Back to Journals » Journal of Multidisciplinary Healthcare » Volume 14
Clinicians’ Perceptions of Picture Archiving and Communication System (PACS) Use in Patient Care in Eastern Province Hospitals in Saudi Arabia
Authors Al-Kahtani N , Al-Dhaif E , Alsaihtati N, Farid K, AlKhater S
Received 19 December 2020
Accepted for publication 9 March 2021
Published 31 March 2021 Volume 2021:14 Pages 743—750
DOI https://doi.org/10.2147/JMDH.S296828
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Nouf Al-Kahtani, Esra Al-Dhaif, Noor Alsaihtati, Khalid Farid, Suzan AlKhater
Department of Health Information Management and Technology, College of Public Health, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
Correspondence: Nouf Al-Kahtani
Department of Health Information Management and Technology, College of Public Health, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
Email [email protected]
Purpose: The picture archiving and communication system (PACS) is one of the most important tools used in patient care in many hospitals worldwide. It allows clinicians to remotely communicate and consult with other clinicians on patient cases and view diagnostic images from different angles, thus facilitating patient diagnosis and treatment. Several studies have been conducted in Saudi Arabia to evaluate different aspects of PACS use; however, no comprehensive study has been conducted in its Eastern Province. This study aimed to investigate clinicians’ perceptions of the advantages and disadvantages of the use of PACS in Eastern Province hospitals in Saudi Arabia and identify the factors that affect their perceptions and its use. In addition, it aimed to gather recommendations of clinicians for improving the system and its implementation.
Methods: A qualitative approach with grounded theory method was employed. A sample of 18 residents, radiologists, and consultants from three Eastern Province hospitals in Saudi Arabia participated in the study. Data were collected using semi-structured interviews over a period of 7 months.
Results: The perceived advantages of PACS included providing quality images and the ability to manipulate their resolution, whereas the perceived barriers included low-speed internet connections and technical problems. Participants recommended providing clinicians remote access to the system and implementing a mobile PACS application. The theory that emerged from the analysis revealed that demographic, system-related, and hospital-related factors affected participants’ perspectives of PACS and its use.
Conclusion: The results of this study and its theoretical model can help identify areas of improvement and inform policy and strategic planning for the effective implementation of PACS in patient care in Saudi Arabia.
Keywords: radiology, healthcare technology, medical technology, patient care
Corrigendum for this paper has been published
Introduction
The picture archiving and communication system (PACS), “provides a centralized repository for all imaging data and delivers diagnostic images and radiology reports electronically to clinicians at the point of care”.1 PACS, which is primarily used in radiology departments, has evolved to integrate medical images from other departments, such as cardiology, oncology, and dermatology.2 Many hospitals worldwide have implemented PACS to support their routine workflow and improve the provision of patient care. However, several barriers affect its use, such as staff resistance to the system, required system downtime, and insufficient staff training for its use.3,4 Saudi Arabia is among the countries that have adopted PACS and experienced its advantages and disadvantages and is moving toward effective system utilization in its hospitals.
PACS Use in Saudi Arabia
PACS has been implemented in several hospitals in Saudi Arabia. However, studies on PACS in Saudi Arabia have largely been conducted in Riyadh. A study of three hospitals in Riyadh that implemented PACS in their practice concluded that clinicians and radiologists had strong positive perceptions of the system because of the benefits it offers.4 Two studies conducted at the National Guard Health Affairs, King Abdulaziz Medical City, revealed that PACS had a positive impact on users’ work and increased their satisfaction.5 Aldosari et al’s study in the radiology department of a hospital in Riyadh found that PACS users believed that the system improved their work quality and enhanced the provision of patient care.6
Advantages of PACS Use
The importance of PACS has increased with time, and its advantages have been confirmed in numerous studies. Studies have shown that PACS improves the productivity of radiology departments and provides users with rapid online access and faster web-based access to diagnostic images.7,8 Moreover, PACS has been shown to increase clinicians’ efficiency, enhance diagnostic efficacy, and shorten the average turnaround time for radiology reports from 80 h to 20 h.7 Access to PACS images and reports from multiple locations allows immediate and better clinician decision-making and increases the quality of patient information by making it more accurate, relevant, and timely, improving the continuity of the patient care process.3 PACS is cost effective because it prevents the loss of images and unreadable and duplicate films, reduces the need to purchase and use film, and minimizes the need for film library space.7 PACS enables timely image retrieval and “voice recognition, transcription, and real-time monitoring”.4
Studies focused on the user perspective found that the perceived benefits of PACS are that it enables easy access to patient data, provides better access to diagnostic images than traditional film, and reduces practice time by 30 min to 1 h a day.3 According to some studies, PACS can decrease patients’ length of stay (LOS) in the hospital.4 Nitrosi’s study concluded that PACS reduced LOS by 12% among patients in the neurology department.9 Watkins’s study revealed that LOS decreased by 25% in patients who underwent knee replacement,10 and Hurlen found that PACS reduced LOS of patients who underwent a computed tomography scan from 5.3 to 3.9 days.11 Conversely, Crowe and Sim’s study found no relationship between PACS use and reduced LOS.12
Barriers to PACS Use
Despite the significant benefits of PACS, the implementation of such innovative technologies in hospital settings is challenging. Numerous studies have identified factors that affect PACS use and hinder the attainment of its desired outcomes. One of the most significant factors that influence the use of PACS is users’ acceptance of or resistance toward the system. According to Ahmadi, “There is a positive relationship between the effectiveness of technology and its acceptance by the users”.13 Insufficient understanding of the usefulness of the system may result in resistance toward it and have a negative impact on work performance and staff productivity.13 Moreover, insufficient training on the system is considered a barrier to PACS use.4 From a technical perspective, repeated interruptions in the system is one of the main issues that impede its utility.3,4 One study found that the internet network connection plays a significant role in the implementation of PACS.7 Providing a stable network connection can improve the system’s performance and facilitate its use to complete work as required. Technological barriers are common and a critical issue worldwide. Insight into these barriers and recommendations so as to address them can contribute to improving the use of PACS in hospitals and for patient care.
Patient Safety
Successful implementation and integration of PACS with other health information systems will increase the productivity of clinicians and patient safety. Maintaining and improving levels of safety will depend on developing systems and a culture that can intelligently integrate individuals with technology and processes to create a safer patient care environment.14
Effective and efficient digital medical achieving and communication system improves patient safety through access to medical images of patients in the shortest possible time and with accurate diagnosis and timely medical care.15 PACS increases patient safety by reducing errors of unread exams. Other studies have found that PACS is decreasing the need for re-imaging and patients’ exposure to harmful rays.15,16 Further, PACS is reducing the average waiting time for patients.8
Research Aims
The primary aims of this study were to investigate clinicians’ perceptions of PACS, how they use the system and the advantages and disadvantages of its use, and to obtain their suggestions for improving its implementation. Finally, the study aimed to identify the factors that influence clinicians’ perceptions and use of PACS in order to provide insight into ways to enhance its use. The following research questions were addressed:
- Do hospital clinicians use PACS in their practice?
- What are the perceived advantages of PACS use?
- What are the perceived disadvantages of and/or barriers to PACS use?
- What are clinicians’ recommendations for improving PACS use?
Materials and Methods
This study employed a qualitative research approach and grounded theory to investigate the use of PACS in three hospitals in the Eastern Province of Saudi Arabia from a clinician’s perspective. Qualitative research “discovers the world from the participants’ perspective”.17 Data were collected using semi-structured interviews and analyzed using grounded theory methods. A grounded theory study “is an inductive study that builds abstractions, concepts, hypothesis, and theories from participants’ words”.17 The data collected in the interviews were used to formulate a theory on the phenomenon explored: PACS use in patient care in hospitals.
Participant Sample
Participants were clinicians who use PACS and were recruited from various clinical departments of three hospitals: one government hospital (King Fahad University Hospital, in the city of Al-Khobar) and two private hospitals (Arrawdha Hospital and Mouwasat Hospital in the city of Dammam). A total of 18 male and female clinicians, including residents, radiologists, and consultants participated in the study; 12 participants were from King Fahad University Hospital, 4 were from Mouwasat Hospital, and 2 were from Arrawdha Hospital.
Data Collection
The study was conducted in 2018 for 7 months, from January to July. Data were collected using semi-structured interviews at the three hospitals. After obtaining the Institutional Review Board approval, individual interviews with each of the 18 participants were conducted. Participants were informed of the study’s purpose and objectives and that their participation will remain confidential. The participants’ responses during the interviews were documented in notes. A theoretical sampling method was followed in collecting data for this study. According to Glaser and Strauss,
Theoretical sampling is the process of data collection for generating the theory whereby the analyst jointly collects, codes, and analyzes his data and decides what data to collect next and where to find them in order to develop his theory as it emerges.18
Data collection ended when saturation had been reached, which is the point where no new information emerged.
Data Analysis
Applying grounded theory analysis methods, data analysis was conducted in tandem with data collection at the different hospitals.17,19 The analysis included systemic review, organization, and coding of the interview data and was ongoing during data collection and after the data was collected “because they influence each other”.14 Data collection was modified based on the data analysis; and the analysis evolved, in turn, based on the data collected. The researchers read the interview notes and identified potential categories in the data. Then, based on the categories that emerged, the researchers compared the interview data and analyzed the relationships among them. Finally, based on the analysis, the researchers built a theoretical model, which was continually refined based on the results.17 The data analysis process was manually conducted by the research team without using any software.
Results
The results are presented in the form of a narrative report and address the four research questions, using “quotes from interviews that illuminate the theory”.17 Following these results, a theoretical model of the factors that influenced participants’ perceptions and use of PACS is presented (Figure 1).
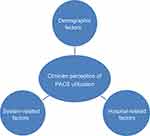 |
Figure 1 Factors affecting perception and usage of picture archiving and communication system (PACS). |
Research Question 1: Do the Participants Use PACS in Their Practice?
Data analysis revealed that all participants (18) used PACS on a daily basis. One participant stated, “PACS is very important in every hospital; we use it continuously.” The clinicians in the radiology department used PACS directly and continuously, whereas participants in the hospital clinics used PACS only when it was necessary for patient care.
Research Question 2: What are the Perceived Advantages of PACS Use?
Results show that all participants had positive perceptions of PACS, and they reported a number of different advantages to using PACS in their daily practice. The perceived advantages are presented in descending order of prevalence:
Fast workflow processes (n = 10): Over half of the participants reported that PACS provides rapid services and fast workflow processes. One participant stated, “PACS provides a fast process.”
Image resolution manipulation (n = 10): Over half of the participants indicated that PACS enabled them to change and control image brightness or color contrast to suit their needs. One participant reported, “PACS allows us to control the contrast resolution.”
Multi-plane image reconstruction (n = 9): Half of the participants reported that they can view images from different angles using PACS. One participant reported, “It provides the ability to view pictures from different angles.”
Increased diagnostic accuracy (n = 7): Seven participants stated that PACS allowed them to make better and accurate diagnoses. According to one participant, “PACS increases the accuracy of diagnosis.”
Patient reports attached to images (n = 7): Seven participants indicated that a significant advantage of PACS is the ability to attach patient reports to the images. One participant shared,
“PACS enable us to attach the reports with the pictures.”
High-quality images (n = 6): Six participants reported that PACS provides high-quality images, which improved their diagnoses. One participant shared, “It provides high-quality images.”
Remote consultation and communication (n = 4): The participants from Mouwasat Hospital reported that PACS enabled them to communicate with branches of the hospital in other cities and allowed for remote consultations. One participant stated, “We have a remote consultation feature.”
Research Question 3: What are the Perceived Disadvantages of and/or Barriers to PACS Use?
Based on participant responses, a number of issues impeded PACS use in their hospitals and daily practice. The perceived barriers are presented in descending order of prevalence:
Low-speed network connection (n = 6): Six participants revealed that PACS was at times affected by slow internet network connections, which causes delays in their work. One participant noted that “slow network connections,” interrupted their work.
Lack of training on PACS (n = 6): Clinicians from King Fahad Teaching Hospital who work in the outpatient clinic believed that they did not receive sufficient training on PACS. One participant stated, “I need training to deal with PACS.”
Costly system maintenance and upgrades (n = 5): Five of the participants stated that PACS requires ongoing upgrades to add new features and frequent maintenance, which are costly, as one participant stated, “PACS maintenance, either hardware or software, is considered costly.”
Loss of data (n = 4): Four participants reported frequent loss of patient data and images in the system, which requires regular backup. One participant stated, “PACS needs online backup.”
Technical problems (n = 3): A few participants commented that technical issues related to hardware and software, such as the type of computers they used, affected PACS use. One participant shared, “There are some technical problems affecting the use of PACS.”
In addition, participants at Arrawdha Hospital (n = 2) reported that a customized PACS is used at their hospital for viewing images alone. The system is not integrated with patient records at the hospital and lacks the ability to attach reports or align images with patients’ files. One of the participants commented, “PACS lacks integration with patient’s records.”
Research Question 4: What are Participants’ Recommendations for Improving PACS Use?
Participants shared a number of practical suggestions to enhance the system and improve its processes.
Remote access (n = 4) and mobile application (n = 5): Four participants suggested that providing remote access to the system could facilitate and accelerate the process of reviewing images and making diagnoses, as one participant articulated, “We suggest enabling us to access PACS remotely.”; and five participants further suggested installing a PACS mobile application for smartphones so clinicians can access images faster and at any time. One participant stated, “We suggest making it available on phones.”
Regular data backup (n = 5): Four participants stated that PACS must be supported by the regular backup of patient data to meet patients’ needs and provide continuous quality of care, as one participant shared, “For successful PACS implementation, it should have regular backup of patients’ data.”
High-speed network connection (n = 5): Five clinicians reported that a better and faster internet network connection is necessary to support workflow and enhance daily practice with PACS. One participant stated, “We need a faster connection.”
Participants from Arrawdha Hospital (n = 2), where adequate monitors to display and view PACS images were absent and the system was not integrated with patients’ medical records, recommended that these issues be addressed to improve PACS implementation at the hospital.
Factors That Influence PACS Perceptions and Use: A Theoretical Model
Based on the theoretical interpretation of the participants’ perceptions, three main factors affected their perceptions and use of PACS: demographic, system-related, and hospital-related factors (See Figure 1). The demographic factors that played an important role in participants’ perceptions of PACS were,
Professional rank: The higher the professional rank of the clinician, the more positive their perception of PACS, which resulted in more effective use of the system. Consultants’ perceptions of PACS were more positive compared to residents; and
Clinical expertise: Clinicians who specialized in using PACS and clinicians who frequently used PACS, such as radiologists and consultants in the radiology department, had more positive perceptions of PACS compared to clinicians who worked in outpatient clinics.
System-related factors had a significant influence on participants’ perceptions and use of PACS, including,
System’s speed: The high speed of PACS was extremely important to participants. It increased their acceptance of the system and affected the diagnosis process;
Ease of use: PACS is user-friendly and this enhanced the participants’ use of the system;
Quality of images: The clarity and quality of images in PACS increased participants’ positive perceptions of the system and the quality of their diagnoses;
Integration with patient records: PACS’ integration with patients’ electronic health records is extremely important to continuity of patient care and increased clinicians’ acceptance of the system;
Auto-backup of data: Automatic backup of data is a significant feature of PACS, which can prevent data loss and support continuous healthcare provision. When not available or in use, this had a negative impact on clinicians’ perceptions of the system; and, finally,
Remote access: The web-based PACS enables users to access the system from anywhere at any time, which could facilitate increased productivity and affect clinicians’ perceptions and use.
Hospital-related factors play a key role in influencing PACS itself and clinicians’ perceptions of it.
System maintenance and upgrade costs: PACS has many useful features, which must be implemented to improve diagnosis and treatment process. Without an allocated budget to develop these features, the system is less effective, with a negative impact on clinicians’ perceptions and use.
Infrastructure: Appropriate infrastructure, such as a high-speed internet network and suitable workstations and monitors, could have a significant impact on clinicians’ use of the system. Support: Hospital support includes financial support, appropriate training, and system improvements, which are needed to enhance PACS use and have a significant impact on its acceptability.
Discussion
All participants in this study had positive perceptions of PACS. This finding coincides with previous studies conducted in Saudi Arabia.4,6,20 The participants cited a number of PACS advantages. These advantages had a positive influence on PACS use and motivated staff to use the system regularly. One of the most prevalent perceived advantages of PACS was the system’s speed and the fast workflow process it affords. Similarly, previous studies conducted in Iran showed that PACS decreased radiologist reporting time and increased the utilization rate of radiology services.8 In addition, other studies conducted in Saudi Arabia similarly found that PACS use resulted in increased efficiency. Aldosari et al’s study of 100 PACS users in the radiology department of KAMC-National Guard in Riyadh found that PACS use resulted in efficient workflow.20 Alalawi et al’s study of clinicians at three Riyadh hospitals found that PACS improved efficiency and physician’s ability to make decisions regarding patient care.4 Many of the participants in our study cited the high quality of PACS images and its multiple viewing functions, which allow for increased accuracy and improved diagnoses. A number of participants referred to the ability to attach a report to the images in patients’ medical records; however, PACS was not integrated with regular patient records at Arrawdha Hospital and this feature was not available to them. Furthermore, participants from Mouwasat Hospital (n = 4) were able to utilize the remote consultation and communication feature of the PACS with other branches of the hospital; however, this feature was not applicable to participants at the other two hospitals.
The disadvantages of and barriers to its use had a negative influence on participants’ perceptions of PACS and prevented staff from using the system. Some of the perceived barriers found in this study support findings from previous studies conducted in Saudi Arabia. A number of participants identified low-speed network connections as a barrier to PACS use. Alalawi et al similarly reported repeated interruptions in the system.4 Furthermore, clinicians from King Fahad Teaching Hospital outpatient clinic (n = 6) reported that they did not receive sufficient training, as did participants in Alalawi et al’s study.4 Conversely, Aldosari et al found that 77% of participants in their study received PACS training.20 A number of participants in our study cited costly maintenance and system upgrades as a disadvantage of PACS. Although studies have shown that PACS is cost effective,5,7 the rapid changes innovative technologies undergo increase their cost.5 Other disadvantages reported were loss of data because of lack of data backup and disruptive technical problems. Participants from Arrawdha Hospital further cited insufficient integration of the system with patient records. This disadvantage was revealed in a previous study conducted in Iran, which showed that PACS has not fully met all the demands of physicians and has not achieved its predetermined objectives in some healthcare centers, such as all-access from different locations.15
The disadvantage of the ever-diminishing face-to-face contact, discussions, and learning between radiologists and their ordering colleagues on behalf of improving patient care that used to routinely occur before the advent of PACS was not perceived during the data collection of this study. In contrast, the result of this study showed that PACS was perceived to have a benefit of enabling participants to communicate with branches of the hospital in other cities and allowed remote consultations. Thus, participants are sensing the benefit of PACS and favor the work from distance through any type of devices, such as computers and mobile phones. Therefore, with the advancement of technology, people favor working from distance through different types of devices. Today, clinicians and specialists desire immediate access to imaging studies from the hospital and at home 24 h a day, 7 days a week, on computers running all operating systems and mobile devices.21 Health strategic planners should consider users' requirement and need of implementing PACS systems that are integrated with other health information systems, which can be accessed at any time from any place and through different types of devices, to increase the quality of healthcare.
Participants’ main recommendations included providing remote web-based access to PACS and installing a PACS mobile application for viewing images, regularly backing up data to avoid data loss, and providing higher network connection speed. The theoretical model, developed based on study results, further contributes to identifying areas of improvement for effective PACS implementation in hospital settings.
The theoretical model identifies three key factors that affected clinicians’ perceptions and use of PACS: demographic, system-related, and hospital-related factors. User’s acceptance of the system is key to its successful implementation.4 Demographic factors included their professional rank and clinical expertise. Similar to the findings in Alalawi et al’s study, in this study, the perceptions of radiologists and consultants in the radiology department were more positive compared to clinicians who worked in outpatient clinics.4 System-related factors included internet speed, system’s ease of use, quality of images, web-based factors, integration in the hospital workflow, and system auto-backup. Finally, hospital-related factors included system maintenance and upgrade costs, infrastructure, and support, including training. Mansoori et al’s study of the implementation of PACS in a health system in Northern Ohio found that system-related factors (ie, internet network upgrades and integration into hospital workflow) and hospital-related factors (ie, infrastructure upgrades, budget allocation, and support) are key to successful PACS implementation.7 Our study did have one limitation that the sample size was very small (n = 18); as such, the generalizability of the study findings is limited. Further research is required to determine the applicability of the study findings to a larger sample in a hospital setting in Saudi Arabia and beyond.
Conclusion
Clinicians’ acceptance of PACS is key to the successful implementation of the system; their acceptance is affected by the perceived advantages and disadvantages of the system and its use. The theoretical model developed in this study identifies three key factors that influence clinicians’ perceptions: demographic, system-related, and hospital-related factors. These factors can help identify areas of improvement for effective PACS implementation in hospital settings.
Ethics Approval and Informed Consent
Ethical approval was obtained from the Institutional Review Board, Office of Vice President for Research and Higher Studies at Imam Abdulrahman bin Faisal University (Reference number IRB-UGS-2018-03-020). All participants provided informed consent in writing prior to their participation in the study. This study was conducted in accordance with the Declaration of Helsinki.
Acknowledgments
The authors would like to thank Enago (www.enago.com) for the English language review.
Author Contributions
All authors have made a significant contribution to the work reported, whether that is in the conception, study design, execution, and data acquisition, analysis, and interpretation. Authors participated in drafting, revising, or critically reviewing the article; approved the final version to be published; agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
The authors declare that there is no funding relevant to this work.
Disclosure
The authors have no conflicts of interest to declare.
References
1. Hains IM, Georgiou A, Westbrook JI. The impact of PACS on clinician work practices in the intensive care unit: a systematic review of the literature. J Am Med Inform Assoc. 2012;19(4):506–513. doi:10.1136/amiajnl-2011-000422
2. SearchHealth IT. What is PACS (picture archiving and communication system)?—Definition. WhatIs.com [online]; 2017. Available from: http://searchhealthit.techtarget.com/definition/picture-archiving-and-communication-system-PACS.
3. Buabbas AJ, Al-Shamali DA, Sharma P, Haidar S, Al-Shawaf H. Users’ perspectives on a Picture Archiving and Communication System (PACS): an in-depth study in a teaching hospital in Kuwait. JMIR Med Inform. 2016;4(2):e21. doi:10.2196/medinform.5703
4. Alalawi ZM, Eid MM, Albarrak AI. Assessment of picture archiving and communication system (PACS) at three of ministry of health hospitals in Riyadh region—content analysis. J Infect Public Health. 2016;9(6):713–724. doi:10.1016/j.jiph.2016.09.004
5. Alhajeri M, Aldosari H, Aldosari B. Evaluating latest developments in PACS and their impact on radiology practices: a systematic literature review. Inform Med Unlocked. 2017;9:181–190. doi:10.1016/j.imu.2017.08.005
6. Aldosari B. User acceptance of a picture archiving and communication system (PACS) in a Saudi Arabian hospital radiology department. BMC Med Inform Decis Mak. 2012;12(1):44. doi:10.1186/1472-6947-12-44
7. Mansoori B, Erhard KK, Sunshine JL. Picture Archiving and Communication System (PACS) implementation, integration, and benefits in an integrated health system. Acad Rad. 2012;19(2):229–235. doi:10.1016/j.acra.2011.11.009
8. Hasani N, Hosseini A, Sheikhtaheri A. Effect of implementation of picture archiving and communication system on radiologist reporting time and utilization of radiology services: a case study in Iran. J Digit Imaging. 2020;33(3):595–601. doi:10.1007/s10278-019-00314-z
9. Nitrosi A, Borasi G, Nicoli F, et al. A filmless radiology department in a full digital regional hospital: quantitative evaluation of the increased quality and efficiency. J Digit Imaging. 2007;20(2):140–148. doi:10.1007/s10278-007-9006-y
10. Watkins J. A hospital-wide picture archiving and communication system (PACS): the views of users and providers of the radiology service at Hammersmith Hospital. Eur J Radiol. 1999;32(2):106–112. doi:10.1016/S0720-048X(99)00134-5
11. Hurlen P. Introducing information and communication technology to radiologists: impact on process and outcome; 2010. Available from: https://www.duo.uio.no/bitstream/handle/10852/27963/dravh-Hurlen.pdf?isAllowed=y&sequence=2.
12. Crowe B, Sim L. Implementation of a radiology information system/picture archiving and communication system and an image transfer system at a large public teaching hospital—assessment of success of adoption by clinicians. J Telemed Telecare. 2004;10(Suppl. 1):25–27. doi:10.1258/1357633042614339
13. Ahmadi M, Mehrabi N, Sheikhtaheri A, Sadeghi M. Acceptability of picture archiving and communication system (PACS) among hospital healthcare personnel based on a unified theory of acceptance and use of technology. Electron Phys. 2017;9(9):5325–5330. doi:10.19082/5325
14. Larson DB, Kruskal JB, Krecke KN, Donnelly LF. Key concepts of patient safety in radiology. RadioGraphics. 2015;35(6):1677–1693. doi:10.1148/rg.2015140277
15. Abbasi R, Sadeqi Jabali M, Khajouei R, Tadayon H. Investigating the satisfaction level of physicians in regard to implementing medical Picture Archiving and Communication System (PACS). BMC Med Inform Decis Mak. 2020;20:180. doi:10.1186/s12911-020-01203-0
16. Abdekhoda M, Salih KM. Determinant factors in applying picture archiving and communication systems (PACS) in healthcare. Perspect Health Inf Manag. 2017;14(Summer):1c.
17. Creswell J. Research Design. Thousand Oaks, CA: SAGE; 1994.
18. Glaser B. Basics of Grounded Theory Analysis: Emergence vs. Forcing. Mill Valley, CA: Sociology Press; 1992.
19. Smith J, Harré R, Langenhove L. Rethinking Methods in Psychology. London: SAGE; 1996.
20. Aldosari H, Saddik B, Al Khadi K. Impact of picture archiving and communication system (PACS) on radiology staff. Inform Med Unlocked. 2018;10:1–16. doi:10.1016/j.imu.2017.11.001
21. Berkowitz SJ, Wei JL, Halabi S. Migrating to the modern PACS: challenges and opportunities. Radiographics. 2018;38:1761–1772. doi:10.1148/rg.2018180161
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
