review of protection motivation theory. J Appl Soc Psychol. 2000;30(1):106–143. doi:10.1111/j.1559-1816.2000.tb02308.x
20. Maddux JE. Social cognitive models of health and exercise behavior: an introduction and review of conceptual issues. J Appl Sport Psychol. 1993;5(2):116–140. doi:10.1080/10413209308411310
21. Füzéki E, Groneberg DA, Banzer W. Physical activity during COVID-19 induced lockdown: recommendations. J Occup Med Toxicol. 2020;15(1). doi:10.1186/s12995-020-00278-9
22. Mehta P, McAuley DF, Brown M, Sanchez E, Tattersall RS, Manson JJ. Covid-19: consider cytokine storm syndromes and immunosuppression. Lancet. 2020;395(10229):1033–1034. doi:10.1016/s0140-6736(20)30628-0
23. Pedersen BK, Saltin B. Exercise as medicine - evidence for prescribing exercise as therapy in 26 different chronic diseases. Scand J Med Sci Sports. 2015;25:1–72. doi:10.1111/sms.12581
24. Abbas AH. Politicizing the pandemic: a schemata analysis of COVID-19 news in two selected newspapers. Int J Semiotics Law. 2020. doi:10.1007/s11196-020-09745-2
25. Hakala S, Rintala A, Immonen J, Karvanen J, Heinonen A, Sjögren T. Effectiveness of technology-based distance interventions promoting physical activity: systematic review, meta-analysis and meta-regression. J Rehabil Med. 2017;49(2):97–105. doi:10.2340/16501977-2195
26. Middelweerd A, Mollee JS, van der Wal CN, Brug J, te Velde SJ. Apps to promote physical activity among adults: a review and content analysis. IntJ Behav Nutr Physical Activity. 2014;11(1). doi:10.1186/s12966-014-0097-9
27. Knight E, Stuckey MI, Prapavessis H, Petrella RJ. Public health guidelines for physical activity: is there an app for that? A review of android and apple app stores. JMIR mHealth uHealth. 2015;3(2):e43. doi:10.2196/mhealth.4003
28. Kay M, Santos J, Takane M. mHealth: new horizons for health through mobile technologies: based on the findings of the second global survey on eHealth; 2011. Available from: https://www.who.int/goe/publications/goe_mhealth_web.pdf.
29. Dennison L, Morrison L, Conway G, Yardley L. Opportunities and challenges for smartphone applications in supporting health behavior change: qualitative study. J Med Internet Res. 2013;15(4):e86. doi:10.2196/jmir.2583
30. Smelser NJ, Baltes PB. Preface. Int Encyclopedia Soc Behav Sci. 2001;xxvii–xxix. doi:10.1016/b0-08-043076-7/04687-8
31. Brown A, Horton R. A planetary health perspective on covid-19: a call for papers. Lancet. 2020;395(10230):1099. doi:10.1016/s0140-6736(20)30742-x
32. Chu DK, Duda S, Solo K, Yaacoub S, Schunemann H. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-COV-2 and COVID-19: a systematic review and meta-analysis. J Vasc Surg. 2020;72(4):1500. doi:10.1016/j.jvs.2020.07.040
33. Jiménez-Pavón D, Carbonell-Baeza A, Lavie CJ. Physical exercise as therapy to fight against the mental and physical consequences of covid-19 quarantine: special focus in older people. Prog Cardiovasc Dis. 2020;63(3):386–388. doi:10.1016/j.pcad.2020.03.009
34. Luxton DD, McCann RA, Bush NE, Mishkind MC, Reger GM. MHealth for mental health: integrating smartphone technology in behavioral healthcare. Prof Psychol Res Pr. 2011;42(6):505–512. doi:10.1037/a0024485
35. WHO. Global recommendations on physical activity for health. Available from: https://www.who.int/publications-detail-redirect/9789241599979.
36. Yang J, Menhas R, Dai J, et al. Virtual Reality Fitness (VRF) for behavior management during the COVID-19 pandemic: a mediation analysis approach. Psychol Res Behav Manag. 2022;15:171–182. doi:10.2147/PRBM.S350666
37. Urbach N, Ahlemann F. Structural equation modeling in information systems research using partial least squares. J Info Technol Theory Appl. 2010;11(2):5–40.
38. Nunnally JC. Psychometric Theory 3E. Tata McGraw-Hill Education; 1994.
39. Jakobsson J, Malm C, Furberg M, Ekelund U, Svensson M. Physical activity during the coronavirus (COVID-19) pandemic: prevention of a decline in metabolic and immunological functions. Front Sports Active Living. 2020;2. doi:10.3389/fspor.2020.00057
40. Marchant G, Bonaiuto F, Bonaiuto M, Guillet Descas E. Exercise and physical activity eHealth in COVID-19 pandemic: a cross-sectional study of effects on motivations, behavior change mechanisms, and behavior. Front Psychol. 2021;12. doi:10.3389/fpsyg.2021.618362
41. Jong ST, Drummond MJ. Exploring online fitness culture and young females. Leisure Stud. 2016;35(6):758–770. doi:10.1080/02614367.2016.1182202
42. Almalki M, Giannicchi A. Health apps for combating covid-19: descriptive review and taxonomy. JMIR mHealth uHealth. 2021;9(3):e24322. doi:10.2196/24322
43. Chen M, Xu S, Husain L, Galea G. Digital health interventions for COVID-19 in China: a retrospective analysis. Intel Med. 2021;1(1):29–36. doi:10.1016/j.imed.2021.03.001
44. Gios L, Crema Falceri G, Micocci S, et al. Use of eHealth platforms and apps to support monitoring and management of home-quarantined patients with covid-19 in the province of Trento, Italy: app development and implementation (preprint). JMIR Formative Res. 2021;5(5):e25713. doi:10.2196/preprints.25713
45. Nyenhuis SM, Greiwe J, Zeiger JS, Nanda A, Cooke A. Exercise and fitness in the age of social distancing during the COVID-19 pandemic. J Allergy Clin Immunol. 2020;8(7):2152–2155. doi:10.1016/j.jaip.2020.04.039
46. Bui LV, Ha ST, Nguyen HN, et al. The contribution of digital health in the response to covid-19 in Vietnam. Front Public Health. 2021;9. doi:10.3389/fpubh.2021.672732
47. Wang W, Sun L, Liu T, Lai T. The use of E-health during the COVID-19 pandemic: a case study in China’s Hubei province. Health Sociol Rev. 2021;1–17. doi:10.1080/14461242.2021.1941184
48. Cong W. From pandemic control to data-driven governance: the case of China’s health code. Front Political Sci. 2021;3. doi:10.3389/fpos.2021.627959
49. Krebs P, Duncan DT. Health app use among US mobile phone owners: a national survey. JMIR mHealth uHealth. 2015;3(4):e101. doi:10.2196/mhealth.4924
50. Xie Z, Nacioglu A, Or C. Prevalence, demographic correlates, and perceived impacts of mobile health app use amongst Chinese adults: cross-sectional survey study. JMIR mHealth uHealth. 2018;6(4):e103. doi:10.2196/mhealth.9002
51. Wardle J. Socioeconomic differences in attitudes and beliefs about healthy lifestyles. J Epidemiol Community Health. 2003;57(6):440–443. doi:10.1136/jech.57.6.440
52. Hong YA, Zhou Z. A profile of eHealth behaviors in China: results from a national survey show a low of usage and significant digital divide. Front Public Health. 2018;6. doi:10.3389/fpubh.2018.00274
53. Anderson K, Burford O, Emmerton L. Mobile health apps to facilitate self-care: a qualitative study of user experiences. PLoS One. 2016;11(5):e0156164. doi:10.1371/journal.pone.0156164
54. Zhao J, Freeman B, Li M. Can mobile phone apps influence people’s health behavior change? An evidence review. J Med Internet Res. 2016;18(11):e287. doi:10.2196/jmir.5692
55. Tian M, Zhang J, Luo R, et al. MHealth interventions for health system strengthening in China: a systematic review. JMIR mHealth uHealth. 2017;5(3):e32. doi:10.2196/mhealth.6889
56. Hong YA, Zhou Z, Fang Y, Shi L. The digital divide and health disparities in China: evidence from a National Survey and Policy Implications. J Med Internet Res. 2017;19(9):e317. doi:10.2196/jmir.7786
57. Viswanath K, Kreuter MW. Health disparities, communication inequalities, and eHealth. Am J Prev Med. 2007;32(5):S131–S133. doi:10.1016/j.amepre.2007.02.012
58. Jerdan SW, Grindle M, van Woerden HC, Kamel Boulos MN. Head-mounted virtual reality and mental health: critical review of current research. JMIR Serious Games. 2018;6(3):e14. doi:10.2196/games.9226
59. Hassett L, van den Berg M, Lindley RI, et al. Effect of affordable technology on physical activity levels and mobility outcomes in rehabilitation: a protocol for the activity and mobility using technology (amount) rehabilitation trial. BMJ Open. 2016;6(6):e012074. doi:10.1136/bmjopen-2016-012074
60. Stables J. Garmin data reveals how the world is working out during the lockdown; 2020. Available from: https://www.wareable.com/garmin/garmin-data-lockdown-7940.
61. Agarwal S. Cardiovascular benefits of exercise. Int J Gen Med. 2012;541. doi:10.2147/ijgm.s30113
62. Bravata DM, Smith-Spangler C, Sundaram V, et al. Using pedometers to increase physical activity and improve health. JAMA. 2007;298(19):2296. doi:10.1001/jama.298.19.2296
63. Dominski FH, Brandt R. Do the benefits of exercise in indoor and outdoor environments during the COVID-19 pandemic outweigh the risks of infection? Sport Sci Health. 2020;16(3):583–588. doi:10.1007/s11332-020-00673-z
64. Chen H. Smart health facilitator: Chinese consumers’ perceptions and interpretations of fitness mobile apps. Mobile Commun Asia. 2017;109–122. doi:10.1007/978-94-024-1251-2_7
65. Barreto FS, Carvalho GO, Silva LC, et al. Electronic tools for physical activity and quality of life of medical students during COVID-19 pandemic social isolation. Motriz. 2021;27. doi:10.1590/s1980-65742021002121
66. Romeo A, Edney S, Plotnikoff R, et al. Can smartphone apps increase physical activity? Systematic Review and meta-analysis. J Med Internet Res. 2019;21(3):e12053. doi:10.2196/12053
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
