Back to Journals » International Journal of Nanomedicine » Volume 15
Biodegradable Nanopolymers in Cardiac Tissue Engineering: From Concept Towards Nanomedicine
Authors Mohammadi Nasr S , Rabiee N , Hajebi S, Ahmadi S, Fatahi Y , Hosseini M, Bagherzadeh M, Ghadiri AM , Rabiee M, Jajarmi V, Webster TJ
Received 14 January 2020
Accepted for publication 2 April 2020
Published 18 June 2020 Volume 2020:15 Pages 4205—4224
DOI https://doi.org/10.2147/IJN.S245936
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Anderson Oliveira Lobo
Saeed Mohammadi Nasr,1 Navid Rabiee,2 Sakineh Hajebi,3,4 Sepideh Ahmadi,5 Yousef Fatahi,6– 8 Masoumehossadat Hosseini,9,10 Mojtaba Bagherzadeh,2 Amir Mohammad Ghadiri,2 Mohammad Rabiee,11 Vahid Jajarmi,12,13 Thomas J Webster14
1Faculty of Chemical Engineering, Sahand University of Technology, Tabriz, Iran; 2Department of Chemistry, Sharif University of Technology, Tehran, Iran; 3Faculty of Polymer Engineering, Sahand University of Technology, Tabriz, Iran; 4Institute of Polymeric Materials, Sahand University of Technology, Tabriz, Iran; 5Student Research Committee, Department of Medical Biotechnology, School of Advanced Technologies in Medicine, Shahid Beheshti University of Medical Sciences, Tehran, Iran; 6Department of Pharmaceutical Nanotechnology, Faculty of Pharmacy, Tehran University of Medical Sciences, Tehran, Iran; 7Nanotechnology Research Centre, Faculty of Pharmacy, Tehran University of Medical Sciences, Tehran, Iran; 8Universal Scientific Education and Research Network (USERN), Tehran, Iran; 9Department of Chemistry, Faculty of Chemistry and Petroleum Sciences, Shahid Beheshti University, Tehran, Iran; 10Soroush Mana Pharmed, Pharmaceutical Holding, Golrang Industrial Group, Tehran, Iran; 11Biomaterial Group, Department of Biomedical Engineering, Amirkabir University of Technology, Tehran, Iran; 12Department of Medical Biotechnology, School of Advanced Technologies in Medicine, Shahid Beheshti University of Medical Sciences, Tehran, Iran; 13Cellular and Molecular Biology Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran; 14Department of Chemical Engineering, Northeastern University, Boston, MA 02115, United States
Correspondence: Thomas J Webster Email [email protected]
Abstract: Cardiovascular diseases are the number one cause of heart failure and death in the world, and the transplantation of the heart is an effective and viable choice for treatment despite presenting many disadvantages (most notably, transplant heart availability). To overcome this problem, cardiac tissue engineering is considered a promising approach by using implantable artificial blood vessels, injectable gels, and cardiac patches (to name a few) made from biodegradable polymers. Biodegradable polymers are classified into two main categories: natural and synthetic polymers. Natural biodegradable polymers have some distinct advantages such as biodegradability, abundant availability, and renewability but have some significant drawbacks such as rapid degradation, insufficient electrical conductivity, immunological reaction, and poor mechanical properties for cardiac tissue engineering. Synthetic biodegradable polymers have some advantages such as strong mechanical properties, controlled structure, great processing flexibility, and usually no immunological concerns; however, they have some drawbacks such as a lack of cell attachment and possible low biocompatibility. Some applications have combined the best of both and exciting new natural/synthetic composites have been utilized. Recently, the use of nanostructured polymers and polymer nanocomposites has revolutionized the field of cardiac tissue engineering due to their enhanced mechanical, electrical, and surface properties promoting tissue growth. In this review, recent research on the use of biodegradable natural/synthetic nanocomposite polymers in cardiac tissue engineering is presented with forward looking thoughts provided for what is needed for the field to mature.
Keywords: biodegradable polymer, tissue engineering, cardiac cell, composite, natural, synthetic
Introduction
Cardiovascular disease (CVD) and heart failure, such as myocardial infarction (MI), remain leading causes of morbidity and mortality in developed countries and currently are some of the most outstanding health challenges despite many breakthroughs in medicine. For example, heart failure is due to the inability of the heart to pump blood and the adult heart muscle is incapable of regenerating damaged myocardial tissue which becomes replaced with non-contacting scar tissue.1–8 Currently, no standard clinical procedure is available to restore the damaged myocardium other than complete heart transplantation and pharmaceutical drugs that thin blood, making it easier to pump by a failing heart. Thus, there is an urgent demand to develop new methods to repair damaged cardiac tissue.9–11
Recently, cardiac tissue engineering has emerged as a promising approach to create cardiac grafts, either whole heart substitutes or tissues that can be efficiently implanted in an organism, thereby regenerating tissues for a fully functioning heart without side effects such as immune rejection.12 Tissue engineers can now provide highly controllable three-dimensional environments to mediate cell differentiation and promote functional assembly for use as high-fidelity models to study cardiac development and CVD. For cardiac tissue regeneration, some of the key requirements that need to be met are the selection of a human cell source, establishment of a cardiac tissue matrix, electromechanical cell coupling, robust and stable contractile tissue function, and functional vascularization (Figure 1).13 The major challenge for the reconstruction of an infarct myocardium by cardiac tissue engineering is to generate a bioactive substrate with suitable chemical, biological, and conductive properties, thus mimicking the natural heart extracellular matrix (ECM) both structurally and functionally.14
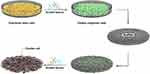 |
Figure 1 Schematic representation of the preparation process of a scaffold and incorporation of growth factors. |
There are two major technologies in tissue engineering and tissue regeneration helpful in this regard: (1) biomaterial technology for the creation of 3-D porous scaffolds to support and guide tissue formation from dissociated cells, and (2) bioreactor cultivation of 3-D cell constructs during ex-vivo tissue engineering which aims to duplicate the normal stresses and flows experienced by heart tissue.15 Traditionally, cardiac tissue engineering mainly uses two classes of materials: 1) scaffolds since they have a porous structure for donor cells and growth factor diffusion to induce and direct the growth of new, healthy tissue, and 2) hydrogels which are water-insoluble, crosslinked polymer matrices with high water content that can be easily injected into damaged heart tissue and fabricated into a wide range of tissue engineering constructs.16,17
The characteristics of biodegradable polymers including adjustable degradation rates, optimal porosity, biocompatibility and elastomeric properties (which can mechanically favor tissue contraction inherent for cardiac function) have attracted much attention for cardiac tissue engineering applications. These include the ability of scaffolds to preserve mechanical properties during tissue growth, their gradual degradation into biocompatible products, and their ability to receive cells, growth factors and so on.18–20
Biodegradable polymers are classified into two main categories: natural and synthetic polymers. Natural polymers can be defined as polymers which are found in nature. However, synthetic polymers are made by humans from non-renewable petroleum resources.21,22 Both types of polymers, natural and synthetic polymers, have their own exceptional set of advantages and disadvantages in cardiac tissue engineering. For some cardiac tissue applications, natural/synthetic composites have been used to combine the advantages of both natural and synthetic polymers.23 Yet, despite such advantages, regenerating cardiovascular tissue using conventional tissue engineering has been difficult, problems which may be solved through the use of nanomedicine.
Impressively, nanomedicine has opened many new directions in fields such as cardiovascular tissue engineering. There are several reasons to use nanomedicine to improve cardiovascular medicine, such as the ability of synthetic nano tissue engineering scaffolds to mimic the surface, mechanical, and electrical properties of natural heart tissues; the unique surface energy one can obtain from nanomaterials (such as nanostructured surfaces, nanoparticles (NPs), nanotubes, self-assembled materials, etc.) which can control immune system and cellular responses; and the ability of NPs to penetrate cells and tissues to promote cardiovascular tissue growth. Nanotechnology can enable the synthesis of materials with specific biological activity at a controlled rate for cardiac tissue engineering.24,25 Polymeric NPs have received consideration in the field of nanotechnology because of their manipulated material properties and easy functionalization.26
In the present review, we will focus on synthetic and natural nanostructured biodegradable polymeric-based biomaterials and recent advances in cardiac tissue engineering that have attracted a considerable amount of attention.
Biodegradable Polymers in Cardiac Tissue Engineering
Biodegradable polymers can be fashioned from natural polymers and synthetic polymers for cardiac tissue engineering.21 These types of polymers offer their own exceptional set of advantages and disadvantages in cardiac tissue engineering. Thus, to combine the advantages of both natural and synthetic polymers, natural/synthetic composites have been proposed for some cardiac tissue applications.23 In this section, recent advances of natural and synthetic biodegradable nanopolymers for cardiac tissue engineering will be discussed.
Natural Polymers
Natural polymers exist as natural sources, such as animals and plants, and because they are natural, they are composed of nanostructured proteins and are, thus, considered nanomaterials.22 These natural polymers because of their biodegradability, renewability, and abundant availability have been used in diverse applications in tissue engineering.27 Some typical natural biodegradable polymers used for cardiac tissue engineering include fibrin gel, collagen, gelatin, chitosan, alginate, and Matrigel.28 Common biodegradable polymers will be discussed in the following subsections and are listed in Table 1 with their advantages and disadvantages.
 |
Table 1 Common Natural Polymers in Cardiac Tissue Engineering |
Fibrin
Fibrin is a common natural polymer (Figure 2) that has been widely used in cardiac tissue engineering approaches and especially for cardiac cell encapsulation.29 Fibrin is formed during the haemostatic coagulation process by rapid polymerization of fibrinogen monomers with the proteolytic enzyme thrombin as a crosslinking agent at ambient temperature.45–47 The mechanical properties and gelation rates of fibrin have been directly related to the modulation of the fibrinogen and thrombin ratio. Owing to its excellent biocompatibility, controllable degradation rate and non-toxicity, fibrin has been extensively proposed and used in cardiac tissue engineering.29,47 However, fibrin exhibits some significant drawbacks such as poor mechanical properties, shrinkage of the gel, and potential disease transmission that are obstacles for the use of a fibrin gel as an ideal candidate for tissue engineering.29
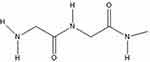 |
Figure 2 Structure of fibrin. |
Fibrin has also been applied as a 3D culture system for developing cell therapeutics for myocardial regeneration and cardiac cell biology. In one study, Kim et al used fibrin as a 3D myocardial organ culture system for the isolation of cardiac stem cells (CSCs) via the recapitulation of cardiac homeostasis. Results indicated that a fibrin-supported 3D myocardial organ culture was able to recapitulate myocardial homeostasis ex vivo and to isolate in vitro renewed and outgrown CSCs. This study demonstrated a selective isolation of CSCs from the fibrin by matrix restricted fibrinolysis without any sophisticated tissue dissociation and purification steps.48 Platelet fibrin gel (also known as a platelet fibrin scaffold) and stem cells have been investigated for therapeutic cardiac repair. For example, Shen et al studied the effects of matrix metalloproteinases (MMPs) on the performance of a platelet fibrin gel spiked with CSCs for heart repair. This study illustrated the advantages of the intramyocardial injection of a cell-gel in a rat model of acute myocardial infarction (MI) with or without the broad-spectrum MMP inhibitor GM6001. As a result of this study, metalloproteinase inhibition diminished the structural and functional benefits of the cell-gel construct in treating MI which was proven via echocardiography and histology 3 weeks after treatment. Therefore, one of the extremely significant parameters for the successful therapeutic benefits of a platelet fibrin gel spiked with CSCs for treating MI include MMP incorporated fibrin.49
Fibrin was also used as a platform for stimulating cardiac angiogenesis. In one research study, Melly et al investigated an optimized fibrin platform for the stimulation of cardiac angiogenesis through growth factors (vascular endothelial growth factor (VEGF) and platelet-derived growth factor-BB (PDGF-BB)). This fibrin platform stimulated angiogenesis within a limited time duration of treatment and without introducing any genetic material. This study illustrated that fibrin plays a critical role for the improvement of efficacy and safety of therapeutic angiogenesis in the heart.50
Collagen
Collagen is one of the most common high-weight molecular natural polymers or proteins used for cardiac tissue engineering (Figure 3). Collagen has advantages including thermal reversibility, biocompatibility, and strong cellular activities for cardiac tissue engineering efforts. Collagen has many different types (28) discovered from various human tissues such as bone, skin, ligaments, tendons, and cartilage.51 However, collagen types I, II, III, and IV are commonly studied in tissue engineering.52 Among these types of collagen, type I has been the most frequently used in tissue engineering because of its suitable biocompatibility.53–58 Collagen is one of most preferred biodegradable polymers in diverse tissue engineering applications (especially in cardiac tissue engineering) because of its high biocompatibility, biodegradability, hyposensitivity and low toxicity.32,59
 |
Figure 3 Structure of collagen. |
Collagen scaffolds, especially nanofibrous scaffolds, have been investigated for cardiac tissue engineering. In one study, one of the most facile recent techniques for generating nanofibrous scaffolds out of collagen uses an electric field between a grounded collector and polymer solution by Punnoose et al. Fluoroalcohols (such as 2,2,2-trifluoroethanol (TFE) and 1,1,1,3,3,3–hexafluoro-2-propanol (HFIP)) were used to produce nanofibrous scaffolds out of collagen type 1, which has been the main choice for the production of collagen-based biomaterials. However, fluoroalcohols are expensive and also corrosive, therefore, many studies have been performed with the hopes of finding a nontoxic and economical solvent. For example, in one study, Punnoose et al reported a simple benign binary solvent system consisting of acetic acid and dimethylsulphoxide which was used for electrospinning nanofibers out of type 1 collagen (diameters ranged from 200nm–1100nm). This solvent was not only low in cost but it also maintained the native integrity of electrospun collagen.59 In other study, Joanne et al investigated electrospun collagen scaffolds with biologically compatible solvents (based on ethanol, water and salts) and cross-linking agents (glycerol). This nanofibrous collagen scaffold was seeded with human induced pluripotent stem cell-derived cardiomyocytes and these scaffolds were epicardially delivered in a mouse model of dilated cardiomyopathy. In vivo and in vitro results indicated that a human induced pluripotent stem cell-derived cardiomyocyte seeded electrospun scaffold was a potent biomaterial for the stabilization of dilated cardiomyopathy and thus suitable for future clinical use.60
Collagen scaffolds have disadvantages that include inferior mechanical properties or low physical strength and a lack structural stability upon hydration. One way to improve the mechanical strength of collagen-based scaffolds is intermolecular cross-linking of collagen scaffolds via chemical and physical methods.31 For example, Lin et al investigated stiffness-controlled 3D collagen type I scaffolds for the differentiation and proliferation of mesenchymal stem cells into cardiac progenitor cells. To obtain the stiffness required in 3D collagen type I scaffolds, collagen was cross-linked with different ratios of hydroxysuccinimide (NHS) and 1-ethyl-3-(3-dimethylaminopropyl) carbodiimide (EDC) cross-linkers. Results illustrated that the collagen scaffolds cross-linked with 50/50 EDC mM/NHS mM cross-linkers not only demonstrated a higher Young’s modulus (31.8 kPa) but also showed a better interconnectivity. Moreover, mesenchymal stem cells, in these stiffness-controlled collagen scaffolds, were able to proliferate and differentiate into cardiac progenitor cells in the absence or presence of TGF-β2.32
Another way to improve the mechanical strength of collagen scaffolds is blending collagen with other materials, such as inorganic materials and natural synthetic polymers.31 In some studies, carbon nanotubes (CNTs), because of their excellent mechanical strength, electrical conductivity, and high aspect ratios were blended with collagen to improve electrical and mechanical strength.61,62 In one particular study, Sun and co-workers fabricated CNT-incorporated collagen hydrogels and evaluated the behavior and growth of cardiomyocytes in such hydrogels. Figure 2 shows a schematic describing the study. The results showed that the incorporation of CNTs (0, 0.5, 1, and 2 wt%) within collagen hydrogels improved respective elastic moduli values to 13.2±0.1, 21.1±0.1, 24.6±0.07, and 28.8±0.092 kPa, enhanced conductivity compared with pure collagen hydrogels, and enhanced cell–cell alignment and the assembly of neonatal cardiomyocytes. However, cellular toxicity was observed at higher concentrations of CNTs incorporated within hydrogels (CNTs up to 2 wt%).61
In similar work, type I collagen hydrogels were combined with CNTs for the fabrication of CNT-collagen hydrogels by Yu et al. For this work, CNT-collagen hydrogel samples (type I collagen concentration of 2 mg/mL) with CNT loading levels of 0 wt.% (pure collagen group), 1 wt.%, 2 wt.%, 5 wt.%, and 10 wt.% and a dense collagen hydrogel sample (type I collagen concentration of 4 mg/mL) were prepared. Results indicated that CNTs were uniformly dispersed in the CNT-collagen hydrogels and collagen fibers were coated on the surface of CNTs (Figure 4A). In addition, fiber thickness and pore size of the CNT-collagen hydrogels had no change in comparison with pure collagen hydrogels (Figure 4B). Moreover, LX-2 cells were seeded within the collagen hydrogels with/without CNTs. The results of culturing of LX-2 cells after 3 days illustrated that no obvious cell death or morphologic changes were detected with the incorporation of CNTs in the collagen hydrogels (Figure 4C). Also, cardiomyocytes were seeded within the CNT-collagen hydrogels and these hydrogels improved cardiac cell functions in comparison with pure collagen hydrogels. Moreover, CNTs with type I collagen hydrogels improved the electrical performance and mechanical strength of the scaffolds and also maintained the native sub-micron fibrous structure of the hydrogels (Figure 4D).62
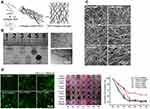 |
Figure 4 Carbon nanotubes (CNTs) used in cardiac tissue engineering. (A, B) CNT-incorporated collagen hydrogel preparation and different levels of CNTs loaded in CNT-collagen hydrogels. In (A), the arrows indicate the progression of fabricating the construct. (C) SEM images of the fiber thickness and unchanged pore size and fiber thickness in combination with CNTs with collagen hydrogels. (D) LX-2 cell viability and absence of cell death and morphological changes with the combination of CNTs and collagen hydrogels. Reprinted (adapted) with permission from Yu H, Zhao H, Huang C, et al. Mechanically and electrically enhanced CNT–collagen hydrogels as potential scaffolds for engineered cardiac constructs. ACS Biomater Sci Eng. 2017;3(11):3017–3021.62 Copyright (2020) American Chemical Society. |
In recent years, collagen-based cardiac patches with incorporated electroconductive properties have been investigated for their therapeutic potential for treating myocardial infarction. For example, Hosoyama et al fabricated nano-engineered collagen-based cardiac patches for MI repair. To fabricate the nano-engineered collagen-based cardiac patches consisting of an elastic hydrogel and nano-engineered aligned fibers, AgNPs and AuNPs were used as the electroconductive components. Both AuNPs and AgNPs containing patches were prepared and tested for promoting the electrical and mechanical repair of the IM in a clinically relevant murine model. Results of investigations of the prepared and tested patches indicated that only the AuNPs containing patches increased connexin-43 expression in neonatal rat cardiomyocytes cultured under electrical stimulation and recovered cardiac function in an in vivo model of an established myocardial scar. Moreover, AuNPs containing fibers exhibited suitable electrical conductivity and stability under physiological conditions. However, AgNPs containing fibers demonstrated reduced stability because the AgNPs containing fibers promoted the degradation of the nanoparticles. Thus, AuNPs containing patches are suitable as a therapeutic potential for treating myocardial infarction but may need more attention towards stability.63
Gelatin
Gelatin, a derivative of collagen, is another natural polymer. Gelatin is used as a potential biomaterial for cardiac tissue repair because collagen mostly exists in the ECM in many organs such as the heart.64 Gelatin due to its biocompatibility, biodegradability, nontoxicity, and limited immunogenicity has been used extensively in the field of cardiac tissue engineering.65 In a recent study, gelatin nanofibrous matrices were electrospun using a benign binary solvent (acetic acid, dimethylsulfoxide (DMSO)) and characterized for primary cardiomyocyte growth and function by Elamparithi et al. The studies showed that the matrices enhanced scaffold stability without blending with other natural or synthetic polymers. Moreover, the scaffolds possessed a Young’s modulus of 19.6±3.6 kPa (similar to native human myocardium tissue) and a tensile strength of 4.8 ± 1.5 kPa with fiber diameters of 200–600 nm. The biophysical and mechanical properties of the gelatin electrospun nanofibrous matrices were suitable for contracting cardiomyocytes.66 Gelatin scaffolds demonstrated a lack of strength and suture retention strength.
In cardiovascular tissue applications, creating gelatin microfiber scaffolds is one way to enhance the strength of gelatin. For example, Elsayed et al fabricated and characterized biomimetic, electrospun gelatin fiber scaffolds for tunica media-equivalent, tissue engineered vascular grafts. Results indicated that the Young’s modulus of the produced wet tubular scaffolds were in the range of 0.1–1.2 MPa. Moreover, a high suture retention strength (1.8–1.94 N) was obtained for wet acellular scaffolds which was equal or better than the suture retention strength of a fresh saphenous vein (1.81 N). In static cell culture medium, the scaffolds demonstrated suitable performance for human smooth muscle cell (SMC) proliferation.67
However, gelatin hydrogels have disadvantages such as weak mechanical stability and durability and are highly hydrated. Thus, crosslinking gelatin, such as via enzymatic crosslinking, chemical crosslinking, and physical crosslinking has been used to produce gelatin-based biomaterials. In one study, Yang et al studied an enzymatically cross-linked gelatin which promoted the proliferation of adipose tissue-derived stromal cells. The gelatin hydrogel was cross-linked by microbial transglutaminase (mTG). Gelatin/mTG hydrogels were prepared by mixing 10% of a mTG solution with different concentrations of gelatin (1%, 2%, 4%, 6%, 8%, and 10% (w/v)). The low-concentration gelatin solution demonstrated a long gelation time, but, the gelation time was shortened for the high-concentration gelatin solution. In both 2D and 3D cultures, the gel concentration affected cell growth morphology and proliferative capability. The cell growth morphology for the 2% gelatin hydrogels showed a round or stick-like shape because of low gel strength. Thus, 2% gelatin hydrogels are not suitable for cell migration and subcutaneous implantation. Moreover, the cross-linked gelatin promoted cell differentiation, proliferation, and adhesion. Additionally, mechanical properties of the gelatin/mTG hydrogels were adjustable and were non-toxic. In addition, these hydrogels affected cardiac differentiation of adipose tissue-derived stromal cells.33
Some techniques, such as the 3D bioprinting of channels and grooves, have been of high interest in recent years because such techniques can vary surface features to have a large influence over cell behavior, phenotype and morphology. For example, in one study, Tijore et al investigated a gelatin scaffold with 3D bioprinted pattern for the induction of a stem cell myocardial lineage. Also, the topographical guidance for cell attachment and the effect of varying channel width was studied. Results indicated that stable cell alignment microchannels could be produced by 3D bioprinting a gelatin hydrogel cross-linked with enzyme MTGase. These microchannels enhanced the organization and rhythmic beating of cardiomyocytes serving as model cells, promoted a myocardial lineage commitment, and could also orientate human mesenchymal stem cells.68
Alginate
Alginate is a natural linear polysaccharide (Figure 5) which is typically obtained from the cell walls of brown algae.69 Alginate is a potential biodegradable polymer for cardiac tissue engineering because of its high biocompatibility, biodegradability, and non-toxicity, as well as its relatively economical, mild and physical gelation process, and non-thrombogenic nature.37,39,70
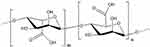 |
Figure 5 Structure of alginate. |
Several methods such as crosslinking, immobilization of specific ligands, and the conjugation of other materials have been used for the modification of gelation and mechanical properties of alginate.38 In one study, Sondermeijer et al modified an alginate scaffold with a covalently attached synthetic cyclic RGDfK (Arg‐Gly‐Asp‐D‐Phe‐Lys)‐peptide to improve the survival of transplanted cells and angiogenesis in damaged myocardium tissue. The modified scaffolds seeded with hMPCs were investigated in rats with MI and more vascularization at the infarct border zone were obtained for scaffolds seeded with 1×106 hMPCs than and the scaffolds with a higher dose of hMPCs (3×106) and without cells (7 days). Moreover, the epicardial scaffolds exhibited an absence of a foreign body responses against the scaffold material 1 week following implantation as shown in Figure 6. Consequently, the purified 3D‐alginate scaffold modified with a cyclic RGDfK peptide could enhance cell viability and promote angiogenesis demonstrating its non-immunogenic and biocompatible properties.71
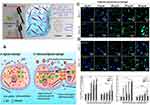 |
Figure 6 Fullerenol/alginate hydrogel preparation. (A) Schematic illustration of the MAPK pathway and cardiac gene expression under an oxidative stress microenvironment and cell proliferative behaviors, survival and cardiomyogenic differentiation of BADSCs in alginate hydrogels and fullerenol/alginate hydrogels. (B) The combination of folerolol with hydrogenated alginate improves cardiomyogenic differentiation of BADSC under oxidative stress conditions, (C) cTnT and (D) α-actinin immunofluorescence staining of BADSCs seeded in fullerenol/alginate hydrogels at day 7 and 14 in the presence of H2O2, in which * indicates meaningful changes between the first row and second row, and ** indicates meaningful changes between the first and third row values. Adapted with permission from Hao T, Li J, Yao F, et al. Injectable fullerenol/alginate hydrogel for suppression of oxidative stress damage in brown adipose-derived stem cells and cardiac repair. ACS Nano. 2017;11(6):5474–5488.72 Copyright (2020) American Chemical Society. |
One main drawback of alginate is its high hydrophilicity, which can cause weak cell adhesion and proliferation. In one study, Hao et al developed a fullerenol/alginate hydrogel with antioxidant activity as a stem cell delivery vehicle for cardiac repair. The results indicated that this hydrogel had no cytotoxicity effects on brown adipose-derived stem cells (BADSCs). Moreover, the cardiomyogenic differentiation of BADSCs was improved with the addition of fullerenol. This hydrogel improved the retention and survival of implanted BADSCs and reduced reactive oxygen species (ROS) levels in a MI rat model.72 A three‐dimensional (3D) bioprinting method for the fabrication of cardiac alginate implants can be used to modulate porosity of hydrogel constructs and electrical/mechanical properties.
Izadifar et al bioprinted alginate implants laden with human coronary artery endothelial cells (HCAECs) for the investigation of electrical/mechanical properties of cardiac alginate implants. In this study, the surgically implanted cardiac patches were evaluated by the PCI‐CT‐based quantitative imaging performance to estimate electrical/mechanical behavior. Results showed that the 3D‐printing patterns had considerable effects on electrical conductivity and porosity of the alginate cardiac implants and compression modulus. They also found a suitable architectural design with a 3D‐printing pattern with a distance of 900µm and strand alignment angle of 0/45/90/135°. This pattern exhibited suitable porosity, higher electrical conductivity and stiffness, and retained high cell viability (over 7 days).73
Matrigel
Matrigel is a gelatinous ECM protein containing natural polymers secreted by Engelbreth-Holm-Swarm (EHS) mouse sarcoma cells, commonly used as a cell culture matrix.74–76 Matrigel is commonly used as a substrate coating to improve cell adhesion; however, matrigel hydrogels have also been used in cardiac tissue repair. Matrigel hydrogels contain critical growth factors and cytokines for cell growth and also they have been considered as a cytocompatible gel.74 However, one main drawback which makes it unsuitable in clinical use is its animal origin (derived from murine sarcoma cells).41 In one study of the application of Matrigel in cardiac tissue engineering, Feaster et al investigated a Matrigel mattress for the generation of single contracting human-induced pluripotent stem cell–derived cardiomyocytes (hiPSC-CMs). In this study, a rapid method was reported for producing rod-shaped hiPSC-CMs with aligned myofilaments. hiPSC-CMs were cultured on a Matrigel mattress (0.4- to 0.8-mm thick) for 5–7 days and were compared with hiPSC-CMs maintained on a control substrate. Results indicated that the mattress hiPSCCMs demonstrated significantly increased sarcomere length, a more rod-shape morphology, and robust contractile responses to positive inotropic agents. Thus, this method could be valuable for preclinical cardiotoxicity testing and disease modeling because it permitted the quantification of contractile performance at the single cell level.77
In other work, Zhang et al fabricated vascularized pacemaker tissues by cardiac progenitor cells (CPCs) and endothelial progenitor cells (EPCs) into Matrigel. The transplantation of a tissue engineered cardiac pacemaker (TECP), fabricated from CPCs-derived pacemaking cells and vascularization of TECP (vTECP) by mixing CPCs and EPCs, was investigated using in vitro (21 days) and in vivo (4 weeks) implantation (implanted into rat hearts) for cardiac sinus node dysfunction. Results indicated an increase of individual survival in sinus node damage models after TECP implantation and the implanted TECP exhibited electrical activity. In addition, the maximum vascularization in vitro, for vTECP, was obtained at the optimal ratio (1:1 proportion of EPCs and CPCs-derived pacemaker cells) between EPCs and CPCs derived pacemaking cells. Also, the implantation of vTECP increased electrical activity in vivo. However, the main drawback was a lack of efficient vasculature of engineered tissues which is a strong obstacle for its use in cardiac tissue engineering.78
Chitosan
Chitosan is a linear polysaccharide (Figure 7) derived from chitin by partial deacetylation.79,80 Chitosan, because of its structural similarity to natural glycosaminoglycans, is characterized by low toxicity and high biocompatibility. During in vivo tissue applications, chitosan, through enzymatic hydrolysis, biodegrades into nontoxic products. Chitosan, and its derivatives, increase cell recognition and cytocompatibility for tissue-engineering applications, and are often coated or grafted onto scaffold surfaces.81 However, the drawback of chitosan is it is poorly soluble at physiological pH.44 Chitosan-based hydrogels have been recently tested as a biodegradable material for cardiac tissue engineering applications because their biodegradability can be controlled and their degradation products are biocompatible.82–84 For example, Xu et al used a temperature-responsive chitosan hydrogel as an injectable scaffold to deliver MSCs. The results of this study illustrated that a temperature-responsive chitosan hydrogel enhanced graft size and cell retention in an ischemic heart, enhanced the effects of MSCs on neovasculature formation, and promoted MSC differentiation into cardiomyocytes. In addition, this hydrogel enhanced cardiac function and hemodynamics (5 weeks after cell transplantation) in the infarcted area of rats following MI.83
 |
Figure 7 Structure of chitosan. |
Chitosan hydrogels have also been studied as scaffolds for cardiovascular applications. For example, Aussel et al investigated chitosan-based hydrogels for developing a small-diameter vascular graft. Results from in vivo studies in small and large animals (rat and sheep) and in vitro studies of chitosan-based hydrogels indicated that the hydrogel exhibited good hemocompatibility properties in vivo and promising in vitro biocompatibility.85
The electrical properties of implanted grafts are significant challenges for the regeneration of infarcted heart tissue. Distribution of AuNPs throughout chitosan is one way to enhance electrical coupling between adjacent cells within chitosan scaffolds. In one study, Baei et al developed a facile process to fabricate thermosensitive electro-conductive AuNP-chitosan injectable hydrogels for cardiac tissue engineering applications. In this study, the gold nanoparticle-chitosan hydrogel was seeded with MSCs. The results demonstrated that the concentration of AuNPs/chitosan (0, 1, 1.5, and 2%w/w) controlled the gelation and conductive properties. The electrical conductivity of 1% (w/w) was closer to the electrical properties of the native myocardium (0.13 Sm−1). Moreover, the chitosan-AuNP hydrogel stimulated differentiation into cardiac lineages by harnessing the electrical properties of AuNPs and it also maintained the viability and growth rate of cultivated MSCs.86
Despite the effective applications of Au NPs in cardiac tissue engineering, one of their disadvantages is their toxicity.87 Selenium NPs (SeNPs) are among those naturally produced in the body, and have been used for its therapeutic potential for cardiovascular disease, because diseased individuals have very low levels of this element in blood.88,89 In 2018, Kalishwaralal et al synthesized a chitosan-selenium NP (SeNP) nanocomposite film with high electrical conductivity (0.0055S cm−1) and a suitable tensile strength of 419 kPa which matched properties of the native myocardium. Evaluation of this film by a H9C2 cell line showed that cells grew on the chitosan-SeNPs films, were capable of proliferation and also formed membrane nanotubes, indicating the transmission of electrical signals between cells and the conductive matrices and the communication between cells, causing more cardiac cell activity, cardiac repair and increases in electrical conductivity more than the natural myocardium of the heart. Some of the most important issues in cardiac tissue engineering are inflammation and immunogenicity produced by the implant. Smooth surfaces play a greater role in inflammation and capsular fibrosis, and in this study, rough surfaces showed a reduced risk of inflammation. In addition, the morphology of the polymeric nano fibers (as the substrate for the nanoparticles or nanomaterials) is really important in cardiac tissue engineering. By utilizing different methods in the synthesis of these polymeric nano fibers, or even in the sterilizing process, the desired morphoology can be obtained. Figure 8 shows the difference between the morphologies of a typical nano fiber preparation by using different sterilizing methods88 (Figure 8).
 |
Figure 8 Morphology of PLA nanofibers for the construction of cardiac tissue engineering scaffolds with different magnifications and techniques: (A) non-sterilized, (B) sterilized by ethylene oxide, (C) sterilized by UV, and (D) sterilized by gamma irradiation. Reprinted with permission from Valente T, Silva D, Gomes P, Fernandes M, Santos J, Sencadas V. Effect of sterilization methods on electrospun poly (lactic acid)(PLA) fiber alignment for biomedical applications. ACS applied materials & interfaces. 2016;8(5):3241–3249.90 Copyright (2020) American Chemical Society. |
However, these natural polymers have some drawbacks such as rapid degradation, insufficient electrical conductivity, immunological reaction, and poor mechanical properties for cardiac tissue engineering.31,91
Synthetic Polymers
Synthetic biodegradable polymers including polylactide (PLA), poly(glycolic acid) (PGA), polylactide-glycolic acid (PLGA), poly ethylene glycol (PEG), polyurethane, polycaprolactone (PCL), and poly(N-isopropylacrylamide) have all been used in cardiac tissue engineering applications. Synthetic biodegradable polymers are considered as potential materials for cardiac tissue engineering because of their attractive physical and chemical properties such as strong mechanical properties, controlled structure, great processing flexibility, and no immunological concerns.92 These properties are critical requirements for cardiac muscle tissue engineering. Typical biodegradable synthetic polymers used in cardiac tissue engineering will be explored in the following subsections and are listed in Table 2 with chemical structures and advantages/disadvantages.
 |
Table 2 Common Synthetic Polymers Used in Cardiac Tissue Engineering |
Poly(Glycolic Acid)
Poly(glycolic acid) (PGA), the simplest linear aliphatic polyester, was one of the first studied biodegradable synthetic polymers for biomedical applications.108,109 PGA is a highly crystalline polymer (40–55%) with a high melting point (higher than 200°C), a glass transition temperature of 35–40°C, a high tensile strength (12.5GPa) and negligible solubility in organic solvents.94 PGA has non-toxic degradation products and suitable biodegradability, biocompatibility and mechanical properties.93 Owing to its hydrophilic nature and quick water uptake, PGA is not sustainable in vivo because PGA loses its mechanical strength usually over a period of 2 to 4 weeks after implantation and completely disappears several months after implantation.94,110 In cardiovascular applications, PGA is usually applied as a temporary scaffold or support substrate. Other drawbacks of untreated surfaces of PGA are its weak performance for cell adhesion and proliferation. Thus, surface modification as a strategy can enhance cell adhesion and proliferation on PGA surfaces. For example, Huang et al developed a short peptide to modify PGA surfaces to improve endothelial cell adhesion and spreading. Results indicated that the use of hetero-bifunctional peptide linkers (interfacial biomaterials) for the surface modification of PGA can improve interactions between PGA and human umbilical vein endothelial cell integrin receptors.111
Poly(Lactic Acid)
Polylactide (PLA), a hydrolyzable aliphatic semicrystalline polyester polymerized by lactic acid, is a biodegradable synthetic polymer that has a variety of applications in tissue engineering.78 PLA has a low degradation rate and is more hydrophobic than PGA.112 PLA is present in four different stereoisomeric forms: poly(D-lactic acid) (PDLA), poly(L-lactic acid) (PLLA), poly(D, L-lactic acid) (PDLLA), and meso-poly(lactic acid). PDLA is a crystalline material and PLLA is a semi-crystalline material, while PDLLA and meso-poly(lactic acid) are amorphous materials.113 Among the four forms of lactides, the semi-crystalline PLLA has been widely studied for cardiac tissue applications because of its biocompatibility, biodegradability, nontoxicity, and good mechanical integrity.94,95 However, the long degradable time of PLLA is a main drawback for its use in cardiac tissue applications.96 In one study, porous nanofibrous PLLA scaffolds for the construction of cardiac tissue with CPCs were developed. In this study, the CPCs derived from mouse embryonic stem cells (ESCs) were seeded into scaffolds to engineer cardiac constructs in vitro and were implanted subcutaneously in nude mice. In addition, the morphology of typical nano fibers for another similar study are shown in Figure 9. Results showed that the scaffolds facilitated cell attachment, extension, and differentiation after 1, 5 and 7 days. Moreover, the cell/scaffold constructs supported a large number of living cells expressing key endothelial cell (CD31), smooth muscle cell (SM22-α and α-SMA), and cardiomyocyte marker proteins (cTnT).114,90
 |
Figure 9 SEM images of (A) a typical fibrous mat of the PLA fibers and (B) PANI/PLA coaxial fibers. Reprinted with permission from Dong H, Prasad S, Nyame V, Jones WE. Sub-micrometer conducting polyaniline tubes prepared from polymer fiber templates. Chem Mater. 2004;16(3):371–373.115 ©Copyright (2020) American Chemical Society. |
In other work, Giménez et al studied the effect of PLLA scaffolds seeded with aligned diaphragmatic myoblasts (DM) overexpressing connexin-43 on infarct size and ventricular function in sheep with acute coronary occlusion. Results showed that PLLA sheets seeded with DM overexpressing cx43 reduced infarct size, decreased fibrosis in the infarct border, and induced angiogenesis after 45 days. The PLLA sheets with DM overexpressing cx43 and PLLA sheets with DM sheets similarly improved ventricular function.116
The combination of PLA/(polyaniline) PANI can be an important candidate for cardiac tissue engineering applications. PANI is a synthetic polymer which has been of high interest to researchers due to its high electrical conductivity and other special properties. Electrospun conductive nanofibrous PLA/PANI scaffolds (diameter of the nanofibers were about 500 nm) were developed by Wang et al. This PLA/PANI nanofibrous sheet showed a structure similar to the ECM and conductivity for electrical propagation similar to the native myocardium. It also improved cell-cell communication and maturation, as shown by the increased secretion of α-actinin and CX43. Thus, this nanofibrous sheet presents a promising potential in cardiomyocyte-based 3D bioactuators and cardiac tissue engineering. In this study, the electrospinning method was used to synthesize the sheets. Although the sheets showed a similar fiber diameter, an increase in conductivity was observed with increasing PANI from 0 to 3 wt.%. Also, another study showed that the surface morphology of different prepared electrospun nano fibers with different ratios of polymers (in this case, PLA to chitosan) can led to different properties, which come from the total porosity as well as the cracks on the surface, and also the hydrophobicity potential of those nano fibers117,115 (Figure 10).
 |
Figure 10 Surface morphologies for electrospun fibers: (A) SEM image for PLA/CS (1:3) core/shell fibers, (B) SEM image for PLA/CS (1:3) core/shell fibers produced with higher magnification, (C) SEM image for fibers with PLA/CS (1:1); as shown in the red square, the fibers agglomerate, and (D) SEM image for PLA/CS (1:1), the fibers with higher magnification; as shown in the red circle, the diameters of the fibers were not uniform. Reprinted with permission from Wang T, Ji X, Jin L, et al. Fabrication and characterization of heparin-grafted poly-L-lactic acid–chitosan core–shell nanofibers scaffold for vascular gasket. ACS Applied Materials & Interfaces. 2013;5(9):3757–3763.138 ©Copyright (2020) American Chemical Society. |
Poly(Lactic-co-Glycolic Acid)
Poly(lactic-co-glycolic) acid (PLGA) is a block copolymer of PGA and PLA which has been considered as one of the most potent candidates for biomedical applications.118,119 PLGA has been extensively used to fabricate tissue engineering scaffolds due to its biocompatibility, adjustable degradation rate, non-toxicity, solubility in organic solvents and tunable mechanical properties.98 Moreover, PLGA has been extensively applied for cardiac tissue engineering applications. For example, Zamani et al developed a stromal derived factor-1a (SDF-1a) incorporated PLGA core–shell particle by an electrospraying technique, and employed it as an injectable drug delivery system for MI treatment. In this study, a distinct core–shell structure with a uniform size distribution (4.30 ± 0.75 µm) was obtained for the SDF-1α incorporated PLGA particles. In addition, the electrosprayed SDF-1α loaded core–shell particles exhibited a sustained release of SDF-1α for at least 40 days and enhanced MSCs migration and proliferation in vitro.120
In other study, Asiri et al determined greater cardiomyocyte functions on aligned compared to random carbon nanofibers in PLGA. Results indicated that cardiomyocyte functions improved on carbon nanofibers aligned in PLGA compared to randomly oriented in PLGA since the carbon nanofibers were more hydrophobic than PLGA and attracted the adsorption of key proteins (laminin, vitronectin, and fibronectin) to mediate their adhesion and morphology.121 One of the main drawbacks of PLGA in cardiac tissue engineering is its weak cell attachment and its acidic degradation products which sometimes do more harm than good towards cytocompatibility.99
Polycaprolactone
Polycaprolactone (PCL) is a synthetic biodegradable polymer prepared by the ring opening polymerization of ε-caprolactone.122 This material is one of the most widely used synthetic polymers in tissue engineering because of its biocompatibility, excellent elasticity and toughness, and good mechanical properties.123,124 PCL is a suitable biodegradable polymer for applications where a long degradable time is needed, because it has a long degradation time (about 2–3 years).103,124 However, PCL exhibits a long degradation time which it is an obstacle for use in cardiac tissue engineering.101 Two strategies have been used for the modulation and enhancement of mechanical and degradation properties of PCL: the incorporation of a nanostructured filler material into the PCL material and the use of PCL as a copolymer or as one of the components of a blended material.102 In one work, Ghaziof et al prepared PCL/multiwalled carbon nanotube (MWCNT) composite scaffolds, with different amounts of MWCNTs, via a solvent casting and a vacuum drying technique for myocardial tissue engineering. Results showed that the addition of the MWCNTs in the nanocomposite scaffolds enhanced mechanical properties and electrical conductivity of the construct. The elastic modulus increased about 85%, 45%, and 45% for 1, 0.75, and 0.5 wt.% of MWCNTs, respectively. Moreover, through the addition of MWCNTs to the nanocomposites (1, 0.75, and 0.5 wt.%), the electrical conductivity obtained was 11.32, 8.15, and 5.23 (µS/cm), respectively.125
In other study, Castilho et al developed melt electrospinning writing of poly-hydroxymethylglycolideco-ε-caprolactone (pHMGCL)-based scaffolds for cardiac tissue engineering. Results indicated improvement of the cellular response according to the mechanical anisotropy that was obtained by using pHMGCL after a melt electrospinning writing. In addition, a higher degree of cellular alignment was exhibited on pHMGCL-based polymers compared with a commonly used PCL polyester.126
Moreover, to enhance engineered cardiac tissue function, polypyrrole (a conductive and electroactive polymer) was investigated with PCL. In one study, Spearman et al studied a conductive interpenetrating network of polypyrrole-PCL for use as an electroactive substrate for cardiomyocyte culture. Results of this work indicated that conductive polypyrrole-PCL films effectively supported cardiomyocyte culture. In addition, the treatment of PCL films with sodium hydroxide resulted in increased cardiomyocyte attachment, decreased cell size, and decreased surface hydrophobicity. Furthermore, cardiomyocytes were cultured on the electrically-conductive polypyrrole-PCL, and results illustrated that more cells had peripherally localized gap junction protein Cx43 on the polypyrrole-PCL (60.3 ± 4.3%) as compared to cells on the sodium hydroxide-treated PCL (46.6 ± 5.7%). Cx43 gene expression remained unchanged between materials. Additionally, HL-1 cardiomyocytes grown on polypyrrole-PCL and PCL films were similar to Cx43 gene expression. However, the Cx43 protein localization differed: when HL-1 cells were cultured on polypyrrole-PCL, Cx43 was more frequently observed to be along the cell periphery. HL-1 cells grown on the conductive polypyrrole-PCL films (following 10–12 days of culture on the films) showed significantly lower calcium transient duration (910 ± 63 ms) and significantly faster calcium transient velocities (1612 ± 143 µm/s) when compared to HL-1 cells grown on the control PCL films (1130 ± 20 ms, 1129 ± 247 µm/s).127
Polyurethanes
Polyurethanes (PUs), a series of synthetic polymers, are extensively used in medical applications (such as an artificial heart, bladders, heart assist balloon pumps, and vascular grafts). PUs have achieved biomedical relevance because they have excellent biocompatibility, good mechanical properties, stability, and relatively long durability.128 However, PUs exhibit a long degradation time which limit its application in cardiac tissue engineering.104 Recently, the incorporation of a nanostructured filler material into PUs and its effects on scaffold properties were investigated for cardiovascular tissue applications. Specifically, graphene‐silver/polyurethane nanofibrous scaffolds were fabricated via an electrospinning technique for cardiac tissue engineering by Nazari et al. Results indicated that the incorporation of rGO‐Ag nanocomposites into PU nanofibers significantly increased its electrical conductivity, tensile strength, and wettability. Moreover, in vitro studies for these biocompatible scaffolds exhibited enhanced cellular attachment and an inducement of cardiogenic differentiation of cardiac progenitor cells (hCPCs) without providing any cardiogenic biochemical supplements in the cell culture medium.129
In other study, Shokraei et al fabricated carbon nanotube (CNT)/PU nanofibrous scaffolds using a simultaneous electro spray/spinning method. Results indicated that adding CNTs enhanced electrical conductivity, Young’s modulus, tensile strength, and hydrophilicity of the CNT/PU nanocomposites. Also, increasing CNTs decreased the diameter of the composite nanofibers. Moreover, the simultaneous electro spray/spinning method led to the fabrication of scaffolds with good mechanical properties and excellent conductivity at low CNT concentrations. The scaffolds revealed suitable attachment, high viability, and proliferation of cardiomyoblasts on these composite patches.130
Poly(Ethylene Glycol)
Poly(ethylene glycol) (PEG), a common synthetic biodegradable polymer, was synthesized by ring-opening polymerization of ethylene oxide and has been used as a tissue engineering biomaterial.131–133 PEG properties, including solubility in water and organic solvents, nontoxicity and low cell adhesion and protein binding, make it a suitable candidate for tissue engineering efforts.107,134 However, the PEG polymer is bio-inert, thus, it is not an ideal environment for cell growth, adhesion, and survival.106 PEG-based gels are usually used in cardiac regeneration approaches because they have advantages over natural hydrogels, such as easy control of chemical composition and scaffold architecture, and adjustable mechanical properties.131 In one study, Somekawa et al investigated the effect of thermoresponsive PLA–PEG gel injection on LV remodeling in a rat MI Model compared with an alginate gel as a positive reference and with saline as an experimental control in terms of infarct size, LV cavity area, and CD68 positive immunostaining. Result showed that the PLLA-PEG/PDLA-PEG and alginate gel improved %FS and preserved cardiac function and decreased infract size in comparison with saline (after 4 weeks). In addition, a greater reduction in LV cavity area was observed for the PLLA-PEG/PDLA-PEG gel in comparison with the alginate gel.135 Synthetic polymers, however, have some drawbacks such as a lack of cell attachment and less biocompatibility in cardiac tissue engineering.136
Natural/Synthetic Composites
In general, biodegradable polymers for cardiac tissue engineering have some attractive properties such as low toxicity and biocompatibility. Natural polymers have advantages in cardiac tissue engineering such as better biodegradability, renewability, and low toxicity while synthetic polymers have exhibited improved tailored properties, such as mechanical strength, conductivity and degradation rate. A strategy for improvement is to use the advantages of both natural and synthetic polymers for cardiac tissue engineering through the design of natural/synthetic composites. In one study, PLA/chitosan nanofibrous scaffolds with different ratios of PLA to chitosan were fabricated by conventional electrospinning for cardiac tissue engineering. According to the results, the scaffolds with aligned and random PLA/chitosan nanofibers promoted cardiomyocyte attachment and viability. In particular, biocompatibility and mechanical strength of the scaffolds with aligned fibers were higher than scaffolds with randomly oriented fibers. Furthermore, scaffolds with aligned fibers with a PLA:chitosan ratio of 7:1 (w:w) increased cell-scaffold interactions137,138 (Figure 11).
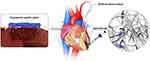 |
Figure 11 A schematic illustration of a typical cardiac tissue engineering scaffold based on natural and synthesis polymers. |
A recent strategy to obtain new properties and enhanced properties is the combination of inorganic nanoparticles in biocompatible nanocomposite hydrogels. For example, Liu et al developed TiO2 nanoparticles fabricated PEG/chitosan nanocomposite hydrogels with enhanced physico-chemical and biological properties for cardiac tissue repair. In this study, TiO2 nanoparticles were homogeneously dispersed and cross-linked on the surface of hydrogels. Results indicated that the TiO2-PEG/chitosan hydrogels, as compared to the PEG/chitosan hydrogels, exhibited an enhanced compressive modulus and favorable swelling behavior. Also, the nanoparticle network enhanced cell retention activity and adhesion of cardiomyocytes on the TiO2-PEG/chitosan hydrogels. In addition, a TiO2-PEG/chitosan hydrogel demonstrated excellent cell-hydrogel matrix interactions, with more healthy and synchronous activity.139
In other work, Chen et al studied electrospun gelatin/PCL/graphene nanofibers for use as a bypass tract for electrical conduction. In this study, in vitro, neonatal rat ventricular myocytes were seeded onto scaffolds with different concentrations of graphene, and in vivo, the scaffolds with different fractions of graphene were implanted into rats. Results of this study illustrated that if the mass fraction of graphene was lower than 0.5%, the cells grew and survived well on the hybrid scaffolds. Moreover, the implanted scaffolds exhibited no inflammatory cells around the nanomaterials after being implanting into rats for 4, 8 or 12 weeks. In addition, the gelatin/PCL/graphene nanofibers exhibited favorable electrical conductivity and biological properties which may be suitable for their use in the treatment of atrioventricular block.140 Table 3 provides a review of recent natural/synthetic composites used in cardiac tissue engineering.
 |
Table 3 Recent Natural/Synthetic Composites in Cardiac Tissue Engineering and Their Advantages |
Conclusions and Future Perspectives
Nanotechnology not only has the potential to be used in the treatment of heart disease, but also to significantly improve it. Nanomedicine can be used to create cardiac tissue engineering materials that mimic the natural cardiovascular tissue more than those made conventionally. Further, nanoparticles can be made that activate select cells to improve cardiac tissue engineering. Investments should be made so that nanomaterials and other related technologies can reach clinical trials and enter the market. In fact, as this chapter demonstrated, while nanotechnology promises a positive impact on the cardiac health of the individual, more work is needed. Specifically, in order to have the greatest possible impact on medicine, further studies on nanomaterials in vivo are needed and nanomaterial behavior in the body needs to be fully understood. Further, missing from all of this incorporation of nanomedicine into cardiovascular applications is preventive medicine. While a great deal of attention has been paid on developing improved materials for healing cardiac tissue, little to no effort has been paid to prevent cardiovascular disease with nanomaterials.
Moreover, there are many studies presented here on the synthesis and development of polymer nanocomposite patches in cardiac tissue engineering with very promising results. However, presently, the ideal biodegradable polymer with all essential requirements for cardiac tissue engineering, does not exist. This requires specific improved properties, including biocompatibility, which must be considered when selecting a suitable scaffold. Further research is needed on the synthesis of compatible polymer compounds, both in vitro and in vivo, as well as clinical studies. Consequently, some strategies have been developed to modify the properties of biodegradable polymers, such as the incorporation of additional materials into a polymer to create a composite material to improve cardiac tissue engineering.
In summary, here, we reviewed recent advances of biodegradable synthetic polymers, natural materials, and nanomedicine which have been utilized for improving cardiac tissue engineering applications. Presently, the ideal cardiac tissue engineering material does not exist, but nanomedicine promises to be an integral partner. Such nanomedicine results give strong hope for the design of a healthy and active heart, no matter what damage or disease has occurred.
Acknowledgment
We would like to thank Prof. Rassoul Dinarvand for his help in revising the manuscript.
Disclosure
At the time of the review, Masoumehossadat Hosseini was an employee of Soroush Mana Pharmed, Pharmaceutical Holding, Golrang Industrial Group, Tehran, Iran. The authors report no other possible conflicts of interest in this work.
References
1. Curtis MW, Russell B. Cardiac tissue engineering. J Cardiovasc Nurs. 2009;24(2):87.
2. Kai D, Prabhakaran MP, Jin G, et al. Polypyrrole‐contained electrospun conductive nanofibrous membranes for cardiac tissue engineering. J Biomed Mater Res A. 2011;99(3):376–385. doi:10.1002/jbm.a.33200
3. Nour S, Baheiraei N, Imani R, et al. Bioactive materials: a comprehensive review on interactions with biological microenvironment based on the immune response. J Bionic Eng. 2019;16(4):563–581. doi:10.1007/s42235-019-0046-z
4. Rabiee N, Yaraki MT, Garakani SM, et al. Recent advances in porphyrin-based nanocomposites for effective targeted imaging and therapy. Biomaterials. 2019;119707.
5. Bahrami S, Baheiraei N, Mohseni M, et al. Three-dimensional graphene foam as a conductive scaffold for cardiac tissue engineering. J Biomater Appl. 2019;0885328219839037.
6. Nasseri B, Soleimani N, Rabiee N, et al. Point-of-care microfluidic devices for pathogen detection. Biosens Bioelectron. 2018;117:112–128. doi:10.1016/j.bios.2018.05.050
7. Bahrami S, Baheiraei N, Mohseni M, et al. Three-dimensional graphene foam as a conductive scaffold for cardiac tissue engineering. J Biomater Appl. 2019;34(1):74–85. doi:10.1177/0885328219839037
8. Toudeshkchoui MG, Rabiee N, Rabiee M, et al. Microfluidic devices with gold thin film channels for chemical and biomedical applications: a review. Biomed Microdevices. 2019;21(4):93. doi:10.1007/s10544-019-0439-0
9. Bearzi C, Gargioli C, Baci D, et al. PlGF–MMP9-engineered iPS cells supported on a PEG–fibrinogen hydrogel scaffold possess an enhanced capacity to repair damaged myocardium. Cell Death Dis. 2014;5(2):e1053. doi:10.1038/cddis.2014.12
10. Hajebi S, Rabiee N, Bagherzadeh M, et al. Stimulus-responsive polymeric nanogels as smart drug delivery systems. Acta Biomater. 2019;92:1–18. doi:10.1016/j.actbio.2019.05.018
11. Nour S, et al. A review of accelerated wound healing approaches: biomaterial-assisted tissue remodeling. J Mater Sci Mater Med. 2019;30(10):120.
12. Zimmermann W-H, Eschenhagen T. Cardiac tissue engineering for replacement therapy. Heart Fail Rev. 2003;8(3):259–269. doi:10.1023/A:1024725818835
13. Vunjak-Novakovic G, Tandon N, Godier A, et al. Challenges in cardiac tissue engineering. Tissue Eng Part B Rev. 2009;16(2):169–187. doi:10.1089/ten.teb.2009.0352
14. Eng G, et al. Cardiac tissue engineering. In: Principles of Tissue Engineering. Elsevier; 2014:771–792.
15. Shachar M, Cohen S. Cardiac tissue engineering, ex-vivo: design principles in biomaterials and bioreactors. Heart Fail Rev. 2003;8(3):271–276. doi:10.1023/A:1024729919743
16. Huang S, Yang Y, Yang Q, et al. Engineered circulatory scaffolds for building cardiac tissue. J Thorac Dis. 2018;10(Suppl 20):S2312. doi:10.21037/jtd.2017.12.92
17. Saludas L, Pascual-Gil S, Prósper F, et al. Hydrogel based approaches for cardiac tissue engineering. Int J Pharm. 2017;523(2):454–475. doi:10.1016/j.ijpharm.2016.10.061
18. Rodrigues ICP, Kaasi A, Maciel Filho R, et al. Cardiac tissue engineering: current state-of-the-art materials, cells and tissue formation. Einstein (São Paulo). 2018;16(3). doi:10.1590/s1679-45082018rb4538.
19. Kroeze R, Helder M, Govaert L, et al. Biodegradable polymers in bone tissue engineering. Materials. 2009;2(3):833–856. doi:10.3390/ma2030833
20. Cortizo MS, Belluzo MS. Biodegradable polymers for bone tissue engineering. In: Industrial Applications of Renewable Biomass Products. Springer, Cham; 2017:47–74.
21. Vroman I, Tighzert L. Biodegradable polymers. Materials. 2009;2(2):307–344. doi:10.3390/ma2020307
22. Garbayo E, Pascual-Gil S, Prosper F, Blanco-Prieto MJ. Bioresorbable polymers for next-generation cardiac scaffolds. In: Bioresorbable Polymers for Biomedical Applications. Elsevier; 2017:445–467.
23. Hasan A, Khattab A, Islam MA, et al. Injectable hydrogels for cardiac tissue repair after myocardial infarction. Advan Sci. 2015;2(11):1500122. doi:10.1002/advs.201500122
24. Chandarana M, Curtis A, Hoskins C. The use of nanotechnology in cardiovascular disease. Appl Nanosci. 2018;8(7):1607–1619. doi:10.1007/s13204-018-0856-z
25. Passaro F, Testa G, Ambrosone L, et al. Nanotechnology-based cardiac targeting and direct cardiac reprogramming: the Betrothed. Stem Cells Int. 2017;2017:4940397. doi:10.1155/2017/4940397
26. Huang H-J, Tsai Y-L, Lin S-H, et al. Smart polymers for cell therapy and precision medicine. J Biomed Sci. 2019;26(1):73. doi:10.1186/s12929-019-0571-4
27. Puoci F, Biodegradable natural polymers. In: Advanced Polymers in Medicine. Springer; 2015:33–66.
28. Dhandayuthapani B, Yoshida Y, Maekawa T, et al. Polymeric scaffolds in tissue engineering application: a review. Int J Polym Sci. 2011;2011:1–19. doi:10.1155/2011/290602
29. Li Y, Meng H, Liu Y, et al. Fibrin gel as an injectable biodegradable scaffold and cell carrier for tissue engineering. Sci World J. 2015;2015:1–10. doi:10.1155/2015/685690
30. Barsotti MC, Felice F, Balbarini A, et al. Fibrin as a scaffold for cardiac tissue engineering. Biotechnol Appl Biochem. 2011;58(5):301–310. doi:10.1002/bab.49
31. Dong C, Lv Y. Application of collagen scaffold in tissue engineering: recent advances and new perspectives. Polymers. 2016;8(2):42. doi:10.3390/polym8020042
32. Lin YL, Chen C-P, Lo C-M, et al. Stiffness‐controlled three‐dimensional collagen scaffolds for differentiation of human Wharton’s jelly mesenchymal stem cells into cardiac progenitor cells. J Biomed Mater Res A. 2016;104(9):2234–2242. doi:10.1002/jbm.a.35762
33. Yang G, Xiao Z, Ren X, et al. Enzymatically crosslinked gelatin hydrogel promotes the proliferation of adipose tissue-derived stromal cells. PeerJ. 2016;4:e2497. doi:10.7717/peerj.2497
34. Feyen DA, Gaetani R, Deddens J, et al. Gelatin microspheres as vehicle for cardiac progenitor cells delivery to the myocardium. Adv Healthc Mater. 2016;5(9):1071–1079. doi:10.1002/adhm.201500861
35. Nikkhah M, Akbari M, Paul A, et al. Gelatin‐based biomaterials for tissue engineering and stem cell bioengineering. Biomater Nat Advan Ther. 2016;37–62.
36. Masutani EM, Kinoshita CK, Tanaka TT, et al. Increasing thermal stability of gelatin by UV-induced cross-linking with glucose. Int J Biomater. 2014;2014:1–9. doi:10.1155/2014/979636
37. Kumar Giri T, Thakur D, Badwaik H, et al. Alginate based hydrogel as a potential biopolymeric carrier for drug delivery and cell delivery systems: present status and applications. Curr Drug Deliv. 2012;9(6):539–555. doi:10.2174/156720112803529800
38. Sun J, Tan H. Alginate-based biomaterials for regenerative medicine applications. Materials. 2013;6(4):1285–1309. doi:10.3390/ma6041285
39. Ruvinov E, Cohen S. Alginate biomaterial for the treatment of myocardial infarction: progress, translational strategies, and clinical outlook: from ocean algae to patient bedside. Adv Drug Deliv Rev. 2016;96:54–76. doi:10.1016/j.addr.2015.04.021
40. Cadar AG, Feaster TK, Durbin MD, et al. Production of single contracting human induced pluripotent stem cell‐derived cardiomyocytes: matrigel mattress technique. Curr Protoc Stem Cell Biol. 2017;42(1):
41. Feijão T, Torress AL, Araujo M, Barrias CC. Peptide-modified hydrogels for therapeutic vascularization. In: Biomedical Applications of Functionalized Nanomaterials. Elsevier; 2018:599–620.
42. Sivashankari P, Prabaharan M. Chitosan/carbon-based nanomaterials as scaffolds for tissue engineering. In: Biopolymer-Based Composites. Elsevier; 2017:381–397.
43. Jing X, Mi H-Y, Napiwocki BN, et al. Mussel-inspired electroactive chitosan/graphene oxide composite hydrogel with rapid self-healing and recovery behavior for tissue engineering. Carbon. 2017;125:557–570. doi:10.1016/j.carbon.2017.09.071
44. Croisier F, Jérôme C. Chitosan-based biomaterials for tissue engineering. Eur Polym J. 2013;49(4):780–792. doi:10.1016/j.eurpolymj.2012.12.009
45. Perka C, Spitzer R-S, Lindenhayn K, et al. Matrix‐mixed culture: new methodology for chondrocyte culture and preparation of cartilage transplants. J Biomed Mater Res. 2000;49(3):305–311. doi:10.1002/(SICI)1097-4636(20000305)49:3<305::AID-JBM2>3.0.CO;2-9
46. Janmey PA, Winer JP, Weisel JW. Fibrin gels and their clinical and bioengineering applications. J R Soc Interface. 2008;6(30):1–10. doi:10.1098/rsif.2008.0327
47. Shaikh FM, Callanan A, Kavanagh EG, et al. Fibrin: a natural biodegradable scaffold in vascular tissue engineering. Cells Tissues Organs. 2008;188(4):333–346. doi:10.1159/000139772
48. Kim J-T, Chung HJ, Seo J-Y, et al. A fibrin-supported myocardial organ culture for isolation of cardiac stem cells via the recapitulation of cardiac homeostasis. Biomaterials. 2015;48:66–83. doi:10.1016/j.biomaterials.2015.01.041
49. Shen D, Tang J, Hensley MT, et al. Effects of matrix metalloproteinases on the performance of platelet fibrin gel spiked with cardiac stem cells in heart repair. Stem Cells Transl Med. 2016;5(6):793–803. doi:10.5966/sctm.2015-0194
50. Melly L, Grosso A, Pop CS, et al. Stimulation of cardiac angiogenesis through growth factors with a fibrin gel delivery platform. J Heart Lung Transplant. 2019;38(4):S246. doi:10.1016/j.healun.2019.01.607
51. Ricard-Blum S. The collagen family. Cold Spring Harb Perspect Biol. 2011;3(1):a004978. doi:10.1101/cshperspect.a004978
52. Nair LS, Laurencin CT. Polymers as biomaterials for tissue engineering and controlled drug delivery. In: Tissue Engineering I. Springer, Berlin, Heidelberg; 2005:47–90.
53. Yang Y-L, Motte S, Kaufman LJ. Pore size variable type I collagen gels and their interaction with glioma cells. Biomaterials. 2010;31(21):5678–5688. doi:10.1016/j.biomaterials.2010.03.039
54. Ravichandran R, Islam MM, Alarcon EI, et al. Functionalised type-I collagen as a hydrogel building block for bio-orthogonal tissue engineering applications. J Mater Chem B. 2015;4(2):318–326. doi:10.1039/C5TB02035B
55. Mirsadraee S, Wilcox HE, Korossis SA, et al. Development and characterization of an acellular human pericardial matrix for tissue engineering. Tissue Eng. 2006;12(4):763–773. doi:10.1089/ten.2006.12.763
56. Ariganello MB, Labow RS, Lee JM. In vitro response of monocyte‐derived macrophages to a decellularized pericardial biomaterial. J Biomed Mater Res Part A. 2010;93(1):280–288.
57. Xu T, Molnar P, Gregory C, et al. Electrophysiological characterization of embryonic hippocampal neurons cultured in a 3D collagen hydrogel. Biomaterials. 2009;30(26):4377–4383. doi:10.1016/j.biomaterials.2009.04.047
58. Mirsadraee S, Wilcox HE, Watterson KG, et al. Biocompatibility of acellular human pericardium. J Surg Res. 2007;143(2):407–414. doi:10.1016/j.jss.2007.01.026
59. Punnoose AM, Elamparithi A, Kuruvilla S. Electrospun Type 1 collagen matrices using a novel benign solvent for cardiac tissue engineering. J Cell Physiol. 2015.
60. Joanne P, Kitsara M, Boitard S-E, et al. Nanofibrous clinical-grade collagen scaffolds seeded with human cardiomyocytes induces cardiac remodeling in dilated cardiomyopathy. Biomaterials. 2016;80:157–168. doi:10.1016/j.biomaterials.2015.11.035
61. Sun H, Zhou J, Huang Z, et al. Carbon nanotube-incorporated collagen hydrogels improve cell alignment and the performance of cardiac constructs. Int J Nanomedicine. 2017;12:3109. doi:10.2147/IJN.S128030
62. Yu H, Zhao H, Huang C, et al. Mechanically and electrically enhanced CNT–collagen hydrogels as potential scaffolds for engineered cardiac constructs. ACS Biomater Sci Eng. 2017;3(11):3017–3021. doi:10.1021/acsbiomaterials.6b00620
63. Hosoyama K, Ahumada M, McTiernan CD, et al. Nanoengineered electroconductive collagen-based cardiac patch for infarcted myocardium repair. ACS Appl Mater Interfaces. 2018;10(51):44668–44677. doi:10.1021/acsami.8b18844
64. Corda S, Samuel J-L, Rappaport L. Extracellular matrix and growth factors during heart growth. Heart Fail Rev. 2000;5(2):119–130. doi:10.1023/A:1009806403194
65. Alonzo M, AnilKumar S, Roman B, et al. 3D Bioprinting of cardiac tissue and cardiac stem cell therapy. Transl Res. 2019;211:64–83. doi:10.1016/j.trsl.2019.04.004
66. Elamparithi A, Punnoose AM, Paul SFD, et al. Gelatin electrospun nanofibrous matrices for cardiac tissue engineering applications. Int J Polymeric Mater Polymeric Biomater. 2017;66(1):20–27. doi:10.1080/00914037.2016.1180616
67. Elsayed Y, Lekakou C, Labeed F, et al. Fabrication and characterisation of biomimetic, electrospun gelatin fibre scaffolds for tunica media-equivalent, tissue engineered vascular grafts. Mater Sci Eng C. 2016;61:473–483. doi:10.1016/j.msec.2015.12.081
68. Tijore A, Irvine SA, Sarig U, et al. Contact guidance for cardiac tissue engineering using 3D bioprinted gelatin patterned hydrogel. Biofabrication. 2018;10(2):025003. doi:10.1088/1758-5090/aaa15d
69. Slaughter BV, Khurshid SS, Fisher OZ, et al. Hydrogels in regenerative medicine. Advan Mater. 2009;21(32‐33):3307–3329. doi:10.1002/adma.200802106
70. Rosellini E, Cristallini C, Barbani N, et al. Preparation and characterization of alginate/gelatin blend films for cardiac tissue engineering. J Biomed Mater Res Part A. 2009;91(2):447–453. doi:10.1002/jbm.a.32216
71. Sondermeijer HP, et al. The use of biocompatible alginate scaffolds covalently modified with cyclic RGDfK peptides to improve survival of transplanted cells and angiogenesis in damaged myocardium. J Tissue Sci Eng. 2017.
72. Hao T, Li J, Yao F, et al. Injectable fullerenol/alginate hydrogel for suppression of oxidative stress damage in brown adipose-derived stem cells and cardiac repair. ACS Nano. 2017;11(6):5474–5488. doi:10.1021/acsnano.7b00221
73. Izadifar M, Babyn P, Kelly ME, et al. Bioprinting pattern-dependent electrical/mechanical behavior of cardiac alginate implants: characterization and ex vivo phase-contrast microtomography assessment. Tissue Eng Part C Methods. 2017;23(9):548–564. doi:10.1089/ten.tec.2017.0222
74. Chae M, Hunter-Smith DJ, Murphy SV, et al. 3D bioprinting adipose tissue for breast reconstruction. In: 3D Bioprinting for Reconstructive Surgery. Elsevier; 2018:305–353.
75. Estrada V, Tekinay A, Müller HW. Neural ECM mimetics. In: Progress in Brain Research. Elsevier; 2014:391–413.
76. Arnaoutova I, George J, Kleinman HK, et al. The endothelial cell tube formation assay on basement membrane turns 20: state of the science and the art. Angiogenesis. 2009;12(3):267–274. doi:10.1007/s10456-009-9146-4
77. Feaster TK, Cadar AG, Wang L, et al. Matrigel mattress: a method for the generation of single contracting human-induced pluripotent stem cell–derived cardiomyocytes. Circ Res. 2015;117(12):995–1000. doi:10.1161/CIRCRESAHA.115.307580
78. Zhang L, Li X, Yu X, et al. Construction of vascularized pacemaker tissues by seeding cardiac progenitor cells and endothelial progenitor cells into Matrigel. Life Sci. 2017;179:139–146. doi:10.1016/j.lfs.2017.05.007
79. Hudson S, Smith C. Polysaccharides: chitin and chitosan: chemistry and technology of their use as structural materials. In: Biopolymers from Renewable Resources. Springer; 1998:96–118.
80. Dutta PK. Chitin and Chitosan for Regenerative Medicine. Springer; 2016.
81. Deng C, Li F, Griffith M, Reul M, Suuronen EJ. Application of Chitosan‐based biomaterials for blood vessel regeneration. In: Macromolecular Symposia. Wiley Online Library; 2010.
82. Pang Y, Qin A, Lin X, et al. Biodegradable and biocompatible high elastic chitosan scaffold is cell-friendly both in vitro and in vivo. Oncotarget. 2017;8(22):35583.
83. Xu B, Li Y, Deng B, et al. Chitosan hydrogel improves mesenchymal stem cell transplant survival and cardiac function following myocardial infarction in rats. Exp Ther Med. 2017;13(2):588–594. doi:10.3892/etm.2017.4026
84. Díaz-Herráez P, Saludas L, Pascual-Gil S, et al. Transplantation of adipose-derived stem cells combined with neuregulin-microparticles promotes efficient cardiac repair in a rat myocardial infarction model. J Controlled Release. 2017;249:23–31. doi:10.1016/j.jconrel.2017.01.026
85. Aussel A, Thébaud NB, Bérard X, et al. Chitosan-based hydrogels for developing a small-diameter vascular graft: in vitro and in vivo evaluation. Biomed Mater. 2017;12(6):065003. doi:10.1088/1748-605X/aa78d0
86. Baei P, Jalili-Firoozinezhad S, Rajabi-Zeleti S, et al. Electrically conductive gold nanoparticle-chitosan thermosensitive hydrogels for cardiac tissue engineering. Mater Sci Eng C. 2016;63:131–141. doi:10.1016/j.msec.2016.02.056
87. Abdelhalim MAK. Exposure to gold nanoparticles produces cardiac tissue damage that depends on the size and duration of exposure. Lipids Health Dis. 2011;10(1):205. doi:10.1186/1476-511X-10-205
88. Kalishwaralal K, Jeyabharathi S, Sundar K, et al. A novel biocompatible chitosan–Selenium nanoparticles (SeNPs) film with electrical conductivity for cardiac tissue engineering application. Mater Sci Eng C. 2018;92:151–160. doi:10.1016/j.msec.2018.06.036
89. Kalishwaralal K, Jeyabharathi S, Sundar K, et al. Comparative analysis of cardiovascular effects of selenium nanoparticles and sodium selenite in zebrafish embryos. Artif, Nanomed Biotechnol. 2016;44(3):990–996. doi:10.3109/21691401.2015.1008507
90. Valente T, Silva D, Gomes P, Fernandes M, Santos J, Sencadas V. Effect of sterilization methods on electrospun poly (lactic acid)(PLA) fiber alignment for biomedical applications. ACS applied materials & interfaces. 2016;8(5):3241–3249.
91. Ige OO, Umoru LE, Aribo S. Natural products: a minefield of biomaterials. ISRN Mater Sci. 2012;2012:1–20. doi:10.5402/2012/983062
92. Guo B, Ma PX. Synthetic biodegradable functional polymers for tissue engineering: a brief review. Sci China Chem. 2014;57(4):490–500. doi:10.1007/s11426-014-5086-y
93. Sanko V, Sahin I, Sezer UA, Sezer S. A versatile method for the synthesis of poly (glycolic acid): high solubility and tunable molecular weights. Polymer J. 2019;1.
94. Niaounakis M. Medical, dental, and pharmaceutical applications. In: Niaounakis M, editor. Biopolymers: Applications and Trends. William Andrew Publishing; 2015:291–405.
95. Bertuoli PT, Ordoño J, Armelin E, et al. Electrospun conducting and biocompatible uniaxial and core–shell fibers having poly(lactic acid), poly(ethylene glycol), and polyaniline for cardiac tissue engineering. ACS Omega. 2019;4(2):3660–3672. doi:10.1021/acsomega.8b03411
96. Lopes MS, Jardini A, Maciel Filho R. Poly (lactic acid) production for tissue engineering applications. Procedia Eng. 2012;42:1402–1413. doi:10.1016/j.proeng.2012.07.534
97. Lü J-M, Wang X, Marin-Muller C, et al. Current advances in research and clinical applications of PLGA-based nanotechnology. Expert Rev Mol Diagn. 2009;9(4):325–341. doi:10.1586/erm.09.15
98. Pan Z, Ding J. Poly (lactide-co-glycolide) porous scaffolds for tissue engineering and regenerative medicine. Interface Focus. 2012;2(3):366–377. doi:10.1098/rsfs.2011.0123
99. Tallawi M, Rosellini E, Barbani N, et al. Strategies for the chemical and biological functionalization of scaffolds for cardiac tissue engineering: a review. J R Soc Interface. 2015;12(108):20150254. doi:10.1098/rsif.2015.0254
100. Jirofti N, Mohebbi-Kalhori D, Samimi A, et al. Small-diameter vascular graft using co-electrospun composite PCL/PU nanofibers. Biomed Mater. 2018;13(5):055014. doi:10.1088/1748-605X/aad4b5
101. Song L, Ahmed MF, Li Y, et al. PCL-PDMS-PCL copolymer-based microspheres mediate cardiovascular differentiation from embryonic stem cells. Tissue Eng Part C Methods. 2017;23(10):627–640. doi:10.1089/ten.tec.2017.0307
102. Mondal D, Griffith M, Venkatraman SS. Polycaprolactone-based biomaterials for tissue engineering and drug delivery: current scenario and challenges. Int J Polymeric Mater Polymeric Biomater. 2016;65(5):255–265. doi:10.1080/00914037.2015.1103241
103. Mano JF, Sousa RA, Boesel LF, et al. Bioinert, biodegradable and injectable polymeric matrix composites for hard tissue replacement: state of the art and recent developments. Compos Sci Technol. 2004;64(6):789–817. doi:10.1016/j.compscitech.2003.09.001
104. Gostev AA, Karpenko AA, Laktionov PP. Polyurethanes in cardiovascular prosthetics. Polymer Bull. 2018;75(9):4311–4325. doi:10.1007/s00289-017-2266-x
105. Kucinska-Lipka J, Gubanska I, Janik H, et al. Fabrication of polyurethane and polyurethane based composite fibres by the electrospinning technique for soft tissue engineering of cardiovascular system. Mater Sci Eng C. 2015;46:166–176. doi:10.1016/j.msec.2014.10.027
106. Rane AA, Chuang JS, Shah A, et al. Increased infarct wall thickness by a bio-inert material is insufficient to prevent negative left ventricular remodeling after myocardial infarction. PLoS One. 2011;6(6):e21571. doi:10.1371/journal.pone.0021571
107. Alcantar NA, Aydil ES, Israelachvili JN. Polyethylene glycol–coated biocompatible surfaces. J Biomed Mater Res. 2000;51(3):343–351. doi:10.1002/1097-4636(20000905)51:3<343::AID-JBM7>3.0.CO;2-D
108. Niaounakis M. Biopolymers: Processing and Products. William Andrew; 2014.
109. Ricklefs MKorossis S, Haverich A, Schilling T. Polymeric Scaffolds for Bioartificial Cardiovascular Prostheses. Scaffolds in Tissue Engineering Materials, Technologies and Clinical Applications. 2017:267.
110. Zhang Z, et al. Biodegradable polymers. In: Handbook of Polymer Applications in Medicine and Medical Devices. Elsevier; 2014:303–335.
111. Huang X, Zauscher S, Klitzman B, et al. Peptide interfacial biomaterials improve endothelial cell adhesion and spreading on synthetic polyglycolic acid materials. Ann Biomed Eng. 2010;38(6):1965–1976. doi:10.1007/s10439-010-9986-5
112. Kannan RY, Salacinski HJ, Butler PE, et al. Current status of prosthetic bypass grafts: a review. J Biomed Mater Res Part B. 2005;74(1):570–581.
113. Hadasha W, Bezuidenhout D. Poly (lactic acid) as biomaterial for cardiovascular devices and tissue engineering applications. In: Industrial Applications of Poly (Lactic Acid). Springer; 2017:51–77.
114. Liu Q, Tian S, Zhao C, et al. Porous nanofibrous poly (L-lactic acid) scaffolds supporting cardiovascular progenitor cells for cardiac tissue engineering. Acta Biomater. 2015;26:105–114. doi:10.1016/j.actbio.2015.08.017
115. Dong H, Prasad S, Nyame V, Jones WE. Sub-micrometer conducting polyaniline tubes prepared from polymer fiber templates. Chem Mater. 2004;16(3):371–373.
116. Giménez CS, Olea FD, Locatelli P, et al. Effect of poly (l-lactic acid) scaffolds seeded with aligned diaphragmatic myoblasts overexpressing connexin-43 on infarct size and ventricular function in sheep with acute coronary occlusion. Artif Cells Nanomedicine Biotechnol. 2018;46(sup3):S717–S724. doi:10.1080/21691401.2018.1508029
117. Wang L, Wu Y, Hu T, et al. Electrospun conductive nanofibrous scaffolds for engineering cardiac tissue and 3D bioactuators. Acta Biomater. 2017;59:68–81. doi:10.1016/j.actbio.2017.06.036
118. Arya G, Kumari RM, Sharma N, et al. Polymeric nanocarriers for site-specific gene therapy. In: Drug Targeting and Stimuli Sensitive Drug Delivery Systems. Elsevier; 2018:689–714.
119. Mulinti P, Brooks JE, Lervick B, et al. Strategies to improve the hemocompatibility of biodegradable biomaterials. In: Hemocompatibility of Biomaterials for Clinical Applications. Elsevier; 2018:253–278.
120. Zamani M, Prabhakaran MP, Thian ES, et al. Controlled delivery of stromal derived factor-1α from poly lactic-co-glycolic acid core–shell particles to recruit mesenchymal stem cells for cardiac regeneration. J Colloid Interface Sci. 2015;451:144–152. doi:10.1016/j.jcis.2015.04.005
121. Asiri AM, Marwani HM, Khan SB, et al. Understanding greater cardiomyocyte functions on aligned compared to random carbon nanofibers in PLGA. Int J Nanomedicine. 2015;10:89.
122. Mclauchlin A, Thomas N. Biodegradable polymer nanocomposites. In: Advances in Polymer Nanocomposites. Elsevier; 2012:398–430.
123. Gaspar VM, Moreira AF, de Melo-Diogo Det al. Multifunctional nanocarriers for codelivery of nucleic acids and chemotherapeutics to cancer cells. In: Nanobiomaterials in Medical Imaging. Elsevier; 2016:163–207.
124. Gunatillake PA. Biodegradable synthetic polymers for tissue engineering. European Cells and Materials. 2003;5(1):1–16. doi:10.22203/eCM.v005a01
125. Ghaziof S, Mehdikhani-Nahrkhalaji M. Preparation, characterization, mechanical properties and electrical conductivity assessment of novel polycaprolactone/multi-wall carbon nanotubes nanocomposites for myocardial tissue engineering. Acta Physica Polonica A. 2017;131(3):428–431. doi:10.12693/APhysPolA.131.428
126. Castilho M, Feyen D, Flandes-Iparraguirre M, et al. Melt electrospinning writing of poly-hydroxymethylglycolide-co-ε-caprolactone-based scaffolds for cardiac tissue engineering. Adv Healthc Mater. 2017;6(18):1700311. doi:10.1002/adhm.201700311
127. Spearman BS, Hodge AJ, Porter JL, et al. Conductive interpenetrating networks of polypyrrole and polycaprolactone encourage electrophysiological development of cardiac cells. Acta Biomater. 2015;28:109–120. doi:10.1016/j.actbio.2015.09.025
128. Heath DE, Cooper SL. Polyurethanes. In: Biomaterials Science. Elsevier; 2013:79–82.
129. Nazari H, Azadi S, Hatamie S, et al. Fabrication of graphene‐silver/polyurethane nanofibrous scaffolds for cardiac tissue engineering. Polym Adv Technol. 2019;30(8):2086–2099. doi:10.1002/pat.4641
130. Shokraei N, Asadpour S, Shokraei S, et al. Development of electrically conductive hybrid nanofibers based on CNT‐polyurethane nanocomposite for cardiac tissue engineering. Microsc Res Tech. 2019;82(8):1316–1325. doi:10.1002/jemt.23282
131. Zhu J. Bioactive modification of poly (ethylene glycol) hydrogels for tissue engineering. Biomaterials. 2010;31(17):4639–4656. doi:10.1016/j.biomaterials.2010.02.044
132. Tan H, Marra KG. Injectable, biodegradable hydrogels for tissue engineering applications. Materials. 2010;3(3):1746–1767. doi:10.3390/ma3031746
133. Odian G. Principles of Polymerization. John Wiley & Sons; 2004.
134. Lin C-C, Anseth KS. PEG hydrogels for the controlled release of biomolecules in regenerative medicine. Pharm Res. 2009;26(3):631–643. doi:10.1007/s11095-008-9801-2
135. Somekawa S, Mahara A, Masutani K, et al. Effect of thermoresponsive poly (L-lactic acid)–poly (ethylene glycol) gel injection on left ventricular remodeling in a rat myocardial infarction model. Tissue Eng Regenerat Med. 2017;14(5):507–516. doi:10.1007/s13770-017-0067-9
136. Do AV, Khorsand B, Geary SM, et al. 3D printing of scaffolds for tissue regeneration applications. Adv Healthc Mater. 2015;4(12):1742–1762. doi:10.1002/adhm.201500168
137. Liu Y, Wang S, Zhang R. Composite poly (lactic acid)/chitosan nanofibrous scaffolds for cardiac tissue engineering. Int J Biol Macromol. 2017;103:1130–1137. doi:10.1016/j.ijbiomac.2017.05.101
138. Wang T, Ji X, Jin L, et al. Fabrication and characterization of heparin-grafted poly-L-lactic acid–chitosan core–shell nanofibers scaffold for vascular gasket. ACS applied materials & interfaces. 2013;5(9):3757–3763.
139. Liu N, Chen J, Zhuang J, et al. Fabrication of engineered nanoparticles on biological macromolecular (PEGylated chitosan) composite for bio-active hydrogel system in cardiac repair applications. Int J Biol Macromol. 2018;117:553–558. doi:10.1016/j.ijbiomac.2018.04.196
140. Chen X, Feng B, Zhu D-Q, et al. Characteristics and toxicity assessment of electrospun gelatin/PCL nanofibrous scaffold loaded with graphene in vitro and in vivo. Int J Nanomedicine. 2019;14:3669. doi:10.2147/IJN.S204971
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
