Back to Journals » Journal of Multidisciplinary Healthcare » Volume 17
A Systematic Review of the Application of Artificial Intelligence in Nursing Care: Where are We, and What’s Next?
Authors Ruksakulpiwat S , Thorngthip S , Niyomyart A , Benjasirisan C , Phianhasin L , Aldossary H , Ahmed BH , Samai T
Received 16 January 2024
Accepted for publication 5 March 2024
Published 12 April 2024 Volume 2024:17 Pages 1603—1616
DOI https://doi.org/10.2147/JMDH.S459946
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Suebsarn Ruksakulpiwat,1 Sutthinee Thorngthip,2 Atsadaporn Niyomyart,3 Chitchanok Benjasirisan,1 Lalipat Phianhasin,1 Heba Aldossary,4 Bootan Hasan Ahmed,5 Thanistha Samai6
1Department of Medical Nursing, Faculty of Nursing, Mahidol University, Bangkok, Thailand; 2Department of Nursing Siriraj Hospital, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand; 3Ramathibodi School of Nursing, Faculty of Medicine Ramathibodi Hospital, Mahidol University, Bangkok, Thailand; 4Department of Nursing, Prince Sultan Military College of Health Sciences, Dammam, Saudi Arabia; 5Frances Payne Bolton School of Nursing, Case Western Reserve University, Cleveland, OH, USA; 6Department of Public Health Nursing, Faculty of Nursing, Mahidol University, Nakhon Pathom, Thailand
Correspondence: Suebsarn Ruksakulpiwat, Email [email protected]
Background: Integrating Artificial Intelligence (AI) into healthcare has transformed the landscape of patient care and healthcare delivery. Despite this, there remains a notable gap in the existing literature synthesizing the comprehensive understanding of AI’s utilization in nursing care.
Objective: This systematic review aims to synthesize the available evidence to comprehensively understand the application of AI in nursing care.
Methods: Studies published between January 2019 and December 2023, identified through CINAHL Plus with Full Text, Web of Science, PubMed, and Medline, were included in this review. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines guided the identification, screening, exclusion, and inclusion of articles. The convergent integrated analysis framework, as proposed by the Joanna Briggs Institute, was employed to synthesize data from the included studies for theme generation.
Results: A total of 337 records were identified from databases. Among them, 35 duplicates were removed, and 302 records underwent eligibility screening. After applying inclusion and exclusion criteria, eleven studies were deemed eligible and included in this review. Through data synthesis of these studies, six themes pertaining to the use of AI in nursing care were identified: 1) Risk Identification, 2) Health Assessment, 3) Patient Classification, 4) Research Development, 5) Improved Care Delivery and Medical Records, and 6) Developing a Nursing Care Plan.
Conclusion: This systematic review contributes valuable insights into the multifaceted applications of AI in nursing care. Through the synthesis of data from the included studies, six distinct themes emerged. These findings not only consolidate the current knowledge base but also underscore the diverse ways in which AI is shaping and improving nursing care practices.
Keywords: artificial intelligence, nursing care, patient care, systematic review
Background
Artificial intelligence, commonly referred to as AI, is a field within computer science dedicated to the development of intelligent machines capable of emulating human thought processes and actions.1 The decision-making process in AI involves learning from the environment and the information it gathers.2 AI encompasses different types, among them machine learning (ML)—an algorithm that learns from data to make predictions.3 Another category is Natural Language Processing (NLP), which utilizes algorithms to comprehend and generate human-like conversations.4 In recent times, AI has found application in diverse areas, including medical diagnosis,5 the Internet of Things (IoT),6 and artificial intelligence of things.6 Moreover, AI integration into healthcare, marked by substantial progress in the past decade, has changed the landscape of patient care and healthcare delivery. ML algorithms, NLP, and predictive analytics have become indispensable tools, empowering healthcare professionals to extract actionable insights from vast datasets.7–9 This data-driven approach expedites decision-making processes and fosters a nuanced understanding of patient needs and medical conditions. A recent systematic review examined the existing evidence regarding the utilization of the Generative Pre-trained Transformer (ChatGPT), an NLP system, in medical research.10 The applications explored encompassed a wide range, including but not limited to treatment, diagnosis, and medication provision. The review revealed that ChatGPT has been employed in drug development, enhancing medical reports, offering treatment and medical information, composing literature reviews on health-related subjects, refining research methodologies, conducting data analysis, and personalizing medicine. However, the review emphasizes the need for in-depth discussions and improvements in areas such as accuracy, originality, academic integrity, and ethical considerations before considering widespread implementation of ChatGPT in clinical research and medical practice.10
Within the transformative wave, nursing care has emerged as a critical domain for AI integration, given nurses’ pivotal role as frontline healthcare providers.11,12 The relevance of AI in nursing care extends beyond automation, encompassing the augmentation of nursing capabilities through technologies capable of analyzing complex datasets, predicting patient needs, and aiding in clinical decision-making.11 As technological advancements continue to shape nursing care, the potential impact on patient outcomes becomes increasingly significant.13 AI-driven systems offer real-time monitoring of vital signs, early detection of deteriorating conditions, and the development of personalized care plans tailored to individual patient needs.13,14 This not only enhances the quality of care nurses provide but also contributes to timely interventions, thereby reducing the likelihood of adverse events and complications. The significance of this study lies in its capacity to systematically synthesize existing evidence, providing a comprehensive understanding of the implications of AI in nursing care. By addressing both the positive outcomes and potential challenges associated with AI integration, this research aims to inform evidence-based practices, guide policy decisions, and contribute to the ongoing discourse on optimizing the use of AI technologies in nursing care. Ultimately, this study seeks to bridge the gap between technological innovation and the frontline of healthcare, fostering a more informed and effective integration of AI in nursing care for the benefit of patients and healthcare professionals alike.
Objective
To synthesize the available evidence to comprehensively understand the application of AI in nursing care.
Methods
Identify Relevant Studies
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines15 were employed to direct the identification, screening, exclusion, and inclusion of articles in this review. In December 2023, searches were conducted on four electronic databases—CINAHL Plus with Full Text, Web of Science, PubMed, and Medline—to locate articles published between 2019 and 2023 that pertaining to or aiming to determine the use of AI in nursing care. The inclusion of articles published within the last five years is warranted to capture the most recent and impactful contributions within the rapidly evolving landscape of AI. The search terms (Artificial Intelligence OR Computational Intelligence OR Machine Intelligence OR Computer Reasoning OR AI OR Computer Vision System* OR Knowledge Acquisition OR Knowledge Representation* OR Machine Learning OR Transfer Learning OR Learning, Machine OR Transfer Learning OR Learning, Transfer OR Deep Learning OR Hierarchical Learning OR Supervised Machine Learning OR Semi-supervised Learning OR Inductive Machine Learning OR Active Machine Learning OR Machine Learning with a Teacher OR Learning from Labeled Data OR Unsupervised Machine Learning) AND (Nursing Care OR Nursing Care Management OR Nonprofessional Home Care OR Home Nursing OR Respite Care* OR In-Home Respite Care* OR In-Home Respite OR Primary Care Nursing) were utilized for this purpose. Additionally, the reference lists of the included studies were manually scrutinized to identify pertinent research, and all references were cataloged in EndNote. A flow diagram, in accordance with the PRISMA guidelines, was generated to visually represent the outcomes of the search and screening process.
Study Selection
The authors conducted an independent screening of the titles and abstracts of the identified studies to assess their relevance. Subsequently, the full text of the selected articles was also examined to verify compliance with the inclusion criteria. These criteria were applied rigorously to ensure that only studies aligned with the review’s objective were included. Likewise, exclusion criteria were employed to eliminate literature unrelated to the scope of the review (Table 1).
 |
Table 1 Inclusion and Exclusion Criteria |
Data Extraction
The standardized chart for data extraction consisted of the following data for each study: reference, year, country, study design, sample size, focus population, age, objective, AI included in the study, nursing care involved, results, AI in nursing care (theme), suggestions for future research.
Data Synthesis
In this review, the convergent integrated analysis framework proposed by the Joanna Briggs Institute (JBI) for systematic reviews was employed to synthesize the data from the included studies.16 During the data synthesis process, themes related to AI in nursing care will be derived from the key findings of the included studies, with an examination of the similarities and differences between the main findings. Additionally, if necessary, sub-themes will be abstracted to address more specific aspects of the corresponding findings, akin to the approach used by qualitative researchers in theme development.16
Results
Search Results
A total of 337 records were identified from CINAHL Plus with Full Text (N = 179), Web of Science (N = 64), PubMed and Medline with full text (N = 94). No additional records were identified through other resources. Results with abstracts were subsequently exported into Endnote. Out of the 337 articles, 35 duplicates were removed, and 302 records were screened for eligibility. After applying the inclusion and exclusion criteria, 280 articles were excluded as they were irrelevant to the topic of interest, leaving 22 articles eligible for full-text screening. Subsequently, 11 articles were excluded for the following reasons: review article (N = 3), editorial (N = 3), letter to editor (N = 1), non-English article (N = 1), not included AI in nursing care (N = 2), and retraced article (N = 1). Finally, 11 studies were included in this review (Figure 1).
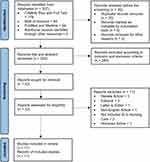 |
Figure 1 Flow Chart Diagram. Adapted from Page MJ, McKenzie JE, Bossuyt PM, Boutron I, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. Creative Commons.15 |
Characteristics of Included Studies
Characteristics of the included studies are presented in Table 2. The majority of these studies were published in 2023 (N = 4, 36.36%) and 2019 (N = 3, 27.27%), with the primary locations being the United States (N = 6, 54.54%) and China (N = 3, 27.27%). The study designs were diverse; three studies (27.27%) were retrospective, and two studies (18.18%) focused on tool development. Other designs included cross-sectional, discussion papers, multiple case studies, exploratory studies, commentary, and methodology research, each accounting for 9.09%. The sample sizes varied, ranging from 1 to 1000 (N = 2, 18.18%), between 1000 and 5000 (N = 4, 36.36%), and more than 5000 (N = 1, 9.09%). The focus population across the included studies was diverse, with the majority (N = 4, 36.26%) concentrating on the adult population with different conditions. The AI algorithms employed in these studies varied based on the research objectives. The top three AI methods were Classification and Regression Tree (CART) (N = 2, 15.38%), Deep Learning (N = 2, 15.38%), and Unsupervised Classification (N = 2, 15.38%).
 |
Table 2 Characteristics of Included Studies |
AI in Nursing Care
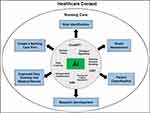
A summary of the findings related to AI in nursing care themes, as per data synthesis, is provided in Table 3. Scrutiny of Table 3 reveals six major themes: 1) Risk Identification, 2) Health Assessment, 3) Patient Classification, 4) Research Development, 5) Improved Care Delivery and Medical Record, and 6) Developing a Nursing Care Plan. A model summary of AI in nursing care in the healthcare context based on data synthesis is shown in Figure 2. Details of each included study can be found in Supplementary Table 1.
 |
Table 3 Artificial Intelligence in Nursing Care Themes |
Risk Identification
Five included studies reveal that nurses implemented AI for patient risk identification.17,21,23,26,27 For instance, a retrospective study by Brom et al utilized CART analysis and electronic health record (EHR) data to identify the risk of readmission in adult patients discharged from medical services. The results showed a 30-day readmission rate of 11.2%, and CART analysis revealed the highest risk for readmission among patients who visited the emergency department, had ≥ 9 comorbidities, were insured through Medicaid, and were ≥ 65 years old.17
Another example from the study by Kwon et al included patients with a primary diagnosis of diabetes and aimed to demonstrate how ML techniques (Regularized Logistic Regression, Random Forest, Extreme Gradient Boosting) could support nursing work.26 The study discussed how nurses can contribute to improving the relevance and performance of these techniques, highlighting the most significant predictors of readmission. The results identified the top two significant predictors of readmission in patients with diabetes as the primary diagnosis: the number of inpatient visits in the previous year and discharge disposition. Moreover, the authors suggested that nurses can enhance machine learning algorithms by 1) filling data gaps with nursing-relevant information that provides personalized context about the patient, 2) improving data preprocessing techniques, and 3) evaluating potential value in practice.26
Health Assessment
Health assessment is another theme emerging from the synthesis of included studies. The multiple-case study by Jain et al involved 1048 patients with different skin conditions and aimed to evaluate an AI-based tool (deep learning) that assists nurse practitioners in the assessment of dermatologic conditions.19 The results demonstrated that the developed deep learning algorithm was significantly associated with a higher agreement with diagnoses made by a dermatologist panel. There was an increase from 48% to 58% for primary care physicians and an increase from 46% to 58% for nurse practitioners.19
Patients Classification
A cross-sectional study conducted by An et al yielded results supporting the theme of patient classification.24 This study involved 300 adult patients admitted to the intensive care unit, with the aim of developing a patient classification system that stratifies patients based on their disease severity and care needs. The researchers employed unsupervised classification methods, specifically clustering, to help nurse managers identify homogeneous patient groups and enhance the management of critically ill patients. The results revealed that cluster analysis identified three sub-groups of critically ill patients with different levels of clinical trajectories. These subgroups demonstrated significant differences in disease severity and nursing workload. The predicted value ranges of the regression model for Classes A, B, and C were < 1.44, 1.44–2.03, and > 2.03, respectively, and the model demonstrated a good fit and satisfactory prediction efficiency, as confirmed by 200 permutation tests.24
Research Development
Nurses utilized AI for research development, as evidenced by the methodological research conducted by Fritz & Dermody (2019). This study focused on older adults with chronic illnesses and provided practical guidance to nurse investigators interested in multidisciplinary research, including the development of AI algorithms for “smart” health management and aging-in-place.25 The authors proposed a practical framework to guide nurse investigators in integrating clinical data with sensor data for training ML algorithms, potentially enhancing the capacity of nurses to make significant contributions to the development of AI for healthcare-assistive smart homes. Furthermore, the researchers recommended 1) employing a practical and consistent method for collecting field data, 2) utilizing nurse-driven measures for data analytics, and 3) facilitating multidisciplinary communication on an engineering-preferred platform.25
Improved Care Delivery and Medical Record
The utilization of AI to improve care delivery and medical records is highlighted in the publication by Pailaha (2023). The study explores and discusses the impact of applying AI in nursing science and the healthcare system to approximate nursing care. The main findings suggest that the current evaluation of AI technology systems in nursing and healthcare reveals several notable impacts, including expanded access to quality medical care, enhancements in medical record management, and overall improvements in service quality. These positive effects underscore the advantages and the pressing need for integrating AI technology systems in healthcare, with the aim of optimizing healthcare services for greater efficiency and effectiveness.22
Developing a Nursing Care Plan
Four included studies demonstrate the utilization of AI by nurses to assist in developing nursing care plans.18,20,21,27 In a discussion paper by Woodnutt et al, ChatGPT was employed to generate a mental health nursing care plan, and its output quality was evaluated against the authors’ clinical experience and existing guidance. The findings indicated that ChatGPT provided a care plan incorporating some principles of dialectical behavior therapy. However, the output exhibited significant errors and limitations.18
Another study by Li et al focused on tool development, utilizing support vector machines (SVM) to construct an intelligent wearable device system and prediction module for predicting stroke patients’ care needs, such as physical function, pain, and medication adherence. The results suggested that the application of wearable devices can enhance the recovery of a patient’s physiological functions, alleviate body pain, and increase vitality. By improving patient health indicators, wearable devices enable patients to determine when, how long, and how often to exercise, thereby fostering healthy behaviors and habits. Additionally, reminders for medication times through wearable smart devices can help patients intuitively recognize the importance of adhering to a regular medication schedule.20
Discussion
The integration of AI into nursing practices for risk identification presents a transformative opportunity to enhance patient outcomes.17,21,23,26,27 The studies highlighted not only illustrate the diverse applications of AI and ML, encompassing the prediction of readmission risks and facilitating the management of chronic conditions but also emphasize the precision achieved through the identification of key risk factors. This precision enables targeted interventions, potentially leading to a reduction in healthcare costs and an overall improvement in patient care quality. These findings align with other research endeavors within the healthcare domain that leverage ML. Studies such as those conducted by Li et al,28 Zhong et al,29 and Guo et al30 delve into candidate selection processes, evaluating patients’ physical and mental readiness for procedures to prevent risk of complications. Additionally, investigations by Labott et al31 focus on predicting unplanned hospitalizations post-discharge, while Wei et al32 contribute insights into discharge predictions based on significant predictor variables, including identifying factors associated with “unsafe” procedures and management. These findings underscore the transformative impact of integrating AI and ML in healthcare. This advancement alleviates burdens on healthcare professionals, enhancing accuracy and predictive capabilities.33 ML’s influence is evident in fostering swift, efficient, and cost-effective decision-making.34 This technological evolution not only signifies a paradigm shift in healthcare practices but also positions AI and ML as pivotal contributors to the evolution of modern healthcare, promising a future characterized by heightened efficiency, improved patient outcomes, and sustainable healthcare solutions.
Moving forward, advancing AI applications in nursing requires interdisciplinary collaboration to fully harness their potential in enhancing patient care. Given nurses’ involvement throughout the patient care continuum — collaborating across disciplines from admission to discharge35– it is imperative to value nursing perceptions and insights. The integration of AI should extend beyond nursing to include diverse fields such as other healthcare professionals, data scientists, informatics, and healthcare administration. This collaborative, multidisciplinary approach ensures a comprehensive understanding of patient needs, aligning AI solutions with the practical intricacies of healthcare delivery. It is a crucial factor for the successful implementation of AI, enhancing adaptability and efficiency in real-world healthcare scenarios by merging clinical expertise with technological innovation. Nevertheless, it’s crucial to clarify that the integration of AI and ML does not imply a substitution for the role of healthcare professionals. Rather, these technologies are poised to function as valuable assistants and reliable aides, serving to complement the expertise of healthcare professionals by mitigating the risk of errors and addressing areas that might be overlooked. This collaborative approach harnesses the strengths of both human professionals and advanced technologies, fostering a synergy that holds the potential to significantly enhance overall healthcare quality and efficiency.
It is important to acknowledge the positive impact on diagnostic agreement, particularly for nurse practitioners who play a crucial role in primary care settings. The study result from Jain et al19 signifies the potential of AI as a valuable supportive tool for nursing professionals, facilitating more accurate and timely assessments. This showcases how AI technologies can be integrated into nursing practice, particularly in nurse practitioner, to augment diagnostic capabilities. To emphasize again, embracing AI in health assessment does not diminish the role of nurse practitioners but rather empowers them with enhanced diagnostic support.
While the study primarily focuses on dermatologic assessments, the success observed in this context prompts further exploration into diverse areas of health assessment where AI could enhance diagnostic precision. This extension particularly applies to health assessment and screening beyond dermatology. Currently, AI integration in health assessment predominantly revolves around diagnostic methods and screening tools. Examples include thyroid pathology diagnosis Dov et al,36 depression screening Nickson et al,37 ADHD diagnosis Goh et al,38 and osteoporosis and osteopenia screening Sebro & Elmahdy.39 These studies demonstrate promising results, indicating that the incorporation of AI in diagnostic and screening methods holds significant potential, effectively reducing the workloads of healthcare professionals while maintaining effectiveness and efficiency. However, there is a gap in the literature concerning the application of AI in nursing assessment. This represents an opportunity for future nursing research to delve into the integration of AI to support various aspects of nursing assessment and diagnosis. Potential areas of exploration may include leveraging AI to assist nurses in evaluating pressure injuries among in-patients, assessing nutrition needs, gauging the risk of impaired respiratory function, and identifying potential fall risks. By addressing this research gap, we can unlock innovative approaches to enhance the precision and efficiency of nursing assessments, ultimately contributing to improved patient care and outcomes.
The findings of An et al indicate that ML can help develop a Patient Classification System (PCS) and identify three clinically relevant subgroups; however, the findings reveal that the severity of illness of adult ICU patients does not always correlate with the intensity of nursing.24 Our results were consistent with a recent meta-analysis and literature review, which compared the severity of illness scores with AI models for predicting ICU patients’ severity, the results demonstrated that patient classifications are important in guiding organizational resource planning.40 In contrast, another recent study found that AI could be used as a tool for clinicians, patients, and the healthcare system to detect disease, predict outcomes, plan treatment, and forecast outcomes.41 Even though AI has been used for a variety of purposes, it is becoming a potential tool in the healthcare field and is increasingly used for decision-making and judgment; further, it has the potential to revolutionize the way clinicians practice medicine by transforming their roles and revolutionizing the way medical professionals make decisions.42 Incorporating AI into healthcare is therefore necessary as it can help make critical decisions and classify patients, thus improving patient safety.43
Based on Fritz and Dermody’s (2019)25 findings, nurse researchers and engineers can collaborate on the development and training of AI-based technologies, for example, smart homes can be used to assess the normal movement patterns of older adults and facilitate interventions based on abnormal patterns. The results of our study were in line with those of studies that used technology to support older adults over 65 and older adults with cognitive impairment living in the community; these studies examined whether AI could facilitate independent living by monitoring the Activities of Daily Living (ADL) and detecting residents’ presence.44,45 Along with AI smart homes, AI has brought about significant changes to nursing research to enhance the quality of nursing care. An example of how AI is transforming healthcare and nursing research is the integration of AI to predict falls among elderly inpatients, predict ICU transfers within 24 hours in hospitalized COVID-19 patients and flow of operation, and use ML to identify nursing home residents’ pressure ulcer risk factors.46–48 With AI-driven technologies, nurse researchers can, therefore, analyze a vast amount of data quickly and efficiently to identify patterns, correlations, and trends that may not be easily detected through traditional methods. As AI has been used in nursing research to sort big data and extract relevant information from a wide range of resources, ethical issues related to data bias and appropriate training in AI technology are the next important steps to be considered in the research development.
AI and ML have made a significant contribution to the patient journey from home to hospital discharge. They have been integrated into the healthcare delivery system to help organize people, institutions, and resources to provide high-quality healthcare services that meet the needs of a specific population.49,50 The review results showed that AI could be incorporated into EHR in terms of recording, organizing, and managing EHR data for optimal use, reducing time and effort, and increasing the quality of care.22 For instance, one of the examples was the implementation of a voice-based AI system that provided real-time assistance for medical record input during the triage process in the emergency department. This system was trained on speech-to-text data and could reduce the triage time and improve the efficiency of emergency care.51 Another example was the utilization of a natural language processing-bidirectional recurrent neural network (NLP-BIRNN) algorithm for selecting the appropriate ICD codes for medical records.52 This algorithm could facilitate the EHR recording process and save time compared to the manual method. However, the accuracy and specificity of the AI-generated triage notes and ICD codes were still lower than the human-generated ones, which suggested the need for further improvement of the AI tools in EHR systems.51,52 Moreover, the use of AI could also assist in organizing EHR data according to a standardized format and selecting relevant features for EHR analysis for each stakeholder.53 This could support healthcare providers in making informed decisions and enhancing the quality of care in terms of efficiency, safety, and access to healthcare through collaboration, coordination, and communication among different healthcare disciplines.
Nevertheless, there were also some challenges and limitations associated with the use of AI in EHR systems. One of the major concerns was the possibility of introducing human bias or social bias into the AI products, as the training data might not be free from such biases.54 Therefore, it was essential to ensure the fairness and transparency of the AI algorithms and to avoid any potential discrimination or harm to patients or healthcare professionals. Another challenge was to validate and verify the reliability and validity of the classification algorithms used for health-related decision-making, as they could have significant implications for patient safety and clinical outcomes.55 Furthermore, one of the potential implications of replacing aspects of human expertise with autonomous AI system technology was the legal implications of clinical accountability.56 It was unclear who would be responsible for any errors or adverse events caused by the AI systems and how to establish a clear framework for liability and regulation.
AI aids in developing a nursing care plan in both direct and indirect methods. For the direct method, our findings showed that AI helped develop a mental health nursing care plan by incorporating principles of dialectical behavior therapy but exhibited significant errors and limitations.18 In a study of competencies for the use of AI-based tools by healthcare professionals, 15 experts in the use of AI-based tools in healthcare settings reported that AI integrated diverse sources of information in developing patient-centered care plans.57 However, the study did not mention errors or limitations in the utilization of AI in clinical settings.
In terms of the indirect method, AI helps to track patients’ symptoms and activities, which leads to symptom prediction and an optimized plan of care. One of the included studies reported that the application of wearable devices can enhance recovery among patients with stroke.20 The result findings are congruent with a study of symptom tracking in endometriosis using digital technologies, which aims to discuss how digital technologies may be used in endometriosis to facilitate symptom tracking.58 The study suggested that objective measures extracted from wearable devices can be integrated with self-reported symptom measures to provide insight into symptom trajectories and the association between objective behaviors and subjective symptoms.58 In addition, a study of AI aiding in diagnosing and tracking the recovery of COVID-19 using deep learning on chest Computed Tomography (CT) scans reported that AI aided in tracking how patient conditions change through quantitative analysis of CT features, which is difficult to ascertain manually by radiologists to go through multiple slices of the CT scan.59 With the benefit of data analysis and tracking by AI, it helps nurses develop better nursing plans of care for better patient outcomes and quality of life.
The systematic review has certain limitations that should be noted. Firstly, the inclusion criteria requiring studies to be in English acted as a limiting factor. As a result, qualified studies reported in other languages may have been omitted, potentially leading to a language bias in the review. Secondly, each of the included studies featured different sample sizes, study designs, focus populations, and AI algorithms. These variations were present in studies conducted in different countries. This diversity may have introduced heterogeneity, which could account for the differences observed in the study outcomes. Lastly, this review presents a limited view of AI in healthcare fields, crucially outside nursing and healthcare, given the fact that this systematic review only focuses on synthesizing the available evidence to understand the application of AI in nursing care. This limitation restricts the generalizability of our results.
Future Direction of Nursing Care
The rapid expansion of AI marks a critical turning point for the nursing profession. Even though AI has the potential to transform how patients experience healthcare, successfully handling this shift needs a clear vision for the future of the profession. This perspective is not about AI taking the place of nurses; instead, it’s about a working partnership where AI helps nurses provide personalized, ethical, and caring healthcare. At the heart of this partnership will be nurses’ active involvement in shaping how AI is developed and used. Their deep understanding of patients, the context of care, and their clinical instincts will be essential in making sure AI algorithms are focused on what truly matters to patients. Encouraging a culture of innovation within the nursing field, equipping nurses with the skills to understand and use AI effectively, and setting up strong feedback channels will be crucial steps in achieving this powerful collaboration. One of the most promising applications of AI in nursing is its ability to personalize care plans. By integrating AI-powered tools that predict potential problems and suggest best practices, nurses can tailor their interventions to each patient’s specific needs, making treatment more effective and using resources efficiently. This personalized approach sees AI as a tool that helps nurses do their jobs better, not as a replacement, allowing them to provide more holistic and effective care while maintaining their irreplaceable role in making decisions and advocating for patients. However, as AI becomes more common in nursing, we must pay close attention to ethical concerns. Nurses must be vigilant in addressing issues like protecting patient privacy, preventing bias in AI algorithms, and making sure decisions are always transparent. Building trust and confidence requires strong ethical frameworks that ensure fairness, accountability, and human oversight in AI applications. Open communication and transparency about how AI are used will empower patients and make sure their care aligns with their values and preferences. Continuous learning and adaptability will be another key feature of nursing in the AI era. Nursing education will need to integrate AI literacy into its curriculum, equipping nurses with the skills to leverage AI effectively while maintaining their critical thinking and clinical judgment. This ongoing learning process will ensure nurses remain competent and confident partners in an AI-powered healthcare ecosystem. Finally, while AI has the potential to automate administrative tasks and free up nurses’ time for patient interaction, it should never come at the expense of the human connection that is central to compassionate care. AI tools should be designed and implemented with the needs of both nurses and patients in mind, seamlessly integrating into existing workflows without compromising the human connection that remains irreplaceable in healthcare delivery.
Conclusion
The systematic review contributes to our understanding of the multifaceted implications of AI in nursing care. It sheds light on potential avenues for future research, such as utilizing AI for the early identification of patients at high risk of readmission, patient classification, improving care delivery and medical records, and developing nursing care plans. These findings not only consolidate the current knowledge base but also underscore the diverse ways in which AI is shaping and improving nursing care practices.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors. Mahidol University, Thailand, supported the Article Processing Charge.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Deng J, Lin Y. The benefits and challenges of ChatGPT: an overview. Front Comput Intell Sys. 2022;2(2):81–83.
2. Wu J, Shang S. Managing uncertainty in AI-enabled decision making and achieving sustainability. Sustainability. 2020;12(21):8758.
3. Sarker IH. Machine Learning: algorithms, Real-World Applications and Research Directions. SN Comput Sci. 2021;2(3):160. doi:10.1007/s42979-021-00592-x
4. Pruneski JA, Pareek A, Nwachukwu BU, et al. Natural language processing: using artificial intelligence to understand human language in orthopedics. Knee Surg Sports Traumatol Arthrosc. 2023;31(4):1203–1211. doi:10.1007/s00167-022-07272-0
5. Bitkina OV, Park J, Kim HK. Application of artificial intelligence in medical technologies: a systematic review of main trends. Digit Health. 2023;9:20552076231189331. doi:10.1177/20552076231189331
6. Chang H, Choi JY, Shim J, Kim M, Choi M. Benefits of information technology in healthcare: artificial intelligence, internet of things, and personal health records. Healthcare Informatics Research. 2023;29(4):323–333. doi:10.4258/hir.2023.29.4.323
7. Alowais SA, Alghamdi SS, Alsuhebany N, et al. Revolutionizing healthcare: the role of artificial intelligence in clinical practice. BMC Med Educ. 2023;23(1):689. doi:10.1186/s12909-023-04698-z
8. Razzak MI, Imran M, Xu G. Big data analytics for preventive medicine. Neural Comput Appl. 2020;32(9):4417–4451. doi:10.1007/s00521-019-04095-y
9. Ruksakulpiwat S, Thongking W, Zhou W, et al. Machine learning-based patient classification system for adults with stroke: a systematic review. Chronic Illness. 2021;19(1):26–39. doi:10.1177/17423953211067435
10. Ruksakulpiwat S, Kumar A, Ajibade A. Using ChatGPT in medical research: current status and future directions. J Multidiscipl Healthc. 2023;2:1513–1520.
11. Seibert K, Domhoff D, Bruch D, et al. Application scenarios for artificial intelligence in nursing care: rapid review. J Med Int Res. 2021;23(11):e26522. doi:10.2196/26522
12. Hassmiller SB, Wakefield MK. The future of nursing 2020–2030: charting a path to achieve health equity. Nurs Outlook. 2022;70:6.
13. Pepito JA, Locsin R. Can nurses remain relevant in a technologically advanced future? Int J Nurs Sci. 2019;6(1):106–110. doi:10.1016/j.ijnss.2018.09.013
14. Al Kuwaiti A, Nazer K, Al-Reedy A, et al. A review of the role of artificial intelligence in healthcare. J Pers Med. 2023;13:6.
15. Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. doi:10.1136/bmj.n71
16. Moola S, Munn Z, Tufanaru C, et al. Chapter 7: systematic reviews of etiology and risk. Joan Brig Instit Rev. 2017;5:3.
17. Brom H, Carthon MB, Ikeaba U, Chittams J. Applying machine learning to identify patients at high risk for readmissions: an innovative approach to target nursing care. Nurs Res. 2019;68:2.
18. Woodnutt S, Allen C, Snowden J, et al. Could artificial intelligence write mental health nursing care plans? J Psychiatr Ment Health Nurs. 2023. doi:10.1111/jpm.12965
19. Jain A, Way D, Gupta V, et al. Development and assessment of an artificial intelligence-based tool for skin condition diagnosis by primary care physicians and nurse practitioners in teledermatology practices. JAMA network open. 2021;4(4):e217249. doi:10.1001/jamanetworkopen.2021.7249
20. Li F, Tao Z, Li R, Qu Z. The early warning research on nursing care of stroke patients with intelligent wearable devices under COVID-19. Pers Ubiquitous Comput. 2023;27(3):767–779. doi:10.1007/s00779-021-01520-9
21. Hewner S, Smith E, Sullivan SS. Identifying high-need primary care patients using nursing knowledge and machine learning methods. Appl Clin Inform. 2023;14(03):408–417. doi:10.1055/a-2048-7343
22. Pailaha AD. The impact and issues of artificial intelligence in nursing science and healthcare settings. SAGE Open Nurs. 2023;9:23779608231196847. doi:10.1177/23779608231196847
23. Brom H, Carthon JMB, Ikeaba U, Chittams J. Leveraging electronic health records and machine learning to tailor nursing care for patients at high risk for readmissions. J Nurs Care Qual. 2020;35(1):27–33. doi:10.1097/ncq.0000000000000412
24. An R, Chang GM, Fan YY, Ji LL, Wang XH, Hong S. Machine learning-based patient classification system for adult patients in intensive care units: a cross-sectional study. J Nurs Manag. 2021;29(6):1752–1762. doi:10.1111/jonm.13284
25. Fritz RL, Dermody G. A nurse-driven method for developing artificial intelligence in ”smart” homes for aging-in-place. Nurs Outlook. 2019;67(2):140–153. doi:10.1016/j.outlook.2018.11.004
26. Kwon JY, Karim ME, Topaz M, Currie LM. Nurses “seeing forest for the trees” in the age of machine learning: using nursing knowledge to improve relevance and performance. Comput Inform Nurs. 2019;37(4):203–212. doi:10.1097/CIN.0000000000000508
27. Xu CM, Gao Y, Qi L, et al. Research and application of artificial intelligence and computer big data technology in the. Individ Nurs Care Platform. 2022;3:421–425.
28. Li Q, Zhong H, Girardi FP, et al. Machine learning approaches to define candidates for ambulatory single level laminectomy surgery. Glob Spine J. 2022;12(7):1363–1368.
29. Zhong H, Poeran J, Gu A, et al. Machine learning approaches in predicting ambulatory same day discharge patients after total Hip arthroplasty. Reg Anesth Pain Med. 2021;3:1.
30. Guo J, He Q, Peng C, et al. Machine learning algorithms to predict risk of postoperative pneumonia in elderly with Hip fracture. J Orthopaedic Surg Res. 2023;18(1):571.
31. Labott JR, Lu Y, Salmons HI, Camp CL, Wyles CC, Taunton MJ. Health and socioeconomic risk factors for unplanned hospitalization following ambulatory unicompartmental knee arthroplasty: development of a patient selection tool using machine learning. J Arthroplast. 2023;2:1.
32. Wei C, Quan T, Wang KY, et al. Artificial neural network prediction of same-day discharge following primary total knee arthroplasty based on preoperative and intraoperative variables. Bone Joint J. 2021;103(8):1358–1366.
33. Habehh H, Gohel S. Machine learning in healthcare. Curr Geno. 2021;22(4):291.
34. Jayatilake SMDAC, Ganegoda GU. Involvement of machine learning tools in healthcare decision making. J Healthc Engin. 2021;2021:1.
35. Harper MG, Maloney P. Nursing Professional Development: Standards of Practice. Chicago, IL: Association of Nursing Professional Development; 2016.
36. Dov D, Kovalsky SZ, Feng Q, et al. Use of machine learning–based software for the screening of thyroid cytopathology whole slide images. Arch Pathol Lab Med. 2022;146(7):872–878.
37. Nickson D, Meyer C, Walasek L, Toro C. Prediction and diagnosis of depression using machine learning with electronic health records data: a systematic review. BMC Med Inf Decis Making. 2023;23(1):271.
38. Goh PK, Elkins AR, Bansal PS, Eng AG, Martel MM. Data-driven methods for predicting ADHD diagnosis and related impairment: the potential of a machine learning approach. Res Child Adole Psychopathol. 2023;2:1–13.
39. Sebro R, Elmahdy M. Machine learning for opportunistic screening for osteoporosis and osteopenia using knee CT scans. Canad Associat Radiol J. 2023;3:08465371231164743.
40. Barboi C, Tzavelis A, Muhammad LN. Comparison of severity of illness scores and artificial intelligence models that are predictive of intensive care unit mortality: meta-analysis and review of the literature. JMIR Med Inform. 2022;10(5):e35293. doi:10.2196/35293
41. Poalelungi DG, Musat CL, Fulga A, et al. Advancing patient care: how artificial intelligence is transforming healthcare. J Personal Med. 2023;13(8):1214.
42. Selten FR. Marcel; Grimmelikhuijsen, Stephan ‘Just like I thought’: street-level bureaucrats trust AI recommendations if they confirm their professional judgment. Public Administration Rev. 2023;82(2):263–274. doi:10.1111/puar.13602
43. Choudhury A, Asan O. Role of artificial intelligence in patient safety outcomes: systematic literature review. JMIR Med Inform. 2020;8(7):e18599. doi:10.2196/18599
44. Urwyler P, Stucki R, Rampa L, Müri R, Mosimann UP, Nef T. Cognitive impairment categorized in community-dwelling older adults with and without dementia using in-home sensors that recognise activities of daily living. Sci Rep. 2017;7:42084. doi:10.1038/srep42084
45. Wang S, Bolling K, Mao W, et al. Technology to Support Aging in Place: older Adults’ Perspectives. Healthcare. 2019;7(2):60.
46. Chen YH, Xu JL. Applying artificial intelligence to predict falls for inpatient. Front Med. 2023;10:1285192. doi:10.3389/fmed.2023.1285192
47. Cheng FY, Joshi H, Tandon P, et al. Using machine learning to predict ICU transfer in hospitalized COVID-19 patients. J Clin Med. 2020;9:6.
48. Lee SK, Shin JH, Ahn J, Lee JY, Jang DE. Identifying the risk factors associated with nursing home residents’ pressure ulcers using machine learning methods. Int J Environ Res Public Health. 2021;18:6.
49. Nazir T, Mushhood Ur Rehman M, Asghar MR, Kalia JS. Artificial intelligence assisted acute patient journey. Mini Review. Front Artifi Intel. 2022;5. doi:10.3389/frai.2022.962165
50. Piña IL, Cohen PD, Larson DB, et al. A framework for describing health care delivery organizations and systems. Am J Public Health. 2015;105(4):670–679. doi:10.2105/ajph.2014.301926
51. Cho A, Min IK, Hong S, Chung HS, Lee HS, Kim JH. Effect of applying a real-time medical record input assistance system with voice artificial intelligence on triage task performance in the emergency department: prospective interventional study. JMIR Med Inform. 2022;10(8):e39892. doi:10.2196/39892
52. Wang C, Yao C, Chen P, Shi J, Gu Z, Zhou Z. Artificial intelligence algorithm with ICD coding technology guided by embedded electronic medical record system in medical record information management. Microprocess Microsyst. 2023;104962. doi:10.1016/j.micpro.2023.104962
53. Rachel K, Katherine PL. From real-world electronic health record data to real-world results using artificial intelligence. Ann Rheumatic Dis. 2023;82(3):306. doi:10.1136/ard-2022-222626
54. Davy van de S, Michel EVG, Jim MS, et al. Developing, implementing and governing artificial intelligence in medicine: a step-by-step approach to prevent an artificial intelligence winter. BMJ Health Care Inform. 2022;29(1):e100495. doi:10.1136/bmjhci-2021-100495
55. Obermeyer Z, Powers B, Vogeli C, Mullainathan S. Dissecting racial bias in an algorithm used to manage the health of populations. Science. 2019;366(6464):447–453. doi:10.1126/science.aax2342
56. Choudhury A, Asan O. Impact of accountability, training, and human factors on the use of artificial intelligence in healthcare: exploring the perceptions of healthcare practitioners in the US. Hum Fact Healthc. 2022;2:100021. doi:10.1016/j.hfh.2022.100021
57. Russell RG, Lovett Novak L, Patel M, et al. Competencies for the use of artificial intelligence–based tools by health care professionals. Acad Med. 2023;98:3.
58. Edgley K, Horne AW, Saunders PT, Tsanas A. Symptom tracking in endometriosis using digital technologies: knowns, unknowns, and future prospects. Cell Rep Med. 2023;4:9.
59. Kuchana M, Srivastava A, Das R, Mathew J, Mishra A, Khatter K. AI aiding in diagnosing, tracking recovery of COVID-19 using deep learning on Chest CT scans. Multimedia Tools Appl. 2021;80(6):9161–9175. doi:10.1007/s11042-020-10010-8
 © 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.