Back to Journals » International Journal of General Medicine » Volume 14
A Scale for Predicting the Outcomes of Patients with Epilepsy: A Study of 141 Cases
Authors Chen X, Ma XB, Zhang Q, Yin Q, Li XH
Received 19 January 2021
Accepted for publication 8 March 2021
Published 28 April 2021 Volume 2021:14 Pages 1565—1574
DOI https://doi.org/10.2147/IJGM.S302735
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Xu Chen,1,2 Xiao-Bo Ma,3 Qiang Zhang,3 Qing Yin,1 Xiao-Hong Li1
1Department of Neurology, Jinan Central Hospital, Cheeloo College of Medicine, Shandong University, Jinan, People’s Republic of China; 2Department of Neurology, ShuLan (Hangzhou) Hospital, Hangzhou, People’s Republic of China; 3Department of Neurology, Jen Ching Memorial Hospital, Kunshan, People’s Republic of China
Correspondence: Xiao-Hong Li
Department of Neurology, Jinan Central Hospital, Cheeloo College of Medicine, Shandong University, No. 105 of Jiefang Street, Lixia District, Jinan, People’s Republic of China
Tel +86 035155863234
Fax +86 035155863234
Email [email protected]
Objective: This study aimed to identify the factors relevant for developing a scale to estimate the prognosis of patients with epilepsy.
Methods: This study followed 141 patients with newly or previously diagnosed epilepsy for between four and nine years. The patients were divided into three groups on the basis of their outcomes during the follow-up period: patients that were seizure-free without anti-epileptic drugs (AEDs) (group A, n = 48), patients with pharmacoresponsive epilepsy (group B, n = 52), and patients with pharmacoresistant epilepsy (group C, n = 41). The predictors of the prognosis of epilepsy were determined using logistic regression models and optimum subsets regression, and a scale for estimating the prognosis of epilepsy (SEPE) was developed.
Results: The SEPE was able to distinguish between better and worse outcomes for the three groups. A score ≤ 3 on the SEPE predicted that a patient would become seizure-free without the use of AEDs, with a specificity of 67% and a sensitivity of 50%. A score ≤ 4 on the SEPE predicted that a patient may have a positive outcome; scores in this range were assigned to 97.9% of patients that were seizure-free without the use of AEDs and 65% of patients with pharmacoresponsive epilepsy, with a specificity of 80%, a sensitivity of 81%. Scores ≥ 6 on the SEPE predicted a poor outcome.
Conclusion: Of the patients with a SEPE score ≤ 3, some were able to become seizure-free without the use of AEDs, while for other patients, it may be possible that AED use can be discontinued. Patients with a SEPE score ≤ 4 have the potential to achieve long-term remission. Patients with a SEPE score ≥ 6 are more likely to have pharmacoresistant epilepsy.
Keywords: epilepsy, prognosis, factors, score
Introduction
Epilepsy is a disorder of the brain that is characterized by the long-term occurrence of epileptic seizures, and epileptogenesis is the process by which a neuronal network develops in such a way that spontaneous seizures occur.1 Because the cause of epileptogenesis is unknown, the classification of epilepsies and seizures has played a central role in research on epilepsy and its clinical treatment. Epilepsy and epileptic seizures may be a manifestation of brain insults or systemic diseases. The prognosis of patients diagnosed with epilepsy has important epidemiological and clinical implications because the risk profile of a given patient may be used to tailor the treatment strategy.
The results of longitudinal cohort studies carried out since the late 1970s have transformed our understanding of the prognosis of epilepsy. Using a card-based record linkage system, Annegers et al2 retrospectively examined cases that were initially diagnosed between 1935 and 1974. At 5 years after diagnosis, 42% of cases were in remission; this percentage rose to 65% at 10 years after diagnosis and 70% at 20 years after diagnosis. (A further 6% of patients that had previously been in 5-year remission relapsed.) Thus, by the end of the study period, over three-fourths of all patients were in terminal remission, and approximately half of all patients had been able to discontinue the use of anti-epileptic drugs (AEDs). MacDonald et al3 used the Cox proportional hazards regression model to analyze the factors predicting patient outcome (remission or relapse). The study had two influential findings: First, that the number of seizures experienced in the early phase of epilepsy is the most important predictor of both early and long-term remission, and second, that the longer that seizures continue, the worse the long-term prognosis.
A recent study suggested that praxis induction, a reflex trait associated with juvenile myoclonic epilepsy, is related to seizures that do not occur at a particular point during the wake–sleep cycle and that have a reduced response to AEDs.4 Another recent study demonstrated that the predictors of poor outcome include partial seizure presentation, the presence of mesial temporal sclerosis or bitemporal epilepsy, and the use of a greater number of AEDs.5
In this study, we examined data collected from a cohort of patients that was followed up for a median of 9.1 years. We investigated the possible clinical differences of patients that were seizure-free without the use of AEDs, patients that had pharmacoresponsive epilepsy, and patients that had pharmacoresistant epilepsy. On the basis of this investigation, we developed a scale that can be used to evaluate the prognosis of patients with epilepsy. Hence we will divide the study into two sections; analyzing predictors that were associated with outcome as seen in 141 patients with epilepsy; developing a scale for estimating the prognosis of epilepsy.
The Study of 141 Cases
Patients and Methods
Study Populations
We retrospectively collected data from 217 patients that had been newly or previously diagnosed with epileptic seizures between January 1, 2010, and April 30, 2015, which included any age at the time of study. The patients were recruited from Jen Ching Memorial Hospital in Suzhou, Jiangsu, China, and the patient group included both inpatients and outpatients. The diagnoses and definitions used in this study were in accordance with the 2014 criteria of the International League Against Epilepsy,6 inclusion criteria included the following: (i) at least two unprovoked (or reflex) seizures occurring >24 h apart, (ii) one unprovoked (or reflex) seizure and a probability of further seizures similar to the general recurrence risk (at least 60%) after two unprovoked seizures, occurring over the next 10 years (iii), diagnosis of an epilepsy syndrome; Exclusion criteria were as follows: (i) acute symptom onset, occurring in close temporal relationship with an acute central nervous system insult, which may be metabolic, toxic, structural, infectious, or due to inflammation; (ii) febrile seizures.
We gathered the following data from each patient’s medical records: sex, the patient’s family history of epilepsy, the adult or ≥14 year old patient’s history of febrile seizures, the types of seizures experienced by the patient and the age of onset of epileptic seizures, the time to progression since initial diagnosis, the patient’s history of drug use and response, the duration of the patient’s treatment, and the results of magnetic resonance imaging (1.5TMRI) and ambulatory electroencephalography (AEEG) at the time of diagnosis.
In addition, a structured telephone questionnaire was administered to patients on a voluntary basis in December 2019. The questionnaire collected information about whether seizures recurred after the discontinuation of treatment, what type of seizures were experienced, whether terminal remission had been achieved, and what current treatment the patient was receiving. Because 65 patients were lost to follow-up, and some patients were excluded from the follow-up investigation if they suffered from symptomatic epilepsy due to a stroke, traumatic brain injury, or infection of the central nervous system. The telephone questionnaire on long-term outcomes was administered to 152 patients. In addition, 11 patients that suffered febrile seizures were excluded as a result. This resulted in a final cohort of 141 patients with epilepsy.
Dividing into Groups and Collecting Data
The 141 patients with epilepsy were divided into three groups according to their follow-up outcomes. Group A (cases that were seizure-free without the use of AEDs; n = 48, 34%) comprised patients that had been seizure-free for more than 12 months without taking AEDs or that had not taken AEDs from their time of diagnosis to the end of the follow-up period, the latter is comprised of no following doctor’s advice and refusing to take AEDs’ patients. Group B (pharmacoresponsive cases, which means that the epilepsy will be likely to be controlled with appropriate antiepileptic therapy;7 n = 52, 37%) comprised patients that remained in remission for more than 12 months by continuously taking AEDs. Group C (pharmacoresistant cases, which can be practically defined as failure to achieve seizure freedom following adequate trials of two tolerated and appropriately chosen AEDs;8 n = 41, 29%) comprised patients that still experienced seizures even though they may have experienced partial improvement by continuously taking AEDs. Figure 1 presents a flowchart of patients during the study.
 |
Figure 1 Flowchart of patients screened in the study. |
All patient demographics (sex, age, and family history of epilepsy) were recorded. The collected information related to age included the age of onset, the age at which treatment began, and the age at the end of the follow-up period. The following clinical manifestations were also recorded for each patient: (i) the time of the seizures (during the sleeping period, the waking period, or both), (ii) the type or types of seizures that had been experienced during the period of investigation, (iii) the frequency of the seizures, (iv) the presence of mental decay, (v) the children with history of febrile seizures, (vi) to show paroxysmal AEEG abnormalities during the waking period and stages I and II of sleep, (vii) the results of MRI scans, and (viii) the treatment that the patient had received.
Statistical Analysis
Statistical analysis was performed using SPSS 24.0 (IBM Corp., Armonk, NY, USA). All data related to age were presented as the range, mean, standard deviation, and median with interquartile range.
Comparison among groups was performed using one-way analysis of variance (ANOVA) for continuous variables. The level of statistical significance was set at P < 0.05. For comparison between groups, the chi-square test was used for categorical variables, and adjusted residual analysis was performed for R×C tables when P < 0.05. The predictors of the prognosis of epilepsy were determined using logistic regression models and optimum subsets regression; P < 0.05 (two-sided) was considered to be statistically significant.
Results
Demographics and Baseline Clinical Characteristics
Of the 141 patients with epilepsy included in the study, 89 (63%) were male, and 52 (37%) were female. The mean age at onset (± standard deviation) was 22.18 (± 1.38) years, the range was 1 month to 78 years, the 50th percentile was 19.83 years, and the 75th percentile was 28.94 years. The duration of epilepsy was defined as the time of onset to the end of the follow-up period. The mean duration of epilepsy (± standard deviation) was 11.3 (± 0.6) years, the range was 4–45 years, the 50th percentile was 9.11 years, and the 75th percentile was 12.93 years. The mean age at the end of the follow-up period (± standard deviation) was 33.49 (± 1.42) years, the range was 7–85 years, the 50th percentile was 31.2 years, and the 75th percentile was 41.5 years.
Table 1 presents the results of analyzing the age of onset and the time course of epilepsy for the three groups using ANOVA. There were significant differences in the three groups (P < 0.0001) in the time course of epilepsy. There were no significant difference in the age of onset.
 |
Table 1 Comparison of Baseline Clinical Characteristics of Epileptic Seizure in Three Groups |
Particular attention was paid to the time at which seizures occurring during the sleep–wake cycle (ie, during the sleeping period, the waking period, or both). Seizures that occurred during the sleeping period were distinguished from those that occurred during the waking period or during both periods. Patients that only experienced seizures during the sleeping period had a better prognosis than patients that experienced seizures during the waking period or during both periods (P = 0.045) (Table 1).
We compared the three groups in terms of the types of epileptic seizures that were experienced, and we recorded whether patients experienced one type or multiple types of seizures. The results of the statistical analysis demonstrated that patients that experienced two or more types of seizures had a worse prognosis than patients that experienced only one type of seizure (P < 0.0001). Although the patients in all three groups exhibited paroxysmal abnormal AEEG patterns, there were no significant differences in the three groups (p = 0.534) (Table 1).
The Possible Risk Factors of the Pharmacoresistant Cases and the Analysis of the Other Data
Table 2 presents the results of the logistic regression models and the analysis of group C, the patients with pharmacoresistant epilepsy. These results demonstrate that five factors potentially increased the risk of pharmacoresistance: female gender (51.2% vs 31%, P = 0.004), the frequency of seizures over two months (OR = 19.547, 95% CI = [1.228, 311.219], P = 0.035), the presence of mental decay (17% vs 0%), a family history of epilepsy (7% vs 1%, P = 0.022), and abnormal MRI results (19.5% vs 7%, P = 0.012).
 |
Table 2 The Possible Risk Factors of the Pharmacoresistant Cases |
The other data collected include the following: (i) Of the 48 patients in group A (cases that were seizure-free without the use of AEDs), 31 patients (65%) had not taken AEDs since the onset of epilepsy; out of these, there were 2 patients with automatisms, 5 patients with cognitive seizures, 1 patient with autonomic seizures, and 23 patients with generalized tonic–clonic seizures. (ii) Of the 52 patients in group B (pharmacoresponsive cases), 7 (13%) chose to take a combination of drugs, and 45 chose to take a single drug. (iii) Of the 41 patients in group C (pharmacoresistant cases), 3 patients took drugs irregularly, and 1 patient had a 22-year duration of epilepsy, during which time seizures occurred once every one or two years and the patient did not take any AEDs. However, because the patient began to take AEDs when her seizures increased in frequency over the past six years, her remission period was less than 12 months.
Discussion
A study of the natural history of untreated epilepsy, largely based on developing countries, shows that 30–40% of patients obtain between 5- and 10-year remission without treatment. In developed countries, by contrast, treatment is generally started after two unprovoked seizures have taken place, and the likelihood of 5-year remission is approximately 60% in patients followed for 10 years and 70% in patients followed for 20 years. The rate of 5-year remission in children in developed countries is approximately 75%. Approximately 60% of patients achieve long-term freedom from seizures, with 35–40% of patients experiencing early remission and 20–25% of patients experiencing late remission; an additional 16% of patients alternate between relapse and remission, and approximately 25% never achieve remission.9
In our study, all of the 141 patients included in the study had relevant medical histories of at least 4 years, and some patients had histories of more than 20 years; the mean length was 11.3 (± 0.6) years, the 50th percentile was 9.11 years, and the 75th percentile was 12.93 years. There were significant differences in the lengths of the medical histories of the patients in groups A, B, and C (p < 0.0001). A longer duration of epilepsy appears to correspond to a worse prognosis. In addition, the longer the duration of epilepsy, the higher the reported rate of recurrence: Annegers et al10 reported a rate of recurrence of 36% within one year and 56% within five years. Similarly, the National General Practice Study of Epilepsy, a prospective community-based study of seizure recurrence, reported a rate of recurrence of 67% within one year and 78% within three years.11 In our study, two patients that had been seizure-free for more than five years after discontinuing the use of AEDs experienced seizures after the end of the follow-up period. As a result, neurologists face the dilemma of whether to withdraw AEDs or continue to prescribe them when a patient has been seizure-free for four to five years.
The relationship between sleep and epilepsy is well-established and has been recognized since antiquity. In more recent years, the widespread availability of long-term sleep monitoring and polysomnography has made early observation more possible and has resulted in a surge of interest among clinicians that treat people with epilepsy. The relationship between a patient’s prognosis and the sleep–wake cycle in epilepsy patients is a complex one. Gibberd and Bateson12 studied the natural history of sleep-related epilepsies, which occurred in 12% of the 645 patients that they studied. They found that only 30% of these cases achieved remission, while an additional 30% developed either waking epilepsy or diffuse epilepsy (ie, epilepsy occurring during both the waking and sleeping periods). Hopkins and Clarke found that patients with nocturnal seizures exhibited higher rates of recurrence,13 especially when the seizures are refractory to therapy.14,15 In our study, by contrast, the results of statistical analysis using the chi-square test demonstrated that patients that only experienced seizures during the sleeping period had a good prognosis (P = 0.045). In addition, the results of logistic regression models indicated that the occurrence of seizures during the sleeping period was not a significant risk factor for pharmacoresistant epilepsy (OR = 0.610, 95% CI = [0.128, 2.90], P = 0.534).
Previous research has shown that the presence of multiple types of epileptic seizures is linked with a worse patient prognosis.16–18 Our study obtained a similar outcome: Patients with pharmacoresistant epilepsy were significantly more likely to experience multiple types of seizures than seizure-free patients or patients with pharmacoresponsive epilepsy were (P < 0.0001). In addition, we observed a relationship between prognosis and the type of seizures that were experienced: Whereas jamais vu seizures, memory impairment seizures, and seizures with automatisms were associated with a good prognosis, myoclonic seizures were among the types of seizures that were associated with a poor prognosis.
A particularly poor prognosis has been reported for patients that experience high-frequency tonic–clonic seizures, either prior to receiving treatment18–20 or without reference to medication.21,22 We tracked the frequency of seizures over two-month periods in patients that had taken AEDs and found that patients that experienced at least one seizure every two months had a poor outcome (OR = 19.547, 95% CI = [1.228, 311.219], P = 0.035).
In our study, patients that experienced mental decay had a poor prognosis, and patients with a family history of epilepsy were also at risk of a poor prognosis (P = 0.022). MRI abnormalities also appeared to be related to a poor prognosis (P = 0.012), where the cases of abnormal MRI results considered in this study included punctate ischemia, lacunar infarction, and encephalomalacia. At the same time, however, a previous study found that encephalomalacia may reduce the risk of drug-resistant focal epilepsy in adults.5 Patient prognosis was not related to AEEG abnormalities, either in general or during specific parts of the sleep–wake cycle.
Conclusion
On the basis of a cohort study, we determined which factors were relevant for the prognosis of patients with epilepsy. The results can be summarized as follows: (i) Longer durations of epilepsy were associated with a higher rate of recurrence and a worse prognosis. (ii) Female patients had a greater probability of having pharmacoresistant epilepsy than male patients did. (iii) Epilepsy was self-limiting in 22% (31/141) of patients, who were able to maintain a seizure-free status without the use of AEDs. (iv) The occurrence of multiple types of seizures was associated with a poor prognosis. (v) A high frequency of seizures was predictive of a poor prognosis. (vi) Patients that experienced mental decay had poor outcomes. (vii) Patients with a family history of epilepsy were more likely to have a poor prognosis. (viii) Patients with MRI abnormalities tended to have a worse prognosis. (ix) More work must be done to determine the relationship between patient prognosis and the sleep–wake cycle: Although logistic regression models did not return a significant correlation between the prognosis and the sleep–wake cycle, we had expected that seizures during the sleeping period would be associated with a more positive prognosis; whereas previous research has shown:23 seizures that took place throughout the sleep–wake cycle would be predictive of a poor prognosis.
Developing a Scale for Estimating the Prognosis of Epilepsy
The question of primary interest for a person that develops epilepsy and seizures is, “What is the likelihood that the seizures will go away?” This is a challenging question, not only for patients that suffer from epilepsy but also for neurologists that research it. Therefore, in view of our study of 141 cases, we attempted to identify the factors relevant for developing a scale to estimate the prognosis of patients with epilepsy.
Data and Methods
On the basis of the results of our study and those of previously published work (eg the relationship between patient prognosis and the sleep–wake cycle), we developed the scale for estimating the prognosis of epilepsy (SEPE).
From logistic regression models and optimum subsets regression, the scores were allocated to the predictors and summarized to give a predictive score. We simply included in the score any variable that was a univariate predictor of the outcome of patients with epilepsy with a significance of p<0·05, with each bivariate risk factor allocated integer values of 0 and 1, and each trivariate factor allocated values of 0.1, and 2, et cetera, 0,1,2,3, the predictive scores shown in Table 3.
 |
Table 3 Scoring for Estimating Prognosis of Epilepsy (SEPE) |
We applied the SEPE to the patients in our study in order to verify the proposed scoring system. Using SPSS 24.0, we assigned scores to the members of group A (n = 48), group B (n = 52), and group C (n = 41) on the basis of the collected data, which were described in terms of their ranges, means, standard deviations, and medians with interquartile ranges. The results are shown in Table 4. ANOVA was then used to compare the scores among the groups (Table 5). As shown in Table 5, the SEPE may be able to distinguish between good and poor prognoses for the patients in the three groups. We analyzed Table 4 to obtain the sensitivity and specificity values. Table 6 presents the results of this analysis.
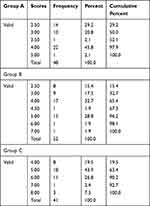 |
Table 4 The Summary Data of Scores in Three Groups |
 |
Table 5 Comparison of Using ANOVA for Scores Among Three Groups |
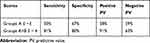 |
Table 6 The Sensitivity and Specificity of Utilizing SEPE |
Results
(i) A score ≤3 on the SEPE predicted that a patient may become seizure-free without the use of AEDs, with a specificity of 67% and a sensitivity of 50%. (ii) A score ≤4 on the SEPE predicted that a patient would have a positive outcome; scores in this range were assigned to 97.9% of patients that were seizure-free without the use of AEDs and 65% of patients with pharmacoresponsive epilepsy, with a specificity of 80%, a sensitivity of 81%, a positive predictive value of 91%, and a negative predictive value of 63%. (iii) Scores between 4.5 and 5 were assigned to 2.1% of patients that were seizure-free without the use of AEDs, 30.7% of patients with pharmacoresponsive epilepsy, and 43.9% of patients with pharmacoresistant epilepsy. (iv) Scores ≥6 were assigned to 3.8% of patients with pharmacoresponsive epilepsy and 36.5% of patients with pharmacoresistant epilepsy.
Conclusion
In this study, 141 patients that had been followed up for between four and nine years were divided into three groups, namely patients that were seizure-free without the use of AEDs (n = 48), patients with pharmacoresponsive epilepsy (n = 52), and patients with pharmacoresistant epilepsy (n = 41). We used statistical analysis to determine the factors that were predictive of patient outcomes, and we used these predictors to design the SEPE and assign scores to evaluate each patient’s prognosis. We drew the following conclusions: (i) Some patients with a SEPE score ≤3 will experience self-limiting epilepsy and become seizure-free without the use of AEDs; for other patients with a SEPE score ≤3, it may be possible that the use of AEDs can be discontinued. For patients with a score ≤3, the SEPE had a specificity of 67% and a sensitivity of 50%. (ii) If a patient has a SEPE score ≤4, it is possible that long-term remission will be achieved, with a specificity of 80%, a sensitivity of 81%, a positive predictive value of 91%, and a negative predictive value of 63%. (iii) Patients with a SEPE score ≥6 may experience pharmacoresistance.
Limitations and Strengths of the Study
Our study has several limitations. First, the sample size of the cohort was relatively small and, as a result, it is possible that certain prognostic factors may have been overlooked. Studies with larger cohorts should be carried out in the future to address this. Second, the study used retrospective methods, namely the review of medical reports, in addition to prospective ones. Future studies that utilize more prospective methods will be better able to avoid bias of data. Third, the study used a convenience sample drawn from a single specialized epilepsy center. However, we posit that the SEPE designed on the basis of that sample can be used to estimate the prognoses of other patients with epilepsy.
Abbreviations
AED, anti-epileptic drug; AEEG, Ambulatory electroencephalography; ANOVA, analysis of variance; SEPE, scoring for estimating prognosis of epilepsy.
Ethics Approval and Consent to Participate
This study was conducted with approval from the Ethics Committee of Jinan Central Hospital and Jen Ching Memorial Hospital (2021, No.1). This study was conducted in accordance with the declaration of Helsinki. Written informed consent was obtained from all participants.
Acknowledgments
We would like to acknowledge the hard and dedicated work of all the staff that implemented the intervention and evaluation components of the study.
Funding
There is no funding to report.
Disclosure
The authors declare that they have no competing interests.
References
1. Duncan JS, Sander JW, Sisodiya SM, Walker MC. Adult epilepsy. Lancet. 2006;367:1087–1100. doi:10.1016/S0140-6736(06)68477-8
2. Annegers JF, Hauser WA, Elveback LR. Remission of seizures and relapse in patients with epilepsy. Epilepsia. 1979;20:729–737. doi:10.1111/j.1528-1157.1979.tb04857.x
3. MacDonald BK, Johnson AL, Goodridge DM, Cockerell OC, Sander JW, Shorvon SD. Factors predicting prognosis of epilepsy after presentation with seizures. Ann Neurol. 2000;48:833–841. doi:10.1002/1531-8249(200012)48:6<833::AID-ANA3>3.0.CO;2-U
4. Uchida CG, de Carvalho KC, Guaranha MS, et al. Phenotyping juvenile myoclonic epilepsy. Praxis induction as a biomarker of unfavorable prognosis. Seizure. 2015;32:62–68. doi:10.1016/j.seizure.2015.09.011
5. Roy PL, Ronquillo LH, Ladino LD, Tellez-Zenteno JF. Risk factors associated with drug resistant focal epilepsy in adults: a case control study. Seizure Eur J Epilepsy. 2019;73:46–50. doi:10.1016/j.seizure.2019.10.020
6. Fisher RS, Acevedo C, Arzimanoglou A, et al. ILAE official report: a practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475–482. doi:10.1111/epi.12550
7. Ingrid E. Scheffer, Samuel Berkovic, Giuseppe Capovilla, et al ILAE classification of the epilepsies. Epilepsia. 2017;58(4):512–521. doi:10.1111/epi.13709
8. Mubeen J, Brodieb MJ, Patrick K. Pharmacoresistance – epidemiology, mechanisms, and impact on epilepsy treatment. Neuropharmacology. 2020;168:107790. doi:10.1016/j.neuropharm.2019.107790
9. Brodie MJ, Barry SJ, Bamagous GA, Norrie JD, Kwan P. Patterns of treatment response in newly diagnosed epilepsy. Neurology. 2012;78:1548–1554. doi:10.1212/WNL.0b013e3182563b19
10. Annegers JF, Shirts SB, Hauser WA, Kurland LT. Risk of recurrence after an initial unprovoked seizure. Epilepsia. 1986;27:43–50. doi:10.1111/j.1528-1157.1986.tb03499.x
11. Hart YM, Sander JW, Johnson AL, Shorvon SD. National general practice study of epilepsy: recurrence after a first seizure [see comments]. Lancet. 1990;336:1271–1274. doi:10.1016/0140-6736(90)92960-P
12. Gibberd FB, Bateson MC. Sleep Epilepsy: its pattern and prognosis. BMJ. 1974;25:403–405. doi:10.1136/bmj.2.5916.403
13. Hopkins A, Garman A, Clarke C. The first seizure in adult life: value of clinical features, electroencephalogram, and computerised tomography scanning in prediction of recurrence. Lancet. 1988;721–726. doi:10.1016/S0140-6736(88)91535-8
14. Foldvary-Schaefer N, Grigg-Damberger M. Sleep and Epilepsy: what we know, don’t know. J Clin Neurophysiol. 2006;23:4–20. doi:10.1097/01.wnp.0000206877.90232.cb
15. Krumholz A, Wiebe S, Gronseth GS, et al. Evidence-based guideline: management of an unprovoked first seizure in adults: report of the guideline development subcommittee of the american academy of neurology and the american epilepsy society. Neurology. 2015;84(16):1705–1713. doi:10.1212/WNL.0000000000001487
16. Bronson LO, Wranne L. Long-term prognosis in childhood epilepsy: survival and seizure prognosis. Epilepsia. 1987;28:324–330. doi:10.1111/j.1528-1157.1987.tb03651.x
17. Beghi E, Tognoni G. Prognosis of epilepsy in newly referred patients: a multicenter prospective study. Collaborative group for the study of epilepsy. Epilepsia. 1988;29:236–243. doi:10.1111/j.1528-1157.1988.tb03712.x
18. Collaborative Group for the Study of Epilepsy. Prognosis of epilepsy in newly referred patients: a multicenter prospective study of the effects of monotherapy on the long-term course of epilepsy. Epilepsia. 1992;33:45–51. doi:10.1111/j.1528-1157.1992.tb02281.x
19. Camfield C, Camfield P, Gordon K, Dooley J. Does the number of seizures before treatment influence ease of control or remission of childhood epilepsy? Not if the number is 10 or less. Neurology. 1996;46:41–44. doi:10.1212/WNL.46.1.41
20. Shorvon SD, Goodridge DM. Longitudinal cohort studies of the prognosis of epilepsy: contribution of the National General Practice Study of Epilepsy and other studies. Brain. 2013;136:3497–3510. doi:10.1093/brain/awt223
21. Sillanpaa M. Remission of seizures and predictors of intractability in long-term follow-up. Epilepsia. 1993;34:930–936. doi:10.1111/j.1528-1157.1993.tb02114.x
22. Sander JW. Some aspects of prognosis in the epilepsies: a review. Epilepsia. 1993;34:1007–1016. doi:10.1111/j.1528-1157.1993.tb02126.x
23. Melissa Méndez MD, Rodney A, Radtke MD. Interactions between sleep and epilepsy. J Clin Neurophysiol. 2001;18(2).
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
