Back to Journals » Journal of Hepatocellular Carcinoma » Volume 11
A Novel Nomogram to Predict Prognosis of Advanced Hepatocellular Carcinoma Treated with Intensity-Modulated Radiotherapy Plus Anti-PD1
Authors He M, Liang C, Pang Y, Jiang M, Long M, Yao Z, Wang X, Zhang R, Wu Q, Liang S, Li J
Received 24 February 2024
Accepted for publication 7 May 2024
Published 22 May 2024 Volume 2024:11 Pages 913—925
DOI https://doi.org/10.2147/JHC.S459683
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Manal Hassan
Meiling He,1 Chunfeng Liang,1 Yadan Pang,1 Mengjie Jiang,1 Meiying Long,2 Zhongqiang Yao,3 Xiaoting Wang,1 Ruijun Zhang,1 Qiaoyuan Wu,1 Shixiong Liang,1 Jianxu Li1
1Department of Radiation Oncology, Guangxi Medical University Cancer Hospital, Nanning, 530021, People’s Republic of China; 2School of Public Health, Guangxi Medical University, Nanning, 530021, People’s Republic of China; 3Department of General Affairs, Guangxi Medical University Cancer Hospital, Nanning, 530021, People’s Republic of China
Correspondence: Shixiong Liang; Jianxu Li, Tel +86 13917716605 ; +86 18878732921, Email [email protected]; [email protected]
Purpose: The combination of radiotherapy and monoclonal antibody against programmed cell death 1 (anti-PD1) showed preliminary efficacy in hepatocellular carcinoma (HCC). This study aimed to identify the prognostic factors and construct a nomogram to predict the overall survival (OS) of patients with advanced HCC after treatment with intensity-modulated radiotherapy (IMRT) plus anti-PD1.
Patients and Methods: The OS and progression-free survival (PFS) of 102 patients with BCLC stage C HCC was analyzed using the Kaplan-Meier method. Potential independent prognostic factors were determined using univariate and multivariate Cox regression analyses. A nomogram was established to predict prognosis whose accuracy and reliability was verified by a calibration curve and area under the receiver operating characteristic curve (AUROC).
Results: The median PFS and OS rates of the 102 patients with advanced HCC were 9.9 months and 14.3 months, respectively. Ninety-three patients were evaluated for efficacy, including five (5.38%) with complete response and 48 (51.61%) with partial response, with an overall response rate of 56.99%. Grade 3 and 4 adverse reactions (AEs) were observed in 32.35% of patients; no grade 5 AEs occurred. Multivariate Cox analysis revealed albumin and alpha-fetoprotein levels, neutrophil counts 3– 4 weeks after IMRT initiation, and platelet-to-lymphocyte ratio 3– 4 weeks after IMRT initiation to be independent prognostic factors. The nomogram model constructed using these factors had good consistency and accuracy with 1– 3 years AUROC of 78.7, 78.6, and 93.5, respectively.
Conclusion: IMRT plus anti-PD1 showed promising efficacy and controllable adverse reactions in treating advanced HCC. The nomogram model demonstrated good reliability and clinical applicability.
Plain Language Summary: The combination of radiotherapy and monoclonal antibody against programmed cell death 1 (anti‑PD1) showed preliminary efficacy and manageable safety in HCC. We retrospectively evaluated the efficacy and safety of 102 patients with advanced HCC treated with intensity-modulated radiotherapy (IMRT) plus anti-PD1. The study shows that the combination showed promising efficacy with a median PFS and OS of 9.9 months and 14.3 months, respectively. The adverse reactions were controllable. The novel nomogram model established based on independent prognostic factors including albumin, alpha-fetoprotein, neutrophils count 3– 4 weeks after IMRT initiation and platelet-to-lymphocyte ratio 3– 4 weeks after IMRT initiation demonstrated good reliability.
Keywords: hepatocellular carcinoma, advanced, intensity-modulated radiotherapy, antibody against programmed cell death 1, nomogram
Introduction
Hepatocellular carcinoma (HCC) is the sixth most common malignancy and fourth leading cause of cancer death globally.1 Half of these cases occur in China, making it the fourth most common malignant tumor in China, with the second-highest fatality rate among all cancers.2 Of these, 53.6% patients with HCC are diagnosed in advanced stage with poor prognosis.3 Sorafenib and lenvatinib were recommended as the first-line therapy for unresectable HCC, which has median overall survival (OS) and median progression-free survival (PFS) of 10.7 months, 5.5 months and 13.6 months, 7.4 months, respectively.4,5 In comparison, the median OS and PFS of atezolizumab plus bevacizumab were 19.2 months, 6.8 months, with better OS and PFS outcomes.6 However, the treatment outcomes in patients with advanced HCC remain unsatisfactory.
Radiotherapy (RT) is a highly effective anticancer therapy that can achieve local control rates between 30% and 50% in advanced HCC.7 In recent years, monoclonal antibodies against programmed cell death 1 pathway (anti‑PD1) have been shown to have a positive therapeutic effect in patients with advanced HCC, with an overall response rate (ORR) of approximately 14–17%.8–10
Anti‑PD1 can regulate tumor immune environment, while RT causes local tumor killing and systemic immune regulation effects, thus enhancing the role of anti‑PD1. RT combined with anti‑PD1 can achieve certain synergistic effect, which can turn “cold” tumors into “hot” tumors, improving the immunogenicity of tumors, thereby enhancing their therapeutic effect.11,12 Therefore, the combination of RT and anti‑PD1 may be a useful strategy to enhance the anti-tumor immune response. Recent studies have found this combination to show significantly promising efficacy and manageable safety13,14 providing a novel effective therapeutic strategy for HCC.
Recently, an increasing number of indicators of potential inflammation in peripheral blood, such as the platelet-to-lymphocyte ratio (PLR), neutrophil-to-lymphocyte ratio (NLR), and systemic immune-inflammation index (SII), have been identified to predict the prognosis of patients with HCC in clinical practice. Our previous studies found that inflammatory markers were closely associated with the prognosis of patients with unresectable HCC treated with intensity-modulated radiotherapy (IMRT).15 In addition, immunotherapy is closely associated with inflammatory markers.16,17 Therefore, we retrospectively evaluated the efficacy and safety, identified prognostic factors including inflammatory markers, and constructed a nomogram to predict the OS of patients with advanced HCC treated with IMRT plus anti‑PD1.
Materials and Methods
Study Design and Patients
This retrospective study was approved by the Institutional Ethics Committee of the Guangxi Medical University Cancer Hospital (LW2023043). The major inclusion criteria were as follows: histologically or clinically confirmed HCC according to the American Association for the Study of Liver Diseases criteria, Barcelona Clinic Liver Cancer (BCLC) stage C; Complete follow-up data, treatment with IMRT combined with anti‑PD1, and patients with or without prior therapy. Patients with BCLC stage A or B disease and those with combined intrahepatic cholangiocarcinoma were excluded (Figure 1).
IMRT
The main indication for IMRT included liver tumors with macrovascular invasion; distant metastasis treated with palliative IMRT. For patients with bilobar multiple HCCs, as many lesions as possible were chosen for IMRT without exceeding the tolerance limits of the organs at risk. All patients underwent enhanced computed tomography (CT) scan at 2.5–5 mm slice thickness for IMRT planning. CT-positron emission tomography fusion and magnetic resonance imaging fusion were performed for identifying extrahepatic metastasis and intrahepatic lesions, respectively. Gross tumor volume (GTV) was defined as the tumor focus. The GTV and at-risk organs were contoured using the Pinnacle 3 system (Philips, Netherlands) or the MIM software (version 6.8; MIM, USA). The planned target volume (PTV) was defined as the GTV plus an asymmetrical dilation of 1 cm in the craniocaudal direction and 5 mm in the axial direction to set the uncertainty and respiratory movement. The IMRT plans were designed using Pinnacle 3 or the Monaco treatment planning system version 5.1. The final median biologically effective dose, which used α/β ratio = 10 according to the linear-quadratic model, was 51 Gy (interquartile range, 40–51 Gy). IMRT was delivered via a 6 MV X-ray linear accelerator (ELEKTA Synergy or ELEKTA Versa-HD, Sweden) using cone-beam CT to correct the positions.18
Anti‑PD1 Therapy
Anti‑PD1 mainly include camrelizumab (Jiangsu HengRui Medicine Co., Ltd.), tislelizumab (BeiGene), pembrolizumab (Merck Sharp & Dohme Co., Inc.), sintilimab (Innovent Biologics Co., Ltd.), and toripalimab (Shanghai Junshi Biosciences Co., Ltd.). The dose, injection method, and duration were selected according to manufacturer’s instructions. Anti‑PD1 therapy was administered continually every 2–3 weeks until disease progression or signs of intolerable toxicity were observed.
Peripheral Blood Immune Parameters
Peripheral blood was collected within 1 week before IMRT to determine the lymphocyte, neutrophil, and platelet counts. Post-treatment peripheral blood was tested 3–4 weeks after initiation of IMRT and 1 month after the end of IMRT. The ratios and changes in values were calculated as follows: PLR = platelet count / lymphocyte count; NLR = neutrophil count / lymphocyte count; SII = (platelet count × neutrophil count) / lymphocyte count; post-PLR = post-platelet count / post-lymphocyte count; post-NLR = post-neutrophil count / post-lymphocyte count; post-SII = (post-platelet count × post-neutrophil count) / post-lymphocyte count; delta-NLR = post-NLR – NLR; delta-PLR = post-PLR – PLR; and delta-SII = post-SII – SII; change-PLR =(post-PLR – PLR) / PLR; change-NLR =(post-NLR – NLR) / NLR; change-SII =(post-SII – SII) / SII. The optimal cutoff values for immune parameters were selected according to the area under the receiver operating characteristic (ROC) curve.
Efficacy and Safety
Briefly, the enrollment date was defined as the day IMRT began. Follow-up and imaging examinations including the liver image study was performed every 3 months for 2 years and every 6 months thereafter. Its efficacy and safety have been previously described.13 The OS was defined as the time from enrollment to death from any cause. Tumor responses were evaluated according to the Response Evaluation Criteria in Solid Tumors, version 1.1 (RECIST 1.1). PFS was defined as the time between enrollment and the onset of disease progression or death. ORR was defined as the proportion of patients showing complete response (CR) or partial response (PR). Best overall response corresponds to the best overall tumor response assessment at any time-point from the start of the treatment until disease progression. Routine laboratory investigations, including full blood count, liver and renal function tests, thyroid function tests, and routine urine and stool tests, were conducted to check for adverse reactions. The adverse reactions (AEs) were classified into G0-G5 according to the Common Terminology Criteria for Adverse Events of the National Cancer Institute version 5.0.
Statistical Analysis
The R language (version 4.0.3) was used for statistical analysis. Through histogram visualization and the Kolmogorov–Smirnov test, non-normal distributions were expressed as the median (quartile). Categorical variables were expressed as numbers and percentages. The ROC curve was used to obtain the best cutoff values for continuous variables. The Cox proportional hazard model was used to determine the prognostic indicators. A univariate analysis was performed for all variables, and the significant ones were included in the multivariate model. Backward stepwise selection was used to select the characteristics of multivariate regression models. OS and PFS were estimated using the Kaplan–Meier method. The follow-up duration was calculated using the reverse Kaplan–Meier estimate of OS. Statistical significance was set at P < 0.05.
Results
Patient Characteristics
A total of 102 patients with BCLC stage C HCC treated with IMRT combined with anti‑PD1 at Guangxi Medical University Cancer Hospital were recruited from November 2018 to December 2021. Most patients were infected with hepatitis B, 75% had multiple tumors, 66.67% had macrovascular invasion (MVI), 48.04% had extrahepatic metastases, and 25.49% could be classified under Child-Pugh class B. Seventy seven percent of these patients received IMRT synchronous anti‑PD1 treatment. This study included 48 cases receiving IMRT synchronous anti‑PD1 treatment as first-line treatments, 40 cases as second-line treatments, 11 cases as third-line treatments, and 4 cases as four-line treatments. The detailed baseline characteristics of the patients are shown in Table 1.
 |
Table 1 Baseline Characteristics of the Patients |
Efficacy
The follow-up cutoff date was July 10, 2022. The median PFS and OS of 102 patients with BCLC stage C were 9.9 months (95% CI:5.20–14.54) and 14.3 months (95% CI:9.36–19.18), respectively, after a median follow-up of 13.7 months (95% CI:11.21–16.25) (Figure 2, Table 2). The 6-, 9-, and 12-month OS rates were 86.2%, 74.2%, and 61.5%, respectively. (Table 2).
 |
Table 2 Summary of Efficacy Outcomes (N=93) |
 |
Figure 2 Kaplan–Meier analysis of overall and progression free survival. |
Among these patients, 93 showed the best overall response when evaluated based on RECIST 1.1, including 5 patients (5.38%) with CR, 48 patients (51.61%) with PR, 20 patients with stable disease and 20 patients with progressive disease. The ORR reached 56.99% and the overall efficacy rate was satisfactory (Table 2). The best percentage change from baseline in the sum of the longest diameters of the target lesions in the 93 patients is shown in the waterfall plot (Figure 3). Briefly, 86 patients (92.5%) achieved tumor target lesion shrinkage, and 61 patients (65.6%) achieved ≥ 30% tumor target lesion shrinkage when compared to baseline. One patient with intrahepatic lesions and left supraclavicular node metastasis exhibited hyperprogression of the target lesions, extensive peritoneal and pleural effusions, and numerous new intrahepatic lesions. The patient died after rapid tumor progression.
 |
Figure 3 Best percentage change from baseline in sums of diameters of target lesions. Abbreviations: CR, complete response; PD, progressive disease; PR, partial response; SD, stable disease. |
Univariate and Multivariate Analyses for OS and PFS
Cox univariate analysis showed that albumin (Alb), alpha-fetoprotein (AFP), number of tumors, and maximum tumor diameter affected prognosis. However, extrahepatic metastasis, MVI, cirrhosis, and treatment options did not significantly affect the OS. The inflammatory indicators were divided into high and low groups according to the cutoff value of the ROC curve. We found that the inflammatory indicators 3–4 weeks after IMRT began (3–4W) had a greater impact on OS, including neutrophil count, PLR, NLR, and SII, and changed the NLR 1 month after completion of IMRT. In Cox multivariate analysis, Alb > 35 and ≤ 35 g/L (HR = 0.047, 95% CI: 0.22–0.99, P = 0.047), AFP > 400 and ≤ 400 ng/mL (HR = 2.33, 95% CI: 1.19–4.58, P = 0.014), neutrophil count 3–4W > 6.75 and ≤ 6.75 * 109/L (HR = 5.23, 95% CI: 1.78–15.33, P = 0.003), PLR 3–4W > 337.5 and ≤ 337.5 (HR = 2.94, 95% CI: 1.22–7.08, P = 0.017) were independent risk factors affecting OS. In addition, Alb, AFP, the number of tumors, concurrent targeted therapy with IMRT and anti‑PD1 affected PFS, and AFP also was an independent factor (HR = 1.8, 95% CI:1.04–3.11, P = 0.036) (Table 3, showing mainly statistically significant indicators in the univariate analysis).
 |
Table 3 Univariate and Multivariate Cox Regression Analyses for Overall Survival and Progression-Free Survival |
Nomogram and Verification for OS
Four independent risk factors–Alb, AFP, neutrophil count 3–4W, and PLR 3–4W were selected to construct a nomogram for predicting the survival of patients with advanced HCC for 1–3 years. A score was assigned to each variable in the score table, and the total score was used to predict the survival rate (Figure 4A). The AUROC values for 1–3 years were 78.7 (95% CI: 67.8 −89.6), 78.6 (95% CI: 64.0–93.2), 93.5 (95% CI: 87.5–99.6), respectively (Figure 4B). According to the correction curve, the 1-year predicted survival rate was consistent with the observed values (Figure 4C). As the follow-up time was not sufficiently long, the correction curves at 2 and 3 years are not shown.
Safety
Based on the analysis of routine laboratory test results, laboratory-related AEs were observed till 1 month after the completion of IMRT. No grade 5 AEs were observed. Grade 3 and 4 AEs were observed in 32.35% of the patients and mainly manifested as leukopenia (14%), thrombocytopenia (16%), and a decrease in hemoglobin (10%). No grade 3 or 4 AEs were observed during routine treatment of other liver and kidney functions, thyroid functions, or bowel movements, which were tested in most patients. Detailed AEs of the patients are presented in Table 4.
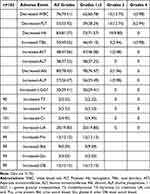 |
Table 4 Adverse Events of Laboratory Testing After IMRT+ Anti-PD1 Treatment |
Discussion
With the development of systemic therapy, anti‑PD1-based combination regimen has changed the treatment landscape for patients with advanced HCC. The combination of RT and anti‑PD1 demonstrated promising efficacy and manageable safety in previous studies. However, few studies have explored the prognostic indicators in patients with advanced HCC treated with IMRT combined with anti‑PD1. Based on the results of this study, independent risk factors, including Alb, AFP, neutrophil count 3–4W and PLR 3–4W were used to construct a nomogram model to predict survival.
Advanced HCC is associated with a poor prognosis. Sorafenib is recommended for patients with advanced HCC in the Asia-Pacific region, and shows a median OS of 5.6 months.19 In the REFLECT trial, lenvatinib treatment resulted in a median OS of 11.8 months in patients with BCLC stage C HCC.5 In the present study, the median OS of patients with BCLC stage C HCC was 14.3 months, indicating better OS outcome. Although atezolizumab plus bevacizumab achieved a better median OS of 17.5 months for patients with BCLC stage C HCC in the IMbrave150 updated efficacy data after a median follow-up of 15.6 months,20 IMRT combined with anti‑PD1 resulted in better median PFS of 9.9 months than the 6.5 months provided by atezolizumab plus bevacizumab, indicating better efficacy.21 Notably, patients with Child-Pugh B liver function accounted for 25.49% in the present study, whereas none were included in the IMbrave150 trial. Meanwhile, the number of patients infected with hepatitis B was higher in this study than in the IMbrave150 trial (88% vs 49%, respectively). Child–Pugh B liver function and hepatitis B virus infection are known to be associated with poor OS.22 Moreover, atezolizumab plus bevacizumab is significantly more expensive.
RT has been shown to work synergistically with immunomodulatory therapy via various mechanisms. RT can trigger the release of pro-inflammatory mediators, increase tumor-infiltrating immune cells, reprogram the tumor microenvironment, upregulate the expression of PD-1/PD-L1, promote anti-tumor immune response, and activate the immune system.12,23,24 It was confirmed in the preclinical model of HCC, that RT combined with ICI could increase the clinical benefit of the non-irradiated site from 33% to 71%.25 Moreover, in a Phase II clinical trial, the median PFS and OS of patients with unresectable HCC tumors receiving stereotactic body radiotherapy plus camrelizumab were 5.8 and 14.2 months, respectively, and of the 95.2% patients with advanced HCC were 5.8 and 17.4 months, respectively.14 Similarly, the combination of RT and anti‑PD1 achieved a better median PFS of 5.86 months and a trend toward longer median OS of 17.4 months than TACE plus sorafenib among patients with unresectable HCC. Meanwhile, RT plus anti‑PD1 was associated with a significantly better OS than TACE plus sorafenib among patients with BCLC stage C (11.8 vs 9.7 months, P = 0.031).13 Similarly, the feasible efficacy evaluation results showed that the ORR of IMRT combined with anti‑PD1 was 56.99%, the PR rate was 51.61%, and the CR rate was 5.38%, with an encouraging OS of 14.3 months in the present study. IMRT combined with anti‑PD1 seems to have considerable clinical efficacy in the treatment of advanced HCC. However, some patients still do not benefit from the treatment; thus, predictive factors are needed to identify patients with advanced HCC who may benefit from IMRT and anti‑PD1 combination therapy.
Alb reflects liver function and nutritional status and determines the sustainability and prognosis of immunotherapy in patients with HCC. A previous study has shown that the nutritional status of patients with advanced HCC is strongly and positively correlated with the efficacy and survival benefits of anti-PD1 therapy.26 Hypoalbuminemia may lower the systemic immune system and lead to tumor cell proliferation.27 AFP is an effective factor for prognostic and recurrence monitoring of HCC. Clinical data have shown that an AFP > 400ng/mL is associated with poor OS in HCC.28 This study showed that AFP > 400ng/mL was almost statistically significant for poor prognosis of HCC (HR = 1.79, 95% CI:0.99–3.22, P = 0.054). This may be due to the relationship between high AFP levels and the roles of VEGF and VEGFR-2 in angiogenesis and tumor growth promotion.29 Neutrophils play important roles in the occurrence, development, and metastasis of HCC. It has been reported that neutrophils are mainly concentrated in the peritumoral interstitium of liver cancer tissue, and the increase of neutrophils count is averse to HCC treatment and becomes an independent prognostic factor for HCC.30–32 Similarly, the present results showed that neutrophil counts 3–4W > 6.75 * 109/L had a poor prognosis for HCC (P = 0.003). Platelets promote the release of endothelial growth factors and alter the immune environment, enhancing tumor proliferation and invasion.33,34 After RT, lymphocytopenia impairs the immune system.15,35 The inflammatory microenvironment is associated with the occurrence and development of 90% of HCC cases. One analysis of anti-PD1 treatment of HCC found that PLR in the high-value group was associated with poor OS, and the concurrent increase in both was associated with an 8-fold risk of death.36 A high PLR is associated with poor prognosis in patients with unresectable HCC receiving IMRT.15 Similarly, in the present study, PLR and the changes before and after treatment were analyzed, and it was found that the group with a high PLR showed poor prognosis 3–4 weeks after IMRT initiation, making PLR an independent prognostic factor. An elevated PLR may indicate the disruption of immune regulation in the tumor microenvironment, thus predicting a poor prognosis. Inflammatory markers may also serve as predictive prognostic biomarkers for IMRT combined with anti‑PD1 treatment in advanced HCC.
Nomograms have been proven to be more accurate than traditional staging systems in predicting cancer prognosis. Zeng, Pu et al combined multiple inflammatory indicators and clinical parameters such as AFP, PLR, NLR, tumor size, and vascular invasion to construct a nomogram model to predict the prognosis of HCC at 1, 3, and 5 years after resection, which was better than BCLC and the 8th AJCC staging system to predict the prognosis and recurrence of HCC.37,38 In this study, a nomogram model was established by incorporating Alb, AFP, neutrophil count 3–4W and PLR 3–4W as predictors for predicting the OS of patients with advanced HCC for 1, 2, and 3 years. The nomogram predicted the OS supported by the AUC and calibration curves.
While the efficacy has increased, AEs associated with combination therapy also need to be considered. In phase II and III clinical trials of anti‑PD1 for unresectable HCC, 20% of adverse events were grade 3 or 4, with the most common being elevated transaminase levels and decreased neutrophil count.8,10 In this study, the analysis of routine laboratory test results showed similar results: grade 5 AEs were not observed, and 32.35% of the patients had grade 3 or 4 AEs, among which 66.67% had only one grade 3 or grade 4 reaction. Leukopenia, thrombocytopenia, and decreased hemoglobin levels were identified as the main AEs. The safety of IMRT plus anti - PD1 therapy in this population was consistent with that of RT +PD1 in previously reported studies.13,14 However, in IMbrave150 study, grade 3 or 4 AEs occurred in 56.5% of patients treated with atezolizumab plus bevacizumab.6 In summary, no short-term fatal AEs were observed following IMRT and anti-PD1 combination treatment.
This study has several limitations. First, data were obtained from a single institution. Second, renal and thyroid function tests, stool and urine analysis were not performed for all the patients. In addition, we failed to collect symptoms data of the patients themselves, which failed to reveal all the toxic and side effects. Third, because it is not mandatory for patients to provide tumor samples, the lack of samples available for PD-1/PD-L1 testing may be considered a limitation.
Conclusion
This study showed that combination of IMRT with anti‑PD1 achieved encouraging efficacy and tolerable toxicity in the treatment of advanced HCC. The nomogram model established based on Alb, AFP, neutrophils count 3–4W and PLR, is expected to be a clinical tool to predict the prognosis of IMRT combined with anti‑PD1 in the treatment of advanced HCC, which needs further study.
Abbreviations
Anti‑PD1, monoclonal antibodies against programmed cell death 1 pathway; Alb, albumin; AFP, alpha-fetoprotein; AEs, adverse reactions; BCLC, Barcelona Clinic Liver Cancer; CT, computed tomography; CR, complete response; GTV, Gross tumor volume; HCC, Hepatocellular carcinoma; IMRT, intensity-modulated radiotherapy; NLR, neutrophil-to-lymphocyte ratio; OS, overall survival; ORR, overall response rate; PFS, progression-free survival; PR, partial response; PLR, platelet-to-lymphocyte ratio; PTV, planned target volume; RT, radiotherapy; RECIST 1.1, Response Evaluation Criteria in Solid Tumors, version 1.1; SII, systemic immune-inflammation index.
Data Sharing Statement
The data underlying this article will be shared on reasonable request to the corresponding author.
Ethics Approval
The protocol of this retrospective study conformed to the Declaration of Helsinki (1975) and its amendments and was approved by the Ethics Review Committee of the Guangxi Medical University Cancer Hospital (LW2023043), which waived the requirement for written informed consent because patients or their legal guardians had consented, upon admission, to analysis and publication of anonymized medical data for research purposes.
Acknowledgments
We wish to thank all patients involved in this research and our colleagues at Guangxi Medical University Cancer Hospital.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This study was supported by the Self-Raised Scientific Research Fund of the Ministry of Health of Guangxi Province (Z20201371), the Youth Program of Scientific Research Foundation of Guangxi Medical University Cancer Hospital (2021-10), and the Promoting Project of Basic Capacity for Young and Middle-aged University Teachers in Guangxi (2022KY0079).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Llovet JM, Castet F, Heikenwalder M, et al. Immunotherapies for hepatocellular carcinoma. Nat Rev Clin Oncol. 2022;19(3):151–172. doi:10.1038/s41571-021-00573-2
2. Xie DY, Ren ZG, Zhou J, Fan J, Gao Q. 2019 Chinese clinical guidelines for the management of hepatocellular carcinoma: updates and insights. Hepatobiliary Surgery Nutrition. 2020;9(4):452–463. doi:10.21037/hbsn-20-480
3. Zhong JH, Peng NF, You XM, et al. Tumor stage and primary treatment of hepatocellular carcinoma at a large tertiary hospital in China: a real-world study. Oncotarget. 2017;8(11):18296–18302. doi:10.18632/oncotarget.15433
4. Llovet JM, Ricci S, Mazzaferro V, et al. Sorafenib in advanced hepatocellular carcinoma. New Engl J Med. 2008;359(4):378–390. doi:10.1056/NEJMoa0708857
5. Kudo M, Finn RS, Qin S, et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: a randomised Phase 3 non-inferiority trial. Lancet. 2018;391(10126):1163–1173. doi:10.1016/s0140-6736(18)30207-1
6. Finn RS, Qin S, Ikeda M, et al. Atezolizumab plus Bevacizumab in Unresectable Hepatocellular Carcinoma. New Engl J Med. 2020;382(20):1894–1905. doi:10.1056/NEJMoa1915745
7. Chen W, Chiang CL, Dawson LA. Efficacy and safety of radiotherapy for primary liver cancer. Chine Clin Oncol. 2021;10(1):9. doi:10.21037/cco-20-89
8. Zhu AX, Finn RS, Edeline J, et al. Pembrolizumab in patients with advanced hepatocellular carcinoma previously treated with sorafenib (KEYNOTE-224): a non-randomised, open-label Phase 2 trial. Lancet Oncol. 2018;19(7):940–952. doi:10.1016/s1470-2045(18)30351-6
9. Yau T, Hsu C, Kim TY, et al. Nivolumab in advanced hepatocellular carcinoma: sorafenib-experienced Asian cohort analysis. J Hepatol. 2019;71(3):543–552. doi:10.1016/j.jhep.2019.05.014
10. Qin S, Ren Z, Meng Z, et al. Camrelizumab in patients with previously treated advanced hepatocellular carcinoma: a multicentre, open-label, parallel-group, randomised, phase 2 trial. Lancet Oncol. 2020;21(4):571–580. doi:10.1016/s1470-2045(20)30011-5
11. Lee YH, Tai D, Yip C, Choo SP, Chew V. Combinational Immunotherapy for Hepatocellular Carcinoma: radiotherapy, Immune Checkpoint Blockade and Beyond. Front Immunol. 2020;11:568759. doi:10.3389/fimmu.2020.568759
12. McLaughlin M, Patin EC, Pedersen M, et al. Inflammatory microenvironment remodelling by tumour cells after radiotherapy. Nat Rev Cancer. 2020;20(4):203–217. doi:10.1038/s41568-020-0246-1
13. Li JX, Deng WX, Huang ST, et al. Efficacy and safety of radiotherapy plus anti-PD1 versus transcatheter arterial chemoembolization plus sorafenib for advanced hepatocellular carcinoma: a real-world study. Radiat Oncol. 2022;17(1):106. doi:10.1186/s13014-022-02075-6
14. Li JX, Su TS, Gong WF, et al. Combining stereotactic body radiotherapy with camrelizumab for unresectable hepatocellular carcinoma: a single-arm trial. Hepatol Internat. 2022;16(5):1179–1187. doi:10.1007/s12072-022-10396-7
15. Li JX, He ML, Qiu MQ, et al. Prognostic value of a nomogram based on peripheral blood immune parameters in unresectable hepatocellular carcinoma after intensity-modulated radiotherapy. BMC Gastroenterol. 2022;22(1):510. doi:10.1186/s12876-022-02596-0
16. Muhammed A, D’Alessio A, Enica A, et al. Predictive biomarkers of response to immune checkpoint inhibitors in hepatocellular carcinoma. Expert Rev Mol Diagn. 2022;22(3):253–264. doi:10.1080/14737159.2022.2049244
17. Mattos ÂZ, Debes JD, Boonstra A, Vogel A, Mattos AA. Immune aspects of hepatocellular carcinoma: from immune markers for early detection to immunotherapy. World J Gastrointest Oncol. 2021;13(9):1132–1143. doi:10.4251/wjgo.v13.i9.1132
18. Su TS, Li LQ, Liang SX, et al. A Prospective Study of Liver Regeneration After Radiotherapy Based on a New (Su’S) Target Area Delineation. Front Oncol. 2021;11:680303. doi:10.3389/fonc.2021.680303
19. Cheng AL, Guan Z, Chen Z, et al. Efficacy and safety of sorafenib in patients with advanced hepatocellular carcinoma according to baseline status: subset analyses of the Phase III Sorafenib Asia-Pacific trial. Eur J Cancer. 2012;48(10):1452–1465. doi:10.1016/j.ejca.2011.12.006
20. Cheng AL, Qin S, Ikeda M, et al. Updated efficacy and safety data from IMbrave150: atezolizumab plus bevacizumab vs. sorafenib for unresectable hepatocellular carcinoma. J Hepatol. 2022;76(4):862–873. doi:10.1016/j.jhep.2021.11.030
21. Llovet JM, Villanueva A, Marrero JA, et al. Trial Design and Endpoints in Hepatocellular Carcinoma: AASLD Consensus Conference. Hepatology. 2021;73(Suppl 1):158–191. doi:10.1002/hep.31327
22. Rimassa L, Personeni N, Czauderna C, Foerster F, Galle P. Systemic treatment of HCC in special populations. J Hepatol. 2021;74(4):931–943. doi:10.1016/j.jhep.2020.11.026
23. Craciun L, de Wind R, Demetter P, et al. Retrospective analysis of the immunogenic effects of intra-arterial locoregional therapies in hepatocellular carcinoma: a rationale for combining selective internal radiation therapy (SIRT) and immunotherapy. BMC Cancer. 2020;20(1):135. doi:10.1186/s12885-020-6613-1
24. Du SS, Chen GW, Yang P, et al. Radiation Therapy Promotes Hepatocellular Carcinoma Immune Cloaking via PD-L1 Upregulation Induced by cGAS-STING Activation. Int J Radiat Oncol Biol Phys. 2022;112(5):1243–1255. doi:10.1016/j.ijrobp.2021.12.162
25. Sung W, Hong TS, Poznansky MC, Paganetti H, Grassberger C. Mathematical Modeling to Simulate the Effect of Adding Radiation Therapy to Immunotherapy and Application to Hepatocellular Carcinoma. Int J Radiat Oncol Biol Phys. 2022;112(4):1055–1062. doi:10.1016/j.ijrobp.2021.11.008
26. Jiang Y, Tu X, Zhang X, et al. Nutrition and metabolism status alteration in advanced hepatocellular carcinoma patients treated with anti-PD-1 immunotherapy. Support Care Cancer. 2020;28(11):5569–5579. doi:10.1007/s00520-020-05478-x
27. Wang D, Hu X, Xiao L, et al. Prognostic Nutritional Index and Systemic Immune-Inflammation Index Predict the Prognosis of Patients with HCC. J Gastrointest Surg. 2021;25(2):421–427. doi:10.1007/s11605-019-04492-7
28. Lim DH, Casadei-Gardini A, Lee MA, et al. Prognostic implication of serum AFP in patients with hepatocellular carcinoma treated with regorafenib. Future Oncol. 2022;18(27):3021–3030. doi:10.2217/fon-2022-0524
29. Galle PR, Foerster F, Kudo M, et al. Biology and significance of alpha-fetoprotein in hepatocellular carcinoma. Liver Int. 2019;39(12):2214–2229. doi:10.1111/liv.14223
30. Li X, Xing YF, Lei AH, et al. Neutrophil count is associated with myeloid derived suppressor cell level and presents prognostic value of for hepatocellular carcinoma patients. Oncotarget. 2017;8(15):24380–24388. doi:10.18632/oncotarget.15456
31. Hong YM, Yoon KT, Hwang TH, Cho M. Pretreatment peripheral neutrophils, lymphocytes and monocytes predict long-term survival in hepatocellular carcinoma. BMC Cancer. 2020;20(1):937. doi:10.1186/s12885-020-07105-8
32. Poto R, Cristinziano L, Modestino L, et al. Neutrophil Extracellular Traps, Angiogenesis and Cancer. Biomedicines. 2022;10(2). doi:10.3390/biomedicines10020431
33. Bihari C, Rastogi A, Shasthry SM, et al. Platelets contribute to growth and metastasis in hepatocellular carcinoma. APMIS. 2016;124(9):776–786. doi:10.1111/apm.12574
34. Pavlovic N, Rani B, Gerwins P, Heindryckx F. Platelets as Key Factors in Hepatocellular Carcinoma. Cancers. 2019;11(7):1022. doi:10.3390/cancers11071022
35. Sung W, Cho B. Modeling of radiation effects to immune system: a review. j Korean Phys Soc. 2022;81(11):1013–1019. doi:10.1007/s40042-022-00574-z
36. Dharmapuri S, Özbek U, Lin JY, et al. Predictive value of neutrophil to lymphocyte ratio and platelet to lymphocyte ratio in advanced hepatocellular carcinoma patients treated with anti-PD-1 therapy. Cancer Med. 2020;9(14):4962–4970. doi:10.1002/cam4.3135
37. Zeng J, Zeng J, Wu Q, et al. Novel inflammation-based prognostic nomograms for individualized prediction in hepatocellular carcinoma after radical resection. Ann Translat Med. 2020;8(17):1061. doi:10.21037/atm-20-1919
38. Pu T, Li ZH, Jiang D, et al. Nomogram based on inflammation-related markers for predicting survival of patients undergoing hepatectomy for hepatocellular carcinoma. World j Clin Cases. 2021;9(36):11193–11207. doi:10.12998/wjcc.v9.i36.11193
 © 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


