Back to Journals » Therapeutics and Clinical Risk Management » Volume 15
Well leg compartment syndrome in trauma surgery – femoral shaft fracture treated by femoral intramedullary nailing in the hemilithotomy position: case series and review of the literature
Authors Brouze IF , Steinmetz S, McManus J, Borens O
Received 18 June 2018
Accepted for publication 23 November 2018
Published 8 February 2019 Volume 2019:15 Pages 241—250
DOI https://doi.org/10.2147/TCRM.S177530
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Garry Walsh
Iris F Brouze, Sylvain Steinmetz, John McManus, Olivier Borens
Service of Orthopaedic surgery and Traumatology, CHUV – University Hospital Vaud, Lausanne, Switzerland
Abstract: Well leg compartment syndrome (WLCS) is a rare complication which can occur following urological, gynecological, general surgical or orthopaedic surgeries carried out with the lower limb in the hemilithotomy position. WLCS is associated with significant morbidity and mortality because delay in diagnosis and treatment can lead to loss of function and even life-threatening complications. During orthopaedic surgeries on a traction table, such as femoral nailing, the contralateral “well leg” is often placed in the hemilithotomy position, thus facilitating the use of fluoroscopy. This position (also named the Lloyd-Davis position) consists of hip flexion, abduction, external rotation and knee flexion. We present the cases of two teenaged patients who underwent femoral nailing on an extension table of a femoral fracture and developed WLCS. We also present a review of the literature and a discussion of the pathophysiology, risk factors and treatment of this condition. Clinicians need to be aware of the risk factors for WLCS and have high index of suspicion. Further studies looking at the risks, benefits and feasibility of ways to reduce this risk are required.
Keywords: WLCS, well leg compartment syndrome, femoral shaft fracture, intramedullary nailing, hemilithotomy position, case series
Background
Well leg compartment syndrome (WLCS) has been described after urological, gynecological and general surgical procedures where the legs have been positioned in flexion to provide access to the perineum or abdomen. This iatrogenic compartment syndrome was first described by Leff and Shapiro in 1979 following a urological intervention.1
The pathophysiological mechanism is perioperative hypoperfusion leading to ischaemia and capillary permeability, followed by reperfusion injuries in the postoperative phase linked to interstitial edema secondary to capillary leakage and the release of inflammatory factors as a result of the ischaemia.
According to Halliwill, who analyzed the preliminary data of a retrospective study of cases at the Mayo Clinic, WLCS occurs in approximately one in 3,500 interventions using the classical lithotomy position.2
WLCS has been less frequently described in orthopedic and trauma surgery. During intramedullary (IM) nailing for femoral fractures the contralateral “well leg” is placed with the hip in flexion abduction, with flexion of the knee and the ankle loose, known as the hemilithotomy position (Figure 1).
  | Figure 1 Positioning scheme of the legs in the hemilithotomy position. (IF Brouze). |
We present the cases of two teenaged patients who underwent femoral nailing of a femoral fracture and developed WLCS. We also present a review of the literature and discussion of the pathophysiology, risk factors and treatment of this condition.
Case reports
We confirm that all patients involved were contacted and were given information about the use of their data for scientific purposes including this publication for which they signed a written consent form.
Case number 1
A 19-year-old male driver, Body Mass Index (BMI) 25.7 kg/m2 without medical history of note, who was admitted following a motor vehicle accident.
The workup revealed an open diaphyseal wedge fracture of the left femur (AO 33-A3, Gustilo II) and a suprapatellar traumatic arthrotomy of the right knee.
The patient was brought to the operating room within 6 hours, and under general anesthetic underwent debridement of the right knee followed by IM nailing of the left femur. In total, the intervention lasted 6 hours, and was carried out in two distinct stages.
The first part of the operation was the exploration, debridement and washout of the right knee, with the left leg placed flat on the operating table without traction.
The second stage was the reduction and IM nailing of the left femur lasting 4 hours, with the right leg placed in the hemilithotomy position (Figure 1) at a height of approximately 40–60 cm above the level of the right atrium. The intervention was longer than usual as we had to extract bony fragments from IM canal.
The patient presented an episode of hypotension with 70 mmHg systolic and responded to 500 mL of Ringer’s lactate. The mean arterial blood pressure fluctuated between 84 and 112 mmHg. The patient received noradrenaline throughout the procedure (between 1 and 5 μg/minute).
In total, the patient received 3 units of FFP, 2 g of tranexamic acid, 2 g of fibrinogen, 3 L of crystalloids, 1 L of colloids and 2.2 g of co-amoxicillin. Blood loss was estimated at 2 L with 480 mL recuperated using a cell saver.
Two hours after the end of the intervention, the patient presented severe pain in the right lower leg, associated with induration. The intramuscular pressures were taken with an arterial catheter OR Centurion© intra-compartmental pressure monitor (Centurion Medical Products, Williamston, MI, USA). They were measured in the right lower leg at 34 mmHg in the anterior compartment, 105 mmHg in the superficial posterior compartment, 95 mmHg in the deep posterior and 54 mmHg in the lateral compartment.
Four hours after the onset of the symptoms, the patient underwent emergent fasciotomy of the four compartments using the two-incision technique. The incisions subsequently underwent staged secondary closure (complete closure at day 3 for the external wound and day 6 for the internal wound) with uncomplicated evolution.
At the 5-month follow-up, the patient did not have any problems or complaints following the fasciotomies and the left femoral fracture had healed well. The patient was able to return to work at 6 months post-op without any loss of strength or problems during sport.
Case number 2
A 17-year-old male, BMI 21.2 kg/m2 without previous medical problems was admitted following a skiing accident.
The workup showed a closed right femoral fracture (AO 32-C1), an undisplaced right acetabular anterior wall fracture, a fracture of the left posterosuperior alar wing and fractures of the left transverse spinous processes of L2 and L3. He also presented a left rib fracture, fracture of the ulnar styloid, scaphoid and the base of the fourth and fifth metacarpals. There was also a right maxillary fracture and fracture of the right orbit. The workup also revealed an amount of perihepatic fluid.
The patient was brought to the operating room approximately 12 hours after his arrival for an exploratory laparoscopy, followed by reduction and osteosynthesis of the femoral fracture. The laparoscopy lasted approximately 45 minutes and did not reveal any lesions. Reduction and fixation of the right femur lasted 4 hours and 49 minutes during which the patient was positioned in the hemilithotomy position (Figure 1) with the left leg at a height of 30–55 cm above the level of the right atrium, with the right leg under traction using a boot and traction table.
The patient presented two hypotensive episodes, in which both responded to 25 μg of ephedrine and perfusion of Ringer’s lactate during the laparoscopy. During the reduction and nailing of the right femur, the patient presented six hypotensive episodes with a systolic blood pressure below 90 mmHg: at the time of incision, then subsequently at 20, 50, 70, 110, and 230 minutes, which responded to noradrenaline and perfusion of Ringer’s lactate.
The patient received a total of 1,000 μg of noradrenaline and 25 μg of ephedrine, 4 L of Ringer’s lactate, 1 g of tranexamic acid and a total of 2,250 mg of cefuroxime. Blood loss was negligible during the laparoscopy and estimated at 900 mL during the orthopedic portion of the operation.
One hour after the end of the intervention, the patient presented swelling of the left lower leg, accompanied by severe pain resistant to treatment by morphine and exacerbated by passive mobilization of the big toe. We felt that the clinical diagnosis was sufficiently clear and did not carry out pressure measurements of different compartments. The patient rapidly underwent fasciotomies of the four compartments by the two-incision technique, with staged secondary closure (internal closure at day 2 and external closure at day 5 without closing the fascia) without complications.
Four months following the injury, the patient had fully recovered from the compartment syndrome and had good healing of his fractures.
Discussion
Analysis of the literature (Table 1)
The first cases of WLCS published in the orthopedic literature were published by Lieutenant Dugdale et al in 1989.3 Table 1 is a review of the literature from the last 30 years.
  | Table 1 Our review of case reports in the literature |
The information provided on the cases presented in the literature is rarely complete. The BMI,3–8 intramuscular pressure measurements,3–6,9,10 time delay until presentation of symptoms of WLCS,3 the side4 or the height of the limb,3–11 are not systematically recorded.
Much of this information, such as intramuscular pressure measurements are not necessary to be able to establish the diagnosis,12 but provide more precise information as to which compartments are most likely affected by WLCS, depending on the position adopted.
Other comorbidities such as arterial or venous problems and perioperative hypotension are not published and could play a role in the development of WLCS.
Duration of surgery
It is impossible to define precisely when exactly WLCS develops.
The first cases of WLCS published in the orthopedic literature were of femoral nailing with long surgical durations (up to 6 hours),3 however, we found large variation with values from 2 hours 30 minutes to 7 hours 30 minutes.10,13
Raza et al reported a significant increase in the risk of WLCS in operations lasting more than 4 hours,14 and von Keudell et al mentioned that when ischaemia persists for more than 6 hours, irreversible changes are likely to occur, causing an irreversible, inflammatory cascade that results in fibrosis in necrotic muscle tissue, which causes further functional impairments, such as contracture.12
Tan et al measured the evolution of intramuscular pressure in the anterior and deep posterior compartments in the uninjured leg of patients undergoing femoral nailing.15 He showed that the intramuscular pressure increased when the leg was placed on the support and that the pressure increased by an average of 1.1 mmHg/hour.
The majority of authors suggest that mobilization of the unaffected leg every 2 hours; a similar timeframe to the commonly accepted maximal duration of a tourniquet. One author recommends mobilization every 2 hours for interventions lasting over 4 hours,14 however, other authors recommend mobilization every 2 hours regardless of the total duration of the surgery.9,13,15,16
Position
Christodoulou et al recommended the use of leg supports (described as Göpel supports) with the ankle free, instead of the use of boots immobilizing the ankle.5 This technique has not completely eliminated the risk of WLCS, as shown by our two case reports (Figure 2) and other cases reported in the literature.6,7,9,10
  | Figure 2 Göpel type support, example of which was used for our cases photography taken by the authors in the Operation room with authorization of the heads of department and the institution. |
The height to which the leg is elevated may also have an effect on the development of WLCS. Matsen showed that for each centimeter of increased elevation of the leg, the local arteriolar pressure decreases by 0.78 mmHg.17
Positioning of the limb using a Göpel type support significantly increases the intramuscular pressure and thus decreases the perfusion pressure as described by Meyer et al, who carried out dynamic pressure measurement of pressures in each compartment of the leg in healthy subjects when lying flat, compared to when positioned on a classical leg support.18
The height of the limb and the use of a support worsens the perfusion by increasing the intramuscular pressure and reducing the perfusion pressure. These physiological changes show that the positioning of the leg and the use of supports can have important effects on the development of WLCS.
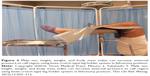
Bible and Mir suggested an alternative to positioning the patient in abduction with elevation of the uninjured leg.19 Their aim was to find the safest position for the leg without hindering the use of radioscopy for the intervention. They suggest positioning the leg, without the use of an intermittent compression boot, along the traction bar of the table for the unaffected leg. They used cushions between the bar and the limb, and attached the limb using bandages (Figure 3). This technique was used for 93 interventions over the period of 2 years and 4 months, including 14 percutaneous fixation of femoral neck fractures, 8 with plate/screw type implants for intertrochanteric or subtrochanteric fractures, 37 IM nailing for femoral shaft fracture. They did not report any difficulties concerning the manipulation of the radioscopy and noted the absence of perioperative complications. They also reported that they did not have to move the unaffected leg during the procedure. However, they did not describe the characteristics of the patient group. They mention success of this procedure in polymorbid obese patients without further discussion. The question whether the use of this technique is appropriate in patients with thromboembolic disorders remains unclear.
  | Figure 3 Well leg positioning on a fracture table: using a pillow sling. |
Diagnosis and pertinence of intramuscular pressure measurement
The diagnosis of WLCS can be made clinically, but also supported by a reduced perfusion pressure, which is the difference between the diastolic blood pressure and the intramuscular pressure.
McQueen and Court-Brown evaluated 116 patients with a fractured tibia, using continuous intramuscular pressure monitoring.20 He described a delta value = [diastolic arterial blood pressure − intramuscular pressure] of lower than or equal to 30 mmHg as a cut-off value for ischaemia and thus an indication for fasciotomy. He carried out four compartment fasciotomies on all patients with a delta value ≤30 mmHg. None of his patients, either operated or unoperated, suffered from complications of compartment syndrome.
This cut-off value was correlated by Meyer et al, who observed pathological delta values (between 4.1 and 23.7 depending on the compartment) when a classical support was used.18 However, the delta value was shown to increase (between 26 and 35.1 mmHg) when the leg was supported at the ankle and the knee, leaving the calf unsupported.
These values were also confirmed in 2015 when von Keudell et al, writing in The Lancet proposed guidelines on the diagnosis and treatment of compartment syndrome based on the current literature.12 The diagnostic methods used for a suspicion of WLCS are the same as for any suspected compartment syndrome. von Keudell et al mentioned that the diagnosis of compartment syndrome can be made on the basis of symptoms and/or based on intramuscular pressure measurements.
The principal symptoms are excessive limb pain, pain on passive stretching of the compartment, paraesthesia and paresis.12 We also commonly consider pain out of proportion that is not relieved by suitable painkillers. The subjective examination of a distended compartment is insufficient and unreliable to establish the diagnosis.12 Neurovascular symptoms are known for their late onset.
In cases where there is doubt, intramuscular pressure measurement can be carried out using a catheter. Such measurements need to be carried out in all compartments of the segment of the limb in order to confirm the absence of a compartment syndrome. One normal value in one compartment is not sufficient. The range of normal values is between 0 and 10 mmHg.14,21
A delta value of lower than or equal to 30 mmHg confirms the diagnosis of compartment syndrome.20 The question of the absolute values of intramuscular pressure remains controversial as the oxygenation of the tissues is partly dependent on the blood pressure of the patient.12
Pain that cannot be relieved by adequate pain relief, or a delta value lower than or equal to 30 mmHg are both sufficient to justify the diagnosis of compartment syndrome and justify emergent fasciotomy of the affected segment of the limb.
BMI
Peters et al presented two cases of WLCS associated with pelvic surgery and carried out a study into the arterial blood pressure in healthy volunteers.22 He used a blood pressure cuff and an ultrasound to measure the blood pressure at the ankle in the standard positions used for colorectal surgery. The results suggest a highly significant correlation (P<0.01) between those patients who are overweight (BMI >25 kg/m2) and reduced ankle blood pressure while in the Lloyd-Davis position.
Tan et al showed a significant correlation between the BMI and the intramuscular pressure measurements.15 He used catheters in two compartments of the healthy leg to measure the intramuscular pressures, with the leg flat, then while placed in the hemilithotomy position, then afterward when placed flat again. These measurements were carried out in 10 patients undergoing IM nailing of the contralateral femur, with the unaffected leg on a leg support.
They found a significant correlation between the BMI and leg pressure during the continuous pressure monitoring. These records were achieved with in-dwelling slit catheters inserted into the calf compartments of the well leg at baseline (supine position), during hemilithotomy position and post-hemilithotomy with 10 patients who underwent IM nailing of a fractured femur in the hemilithotomy position (with a well leg holder). No threshold value of BMI was reported as being significantly at risk.
Meyer et al carried out a similar study in which they measured the dynamic intramuscular pressures in healthy subjects positioned on a classic leg support compared to a support at the ankle and knee with the calf free.18 Contrary to Tan et al’s findings,15 Meyer et al did not find a correlation between the BMI and the intramuscular pressures measured in the different positions.18
Mizuno and Takahashi studied the relationship between the external pressure applied to the leg and certain physical characteristics.21 The external pressure measurement was a noninvasive alternative to intramuscular pressure measurements. Twenty-one Japanese volunteers aged between 20 and 22 years and in good general health, with an average BMI of 21.4 kg/m2 took part in the study. Diabetics and those with neuromotor problems were excluded. The team used a knee crutch-like holder which corresponds to the support used in our cases (Figure 4) on which they placed a pressure-sensitive measuring mat (BIG-MAT) which was used to measure the evolution of external pressure applied to the leg as time progressed. The volunteers were placed with both legs at 90° of hip flexion, 40° of external rotation and 20° of abduction with the knees at 90° flexion. They noted a correlation between the pressures measured and the BMI. These external pressure measurements were not correlated with intramuscular measurements. No cut-off value of BMI was suggested as being significantly at risk.
Treatment
Hutton et al showed in 1982 that mannitol could be used to reduce the intramuscular pressures when used in a canine model.23 He also administered the mannitol to a patient with an intramuscular pressure measurement of 110 mmHg in the anterolateral compartment. The treatment was successful and they avoided carrying out a fasciotomy. Another American study carried out by a team of vascular surgeons suggested the use of mannitol to treat reperfusion injuries to lower the number of fasciotomies, however, the study was carried out in 1996.24 Mannitol reduces vascular resistance, increases the circulating blood volume, vasodilates the kidneys and reduces the number of free radicals. The current literature remains vague on the use of mannitol vs fasciotomy to treat compartment syndrome.
The only reliable treatment to reduce intramuscular pressure remains a fasciotomy.
The literature remains divided over the recommended technique. The majority of surgeons prefer a four-compartment fasciotomy using a two-incision technique, with the argument that the deep posterior compartment is easier to locate and therefore release successfully. Maheshwari et al carried out a retrospective study on fasciotomies carried out by the single incision technique in cases with a fractured tibia.25 There were 58 fasciotomies carried out over 6 years. There were three deaths because of their associated injuries and 29 debridements; however, there were no cases which had to be revised because of insufficient compartment release. The advantage of this technique is the single incision, but the compartments are more difficult to identify and there is the risk of damage to the superficial peroneal nerve.
From our experience, we recommend the two-incision technique. In every case, decompression of the four compartments must be carried out according to von Keudell et al and McQueen and Court-Brown.12,20
The treatment must be carried out without delay to reduce further damage to the tissues such as irreversible neurovascular damage, tissue necrosis or even gangrene. The dissemination of creatine kinase can also induce acute renal failure.14 To prevent this we recommend aggressive fluid resuscitation and alkalization of the urine to prevent the precipitation of myoglobin.6
Recommendations
Following our cases and based on our review of the literature, we have developed the following practical guidelines:2,5,14,16
- Every patient whose surgery lasts more than 2 hours must be considered at risk of developing WLCS.
- Reduce the time in the hemilithotomy position to a minimum. Complete the installation by placing the uninjured leg on the support last, just before fracture reduction under radioscopic control.
- Reduce the flexion of the hip and knee in order to place the limb as close as possible to the level of the right atrium. Measure the height of the lower limb compared to the anteroposterior midpoint of the thorax.
- Mobilize the uninjured leg every 2 hours.
- Avoid the Trendelenburg position.
- Avoid hard supports at the level of the knee or calf. Keep the ankle free. Avoid compressive bandages.
- Avoid hypovolemia before, during and after the intervention.
- Avoid vasoconstrictors.
- Inform nursing staff and junior colleagues of the recommendations and of the first signs of compartment syndrome.
- Never delay a fasciotomy.
We recommend systematically recording the following information in cases of WLCS.
- Age, sex, BMI.
- AO classification of the fracture, with side of injury.
- Precise description of the installation with height of the leg above the right atrium.
- Precise description of the operation carried out, with duration of each step, and of the delay before surgery.
- Monitoring of arterial pressure during the intervention and the steps taken to correct it.
- Precise description of the fasciotomy carried out (number of incisions, compartments released) as well as any further treatment carried out.
- Description of the evolution and outcome at follow-up.
Conclusion
WLCS is rare, but knowledge of the pathophysiology is essential to rapidly recognize this important complication and prevent the potentially irreversible complications. There are still reported cases despite the fact that WLCS is preventable.
The diagnosis is primarily clinical, based on pain resistant to pain relief, and can be confirmed by intramuscular pressure measurements in case of doubt.
Patient positioning, operation duration and patient BMI are all contributing factors.
Following our analysis of the literature, we have proposed guidelines to reduce the occurrence of WLCS. We regret the lack of precision in the reporting of previous cases of WLCS, and we propose a set of criteria which we feel are essential to future publications on the subject.
Approval statement
This case series was approved by the institutional department head at University Hospital Vaud, Department of Musculoskeletal Health, Orthopedics and Traumatology, Avenue Pierre Decker 4, CH-1011 Lausanne, Switzerland.
Disclosure
The authors report no conflicts of interest in this work.
References
Leff RG, Shapiro SR. Lower extremity complications of the lithotomy position: prevention and management. J Urol. 1979;122(1):138–139. | ||
Halliwill JR, Hewitt SA, Joyner MJ, Warner MA. Effect of various lithotomy positions on lower-extremity blood pressure. Anesthesiology. 1998;89(6):1373–1376. | ||
Dugdale TW, Schutzer SF, Deafenbaugh MK, Bartosh RA. Compartment syndrome complicating use of the hemi-lithotomy position during femoral nailing. A report of two cases. J Bone Joint Surg Am. 1989;71(10):1556–1557. | ||
Anglen J, Banovetz J. Compartment syndrome in the well leg resulting from fracture-table positioning. Clin Orthop. 1994;301:239–242. | ||
Christodoulou M, Garofalo R, Echeverri S, Pelet S, Mouhsine E. Hemilithotomy position for intramedullary nailing of the femur and compartment syndrome of the healthy leg. Swiss Surg. 2002;8(4):193–196. | ||
Carlson DA, Dobozi WR. Rabin S. Peroneal nerve palsy and compartment syndrome in bilateral femoral fractures. Clin Orthop Relat Res. 1995;320:115–118. | ||
Adler LM, Heppenstall RB, Esterhai JL. Compartment syndrome in the well leg: a complication of the hemilithotomy position. Techn Orthop. 1997;12(2):133–135. | ||
Meldrum R, Lipscomb P. Compartment syndrome of the leg after less than 4 hours of elevation on a fracture table. South Med J. 2002;95(2):269–271. | ||
Noordin S, Allana S, Wajid MA. Well leg compartment syndrome: the debit side of hemilithotomy position. J Ayub Med Coll Abbottabad. 2009;21(1):166–168. | ||
Meena S, Trikha V, Saini P, Kumar N, Kr S. Well-leg compartment syndrome after fracture fixation in hemilithotomy position: case report of a preventable condition. Med Princ Pract. 2014;23(3):275–278. | ||
Weber O, Kabir K, Goost H, Wirtz DC, Burger C. The “well-leg” syndrome: calf compartment after lithotomy position. Z Orthop Unfall. 2008;146(2):261–263. German. | ||
von Keudell AG, Weaver MJ, Appleton PT, et al. Diagnosis and treatment of acute extremity compartment syndrome. The Lancet. 2015;386(10000):1299–1310. | ||
Mathews PV, Perry JJ. Murray PC. Compartment syndrome of the well leg after less than 4 hours of elevation on a fracture table. J Orthop Trauma. 2001;15(8):580–583. | ||
Raza A, Byrne D, Townell N. Lower limb (well leg) compartment syndrome after urological pelvic surgery. J Urol. 2004;171(1):5–11. | ||
Tan V, Pepe MD, Glaser DL, Seldes RM, Heppenstall RB, Esterhai JL Jr. Well-leg compartment pressures during hemilithotomy position for fracture fixation. J Orthop Trauma. 2000;14(3):157–161. | ||
Bauer ECA, Koch N, Janni W, Bender HG, Fleisch MC. Compartment syndrome after gynecologic operations: evidence from case reports and reviews. Eur J Obstet Gynecol Reprod Biol. 2014;173:7–12. | ||
Matsen FA 3rd. A practical approach to compartmental syndromes. Part I. Definition, theory, and pathogenesis. Instr Course Lect. 1983;32:88–92. | ||
Meyer RS, White KK, Smith JM, Groppo ER, Mubarak SJ, Hargens AR. Intramuscular and blood pressures in legs positioned in the hemilithotomy position: clarification of risk factors for well-leg acute compartment syndrome. J Bone Joint Surg Am. 2002;84-A(10):1829–1835. | ||
Bible JE, Mir HR. Well-leg positioning on a fracture table: using a pillow sling. Am J Orthop (Belle Mead NJ). 2014;43(12):571–573. | ||
McQueen MM, Court-Brown CM. Compartment monitoring in tibial fracture: the pressure threshold for decompression. J Bone Joint Surg Br. 78(1):99–104. | ||
Mizuno J, Takahashi T. Male sex, height, weight, and body mass index can increase external pressure to calf region using knee-crutch-type leg holder system in lithotomy position. Ther Clin Risk Manag. 2016;12:305–312. | ||
Peters P, Baker SR, Leopold PW, Taub NA, Burnand KG. Compartment syndrome following prolonged pelvic surgery. Br J Surg. 1994;81(8):1128–1331. | ||
Hutton M, Rhodes RS, Chapman G. The lowering of postischemic compartment pressures with mannitol. J Surg Res. 1982;32(3):239–242. | ||
Shah DM, Bock DE, Darling RC 3rd, Chang BB, Kupinski AM, Leather RP. Beneficial effects of hypertonic mannitol in acute ischemia – reperfusion injuries in humans. Cardiovasc Surg. 1996;4(1):97–100. | ||
Maheshwari R, Taitsman LA, Barei DP. Single-incision fasciotomy for compartmental syndrome of the leg in patients with diaphyseal tibial fractures. J Orthop Trauma. 2008;22(10):723–730. |
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.