Back to Journals » International Journal of General Medicine » Volume 13
Anesthesia During Functional Endoscopic Sinus Surgery for Kartagener’s Syndrome: A Case Report and Literature Review
Authors EL-Radaideh K , Al-Qudah M , Alali M , Alhowary A
Received 24 February 2020
Accepted for publication 9 April 2020
Published 1 May 2020 Volume 2020:13 Pages 157—161
DOI https://doi.org/10.2147/IJGM.S251060
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Khaled EL-Radaideh,1 Mohannad Al-Qudah,2 Maulla Alali,2 Ala”a Alhowary1
1Department of Anesthesiology and Intensive Care, Faculty of Medicine, Jordan University of Science and Technology, Irbid 21110, Jordan; 2Department of Special Surgery, Division of Otorhinolaryngology-Head and Neck Surgery, Faculty of Medicine, Jordan University of Science and Technology, Irbid 21110, Jordan
Correspondence: Khaled EL-Radaideh
Faculty of Medicine, Department of Anesthesiology and Intensive Care, Jordan University of Science and Technology, Irbid 21110, Jordan
Tel +962 799051167
Email [email protected]
Introduction: Kartagener’s syndrome (KS) is a ciliopathic, autosomal recessive disorder characterized by the triad of situs inversus, chronic sinusitis, and bronchiectasis. The abnormal ciliary structure and function lead to variable clinical manifestations, including dextrocardia, pneumonia, bronchitis, chronic rhinosinusitis, otitis media, reduced fertility in women, and infertility in men. This article reports our experience on general anesthesia with endotracheal intubation during functional endoscopic sinus surgery (FESS) in a patient with KS.
Case Presentation: A 44-year-old man was admitted to our hospital with chronic nasal obstruction, postnasal drip, chronic sinusitis, and chronic non-productive cough for FESS. The patient’s heart was on the right side of his chest. A chest roentgenogram and a high-resolution chest and abdomen computed tomography (CT) scan identified dextrocardia, situs inversus, and chronic bronchitis and bronchiectasis involving both lung bases. CT sinuses showed mucosal thickening of bilateral maxillary and ethmoid and sphenoid sinuses. The patient was prescribed oral medications and nasal spray for crepitations and wheezes heard over bilateral lung fields. Intensive chest physiotherapy and supportive care prior to surgery were provided to prevent worsening of lung function. FESS with bilateral frontal polypectomy was performed. All hemodynamic parameters were stable. The emergence from anesthesia was smooth. After ∼ 20 minutes in the post-anesthesia care unit, the patient was fully awake and pain-free. He was then transferred to the surgical intensive care unit and subsequently to the ward. The postoperative period was uneventful. The patient felt subjectively “very well” and was discharged from the hospital on the 2nd postoperative day.
Conclusion: Anesthesiologists must be aware of cardiopulmonary inversion that could challenge the management of patients with KS. To avoid respiratory depression caused by long-acting systemic opioids, we suggest using short-acting opioids during general anesthesia and for postoperative pain relief.
Keywords: case report, FESS, general anesthesia, Kartagener’s syndrome, sinusitis
Introduction
Primary ciliary dyskinesia (PCD) is a group of autosomal recessive disorders, and the subgroup that presents with the triad of sinusitis, bronchiectasis, and dextrocardia is called Kartagener’s syndrome (KS).1 Described by Kartagener in 1933,2 this syndrome has an incidence of1–2/30,000 birth3 and is seen in 40% to 50% of patients with PCD.4
The ciliary dyskinesia and ineffective mucociliary clearance affect many tissues and organs such as the nasal mucosa and paranasal sinuses. However, the pharynx and the lower respiratory tract down to the respiratory bronchioles are covered by unciliated epithelium.5
Patients presenting with respiratory distress, chronic pulmonary disease, bronchiectasis, and sinusitis in the setting of KS are a challenge to the anesthesiologist due to the potential respiratory or cardiac complications.6,7 Therefore, anesthetic management of patients with KS must be conducted carefully. Herein, we describe a case of successful general anesthetic management of a patient with KS who underwent functional endoscopic sinus surgery (FESS).
Case Presentation
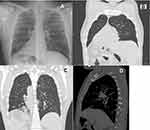
A 44-year-old man was admitted to the Ear, Nose, and Throat department of our hospital in August 2019 with chronic nasal obstruction, postnasal drip, chronic sinusitis, and chronic non-productive cough for FESS. During history-taking, the patient stated that his heart was on the right side of his chest. A chest roentgenogram and a high-resolution chest and abdomen computed tomography (CT) scan identified dextrocardia (Figure 1A), situs inversus (Figure 1B), and chronic bronchitis and bronchiectasis involving both lung bases (Figure 1C and D). CT sinuses showed mucosal thickening of bilateral maxillary and ethmoid and sphenoid sinuses (Figure 2). KS was diagnosed based on the presence of the classical triad.
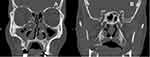 |
Figure 2 High-resolution computed tomography of the sinuses. (A) Shows a mucosal thickening in both maxillary and ethmoid and (B) sphenoid sinuses with diagnosis of chronic sinusitis. |
On admission, the patient’s vital signs, including blood pressure (systolic 112, diastolic 74 mmHg), heart rate (80 beats per minute), respiratory rate (19/min), and the peripheral capillary oxygen saturation (SpO2; 94%), were within normal range. The complete blood count and renal and liver function test results were unremarkable. The 12-lead electrocardiogram (ECG) with reversal of the limb and precordial leads showed sinus rhythm and a normal tracing. The patient had a known allergy to acetylsalicylic acid (Aspirin®) and nonsteroidal anti-inflammatory drugs, and an allergy panel was performed, which revealed positive hazelnut antibodies. Since crepitations and wheezes were heard over bilateral lung fields, the patient was prescribed oral prednisolone (50 mg, once daily (QD), oral lansoprazole (30 mg, QD), oral levofloxacin (500 mg, QD), and 0.1% xylometazoline hydrochloride nasal spray (every 8 h). Intensive chest physiotherapy and supportive care prior to surgery were provided to prevent worsening of the lung function. Additional hypertonic saline nebulizer (every 8 h) and salbutamol nebulizer (5 mg, twice daily) were provided during pre-anesthetic evaluation in order to prepare the patient for safe anesthesia and surgery. The METs estimated by preoperative history at the preoperative evaluation visit were approximately 4 with moderate-intensity activities. He could walk on a flat surface for one or two blocks and up to two flights of stairs.
In the operating theater, an intravenous (IV) access, neuromuscular monitoring, and routine monitors (ECG, non-invasive blood pressure, and pulse oximetry for SpO2) were established. The patient was pre‑oxygenated with a face mask for 3 minutes. General anesthesia was induced with 2 µg/kg IV fentanyl and 2–2.5 mg/kg IV propofol. Neuromuscular blockade was achieved with 0.5 mg/kg atracurium. The trachea was intubated in a single attempt using a single-lumen cuffed tube of internal diameter 8.0 mm. The anesthesia was maintained with 50% O2, N2O, and isoflurane. Remifentanil was given continuously with a syringe infusion pump (Perfusor® Space; B. Braun, Germany) at a rate of 0.1 µg/kg/min adjusted per the patient’s heart rate.
The patient’s lungs were ventilated with a 50% fraction of inspired oxygen. A tidal volume of 7–10 mL/kg and respiratory rate of 10–12 breaths/min were adjusted to maintain the End-tidal CO2 between 30 and 36 mmHg. To increase the lung functional residual capacity a small amount of PEEP (5 cmH2O) was applied during the mechanical ventilation of the patient. A single dose of IV cefotaxime 1 g was administered intraoperatively.
About 20 minutes before the end of the surgery, 1 g paracetamol with 100mg tramadol was infused for 15 minutes. Dexamethasone 8 mg and metoclopramide 10 g were also given intravenously.
The duration of FESS with bilateral frontal polypectomy was 95 minutes. All hemodynamic parameters were stable, and no additional muscle relaxant or fentanyl was required throughout the procedure. At the end of the surgery, the residual neuromuscular block was reversed with IV neostigmine 0.05 mg/kg and IV atropine 1 mg.
Lungs suctioning through the endotracheal tube and oral suctioning were performed gently. Tracheal extubation was performed when the patient was able to open the eyes and ventilate spontaneously. The emergence from anesthesia was smooth and without complications. After ~20 minutes in the post-anesthesia care unit, the patient was fully awake and pain-free (pain scale 2). The patient was then transferred to the surgical intensive care unit for 8 hours, and subsequently to the ward. An arterial blood gas analysis on room air showed pH = 7.419, oxygen concentration (PaO2) = 70 mm Hg, carbon dioxide concentration (PaCO2) = 36 mm Hg, bicarbonate ion concentration (HCO3−) = 23 mmol/L, O2 saturation = 94%, and base excess = −1 mmol/L. The postoperative period was uneventful. The patient felt subjectively “very well” and was discharged from the hospital on the second postoperative day.
Discussion and Conclusion
KS is the most common type of PCD, characterized by chronic recurrent rhinosinusitis, bronchiectasis, and situs inversus. As a rare autosomal recessive inherited disease, its incidence is estimated to be 1 in 32,000.2 Dysfunction of the motile cilia causes ineffective mucus clearance and organ laterality defects. Affected patients usually present with chronic infections of the upper and lower respiratory tract, otitis media, pneumonia, and bronchiectasis, often complicated by infections with Pseudomonas spp.8,9
Impaired ciliary motility could cause perioperative respiratory difficulty in patients with KS.10 Serapinas et al11 recommend a combination of physiotherapy and physical exercise to enhance respiratory tract clearance, along with the aggressive treatment of upper and lower respiratory tract infections. We provided intensive physiotherapy and supportive pulmonary care prior to surgery for our patient, along with the antibiotic levofloxacin for preventing the progressing of the respiratory tract infection. Appropriate preoperative respiratory tract management is also essential to prevent potential peri- and postoperative morbidities such as acute respiratory failure and pulmonary edema.12
General anesthesia or regional techniques such as neuraxial anesthesia could be chosen for patients with KS, with the regional techniques presenting fewer risks than general anesthesia. In our patient, we used propofol for the induction of anesthesia. Propofol dilates the bronchi, slightly decreases mucus production, and suppresses the airway reflexes.10 Wu et al13 report significantly better protection against an increase in airway resistance using propofol than that using thiopentone after tracheal intubation. To achieve muscle relaxation for facilitating endotracheal intubation, we chose atracurium for our patient, primarily due to its ability to degrade spontaneously in plasma and tissues at normal body pH and temperature (Hofmann degradation). We maintained anesthesia with 1–1.3 minimum alveolar concentration of isoflurane as inhalational anesthetics cause bronchodilation in a dose-related manner.13 This is especially important in patients with a compromised respiratory tract due to KS.
Dextrocardia has an incidence rate of ~2 per 10,000 births. Associated congenital cardiac anomalies occur in less than 3% with dextrocardia and include inter alia, atrial septal defects, ventricular septal defects, and pulmonary valve stenosis. When ECG leads are reversed, patients with dextrocardia show sinus rhythm and the heart mostly appears normal without other abnormalities, as seen in our patient.14,15
In conclusion, anesthesiologists must be aware of cardiopulmonary inversion that could challenge the pre-, peri-, and postoperative management of patients with KS. To avoid the respiratory depression caused by long-acting systemic opioids, we suggest using short-acting opioids during general anesthesia and for postoperative pain relief. Cardiopulmonary complications could be prevented to a large extent by proper perioperative suctioning of the pharynx and pulmonary tract and adequate postoperative management to prevent nausea and vomiting.
Abbreviations
CT, Computed tomography; FESS, functional endoscopic sinus surgery; KS, Kartagener’s syndrome; PCD, primary ciliary dyskinesia; QD, once daily; ECG, electrocardiogram; IV, intravenous.
Data Sharing Statement
The data that support the findings of this study are available on request from the corresponding author, KEL.
Ethics and Consent Statement
Based on the regulations of the department of research of the Jordan University of Science and Technology, an institutional review board approval is not required for case reports.
Consent for Publication
A written permission for the use of patient data for publication was obtained.
Author Contributions
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Funding
The authors declared that this case has received no financial support.
Disclosure
The authors declare that they have no competing interests.
References
1. Kumar A, Verma AK, Kumar A, et al. Kartagener syndrome: a review of three cases. Sahel Med J. 2015;18:203–206.
2. Potdar PV, Nayak MM, Chitnis A. Kartagener’s syndrome. Med J DY Patil Univ. 2012;5:158–160. doi:10.4103/0975-2870.103349
3. Taušan Đ, Ristić A, Zvezdin B. Kartagener’s syndrome: a case report. Vojnosanit Pregl. 2016;73:873–876. doi:10.2298/VSP141020072T
4. Shapiro AJ, Davis SD, Ferkol T, et al. Laterality defects other than situs inversus totalis in primary ciliary dyskinesia: insights into situs ambiguous and heterodoxy. Chest. 2014;146:1176–1186. doi:10.1378/chest.13-1704
5. Leigh MW, Pittman JE, Gerson JL, et al. Clinical and genetic aspects of primary ciliary dyskinesia/Kartagener syndrome. Genet Med. 2009;11:473–487. doi:10.1097/GIM.0b013e3181a53562
6. Goutaki M, Meier AB, Halbeisen FS, et al. Clinical manifestations in primary ciliary dyskinesia: systematic review and meta-analysis. Eur Respir J. 2016;48:1081–1095. doi:10.1183/13993003.00736-2016
7. Lucas JS, Barbato A, Collins SA, et al. European Respiratory Society guidelines for the diagnosis of primary ciliary dyskinesia. Eur Respir J. 2017;49:
8. Pereira R, Barbosa T, Gales L, et al. Clinical and genetic analysis of children with Kartagener syndrome. Cells. 2019;8:
9. Skeik N, Jabr FI. Kartagener syndrome. Int J Gen Med. 2011;4:41–43. doi:10.2147/IJGM.S16181
10. Bhosale GP, Shah VR. Anesthesia for percutaneous nephrolithotomy in a case of Kartagener’s syndrome. J Anaesthesiol Clin Pharmacol. 2013;29(2):280–282.
11. Serapinas D, Staikūnienė J, Barkauskienė D, Jackutė J, Sakalauskas R. An unusual regression of the symptoms of Kartagener syndrome. Arch Bronconeumol. 2013;49:28–30. doi:10.1016/j.arbres.2012.02.021
12. Savitha KS, Sunanda S, Vijayan R. Kartagener’s syndrome-anaesthetic implications. Indian J Anaesth. 2006;50(6):469–471.
13. Wu RS, Wu KC, Sum DC, Bishop MJ. Comparative effects of thiopentone and propofol on respiratory resistance after tracheal intubation. Br J Anaesth. 1996;77:735–738. doi:10.1093/bja/77.6.735
14. Reidy J, Sischy S, Barrow V. Anaesthesia for Kartagener’s syndrome. Br J Anaesth. 2000;85:919–921. doi:10.1093/bja/85.6.919
15. Bajwa SJ, Kulshrestha A, Kaur J, Gupta S, Singh A, Parmar SS. The challenging aspects and successful anaesthetic management in a case of situs inversus totalis. Indian J Anaesth. 2012;56:295–297. doi:10.4103/0019-5049.98781
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.