Back to Journals » Clinical Optometry » Volume 10
Demodex blepharitis: clinical perspectives
Authors Fromstein SR, Harthan JS , Patel J , Opitz DL
Received 30 January 2018
Accepted for publication 17 April 2018
Published 4 July 2018 Volume 2018:10 Pages 57—63
DOI https://doi.org/10.2147/OPTO.S142708
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Mr Simon Berry
Stephanie R Fromstein, Jennifer S Harthan, Jaymeni Patel, Dominick L Opitz
Department of Clinical Education, Illinois College of Optometry, Chicago, IL, USA
Abstract: Demodex folliculorum and Demodex brevis are two mites which infest the human eye and which may, in excess, lead to a wide range of anterior segment findings. Demodex mites have been implicated in anterior and posterior blepharitis, blepharoconjunctivitis, blepharokeratitis, and beyond. Due to significant overlap with other anterior segment conditions, Demodex infestation remains underdiagnosed and undertreated. Definitive diagnosis can be made with lash sampling, and the most common mode of treatment is with tea tree oil in varying concentrations. This article summarizes elements of pathogenesis, diagnosis, and management critical to clinical care of this common condition.
Keywords: Demodex folliculorum, Demodex brevis, blepharitis, blepharoconjunctivitis, meibomian gland dysfunction, ocular rosacea
A Letter to the Editor has been received and published for this article.
Introduction
The Demodex mite – of phylum Arthropoda – comes in two forms, Demodex folliculorum and Demodex brevis.1,2 D. folliculorum is larger (0.3–0.4 mm) and tends to inhabit the base of the lashes, as the name would suggest. D. brevis is smaller (0.2–0.3 mm), and preferentially inhabits the sebaceous glands.3 These are the only two mites that affect the human eye, and in turn humans are the only mammals to host them.4 Both mites in their adult form are cigar-shaped with four pairs of legs to grip cylindrical structures such as an eyelash.2,5 The mites take approximately 2 weeks to mature from the egg to the larval stage, with an overall life span of up to 3 weeks.3
How these mites spend this life span – and specifically whether these mites are benign or should be maligned – remains an area of dispute. That Demodex is a normal part of the lid flora is well established; in fact, these mites are the most common microscopic ectoparasite on the human skin.3 However, Demodex mites are found in both symptomatic and asymptomatic individuals, and there is poor correlation between Demodex infestation and symptoms, as paralleled in other anterior segment conditions such as blepharitis.5,6
On the other hand, infestation by these mites – deemed demodicosis – has been implicated in a variety of anterior segment conditions, where literature suggests a correlation between Demodex mites and blepharitis, changes to the eyelashes (loss and misalignment), conjunctivitis, keratitis, and basal cell carcinoma of the lid, among others.4,7 To bridge these findings, it has been suggested that density and overpopulation may play a role in tipping the anterior segment ecosystem from homeostasis to disease.1–4,6–9 Authors postulate a role for Demodex in a balanced ocular ecology, acting as lash cleaners by grazing on bacteria, defending against other mite species, and as immune regulators and buffers.5 However, as these mites proliferate in the proverbial “hard-to-reach” places of the eyelid (surrounded by the nose, brow, and cheek) and density increases with age (100% of the general population over 70 years of age has been shown to have Demodex mites), so do the ocular complications.3,6 This uncertainty leads to underdiagnosis and undertreatment of Demodex infestations. Combined with its comorbidities and ability to masquerade as a number of other ocular conditions (most notably recalcitrant herpetic keratitis), Demodex should be a top differential in the diagnosis and management of anterior segment inflammation. This article summarizes the current understanding of the pathogenesis, diagnosis, comorbidities, and treatment options for Demodex to help the eye care practitioners better manage affected patients.
Pathogenesis
The Demodex duo can have multiple impacts on the anterior ocular surface, including anterior blepharitis, posterior blepharitis and meibomian gland dysfunction (MGD), ocular rosacea, and keratitis. The mechanisms of each species of Demodex are discussed below.
Demodex and anterior blepharitis
D. folliculorum finds its primary habitat at the base of the lash follicle, where it feeds on follicular and glandular epithelial cells, causing direct mechanical damage as it does so.3,8 These microscopic epithelial abrasions can cause epithelial hyperplasia and reactive hyperkeratinization.8,9 In addition to feeding, the mites lay their eggs at the base of the lashes resulting in follicular distention and misdirected lashes.10 As these mites have no excretory organs, undigested material is regurgitated and combines with these epithelial cells, keratin, and eggs to form the bulk of the cylindrical lash deposits pathognomonic of Demodex infestation.5,10 These deposits, in turn, contain proteases and lipases, which cause symptoms of irritation.5 In fact, of all ocular symptoms investigated, the only symptom to correlate directly with Demodex was lid irritation. Specifically, this irritation is caused both directly by biting of the mites and by lipolytic enzymes used to digest sebum, their main food source.2,3,5
In addition to contributing to surface irritation and inflammation through the above mechanisms, the mites may also activate inflammatory cascades through toxins on their surface and inside of the organisms. Streptococci and staphylococci on the surface of the mites are directly implicated in microbial blepharitis, both anterior and posterior.3 Additionally, bacteria harbored inside the mites (Bacillus oleronius) have also been shown to activate the host’s immune response.3,5 Even in their death, mites may elicit an inflammatory response by releasing a number of bacterial antigens that trigger the host’s inflammatory cascade.3
Finally, the debris released by mites is thought to cause a delayed hypersensitivity immune response – this is backed up by the fact that an increase in the number of CD4+ T cells, macrophages, and Langerhans cells was observed only in subjects with a positive D. folliculorum finding.3,5,11 Measuring these host inflammatory responses may be a valuable noninvasive test for Demodex.5
Demodex and posterior blepharitis
D. brevis has been linked to symptomatic MGD, in part due to its predisposition toward the meibomian gland where it causes a primary mechanical blockage of the orifice.8 Accordingly, severity of MGD has been found to correlate with demodicosis by D. brevis and not by D. folliculorum.12 Accumulation of parasite excreta further contributes to this blockage and may also elicit a cell-mediated reaction.2 This blockage leads to filling, swelling, and enlargement of the gland.
Additionally, the chitinous exoskeleton of the mite has been hypothesized to act as a foreign body, causing a localized granulomatous reaction.13 This granuloma may develop into a hordeolum or chalazion, which is suspected to be caused by a host response to a foreign body derived from several pathogens.4 This hypothesis is further borne out by the evidence that D. brevis mite has been observed at the center of meibomian granulomas such as chalazia and the overall high correlation between the prevalence of D. brevis and chalazia.3,10 In a recent study, D. brevis also tended to be more highly associated with recurrence of chalazia after surgical excision.4
Demodex and adjacent inflammation
Inflammation of the lid margin can spill over and cause inflammation of the conjunctiva, thus resulting in blepharoconjunctivitis whose treatment by other means – antibiotic, antiviral, or lubrication – seems to be ineffective.3 This appears to hold true not only for adults but for children as well, typically thought to be excluded from Demodex infection. In a study of 12 healthy pediatric patients, recalcitrant blepharoconjunctivitis which did not respond to traditional therapy resolved after a short course of tea tree oil.14 Staphylococcus epidermidis and Staphylococcus aureus are the main pathogens in pediatric blepharoconjunctivitis, and as has been mentioned, Demodex mites may be a vector for these bacteria in the eye.14
Kheirkhah et al were the first to report on Demodex-induced changes to the cornea.1 Inflammation from anterior and posterior blepharitis may impact the cornea, causing otherwise unexplained superficial punctate keratopathy, corneal neovascularization, stromal and marginal infiltration, phlyctenular lesions, superficial opacities, nodular scars, limbitis, and even perforation.1,4 Superficial punctate keratopathy was significantly more common in patients with known Demodex than in their matched controls.4 D. brevis is thought to be the main causative agent in Demodex keratitis as the D. brevis mite is closer to the cornea and more likely to cause corneal inflammation.1,3,7 In some cases of keratitis, findings can be so severe as to mimic herpes keratitis – in one study, all cases of demodicosis keratitis had been previously misdiagnosed as a viral infection but failed to respond to antiviral therapy.4 Importantly, mite sampling and response to therapy can be used to distinguish the two entities.4
Demodex and comorbidities
Demodex has been implicated not only in facial rosacea but also in cases of ocular rosacea.1 Inflammatory/immune reactions as well as the mites as vectors for bacteria (as in blepharitis) have been postulated as causes.1 Specifically, superantigens produced by streptococci and staphylococci bacteria – carried on the mites – have been implicated in the induction of rosacea.3 With this in mind, the correlation between Demodex and the severity of ocular rosacea has also been demonstrated.3 With regard to rosacea, comorbid factors that may change the flora environment and allow for mite proliferation include skin phototype, sunlight exposure, alcohol intake, smoking, stress, hot beverages, spicy food, and abrupt changes in temperature.3
Demodex infestation is not isolated to the eyelid margins, eyelashes, and meibomian glands. The dermatology literature suggests that Demodex may also be associated with a multitude of skin conditions as well as basal and sebaceous cell carcinoma.3,15–17 Although argument exists as to whether Demodex of the normal skin flora does or does not in part cause the development of inflammatory skin eruptions, there is evidence for demodicosis of papulopustular rosacea, granulomatous-like rosacea, and blepharitis especially when Demodex density exceeds a normal threshold.18–20 In cancer patients who were taking epidermal growth factor receptor inhibitors, it was reported that Demodex mite colonization was increased which increased the risk of dermatologic conditions such as annular facial eruptions. There were also reported cases of Demodex folliculitis mimicking acute cutaneous graft-versus-host disease (GVHD).21–26 Tissue samplings of the affected skin tissue confirmed the diagnosis of Demodex in the suspected GVHD patients. Once Demodex was diagnosed and treated in these GVHD patients, the skin lesions cleared.
Diagnosis
The clinical diagnosis of Demodex blepharitis is more commonly made based on signs rather than symptoms, as demodicosis symptoms cross over with a number of other anterior segment conditions, including anterior and posterior blepharitis, evaporative and non-evaporative dry eye, as well as other sources of ocular surface inflammation. Patients may complain of itching, burning, foreign body sensation, crusting or matted lashes, tearing, blurry vision, ocular discomfort or irritation, and crossover symptoms to myriad of other conditions.4,27 Demodex blepharitis should be suspected in cases of symptomatic patients who are nonresponsive to treatment of other anterior segment conditions; management of adjacent conditions will not be successful at stemming demodicosis and alleviating symptoms.7
D. folliculorum signs include cylindrical dandruff (CD) and eyelash disorders such as trichiasis, distichiasis, madarosis, and erythema of the eyelid margin.4,27 CD consists of fine, waxy, dry debris concentrated at the base of the lash and is considered pathognomonic of Demodex (Figures 1 and 2).4,7,27 CD indicates the presence of high-density Demodex mite infestation.
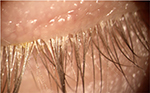  | Figure 1 Example of a patient with Demodex folliculorum. Note the cylindrical dandruff at the base of the eyelashes which are pathognomonic of demodicosis. |
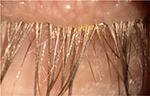  | Figure 2 Another example of a patient with demodicosis and cylindrical dandruff caused by Demodex folliculorum. |
The associated anterior segment findings may be extensive and should prompt suspicion of demodicosis. Lid margin inflammation stems from the aforementioned mechanical and hypersensitivity impacts of the Demodex mite. MGD may be exacerbated to the point of hordeola or chalazia, often chronic. Blepharoconjunctivitis and blepharokeratitis may also be noted, and speak to the wide-ranging impacts that the Demodex mites may have on the ocular surface. Non-resolving cases of blepharoconjunctivitis have been successfully resolved with the treatment of Demodex. Similarly, in cases of corneal changes, including neovascularization, infiltration, opacification, and scarring – especially those non-resolving on therapy – Demodex should be considered as a potential etiology.3
A definitive diagnosis of Demodex infestation is made by sampling lashes and examining samples with a confocal microscope.4 Standard sampling, defined by Coston, recommends the random epilation of four nonadjacent lashes per eyelid.27,28 It should be noted that sampling of lashes with CD is more likely to yield results, however (Figure 3).3 Lashes are then mounted to a coverslip with the addition of a droplet of oil.28 This method has been shown to underestimate the density of infestation. As CD indicates higher detection of mites, Demodex counts may vary based on the presence of CD at the base of the epilated lash.5
  | Figure 3 Microscope photograph of an epilated eye lash showing Demodex folliculorum. Photography courtesy of Scott Hauswirth, OD. |
Modifications have been made to the Coston method of sampling including adding sodium fluorescein and other liquids to dissolve the debris. Sodium fluorescein, peanut oil, or 75% alcohol helps release embedded Demodex. Hom et al describes an additional method of exposing mites by rotating the lashes to scrape out mites residing deeper in the follicle.27 This method may change future clinical patterns and standard of care, as lashes do not need to be epilated. In vivo confocal laser scanning microscopy (CLSM) is an alternate method to confirm diagnosis. It allows for a noninvasive magnified view of the affected follicles.7 With CLSM, mites appear round or cone-shaped; however, the two species of Demodex cannot be differentiated with this method.4 This method has been found to be a superior diagnostic tool compared to standard eyelash sampling with microscope viewing.29 CLSM can not only provide insightful information regarding MGD and conjunctival involvement but also assist in monitoring the condition for improvement.30 Unfortunately, patient cooperation is key with either method, and especially challenging in pediatric populations.3
After sampling, the question remains what number of mites represents normal infestation versus pathognomonic overgrowth or what number of mites is required to elicit symptoms. Further research is needed in these areas.
Management
One of the primary goals in treating Demodex is to reduce parasitic overpopulation in the lids and lashes to decrease inflammation, providing a healthier environment for the ocular surface. While therapy for traditional blepharitis includes warm compresses and antibiotic/steroid combinations, these therapies do not eradicate Demodex, often causing the condition to persist.31 If left untreated – or when poorly managed – adverse effects such as redness, inflammation, telangiectasia, MGD, and ocular allergy may persist.
Patients must understand that long-term lid hygiene is required as Demodex is a chronic condition requiring chronic therapy. Prior to initiating therapy, there are several effective in-office demonstrations that have proven to increase compliance among patients with Demodex, as many lid therapies targeted specifically for Demodex cause ocular discomfort contributing to therapy dropout.32 Anterior segment imaging, epilation of lashes, and use of an allergy or ocular symptom survey may be beneficial to help increase compliance with therapy, monitor the progression of the condition, as well as subjective improvement.4,27 While allergy surveys may not specifically target Demodex symptoms, they may help monitor for improvement in some of the subjective symptoms associated with Demodex such as ocular itching.33,34
When treating Demodex, the primary goal is to reduce the number of mites as the entire mite population cannot be completely eliminated.35,36 There are a number of effective treatment options for patients with Demodex, and selection is based on the severity of the condition. Management may include a combination of lid scrubs and removal of the eyelash collarettes with the use of a blepharitis brush or a cotton-tipped applicator and lid foam. Recent publications have demonstrated that baby shampoo should not be used for lid hygiene as it is ineffective and may have a negative effect on the tear film; the survival time of D. folliculorum in 50% baby shampoo was >150 min and showed no change in quantity over the course of 350 days.35
Demodex mites are resistant to a wide range of antiseptic agents including 75% alcohol, 10% povidone-iodine, and erythromycin.32 The most effective and commonly used treatment agent for Demodex is tea tree oil.32,35,37 Tea tree oil is currently the go-to in-office and at-home treatment option for Demodex.32,35,37 Terpinen-4-ol – a terpene with antimicrobial, antifungal, antiviral, antiseptic, and acaricidal properties – is the active ingredient in tea tree oil.35,37
Terpinen-4-ol has acetylcholinesterase-inhibiting effects that produce the acaricidal effect.37 This leads the mite to exit the hair follicle and migrate onto the skin before mating.9,32,37 Studies have demonstrated that as low as 5% concentration (when applied to the lids twice daily) and as high as 50% concentration (when applied once weekly) of tea tree oil are effective at reducing Demodex infestation when applied to the lids and base of the eyelash follicle.32,37 A 38% concentration of terpinen-4-ol has been shown to reduce Demodex effectively over a period of 4 weeks.37
In patients with skin sensitivities, tea tree oil may cause dermatitis, allergy, and ocular irritation, especially with higher concentrations.38 For this reason, it is recommended that treatment with high concentrations of tea tree oil (50%) be performed in office.39 The goal of the weekly office lid scrub with 50% tea tree oil solution it to stimulate the mites’ migration out of the lash follicle. This is then followed by daily home lid scrub with tea tree oil to prevent Demodex replication on the surface of the skin.35,40 Patients typically need to return for several in-office treatments of tea tree oil over the course of weeks to months in addition to performing daily home therapy.
Patients with Demodex are typically prescribed an eyelid cleanser that contains tea tree oil twice daily in order to eradicate the Demodex mites. They are instructed to cleanse the lids and lashes, as well as smear the lid cleanser onto the eyelash roots of both the upper and lower eyelid margin.4,41 Complete coverage of the eyelash base by the tea tree oil lid cleanser is necessary to be effective so that mites are unable to lay eggs and hatch more Demodex mites.41 Patients should be instructed to use the wipes on their eyelashes, forehead, eyebrows, and cheeks as the mites live in all of those areas.32,39
There are many commercially available products that contain tea tree oil. Some practitioners have found it beneficial to dilute commercially available tea tree oil with macadamia nut or walnut oil to decrease patient discomfort and toxicity to the ocular surface while maintaining efficacy in eradicating the mites.38 However, caution must be taken in those patients with nut allergies. The most commonly used over-the-counter lid cleansing wipes (Table 1) for the management of Demodex include Cliradex® (Bio-Tissue, Inc., Miami, FL, USA) and OCuSOFT® Lid Scrub Plus (OCuSOFT, Richmond, TX, USA). Cliradex® is a lid wipe that contains terpinen-4-ol.39–41 OCuSOFT® Lid Scrub Plus contains a 0.5% solution of 1,2-octanediol, which when used over a 4-week period has been shown to decrease Demodex infestation.41 In addition to branded Avenova® (NovaBay Pharmaceuticals, Emeryville, CA, USA), some mild generic lid cleansers contain detergents or hypochlorous acid, which are active against bacterial, fungal, and viral pathogens.39,41 Hypochlorous acid has been shown to be effective in controlling biofilms and in wound healing. Studies have shown a reduction in the number of Demodex mites with management of hypochlorous acid.39,41
  | Table 1 Summary of lid cleansers for Demodex |
Mild cases are prescribed at-home treatments of once-a-day tea tree oil shampoo and facial wash.4 Moderate-to-severe patients are managed with weekly in-office treatments of high-concentration tea tree oil for 3 consecutive weeks and tea tree oil lid wipes or lid cleanser twice per day at home. In addition, every 3–6 months, severe patients may be treated with BlephEx™, a device by Rysurg utilized to remove the eyelash collarettes by a method known as microblepharoexfoliation.39 Microblepharoexfoliation involves removal of the biofilm on the surface of the lids and lashes using a high-speed rotary sponge soaked in lid cleanser.39 This also helps remove the eggs of the mites at the base of the eyelash follicle. Patients of all severity levels should also be instructed to discard their make-up, use hot water to wash their clothes, and dry linens on the high-dryer setting.
While treatment methods including tea tree oil and microblepharoexfoliation are effective at reducing Demodex, studies have shown that no single management option fully eradicates Demodex after 4 weeks of therapy, highlighting the chronic nature of the condition and requirement for long-term therapy.41
Conclusion
Ocular Demodex is a common, but clinically underdiagnosed condition. From lashes to lid, conjunctiva to cornea, its effects can be widespread. To identify Demodex as the underlying cause, lash sampling and microscopic evaluation may be useful, but clinical signs – especially CD – should also be considered. Failure to diagnose Demodex as the underlying cause of patients’ signs and symptoms may result in noneffective treatment, which can result in frustration for both the clinician and patient. Treatment to completely eradicate the mite is often unrealistic. More importantly, the goal of treatment is to reduce the overgrowth which will alleviate clinical signs and improve patient symptoms.
Disclosure
Jennifer S Harthan serves as a consultant and advisory board member for Allergan and Shire Pharmaceuticals, key opinion leader for SynergEyes, and consultant and lecturer for Metro Optics. Dominick L Opitz serves as a consultant for Shire Pharmaceuticals and as a speaker and consultant for Bausch + Lomb. Stephanie R Fromstein and Jaymeni Patel report no conflicts of interest in this work.
References
Kheirkhah A, Casas V, Li W, Raju VK, Tseng SC. Corneal manifestations of ocular demodex infestation. Am J Ophthalmol. 2007;143(5):743–749. | ||
Bhandari V, Reddy JK. Blepharitis: always remember demodex. Middle East Afr J Ophthalmol. 2014;21(4):317–320. | ||
Liu J, Sheha H, Tseng SC. Pathogenic role of Demodex mites in blepharitis. Curr Opin Allergy Clin Immunol. 2010;10(5):505–510. | ||
Luo X, Li J, Chen C, Tseng S, Liang L. Ocular demodicosis as a potential cause of ocular surface inflammation. Cornea. 2017;36 Suppl 1:S9–S14. | ||
Nicholls SG, Oakley CL, Tan A, Vote BJ. Demodex species in human ocular disease: new clinicopathological aspects. Int Ophthalmol. 2017;37(1):303–312. | ||
Post CF, Juhlin E. Demodex folliculorum and blepharitis. Arch Dermatol. 1963;88:298–302. | ||
Cheng AM, Sheha H, Tseng SC. Recent advances on ocular Demodex infestation. Curr Opin Ophthalmol. 2015;26(4):295–300. | ||
English FP, Nutting WB. Demodicosis of ophthalmic concern. Am J Ophthalmol. 1981;91(3):362–372. | ||
Gao YY, Di Pascuale MA, Li W, et al. High prevalence of Demodex in eyelashes with cylindrical dandruff. Invest Ophthalmol Vis Sci. 2005;46:3089–3094. | ||
Liang L, Ding X, Tseng SC. High prevalence of Demodex brevis infestation in chalazia. Am J Ophthalmol. 2014;157(2):342–348.e1. | ||
Bevins CL, Liu FT. Rosacea: skin innate immunity gone awry? Nat Med. 2007;13(8):904–906. | ||
Liang L, Liu Y, Ding X, Ke H, Chen C, Tseng SCG. Significant correlation between meibomian gland dysfunction and keratitis in young patients with Demodex brevis infestation. Br J Ophthalmol. Epub 2017 Oct 21. | ||
Yam JC, Tang BS, Chan TM, Cheng AC. Ocular demodicidosis as a risk factor of adult recurrent chalazion. Eur J Ophthalmol. 2014;24(2):159–163. | ||
Liang L, Safran S, Gao Y, Sheha H, Raju VK, Tseng SC. Ocular demodicosis as a potential cause of pediatric blepharoconjunctivitis. Cornea. 2010;29(12):1386–1391. | ||
Erbagci Z, Erbagci I, Erkilic S. High incidence of demodicidosis in eyelid basal cell carcinomas. Int J Dermatol. 2003;42(7):567–571. | ||
Galea M, Sharma R, Srinivasan S, Roberts F. Demodex blepharitis mimicking eyelid sebaceous gland carcinoma. Clin Exp Ophthalmol. 2014;42(2):208–210. | ||
Morrás PG, Santos SP, Imedio IL, Echeverria ML, Hermosa JM. Rosacea-like demodicidosis in an immunocompromised child. Pediatr Dermatol. 2003;20(1):28–30. | ||
Elston DM. Demodex mites: facts and controversies. Clin Dermatol. 2010;28(5):502–504. | ||
Hsu CK, Hsu MM, Lee JY. Demodicosis: a clinicopathological study. J Am Acad Dermatol. 2009;60(3):453–462. | ||
Zhao YE, Wu LP, Peng Y, Cheng H. Retrospective analysis of the association between Demodex infestation and rosacea. Arch Dermatol. 2010;146(8):896–902. | ||
Aisa Y, Mori T, Tanikawa A, et al. Demodicidosis as a cause of facial eruption developing early after allogeneic hematopoietic stem cell transplantation. Transpl Int. 2008;21(12):1192–1193. | ||
Cotliar J, Frankfurt O. Demodex folliculitis mimicking acute graft-vs-host disease. JAMA Dermatol. 2013;149(12):1407–1409. | ||
Gerber PA, Kukova G, Buhren BA, Homey B. Density of Demodex folliculorum in patients receiving epidermal growth factor receptor inhibitors. Dermatology. 2011;222(2):144–147. | ||
Lotze C, Krüger WH, Kiefer T, et al. Facial rash mimicking cutaneous acute graft-versus-host disease after allogeneic stem cell transplantation for osteomyelofibrosis – was Demodex the culprit? Bone Marrow Transplant. 2006;37(7):711–712. | ||
Martinez-Diaz GJ, Clark KM, Vasquez JG, English JC 3rd. Facial erythematous annular plaques: a case of annular Demodex facial dermatitis? J Am Acad Dermatol. 2012;67(6):e268–e269. | ||
Román-Curto C, Meseguer-Yebra C, Cañueto J, et al. Demodicidosis simulating acute graft-versus-host disease after allogeneic stem cell transplantation in one patient with acute lymphoblastic leukemia. Transpl Infect Dis. 2012;14(4):387–390. | ||
Hom MM, Mastrota MK, Schachter SE. Demodex: clinical cases and diagnostic protocol. Optom Vis Sci. 2013;90:198–205. | ||
Coston TO. Demodex folliculorum blepharitis. Trans Am Ophthalmol Soc. 1967;65:361–392. | ||
Randon M, Liang H, El Hamdaoui M, et al. In vivo confocal microscopy as a novel and reliable tool for the diagnosis of Demodex eyelid infestation. Br J Ophthalmol. 2015;99(3):336–341. | ||
Kojima T, Ishida R, Sato EA, et al. In vivo evaluation of ocular demodicosis using laser scanning confocal microscopy. Invest Ophthalmol Vis Sci. 2011;52(1):565–569. | ||
Leibowitz HM, Capino D. Treatment of chronic blepharitis. Arch Ophthalmol. 1988;106(6):720. | ||
Gao YY, Di Pascuale MA, Elizondo A, Tseng SC. Clinical treatment of ocular demodecosis by lid scrub with tea tree oil. Cornea. 2007;26(2):136–143. | ||
Bielory L, Katelaris CH, Lightman S, Naclerio RM. Treating the ocular component of allergic rhinoconjunctivitis and related eye disorders. MedGenMed. 2007;9(3):35. | ||
Abelson MB, Gomes P, Smith L, Hollander DA. QoL Questions: Measuring Happiness. The importance of valid questionnaires when treating patients who suffer from ocular allergy. Rev Ophthalmol. Epub 2017 Apr 7. | ||
Gao YY, Di Pascuale MA, Li W, et al. In vitro and in vivo killing of ocular Demodex by tea tree oil. Br J Ophthalmol. 2005;89(11):1468–1473. | ||
Schachter S. A different approach to treating demodex blepharitis. Optometry Times. Epub 2014 Jan 3. | ||
Tighe S, Gao YY, Tseng SC. Terpinen-4-ol is the most active ingredient of tea tree oil to kill Demodex mites. Transl Vis Sci Technol. 2013;2:2. | ||
Koo H, Kim TH, Kim KW, Wee SW, Chun YS, Kim JC. Ocular surface discomfort and Demodex: effect of tea tree oil eyelid scrub in Demodex blepharitis. J Korean Med Sci. 2012;27(12):1574–1579. | ||
Murphy O, O’Dwyer V, Lloyd-McKernan A. The efficacy of tea tree face wash, 1,2-octanediol and microblepharoexfoliation in treating Demodex folliculorum blepharitis. Cont Lens Anterior Eye. 2018;41(1):77–82. | ||
Gao YY, Xu DL, Huang IJ, Wang R, Tseng SC. Treatment of ocular itching associated with ocular demodicosis by 5% tea tree oil ointment. Cornea. 2012;31(1):14–17. | ||
Ngo W, Jones L, Bitton E. Short-term comfort responses associated with the use of eyelid cleansing products to manage Demodex folliculorum. Eye Contact Lens. Epub 2017 Sep 21. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
