Back to Journals » Neuropsychiatric Disease and Treatment » Volume 17
Assessment of Psychological Distress and Associated Factors among Hospitalized Patients During the COVID-19 Pandemic at Selected Hospitals in Southwest Ethiopia
Authors Hambisa S , Siraj J , Mesafint G , Yimam M
Received 15 December 2020
Accepted for publication 19 February 2021
Published 22 March 2021 Volume 2021:17 Pages 885—892
DOI https://doi.org/10.2147/NDT.S297460
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Roger Pinder
Solomon Hambisa,1 Jafer Siraj,2 Gebremeskel Mesafint,3 Mohammed Yimam4
1Department of Pharmacy, College of Medicine and Health Sciences, Ambo University, Ambo, Ethiopia; 2Department of Pharmacy, College of Medicine and Health Sciences, Mizan-Tepi University, Mizan-Aman, Ethiopia; 3Department of Nursing, College of Medicine and Health Sciences, Mizan-Tepi University, Mizan-Aman, Ethiopia; 4Department of Pharmacy, College of Health Sciences, Debre Brehan University, Debre Brehan, Ethiopia
Correspondence: Solomon Hambisa
Department of Pharmacy, College of Medicine and Health Sciences, Ambo University, PO Box 19, Ambo, Ethiopia
Email [email protected]
Background: The aim of this study was to assess the prevalence of psychological distress and associated factors among hospitalized patients during the COVID-19 pandemic at three selected hospitals in southwest Ethiopia.
Methods: An institution-based cross-sectional study design was conducted among hospitalized patients during the COVID-19 pandemic at Mizan-Tepi University Teaching Hospital, Tepi General Hospital, and Gebre Tsadik Shawo General Hospital, southwest Ethiopia from May 10 to August 10, 2020. Sample size was computed using a single-proportion formula, and systematic sampling was employed to recruit study participants. Data were collected using a structured interviewer-administered questionnaire. Psychological distress was assessed with the Kessler Psychological Distress Scale, which has been validated in Ethiopia. SPSS 21.0 was used for analysis. Descriptive statistics were calculated to characteristize the study population. Predictors of psychological distress were identified by logistic regression analyses.
Results: Among the 337 study participants enrolled, about 41% were aged 25– 34 years. The overall prevalence of psychological distress was 57.9% (95% CI 52.8%– 63.5%). Being female (AOR 3.69, 95% CI 2.08– 6.55), having high (AOR 5.45, 95% CI 2.35– 12.66) and medium perceived life threat (AOR 3.37, 95% CI 1.75– 6.48), poor (AOR 3.97, 95% CI 1.70– 9.29) and moderate social support (AOR 3.17, 95% CI 1.36– 7.41), and current khat use (AOR 4.16, 95% CI 1.67– 10.35) were statistically associated with psychological distress during the COVID-19 pandemic at P value < 0.05.
Conclusion: The prevalence of psychological distress was high among hospitalized patients during the COVID-19 pandemic. The study findings highlight the need to develop psychological support strategies to improve mental health and psychological resilience.
Keywords: psychological distress, SARS-CoV2, hospitalized patients, Southwestern Ethiopia
Background
Coronaviruses are emerging respiratory viruses and known to cause illness ranging from the common cold to severe acute respiratory syndrome.1 COVID-19 initially emerged in Wuhan, China at the end of 2019 and spread dramatically to other countries. As a result, the World Health Organization (WHO) was forced to declare COVID-19 a global health emergency of international concern.2 Presently, this pandemic is becoming the most important issue and public health problem for health-care systems and governments throughout the world.3
During the pandemic, fear, panic, and distress may increase, because of the emergence of several conditions related to this infectious disease.4,5 COVID-19 is posing public mental health problems that require close attention.6 It is associated with different degrees of negative and profound mental and psychological problems to both infected and uninfected people.7–9 A lack of relevant information about disease outbreak in societies may also exacerbate the situation.4 The adverse psychological impact of infectious disease outbreak includes acute stress disorder, insomnia, posttraumatic symptoms, and depression.10 Psychological distress is defined as an unpleasant emotional experience caused by a variety of factors, which can manifest as tension, fear, anxiety, psychological instability, and even serious psychological disorders, such as depression. Psychological distress can also be caused by infectious diseases.11,12
Several studies have demonstrated an increase in mental health problems and psychological distress among healthy uninfected people caused by the increasing risk of COVID-19 infection, strict quarantine measures, mandatory home quarantine, and other events.13–15 During the current COVID-19 pandemic, >50% of the general population have rated the psychological impact of the outbreak as moderate or severe.16 Evidence-based data show that 35% of the Chinese population are psychologically distressed.17 In addition, empirical evidence has revealed that 40% of the Saudi population are distressed due to the COVID-19 pandemic, of whom approximately 33% are mildly distressed and 7% severely distressed.15 However, the majority of studies have focused on COVID-19 screening and treatment methods.18 As hospitalized patients are susceptible to complex emotional reactions and psychological distress, the present study aimed to assess psychological distress and associated factors among hospitalized patients during the COVID-19 pandemic at three selected hospitals in southwest Ethiopia.
Methods
Study Design and Setting
This institution-based cross-sectional study was conducted among hospitalized patients during the COVID-19 pandemic at Mizan-Tepi University Teaching Hospital (MTUTH), Tepi General Hospital, and Gebre Tsadik Shawo General Hospital from May 10 to August 10, 2020. MTUTH is a teaching hospital located in Mizan-Aman town, Bench Sheko zone, Southern Nations, Nationalities, and Peoples’ Region (SNNPR), southwest Ethiopia. Gebre Tsadik Shawo General Hospital is located in Bonga town, Kefa zone, SNNPR. Tepi General Hospital is located in Tepi town, Sheka zone, SNNPR. These hospitals provide inpatient and outpatient health-care services for >3 million people. The hospitals contain different wards, including surgery, internal medicine, maternity, and pediatrics, to render medical care. During the data collection period, though there was a paucity of data regarding COVID-19 infection rates and deaths in southwest Ethiopia, three individuals tested positive for the virus responsible for COVID-19 infection according to information obtained from hospitals located in this area.
Sample Size and Sampling Technique
Sample size was computed using a single-proportion formula with assumptions of a 5% margin of error (95% CI) and 50% prevalence of psychological distress among hospitalized patients. With the use of a correction formula and taking into account a 10% nonresponse rate, the estimated sample size was 337. Systematic sampling was employed to recruit study participants. All patients admitted to the internal medicine, surgery, and maternity wards of the hospitals during the data-collection period were included in the study. Patients aged ≥18 years were enrolled. Hospitalized patients that were not willing to participate in the study and those unable to respond due to severe physical and mental illness were excluded.
Data Collection
Data were collected using a structured interviewer-administered questionnaire. The questionnaire addressed basic demographic variables and clinically related characteristics of the study participants. The outcome variable, psychological distress was assessed with the Kessler Psychological Distress Scale (K10) which has been validated in Ethiopia. It has also been validated for screening for common mental disorders in developing countries. This scale measures symptoms over the preceding 30 days by asking:
In the past 30 days, how often did you feel: nervous; so nervous that nothing could calm you down; hopeless; restless or fidgety; so restless that you could not sit still; depressed; that everything was an effort; so sad that nothing could cheer you up; worthless; tired for no good reason?
The K10 is a ten-item questionnaire developed on the basis of item response–theory models. It has five possible responses for each question, ranging from “none of the time” (score 1) to “all of the time” (score 5). All responses were collected to obtain a total score. A total score <20 was considered normal and ≥20 taken as the presence of psychological distress.19
Social support was measured with the three-item Oslo Social Support Scale,which has been used in several studies. This scale has sum scores of 3–14, classified as poor support (3–8), moderate support (8–10), and strong support (12–14).20 The Perceived Life Threat Scale was used to measure perceived life events. Possible scores are 0–40: low perceived stress, moderate perceived stress, and high perceived stress (0–13, 14–26, and 27–40, respectively).21 The use of a specific substance at least once within the last 3 months was assessed by using the options “yes” or “no”.22
Six nurses were recruited to assist the data collection process. To ensure the quality of the data, data collectors were trained and the English version of the data-collection questionnaire was translated into the local language (Amharic) and translated back to English. In addition, completeness of collected data was checked by the supervisors.
Data Analysis
Final data were entered into EpiData 4.1, then exported to SPSS 21.0 for analysis. Frequencies, percentages, and means ± SD were calculated to describe characteristics of the study population. Predictors of psychological distress were identified by logistic regression analyses. The association between psychological distress and each covariate was assessed firstly by bivariate logistic regression to identify candidate variables for the final model. Variables with P<0.25 progressed to multivariate logistic regression to identify independent factors of psychological distress. Finally, independent factors of psychological distress were declared at P<0.05 and strength of association was assessed using AORs with corresponding 95% CIs.
Ethics
Ethical approval was obtained from the Ethics Committee of the College of Medicine and Health Sciences, Mizan-Tepi University. Permission was also granted by chief executive officers of the hospitals, and informed consent was obtained from all participants. The study adhered to the Declaration of Helsinki ethical principles for medical research involving human subjects. Correspondingly, the scientific findings generated does not pose any harm to the study population. Similarly, data were kept anonymous and participants were informed about the confidentiality of the information obtained. The right of patients to withdraw from the study was also respected.
Results
Demographic Characteristics
Of the 337 study participants enrolled in the study, about 41% were aged 25–34 years. The mean age was 32.83±12.29 (range 18–80) years. More than half (54.9%) were males and 141 (41.5%) were Orthodox Christian. Over a quarter (27.6%) of the respondents were Bench by ethnicity, and about 131 (38.9%) had had no formal education. A majority (54.3%) were married, and 89 (26.4%) of the participants were government-employed (Table 1).
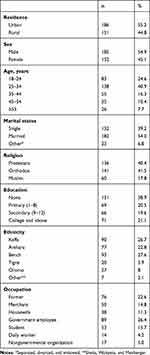 |
Table 1 Demographic characteristics of patients admitted to selected hospitals in southwest Ethiopia, 2020 (n=337) |
Clinically Related Characteristics
As it can be observed from Table 2, 38 (11.3%), 71 (21.1%), and nearly two-thirds (65.3%) of respondents had a history of mental illness, trauma in childhood, and used any specific measures against COVID-19 pandemic, including social distancing and hand-washing, respectively.
 |
Table 2 Clinical characteristics of patients admitted to selected hospitals in southwest Ethiopia, 2020 (n=337) |
Psychosocial and Substance-Related Characteristics
In sum, 163 (48.7%) participants had poor social support and 102 (30.3%) had low perceived life threat. A majority (214, 63.5%) were alcohol users (Table 3).
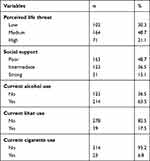 |
Table 3 Psychosocial and substance-related characteristics of respondents admitted to selected hospitals in southwest Ethiopia, 2020 (n=337) |
Prevalence of Psychological Distress
Based on assessment with the Kessler Psychological Distress Scale, the overall prevalence of psychological distress among participants was 57.9% (95% CI 52.8%–63.5%).
Factors Associated with Psychological Distress
Univariate logistic regression analysis of education status, living in an urban setting, female sex, marital status, perceived life threat, history of mental illness, childhood trauma, current alcohol use, poor social support, current khat use, and current cigarette use yielded P<0.25. As such, these variables fulfilled the minimum requirement for multivariate binary logistic regression analysis (Table 4).
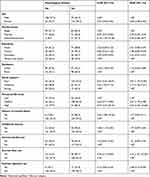 |
Table 4 Factors associated with psychological distress among patients admitted to selected hospitals in southwest Ethiopia, 2020 (n=337) |
Among the variables analyzed on multivariate binary logistic regression, female sex, high and medium perceived life threat, poor and moderate social support, and current khat use were significantly associated with psychological distress during COVID-19 (P<0.05). Accordingly, the odds of psychological distress among female participants were 3.69-fold (95% CI 2.08–6.55) times higher than those of male participants admitted to the three hospitals during the COVID-19 pandemic. The odds of having high and medium perceived life threat during the COVID-19 pandemic among admitted respondents were five- and three fold higher to have psychological distress compared to those with low perceived life treat, respectively (AOR 5.45, 95% CI 2.35–12.66; AOR 3.37, 95% CI 1.75–6.48; Table 4).
Admitted patients with poor and moderate social support were 3.97-fold (95% CI 1.70–9.29), and 3.17-fold (95% CI 1.36–7.41) as likely to have psychological distress as those with strong social support. Similarly, those with khat use in the previous 3 months admitted to hospitals were four fold more likely to have psychological distress than those who had not used khat in the previous 3 months (AOR 4.16, 95% CI 1.67–10.35; Table 4).
Discussion
The present study assessed psychological distress and associated factors among hospitalized patients during the COVID-19 pandemic at three selected hospitals in southwest Ethiopia. Admitted patients were affected by various chronic disorders that predisposed them to comorbid conditions, among which psychological distress was the most common. The WHO has urged preventive measures be undertaken to tackle the negative impact of the COVID-19 pandemic on individual mental health and well-being.23
According to the current study, a majority (57.9%, 95% CI 52.8%–63.5%) of hospitalized patients had psychological distress during the COVID-19 pandemic. The prevalence in the current study is comparable with a Chinese study, which found 54%,16 and higher than studies from Italy and Saudi Arabiac, which were 38% and 35%, respectively.24,25 The higher prevalence in our study could be attributed to differences in study populations: the Italian and Saudi Arabian studies were conducted among the general population, but ours was conducted among hospitalized patients. The variation might also be related to differences in the health-care structures and -delivery systems. Also, the social isolation imposed during hospitalization can increase loneliness and limit social interaction, which predispose people to psychopathological problems. Studies have indicated that medical problems and poor self-evaluation of health are associated with increased psychological distress.16,26
Female sex was significantly associated with psychological distress on univariate and multivariate logistic regression: female patients were four times as likely to have psychological distress as male patients. This finding is in agreement with studies done in Italy27 and China.16 A possible rationale might be women being more vulnerable to sociocultural risk factors associated with mental impact. However, due to the cross-sectional nature of study, it is not possible to say that women definitely suffered more from distress in general or reacted more negatively to the pandemic. Furthermore, compared to males, females experience much more fluctuation in hormonal levels, which are associated with emotional symptoms,28 and are more likely to report negative emotions than men. It should also be noted that a higher rate of domestic violence against women was reported during this outbreak.29
Admitted patients with a history of khat use were four times as likely to have psychological distress as their counterparts. Not surprisingly, khat chewing and psychological distress were positively associated, as this has been observed in another Ethiopian study.30 It is a well-known fact that psychoactive substances produce emotional, cognitive, and behavioral changes.31 The active constituent of khat, cathinone, causes stress primarily by stimulating secretion of the stress hormone cortisol.32
It was found that strong social support was a protective factor against psychological distress compared to poor and moderate social support. Those with poor and moderate social support were four and three times as likely to have psychological distress, respectively., as those with strong social support. This finding is concordant with the study done in China33 and England.9 A longitudinal observational study conducted during the first 3 months of the COVID-19 pandemic in Germany found that maintaining social contacts was associated with fewer symptoms of psychological distress.34 Furthermore, having the feeling of being loved and wanted and having a supportive environment can be instrumental in coping with different psychosocial challenges. Social support may also influence emotional regulation and emotional reactivity that is implicated in the development of psychological distress.
Similarly, perceived life threat was positively associated with psychological distress, in which individuals with moderate and high perceived life threat were four and five times more likely to be psychologically distressed than who felt low perceived life threat, respectively. This might be attributable to the fact that major stressful events may cause changes in brain biochemistry, which can be expressed through physiological, psychological, and behavioral manifestations.31 In addition, it is likely that people within such an outbreak worry about contracting the virus responsible for the pandemic, stigma, and even dying from COVID-19.35
Limitations
This was a cross-sectional study, and as such a causal relationship between the independent and dependent variables cannot be reported. The instrument employed to assess psychological distress in this study, the K10, assesses only broad, aspecific psychological distress, rather than specific types related to specific disorders. This study was conducted during the early stages of the COVID-19 pandemic, and may have underestimated the prevalence of psychological distress. The absence of pre–COVID-19 pandemic assessment of enrolled patients means that we were not able to ascertain whether the distress had been elicited by hospitalization or the pandemic. The data were collected by face-to-face interviews to assess the prevalence of psychological distress among admitted patients, which is prone to social desirability bias.
Conclusion
This study indicated that the prevalence of psychological distress was noticeably high among hospitalized patients during COVID-19. Female sex, high and medium perceived life threat, poor and moderate social support, and current khat use were found to be independent predictors of psychological distress among admitted patients. Our findings highlight the need to develop psychological support strategies to improve mental health and psychological resilience during the COVID-19 pandemic.
Abbreviations
K10, Kessler Psychological Distress Scale; MTUTH, Mizan-Tepi University Teaching Hospital; SNNPR, Southern Nations, Nationalities, and Peoples’ Region; WHO, World Health Organization.
Acknowledgments
We are grateful to Mizan-Tepi University College of Medicine and Health Sciences for providing the opportunity to conduct this research. We are also heartily thankful to the data collectors for their contribution.
Disclosure
The authors declare that they have no conflicts of interest.
References
1. Yin Y, Wunderink RG. MERS, SARS and other coronaviruses as causes of pneumonia. Respirology. 2018;23(2):130–137. doi:10.1111/resp.13196
2. WHO. WHO timeline - COVID-19. 2020. Available from: https://www.who.int/news-room/detail/27-04-2020-who-timeline—covid-19.
3. Phelan AL, Katz R, Gostin LO. The novel coronavirus originating in Wuhan, China: challenges for global health governance. JAMA. 2020;323(8):709–710. doi:10.1001/jama.2020.1097
4. Ren SY, Gao RD, Chen YL. Fear can be more harmful than the severe acute respiratory syndrome coronavirus 2 in controlling the corona virus disease 2019 epidemic. World J Clin Cases. 2020;8(4):652–657. doi:10.12998/wjcc.v8.i4.652
5. Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020;323(11):1061–1069. doi:10.1001/jama.2020.1585
6. Feng L, Dong Z, Yan R, et al. Psychological distress in the shadow of the COVID-19 pandemic: preliminary development of an assessment scale. Psychiatry Res. 2020;291(113202):ISSN 0165–1781. doi:10.1016/j.psychres.2020.113202
7. Lee AM, Wong JG, McAlonan GM, et al. Stress and psychological distress among SARS survivors 1 year after the outbreak. Can J Psychiatry. 2007;52(4):233–240. doi:10.1177/070674370705200405
8. Yoon MK, Kim SY, Ko HS, Lee MS. System effectiveness of detection, brief intervention and refer to treatment for the people with post-traumatic emotional distress by MERS: a case report of community-based proactive intervention in South Korea. Int J Ment Health Syst. 2016;10:51. doi:10.1186/s13033-016-0083-5
9. Holmes EA, O’Connor RC, Perry VH, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020;7(6):547–560. doi:10.1016/S2215-0366(20)30168-1
10. Brooks SK, Webster RK, Smith LE, et al. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. Lancet. 2020;395(10227):912–920. doi:10.1016/S0140-6736(20)30460-8
11. Brody C, Chhoun P, Tuot S, Pal K, Chhim K, Yi S. HIV risk and psychological distress among female entertainment workers in Cambodia: a cross-sectional study. BMC Public Health. 2016;16:133. doi:10.1186/s12889-016-2814-6
12. Tola HH, Shojaeizadeh D, Garmaroudi G, Tol A, Yekaninejad MS, Ejeta LT. Psychological distress and its effect on tuberculosis treatment outcomes in Ethiopia. Glob Health Action. 2015;8(1):29019. doi:10.3402/gha.v8.29019
13. Zhu S, Wu Y, Zhu C, et al. The immediate mental health impacts of the COVID-19 pandemic among people with or without quarantine managements. Brain Behav Immun. 2020;87:56–58. doi:10.1016/j.bbi.2020.04.045
14. Losada-Baltar A, Jiménez-Gonzalo L, Gallego-Alberto L, Pedroso-Chaparro MDS, Fernandes-Pires J, Már quez-González M. We’re staying at home”. Association of self-perceptions of aging, personal and family resources and loneliness with psychological distress during the lock-down period of COVID-19. J Gerontol B Psychol Sci Soc Sci. 2020. doi:10.1093/geronb/gbaa048
15. Al-Hanawi KM, Mwale ML, Alshareef N, et al. Psychological distress amongst health workers and the general public during the COVID-19 pandemic in Saudi Arabia. Risk Manag Healthc Policy. 2020;13:733–742. doi:10.2147/RMHP.S264037
16. Wang C, Pan R, Wan X, et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020;17(5):1729. doi:10.3390/ijerph17051729
17. Qiu J, Shen B, Zhao M, Wang Z, Xie B, Xu Y. A nationwide survey of psychological distress among Chinese people in the COVID-19 epidemic: implications and policy recommendations. Gen Psychiatry. 2020;33:e100213. doi:10.1136/gpsych-2020-100213
18. Vafaei H, Roozmeh S, Hessami K, et al. Obstetrics healthcare providers’ mental health and quality of life during COVID-19 pandemic: multicenter Study from eight cities in Iran. Psychol Res Behav Manag. 2020;13:563–571. doi:10.2147/PRBM.S256780
19. Andrews G, Slade T. Interpreting scores on the kessler psychological distress scale (K10). Aust N Z J Public Health. 2001;25(6):494–497. doi:10.1111/j.1467-842X.2001.tb00310.x
20. Dalgard OS, Dowrick C, Lehtinen V, et al. Negative life events, social support and gender difference in depression. Soc Psychiatry Psychiatr Epidemiol. 2006;41(6):444–451. doi:10.1007/s00127-006-0051-5
21. Lavoie JA, Douglas KS. The perceived stress scale: evaluating configural, metric and scalar invariance across mental health status and gender. J Psychopathol Behav Assess. 2012;13(1):34–48. doi:10.1007/s10862-011-9266-1
22. Saitz R, Palfai TP, Cheng DM, et al. Screening and brief intervention for drug use in primary care: the ASPIRE randomized clinical trial. JAMA. 2014;312(5):502–513. doi:10.1001/jama.2014.7862
23. Yao H, Chen JH, Xu YF. Rethinking online mental health services in China during the COVID-19 epidemic. Asian J Psychiatr. 2020;50:102015. doi:10.1016/j.ajp.2020.102015
24. Moccia L, Janiri D, Pepe M, et al. Affective temperament, attachment style, and the psychological impact of the COVID-19 outbreak: an early report on the Italian general population. Brain Behav Immun. 2020;87:75–79. doi:10.1016/j.bbi.2020.04.048
25. Elhessewi GMS, Almoayad F, Mahboub S, Alhashem AM, Fiala L. Psychological distress and its risk factors during COVID-19 pandemic in Saudi Arabia: a cross-sectional study. Middle East Curr Psychiatry. 2021;28:7. doi:10.1186/s43045-021-00089-6
26. Ho CS, Tan EL, Ho RC, Chiu MY. Relationship of anxiety and depression with respiratory symptoms: comparison between depressed and non-depressed smokers in Singapore. Int J Environ Res Public Health. 2019;16(1):163. doi:10.3390/ijerph16010163
27. Mazza C, Ricci E, Biondi S, et al. A nationwide survey of psychological distress among Italian people during the COVID-19 pandemic: immediate psychological responses and associated factors. Int J Environ Res Public Health. 2020;17(9):3165. doi:10.3390/ijerph17093165
28. Pagel MD, Erdly WW, Becker J. Social networks: we get by with (and in spite of) a little help from our friends. J Pers Soc Psychol. 1987;53(4):793–804. doi:10.1037//0022-3514.53.4.793
29. Gausman J, Langer A. Sex and gender disparities in the COVID-19 pandemic. J Womens Health. 2020;29(4):465–466. doi:10.1089/jwh.2020.8472
30. Tesfaye SH, Bune GT. Generalized psychological distress among HIV-infected patients enrolled in antiretroviral treatment in Dilla University Hospital, Gedeo zone, Ethiopia. Glob Health Action. 2014;7(1):23882. doi:10.3402/gha.v7.23882
31. Chirita V, Untu I. Kaplan and Sadock’s synopsis of psychiatry: behavioural sciences/clinical psychiatry. Bull Integr Psychiatry. 2016;22(1):119–123.
32. al’Absi M, Khalil NS, Al Habori M, Hoffman R, Fujiwara K, Wittmers L. Effects of chronic khat use on cardiovascular, adrenocortical, and psychological responses to stress in men and women. Am J Addict. 2013;22(2):99–107. doi:10.1111/j.1521-0391.2013.00302.x
33. Du J, Dong L, Wang T, et al. Psychological symptoms among frontline healthcare workers during COVID-19 outbreak in Wuhan. Gen Hosp Psychiatry. 2020;67:144–145. doi:10.1016/j.genhosppsych.2020.03.011
34. Bendau A, Plag J, Kunas S, Wyka S, Ströhle A, Petzold MB. Longitudinal changes in anxiety and psychological distress, and associated risk and protective factors during the first three months of the COVID‐19 pandemic in Germany. Brain Behav. 2020;00:e01964. doi:10.1002/brb3.1964
35. Hall RC, Hall RC, Chapman MJ. The 1995 kikwit ebola outbreak: lessons hospitals and physicians can apply to future viral epidemics. Gen Hosp Psychiatry. 2008;30(5):446–452. doi:10.1016/j.genhosppsych.2008.05.003
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
