Back to Journals » Pediatric Health, Medicine and Therapeutics » Volume 15
Acute Computer Tomography Findings in Pediatric Accidental Head Trauma-Review
Authors Popescu CM ![]() , Marina V
, Marina V ![]() , Munteanu A
, Munteanu A ![]() , Popescu F
, Popescu F ![]()
Received 31 January 2024
Accepted for publication 20 May 2024
Published 11 June 2024 Volume 2024:15 Pages 231—241
DOI https://doi.org/10.2147/PHMT.S461121
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Roosy Aulakh
Cristina-Mihaela Popescu,1 Virginia Marina,2 Anisoara Munteanu,3 Floriana Popescu4
1Dental-Medicine Department, Faculty of Medicine and Pharmacy, “Dunărea de Jos” University, Galati, 800201, Romania; 2Medical Department of Occupational Health, Faculty of Medicine and Pharmacy, “Dunărea de Jos” University, Galati, 800201, Romania; 3Oncology Department of Emergency Hospital, Braila, Romania; 4Department of English, Faculty of Letters, “Dunărea de Jos” University, Galati, 800201, Romania
Correspondence: Virginia Marina, Tel +40-770-89-82-74, Email [email protected]
Abstract: Head trauma in paediatric patients is a worldwide and constant issue. It is the number one cause for childhood mortality and morbidity. Children of all ages are susceptible to sustaining head trauma and the anatomical characteristics of the region put them in a high-risk category for developing severe traumatic brain injuries. Boys are more frequently victims of accidental head traumas, and their injuries are more severe than those encountered in girls. The mechanisms of the trauma are a determining factor for the types of lesions we find. The traumatic injuries fall into two categories, primary and secondary. Primary traumatic injuries can be severe and life threatening, and their presence needs to be documented in order to set the correct therapeutic conduct. Due to their importance, this pictorial review focuses on them and the images used herein are selected from the database of our hospital. It is important to distinguish each of the different injuries that can be encountered. At the same time, radiologists are advised to remember that for children up to five years of age, some non-accidental imaging findings may appear to coincide with those found in accidental head trauma.
Keywords: paediatric accidental head trauma, traumatic brain injury, epidural haematoma, subdural haematoma, traumatic subarachnoid haemorrhage, haemorrhagic cortical contusions
Introduction
Head trauma is the leading cause of emergency room visits all over the world. This is as valid for adults as well as for paediatric patients. At the same time, it is also the number one cause of morbidity and mortality in childhood.1–7 Head trauma can have as a result traumatic brain injuries (TBIs).8 They can either be primary or secondary. Primary traumatic injuries can be severe and life threatening, and their presence needs to be documented in order to set the correct therapeutic conduct. Due to their importance, this pictorial review focuses on them, and the images used herein are selected from the database of our hospital.
Head trauma is divided into two major categories, ie, accidental, and non-accidental.
Although this pictorial review focuses on acute findings in accidental head trauma, there are some things worth mentioning about abuse. It was first described in 1946; in the 1960’s it was known as “Battered Child Syndrome”, and then in 1970’s – “Shaken Baby Syndrome”. Extensive studies on the biomechanics of abusive head trauma have shown that the lesions that are seen in the most serious acute abuse cases are not only the result of shaking, but also of direct impact to the head. Because the severity of the TBIs is not explained only by shaking, the American Academy of Paediatrics issued in 2009 a statement recommending the use of “Abusive Head Trauma”. Some common traumatic lesions found in abusive head trauma are also present in accidental one, although there are some particularities. The presence of retinal haemorrhages, long bone fractures and also cutaneous and spinal injuries may suggest foul play. But the diagnosis of abuse cannot be made or excluded based only on imaging findings. There are more pieces of the puzzle that need to be gathered and connected to each other for such a diagnosis to be made. Some TBIs may be found in both abuse and accidental head trauma, hence both these possible diagnoses should be taken into consideration. One should always consider non-accidental head trauma even if the caregiver declares accidental head trauma has occurred. Both paediatric and elderly patients are prone to sustaining more non-accidental head traumas than the rest of the population. Children may be the victims of abusive head trauma up to five years of age, but more frequently between 0–2 years.9
Fortunately, accidental head traumas exceed the non-accidental ones. Accidental head trauma is less related to age, and it has various causes. Gender, age, rural or urban location, even economic status of the family and the country they live in greatly influence head trauma.9 Boys are more frequently victims of head trauma, no matter the age group.7,8,10,11 When we take age into consideration, things differ from region to region worldwide. In Europe, for example, in a 2014 study based on the reports from 33 countries, the highest incidence is for the 0–4 years group.10 Differences between rural and urban areas are explained by different mechanisms of the trauma which also greatly impacts the lesions.
Relevant Sections
The images used in this pictorial review to illustrate different TBIs are from patients who were scanned in the Radiology Department of the Clinical Emergency Children’s Hospital in Galați, Romania. All these patients came to the emergency room of our hospital after sustaining head traumas. Studies were performed during 2008–2023 using two different CT scanners, ie, Hitachi Eclos and Philips Incisive.
Anatomical Characteristics
The type of TBI is closely related to the mechanism of the trauma and the anatomical particularities of the skull, face bones, brain, and neck muscles.2 The children’s skull has bones with high plasticity and deformity resulting in better absorption of the forces. As a result, fractures are less seen in children than adults. Patent sutures also allow the bones to “move” a little when mechanical forces are applied. They can also widen and prevent a rapid increase in intracranial pressure.2 The new born’s brain has a high percentage of water which makes the brain “softer” and susceptible to sustaining TBIs (shear injuries). Myelination is a process that takes place over time, and it follows certain patterns in the brain. In infants, the percentage of myelin in the brain is lower and it increases with time, which in addition to denser packing of the fibres makes the brain denser. Also, the head/body ratio is different in babies and children than adults. Infants are born with large head/body ratios, and this ratio changes over time. In addition to this, the head is also “heavy”, and it needs the neck muscles and the cervical spine for support. In addition to weak neck muscles, the younger the child, the more the cervical-cranial junction is dependent on the ligaments. When factoring in all these anatomical particularities of the cervical extremity, there is a high risk in also developing cranio-cervical junction lesions.
Injury Mechanisms in Accidental Head Trauma
No matter the way the accidental trauma may occur (motor vehicle accident, falling, being hit by a flying baseball, etc.), the mechanisms are divided into the following main categories: impulsive loading and impact loading. The first one happens when there is an impact on another place of the body and the head moves because of that force. The impact loading occurs when the head hits a stationary object or is hit by a moving object. Since the mechanical forces applied to the brain are different in these two cases, the injury patterns will also be different. After impulsive loading, the most common TBIs are subdural haematomas, and diffuse axonal injuries (more frequently in babies and small children). Impact loading implies the direct contact between the head and an object which can result in scalp lesions, fractures, coup and contrecoup TBIs.
Acute CT Imaging Findings in Accidental Head Trauma
The trauma can have as a result primary lesions - which appear as a direct consequence of the traumatic force exerted on the head - and secondary lesions - which are the effect of the first ones.
TBIs may be either intra- or extra-axial.12 Post-traumatic head lesions can involve all the anatomical structures. Besides the TBIs, the scalp and the skull can also be involved. Based on their location, primary TBIs can be extra- or intra-axial. The former are the epidural haematoma, subdural haematoma, traumatic subarachnoid haemorrhage, and intraventricular posttraumatic haemorrhage. Intra-axial TBIs consist of diffuse axonal injuries (DAI), haemorrhagic cortical contusions, intracerebral haemorrhage, and vascular injuries.
As previously mentioned, secondary TBIs develop over time as a consequence of the primary ones. They can be acute (ie oedema, herniation, or ischemia) or chronic (ie hydrocephalus, encephalomalacia, or cerebrospinal fluid leak). Oedema can be vasogenic or cytotoxic, the latter being more frequently associated with TBI.13 It can lead to increased intracranial pressure and herniation.14 Herniation is the result of mass effect of either primary lesions (eg subdural haematoma, intracerebral haemorrhage) or secondary ones (eg cerebral oedema) that force the brain to “slide” through anatomical “gateways”. In other words, brain parenchyma can herniate under the falx (subfalcine herniation), over the free margin of the tentorium (uncal herniation) or through the tentorium (trans tentorial). Each of these types of hernias have their intrinsic risks that in turn can cause further complications (ischemia, haemorrhage).
When the patient arrives to the emergency room, enough time has passed in order for both primary and secondary lesions to develop. Some may need intensive care supervision; others may require emergency surgical treatment. In order to know which therapeutic road to take, imaging has to be performed without any further delay. Head imaging in trauma has two main goals: 1) to identify the lesions without further delay; 2) to assess any secondary lesions, such as herniation. Non enhanced CT (NECT) scanning is the go-to investigation in this case.4,15,16 It can delineate almost all of the lesions aforementioned, and it will not only show acute primary and secondary findings, but it will also allow us to undertake diligent measures to prevent life threatening secondary lesions.
Most of the acute primary traumatic lesions are hemorrhagic collections. In the hyperacute phase, before blood has had time to form a clot, the density of the hematoma will be under 60 Hounsfield units (HU); it is also a reflection of the patient’s hematocrit. In the acute phase of the blood, the clot is already established, and the density will have increased, measuring between 60–90 HU. This is the time when we get most of our patients to the CT scan. The blood at this time is hyperdense enough to be “seen”. If the thickness of the blood is not large enough to be evaluated with the standard windowing, changing its width and level can help diagnosis. In the subacute phase, days after the trauma, the clot starts to become less dense, and the density is almost the same as that of the cortex. This is the moment when the hematoma becomes isodense to the brain parenchyma and can be easily overlooked. In the chronic stage, the collection becomes isodense to the cerebrospinal fluid.
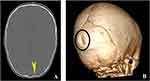
Scalp lesions are a consequence of either blunt force trauma or penetrating trauma to the head. There can be soft tissue lacerations, subgaleal hematoma, cephalhematoma or radio-opaque foreign bodies in the soft tissue. Soft tissue lacerations can have variable extent or thickness. They appear as areas of discontinuity in the scalp. Cephalhaematoma is the accumulation of blood between periosteum and the outer table of the calvaria. It is a small hemorrhage contained by bone, does not cross skull sutures and is seen post-delivery. Subgaleal hematomas (Figure 1) are located between the periosteum of the calvaria and the occipitofrontalis muscle aponeurosis and are hyperdense. It is not contained by sutures and in case of a large blood, the haematoma can extend around the skull. Subgaleal haematomas are the most common soft tissue lesions in blunt force traumas to the head and they seem to be more associated with an underlying skull fracture rather than the impact place itself.17 Foreign bodies in the soft tissue appear as radio-opaque material outside the skull, most of the times accompanied by soft tissue lacerations.
Skull fractures are linear, depressed, elevated, diastatic, and compound. Linear fractures (Figure 2) are a result of low impact blunt force trauma to the head and are usually situated under a subgaleal haematoma. They appear as lucent well-demarcated lines in the skull and can extend on a larger area. Some are easily missed if they are parallel to the plane of the section. The most frequent site of the fracture is the parietal bone, followed by the frontal and temporal one.9,18 Both in accidental and non-accidental head traumas fractures can come in contact with one skull suture, but in accidental trauma it is rare for the fracture to touch more sutures.19,20 Depressed fractures happen when there is an impact with a blunt object, and there is also high energy transferred to a small area of the skull. The bone fragment/fragments are inwardly depressed and there can also be other linear fragments associated. These types of fractures are usually accompanied by other types of traumatic brain injuries.18 A special type of depressed fracture is the ping-pong fracture (Figure 3), an entity almost exclusive to new borns and infants.21 In this situation, there is a sunken area of the skull with no discontinuity of the inner or outer table of the skull. Elevated fractures have an elevated fragment of bone, usually also rotated. They occur when the impact with a heavy object is accompanied by a rotational motion of the head.22 Diastatic fractures widen the sutures. Sometimes there is another linear fracture that abuts the diastatic suture.
Epidural haematomas (EDH) (Figure 4) are a collection of blood between the inner table of the skull and the dura mater. On NECT scans the aspect is of a hyperdense, biconvex, well defined extra-axial collection which displaces the adjacent brain parenchyma. The dura mater is tightly attached to the skull at the sutures, and this is why the extradural haematomas never cross sutures. However, the periosteal walls of the sagittal sinus are not as well connected to the dura accounting for EDH in the region to cross the middle line. EDH is a rare post-traumatic entity in paediatric patients, some accounting for up to 3% of the post-traumatic lesions.3,23,24 In the majority of cases (84%) it is accompanied by a skull fracture.3 Some studies argue that the most frequent location is the temporal location,3,24 while others disagree.23 Although posterior fossa location is rarely encountered, it is known to be the most serious one.25,26 The cause for the blood is a tear in an arterial vessel, which most commonly is the middle meningeal artery.27
 |
Figure 1 Axial NECT of a 2 years 7 months old girl who fell on the stairs. Brain window shows right temporo-parietal epicranial haematoma (Yellow arrow). |
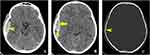 |
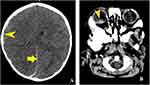
Figure 4 Axial NECT of an 8 years 8 months old girl who hit her head on the concrete while riding a scooter. Right temporo-parietal EDH. (A) Axial NECT brain window shows lenticular hyperdense collection in the right temporo-parietal region - epidural haematoma (yellow pointed arrow). (B) Red arrow shows EDH which is hyperdense because of the clotted blood; yellow pointed arrow indicates hypodense area inside the haematoma suggesting active bleeding (“swirl sign”).4,27 The density of fresh blood is lower than the clotted blood’s one. (C) yellow pointed arrow Axial NECT bone window shows temporo-parietal linear fracture associated with the EHD. |
 |
Figure 8 Axial NECT CT of 16-year-old male who fell from 2 m height. Brain window reveals right frontal haemorrhagic cortical contusion (yellow pointed arrow). |
Subdural haematomas (SDHs) (Figure 5) are a blood accumulation between the inner layer of the dura mater and the arachnoid. The meninges are not so tight together, this is why the blood will diffuse on the whole convexity of the hemisphere. The acute SDHs appear as hyperdense crescent-shape extra-axial collections, mainly distributed along the convexity of the brain parenchyma, but they can also have a parasagittal or tentorial location. Just like EDHs, the posterior fossa SDHs are more ominous.28 Since the volume can increase a lot in a short period of time, SDH can have mass effect on the underlying brain parenchyma and thus entails high risk for herniation.13,29 The only thing that differentiates the age of SDH is the density - subacute ones are isodense to the brain, and the chronic ones are hypodense. The SDH is an entity associated with a high mortality and morbidity,29 and in children under five years is the most common sign of non-accidental trauma.30–32 The typical triad found in abusive head trauma is represented by subdural haematomas, retinal haemorrhages, and encephalopathy.31,33 (Figure 6) These are accompanied most of the time by fractures (either of the skull or of long bones).34 This is a complex situation where the final verdict is set after taking into consideration both the neuroimaging data, clinical exam, and the history of the patient provided by the caretaker as well as the lab results.31,33 Although the neuroimaging lesions described by the radiologist are not the only criterion for abuse diagnosis, the final decision will be based on them as well, making the radiologist’s role crucial.35
Traumatic subarachnoid haemorrhage (tSAH) (Figure 7) is the accumulation of blood between the arachnoid and pia mater. Most of the SAH are caused by head trauma.36–38 Also, in many cases of moderate and severe brain injuries, tSAH is present.38–40 It can be focal, in which case on NECT scans it appears as hyperdense curvilinear shape that follow the anatomy of the convexity sulci (in the vicinity of the contusion) or hyperdense collection in the subarachnoid spaces (most commonly the Sylvian cistern or the frontal inferior subarachnoid spaces). Another form of tSAH is the diffuse haemorrhage and its aspect is that of a hyperdense collection in the basal cisterns and/or in the subarachnoid space.
Intraventricular haemorrhage (IVH) represents the accumulation of blood inside the ventricles. It is usually the consequence of a parenchymal blood ruptured into the ventricles, the blood from the subarachnoid space entering the ventricles via the outflow foramina, or the bleeding from the subependymal veins along the surface of the ventricle. It is not a type of lesion that exists on its own, but it rather accompanies other serious post-traumatic lesions. Unless the blood is a direct consequence of tearing in the subependymal veins due to rotational forces, the IVH is a lesion that makes the transition between the primary and secondary type lesions.
Haemorrhagic cortical contusions (HCCs) (Figure 8) are patchy areas of haemorrhage involving the grey matter and subcortical white matter. On NECT scans they appear as different sized hyperdense cortical foci surrounded by hypodense oedematous brain parenchyma. As far as the location goes, the HCCs form where the brain comes in contact with irregular bony areas of the skull or near dural folds. HCCs can be situated under the site of the trauma and they are known as coup lesions. When situated opposite the site of the trauma, they are called contrecoup lesions. The contrecoup lesions are larger than the coup lesions. As hours go by after the impact, both the size of the initial HCCs and their number may increase due to added local haemorrhage. The HCCs and the surrounding oedema display mass effect on surrounding brain parenchyma. HCCs are associated with moderate and severe trauma.41–43
Diffuse axonal injuries (DAI) (Figure 9) are traumatic intra-axial lesions that represent stretches or tears in the axons in particular locations. DAIs occur when differential in deceleration/acceleration between cortex and deep structures in the brain occurs, causing these structures to have different inertia and stretch axons. Another cause for these types of lesions is either the rotational strain or shear forces. The anatomical structures that are mainly affected by DAIs are the corpus callosum, cortex-white matter junction in the frontal-temporal lobes and the brainstem. On NECT scans, DAIs appear as small hypodense foci if there is no bleeding or small hyperdense foci if haemorrhage is associated. Even if there are DAIs, only in 10% of the cases small bleeding areas are demonstrated on NECT scans.44 Since NECT scans of the head fail to identify most of the DAIs, it is not the imaging tool we rely on to diagnose this pathology.44,45 In this particular situation, MRI is the most suitable imaging tool to diagnose DAI.46 The signal depends on the type of the lesion – haemorrhagic or not – and on the age of the blood. We use use T1-, T2- weighted imaging, T2*GRE or SWI, FLAIR, and DWI sequences. If the acute lesion has a haemorrhagic component to it, it will show up as an area of high signal on T2-, FLAIR, DWI sequences. SWI will show the same areas with low signal because of the blood compounds inside the lesions and their magnetic properties. DAIs with no blood inside will only display the oedema signal throughout the sequences. DAIs usually have bad prognosis, but in paediatric population the outcome seems better than in the adults.47
Intracerebral haemorrhage (ICH)) is an accumulation of blood in the white matter of the brain after the rotational forces tear intraparenchymal blood vessels (be they arteries or veins). The most common sites are the frontotemporal areas and basal ganglia. On NECT they appear as hyperdense collections. If the HCCs only involve the cortical matter and are surrounded by oedema, the ICH is situated in the white matter and has very little hypodense parenchyma around. If the ICH is large enough, it can exert mass effect on adjacent structures. Just like the HCCs, multiple ICHs worsen the prognosis of the patient.4,48,49
Vascular injuries (VI) are a group of traumatic lesions that cause both intra- and extra-axial bleeds. They are the result of interaction between bony ridges and vascular walls. The most vulnerable vessel is the internal carotid artery. The point where it enters the carotid canal and the point where it exits from the cavernous sinus are the sites where vascular injuries can happen. The VI can be pseudoaneurysm, arterial dissection or arteriovenous fistula. Fortunately for the paediatric patients, not many vascular injuries occur. According to a study published in 2007, the percentage of vascular injuries is small and more vascular injuries are caused by a penetrating injury than a blunt trauma.50 It has been concluded that there are less accidental vascular injuries on the internal and/or external carotid artery than other sites51 and accordingly the small percentage of such injuries has been confirmed.
Discussions
The images used to depict the lesions were obtained from patients who were brought to the emergency room of our hospital. Some CT scans revealed primary TBIs, others revealed both primary and secondary lesions. NECT is used for initial imaging, and resorting to different windowing and MPR reconstructions provides information on all the anatomical structures.4,52,53 Although we have seen an increase in the number of CT scans performed worldwide in head trauma during the last years, recent studies show that in low-risk patients it could be omitted, thus decreasing the exposure of children to ionizing radiation.16,54 Doctors should always be aware of the clinical state of the child when arriving at the hospital. If the caregiver mentions mild or moderate head trauma, but the Glasgow Coma score is low, acute cardiorespiratory compromise or prolonged intervals of impaired consciousness are also present, abusive head trauma should be taken into consideration.33 When vascular lesions are suspected, intravenous contrast media will be administered, and additional CT angiography data will complete the initial evaluation.52 Whether there are psychological or physical effects, trauma impacts all members of the family unit, not just the patient.55–57
Conclusion
Head trauma is still a big problem worldwide. Rapid and comprehensive assessment of the head injuries is crucial in managing each case because primary and secondary lesions can be life threatening. The database of our hospital does not include all the possible acute post-traumatic findings described above. Although our hospital is the only paediatric hospital on a 300 km area, there were no intracerebral hemorrhages or traumatic vascular injuries reported throughout the years. In severe head traumas there were different TBIs combined, but we chose only the ones which were singular. This is why we keep a close eye on all trauma cases so that lesions which are not common do not get overlooked. Injuries sustained after head trauma (be it isolated or part of a polytrauma) can have long-term effects on both the children and their families. This is valid for adults also, making head trauma a priority for researchers.
Abbreviations
CT, computer tomography; DAI, Diffuse axonal injury; EDH, Epidural haematoma; HU, Hounsfield units; ICH, Intracerebral haemorrhage; IVH, Intraventricular haematomas; HCC, Haemorrhagic cortical contusions; NECT, non enhanced computer tomography scans; TBI, Traumatic brain injury; tSAH, Traumatic subarachnoid haemorrhage; SDH, Subdural haematoma; VI, Vascular injuries.
Ethics Approval and Consent to Participate
The study was conducted in accordance with the Declaration of Helsinki, and the protocol was approved by the Ethics Committee of Clinical Emergency Hospital, Galati, Romania. (Project identification code: 4579/14.11.2023).
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors declare that they have no competing interests.
References
1. Al Mukhtar A, Bergenfeldt H, Edelhamre M, Vedin T, Larsson PA, Öberg S. The epidemiology of and management of pediatric patients with head trauma: a hospital-based study from Southern Sweden. Scand J Trauma Resusc Emerg Med. 2022;30(1):67. doi:10.1186/s13049-022-01055-9
2. Pinto PS, Poretti A, Meoded A, Tekes A, Huisman TA. The unique features of traumatic brain injury in children. Review of the characteristics of the pediatric skull and brain, mechanisms of trauma, patterns of injury, complications and their imaging findings--part 1. J Neuroimaging. 2012;22(2):e1–e17. doi:10.1111/j.1552-6569.2011.00688.x
3. Cremonini C, Lewis M, Wong MD, Benjamin ER, Inaba K, Demetriades D. Traumatic epidural hematomas in the pediatric population: clinical characteristics and diagnostic pitfalls. J Pediatr Surg. 2020;55(9):1773–1778. doi:10.1016/j.jpedsurg.2020.05.011
4. Mutch CA, Talbott JF, Gean A. Imaging Evaluation of Acute Traumatic Brain Injury. Neurosurg Clin N Am. 2016;27(4):409–439. doi:10.1016/j.nec.2016.05.011
5. Falconi S, Demopoulos A, Collins R, Garza J, Nagy L. Outcomes of Pediatric Traumatic Brain Injury Patients Presenting with or Developing Cerebral Herniation. World Neurosurg. 2023. doi:10.1016/j.wneu.2023.06.125
6. Gaulden AL, Trinidad S, Moody S, Kotagal M, Mangano FT, Patel SK. Utility of the material community deprivation index as a metric to identify at-risk children for severe traumatic brain injury. Neurosurg Focus. 2023;55(5):E8. doi:10.3171/2023.8.FOCUS23448
7. Kennedy L, Nuno M, Gurkoff GG, Nosova K, Zwienenberg M. Moderate and severe TBI in children and adolescents: the effects of age, sex, and injury severity on patient outcome 6 months after injury. Front Neurol. 2022;13:741717. doi:10.3389/fneur.2022.741717
8. Brazinova A, Rehorcikova V, Taylor MS, et al. Epidemiology of Traumatic Brain Injury in Europe: a Living Systematic Review. J Neurotrauma. 2021;38(10):1411–1440. doi:10.1089/neu.2015.4126
9. Derakhshanfar H, Pourbakhtyaran E, Rahimi S, Sayyah S, Soltantooyeh Z, Karbasian F. Clinical guidelines for traumatic brain injuries in children and boys. Eur J Transl Myol. 2020;30(1):8613. doi:10.4081/ejtm.2019.8613
10. Majdan M, Melichova J, Plancikova D, et al. Burden of Traumatic Brain Injuries in Children and Adolescents in Europe: hospital Discharges, Deaths and Years of Life Lost. Children. 2022;9(1):105. doi:10.3390/children9010105
11. El-Fiki M, El-Ghandour N. Traumatic subarachnoid hemorrhage in developed and developing communities. World Neurosurg. 2015;83(2):170–173. doi:10.1016/j.wneu.2014.11.012
12. Quach N, Do J, Dirlikov B, et al. The Prognosis of Axial vs. Extra-Axial Lesions on Functional Status After Traumatic Brain Injury. Front Neurol. 2019;10:1167. doi:10.3389/fneur.2019.01167
13. Vitali M, Marasco S, Romenskaya T, et al. Decompressive Craniectomy in Severe Traumatic Brain Injury: the Intensivist’s Point of View. Diseases. 2023;11(1):22. doi:10.3390/diseases11010022
14. Denniss RJ, Barker LA. Brain Trauma and the Secondary Cascade in Humans: review of the Potential Role of Vitamins in Reparative Processes and Functional Outcome. Behav Sci. 2023;13(5):388. doi:10.3390/bs13050388
15. Sarioglu FC, Sahin H, Pekcevik Y, Sarioglu O, Oztekin O. Pediatric head trauma: an extensive review on imaging requisites and unique imaging findings. Eur J Trauma Emerg Surg. 2018;44(3):351–368. doi:10.1007/s00068-017-0838-y
16. du Plessis J, Gounden SK, Lewis C. Paediatric minor head injury applied to Paediatric Emergency Care Applied Research Network CT recommendations: an audit. SA J Radiol. 2022;26(1):2289. doi:10.4102/sajr.v26i1.2289
17. Ruiz-Maldonado TM, Alsanea Y, Coats B. Age-related skull fracture patterns in infants after low-height falls. Pediatr Res. 2023;93(7):1990–1998. doi:10.1038/s41390-022-02345-9
18. Adetayo OA, Naran S, Bonfield CM, et al. Pediatric Cranial Vault Fractures: analysis of Demographics, Injury Patterns, and Factors Predictive of Mortality. J Craniofac Surg. 2015;26(6):1840–1846. doi:10.1097/SCS.0000000000001982
19. Kriss S, Morris J, Martich V. Pediatric Skull Fractures Contacting Sutures: relevance in Abusive Head Trauma. AJR Am J Roentgenol. 2021;217(1):218–222. doi:10.2214/AJR.20.23081
20. Kriss S, Morris J, Martich V. Cranial Suture Evaluation in Pediatric Head Trauma: importance in Differentiating Abusive from Accidental Injury. Pediatric Emerg Care. 2022;38(2):e703–e708. doi:10.1097/PEC.0000000000002461
21. Minghinelli FE, Marquez YB, Pipolo DO, Recalde RJ, Mantese B, Rugilo C. “Ping-pong” fracture: an exclusive entity of neonates and infants? A case analysis and literature review. Surg Neurol Int. 2023;14:170. doi:10.25259/SNI_211_2023
22. Harsh V, Vohra V, Kumar P, Kumar J, Sahay CB, Kumar A. Elevated Skull Fractures - Too Rare to Care for, Yet too Common to Ignore. Asian J Neurosurg. 2019;14(1):237–239. doi:10.4103/ajns.AJNS_242_17
23. Sobti S, Goyari M, Harpanahalli R, Gupta LN, Choudhary A, Taneja A. Clinico-radiological Correlation with Outcome in Traumatic Pediatric Extradural Hematoma: a Single Institutional Experience. J Pediatr Neurosci. 2021;16(2):113–118. doi:10.4103/jpn.JPN_61_20
24. Ali MFA, Elbaroody M, Alsawy MFM, El Fiki A, El Refaee E, Elshitany HA. Postoperative cerebral infarction after evacuation of traumatic epidural hematoma in children younger than two years: single-center experience. Surg Neurol Int. 2022;13:141. doi:10.25259/SNI_1247_2021
25. Caruso G, Fiore P, Gorgoglione ML, Ricciardo G, Caffo M. Unusual Case of Posterior Fossa Extradural Hematoma in a Child: review of the Literature. Pediatr Neurosurg. 2020;55(6):399–403. doi:10.1159/000511906
26. Jamous MA, Samara QA, Jbarah OF, Ahmed YB. Management of traumatic posterior fossa epidural hematomas in pediatrics: our experience and review of the literature. Childs Nerv Syst. 2021;37(9):2839–2846. doi:10.1007/s00381-021-05248-y
27. Gean AD, Fischbein NJ, Purcell DD, Aiken AH, Manley GT, Stiver SI. Benign anterior temporal epidural hematoma: indolent lesion with a characteristic CT imaging appearance after blunt head trauma. Radiology. 2010;257(1):212–218. doi:10.1148/radiol.10092075
28. Vega RA, Valadka AB. Natural History of Acute Subdural Hematoma. Neurosurg Clin N Am. 2017;28(2):247–255. doi:10.1016/j.nec.2016.11.007
29. Winkler J, Piedade GS, Rubbert C, Hofmann BB, Kamp MA, Slotty PJ. Cerebral perfusion changes in acute subdural hematoma. Acta Neurochir (Wien). 2023;165(9):2381–2387. doi:10.1007/s00701-023-05703-6
30. Feldman KW, Bethel R, Shugerman RP, Grossman DC, Grady MS, Ellenbogen RG. The cause of infant and toddler subdural hemorrhage: a prospective study. Pediatrics. 2001;108(3):636–646. doi:10.1542/peds.108.3.636
31. Orman G, Kralik SF, Meoded A, Desai N, Risen S, Huisman TAGM. MRI Findings in Pediatric Abusive Head Trauma: a Review. J Neuroimaging. 2020;30(1):15–27. doi:10.1111/jon.12670
32. Shekdar K. Imaging of Abusive Trauma. Indian J Pediatr. 2016;83(6):578–588. doi:10.1007/s12098-016-2043-0
33. Goldberg AP, Barron CE. Abusive Head Trauma: historical and Current Perspectives of a Complex Diagnosis. R I Med J. 2013;106(10):20–24.
34. Mamaril-Davis JC, Riordan K, Sumdani H, et al. Subdural hematoma, retinal hemorrhage, and fracture triad as a clinical predictor for the diagnosis of child abuse. J Neurosurg Pediatr. 2023;1:1–7. doi:10.3171/2023.11.PEDS23212
35. Jeon TY, Yoo SY, Eo H, Kim JH. [Diagnostic Imaging for Physical Abuse in Children]. Taehan Yongsang Uihakhoe Chi. 2020;81(4):832–851. doi:10.3348/jksr.2020.81.4.832 Korean.
36. Griswold DP, Fernandez L, Rubiano AM. Traumatic Subarachnoid Hemorrhage: a Scoping Review. J Neurotrauma. 2022;39(1–2):35–48. doi:10.1089/neu.2021.0007
37. Kakarieka A. Review on traumatic subarachnoid hemorrhage. Neurol Res. 1997;19(3):230–232. doi:10.1080/01616412.1997.11740804
38. Armin SS, Colohan AR, Zhang JH. Traumatic subarachnoid hemorrhage: our current understanding and its evolution over the past half century. Neurol Res. 2006;28(4):445–452. doi:10.1179/016164106X115053
39. Kim J, Lee SJ. Traumatic Subarachnoid Hemorrhage Resulting from Posterior Communicating Artery Rupture. Int Med Case Rep J. 2020;13:237–241. doi:10.2147/IMCRJ.S254160
40. Kim MS, Cho MJ, Kim JW, Jang SH. White Matter Abnormalities in Traumatic Subarachnoid Hemorrhage: a Tract-Based Spatial Statistics Study. Med Sci Monit. 2021;27:e933959. doi:10.12659/MSM.933959
41. El-Menyar A, Consunji R, Al-Thani H, Mekkodathil A, Jabbour G, Alyafei KA. Pediatric Traumatic Brain Injury: a 5-year descriptive study from the National Trauma Center in Qatar. World J Emerg Surg. 2017;12:48. doi:10.1186/s13017-017-0159-9
42. Egbohou P, Mouzou T, Tchetike P, et al. Epidemiology of Pediatric Traumatic Brain Injury at Sylvanus Olympio University Hospital of Lomé in Togo. Anesthesiol Res Pract. 2019;2019:4038319. doi:10.1155/2019/4038319
43. Ducrocq SC, Meyer PG, Orliaguet GA, et al. Epidemiology and early predictive factors of mortality and outcome in children with traumatic severe brain injury: experience of a French pediatric trauma center. Pediatr Crit Care Med. 2006;7(5):461–467.
44. Su E, Bell M. Diffuse Axonal Injury. In: Laskowitz D, Grant G, editors. Translational Research in Traumatic Brain Injury. Boca Raton (FL): CRC Press/Taylor and Francis Group; 2016.
45. Provenzale JM. Imaging of traumatic brain injury: a review of the recent medical literature. AJR Am J Roentgenol. 2010;194(1):16–19. doi:10.2214/AJR.09.3687
46. Ferguson NM, Rebsamen S, Field AS, et al. ADAPT MRI Investigators. Magnetic Resonance Imaging Findings in Infants with Severe Traumatic Brain Injury and Associations with Abusive Head Trauma. Children. 2022;9(7):1092. doi:10.3390/children9071092
47. Hershkovitz Y, Kessel B, Dubose JJ, et al.; Israeli Trauma Group. Is Diffuse Axonal Injury Different in Adults and Children? An Analysis of National Trauma Database. Pediatr Emerg Care. 2022;38(2):62–64. doi:10.1097/PEC.0000000000002626
48. Colquhoun IR, Rawlinson J. The significance of haematomas of the basal ganglia in closed head injury. Clin Radiol. 1989;40(6):619–621. doi:10.1016/s0009-9260(89)80324-1
49. Jayakumar PN, Kolluri VR, Basavakumar DG, Arya BY, Das BS. Prognosis in traumatic basal ganglia haematoma. Acta Neurochir (Wien). 1989;97(3–4):114–116. doi:10.1007/BF01772820
50. Klinkner DB, Arca MJ, Lewis BD, Oldham KT, Sato TT. Pediatric vascular injuries: patterns of injury, morbidity, and mortality. J Pediatr Surg. 2007;42(1):178–182. doi:10.1016/j.jpedsurg.2006.09.016
51. Allen CJ, Straker RJ, Tashiro J, et al. Pediatric vascular injury: experience of a level 1 trauma center. J Surg Res. 2015;196(1):1–7. doi:10.1016/j.jss.2015.02.023
52. Shih RY, Burns J, Ajam AA, et al.; Expert Panel on Neurological Imaging. ACR Appropriateness Criteria® Head Trauma: 2021 Update. J Am Coll Radiol. 2021;18(5S):S13–S36. doi:10.1016/j.jacr.2021.01.006
53. Wintermark M, Sanelli PC, Anzai Y, Tsiouris AJ, Whitlow CT. ACR Head Injury Institute; ACR Head Injury Institute. Imaging evidence and recommendations for traumatic brain injury: conventional neuroimaging techniques. J Am Coll Radiol. 2015;12(2):e1–14. doi:10.1016/j.jacr.2014.10.014
54. Çalik M, Ersoy AH, Ekin EE, Öztürk D, Güleç SG. Assessment of Cost-Effectiveness of Computerized Cranial Tomography in Children with Mild Head Trauma. Diagnostics (Basel). 2022;12(11):2649. doi:10.3390/diagnostics12112649
55. Anghele M, Marina V, Moscu CA, Dragomir L, Anghele AD, Lescai AM. Emotional Distress in a Patients Following Polytrauma. J Multidiscip Healthc. 2023;16:1161–1170.
56. Sinopidis X, Kallianezos P, Petropoulos C, et al. Post-Traumatic Stress as a Psychological Effect of Mild Head Injuries in Children. Children. 2023;10(7):1115. doi:10.3390/children10071115
57. Demers LA, Wright NM, Kopstick AJ, et al. Is Pediatric Intensive Care Trauma-Informed? A Review of Principles and Evidence. Children. 2022;9(10):1575. doi:10.3390/children9101575
 © 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.