Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 10
Visceral-to-subcutaneous fat ratio as a predictor of the multiple metabolic risk factors for subjects with normal waist circumference in Korea
Authors Oh YH, Moon JH, Kim HJ , Kong MH
Received 5 September 2017
Accepted for publication 17 November 2017
Published 11 December 2017 Volume 2017:10 Pages 505—511
DOI https://doi.org/10.2147/DMSO.S150914
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Ming-Hui Zou
Yun Hwan Oh,1,2 Ji Hyun Moon,1,2 Hyeon Ju Kim,1,3 Mi Hee Kong1,3
1Department of Family Medicine, Jeju National University Hospital, 2Department of Medicine, Graduate School of Jeju National University, 3Department of Family Medicine, School of Medicine, Jeju National University, Jeju, Republic of Korea
Purpose: Visceral obesity has been recognized as a predictor of metabolic risk factors. However, few studies have evaluated the metabolic risks in subjects with normal waist circumference (WC). We aimed to examine if the visceral-to-subcutaneous fat ratio (VSR) has diagnostic value to identify multiple metabolic risk factors in subjects with normal WC, compared with visceral fat area (VFA) and subcutaneous fat area (SFA).
Methods: This is a cross-sectional study in which we have compared mean VFA, SFA, and VSR according to each metabolic risk factor. We performed a receiver operating characteristic (ROC) curve analysis for VFA, SFA, and VSR to assess their accuracy in picking out two or more non-adipose factors for metabolic syndrome.
Results: For each metabolic risk factor, mean VSRs were significantly different between groups (risk-absent group vs risk-present group) in men and women, except for men with low high-density lipoprotein. However, mean VFAs and SFAs showed no significant differences between groups. VSR showed superior diagnostic values in predicting at least two non-adipose metabolic risk factors in men and similar diagnostic value in women. Areas under ROC curves for VSR and VFA were 0.705 and 0.649 in men (P=0.028) and 0.798 and 0.785 in women (P=0.321).
Conclusion: For men with a normal WC, VSR appeared to effectively predict the presence of multiple metabolic risk factors. Thus, VSR may serve as an indicator for identifying men who have a normal WC and multiple metabolic risk factors.
Keywords: visceral fat, subcutaneous fat, metabolic syndrome, visceral-to-subcutaneous fat ratio
A Letter to the Editor has been received and published for this article.
Introduction
With increasing concerns for obesity because of its reported relationship with risks of developing adverse cardiovascular events and metabolic illnesses, how to define obesity has become an issue to be established. There are known sex differences in body fat distribution, fat metabolism, and health risks from obesity and metabolic syndrome.1,2 Based on accumulated evidence, abdominal obesity has been proven to be more closely associated with cardiovascular and metabolic disorders than general obesity in both sexes.3–7
Subsequently, methods to reflect abdominal obesity have been explored using anthropometric measures, such as waist circumference (WC). In clinical settings, WC is apparently preferred not only because of its great simplicity but also because of its proven accuracy as a reliable predictor for identifying subjects with metabolic aberrance and cardiovascular diseases.8–11
Recently, visceral obesity has been identified as an important factor in the development of metabolic disorders.12 Several studies have reported that visceral obesity is closely related to metabolic risk factors, including hypertension, impaired glucose tolerance, dyslipidemia, and other cardiovascular risk factors.13,14 In defining obesity and its validity to predict metabolic risks, focus has changed from central obesity to visceral obesity.
Of several measurements of abdominal visceral fat accumulation, visceral fat area (VFA) using computed tomography (CT) scan of the abdomen was explored extensively for its usefulness in predicting the presence of metabolic risk factors.15–19 On the other hand, considering the differences of body frame size or shape among people, it seems that the absolute amount of visceral fat may not fully reflect such differences while defining visceral obesity. For this reason, theoretically, visceral-to-subcutaneous fat ratio (VSR) would be a better index to allow evaluating a person’s build. Back in 1987, Fujioka et al20 showed the correlation between visceral fat accumulation represented by VSR and glucose or lipid metabolism in obese subjects; the study introduced the cut-off point of 0.4 for VSR, above which individuals with obesity are likely to show glucose intolerance and hyperlipidemia. Recently, Kim et al17 demonstrated diagnostic accuracy of VFA in predicting metabolic risk factors in Koreans and briefly addressed VSR being inferior to VFA in terms of predictability with its cut-off points. Regarding the association between various metabolic components and visceral obesity, previous studies21–23 have revealed specific relationships between various factors and visceral obesity. However, the predictability of VSR in identifying individual non-adipose components of metabolic syndrome has never been addressed in the Korean population.
While WC remains a fascinating tool to be used in clinical practice, it has limitations as it cannot distinguish between visceral and subcutaneous fat deposits in the abdomen. Therefore, if WC is used as the only evaluation index for visceral obesity, potential metabolic risk factors of participants with normal WC may be overlooked. According to previous research conducted in Iran, about 9.9% of men with a normal WC have metabolic syndrome.24 Another study also showed that 10% of men and 3.1% of women with metabolic syndrome have a WC within the normal range.25 As a result, assessing visceral obesity is particularly important in subjects with normal WC because these subjects are sometimes easily considered as having low metabolic risk.
In this context, the aim of this study was to examine whether VFA, subcutaneous fat area (SFA), and VSR in particular have a diagnostic value in identifying individuals who have a WC within the normal range and multiple metabolic risk factors.
Methods
Study subjects
From the Koreans who spontaneously attended the health promotion center in a local university hospital for their routine health examination from June 1, 2012 to April 30, 2017, we selected those who underwent a CT scan of the abdomen as well as ordinary examinations, for this cross-sectional study. Participants completed a medical history questionnaire, responding to questions about previously diagnosed diseases, prescribed medications, and other topics. Then, they underwent anthropometric evaluation, laboratory tests, and CT scan of the abdomen. Participants with abnormal WC were excluded from the study.
Anthropometric measurements
Participants who were fasting underwent anthropometric evaluations: weight, height, and WC. Weight was measured using calibrated electronic scales while subjects wore light clothing and no shoes; height was obtained by a fixed stadiometer; WC was measured at the level of umbilicus while participants were standing. Body mass index (BMI) was calculated as weight in kilograms divided by the height in meters squared. Blood pressure (BP) was measured using an automatic digital BP monitor FT-700R (Jawon Medical Co. Ltd., Seoul, South Korea) while participants were comfortably seated after resting for least 10 min and refraining from smoking and ingesting caffeine.
Definition of metabolic syndrome and multiple metabolic risk factors
We excluded WC and defined multiple metabolic risk factors as having two or more of the following components of metabolic syndrome according to the modified National Cholesterol Education Program Adult Treatment Panel III:11 fasting blood sugar (FBS) ≥100 mg/dL or taking medication for previously diagnosed diabetes; BP ≥130/85 mmHg or taking medication for previously diagnosed hypertension; serum triglyceride (TG) ≥150 mg/dL; and serum high-density lipoprotein (HDL)-cholesterol <40 mg/dL in men or <50 mg/dL in women. We referred to these factors as hyperglycemia, high BP, high TG, and low HDL-cholesterol, respectively.
Determination of VFA, SFA, and VSR using CT scan of the abdomen
Abdominal visceral and subcutaneous fat amounts were determined using a single-slice CT scan (SOMATOM Definition; Siemens, Munich, Germany), 5 mm thickness, at the L4–5 intervertebral space level with subjects in supine position. SFA and VFA were defined by delineating these areas with a graph pen. Both fat areas were determined by identifying fat surface with attenuation range of −140 to −40 Hounsfield units. VSR was finally calculated using the obtained data.
Statistical analysis
All statistical analyses were conducted with SPSS for Windows version 20.0 (IBM, Armonk, NY, USA) and STATA version 13.0 (StataCorp., College Station, TX, USA). The P-values of all the reported results were two-tailed, and the significance level was set at P<0.05.
First, all the subjects were divided by sex. To compare the basic demographic characteristics, the continuous variables were expressed as means and standard deviations and compared through independent t-test. The categorical variables were expressed as percentages and compared by using the c2 test.
Second, the subjects were divided into two groups according to the presence or absence of each metabolic risk factor (hyperglycemia, high BP, high TG, and low HDL-cholesterol), at least two metabolic risk factors, and metabolic syndrome. Mean VFA, SFA and VSR were calculated. Values were adjusted for age and BMI to control for the effects of the body frame size and aging; differences in adjusted mean VFA, SFA, and VSR between the groups were tested. Additionally, differences in mean VFA, SFA, and VSR between the two groups according to the presence or absence of each metabolic risk factor, at least two metabolic risk factors, and metabolic syndrome were analyzed by independent t-test.
Third, binary logistic regression analysis was used to evaluate the relationship between variables (VFA, VSR, and SFA) and the presence of multiple metabolic risk factors. With a receiver operating characteristic curve, we assessed the predictive accuracy of VFA, SFA, and VSR in identifying individuals with at least two metabolic risk factors. Subsequently, area under curve (AUC) was used to quantify the accuracy of each test.
Ethical approval
The Institutional Review Board of the Jeju National University Hospital approved the design of the present study and ensured that individuals were not identifiable by providing linkable anonymous data to the researchers. Waiver of informed consent for this study was approved by the Institutional Review Board, and the study was approved (Approval No. 2017-04-014) after it was reviewed for ethical issues.
Results
Baseline characteristics of subjects
The mean age of men and women was 52.1±9.9 and 50.6±9.7 years, respectively. Likewise, there were no significant differences between sexes in total cholesterol and number of subjects with metabolic syndrome. However, men showed significantly higher values of BMI, WC, systolic BP, diastolic BP, TG, FBS, VFA, and VSR than women. As for HDL-cholesterol and SFA, women showed higher values than men. Compared to women, there were higher numbers of men taking antihypertensive medications or oral hypoglycemic agents and with at least two risk factors other than central besity (Table 1).
Analyses of adjusted mean VFAs, SFAs, and VSRs according to the presence of metabolic risk factors
Among men, no significant differences were observed in adjusted mean VFA and SFA according to the presence or absence of each metabolic risk factor, multiple metabolic risks, and metabolic syndrome. On the contrary, groups with metabolic risk factors except low HDL-cholesterol showed significantly higher adjusted mean VSR than groups without risk factors.
Among women, groups with the presence of high BP, hyperglycemia, at least two risk factors, and metabolic syndrome showed significantly higher adjusted mean VFA than groups without risk factors. There were no significant differences in mean SFA between groups. Regarding VSR, there were significant differences between the groups according to the presence of metabolic risk factors (Table 2).
AUCs for VFA, SFA, and VSR to predict multiple metabolic risk factors
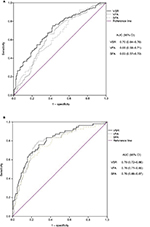
Based on logistic regression analysis, after adjusting for age and BMI, VSR appeared to be an independent predictor of the presence of multiple metabolic risk factors in both men and women (b=1.42, P<0.001; b=2.51, P<0.001, respectively). However, VFA served as a predictor only in women (b=0.01, P=0.034). The AUCs of VSR, VFA, and SFA were 0.705 (95% CI 0.645–0.764), 0.649 (95% CI 0.587–0.712), and 0.636 (95% CI 0.573–0.699) in men and 0.798 (95% CI 0.729–0.867), 0.785 (95% CI 0.716–0.855), and 0.763 (95% CI 0.688–0.838) in women. In men, VSR was superior to VFA (P=0.028). It also seemed that VSR was superior to VFA in women, but it was not statistically significant (P=0.321) (Figure 1).
Discussion
Our study showed differences in adjusted mean VFA, SFA, and VSR according to the status of each metabolic risk factor; our study also compared VFA, SFA, and VSR of subjects with normal WC in association with the presence of metabolic risk factors. Additionally, we evaluated the diagnostic value of VSR to predict multiple metabolic risk factors and proved that it was superior to VFA in this regard.
WC or BMI, commonly used as an indicator for predicting metabolic risk, is a powerful and convenient tool to use, but it varies widely according to the individual’s body frame size and provides little or no information regarding the relative distribution of body fat, especially visceral adiposity. Moreover, some studies have reported that subcutaneous fat tissue might have protective effects against cardiovascular disease.26,27 Obviously, there were some limitations in using WC as a representative index to predict cardiovascular and metabolic risks. Especially in subjects with normal WC and metabolic risk factors, using WC as an index for diagnosing metabolic syndrome can be disadvantageous.
For these reasons, VFA might be an alternative to accurately measure the visceral adipose tissue of the body, but it is also affected by the individual’s body frame size, such as their height, weight, WC, and BMI.28 As a result, it is hard to apply VFA in individuals with diverse body types. Moreover, it cannot fully represent the individual’s propensity to store fat viscerally or subcutaneously because it only suggests absolute amounts of single fat deposits and does not reflect relative distribution of fat in the body. In this respect, our hypothesis was that VSR could represent an individual’s propensity to store fat and be less affected by body type than VFA.
In this respect, our study showed that VSR has diagnostic value as a unique indicator to predict multiple metabolic risk factors regardless of the subject’s age and BMI. After adjusting for age and BMI, mean VSRs were significantly different between groups according to each metabolic risk factor, except for low HDL-cholesterol in men. However, mean VFAs and SFAs showed no significant differences between groups. When we compared mean VFAs, some differences between groups were found in women. Additionally, the diagnostic value of VSR was higher than VFA in men, but similar in women. These findings implicated that the propensity for visceral fat deposits (as opposed to subcutaneous) is associated with metabolic risk factors regardless of age and BMI.
Diagnostic value of VSR to predict multiple metabolic risk factors was higher in women than in men. The mechanism behind this sex-specific result is unclear, but it is probably due to the decreased bioavailability of estrogen in women.22 Further study is required to elucidate causality of this finding.
Our study has some strengths. First, we used standardized and reproducible methods to assess fat deposit amounts through CT scan. Second, all our study subjects had a normal WC, believed in the past to indicate fewer or no metabolic risks. As a result of this study’s design, we confirmed the need for a new index to replace WC, as well as the clinical usefulness of direct measurement of visceral and subcutaneous adipose tissue. So far, to our knowledge, no other studies have shown VSR to be a valuable indicator in predicting metabolic risk components in both sexes regardless of age and BMI.
There are some limitations to our study. First, we performed the study with a relatively small sample size in a single center, which prevents the generalization of results to the entire Korean population. Second, as a cross-sectional study, our data showed only cross-sectional associations between variables and metabolic risk factors. Finally, our study subjects were mostly middle-aged men and women, so we might not be able to generalize our findings to other age groups.
The design of future investigations needs to be on a larger scale, prospective, and include other clinical parameters that better reflect visceral obesity. Ultimately, researchers need to address the direct relationships between health indices and cardiovascular diseases. Additionally, the abdominal cavity should be subdivided into several compartments, and researchers should analyze possible associations of subdivided areas with metabolic disorders or cardiovascular disease.
Disclosure
The authors report no conflicts of interest in this work.
References
Power ML, Schulkin J. Sex differences in fat storage, fat metabolism, and the health risks from obesity: possible evolutionary origins. Br J Nutr. 2008;99(5):931–940. | ||
Pradhan AD. Sex differences in the metabolic syndrome: implications for cardiovascular health in women. Clin Chem. 2014;60(1):44–52. | ||
Lee CM, Huxley RR, Wildman RP, Woodward M. Indices of abdominal obesity are better discriminators of cardiovascular risk factors than BMI: a meta-analysis. J Clin Epidemiol. 2008;61(7):646–653. | ||
Zamboni M, Armellini F, Sheiban I, et al. Relation of body fat distribution in men and degree of coronary narrowings in coronary artery disease. Am J Cardiol. 1992;70(13):1135–1138. | ||
Björntorp P. Abdominal obesity and the development of noninsulin-dependent diabetes mellitus. Diabetes Metab Rev. 1988;4(6):615–622. | ||
Folsom AR, Kaye SA, Sellers TA, et al. Body fat distribution and 5-year risk of death in older women. JAMA. 1993;269(4):483–487. | ||
Folsom AR, Prineas RJ, Kaye SA, et al. Incidence of hypertension and stroke in relation to body fat distribution and other risk factors in older women. Stroke. 1990;21(5):701–706. | ||
Katzmarzyk PT, Janssen I, Ross R, et al. The importance of waist circumference in the definition of metabolic syndrome: prospective analyses of mortality in men. Diabetes Care. 2006;29(2):404–409. | ||
Han T, van Leer EM, Seidell JC, Lean M. Waist circumference action levels in the identification of cardiovascular risk factors: prevalence study in a random sample. BMJ. 1995;311(7017):1401–1405. | ||
Pouliot MC, Després JP, Lemieux S, et al. Waist circumference and abdominal sagittal diameter: best simple anthropometric indexes of abdominal visceral adipose tissue accumulation and related cardiovascular risk in men and women. Am J Cardiol. 1994;73(7):460–468. | ||
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive summary of the Third Report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA. 2001;285(19):2486–2497. | ||
Fox CS, Massaro JM, Hoffmann U, et al. Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation. 2007;116(1):39–48. | ||
Hayashi T, Boyko EJ, Leonetti DL, et al. Visceral adiposity and the risk of impaired glucose tolerance: a prospective study among Japanese Americans. Diabetes Care. 2003;26(3):650–655. | ||
Rosito GA, Massaro JM, Hoffmann U, et al. Pericardial fat, visceral abdominal fat, cardiovascular disease risk factors, and vascular calcification in a community-based sample: the Framingham Heart Study. Circulation. 2008;117(5):605–613. | ||
Kim JA, Choi CJ, Yum KS. Cut-off values of visceral fat area and waist circumference: diagnostic criteria for abdominal obesity in a Korean population. J Korean Med Sci. 2006;21(6):1048–1053. | ||
Seo JA, Kim BG, Cho H, et al. The cutoff values of visceral fat area and waist circumference for identifying subjects at risk for metabolic syndrome in elderly Korean: Ansan Geriatric (AGE) cohort study. BMC Public Health. 2009;9(1):443. | ||
Kim HI, Kim JT, Yu SH, et al. Gender differences in diagnostic values of visceral fat area and waist circumference for predicting metabolic syndrome in Koreans. J Korean Med Sci. 2011;26(7):906–913. | ||
Hayashi T, Boyko EJ, McNeely MJ, Leonetti DL, Kahn SE, Fujimoto WY. Minimum waist and visceral fat values for identifying Japanese Americans at risk for the metabolic syndrome. Diabetes Care. 2007;30(1):120–127. | ||
Oka R, Kobayashi J, Yagi K, et al. Reassessment of the cutoff values of waist circumference and visceral fat area for identifying Japanese subjects at risk for the metabolic syndrome. Diabetes Res Clin Pract. 2008;79(3):474–481. | ||
Fujioka S, Matsuzawa Y, Tokunaga K, Tarui S. Contribution of intra-abdominal fat accumulation to the impairment of glucose and lipid metabolism in human obesity. Metabolism. 1987;36(1):54–59. | ||
Hayashi T, Boyko EJ, McNeely MJ, Leonetti DL, Kahn SE, Fujimoto WY. Visceral adiposity, not abdominal subcutaneous fat area, is associated with an increase in future insulin resistance in Japanese Americans. Diabetes. 2008;57(5):1269–1275. | ||
Taskinen MR, Adiels M, Westerbacka J, et al. Dual metabolic defects are required to produce hypertriglyceridemia in obese subjects. Arterioscler Thromb Vasc Biol. 2011;31(9):2144–2150. | ||
Sironi AM, Gastaldelli A, Mari A, et al. Visceral fat in hypertension: influence on insulin resistance and beta-cell function. Hypertension. 2004;44(2):127–133. | ||
Hadaegh F, Zabetian A, Harati H, Azizi F. Metabolic syndrome in normal-weight Iranian adults. Ann Saudi Med. 2007;27(1):18–24. | ||
Motala AA, Esterhuizen T, Pirie FJ, Omar MA. The prevalence of metabolic syndrome and determination of the optimal waist circumference cutoff points in a rural South African community. Diabetes Care. 2011;34(4):1032–1037. | ||
Tran TT, Yamamoto Y, Gesta S, Kahn CR. Beneficial effects of subcutaneous fat transplantation on metabolism. Cell Metab. 2008;7(5):410–420. | ||
Porter SA, Massaro JM, Hoffmann U, Vasan RS, O’donnel CJ, Fox CS. Abdominal subcutaneous adipose tissue: a protective fat depot? Diabetes Care. 2009;32(6):1068–1075. | ||
Camhi SM, Bray GA, Bouchard C, et al. The relationship of waist circumference and BMI to visceral, subcutaneous, and total body fat: sex and race differences. Obesity (Silver Spring). 2011;19(2):402–408. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.