Back to Journals » Neuropsychiatric Disease and Treatment » Volume 15
Clinical factors influencing resilience in patients with anorexia nervosa
Authors Kane C , Tomotake M, Hamatani S, Chiba S, Kameoka N, Watanabe S, Nakataki M , Numata S, Ohmori T
Received 13 October 2018
Accepted for publication 26 December 2018
Published 30 January 2019 Volume 2019:15 Pages 391—395
DOI https://doi.org/10.2147/NDT.S190725
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Taro Kishi
Chikako Kane,1 Masahito Tomotake,2 Sayo Hamatani,3 Shinichi Chiba,2 Naomi Kameoka,4 Shinya Watanabe,4 Masahito Nakataki,4 Shusuke Numata,4 Tetsuro Ohmori4
1Department of Nursing, Tokushima University Hospital, Tokushima-shi, Tokushima, Japan; 2Department of Mental Health, Institute of Biomedical Sciences, Tokushima University Graduate School, Tokushima-shi, Tokushima, Japan; 3Research Center for Child Mental Development Chiba University, Chuouku, Chiba, Japan; 4Department of Psychiatry, Institute of Biomedical Sciences, Tokushima University Graduate School, Tokushima-shi, Tokushima, Japan
Purpose: This study was to elucidate clinical factors influencing resilience in anorexia nervosa (AN) patients.
Patients and methods: Twenty female patients with AN (median age =30.0 years, quartile deviation =6.8) and 40 female healthy controls (HCs) (median age =30.0 years, quartile deviation =8.6) participated in the present study. Resilience was assessed with the Connor–Davidson resilience scale (CD-RISC). Clinical symptoms were evaluated with the structured interview guide for the Hamilton depression rating scale (SIGH-D) and the eating disorder inventory-2 (EDI-2).
Results: Scores of the CD-RISC in the AN group were lower than those in the HC group, and the SIGH-D score in the AN group was higher than that in the HC group. Scores of interoceptive confusion, interpersonal difficulty and negative self-image subscales of the EDI-2 negatively correlated with the CD-RISC score. Moreover, stepwise regression analysis showed that negative self-image score was an independent predictor of the CD-RISC score.
Conclusion: These results suggest that among these clinical factors including psychopathologies, self-dissatisfaction and feeling of being rejected by others are the most important influencing factors on an AN patients’ resilience.
Keywords: anorexia nervosa, resilience, influencing factor, negative self-image
Introduction
Recently, resilience has been paid attention to in the field of psychiatry because it is considered to be related to psychopathological process.1 Resilience is defined as “the process of adapting well in the face of adversity, trauma, tragedy threats or even significant sources of stress”2 and reflects the ability to maintain a stable equilibrium.3 The concept of resilience includes rebound from adversity.2,4 Moreover, it is said that resilience is a protective factor against development of mental disorders.5 Conner and Davidson reported that resilience might be viewed as measure of stress coping ability and could be an important target of treatment in anxiety, depression and stress reaction such as posttraumatic stress disorder.6 A previous study revealed that resilience negatively correlated with negative indicators of mental health and positively did with positive indicators of it.1 Furthermore, a previous study described that schizophrenia and bipolar disorder patients showed a lower level of resilience than healthy people.7 As for eating disorders, it was reported that resilience predicted improvement in psychological health and social relationship domains of quality of life and reduction of eating disorder symptoms over time.8
Among eating disorders, anorexia nervosa (AN) is well known to be difficult to treat, with many patients remaining ill for years, and patients with AN are reported to suffer from physical, psychological and social problems as a result of the disease.9,10 Preferably, the treatment goal should be full remission of symptoms, but it is often difficult to achieve it in the treatment of AN. Therefore, in addition to symptom reduction, therapists should pay attention to more global indicators such as quality of life and resilience to know patients’ recovery status. As for quality of life of AN patients, researchers reported that some clinical factors such as low body mass index (BMI) and the depressive symptoms were predictors of low quality of life.10–19 However, as there are few studies investigating AN patients’ resilience and its relation to other clinical factors, clinical factors influencing AN patients’ resilience is unclear. In the present study, we hypothesized that some clinical factors such as low BMI, depressive symptoms and eating psychopathology are associated with AN patients’ low resilience.
Methods
Subjects
Clinical data were collected at Department of Psychiatry, Tokushima University Hospital from 1 March 2016 to 30 June 2017. Subjects consisted of 20 female outpatients having a Diagnostic and Statistical Manual of Mental Disorders-520 diagnosis of AN (restricting type =10, binge-eating/purging type =10) and age- and education level-matched 40 female healthy controls (HCs). Patients were excluded if they presented with any organic central nervous system disorder, severe somatic disorder, substance dependence, epilepsy or mental retardation. Of 23 outpatients to whom we explained the research, 20 agreed to participate in the study, and as for HCs, subjects were excluded if they had a history of any psychiatric illness or if their BMI was not within normal range (18.5–24.9).21 We recruited HCs from staff and students at Tokushima University. All subjects were native Japanese speakers and gave us written consent to participate in the study.
Measures
Subjects were examined using the following measures.
- The structured interview guide for the Hamilton depression rating scale (SIGH-D)
Depressive symptoms were evaluated by experienced clinical researchers with Japanese version of the SIGH-D.22,23 The SIGH-D was constructed to standardize the manner of administration of the Hamilton depression rating scale. The Japanese version is reported to have a good reliability and validity.24 In the present study, we used the 21-item version. Higher scores indicate severe depression. - Eating disorder inventory-2 (EDI-2)
The EDI-225,26 is a self-report questionnaire designed to provide a comprehensive assessment of the behavioral and psychological characteristics of eating disorder patients. From the result of factor analysis, it is reported that the Japanese version consists of nine factors.25 The nine factors are as follows: drive for thinness, body dissatisfaction, bulimia, interoceptive confusion, interpersonal difficulty, negative self-image, compulsion for control, impulse regulation and maturity fears. The scoring method is based on Garner’s rationale26 and higher score of this scale indicates more severe AN symptomatology. The reliability and validity of the Japanese version is already confirmed.25 - The Connor–Davidson resilience scale (CD-RISC)
The CD-RISC6 was developed as a short self-report assessment to quantify resilience and to assess treatment response as a clinical measure. This 25-item scale uses a 5-point response scale and the total score ranges from 0 to 100, with higher scores reflecting greater resilience. The reliability and validity of the Japanese version is already confirmed.27
Statistical analysis
Data analysis was done using the predictive Analytics Software Statistics 22 software (IBM Corporation, Armonk, NY, USA). Since several data showed non-normal distribution, we chose the Mann–Whitney U test to compare age, length of education, BMI, the SIGH-D score and the CD-RISC score between AN and HC groups. And r(Z/√N) was calculated to provide effect sizes.28 Then, Spearman rank correlation coefficients were calculated to explore the relationship between the CD-RISC and other clinical variables for the AN group. Statistical significance was adjusted for multiple comparisons (false discovery rate correction).29 Subsequently, choosing the CD-RISC score as a dependent variable and the clinical variables that showed significant correlations with the CD-RISC score as independent valuables, forward stepwise regression analysis was performed to investigate which clinical variables would significantly predict the dependent variable.
Ethical considerations
This study was approved by the Clinical Research Ethics Committee of Tokushima University Hospital and was conducted in accordance with the Helsinki Declaration.30
Results
The demographic and clinical characteristics of the AN and HC groups are shown in Table 1. There was no significant difference in age and length of education between the two groups. The AN group showed significantly lower BMI (U=77.0, P <0.0001, r= −0.65) and higher score in the SIGH-D (U=46.0, P <0.0001, r= −0.81) than the HC group, and the CD-RISC score (U=121.5, P <0.0001, r= −0.56) in the AN group was significantly lower than that in HC group. Correlations between the CD-RISC score and other clinical variables in AN group are shown in Table 2. The scores of interoceptive confusion (ρ= −0.669, P <0.01), interpersonal difficulty (ρ= −0.708, P <0.001) and negative self-image (ρ= −0.763, P <0.001) of the EDI-2 showed significant correlations with the CD-RISC score. Table 3 shows the result of stepwise regression analysis. The CD-RISC score was significantly predicted by the EDI-2 negative self-image score.
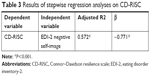  | Table 3 Results of stepwise regression analyses on CD-RISC |
Discussion
Among eating disorders, AN is well known to have relatively poor prognosis.31,32 As for quality of life in AN patients, previous researchers reported their lowered quality of life.16–18 Our research group also investigated quality of life in AN patients and obtained similar results.19 In the recent study, it was reported that self-adaptability/resilience could be regarded as one of the important criteria for eating disorder recovery.33 Therefore, we consider that investigating AN patients’ resilience is obviously crucial. As far as we know, there is no study on clinical factors influencing their resilience; our main goal in this study was to elucidate the predictors of their resilience.
In the present study, as expected, resilience level of the AN group was significantly lower than that of the HC group, and the subsequent correlation analysis for the AN group revealed that certain eating disorder psychopathologies were associated with low resilience level, but surprisingly, we found no significant correlation between resilience and other clinical factors including depression, BMI, length of education, age of onset and duration of illness. Finally, the finding obtained through stepwise regression analysis clearly shows that eating disorder psychopathology of negative self-image has a strong negative impact on AN patients’ resilience level. Negative self-image subscale of the EDI-2 consists of five items25 as follows; “I feel good about myself”, “I feel that I am a good person”, “I feel that I am as good as most people”, “I think other people like me”, “I know that people love me”. As these items are intended to check how much feeling of self-dissatisfaction and being rejected by others the person has,25 these kinds of negative thoughts are considered to have strong effect on AN patients’ resilience level.
As for the resilience of eating disorder patients, Las Hayas et al reported that women recovered from eating disorders gave retrospective accounts that their life seemed chaotic and they felt strained when interacting with other people, and agreed that resilience was generated at a point when they felt deeply dissatisfied with life.34 Another study revealed that resilience factors predicted improvements in psychological health and social relationship aspects of quality of life.8 Although these studies provided important findings about eating disorder patients’ resilience, their subjects included different types of eating disorder patients, and they did not focus on factors influencing their resilience level. Therefore, our findings obtained from AN patients are considered crucial in this area of research.
Considering these results, we could suggest that self-dissatisfaction and social insecurity should be paid attention to as a treatment target to enhance AN patients’ resilience level. To date, researchers have reported that low resilience might be a risk factor of mental disorders,4 and high resilience could help improve their mental conditions.35 Therefore, our findings may contribute to treatment of AN patients through enhancing their resilience.
Limitations
This study has some limitations. First, as this study was a cross-sectional one, we can only guess at the developmental causality. Second, since the sample size was small, further study with a larger sample size would be required to confirm the results. Third, AN patients’ response to the self-report questionnaire might have been influenced by their denial of negative aspects.36
Conclusion
The results suggest that self-dissatisfaction and feeling of being rejected by others are especially crucial influencing factors on AN patients’ resilience level.
Acknowledgment
The authors should like to thank all subjects for participating in this study.
Disclosure
The authors report no conflicts of interest in this work.
References
Hu T, Zhang D, Wang J. A meta-analysis of the trait resilience and mental health. Pers Individ Dif. 2015;76:18–27. | ||
American Psychological Association. The Road to Resilience. Washington, DC: American Psychological Association; 2014. | ||
Bonanno GA, Loss BG. Loss, trauma, and human resilience: have we underestimated the human capacity to thrive after extremely aversive events? Am Psychol. 2004;59(1):20–28. | ||
Bozikas V, Parlapani E. Resilience in patients with psychotic disorder. Psychiatriki. 2016;27(1):13–16. | ||
Shrivastava A, Desousa A. Resilience: a psychobiological construct for psychiatric disorders. Indian J Psychiatry. 2016;58(1):38–43. | ||
Connor KM, Davidson JR. Development of a new resilience scale: the Connor–Davidson resilience scale (CD-RISC). Depress Anxiety. 2003;18(2):76–82. | ||
Deng M, Pan Y, Zhou L, et al. Resilience and cognitive function in patients with schizophrenia and bipolar disorder, and healthy controls. Front Psychiatry. 2018;9:279. | ||
Calvete E, Las Hayas C, Gómez del Barrio A. Longitudinal associations between resilience and quality of life in eating disorders. Psychiatry Res. 2018;259:470–475. | ||
Bamford B, Barras C, Sly R, et al. Eating disorder symptoms and quality of life: where should clinicians place their focus in severe and enduring anorexia nervosa? Int J Eat Disord. 2015;48(1):133–138. | ||
Abbate-Daga G, Facchini F, Marzola E, et al. Health-related quality of life in adult inpatients affected by anorexia nervosa. Eur Eat Disorders Rev. 2014;22(4):285–291. | ||
Pollack LO, McCune AM, Mandal K, Lundgren JD. Quantitative and qualitative analysis of the quality of life of individuals with eating disorders. Prim Care Companion CNS Disord. 2015;17(2). | ||
Muñoz P, Quintana JM, Las Hayas C, Aguirre U, Padierna A, González-Torres MA. Assessment of the impact of eating disorders on quality of life using the disease-specific, health-related quality of life for eating disorders (HeRQoLED) questionnaire. Qual Life Res. 2009;18(9):1137–1146. | ||
Pohjolainen V, Koponen S, Räsänen P, Roine RP, Sintonen H, Karlsson H. Long-term health-related quality of life in eating disorders. Qual Life Res. 2016;25(9):2341–2346. | ||
Mitchison D, Hay P, Mond J, Slewa-Younan S. Self-reported history of anorexia nervosa and current quality of life: findings from a community-based study. Qual Life Res. 2013;22(2):273–281. | ||
Weigel A, König HH, Gumz A, Löwe B, Brettschneider C. Correlates of health related quality of life in anorexia nervosa. Int J Eat Disord. 2016;49(6):630–634. | ||
Bamford B, Sly R. Exploring quality of life in the eating disorders. Eur Eat Disorders Rev. 2010;18(2):147–153. | ||
González-Pinto A, Inmaculada F, Cristina R, et al. Purging behaviors and comorbidity as predictive factors of quality of life in anorexia nervosa. Int J Eat Disord. 2004;36(4):445–450. | ||
Hamatani S, Tomotake M, Takeda T, et al. Influence of cognitive function on quality of life in anorexia nervosa patients. Psychiatry Clin Neurosci. 2017;71(5):328–335. | ||
Kane C, Tomotake M, Hamatani S, Chiba S, Ohmori T. Clinical factors influencing quality of life in anorexia nervosa patients. Open J Psychiatr. 2018;08(01):50–60. | ||
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Association; 2013. | ||
Who Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. The Lancet. 2004;363(9403):157–163. | ||
Williams JB. A structured interview guide for the Hamilton depression rating scale. Arch Gen Psychiatry. 1988;45(8):742–747. | ||
Nakane Y, Williams JBW. Japanese version of structured interview guide for the Hamilton depression rating scale (SIGH-D). Jpn J Clin Psychophrmacol. 2003;6:1353–1368. Japanese. | ||
Narita T, Kim T, Nakane Y, Ozaki N. Reliability and validity of structured interview guide for the Hamilton depression rating scale (SIGH-D). Jpn J Clin Psychophrmacol. 2003;6:72–82. Japanese. | ||
Shimura M, Horie H, Kumano H, Sakano Y, Suematsu H. Reliability and validity of a Japanese version of the eating disorder inventory. Psychol Rep. 2003;92(1):131–140. | ||
Garner DM. Eating Disorder Inventory-2: Professional Manual. Odessa, FL: Psychol Assess Res. Inc; 1991. | ||
Ito M, Nakajima S, Shirai A, Kim Y. Cross-cultural validity of the Connor–Davidson scale; data from Japanese population. Poster presented at 25th Annual Meeting, International Society of Traumatic Stress Studies, Atlanta, GA, November, 2009. | ||
Field A. Discovering Statistics Using SPSS. 2nd ed. London: SAGE Publications; 2005. | ||
Matsuda S. Introduction of FDR and comparisons of multiple testing procedures that control it. JJB. 2008;29(2):125–139. Japanese. | ||
World Medical Association [webpage on the Internet]. WMA Declaration of Helsinki – Ethical Principles for Medical Research Involving Human Subjects. Available from: https://www.wma.net/policies-post/wma-declaration-of-helsinki-ethical-principles-for-medical-research-involving-human-subjects/. Accessed February 20, 2016. | ||
Andrade R, Gonçalves-Pinho M, Roma-Torres A, Brandão I. Treatment of anorexia nervosa: the importance of disease progression in the prognosis. Acta Med Port. 2017;30(7–8):517–523. | ||
Jagielska G, Kacperska I. Outcome, comorbidity and prognosis in anorexia nervosa. Psychiatr Pol. 2017;51(2):205–218. | ||
de Vos JA, Lamarre A, Radstaak M, Bijkerk CA, Bohlmeijer ET, Westerhof GJ. Identifying fundamental criteria for eating disorder recovery: a systematic review and qualitative meta-analysis. J Eat Disord. 2017;5(1):34. | ||
Las Hayas C, Padierna JA, Muñoz P, et al. Resilience in eating disorders: a qualitative study. Women Health. 2016;56(5):576–594. | ||
Ghanei Gheshlagh R, Sayehmiri K, Ebadi A, et al. The relationship between mental health and resilience: a systematic review and meta-analysis. Iran Red Crescent Med J. 2017;19(6):e13537. | ||
de Houwer J. The implicit association test as a tool for studying dysfunctional associations in psychopathology: strengths and limitations. J Behav Ther Exp Psychiatry. 2002;33(2):115–133. |
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


