Back to Journals » Orthopedic Research and Reviews » Volume 13
Assessment of Functional Limitation and Associated Factors in Adults with Following Lower Limb Fractures, Gondar, Ethiopia in 2020: Prospective Cross-Sectional Study
Authors Belete Y, Belay GJ, Dugo T , Gashaw M
Received 5 January 2021
Accepted for publication 19 February 2021
Published 9 March 2021 Volume 2021:13 Pages 35—45
DOI https://doi.org/10.2147/ORR.S300459
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Clark Hung
Yihalem Belete, Gashaw Jember Belay, Tamiru Dugo, Moges Gashaw
Department of Physiotherapy, School of Medicine, College of Medicine and Health Sciences, University of Gondar Comprehensive Specialized Hospital, Gondar, Ethiopia
Correspondence: Moges Gashaw
Department of Physiotherapy, School of Medicine, College of Medicine and Health Sciences, University of Gondar Comprehensive Specialized Hospital, P.O. Box: 196, Gondar, Ethiopia
Tel +251924509390
Email [email protected]
Background: Lower limb fractures account for approximately one-third of all fractures. Lower limb fracture complications are one of the major reasons for hospital stays and have high impact on rehabilitation services. Functional limitations with lower extremities fractures are related to decreased functional mobility, the need for long term use of assistive devices, lack of independence, and the long term need for assistive care. This study aimed to assess the functional limitation and identify the possible predictors among lower limb fracture patients by using the Lower Extremity Functional Scale (LEFS).
Methods: A prospective institutional-based cross-sectional study was conducted from July to October 30/2020, at University of Gondar, comprehensive specialized hospital. The data of 226 participants were collected through face-to-face interviews, patient record review and by physical examination with simple random sampling techniques. Binary logistic regression was used to identify predictors of functional limitation among lower limb fracture with SPSS 25. The strength of the association was present by adjusted odds ratios (OR).
Results: One hundred and eighty-two (n = 182 (80.5%): 95% CI (74.8 to 85.8) patients with following lower limb fracture have functional limitation. Level of education (AOR =5.50; 95% CI: 1.707– 17.742), presence of hospitalized complication AOR=3.26; 95% CI (1.147– 9.294), severity of pain AOR=3.19; 95% CI (1.399– 7.259), duration of onset AOR=9.512; 95% CI (3.585– 25.237), knee flexion limitation AOR=7.13; 95% CI (1.926– 26.368) were the independent risk factors for functional limitation.
Conclusion: The magnitude of functional limitation in following lower limb fracture individual was considerably high in study setup. Level of education, presence of hospitalized complication, severity of pain, duration of onset, knee flexion limitation were the independent risk factors for functional limitation.
Keywords: fracture, lower limb, functional limitation, range of motion, pain
Introduction
Fracture is a medical condition that is a break in the continuity of bone, either complete or incomplete integrity of the bone as result of high force impact, stress, trivial injury or as a result of certain medical conditions.1,2 It is a common public health problem that can lead to mild or severe disability and hinders the quality of life of adults in different countries. More than 90% of traumatic morbidity, mortality, and associated disability related to fractures occurs in low and middle income countries (LMIC).3,4 Different studies reported that the cause of fractures in LMIC was road traffic accidents, personal conflict, interpersonal violence, and work related accidents.5,6 Based on body parts involved; lower extremity, head and hand, multiple part and upper extremity were commonly reported types of fracture.7
Lower limb fracture accounts for approximately one-third of all fractures and may contribute to significant mortality and morbidity.8,9 The most common anatomic site of lower limb fracture is the ankle (22.6%), followed by the tibia/fibula (17.3%), the hip (16.7%), and the tarsal/metatarsal bones (16.7%), and 26.7% are on different parts of the femur.10 The fracture of bone is treated and managed with both operative and non-operative methods. Because of the complication of treatment and lack of early rehabilitation, patient faced reduction of body composition and physical function like muscular and bone hypotrophy, ligament and capsular retraction, pain, joint stiffness, poor circulation, mobility limitation, risk of falls, loss of independent activity of daily living (ADL), limited range of motion (ROM) and decreased muscle strength.4,11
After a fracture of the lower extremity, the duration of immobility of the affected limb and the time of hospitalization may negatively influence the body composition and the physical function of the patients.4 The lower limb fractures complications are one of the major reason for hospital stay and have high impact on the rehabilitations services. Functional limitations related to lower extremities fractures which are related to the decreased functional mobility require long term use of assistive devices, lack of independence, and the long term need for assistive care. Most individuals after suffering a fractured of a limb came to rehabilitation clinics with sever impairments, such as limited ROM, weakness of involved extremities, chronic pain, ambulation with aids and limping while walking, and difficulty in ADL, and with some sort of functional problems.12
Even though numerous studies, reported the cause, burden and pattern of fractures, outcome of treatment in lower limb fractures, lack of evidence seen in developing countries on the assessment of functional limitation associated with lower extremity fracture. Despite the lack of evidence, studies are needed to comprehensively assess the functional limitation associated with following lower limb fracture. So the aim of this study was to assess the functional limitation and identify the possible predictors among following lower limb fracture patients by using Lower Extremity Functional Scale (LEFS), which is one of the region-specific measures and developed for lower extremity musculoskeletal disorders.
Materials and Methods
Study Design, Period and Setting
A prospective institutional based cross-sectional study was conducted from July to October 30/2020, at University of Gondar, comprehensive specialized hospital, in Northwest Ethiopia. The comprehensive hospital is a tertiary level teaching and comprehensive hospital, catering for nearly 700 inpatients and rendering referral health services for over 5 million inhabitants in Northwest Ethiopia. This large number of people from the surrounding zones and nearby regions visit the hospital for different medical services.3,13 This comprehensive hospital has three inpatients wards for traumatic and orthopedics conditions with an orthopedics ward with 39 beds, the surgical ward has 36 beds and 13 beds in the trauma units. The orthopedic OPD works twice per week and an average of 40 to 60 traumatic patients following hospitalization were seen with appointment weekly. Among these patients half of the participants were lower limb fracture (20–30) weekly and 60–140 lower limb fracture patients were visiting the orthopedic OPD monthly.
Inclusion and Exclusion Criteria
Adults with lower limb fractures visiting orthopedics OPD for follow up and evaluation were included in this study. Whereas, lower limb individuals who had open wounds on the joint, patients with deep vein thrombosis (DVT), plaster of Paris (POP), fracture patients managing with amputation, and upper limb and small bone fracture patients were excluded from the study.
Source Population, Study Population, and Sample Size
The source population of this study was individuals with fractures who were visiting the orthopedics department. The study population was all individuals with lower limb fractures who were visiting the University of Gondar referral hospital (orthopedic OPD) during the study period. A sample size was calculated using a single population proportion formula based on the assumptions; 95% confidence interval (CI), 50% prevalence, 5% precision, 15% non-response, and contingencies. Since there was no previous study done in similar area and setting. The sample size of this study was calculated as:
n = (za/2)2 p (1-p)/d2
n= (1.96)2* (0.5)* (0.5)/(0.05)2 = 384.16~385
However the total number of lower limb fracture patients receiving orthopedics treatment annually was below 10,000. So the samples were taken from a relatively small population (N=400), the required sample size was obtained by using the following calculation. Since on average 100 lower limb fracture patients are seen in orthopedics OPD. By considering this, a total of 400 lower limb fracture patients have visited the hospital during the data collection period.
nf =n/1+n/N
n=385/1+385/400=385/1.96=196.4
n=196.4 for the precision considering 15% expected contingency the final sample size is 226. Finally 226 study participant were enrolled with simple random sampling method.
Operational Definitions
Functional limitation is defined as a restriction in the ability to perform an action or activity. Measured by the LEFS and valued as 0–61% limited and 62–100% not limited.14 The LEFS is a questionnaire to assess levels of function after lower limb fracture during rehabilitation to detect functional progress, which has 20 items and scored 0 to 4, Interpretation: 0=extreme difficulty/unable to do, 1=quite a bit of difficulty, 2=moderate difficulty, 3=a little bit of difficulty, 4=no difficulty.15 ROM: how much is the mobility of the proximal and distal joint of the affected extremity. 1=full range of movement, 0.75=shows decrease by ¼, 0.5=half of normal ROM, and 0.25=only ¼ is preserved.16 The severity of pain was described using a 10 cm visual analogous scale (VAS); 0–3cm: no pain to mild pain, 4–6cm: moderate pain, 7–10cm: severe pain.17 Lower limb fracture is based on the involvement of the fracture bone segment in the region of above knee, below knee fracture, and combination of the above knee plus below knee.11
Data Collection Instrument and Procedures
The data was collected using pretested and structured questionnaire. The structured questionnaire was adopted by an extensive review of related studies,11,16,18 WHO's trauma surveillance questionnaire,19 and LEFS questionnaire.15 The questionnaire, which included domains like socio-demographic characteristics: age, gender, occupation; medical comorbidity, behavioral characteristics; and fracture-related characteristics, including types of fracture management, types of fracture, and duration of hospitalization. The assessment of functional activity after lower limb fracture during rehabilitation was assessed by using LEFS which have very good reliability (a=86) and test–retest reliability (R=0.86).20 This tool has a 20-item region specific self-reporting measure designed to assess the functional status of patients with orthopedic conditions of the lower extremity.
The physical measurement of ROM of the proximal and distal joint with universal plastic goniometer and severity of pain using the VAS were performed by physiotherapists. The questionnaire was initially prepared in English by language experts and authors at the University of Gondar and checked for the consistency of the questions. The English version of questionnaire was translated to the local language (Amharic) and again translated back to English by language experts. The original and translated questionnaires were compared and the discrepancies were reviewed and corrections were made accordingly.
Data were collected through face-to-face interviews, patient record review and by physical examination. Data collection was carried out by three senior physiotherapists. Two days' intensive training was given to the data collectors by the principal investigator (YB and MG) on how to approach the study participants, how to use the questionnaire and guidelines, and the techniques of data collection. The investigators closely followed the data collection process and ensured accuracy, completeness, and consistency of the collected questionnaire daily.
Data Analysis Procedure
Data were coded and entered using EPI INFO version 7.1 and exported to SPSS for windows version 25. Missing values and data cleaning were checked. Descriptive statistics for the presentation of demographic data, including percentage, or mean and standard deviation (SD) was used. Binary logistic regression was used to identify predictors of functional limitation among lower limb fracture. Variables with bivariate P<0.20 were fitted into multivariate models for controlling the possible effect of confounders, and finally the variables that had significant associations with functional limitation were identified on the basis of odds ratio (OR), with 95% CI and P<0.05. The variables were entered into the multivariate model using the backward stepwise (likelihood ratio) method.
Results
Socio-Demographic Characteristics of the Study Participants
A total of 226 following lower limb fracture patients participated in the study with the age ranged from 18 to 85 years. The mean age of the participants was 35.98 years (±14.1). The majority (84.1%) of the participants were male, more than half of the participants (58%) were urban dwellers, and half of the participants were married (50%). More than one-third of the participant’s monthly family income was less than 1500 ETB (35.8%) and level of education of the participant was completion of primary school (37.6%). The socio-demographic details of the participants have been provided in Table 1.
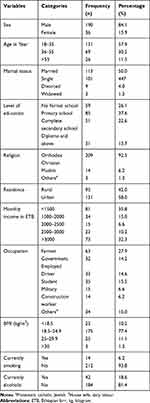 |
Table 1 Socio-Demographic Characteristics of Lower Limb Fracture Patients in Gondar, Ethiopia, (n=226) |
Clinical Characteristics of the Study Participants
This finding revealed that the common cause of lower limb fracture was road traffic accident (36.3%), following a gunshot injury (28.3%). More than half of the study participants had right side lower limb fracture (63.3%) and nearly equal involvement of above knee (47.8%), and below knee (47.3%) fracture were detected in this study. More than half of the participants (53.5%) visited orthopedics OPD after three months since onset while half of the lower limb fracture (50.4%) were open fracture. Among the lower limb fracture patients more than one-third of the participants (36.3%) was treated with intramedullary nailing. Off the total study participants; nearly one in three of the participants did not receive inpatient (72.1%) and outpatient (77.9%) physiotherapy treatment. One quarter of the participants (16.37%) reported severe pain and less than half of the study participants had full knee ROM after lower extremity fracture (Table 2).
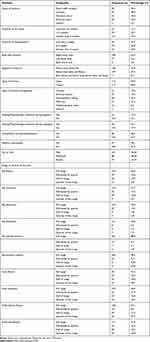 |
Table 2 Clinical Characteristics of Lower Limb Fracture Patients in Gondar, Ethiopia, (n=226) |
Functional Limitation Among Following Lower Limb Fracture Patients
One hundred and eighty-two (n = 182 (80.5%): 95% CI (74.8 to 85.8)) patients with following lower limb fracture have functional limitation. The burden of functional limitation was significantly higher (82.4%, n=150) among men with lower limb fracture and in urban dwellers (53.8%, n=98). Most of the study participants who were in the age range between 18- and 35-years-old reported high levels of functional limitation (56.0%). Higher levels of functional limitation was seen in below knee fracture individuals (82.4%), treated with intramedullary nailing (33.5%), and those individual who had not physiotherapy treatment (74.7%). The finding of functional limitation among lower limb fracture individual are shown in Table 3.
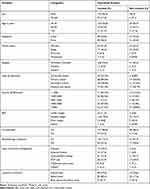 |
Table 3 Functional Limitation Among Following Lower Limb Fracture Individual at Gondar, Ethiopia (n=226) |
Regression Analysis
In the univariate regression analyses, functional limitation was significantly (p < 0.20) associated with Residence, ROM, pain severity, level of education, complication during hospitalization, duration from onset, and BMI. Multivariate regression showed that educational status, severity of pain, complication during hospitalization, and ROM of the joint was significantly associated when adjusting for the other included variables (p<0.05). Table 4 shows the association between dependent and independent variables among the study participants. Being uneducated shows statistically significant association with limited functional activity AOR =5.50; 95% CI (1.707–17.742). Among the study participants had severe pain AOR=3.19; 95% CI (1.399–7.259), duration from onset less than three months AOR=9.512; 95% CI (3.585–25.237) and complication during hospitalization AOR=3.26; 95% CI (1.147–9.294) were significantly associated with limited functional activity compared to their counterparts. According to an ROM examination, knee flexion decreased by three/fourth AOR=7.13; 95% CI (1.926–26.368) were significantly associated with functional limitation.
 |
Table 4 Factors Associated with Functional Limitation with Following Lower Limb at Gondar University, Ethiopia (n=226) |
Discussion
The main purpose of this study was to find out the magnitude of functional limitation by using The LEFS among individuals with lower limb fractures and describe the associated factors in Ethiopia. Among the overall study participants 80.5% with 95% CI (74.8 to 85.8) of individuals with lower limb fractures have reported functional limitations based on LEFS. Urban dwellers (53.8%) were functionally limited which could be because the frequency of urban dwellers is high compared with rural participants, however the expectation was higher for rural dwellers because they are far from services and there is lack of transportation and other environmental barriers. The magnitude of functional limitations in lower limb fracture individuals was considerably higher in the study setting. Level of education, presence of hospitalized complication, severity of pain, duration of onset, knee flexion limitation were the independent risk factors for functional limitation.
The magnitude of following fracture functional limitation was found in 80.5% in our study. This result is slightly consistent with the cross-sectional study done in the USA – which consisted of a sample of 509 participants aged between 15 and 65 years – reported that the level of functional activity was 75%.11 However, our result was considerably higher compared to other studies, which reported 45% in Brazil;4 65% in Maryland, USA. This variation in the current study can be explained by the age range of the study participants in current study was between 18–85 while a study done in Maryland among 302 participants with mean age of 34 years.21 This variation could be due to a different sample size and duration from onset. The participants were recruited after six months of hospitalization, in the current study all lower limb fracture patients visiting outpatient department were included. Similarly, the finding of this study are higher than a cross-sectional study reported in ydney,22 Australia (31.9%), with a convenience sample size of 275 lower limb fractured older adults aged >65 years, which was reported as a level of functional limitation. The possible reason for the difference might be due to a variation of age and duration from onset. The current study included participants aged between 18 and 85 years, whereas a study done in Sydney included older adults only. In addition, the current study included all lower limb fracture patients visiting surgical OPD (acute, subacute and chronic phase), whereas the former study included only one month after onset of fracture (sub-acute).
In the current study, being uneducated mean that the indiviual was 5.503 times more likely to have functional activity than an educated individual. Which is supported by findings from other studies.23 A retrospective observational study conducted in Italy expressed that adults with higher education have the potential to functionally recover following lower limb fracture compared with uneducated adults.24 An epidemiological study in Taiwan reported that those who were uneducated and had a monthly salary less than $1500 showed low level of functional activity. Knowing the natural phase of fracture recovery, following the guidelines from the surgeon and physiotherapist, and being aware how to handle the fractured limb until full weight bearing is recommended are the right means of functional recovery.25
Those who developed complications during hospitalization were 3.264 times more likely to have functional limitations than their counterparts. This finding is supported by a cross-sectional survey conducted among earthquake survivors in China, which discovered that adults with lower limb fractures who were hospitalized for more than 12 days developed many complications, like joint edema, wasting of muscle mass, stiffness and infection, it further hindered levels of functional limitation.26 Those with severe pain were 3.186 times more likely to have functional limitations on lower limb fractures. This finding is in line with the study conducted in Sweden which expressed that persistent severe pain affects ADL and functional performance, the more severe postoperative persistent pain low level of functional recovery is scored.27 The reason can be that pain limits rehabilitation activities and the patient may be depressed and lose future rehabilitation expectation.
Decreased ROM of ankle plantar flexion (PF) by 75% and more were 6.785 times more likely to have functional limitation following lower limb fracture, in contrast with full range, decreased knee flexion by 75% and more were 4.379 times more likely to have functional activity following lower limb fracture in contrast with full range. This finding was supported by a cross-sectional epidemiological survey conducted in Germany, which explored that lower limb fractures to the ankle and knee ROM limitation is a major problem due to immobilization, decreased ankle PF, and knee flexion by half merely affects functional recovery and needs long term rehabilitation.11 The reason could be that ROM limitation is one component in international classification of functional disability and disease (ICF) which is in body function and structure, so impairment can deactivate functional activity.
Conclusion
The magnitude of functional limitation in lower limb fracture individuals was considerably high in our study setup. Level of education, presence of hospitalized complications, severity of pain, duration of onset, and knee flexion limitation were the independent risk factors for functional limitation. Therefore, the orthopedic and physiotherapy staff should assess the level of functional activity, not only the impairment, and should consider early physiotherapy intervention, and appropriate functional limitation reduction strategies.
Strength and Limitation of the Study
This study is the first on the study area as well as in the country. We have used a validated tool that has very good inter- and intra-observer reliability,20 and measured the ROM of the lower limb joint with standard goniometer. For the benefit of future research, there are some noteworthy limitations, some of the variables like muscle power, gait assessment, weight bearing stats, leg length discrepancy, and some of unmeasured societal or lifestyle variables were not considered. These confounders could lead to a possible variation in the estimation of association among functional limitation and other variables. The cross-sectional nature of this study presents limitations in terms of causal association interpretations and long term effects through to the aADL.
Abbreviations
AOR, adjusted odds ratio; ADL, activity of daily living; BMI, body mass index; CI, confidence interval; COR, crude odds ratio; LEFS, Lower Extremity Functional Scale; LMICs, lower and middle income countries; OPD, outpatient department; PF, plantar flexion; POP, plaster of Paris; ROM, range of motion; USA, United States of America; VAS, visual analogous scale; WHO, World Health Organization.
Data Sharing Statement and Availability
All data relevant to our findings are contained within the manuscript. Requests for further details on the dataset and queries concerning data sharing shall be arranged based on a reasonable request to correspondence author: [email protected]
Ethical Approval and Consent to Participate
This study was directed in accordance with the Declaration of Helsinki. To conduct the this study, the ethical approval was obtained from the Ethical Review Board of School of Medicine, College of Medicine and Health Sciences, University of Gondar (Ref. No. SOM/2035/2020), and voluntary informed written consent was taken from each study participant after being informed in detail about the objective, purpose, benefits and risk of the study. Personal identifiers were not noted during the data collection period to assure confidentiality.
Acknowledgments
Firstly, we would like to express our deepest gratitude to the University of Gondar for ethical approval and funding. Our gratitude and appreciation go to data collectors, supervisors, and study participants without their cooperation this study would have not been possible.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This research didn’t receive any grant from any funding agency in the public, commercial, or not-for-profit sectors.
Disclosure
All authors declare that they have no conflicts of interest in this work.
References
1. Singh OG, Singh HS, Singh ST. A hospital based study on pattern of extremity fractures following trauma in Manipur. J Evol Med Dent Sci. 2016;5(82):6097–6101. doi:10.14260/jemds/2016/1378
2. Getu J, Bayisa ETH Factors associated with fracture and its outcome at Wolaita Sodo University teaching and referral Hospital, Wolaita Sodo, Southern Ethiopia; 2017.
3. Zeleke TAABM, Melak GATMF. Magnitude and patterns of injuries among patients in Gondar University Hospital, Northwest Ethiopia: an institutional-based study. Open Access Surg. 2017;10:25–31. doi:10.2147/OAS.S126043
4. Oliveira MA, Macedo OG, Silva LC, Oliveira TS, Bottaro M, Martins WR. Structural and physical-functional deficits in lower limbs with fractures and treated surgically. Fisioterapia em Movimento. 2018;31.
5. Tegegne KT Assessment of the prevalence of trauma cases visited at emergency OPD in Dilla University Referal Hospital from April 20, 2008–May 20, 2008 EC; 2019.
6. Shavaleh R, Motevalian SA, Mahdavi N, Haddadi M, Mohaghegh MR, Hamedi Z. Epidemiological study of hospitalized road traffic injuries in Iran 2011. Med J Islam Repub Iran. 2018;32:50. doi:10.14196/mjiri.32.50
7. Asefa A, Seyoum G, Wamisho B. Common types and pattern of bone fractures among road traf-fic injury victims seen in Addis Ababa Piblic Hospitals. Ethiop Med J. 2019;57(2):149–156.
8. Igho OE, Isaac OA, Eronimeh OO. Road traffic accidents and bone fractures in Ughelli, Nigeria. Spine. 2015;2:0–93.
9. Parameswaran V. Conclusions from analyses of outpatient visit patterns at an orthopedic hospital. Apollo Med. 2018;15(4):214. doi:10.4103/am.am_73_18
10. Wu -H-H, Liu M, Challa ST, et al. Development of squat-and-smile test as proxy for femoral shaft fracture-healing in patients in Dar es Salaam, Tanzania. J Bone Joint Surg Am. 2019;101(4):353–359. doi:10.2106/JBJS.18.00387
11. Zelle B, Brown S, Panzica M, et al. The impact of injuries below the knee joint on the long-term functional outcome following polytrauma. Injury. 2005;36(1):169–177. doi:10.1016/j.injury.2004.06.004
12. Pan S-L, Liang H-W, Hou W-H, Yeh T-S. Responsiveness of SF-36 and Lower Extremity Functional Scale for assessing outcomes in traumatic injuries of lower extremities. Injury. 2014;45(11):1759–1763. doi:10.1016/j.injury.2014.05.022
13. Mohammed A, Seid ME, Gebrecherkos T, Tiruneh M, Moges F. Bacterial isolates and their antimicrobial susceptibility patterns of wound infections among inpatients and outpatients attending the University of Gondar Referral Hospital, Northwest Ethiopia. Int J Microbiol. 2017;2017:1–10. doi:10.1155/2017/8953829
14. Wang Y-C, Hart DL, Stratford PW, Mioduski JE. Clinical interpretation of computerized adaptive test–generated outcome measures in patients with knee impairments. Arch Phys Med Rehabil. 2009;90(8):1340–1348. doi:10.1016/j.apmr.2009.02.008
15. Dingemans SA, Kleipool SC, Mulders MA, et al. Normative data for the lower extremity functional scale (LEFS). Acta Orthop. 2017;88(4):422–426. doi:10.1080/17453674.2017.1309886
16. Bach O, Hope M, Chaheka C, Dzimbiri K. Disability can be avoided after open fractures in Africa—results from Malawi. Injury. 2004;35(9):846–851. doi:10.1016/j.injury.2003.11.014
17. Aicher B, Peil H, Peil B, Diener H. Pain measurement: Visual Analogue Scale (VAS) and Verbal Rating Scale (VRS) in clinical trials with OTC analgesics in headache. Cephalalgia. 2012;32(3):185–197. doi:10.1177/03331024111430856
18. Ibrahim NI, Ahmad MS, Zulfarina MS, et al. Activities of daily living and determinant factors among older adult subjects with lower body fracture after discharge from hospital: a prospective study. Int J Environ Res Public Health. 2018;15(5):1002. doi:10.3390/ijerph15051002
19. Krug EG. Injury surveillance is key to preventing injuries. Lancet. 2004;364(9445):1563–1566. doi:10.1016/S0140-6736(04)17328-5
20. Binkley JM, Stratford PW, Lott SA, Riddle DL; Network NAORR. The Lower Extremity Functional Scale (LEFS): scale development, measurement properties, and clinical application. Phys Ther. 1999;79(4):371–383.
21. Ceroni D, Martin X, Lamah L, et al. Recovery of physical activity levels in adolescents after lower limb fractures: a longitudinal, accelerometry-based activity monitor study. BMC Musculoskelet Disord. 2012;13(1):131. doi:10.1186/1471-2474-13-131
22. Beckenkamp PR, Lin C-WC, Chagpar S, Herbert RD, van der Ploeg HP, Moseley AM. Prognosis of physical function following ankle fracture: a systematic review with meta-analysis. J Orthop Sports Phys Ther. 2014;44(11):841–851. doi:10.2519/jospt.2014.5199
23. Holtslag H, Buskens E, Rommers C, Prevo A, van der Werken C. Long-term outcome after lower extremity injuries in severely injured patients. Eur J Trauma. 2006;32(4):365–373. doi:10.1007/s00068-006-5112-7
24. Zuccarino S, Fattore G, Vitali S, Antronaco G, Frigerio S, Colombo M. The association between education and rehabilitation outcomes: a Population Retrospective Observational Study. Arch Gerontol Geriatr. 2020;91:104218. doi:10.1016/j.archger.2020.104218
25. Fitzharris M, Bowman D, Ludlow K. Factors associated with return‐to‐work and health outcomes among survivors of road crashes in Victoria. Aust N Z J Public Health. 2010;34(2):153–159. doi:10.1111/j.1753-6405.2010.00500.x
26. Xiao M, Ja L, Zhang X, Ze Z. Factors affecting functional outcome of Sichuan-earthquake survivors with tibial shaft fractures: a follow-up study. J Rehabil Med. 2011;43(6):515–520. doi:10.2340/16501977-0813
27. Kristensen M. Factors affecting functional prognosis of patients with hip fracture. Eur J Phys Rehabil Med. 2011;47(2):257–264.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
