Back to Journals » Journal of Multidisciplinary Healthcare » Volume 13
Challenges of Clinical Nursing Training Through Internship Approach: A Qualitative Study
Authors Ahmadi S , Abdi A , Nazarianpirdosti M , Rajati F , Rahmati M , Abdi A
Received 15 April 2020
Accepted for publication 14 July 2020
Published 7 September 2020 Volume 2020:13 Pages 891—900
DOI https://doi.org/10.2147/JMDH.S258112
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Sharare Ahmadi,1 Alireza Abdi,2 Mohammad Nazarianpirdosti,1 Fatemeh Rajati,3 Mahmoud Rahmati,2,3 Arsalan Abdi1
1Student Research Committee, Kermanshah University of Medical Sciences, Kermanshah, Iran; 2Nursing and Midwifery School, Kermanshah University of Medical Sciences, Kermanshah, Iran; 3Research Center for Environmental Determinants of Health, Health Institute, Kermanshah University of Medical Sciences, Kermanshah, Iran
Correspondence: Alireza Abdi
Nursing and Midwifery School, Kermanshah University of Medical Sciences, Kermanshah, Iran
Email [email protected]
Background: Nursing education programs are designed to decrease the gap between theory and practice. It is believed that internship programs can decrease this gap. An internship program has newly been implemented in Kermanshah Nursing School. However, the efficiency of this program has not been assessed. Therefore, the aim of the present study was to explore the challenges related to the internship education of nursing students.
Methods: The study was conducted as qualitative research. The participants were eight nursing students who had at least one semester of experience in internship. They were selected through purposive sampling. Data gathering was done through semi-structured interviews, which were recorded and analyzed through a three-stage content analysis approach. For data management, MAXQDA-10 was used.
Results: Out of the eight participants, three were male, and all were in the final year of their education. In total, 423 primary codes emerged after analyses, which were placed in seven categories, including: education before internship, lack of support, planning difficulties, interaction with staff, invisible evaluation, welfare defects, and professional identity.
Conclusion: The study revealed the challenges of the internship program for nursing students in Iran. Some of the problems were related to educational background, others were associated with the shortcomings of the cultural aspects of the context. Therefore, it is recommended to optimize the clinical training of nursing students in the internship program by addressing these challenges.
Keywords: nursing, clinical education, clinical competency, internship
Background
Nursing is a profession that provides fundamental care to patients, and nurses have to deal with sophisticated and specialized conditions. In order to provide optimal care, nurses need sound theoretical knowledge and perfect practical skills. Research in different countries and ongoing evidence demonstrate a theory–practice gap in nursing.1 In fact, nursing education should encompass three areas of learning: cognitive, emotional, and psychomotor.2 Newly graduated nurses are not ready and confident to enter advanced stages of clinical competence or to enter into the clinical field. According to a systematic review in 2015, the main reason for this problem is the allocation of insufficient time for clinical practice. So, the gap between theoretical issues and clinical practice among nurses remains wide open.3
There are a few programs designed to create a bridge between theory and clinical practice in nursing education. Various approaches have been proposed to address this gap; some researchers have emphasized that simulators are a flexible approach.4 Dadgaran et al argued that theoretical content is a higher priority than clinical practice, and proposed using case reporting and ongoing review in instructional curricula.5 Moreover, Jackson et al (2016) showed that the best way to reduce the gap between theory and practice is to create more opportunities for observation and learning in the clinical setting and engage students in interpersonal communications.6 Having a close connection with clinical settings develops clinical reasoning, critical appraisal, and problem-solving abilities.7
The internship in clinical education is one of the important approaches to reduce the gap between theoretical and practical knowledge.8 This strategy is implemented in the final year of education. This practice was first used during the late 19th century in the United States to prepare medical students for post-graduation clinical practice and create maturity in medical students.9 Internship is a process in which students gain practical experience under the supervision of a faculty member accompanied by experienced nurses, head nurses, and hospital supervisors.10
It is thought that internship programs have some benefits for students (by engaging in real clinical situations), workplaces, and the staff (assigning some clinical tasks to students). It also initiates creativity and adaptability, greater opportunity to learn skills, increases analytical power, and eventually yields job experience.11 Furthermore, internship programs for nursing students improve the readiness for accepting roles and enhance individual and professional abilities,12,13 self-development, and work commitment.14,15 Conversely, some studies have noted that internship has little effect on beliefs about health problems such as mental health,16 and it may lead to health issues such as violence and anxiety.17
The internship program planned for nursing students, in connection with several Iranian universities, was commenced in Kermanshah University of Medical Sciences as a pilot plan (less than two years). At the initial stage, the students spend three days at an orientation workshop and received a booklet guide, then they are introduced to the education center of the hospital. The students are then referred to designated wards and work under the supervision of an expert nurse, head nurse, and supervisor (a faculty member of the school), who also does the final assessment. It is notable that the hospital also pays a monthly salary to the students. Given the lack of studies on the efficiency and challenges of the program, the present study aimed to explore the challenges related to the internship education of nursing students.
Methods
Study Approach
This study was conducted as a qualitative content-analysis work in 2018. Qualitative studies originate from the naturalistic paradigm in which knowledge emerges from researcher–participant interactions.18 In content analysis, as one of the approaches of qualitative research, the researcher reaches a deep understanding of the concepts relevant to the topic of interest and the codes and sentences are systematically subdivided into categories. Through this, the phenomenon is easily understandable through constructing a conceptual model or map.19 Content analysis is applied in both inductive and deductive methods. In the former, there is little information about the phenomenon, while the latter is undertaken on the previous theories or models.19 Inductive content analysis was adopted because there is a lack of evidence about students’ experience of the clinical education approach through internship. Content analysis involves three stages of analysis: preparation, organizing, and reporting.19,20
Research Population
The research population included all nursing students in the internship program. The inclusion criteria were passing at least one semester of internship and desire to cooperate in the study. The participants were selected purposefully and the sample size was determined based on data saturation. Saturation means having sufficient data (not complete).21 Data saturation has to be confirmed by at least two researchers. The researchers must be convinced that no new codes (information) can be found.22 In this study, the saturation was met after seven interviews; however, to be on the safe side, one more interview was performed.
Data Collection
For data collection, permission was secured from the Research and Technology Vice-Chancellor of Kermanshah University of Medical Sciences (KUMS). Afterwards the researcher referred to the educational hospitals affiliated with KUMS and briefed the participants about the objectives of the study and assured them about the anonymity and confidentiality of their personal information. The participants signed a written informed consent. Semi-structured interviews were conducted with the participants using open questions such as: What are your opinions about internship? What are the pros and cons of this program? Explain your experiences with clinical working in internship. In addition, probing questions (e.g. why? How? Explain more, and give an example) were used for more clarification.
Data Analysis
The interviews lasted about 30 to 90 minutes and were recorded by a cell phone and transcribed verbatim. The semantic units were determined during the preparation phase. For this purpose, the written files were read several times and the sentences and matched codes were determined. In the organizing stage, the extracted codes from the previous stage were consistently compared and categories emerged. After naming the categories, the concept map was determined.
Trustworthiness
The rigor of data was ensured via considering the Guba and Lincoln’s criteria. For credibility, some measures such as long-term engagement and continuous observation by the researcher, use of duplicate questions to assure sample responses, and review of codes and categories by research colleagues (peer debriefing) and participants (member check) were implemented. Dependability of the data was addressed by giving a detailed account of how data were collected, specific measures implemented during the research process, taking notes, data analyses, and determining categories. Through this, external auditors can examine the process. Additionally, to facilitate external audit, the research process was explained thoroughly to ensure confirmability. Eventually, the results were provided to three nursing students in another context, who did not participate in the study, for check transferability. Their experiences were compared with our results and consistency was confirmed.23 The data were managed in Maxqda-10 software.
Results
Out of the eight participants, three were male and five were female. They all were undergraduate nursing students (Table 1). A total of 423 initial codes were extracted from the analysis, and seven categories emerged that depicted the challenges of the internship program. The seven categories are “education before internship,” “lack of support,” “planning difficulties,” “interaction with staff,” “invisible evaluation,” “welfare defects,” and “professional identity” (Table 2, Figure 1).
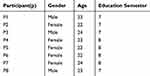 |
Table 1 The Characteristics of the Nursing Students with Internship Program |
 |
Table 2 Categories and Examples of Quotations |
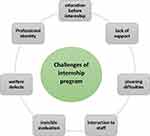 |
Figure 1 Conceptual model of the challenges of the internship program. |
Education Before Internship
The students declared that most of the educational content was expressed theoretically within the pre-internship semesters. They regarded this as a serious challenge to entering the internship. The participants merely reviewed the scientific materials with no chance to employ them directly in practice. The education courses were completed by only observing the clinical procedures rather than practicing them. In this regard, one participant commented on the pre-internship period:
I was not satisfied with the previous six semesters [...] we had only seen suction [as one of the nursing procedures] in the textbooks and it was for the first time in the internship that we used the suction device. These fields are very flawed [...] about CPR, which is very important, we only had it in the sixth semester in the ICU (critical care credit) [...] All we had was theory. Just imagine that the students had problems implemented CPR when a patient was coding [needed CPR]. [P7].
The students considered the internship plan as a way to cover the weaknesses of the previous educational terms. In this regard, a student said:
The plan is good for me. I was a top student in theoretical course; however, I have stress of practical work because the teachers didn’t allow to do practical work. We have had a little training time, 8 to 12 [am] and most of it was dedicated to teaching the theory. [P2]
Before entering the internship, the students should pass the final exam. This is considered as a way to make the student review the theoretical contents of the previous semesters. In this regard, one of the participants stated: “This final (exam) helped us a lot in the internship. If they (teachers) took it at the end of the eighth semester, it would not be useful for us anymore. But because it was at the end of the sixth semester, we reviewed the basics once more.” (P1). Another student mentioned that:
The final was very good; for example, the exercises we did for intubation helped us a lot. I didn’t really remember anything about bandage, but when we practiced for the final, I remembered everything. [P3]
Lack of Support
Students complained about the lack of a support system for resolving conflicts with staff, handling complaints, and insurance for nursing errors. They were often confused about how to express their problems, and worried about possible errors that might be happened. They also had concerns about insurance and supportive institution. Participant 1 remarked:
The nurse is afraid to leave the patient to the student independently to manage. Because if there is a problem for the patient, it is the nurse that is responsible, not me as a student. I have no money to pay as diyat [blood money]. There is a need for some kind of insurance for us. [P1]
In this regard, another student added “If something goes wrong in the ward, they all would blame the students, so I was very anxious and obsessed with this issue” (P8). Some students complained about the inappropriate behaviors of nurses and caregivers, noting that they were unable to resolve their conflicts reasonably with them. Therefore, they had to work in any circumstances. One of the participants said:
By the way, I told the students that if we had to say anything or protest now, they [the supervisors] would give us a reason. For example we asked [the supervisor] for help, and they replied that the head nurse has his own morals and tastes that he treats you this way, and we cannot change her, we say something, and we have to say nothing …. There was an observer in each hospital from the faculty, but students did not see them as a good support. Some of the observers were always absent and did not have any idea of the students’ problem. [P5]
Planning Difficulties
There were criticisms about the planning, the number of students and staff, the length of work shifts, and training programs in the internship. Some students believed that the number of work shifts was too high so that they had neither time to review the content nor the opportunity to update the information for the postgraduate exam. In this regard, the sixth participant stated:
One of the disadvantages of the internship was that it took all our time to study for a master’s degree because the work shifts did not allow us to spend time studying. Let’s read (the shift schedule), but if the time was the same as before, for example, we were in the mornings until twelve [o’clock] and in the evenings until four or five (it was better), and this makes us not have a master’s degree or very little in our next courses. [P6]
Some participants noted that there was a need for a brief meeting for the staff, because they were unfamiliar with this program. The second participant stated that:
When we went in the morning shift, we took the statistics of all the dressings, we checked all the angio-catheters, we both checked the trolley [CPR trolley), and it took up to half past ten [o’clock] to do this. Because the time of administering medicine was 11:30, there was no work in the ward until then and we left to rest, head nurse and nurses shouted that why you entered the staff’s rest room, the students have no right to rest! …, but we did all the works of ward. [P2]
The students suggested that the focus of the program should be on learning all the tasks of the department, not only doing simple and routine works. For example, working with the hospital information system (HIS) and reporting and delivering the patients were the tasks that nurses barely allowed the students to do.
Interaction to Staff
There were some positive and negative comments on the interaction with staff; the positive comments about the fact that the nurses did not treat internship students like other students in the lower semesters and looked at them as colleagues and treated them with respect. On the other hand, some of the students figured that the nurses would treat them like students and even worse, so they were unable to interact well with the staff. Participant No. 1 had a positive comment:
In previous clinical trainings, they [teachers] said [the students should be at work] from Saturdays to Wednesdays, so-and-so [which] hospital or wards should come to your work, but [in the internship] it was very good to be allowed to sit in the internship with our supervisor and arrange shifts. I was busy afternoon or I couldn’t go on Wednesday morning, I could easily modify my shifts, so it was very good. [P1]
The second student also indicated the staff’s positive interaction with them:
The difference [with previous trainings] is that in internships the student interacts better with the staff. For example, some of them said go for a break in the evenings. [P2]
In relation to the negative experiences of students in dealing with the personnel, P4 mentioned:
They do not let us a moment to sit down, if we did, they would overwhelm us with a lot of work … Some nurses and the staff have friendly attitudes, but some do not … Supervisors did not cooperate with us in picking the work shifts, and if we had a problem with a shift, they would not agree to change it, even when there was a good reason. [P4]
Invisible Evaluation
The evaluation system was based on the cumulative opinions of the faculty, hospital supervisors and head nurses’ assessments. The students declared that the supervisors and head nurses did not have full control over students’ work. The fact that the evaluation score was given by a supervisor and head nurse could be used as a tool for abusing students and assigning repetitive tasks. The students requested another assessment system to include the remarkable contribution of nursing staff. The fourth student in connection with this defect stated that:
I didn’t have any problems with the internship, … and I went back and forth in time, and the nurses and patients were happy with me, so that one of the patients wrote my name to give to the nurse. He was happy with the way I treated him and provided him the care. But the head nurse gave me low grade and I asked her about how she gave me that score. She said, I would ask the nurses; but the nurses were all happy with me. I think she did this only because she did not like me. On the other hand, a student who had a very bad record either in theory and practice received 20 out of 20 [highest score]. [P4]
Another participant said:
Another drawback that I think is very important is that now the average score in the undergraduate program has an impact on admittance to an MSc program, and our score has now fallen into the hands of those who have no knowledge of our theoretical and clinical capabilities. They don’t know at all who and how cares about the patient, and I, who am circle around the patient [do appropriate care for patient], and fully support the patient, my score of 16 is noted, because I had a challenge over something with the nurse. If [possible] the score has to be divided more correctly and it’s in the hands of someone who really knows us. [P5]
Welfare Defects
There were no dedicated facilities for students, such as a space for sleep, a locker room, and even extra chairs in the nursing station for students. Therefore, some of the students had to change their clothes in the dorm (it was near the hospital) and wear nursing dress outside of the hospital. They also had no safe place to leave their handbags or precious items. However, providing food was considered as an advantage. The first participant said:
They didn’t give us a locker to put things on it, there was no safe place to leave our precious stuff nor a place to sit in the nurse station. [P1]
Student No. 2 expressed:
It was good thing that they gave us food … Thank God, we didn’t have to night shifts, and we had the same nurses’ pavilion when we were alone[the morning and evening shifts]. However, but sometimes they would say don’t change your clothes here. It is not for yours. [P2]
Professional Identity
While the students worked as nurses during the internship, they only received student benefits. Therefore, there was a kind of identity ambiguity; whether they were staff or students. Most of the students were treated as students and did the nurses’ duties. This was a cause of dissatisfaction and obscured their identity. Participant No. 5 said:
The difference is that we came out of the teachers’ domination and became independent and work like a nurse. If we are a nurse, they should treat us like one, and if we are a student, they should treat us like a student!! [P5]
One of the students uttered:
When we protested that it was not our duty to take 40 vital signs, the nurse or head nurse told us not to protest, you are a student and you have to do your job, and we did it. I did know if we were a colleague or a student after all?! [P7]
However, some students compared their condition with previous semesters, and argued that their performance was more acceptable to patients and nurses. Furthermore, they covered the shifts like other nurses with the same schedule. They described these things as advantages. In this regard, one of the students stated that:
I was in neurosurgery ward, working with another nurse. I would go and sit in his room, I would talk to him, when I had a problem, they would easily change my shifts, and his attitude was great, and the staff never belittled the students. The head nurse told the staff not to let the student do such things easily … The attitude of the staff was better and even the attitude of the coaches was different. “The coaches handed their students [other students in lower semesters] over to us and said, “You’re with Mr. So-and-so who are interns”. [P8]
Discussion
In this study, the challenges related to the internship education of nursing students were examined. This program was held for the first time at Kermanshah University of Medical Sciences and neither the officials of hospitals nor the staff were fully familiar with its requirements and challenges. The primary challenge was linked to the students’ academic background. They expressed that during the pre-internship study, they were not taught in a practical way and most of the attention was on the theoretical content. It is well documented that the most important issue in nursing education was a delay in the learning process due to the gap between theory and practice.24 This causes difficulties for students to employ the information in the clinical arena. This gap or separation has created concerns for nursing students and teachers,25–27 which were frequently demonstrated in other similar studies.25,26,28–30 It is better if the materials are taught in a theoretical and practical way simultaneously. Teachers mostly concentrate on the theoretical part because there are a large number of students in each class (about 70 students). Consequently, the teacher has to assign a short time to a practical procedure for each student. Therefore, the students are deprived of practical lessons, which leads to more difficulties during the internship period.
Another challenge of the internship program was associated with the student support system. While the patient’s health is the major concern for students during the internship, an incomplete education or lack of organization between education and treatment could disturb the viewpoint of patients and society about nurses.31 In a study by Hassanpour et al on the process of formation of critical thinking in nursing education, insecurity and lack of support were the main threats to critical thinking.32 In addition, some studies argued that a one-year internship is short to develop self-management in nursing students.33 However, according to Walsh et al, a supportive supervision relationship was the main element in nursing learning.34 Owing to a paucity of support in the internship program, it seems that nursing students could not apply all their abilities. They were hampered when setting self-management support into practice through the internship.33
The students complained about the problems with planning and described it as a challenge. It is believed that the paradigm of nursing courses in Iran, unintentionally directs students to become a physician or physician assistant and not a nurse.31 In addition, clients are not considered as a whole within the nursing education program; the focus is on disease care instead of patient care.35 Another study reported about the high volume of non-practical content, predominantly medical, as a weakness of the nursing plan in Iran.36 Yazdannik et al also stated that students in the nursing education program were led to be “little doctors” instead of nurses.37 Apparently, all these reasons make nursing students suppose that their work is a routine task; therefore, the internship program in their view appears tedious, long, and of no educational value. There is a need to change the philosophical foundations of the nursing discipline in Iran, and also modify the expectations that systems have from nurses.
The findings signified that the students had interaction challenges with staff. This indicates that asuitable and interactive environment is essential for an optimized education.38 Furthermore, the clinical education of nursing students is indirectly affected by unsolved conflicts and oppositions between students and other health-care workers.27,39,40 Other researchers have concluded that employees’ conflicts and misbehaviors with students interrupt the process of clinical training.27,39 Moreover, as argued by Hanifi et al, the proper communication with students increases their motivation.41 Mohebbi Noubandegani et al disclosed the existence of discrimination between nursing students and other students in various fields (mostly medical)42 that may reduce learning desire. Whereas the literature affirms that students’ experiences during the internship could increase their communication skills with other members of the professional team.8 Although nursing students in the internship education may have no satisfactory organizational position,43 this issue can be solved along with continuing the program, and the system will benefit from the students’ work because of nurse staff shortage.
The students were dissatisfied with the evaluation process in the internship and complained about unfair grades given to students. This may demand crucial attentions to create more objective assessment tools. Alavi and Abedi emphasized that the lecturers should have the main role of evaluation of nursing students in clinical contexts.44 However, in this program, this role is delegated to head nurses and supervisors. Another study remarked on the need for an effective, transparent, and objective instrument for evaluation of clinical training.26 Conversely, some researchers believed that evaluation tools were not applicable for practical skills and have a lack of reliability and visibility.45–47 Willman advised that the similarity, stability, and fairness in the clinical evaluation of nursing students should be maintained.48
The students were unhappy with the welfare facilities and lack of a place for resting in the hospital. Regarding the role of internship students in clinical affairs, it is fundamental to provide better equipment to them such as access to hospital self-service and a decent space for changing clothes and resting, especially in night shifts.49 However, most of these are not feasible in Iranian hospitals because of the deficiency of space.
Identity challenge was another problem associated with the internship program. The students did not know whether they were students or staff. The main purposes of nursing schools are to ensure socialization and professional identity.37 However, literature shows, as a challenge, most of the nursing students do not achieve this.50 A study confirmed that the perception of professional identity would reduce students’ anxiety during the internship.51 Some researchers believe that a clear understanding of the nursing profession by students, and not following the medical model, may reduce the identity challenge in nursing students.36 While the students have a sense of identity problem during the internship, they may act much better after graduation compared to those who do not have this plan.
The internship program has been proven as the main way of creating a great opportunity for education, independence, expertise, proficiency, and confidence for nursing students.52,53 However, it has some pitfalls in Iran. Our results showed some clues about the challenges of the program, and by addressing these shortcomings, the efficacy can be improved. Future research can focus on other elements of internship programs such as satisfaction, expertise, and communication skills through qualitative and quantitative projects.
Limitation
Although the students accepted to participate in the study, they had a concern about criticizing the school and hospital organizations that might affect their final score. In this regard, the researcher made a strong assurance to them that all the interviews would be confidential and the anonymity of the personal information will be respected.
Conclusion
In this study, the challenges of the internship program for nursing students were examined. The students were not totally pleased with the clinical training within the previous semesters before the internship. They also highlighted some challenges including lack of amenities and a support system, interaction difficulties with staff, ambiguity in the evaluation system, and obscurity in identity. These problems should be addressed in the clinical education of nursing students.
Data Sharing Statement
Data are available by contacting the corresponding author.
Ethics Approval and Consent to Participate
The study is confirmed by the research ethics committee of Kermanshah University of Medical Sciences.
Consent for Publication
All the authors and the University consented to publish the study in your journal.
Acknowledgment
This study is based on a research plan approved by the Research and Technology Deputy of Kermanshah University of Medical Sciences (ID: 96233), and the Research Ethics Committee (ethical code: KUMS.REC.1396.230). We appreciate the nursing students who participated in this study.
Author Contributions
SA, AA, and MR performed the conceptual work and designed the study, SA and AA participated in data collection, and data were analyzed by AA, SA, FR, ARA, and MN. The final report and article were written, read, and approved by all the authors. All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors declare that they have no conflicts of interest in this work.
References
1. Cheraghi MA, Salsali M, Safari M. Ambiguity in knowledge transfer: the role of theory-practice gap. Iran J Nurs Midwifery Res. 2010;15(4):155.
2. Salsali M. Evaluating teaching effectiveness in nursing education: an Iranian perspective. BMC Med Educ. 2005;5(1):29. doi:10.1186/1472-6920-5-29
3. Monaghan T. A critical analysis of the literature and theoretical perspectives on theory–practice gap amongst newly qualified nurses within the United Kingdom. Nurse Educ Today. 2015;35(8):e1–e7. doi:10.1016/j.nedt.2015.03.006
4. Wall P, Andrus P, Morrison P. Bridging the theory practice gap through clinical simulations in a nursing under-graduate degree program in Australia. Int J Learn Teach Educ Res. 2014;8(1).
5. Dadgaran I, Parvizy S, Peyrovi H. A global issue in nursing students’ clinical learning: the theory–practice gap. Procedia Soc Behav Sci. 2012;47:1713–1718. doi:10.1016/j.sbspro.2012.06.888
6. Jackson A, Bluteau P, Furlong J. Interprofessional working in practice: avoiding a theory-practice gap. Int J Pract Based Learn Health Social Care. 2013;1:90–92.
7. Sezer H. How should clinical education be in nursing education? J Nurs Res Pract. 2018;2(1):15.
8. Wallace J. Nursing student work-study internship program: an academic partnership. J Nurs Educ. 2016;55(6):357–359. doi:10.3928/01484834-20160516-11
9. Wentz DK, Ford CV. A brief history of the internship. JAMA. 1984;252(24):3390–3394. doi:10.1001/jama.1984.03350240036035
10. Buckalew J. Internships for nurses. Home Healthcare Nurs. 1984;2(4):28–29. doi:10.1097/00004045-198407000-00009
11. Coco M. Internships: a try before you buy arrangement. SAM Adv Manage J. 2000;65(2):41.
12. Cooper C, Taft LB, Thelen M. Preparing for practice: students’ reflections on their final clinical experience. J Prof Nurs. 2005;21(5):293–302. doi:10.1016/j.profnurs.2005.07.002
13. Arguvanli S, Özkan B. Views of final year nursing students about internship in mental health and psychiatric nursing. J Psychiatr Nurs. 2016;7(1):13–17.
14. Esteves LSF, Cunha ICKO, Bohomol E, Santos MR. Clinical supervision and preceptorship/tutorship: contributions to the supervised curricular internship in nursing education. Rev Bras Enferm. 2019;72(6):1730–1735. doi:10.1590/0034-7167-2018-0785
15. Ayaz-Alkaya S, Yaman-Sözbir Ş, Bayrak-Kahraman B. The effect of nursing internship program on burnout and professional commitment. Nurse Educ Today. 2018;68:19–22. doi:10.1016/j.nedt.2018.05.020
16. Çingöl N, Karakaş M, Zengin S, Çelebi E. The effect of psychiatric nursing students‘ internships on their beliefs about and attitudes toward mental health problems; a single-group experimental study. Nurse Educ Today. 2020;84:104243. doi:10.1016/j.nedt.2019.104243
17. Oren B, Zengin N. Assessing health threatening problems among nursing or midwifery students during the clinical education course in Turkey. Iran J Public Health. 2019;48(1):85–94.
18. Zanchetta M, Schwind J, Aksenchuk K, Gorospe FF
19. Hsieh H-F, Shannon SE. Three approaches to qualitative content analysis. Qual Health Res. 2005;15(9):1277–1288. doi:10.1177/1049732305276687
20. Mason M, editor. Sample size and saturation in PhD studies using qualitative interviews. Forum Qual Soc Res. 2010;11(3).
21. Elo S, Kyngäs H. The qualitative content analysis process. J Adv Nurs. 2008;62(1):107–115. doi:10.1111/j.1365-2648.2007.04569.x
22. Walker JL. Research column. The use of saturation in qualitative research. Can J Cardiovasc Nurs. 2012;22:2.
23. Speziale HS, Streubert HJ, Carpenter DR. Qualitative Research in Nursing: Advancing the Humanistic Imperative. Lippincott Williams & Wilkins; 2011.
24. Shenton AK. Strategies for ensuring trustworthiness in qualitative research projects. Educ Inf. 2004;22(2):63–75. doi:10.3233/EFI-2004-22201
25. Corlett J. The perceptions of nurse teachers, student nurses and preceptors of the theory-practice gap in nurse education. Nurse Educ Today. 2000;20(6):499–505. doi:10.1054/nedt.1999.0414
26. Allmark P. A classical view of the theory‐practice gap in nursing. J Adv Nurs. 1995;22(1):18–23. doi:10.1046/j.1365-2648.1995.22010018.x
27. Upton DJ. How can we achieve evidence‐based practice if we have a theory–practice gap in nursing today? J Adv Nurs. 1999;29(3):549–555.
28. Sharif F, Masoumi S. A qualitative study of nursing student experiences of clinical practice. BMC Nurs. 2005;4(1):6. doi:10.1186/1472-6955-4-6
29. Tolley KA. Theory from practice for practice: is this a reality? J Adv Nurs. 1995;21(1):184–190. doi:10.1046/j.1365-2648.1995.21010184.x
30. Rolfe G. Listening to students: course evaluation as action research. Nurse Educ Today. 1994;14(3):223–227. doi:10.1016/0260-6917(94)90085-X
31. Petro‐Nustas W, Mikhail BI, Baker OG. Perceptions and expectations of baccalaureate‐prepared nurses in Jordan: community survey. Int J Nurs Pract. 2001;7(5):349–358. doi:10.1046/j.1440-172X.2001.00320.x
32. Hasanpour M, Mohammadi R, Dabbaghi F, et al. The Need for Change in Medical Sciences Education: A Step Towards Developing Critical Thinking. IJN. 2006;18(44):39–49.
33. Duprez V, Beeckman D, Verhaeghe S, Van Hecke A. Self-management support by final year nursing students: a correlational study of performance and person-related associated factors. Int J Nurs Stud. 2017;74:120–127. doi:10.1016/j.ijnurstu.2017.06.010
34. Walsh T, Jairath N, Paterson MA, Grandjean C. Quality and safety education for nurses clinical evaluation tool. J Nurs Educ. 2010;49(9):517–522. doi:10.3928/01484834-20100630-06
35. Nasrabadi AN, Emami A. Perceptions of nursing practice in Iran. Nurs Outlook. 2006;54(6):320–327. doi:10.1016/j.outlook.2006.06.001
36. Yazdannik A, Yekta ZP, Soltani A. Nursing professional identity: an infant or one with alzheimer. Iran J Nurs Midwifery Res. 2012;17(2Suppl1):S178.
37. Najafi KM, Sharif F, Moattari M, Jamshidi N, Karimi S. Decrease in motivation of nursing students: a qualitative study. 2011.
38. Atack L, Comacu M, Kenny R, LaBelle N, Miller D. Student and staff relationships in a clinical practice model: impact on learning. J Nurs Educ. 2000;39(9):387–392.
39. Baltimore JJ. The hospital clinical preceptor: essential preparation for success. J Contin Educ Nurs. 2004;35(3):133–140. doi:10.3928/0022-0124-20040501-10
40. Dendaas N. The scholarship related to nursing work environments: where do we go from here? Adv Nurs Sci. 2004;27(1):12–20. doi:10.1097/00012272-200401000-00003
41. Hanifi N, Parvizy S, Joolaee S. The miracle of communication as a global issue in clinical learning motivation of nursing students. Procedia Soc Behav Sci. 2012;47:1775–1779. doi:10.1016/j.sbspro.2012.06.899
42. Mohebbi Noubandegani Z, Rambod M, Hashemi F, Mohammadi H, Najafi Dolatabad S, Setoudeh G. View point of the nursing students on challenges in clinical training, Shiraz, Iran. Hormozgan Med J. 2012;16(5):415–421.
43. Jouzi M, Vanaki Z, Mohammadi E. Factors affecting the communication competence in Iranian nursing students: a qualitative study. Iran Red Crescent Med J. 2015;17(3):e19660. doi:10.5812/ircmj.19660
44. Alavi M, Abedi H. Nursing students’ experiences and perceptions of effective instructor in clinical education. Iran J Med Educ. 2008;7(2):325–334.
45. McCutchan JA. The experience of baccalaureate degree seeking nursing students undergoing the process of clinical evaluation appraisal. 2015.
46. Bourbonnais FF, Langford S, Giannantonio L. Development of a clinical evaluation tool for baccalaureate nursing students. Nurse Educ Pract. 2008;8(1):62–71. doi:10.1016/j.nepr.2007.06.005
47. Lee WS, Cholowski K, Williams AK. Nursing students’ and clinical educators’ perceptions of characteristics of effective clinical educators in an Australian university school of nursing. J Adv Nurs. 2002;39(5):412–420. doi:10.1046/j.1365-2648.2002.02306.x
48. Wildeman N. A study of clinical performance by diploma nursing [dissertation]. Canada: The University of Regina; 1989.
49. Dehghani K, Dehghani H, Falahzadeh H. The educational problems of clinical field training based on nursing teachers and last year nursing students’view points. Iran J Med Educ. 2005;5(1):24–33.
50. Cook TH, Gilmer MJ, Bess CJ. Beginning students’ definitions of nursing: an inductive framework of professional identity. J Nurs Educ. 2003;42(7):311–317. doi:10.3928/0148-4834-20030701-08
51. Sun L, Gao Y, Yang J, Zang X-Y, Wang Y-G. The impact of professional identity on role stress in nursing students: a cross-sectional study. Int J Nurs Stud. 2016;63:1–8. doi:10.1016/j.ijnurstu.2016.08.010
52. Keshk LI, Qalawa SA, Ibrahim NA. Effectiveness of an educational program regarding nursing process on acquiring advanced skills among internship nursing students. Int J Nurs. 2018;5(2):32–44. doi:10.15640/ijn.v5n2a4
53. Ahanchian M, Sharafi S, Vafaee M, Hajiabadi F. Evaluate the effectiveness of internship program in nursing student using kirkpatrick’s model. Res Med Educ. 2017;9(1):17–19. doi:10.18869/acadpub.rme.9.1.17
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
