Back to Journals » Biologics: Targets and Therapy » Volume 9
Antidrug antibodies against TNF-blocking agents: correlations between disease activity, hypersensitivity reactions, and different classes of immunoglobulins
Authors Benucci M , Li Gobbi F, Meacci F, Manfredi M, Infantino M, Severino M, Testi S, Sarzi-Puttini P, Ricci C, Atzeni F
Received 18 June 2014
Accepted for publication 12 November 2014
Published 17 February 2015 Volume 2015:9 Pages 7—12
DOI https://doi.org/10.2147/BTT.S69606
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Doris Benbrook
Maurizio Benucci,1 Francesca Li Gobbi,1 Francesca Meacci,2 Mariangela Manfredi,2 Maria Infantino,2 Maurizio Severino,3 Sergio Testi,3 Piercarlo Sarzi-Puttini,4 Cristian Ricci,5 Fabiola Atzeni4
1Rheumatology Unit, 2Immunology and Allergology Laboratory Unit, 3Allergy and Clinical Immunology Unit, Nuovo Ospedale S Giovanni di Dio, Florence, Italy; 4Rheumatology Unit, L Sacco University Hospital, Milan, Italy; 5Department of Epidemiology and Preventive Medicine, University of Regensburg, Regensburg, Germany
Abstract: Although anti-TNF drugs have changed the clinical course of rheumatoid arthritis (RA), survival rates and resistance-to-therapy data confirm that about 30% of RA patients fail to respond. The aim of this study was to evaluate the correlations between the development of antidrug antibodies, specific IgG4 antibodies against TNF inhibitors, and resistance to therapy in RA patients. This retrospective study involved 129 patients with established RA naïve to biological agents (98 females and 32 males, mean age 56.7±12.3 years, disease duration 6.3±1.2 years, baseline Disease Activity Score [DAS]-28 3.2–5.6) who received treatment with anti-TNF agents after the failure of conventional disease-modifying antirheumatic drugs (32 received infliximab [IFX], 58 etanercept [ETN], and 39 adalimumab [ADA]). After 6 months of treatment, the patients were classified as being in remission (DAS28 <2.6), having low disease activity (LDA; DAS28 2.6–3.2), or not responding (NR: DAS28 >3.2). The patients were also tested for serum antidrug antibodies and IgG4 antibodies against TNF inhibitors. After 24 weeks of treatment, 38% of the ETN-treated patients and 28% of those treated with ADA had injection-site reactions; the rate of systemic reactions in the IFX group was 25%. The differences among the three groups were not statistically significant (P=0.382; ETN versus ADA P=0.319). The percentages of patients with adverse events stratified by drug response were: LDA 8% and NR 18% in the ADA group; in remission 3%, LDA 22%, and NR 10% in the ETN group; and LDA 6% and NR 16% in the IFX group (P=0.051). The percentages of patients with antidrug antibodies were: ADA 33.3%, ETN 11.5%, and IFX 10.3% (P=0.025; ADA versus ETN P=0.015). The percentages of patients with IgG4 antibodies were: ADA 6%, ETN 13%, and IFX 26% (P=0.017; ADA versus ETN P=0.437). Associations between antidrug antibodies, specific IgG4 antibodies, and adverse reactions were not significant for any of the three drugs. IgG4 levels were higher in the ADA group than in the other two groups, and higher in the patients with worse DAS28 (NR) and in those experiencing adverse events. These data suggest a possible association between IgG4 levels and worse DAS28 (r2=5.8%, P=0.011). The presence of specific IgG4 antibodies against TNF blockers in patients with RA might affect the drugs’ activity. Patients with injection-site reactions and IgG4 against ETN may show a decreased response.
Keywords: antidrug antibodies, TNF-blocking agents, IgG4 antibodies
Introduction
Over the last 20 years, biological therapies (especially TNF inhibitors) have revolutionized the management of chronic inflammatory diseases, including rheumatoid arthritis (RA). Disease management has been dominated by the three TNF inhibitors infliximab (IFX), adalimumab (ADA), and etanercept (ETN), but despite an acceptable response rate of 60%–70%, a substantial proportion of patients fail to respond (primary failure) or experience significant side effects.1 Some questions have also arisen concerning the safety of TNF inhibitors, because they can trigger immunization, induce rare type I and III hypersensitivity, and cause acute and delayed reactions.
There have been many reports of reactions in patients receiving intravenous IFX, a chimeric IgG1k anti-TNF agent,2 and immunomediated side effects, such as cutaneous reactions, have been encountered during therapy with subcutaneous anti-TNF drugs. One recent paper described injection-site reactions in 29.3% of patients treated with ETN.3 Adverse reactions to biological agents have been categorized into five types, including a complement-mediated reaction with immediate IgE or delayed IgG antibody formation.4 The immunoglobulin IgG4 is an IgG subtype that has been described by some authors (particularly Parish in the 1970s)5 as potentially causing transient sensitization that leads to signs and symptoms comparable with those induced by IgE-mediated reactions; this was initially termed IgG short-term sensitizing by Parish, because upon passive transfer to normal skin, the sensitivity persists for only 2–4 hours. IgG4 differs from IgE insofar as it present in amounts that are large enough to be detected by agglutination or precipitation assays, and its sensitizing activity is not destroyed by heat or (in most cases) chemical reducing agents.4
All biological agents (whether of entirely human origin, chimeric, or “humanized”) can cause an immune response, leading to the formation of antidrug antibodies (ADAbs), which are also known as human antichimeric antibodies or human antihuman antibodies, depending on the nature of the drug. The generation of ADAbs is increasingly recognized as a mechanism explaining the failure of anti-TNF drugs in chronic inflammatory diseases. The lack of a clinical response in patients with ADAbs may be due to the formation of an immune complex between TNF inhibitors and ADAbs that suppresses the drug and restricts its therapeutic activity.1
The aim of this study was to evaluate the correlations between the development of ADAbs and specific IgG4 antibodies against TNF inhibitors, adverse local and general hypersensitivity events, and resistance to therapy in RA patients.
Materials and methods
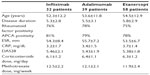
This retrospective study involved 129 patients with established RA naïve to biological agents (98 females and 32 males, mean age 56.7±12.3 years, disease duration 6.3±1.2 years, baseline Disease Activity Score [DAS]-28 scores 3.2–5.6) who received treatment with anti-TNF agents after the failure of conventional disease-modifying antirheumatic drugs: 32 (24.8%) received IFX, 58 (44.9%) ETN, and 39 (30.3%) ADA. Table 1 shows their baseline characteristics.
After 6 months of treatment, the patients were classified as being in remission (DAS28 <2.6), having low disease activity (LDA; DAS28 2.6–3.2), or not responding (NR; DAS28 >3.2). During the 24 weeks of treatment, we also evaluated injection-site reactions in patients treated with ETN or ADA, and systemic reactions in those treated with IFX.
The patients were tested for serum ADAbs with an anti-TNFα-blocker enzyme-linked immunosorbent assay kit (Immundiagnostik, Milan, Italy) and IgG4 antibodies against TNF inhibitors (fluoroenzyme immunoassay kit for ImmunoCap® 250; Phadia, Uppsala, Sweden). ADAb (Immundiagnostik) titers higher than 0.44 OD for ETN, 0.18 OD for ADA, and 0.27 for IFX were considered positive. IgG4 antibodies against TNF inhibitors (ImmunoCap) higher than 5.9 mg arbitrary unit/liter for ETA, 19.5 mg A/L for ADA, and 8.6 mg A/L for IFX were considered positive.
Statistical analysis
Power calculation was performed on correlation coefficients considering Fisher’s Z-transformation, with an α-value of 0.05. For our simulation, we considered the following scenarios: a correlation coefficient ranging from 0.4 to 0.6 and a lower 95% confidence limit of the correlation coefficient (null correlation) ranging from 0.05 to 0.1. In the more conservative scenario (rsp =0.4 and null correlation of 0.1), we calculated that more than 90 subjects inclusive of up to 10% of missing values may be considered sufficient to achieve a nominal power over 90% (Figure S1).
Statistics revised
Continuous variables were expressed as means ± standard deviation and categorical variables were described by percentages. The χ2 test was used to compare categorical variables among groups, and the Pearson correlation coefficient was used to investigate for relations between quantitative variables. An α-value of 0.05 was considered statistically significant, and all statistical tests were two-tailed. IgG4 levels were considered positive if superior to the following cutoff values: ETN 5.9, ADA 19.25, and IFX 8.6. ADAb levels were considered positive if superior to the following cutoff values: ETN 0.446, ADA 0.187, and IFX 0.275. Analyses were performed using Minitab16 software.
Results
After 24 weeks of treatment, 38% of the ETN-treated patients and 28% of those treated with ADA had injection-site reactions; the rate of systemic reactions in the IFX group was 25%. The differences were not statistically significant (P=0.382; ETN vs ADA P=0.319).
The percentages of patients with adverse events stratified by drug response were: LDA 8% and NR 18% in the ADA group; remission 3%, LDA 22%, and NR 10% in the ETN group; and LDA 6% and NR 16% in the IFX group (P=0.051). The percentages of patients with ADAbs were: ADA 33.3%, ETN 11.5%, and IFX 10.3% (P=0.025; ADA vs ETN P=0.015). The percentages of patients with IgG4 antibodies were: ADA 6%, ETN 13%, and IFX 26% (P=0.017; ADA vs ETN P=0.437). Associations between ADAbs, specific IgG4 antibodies and adverse reactions were not significant for any of the three drugs.
A scatter plot showed a positive correlation between IgG4 levels and worse DAS28, (0.241, r2=5.8%; P=0.011; Figure 1). IgG4 quantities were higher in the ADA group than in the other two groups (Figure 2), but the correlation with DAS28 was only significant for the ETN group, (ADA 0.287, P=0.094; ETN 0.299, P=0.039; IFX 0.314, P=0.097). The correlation between ETN and DAS28 was consistent with the higher percentage of ETN patients positive for IgG4 (shown earlier) with respect to the ADA patients. There was a positive correlation between IgG4 levels (regardless of the drug group) in patients experiencing adverse events (Figure 3, red line and dots; subjects having experienced adverse events correlating with DAS28 value =0.578, r2=33.5%; P=0.000).
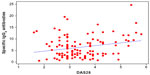  | Figure 1 Scatter plot of specific IgG4 antibodies versus DAS28. |
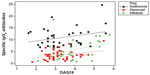  | Figure 2 IgG4 specific antibodies against three different TNF blocking agents and DAS28. |
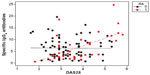  | Figure 3 Correlation between IgG4 specific antibodies, adverse effects and DAS28. |
Discussion
Our results suggest that IgG4 may play a role in the adverse reactions and therapeutic response to biological agents of patients with RA. The role of anti-ADA IgG4 was first detected by means of an immunoassay in 271 consecutive RA patients during 3 years of treatment: anti-ADA antibodies were detectable in 32%, and specific IgG4 antibodies in 29%. Although IgG4 is often considered to be harmless due to its lack of an effector function, the neutralization of ADA by specific IgG4 antibodies leads to a reduced clinical response.6 In our 24-week study, we detected ADAbs in 33.3% of our ADA patients and IgG4 in only 6%.
Approximately 4% of the total IgG in the serum of Caucasian adults is IgG4,7 which is considered an odd antibody insofar that it is the only IgG unable to activate complement and has a low affinity for Fcγ receptors.8,9 Furthermore, it is able to exchange half-molecules in vivo, thus leading to bispecific antibodies that do not cross-link and the consequent formation of small immune complexes.10,11 Because of its limited ability to trigger immunological effector functions and its tendency to form small immune complexes, it is thought that IgG4 has less effect on the clearance of antigens and plays a limited role in inflammation.
Although the percentage of serum IgG4 is generally low, antigen-specific IgG4 has been described as the main isotype produced in some immune responses. As early as the 1970s, it was shown that chronic antigen exposure to grass pollen and bee venom led to the predominant formation of IgG4,12 and increased allergen-specific IgG4 is associated with a beneficial response to specific allergen immunotherapy in allergic patients.13,14 Chronic treatment with biological agents, such as factor VIII, IFNβ, or therapeutic monoclonal antibodies can be considered long-term exposure to protein antigens. There have been frequent reports of the formation of IgG antibodies against biological agents, some of which have been found to produce IgG4. Prolonged exposure to IFNβ can also lead to the development of IgG4 antibodies in patients with multiple sclerosis,15 but although it has been shown that therapeutic monoclonal antibodies can give rise to the formation of IgG4, there is lack of long-term measurements.16,17 The observation that the proportion of IgG4 antibodies may diminish over time is somewhat unusual, and differs from what has been described in the various allergens.18
Our results showed more injection-site reactions in the ETN group than in the ADA group (38% vs 28%), and the presence of anti-ETN IgG4 in 13% of the patients. Although it is not yet known what factors induce class switching to IgG4, it can be speculated that the immunological context of the patients and/or the intensity of treatment (dosing and frequency) may play a role. One of the reasons for the difference in IgG4 responses between ADA-treated and allergic patients may be that the former received 40 mg every 2 weeks, whereas the patients receiving allergen-specific immunotherapy received 20 μg of allergen twice a week. The frequency of treatment could also explain the increase in anti-ETN IgG4.
Our findings indicate a correlation between adverse drug reactions and a poor response, and suggest that anti-ETN IgG4 may have a decreased response to ETN therapy. Other studies have shown that the formation of anti-ADA antibodies is related to lower functional drug levels and a diminished clinical response.19,20 A large proportion of these antibodies are IgG4 antibodies, which suggests IgG4 is not simply an innocent bystander in this case.21 Although IgG4 antibodies cannot activate complement and have a low affinity for Fc receptors, they may still be able to compete with drug-induced TNFα binding to drugs, thus leading to a clinical nonresponse.
We detected anti-ADA antibodies more frequently than anti-ETN antibodies (33% vs 11.5%), whereas the rate of detection of IgG4 anti-ETN was 13%, which may predict a lower response to ETN therapy in patients with injection-site reactions. One limitation of this study is that it did not measure the serum levels of the three drugs. Our study confirms that patients with injection-site reactions and anti-ETN IgG4 may not respond to ETN therapy.
Acknowledgment
The study was supported by the Rheumatology Unit of the Nuovo Ospedale S Giovanni di Dio, Florence, Italy.
Author contributions
MB and FA designed the study and drafted the paper. MM, MI, and FM performed the laboratory analysis. FLG and MB recruited the patients. PSP commented on and critically edited the paper. All authors contributed toward data analysis, drafting and revising the paper and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Vincent FB, Morand EF, Murphy K, Mackay F, Mariette X, Marcelli C. Antidrug antibodies (ADAb) to tumour necrosis factor (TNF)-specific neutralising agents in chronic inflammatory diseases: a real issue, a clinical perspective. Ann Rheum Dis. 2013;72:165–178. | |
Cheifetz A, Smedley M, Martin S, et al. The incidence and management of infusion reactions to infliximab: a large center experience. Am J Gastroenterol. 2003;98:1315–1324. | |
Dore RK, Mathews S, Schechtman J, et al. The immunogenicity, safety, and efficacy of etanercept liquid administered once weekly in patients with rheumatoid arthritis. Clin Exp Rheumatol. 2007;25:40–46. | |
Pichler WJ, Campi P. Adverse side effects to biological agents. In: Pichler WJ, editor. Drug Hypersensitivity. Basel: Karger; 2007:160–174. | |
Parish WE. Short term anaphylactic IgG antibodies in human sera. Lancet. 1970;19;2(7673):591–592. | |
van Schouwenburg PA, Krieckaert CL, Nurmohamed M, et al. IgG4 production against adalimumab during long term treatment of RA patients. J Clin Immunol. 2012;32:1000–1006. | |
Aalberse RC, van der Gaag R, van Leeuwen LJ. Serologic aspects of IgG4 antibodies. I. Prolonged immunization results in an IgG4-restricted response. J Immunol. 1983;130:722–726. | |
Tao MH, Canfield SM, Morrison SL. The differential ability of human IgG1 and IgG4 to activate complement is determined by the COOH-terminal sequence of the CH2 domain. J Exp Med. 1991;173: 1025–1028. | |
Nirula A, Glaser SM, Kalled SL, Taylor FR. What is IgG4? A review of the biology of a unique immunoglobulin subtype. Curr Opin Rheumatol. 2011;23:119–124. | |
Van Der Zee JS, Van Swieten P, Aalberse RC. Serologic aspects of IgG4 antibodies. II. IgG4 antibodies form small, nonprecipitating immune complexes due to functional monovalency. J Immunol. 1986;137: 3566–3571. | |
van der Neut KM, Schuurman J, Losen M, et al. Anti-inflammatory activity of human IgG4 antibodies by dynamic Fab arm exchange. Science. 2007;317:1554–1557. | |
van der Giessen M, Homan WL, van Kernbeek G, Aalberse RC, Dieges PH. Subclass typing of IgG antibodies formed by grass pollen-allergic patients during immunotherapy. Int Arch Allergy Appl Immunol. 1976;50:625–640. | |
Gehlhar K, Schlaak M, Becker W, Bufe A. Monitoring allergen immunotherapy of pollen-allergic patients: the ratio of allergen-specific IgG4 to IgG1 correlates with clinical outcome. Clin Exp Allergy. 1999;29: 497–506. | |
Nouri-Aria KT, Wachholz PA, Francis JN, et al. Grass pollen immunotherapy induces mucosal and peripheral IL-10 responses and blocks IgG activity. J Immunol. 2004;172:3252–3259. | |
Deisenhammer F, Reindl M, Berger T. Immunoglobulin subclasses in patients with neutralizing and non-neutralizing antibodies against IFN-β1b. J Interferon Cytokine Res. 2001;21:167–171. | |
Svenson M, Geborek P, Saxne T, Bendtzen K. Monitoring patients treated with anti-TNF-alpha biopharmaceuticals: assessing serum infliximab and anti-infliximab antibodies. Rheumatology (Oxford). 2007;46:1828–1834. | |
Wouters D, Stapel S, Vis M, et al. Human antichimeric antibodies to infliximab and infusion-related allergic reactions in patients with rheumatoid arthritis. Allergy Clin Immunol Int. 2007;2:198–200. | |
Aalberse RC, Stapel SO, Schuurman J, Rispens T. Immunoglobulin G4: an odd antibody. Clin Exp Allergy. 2009;39:469–477. | |
van Kuijk AW, de Groot M, Stapel SO, Dijkmans BA, Wolbink GJ, Tak PP. Relationship between the clinical response to adalimumab treatment and serum levels of adalimumab and anti-adalimumab antibodies in patients with psoriatic arthritis. Ann Rheum Dis. 2010;69:624–625. | |
Bartelds GM, Wijbrandts CA, Nurmohamed MT, et al. Clinical response to adalimumab: relationship to anti-adalimumab antibodies and serum adalimumab concentrations in rheumatoid arthritis. Ann Rheum Dis. 2007;66:921–926. | |
Bartelds GM, Krieckaert CL, Nurmohamed MT, et al. Development of antidrug antibodies against adalimumab and association with disease activity and treatment failure during long-term follow-up. JAMA. 2011;305:1460–1468. |
Supplementary materials
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.