Back to Journals » Integrated Pharmacy Research and Practice » Volume 12
Community Pharmacy Professional’s Knowledge, Attitude, and Practice with Regard to Pediatric Pain Management
Authors Yabeyu AB , Haile KT , Molore S
Received 27 September 2022
Accepted for publication 7 January 2023
Published 15 January 2023 Volume 2023:12 Pages 1—9
DOI https://doi.org/10.2147/IPRP.S391415
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Jonathan Ling
Abdella Birhan Yabeyu,1 Kaleab Taye Haile,2 Selamu Molore1
1Department of Pharmacy, Ambo University, Ambo, Ethiopia; 2Department of Social Pharmacy, University of Gondar, Gondar, Ethiopia
Correspondence: Abdella Birhan Yabeyu, Email [email protected]
Background: Effective pain relief is an essential component of high-quality healthcare delivery, and pharmacists must be well versed in pain mechanisms, assessment, and management. This study examined community pharmacy professional’s (CPPs) knowledge and attitude towards pediatric pain management in Community pharmacies (CPs) and Drug Retail Outlets (DRO) of Ambo and Ginchi towns, west central Ethiopia.
Methods: A cross sectional study was conducted in Ambo and Ginchi towns, the western part of the nation’s capital. All voluntary CPPs working by CPs and DRSs in the towns of Ambo and Ginchi were included in the current study. SPSS version 25 was then used to process, analyze, and interpret the data.
Results: Among the 131 CPPs who were approached for the study, 104 agreed to participate and returned the questionnaire. CPPs mean knowledge score on pediatric pain management was 6.69 ± 1.92, with a minimum score of 2 and a maximum score of 17. The majority of CPPs 82 (87.2%) in the study did not correctly answer half of the questions. Most of CPPs, 98 (94.3%), admitted they had no training in pain management, and 102 (98.2%) of the respondents said the same about pediatric pain management. The finding indicated that CPPs work experience in CP or DROs had impact on their knowledge about pediatric pain management and similarly, the mean knowledge score of pharmacists was higher than that of pharmacy technicians.
Conclusion: This study revealed that CPPs have inadequate knowledge and attitude to provide effective pediatric pain management service. To bridge the knowledge gap and effectively control pediatric pain, pharmacists who are actively practicing their profession are advised to continue their medical education and training.
Keywords: community pharmacy professionals, pain, pediatrics
Introduction
Pain is widely acknowledged as a complex multidimensional subjective experience that can be difficult to recognize, assess, or manage, especially in children and young adults.1 It is defined as “an unpleasant sensory and emotional experience associated with, or resembling, actual or potential tissue damage.2” It affects infants and children more than adults, and they can encounter it associated with illness, casual activities, trauma, and minor injuries (cuts, bumps, and burns). As a result, they frequently present to healthcare settings, with the global prevalence of chronic pain estimated to be 20–35%.3
Pain management in children requires a multimodal approach as their pain appears to have both physical and psychological component. In addition, children, particularly those of a younger age, may be unable to express their pain verbally. As a result, it requires a cautious approach in which the child, their parents, and healthcare professionals all play an important role in successfully managing their pain experience.4,5 Both pharmacological and non-pharmacological interventions could help in the management of pain. It can be managed with a wide range of medications such as acetaminophen, non-steroidal anti-inflammatory drugs (NSAIDs), and opioids.6,7
Given that, pharmacy professionals are medication experts and amongst the most accessible healthcare professionals,8 those that practice in the community are the most frequently visited places to seek pain management services.9,10 They play an important role in pediatric pain management by dispensing Over the Counter analgesics, offering advice, suggestions, and medication reviews.10–12 Effective pain relief is an essential component of high-quality healthcare delivery, and pharmacists must be well versed in pain mechanisms, assessment, and management.13 However, there can be gaps in their knowledge which may adversely impact on patient outcome.14 Various studies show that children’s pain is widely underdiagnosed and undertreated, increasing the likelihood and severity of complications and causing suffering.15–17 Consequently, negatively affecting the patient’s quality of life and causing stress and anxiety in both the patient and the caregiver.18
Many studies conducted around the world revealed a lack of knowledge and a negative attitude toward pediatric pain management among healthcare professionals. The majority of the studies are carried out in hospital settings, with a focus on nurses, physicians, and medical students.5,9,10,12,19 To date, few studies involved community pharmacists, and none have been conducted in Ethiopia. Community pharmacies are often the first places where advice on management of pediatric pain is sought. As a result, evaluating the knowledge of pharmacy professional is essential and may lead to the identification of gaps that require intervention for improvement. Therefore, this study examined community pharmacy professional’s (CPPs) knowledge and attitude towards pediatric pain management in CPs and Drug Retail Outlets (DRO) of Ambo and Ginchi towns, West central Ethiopia.
Methods
Study Setting, Area and Period
A cross sectional study was conducted in Ambo and Ginchi towns, the western part of the nation’s capital. They are located 119 KM and 88 KM away from Addis Ababa, respectively. In Ambo town, there are thirty DOSs and ten CPs available, but only seven DOSs are available in Ginchi town (Oromia Regional Health Bureau, 2022). The study was carried out from March to April 2022.
Source and Study Population
All CPPs currently working in Ambo and Ginchi town DOSs and CPs were considered target populations. The study population consisted of pharmacy practitioners who were available during data collection and willing to participate in the study.
Eligibility Criteria
All voluntary CPPs working under CPs and DROs in the towns of Ambo and Ginchi were included in the current study. However, professionals with less than a year of experience in CPs or DROs were excluded from the study (they work under supervision of the license holders, they hardly provide pharmaceutical services independently).
Questioner Design and Procedure
The questioner was prepared after a thorough review of relevant literature on pediatric pain management.5,12,20–23 The data collection instrument is divided into two sections: one for the sociodemographic characteristics of CPPs such as age, gender, experience working in CPs, educational qualifications, and so on, and the other for assessing their knowledge, attitudes, and practices on pediatric pain management. The knowledge and attitude questions cover four areas: the multidimensional nature of pain, pain assessment and measurement, pain treatment, and clinical conditions/pain syndromes. The practice questions covered topics like having received prior training in pain management, the number of such trainings, the location and perceived cause of pain experienced, painful conditions that had ever been referred, and what factors influenced the referral and interest in further training, whether one had already received it or not. On a 3-point Likert scale, 11 of the 23 knowledge items were graded (Yes, I agree; I am not sure and No, I disagree). The answers to the 11 items were used to assess knowledge and were graded as correct, incorrect, or unsure. The remaining 13 multiple-choice items were divided into three groups: accurate, incorrect, and uncertain. A pre-test was conducted to ensure the validity of the study instrument validity and questions that did not actually measure participant’s perception were omitted; the Cronbach’s alpha score was 0.798. The data collection was carried out by three data collectors (three BPharm). The principal investigators trained the data collectors about the study instrument and ethical considerations over the duration of two days.
Data Processing and Analysis
The data was entered into Epi-Info Version-7.2.1.0 and analyzed with SPSS version-25. Frequency, median, range, mean, and standard deviation were used to summarize the descriptive data. Skewness and Kurtosis, the Kolmogorov–Smirnov test and histograms were employed to check the normality of the data. To test the difference between the mean score of correct and incorrect responses among the different groups in the study, one-way ANOVA and an independent t-test were used. Statistical significance was determined if the p-value was less than 0.05.
Results
Socio Demographic Profiles of the Participants
Among the 131 CPPs who were recruited for the study, 104 agreed to participate and returned the questionnaire, giving the study a response rate of 79.4%. The majority of study participants 89 (85.6%) were males. Of the pharmacy professionals, 70 (67.3%) held bachelor’s degrees in pharmacy as their highest level of education. More than two-thirds of the participants 76 (73.1%) had one to five years of experience working in CPs or drug DROs. Hospitals were the previous places of employment for the majority of respondents 85 (81.7%) (Table 1).
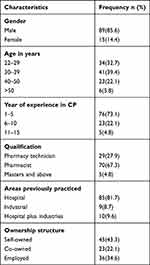 |
Table 1 Sociodemographic Characteristics of the Participants Who Responded to Survey on Pediatric Pain Management in Ambo and Ginchi Towns |
Knowledge and Attitude of CPPs to Pediatric Pain Management
CPPs mean knowledge score on pediatric pain management was 6.69 ±1.92, with a minimum score of 2 and a maximum score of 17. The majority of CPPs 82 (87.2%) in the study did not correctly answer half of the questions. About one-third of 39 (37.5%) respondents gave an accurate response to the statement that pain is one of the crucial symptoms in pediatric patients. When asked whether repeated painful procedures on children increase their pain tolerance, less than half of CPPs 47 (45.2%), were properly answered. 16 (15.4%) of them knew the correct answers about the recommended analgesic dose of paracetamol in children under 3 months of age. Additionally, only 9 (8.7%) of CPPs properly responded to the question about non-pharmacological methods of pediatric pain management (Table 2).
 |
Table 2 CPPs Knowledge and Attitude to Pediatric Pain Management |
CPPs Practice Towards Pediatric Pain Management
Most of CPPs, 98 (94.3%), admitted they had no training in pain management, and 102 (98.2%) of the respondents said the same about pediatric pain management. Regarding grounds for referral in pediatric pain management, the majority of CPPs 47 (45.2%) perceived disease-related factors as the primary cause of pain. Whereas, most of CPP 41 (39.4%) cited “for Better Care” as a primary reason for referral (Table 3).
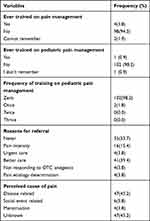 |
Table 3 CPPs Practice Towards Pediatric Pain Management |
Relationship Between Sociodemographic Characteristics and CPPs Knowledge
A one-way ANOVA and independent t-test statistics was performed to determine whether there is a statistically significant relationship between sociodemographic variables and the mean knowledge score of CPPs. The finding indicated that CPPs work experience in CP or DROs had impact on their knowledge about pediatric pain management (p-value= 0.000). Similarly, the mean knowledge score of pharmacists was higher than that of pharmacy technicians (p value= 0.001), as well as an independent t-test statistics was performed but failed to show any association (Table 4).
 |
Table 4 Relationship Between Sociodemographic Characteristics and Mean Knowledge Score |
Discussion
The role of community pharmacists is expanding globally from merely dispensing medication to involving in different public health services and playing a key role in disease state management.24,25 Studies showed that community pharmacists are a major primary healthcare provider that frequently attend to pediatric patients with various painful conditions.26 Considering this, this study, which is the first of its kind, was conducted aimed at assessing CPPs knowledge, attitude and practice towards pediatric pain management in Ethiopia.
In this study, significant portion of the participants did not correctly answer half of the questions (mean=6.69 ±1.92, 87.2%) alarmingly showing the inadequacy of CPPs knowledge towards pediatric pain management. This finding is consistent with findings from studies conducted in Nigeria and Canada, both of which found inadequate knowledge of pediatric pain among community pharmacists.19,27 Moreover, it is also in line with other studies conducted among other healthcare professionals and revealed lack of knowledge about management of pediatric pain. It is critical to have a strong knowledge base in pediatric pain management to ensure optimal pain treatment.28 As a result, this study suggests that a great effort should be made to regularly assess CPPs knowledge, identify appropriate interventions, and improve service delivery quality.
In the present study, less than ten percent of CPPs (8.7%) were familiar with non-pharmacological methods of pediatric pain management. In contrary to this study finding, majority of United Arab Emirates (UAE) community pharmacist had adequate knowledge about non-pharmacologic pain management.5 The variation could be due to difference in source of information, and the availability of continuous and sustainable on-The-job training in the two countries. It is important to note that non-pharmacological approaches to pain management are more advantageous than pharmacological pain management because they are less expensive, easier to apply, have a high potential for pain relief, and can be used in conjunction with drugs or alone.18
This study found that CPPs have misbelief about pediatric pain and pain management. For example, the majority of participants believed that a child’s frequent request for analgesic means he or she is already addicted (87.5%), that infants forget painful episodes faster than adults (71.2%), and that infants feel less pain than adults in similar situations (66.3%). Such erroneous beliefs are concerning and should be seriously considered and addressed through continuing professional development including targeted on job trainings that could help build pharmacist capacity in this area. In the long run, it is recommended that pain management trainings be included in pharmacy curricula to produce pharmacy professionals who are capable of providing appropriate care to pediatric patients.13
In general, CPPs with more than ten years of experience had the highest mean correct answer score. A similar finding was reported in Canada and the UAE, where experience has a significant effect on pain management knowledge.5,19 The positive relationship observed may be because as the number of years of practice increases, professionals are more likely to be exposed to pain management on a regular basis; more experienced CPPs may have more opportunities to gain access to up-to-date information about pain management and gradually from their daily observations and practices.
In this study, the other factor that was significantly associated with CPPs knowledge of pediatric pain management was level of qualification. CPPs with BPharm degree were more likely to have a higher mean score for pediatric pain management than those with a diploma. This finding is consistent with a study conducted in Nigeria, which found that community pharmacists with additional qualifications such as Pharm D had better knowledge of pediatric pain management as compared to other participants in the survey.27 This could be explained by the fact that pharmacists with higher educational levels have a greater opportunity to obtain current information by accessing and reviewing different literatures.
There are a few limitations to this study that should be considered when interpreting and generalizing the study findings. The research was carried out in two Ethiopian cities, in CP and DROs. As a result, when generalizing to CPPs working in other settings or across the country, caution should be taken. Second, because the study responses were primarily self-reported, the study may have been influenced by social desirability and recall bias.
Conclusion
Overall this study showed CPPs have inadequate knowledge and negative attitude to provide effective pediatric pain management service. Educational qualification and years of experience were discovered to be significantly associated with CPPs knowledge, implying that pharmacists who are actively practicing their profession must continue their medical education and training to bridge the knowledge gap and provide better pediatric patient care.
Abbreviations
CP, Community Pharmacy; CPP, Community Pharmacy Professional’s; DOS, Drug Outlet Stores.
Data sharing statement
The data will be obtained after requesting corresponding author.
Ethical consideration
The ethics review committee of Ambo University’s school of pharmacy has given its approval for the study. All participants gave their informed consent both verbally and in writing prior to the study’s initiation. The current study complies with the Declaration of Helsinki.
Acknowledgment
The authors would like to thank the School of Pharmacy, Ambo University and community pharmacy professionals who were participated in the study.
Disclosure
The authors report no conflicts of interest in this work.
References
1. James S, Nelson K, Ashwill J. Nursing Care of Children: Principle and Practice.
2. WHO, Newspaper IASP. IASP Revises Its Definition of Pain for the First Time Since 1979. 2020. https://www.iasp-pain.org/wp-content/uploads/2022/04/revised-definition-flysheet_R2.pdf.
3. King S, Chambers CT, Huguet A, et al. The epidemiology of chronic pain in children and adolescents revisited: a systematic review. Pain. 2011;152(12):2729–2738. doi:10.1016/j.pain.2011.07.016
4. Pope N, Tallon M, McConigley R, Leslie G, Wilson S. Experiences of acute pain in children who present to a healthcare facility for treatment: a systematic review of qualitative evidence. Joanna Briggs Institute. 2017;15:1612–1644.
5. Jairoun AA, Saleh Al-Hemyari S, Shahwan M, Jairoun M, Kurdi A, Godman B. Assessing knowledge, attitude and practice of community pharmacists on the pain management and implications in UAE children. Pharm Pract. 2022;20(2):1–10.
6. Rosenblum A, Marsch LA, Joseph H, Portenoy RK. Opioids and the treatment of chronic pain: controversies, current status, and future directions. Exp Clin Psychopharmacol. 2008;16(5):405–416. doi:10.1037/a0013628
7. Moore RA, Derry C. Efficacy of OTC analgesics. Int J Clin Pract. 2013;67:21–25. doi:10.1111/ijcp.12054
8. Gomes T, Mamdani MM, Dhalla IA, Michael J, LESS IS MORE Opioid Dose and Drug-Related Mortality in Patients With Nonmalignant Pain [Internet]. Available from: www.archinternmed.com.
9. Lalonde L, Leroux-Lapointe Bsc V, Choinière Phd M, et al. Knowledge, attitudes and beliefs about chronic noncancer pain in primary care: a Canadian survey of physicians and pharmacists. Pain Res Manag. 2014;19(5):241–250. doi:10.1155/2014/760145
10. Tabeefar H, Chang F, Cooke M, Patel T. Community pharmacists and chronic pain: a qualitative study of experience, perception, and challenges. Canadian J Pain. 2020;4(3):29–39. doi:10.1080/24740527.2020.1749516
11. Mishriky J, Stupans I, Chan V. The role of the pharmacist in low back pain management: a narrative review of practice guidelines on paracetamol vs non-steroidal anti-inflammatory drugs. In: Pharmacy Practice. Vol. 18. Grupo de Investigacion en Atencion Farmaceutica; 2020:1–8.
12. Ogunyinka I, Yusuff K, Erah PO, et al. Community pharmacists’ knowledge and attitudes towards pediatric pain management in Nigeria. Risk Manag Healthc Policy. 2021;14:4595–4607. doi:10.2147/RMHP.S329387
13. Papastavrou E, Efstathiou G, Lemonidou C, Kalafati M, Katajisto J, Suhonen R. Cypriot and Greek nurses’ perceptions of the professional practice environment. Int Nurs Rev. 2014;61(2):171–178. doi:10.1111/inr.12083
14. Tabeefar H, Chang F, Cooke M, Patel T. Community pharmacists and chronic pain: a qualitative study of experience, perception, and challenges. Canadian J Pain. 2020;4(3):29–39.
15. Stevens BJ, Harrison D, Rashotte J, et al. Pain assessment and intensity in hospitalized children in Canada. J Pain. 2012;13(9):857–865. doi:10.1016/j.jpain.2012.05.010
16. Friedrichsdorf SJ, Postier A, Eull D, et al. Pain Outcomes in a US Children’s Hospital: a Prospective Cross-Sectional Survey. Hosp Pediatr. 2015;5(1):18–26. doi:10.1542/hpeds.2014-0084
17. Walther-Larsen S, Pedersen MT, Friis SM, et al. Pain prevalence in hospitalized children: a prospective cross-sectional survey in four Danish university hospitals. Acta Anaesthesiol Scand. 2017;61(3):328–337. doi:10.1111/aas.12846
18. Tekletsadik EA, Desta AA, Workneh BS. Knowledge, Attitude, and Associated Factors towards Nonpharmacological Pain Management among Nurses Working at Amhara Region Comprehensive Specialized Hospitals, Ethiopia. Crit Care Res Pract. 2021;2021. doi:10.1155/2021/7374915
19. Patel T, Chang F, Mohammed HT, et al. Knowledge, perceptions and attitudes toward chronic pain and its management: a cross-sectional survey of frontline pharmacists in Ontario, Canada. PLoS One. 2016;11(6):e0157151. doi:10.1371/journal.pone.0157151
20. Fishman SM, Young HM, Lucas Arwood E, et al. Review Articles Core Competencies for Pain Management: results of an Interprofessional Consensus Summit [Internet]. Pain Medicine: Vol. 14. Wiley Periodicals, Inc; 2013.
21. Vagnoli L, Mammucari M, Graziani D, Messeri A. Doctors and Nurses’ Knowledge and Attitudes Towards Pediatric Pain Management: an Exploratory Survey in a Children’s Hospital. J Pain Palliat Care Pharmacother. 2019;33(3–4):107–119. doi:10.1080/15360288.2019.1686100
22. Hurley-Wallace A, Wood C, Franck LS, Howard RF, Liossi C. Paediatric pain education for health care professionals. Pain Rep. 2019;4(1). doi:10.1097/PR9.0000000000000701
23. Kholowa ET, Chimwaza AF, Majamanda MD, Maluwa AO. Nurses’ Knowledge and Attitudes towards Pain Management in Children Admitted in the Paediatric Department of Queen Elizabeth Central Hospital, Blantyre, Malawi. J Biosci Med. 2017;05(06):46–59.
24. Anderson C, Blenkinsopp A, Armstrong M. The contribution of community pharmacy to improving the public’s health. Int J Med. 2003;1–85.
25. Hess KM, Dai CW, Garner B, Law A. Measuring outcomes of a pharmacist-run travel health clinic located in an independent community pharmacy. J Am Pharmacists Assoc. 2010;50(2):174–180. doi:10.1331/JAPhA.2010.09204
26. Okai GA, Abekah-Nkrumah G, Asuming PO. Perceptions and trends in the use of community pharmacies in Ghana. J Pharm Policy Pract. 2019;12(1). doi:10.1186/s40545-019-0186-x
27. Ogunyinka I, Yusuff K, Erah PO, et al. Community pharmacists’ knowledge and attitudes towards pediatric pain management in Nigeria. Risk Manag Healthc Policy. 2021;14:4595–4607.
28. Stanley M, Pollard D. Relationship between knowledge, attitudes, and self-efficacy of nurses in the management of pediatric pain. Pediatr Nurs. 2013;39(4):165–171.
 © 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
