Back to Journals » Infection and Drug Resistance » Volume 12
Viral dynamics among HCV infected patients with different genotypes treated with genotypic specific or pan-genotypic direct-acting antiviral agent combinations
Authors Paolucci S , Novazzi F, Piralla A, Maserati R , Gulminetti R, Novati S, Barbarini G, Sacchi P, Fratini A, Bellotti L, Baldanti F
Received 14 February 2019
Accepted for publication 25 March 2019
Published 8 July 2019 Volume 2019:12 Pages 1975—1984
DOI https://doi.org/10.2147/IDR.S205282
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Suresh Antony
Stefania Paolucci,1 Federica Novazzi,1 Antonio Piralla,1 Renato Maserati,2 Roberto Gulminetti,2 Stefano Novati,2 Giorgio Barbarini,3 Paolo Sacchi,3 Alice Fratini,1 Laura Bellotti,1 Fausto Baldanti1,4
1Molecular Virology Unit, Microbiology and Virology Department, Fondazione Istituto di Ricovero e Cura a Carattere Scientifico (IRCCS) Policlinico, San Matteo, Pavia, Italy; 2Institute of Infectious Diseases, University of Pavia, Pavia, Italy; 3Division of Infectious and Tropical Diseases, Fondazione IRCCS Policlinico, San Matteo, Pavia, Italy; 4Department of Clinical, Surgical, Diagnostic and Pediatric Sciences, University of Pavia, Pavia, Italy
Background: New hepatitis C virus (HCV) therapies have improved efficacy, allowed pangenotypic applications, increased barriers to drug resistance and shortened therapy duration.
Methods: Patients infected with different HCV genotypes were divided into two groups: group 1 included 169 patients receiving genotypic specific regimens (GSR), while group 2 included 186 patients receiving pan-genotypic regimens (PGR). Patient’s HCV RNA was quantified and sequenced.
Results: Comparable sustained viral response (SVR) rates were observed in both GSR and PGR treated patients. Nevertheless, even if not significant, a greater proportion of non-detectable levels (NDL) of HCV RNA was observed in patients treated with PGR as compared with GSR. Overall, among patients in the GSR and PGR groups with residual viremia, 124/169 (73.4%) and 125/186 (67.2%) at four weeks, and 66/169 (39.1%) and 58/186 (31.2%) at eight weeks, achieved SVR. No difference was observed in the clinical outcome comparing patients in the GSR and PGR groups according to genotype. While, comparing patients between the two groups, the proportion of patients with NDL HCV RNA at four and eight weeks was higher in patients infected with genotype 1b treated with PGR (p=0.0015). A significantly higher number of patients infected with 1b had RASs at baseline (p=0.0001). In addition, the proportion of patients with treatment failure was higher in patients with RASs at baseline compared with those without (p=0.012). Overall, 2.5% patients failed to achieve SVR after DAA treatment.
Conclusion: A sharp HCV RNA decrease was observed in patients treated with both GSR and PGR. However, even if comparable, a slightly greater number of patients treated with PGR achieved NDL HCV RNA as compared with GSR. A significant difference was observed in patients with baseline RASs, both in relation to treatment failure and genotype. In conclusion, the use of new DAA combinations helps patients achieve a more rapid virologic response.
Keywords: hepatitis C virus, drug resistance, DAA inhibitors, viral dynamics, treatment failure
Introduction
Chronic infection with hepatitis C virus (HCV) affects more than 70 million individuals worldwide, and genotype distribution varies according to different geographic areas.1 These subjects are at risk of liver cirrhosis, hepatocellular carcinoma and liver-related death.1,2
After the introduction of direct-acting antivirals (DAAs), which specifically block key viral enzymes, chronic HCV infections have been successfully treated in cirrhotic, non-cirrhotic patients and those coinfected with HIV-1 and/or HBV.3–5
Recently, improved DAA combinations have been approved and have a safer profile with minimal adverse events. Highly effective and safe interferon (IFN)-free DAA treatments are available, with a very high genetic barrier to resistance, antiviral potency and pangenotypic coverage.6–11 These drugs are associated with a sustained virologic response (SVR) in an even higher percentage of patients (98–100%) in comparison with previously approved DAAs.6,7,12,13 In addition, the duration of treatment has been shortened to eight weeks, which simplifies treatment decisions, adherence, tolerability and potentially allows for the treatment of more patients.14–16 Although the efficacy of these new drugs is extremely high, DAA failure is an unfortunate event that can occur in different clinical situations, and it is frequently associated with the onset of HCV resistance-associated substitutions (RASs).17–20 HCV RASs found after failure generally develop during or at the end of treatment, while in some patients they may even have been present at baseline.21–23
The aims of this study were to evaluate the dynamics of rapid virologic response (RVR) with respect to SVR in patients treated with different DAA combinations during the period from January 2017 to May 2018 and to illustrate the frequency of DAA-resistant variants at baseline in all patients and in patients failing treatment.
Methods
Patients
This study was conducted in accordance with the principles of the Declaration of Helsinki and approved by the Institutional Review Board of the Fondazione IRCCS Policlinico San Matteo (protocol no. 20080009620). Written informed consent was obtained from all study participants. Three hundred and fifty five HCV infected patients with HCV genotypes 1, 2, 3 and 4, referred to the Fondazione IRCCS Policlinico San Matteo, Pavia between January 2017 and September 2018 were enrolled following the inclusion criteria set by the Italian Medicines Agency (AIFA). According to the Italian guidelines patients with hepatocellular carcinoma patients were excluded because treatment were not refundable. Patients were divided into two groups: group 1 included 169 patients receiving genotypic specific regimens (GSR): paritaprevir/ombitasvir/dasabuvir/ritonavir/ribavirin (par/omb/das/rtv/rbv), sofosbuvir/daclatasvir (sof/dac), sofosbuvir/ledipasvir (sof/led) or elbasvir/grazoprevir (elb/graz), and group 2 included 186 patients receiving pan-genotypic regimens (PGR): sofosbuvir/velpatasvir (sof/vel), or pibrentasvir/glecaprevir (pib/gle). Therapeutic decisions were made following the recommendations of the European Association for the Study of the Liver (EASL) clinical practice guidelines17 and AIFA criteria for HCV treatment (http://www.agenziafarmaco.gov.it). Treatment was prolonged to 24 weeks when indicated. All patients were compliant to the therapy. Patients with any adverse event leading to discontinuation were excluded. Only serious adverse events were reported.
Serum samples from each patient were prospectively collected at baseline and at months 1, 2 and 3 to evaluate RVR during treatment depending on the different DAA combinations: Patients were monitored for at least three months after treatment completion to evaluate SVR.
HCV-RNA quantification and genotyping
HCV viral load decreases in patients who achieved SVR and treatment-failing patients were compared at baseline and each month during and after stopping treatment using the Abbott HCV-RNA assay (Abbott Park, Illinois, U.S.A.), with a lower limit of detection of 12 IU/ml. To quantify HCV RNA levels <12 IU/ml, threshold cycles (CT) were used to obtain values with reference to a linear quantification curve. Non-detectable (NDL) HCV RNA levels were defined when target RNA samples were negative. HCV genotypes were defined using the Abbott RealTime HCV Genotype II assay (Abbott Park, Illinois, U.S.A.). In addition, when genotype results were ambiguous, the NS3/NS5B region was sequenced to further subtype HCV strains. Data were analysed using the Blast program (http://blast.ncbi.nlm.nih.gov).
Viral RNA was extracted from serum samples using the automatic Easy Mag extractor (Biomerieux, Lyon, France). Evaluation of RASs in the HCV NS5A, NS3 and/or NS5B genes was performed in 316/355 (89%) patients at baseline according to the drug class included in the DAA regimen.24 Direct Sanger-sequencing of the NS3-protease (aa 1-181), NS5A domain I (aa 1–213), and NS5B (aa 1-591) genes was performed using an automatic sequencer (ABI PRISM 3130xl genetic analyzer DNA Sequencer, Applied Biosystems, Foster City, CA, USA) and the BigDye Terminator v1.1 Cycle Sequencing kit (Applied Biosystems, Foster City, CA, USA). RASs were defined according to the geno2pheno algorithm [http://hcv.geno2pheno.org/index.php] and other clinical and in vitro data for RAS interpretation.18,19,25,26
Statistical analysis
Continuous variables (ie viral load) were compared using the Mann-Whitney U test for independent non-parametric data. Categorical variables were compared by the chi-square or Fisher’s exact test, as appropriate. The Log-rank test was used to compare Kaplan-Meier curves. All of the analyses were two tailed and performed using GraphPad Prism version 5 (GraphPad Software Inc., CA, USA); p-values of ≤0.05 were considered statistically significant. The positive predictive value (PPV) and negative predictive value (NPV) of NDL HCV RNA (less than the lower limit of quantification (<LLOQ) or quantifiable (≥LLOQ)) at four and eight weeks of treatment were calculated for all patients in the GSR and PGR groups.27
Results
Efficacy outcomes by different treatment and genotype
Patient demographic and virological characteristics as well as risk factors are reported in Table 1. All patients were DAA treatment naïve, except for two patients receiving the elb/graz and sof/vel regimen respectively, who had received a DAA protease inhibitor in 2016. The proportion of patients with cirrhosis in the GSR group was slightly higher than that treated with PGR (p=0.09) (Table 1). In detail, the fraction of patients with cirrhosis was higher in the sof/led group (33.3%), while it was lower in the sof/vel group (7.5%).
 |
Table 1 Patient characteristics |
A comparable sustained viral response (SVR) was observed in both GSR and PGR treated patients (Figure 1) (97.0% vs 97.8%; p=0.88). However, in the elb/graz group we only observed SVR in 91.7% of the patients.
 |
Figure 1 End of therapy SVR rates according to different treatments. |
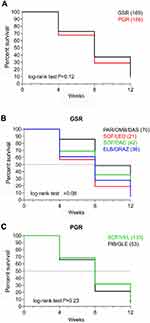
No differences in HCV RNA decay (delta log) between the two groups were observed at four weeks of therapy (p=0.35, data not shown). Nevertheless, even not significant, a slightly greater fraction of NDL HCV RNA was observed in patients treated with PGR as compared with GSR at all time points (27.2% vs 32.3% at four weeks; 62.7% vs 71.1% at eight weeks; and 88.8% vs 91.3% at 12 weeks; p=0.12; Figure 2A). Among patients treated with GSR, the sof/led combinations showed a greater proportion of patients with NDL HCV RNA at four, eight and 12 weeks (respectively, 42.9%, 81.0% and 95.2%) as compared with the combinations: elb/graz (38.9%, 72.2% and 94.4%), sof/dac (31.0%, 64.3% and 90.5%) and par/omb/das (14.3%, 51.4% and 82.9%) (p=0.08; Figure 2B). Among patients treated with PGR, a comparable percentage of NDL HCV RNA at four, eight and 12 weeks was observed in patients treated with the pib/gle (respectively, 34.0%, 78.6% and 94.7%) and sof/vel (31.6%, 68.1% and 90.9%) combinations, (p=0.23; Figure 2C). HCV RNA levels at 24 weeks of treatment were always undetectable in SVR patients.
Overall, no significant difference in the proportion of patients with NDL HCV RNA was observed in the GSR and PGR therapy groups according to genotype (Figure 3A and B, p=0.24 and p=0.76). However, in the GSR group a higher fraction of patients with NDL HCV RNA at four weeks was observed in patients infected with genotypes 1a and 2 (40.0% and 39.3%) and in patients infected with genotype 3 at eight weeks (83.3%; Figure 3A). The lowest proportion of patients with NDL HCV RNA was observed in patients infected with genotype 4 at four and eight weeks (12.5% and 50.0%). Among the PGR patients, a higher proportion with NDL HCV RNA at four weeks was observed in patients infected with genotypes 1b and 4 (34.1% and 33.3%), and at eight weeks in patients infected with genotype 1b (79.5%) (Figure 3B). While, the lowest proportion of patients with NDL HCV RNA at four weeks was observed in patients infected with genotype 3 (28.0%) and at eight weeks in patients infected with genotype 1a (54.3%; Figure 3B). A significant difference was observed only for genotype 1b (p=0.0015); when comparing GSR and PGR groups according to genotype (Figure 3C–G). The proportion of patients with NDL HCV RNA at four and eight weeks was 24.9% and 61.5% in the GSR group and 34.1% and 79.5% in the PGR group.
NDL HCV RNA predictive values for SVR at 4 and 8 weeks
In patients treated with GSR, 36.7% (62/169) had HCV RNA <LLOQ and 34.4% (45/169) had NDL HCV RNA at week 4. Among 62 patients with HCV RNA <LLOQ, 60 patients achieved SVR (PPV, 96.8%) and of the 45 patients with NDL HCV RNA, 44 patients achieved SVR (PPV, 97.8%). A total of 62 treated with GSR had RNA ≥LLOQ at week four, of whom two relapsed (NPV, 3.2%). Overall, 124/169 (73.4%) patients had HCV RNA ≥LLOQ (n=62) or HCV RNA <LLOQ (n=62), of whom only four relapsed (NPV, 3.2%). At week 8, among patients treated with GSR, 29.0% (49/169) had HCV RNA <LLOQ and 60.9% (103/169) had NDL HCV RNA. Among 49 patients with HCV RNA <LLOQ, 47 patients achieved SVR (PPV, 95.9%) and of the 103 patients with NDL HCV RNA, 100 patients achieved SVR (PPV, 97.1%). A total of 17 patients treated with GSR had RNA ≥LLOQ at week 8, none of whom relapsed (NPV, 0%). Overall, 66/169 (39.1%) patients had HCV RNA ≥LLOQ (n=17) or HCV RNA <LLOQ (n=49), only two of whom relapsed (NPV, 3.0%).
In patients treated with PGR, 33.9% (63/186) had HCV RNA <LLOQ and 34.4% (64/186) had NDL HCV RNA at week 4. Among 63 patients with HCV RNA <LLOQ, 60 patients achieved SVR (PPV, 95.2%) and of the 64 patients with NDL HCV RNA, all achieved SVR (PPV, 100%). A total of 62 patients treated with PGR had RNA ≥LLOQ at week 4, of whom one relapsed (NPV, 1.6%). Overall, 125/186 (67.2%) patients had HCV RNA ≥LLOQ (n=62) or HCV RNA <LLOQ (n=63), of whom only four relapsed (NPV, 3.2%). At week 8, among patients treated with PGR, 22.0% (41/186) had HCV RNA <LLOQ and 68.8% (128/186) had NDL HCV RNA. Among 41 patients with HCV RNA <LLOQ, all achieved SVR (PPV, 100%) and of the 128 patients with NDL HCV RNA, 124 patients achieved SVR (PPV, 96.9%). A total of 17 patients treated with PGR had RNA ≥LLOQ at week 8, none of whom relapsed (NPV, 0%). Overall, 58/186 (31.2%) patients had HCV RNA ≥LLOQ (n=17) or HCV RNA <LLOQ (n=41), none of whom relapsed (NPV, 0%). The high PPV and low NPV values observed after both 4 and 8 weeks of treatment with GSR are similar to those observed in patients treated with PGR.
Resistance analysis
An analysis of RASs was performed at baseline in 316/355 (89%) patients. In particular, 88/316 (27.8%) patients were infected with genotype 1b and 228/316 (72.2%) patients with other genotypes. A significantly higher number of patients infected with 1b (18/88, 20.5%) had RASs at baseline compared to those with other genotypes (8/228, 3.5%; p=0.0001). Overall, 140/169 (82.8%) patients were analyzed in the GSR group and 176/186 (94.6%) in the PGR group. HCV RASs were observed in 9/140 (6.4%) in the GSR group and 17/176 (9.7%) in the PGR group. Of these, RASs were present in 4/26 (15.4%) patients with HCV genotype 1a, 18/26 (69.2%) patients with genotype 1b, 1/26 (3.8%) patient with genotype 2c and 3/26 (11.6%) patients with genotype 3a. Of these, RASs associated with the DAA regimen, in at least one of the three target genes, were observed in 21/26 (80.7%) patients, 8/21 (38.1%) patients in the GSR group and 13/21 (61.9%) patients in the PGR group (Table 2, in bold ). In particular, one or more RASs associated with the DAA regimen were observed: 56F in the NS3 gene of 1/26 (3.8%) patients, 28M,30K/R,31M/T and 93H in the NS5A gene of 16/26 (61.5%) patients and 159F, 448H,451H/Y, 556G in the NS5B gene of 5/26 (19.2%) patients (Table 2).
 |
Table 2 DAA baseline RASs in HCV genes |
Overall, 9/355 (2.5%) patients failed to achieve SVR after DAA treatment. The proportion of patients with treatment failure was higher in patients with RASs at baseline (14.3%) compared with those without (6/334, 1.8%) (p=0.012). Of these, 5/169 (3.0%) patients treated with GSR and 4/186 (2.2%) patients treated with PGR, relapsed during the first month following treatment completion (Table 3). Among the 21 patients with baseline RASs to the ongoing DAA regimen, 3/21 (14.3%) patients failed treatment. Of these, a comparable number of patients, 2/8 (25%) in GSR and 1/13 (7.7%) PGR, failed treatment (p=0.53). While no RASs were observed at baseline in the remaining six patients with treatment failure (Table 3). RASs to ongoing therapy in the NS3 gene (56F/H, 168V) and/or in the NS5A gene (28M, 31M, 93H) were observed in 6/9 (66.7%) patients following treatment, four patients from the GSR group and two from the PGR group.
 |
Table 3 DAA RASs in patients with virologic failure |
Discussion
HCV RNA levels have been considered a predictive on-therapy marker of treatment outcome in patients receiving peg-IFN and ribavirin.28 Currently, a number of studies with IFN-free DAA combination therapies reporting a rapid viral decline after a few weeks of treatment have shown SVR rates >90%.6,7,12,13,15 However, it is still unclear whether early RVR during therapy with undetectable HCV RNA, measured with a highly sensitive assay, may be useful to predict virological failure. In monotherapy DAA studies, residual detectable viremia at four weeks of protease inhibitor-based therapies was associated with higher relapse rates.29–31 Recently, highly effective IFN-free DAA treatments have led to RVR in 4–8 weeks of treatment in a high portion of patients.27,32,33 However, using more sensitive assays at early time points, it was shown that residual viremia was detectable as late as 12 weeks of treatment in a portion of patients,27,32,34 who subsequently achieved SVR.
Our data showed that residual viremia, measured in patients treated with GSR and PGR, was detectable in different percentages of patients at 4 to 12 weeks of treatment. Nevertheless, the majority of patients with residual viremia at four and eight weeks achieved SVR and comparably high PPVs and low NPVs between the two groups were observed. In addition, despite a slight difference in the proportion of patients with cirrhosis at baseline between the two groups, no differences were highlighted in the clinical outcome. Similarly, comparable HCV RNA decay and SVR (≥97%) were obtained. Thus, HCV RNA measurements during treatment didn’t add significant advantages in predicting the outcome in this study. In addition, residual viremia at four and eight weeks of treatment was not predictive of relapse with GSR and PGR as also previously reported.27,32 However, differences in RVR at four, eight and 12 weeks of treatment were observed. In fact, even if not significant, a slightly greater fraction of NDL HCV RNA, was observed in patients treated with PGR as compared with GSR. Even though, among the GSR, a comparable proportion of NDL HCV RNA at four, eight and 12 weeks was observed also in the sof/led treated. Therefore, overall PGR seems to be slightly more efficient in eliminating viral load at four, eight and 12 weeks.
Stratifying patients by genotype, it was shown that differences in the levels of HCV decay and proportion of residual viremia, at four, eight and 12 weeks of treatment, were not overall statistically significant in the GSR or PGR groups. Similarly, in these patient subgroups, SVR was achieved regardless of genotype. However, at four weeks, patients infected with genotypes 1a and 2 in the GSR group and with genotype 1b and 4 in the PGR group had a higher fraction of NDL HCV RNA. While, comparing genotypes between the GSR and PGR groups, a proportion of patients with NDL HCV RNA at four and eight weeks was significantly higher in patients infected with genotype 1b treated with PGR.
Among the nine patients with virologic treatment failure, one patient had NDL HCV RNA at four weeks of treatment, while at the same time point eight patients had detectable HCV RNA. In these eight patients, NDL HCV RNA was achieved after 8–12 weeks of treatment. Treatment failure was most likely caused by the onset of RASs (6 patients) or by incomplete HCV RNA suppression (3 patients). Virologic failure in patients treated with GSR and PGR was comparable (3.0% vs 2.2%). Nevertheless, regarding baseline RASs as a risk factor, a significant difference was observed in clinical outcome. In fact, the frequency of treatment failure was higher in patients with RASs at baseline compared to those without. Special attention must be paid to patients infected with genotype 1b who appear to have a more significant chance of having RASs at baseline. This suggests that baseline sequencing, especially in genotype 1b, may help define the most appropriate regimen. In addition, despite the low number of patients in whom RASs were present at baseline in the GSR group a slightly higher proportion of patients failed treatment as compared with those treated with PGR (25.0% vs 7.7%).
In conclusion, considering all of the patients, a significant difference was observed in patients with baseline RASs, both in relation to treatment failure and genotype. Nevertheless, no significant differences were found in clinical outcome comparing the GSR and PGR groups, in relation to the therapy, genotype or baseline RASs. However, the introduction of new and more efficient DAA combinations with good pharmacodynamics has led to better response rates and more rapid decreases in viral load. On the other hand, in difficult to treat patients, or those treated with short-term therapies,14,15,33 should be monitored carefully since short treatment duration may lead to an incomplete suppression of HCV replication or the onset of RASs. In addition, due to high cross-resistance among NS5A-inhibitors and the essential role of this class, NS5A experienced-patients are the most ‘‘difficult to retreat”. This evolution in treatment pharmacodynamics may still improve by using triple combination therapies that affect the three genes of the target virus resulting in more efficient virus elimination and shorter treatment duration.17,20 Hence, the elimination of HCV RNA, which typically initially decreases rapidly, then more slowly with residual viremia,35 may be accelerated. Importantly, this acceleration may also reduce the possibility of transmission in the highest at risk populations.
Strengths of this study are: i) number of patients analyzed with all HCV genotypes were considered; iii) only a limited number of reports considered pan-genotypic vs genotypic specific treatment. Limitations are: i) the number of failures (as expected) is low, then only few patients failing therapy (no. 9) could be included in the post treatment analysis; ii) the RASs analysis was performed using the Sanger technology with a resolution level lower than deep sequencing methodology. Then, some mutants could have been missed. iii) Hepatocellular carcinoma patients could not be included due to the Italian guidelines.
Acknowledgments
We thank Daniela Sartori for careful preparation of the manuscript and Laurene Kelly for English revision. This work was supported by the Ministero della Salute, Fondazione IRCCS Policlinico San Matteo Ricerca Corrente (grant 80207).
Author contributions
Stefania Paolucci: concept or design of the work, data analysis and interpretation, drafted the article. Federica Novazzi, Alice Fratini, Laura Bellotti: data collection. Renato Maserati: critical revision of the article. Roberto Gulminetti, Stefano Novati, Giorgio Barbarini, Paolo Sacchi: patient enrollment. Antonio Piralla: data analysis and interpretation. Fausto Baldanti: critical revision of the article and final approval of the version to be published. All authors contributed toward data analysis, drafting and revising the paper, gave final approval of the version to be published and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. WHO Guidelines on Hepatitis B and C Testing. Geneva: World Health Organization; 2017. Feb.ISBN-13, 978-92-4-154998-1. Available from: https://www.ncbi.nlm.nih.gov/books/NBK442272/. Accessed June 25, 2019.
2. Polaris Observatory HCV, 2017. Global prevalence and genotype distribution of hepatitis C virus infection in 2015: a modelling study. Lancet Gastroenterol Hepatol. 2017;2(3):161–176. doi:10.1016/S2468-1253(16)30181-9
3. Operskalski EA, Kovacs A. HIV/HCV co-infection: pathogenesis, clinical complications, treatment, and new therapeutic technologies. Curr HIV/AIDS Rep. 2011;8(1):12–22. European Association for the Study of the Liver. doi:10.1007/s11904-010-0071-3
4. EASL recommendations on treatment of hepatitis C 2018. J Hepatol. 2018;69(2):461–511. doi:10.1016/j.jhep.2018.03.026
5. American Association for the Study of Liver Disease, Infectious Diseases Society of America. HCV guidance: recommendations for testing, managing, and treating hepatitis C virus. 2017. Available from: http://www.hcvguidelines.org Accessed June 17, 2019.
6. Chan HL, Tsang OT, Hui YT, et al. Real-life efficacy and safety of paritaprevir/ritonavir, ombitasvir, and dasabuvir in chronic hepatitis C patients in Hong Kong. J Gastroenterol Hepatol. 2017;32(6):1230–1233. doi:10.1111/jgh.13663
7. Werner CR, Schwarz JM, Egetemeyr DP, et al. Second-generation direct-acting-antiviral hepatitis C virus treatment: efficacy, safety, and predictors of SVR12. World J Gastroenterol. 2016;22(35):8050–8059. doi:10.3748/wjg.v22.i35.8050
8. Sciences G. EPCLUSA (Sofosbuvir and Velpatasvir) [Package Insert]. CA, Foster City; 2016. Available from: https://ec.europa.eu/health/documents/community-register/2016/20160706135323/anx_135323_it.pdf. Accessed June 25, 2019.
9. Asselah T, Boyer N, Saadoun D, Martinot-Peignoux M, Marcellin P. Direct acting antivirals for the treatment of hepatitis C virus infection: optimizing current IFN-free treatment and future perspectives. Liver Int. 2016;36(Suppl 1):47–57. doi:10.1111/liv.2016.36.issue-S1
10. Pawlotsky JM. New hepatitis C therapies: the toolbox, strategies, and challenges. Gastroenterology. 2014;146(5):1176–1192. doi:10.1053/j.gastro.2014.03.003
11. Zeuzem S, Ghalib R, Reddy KR, et al. Grazoprevir-elbasvir combination therapy for treatment-naive cirrhotic and noncirrhotic patients with chronic HCV genotype 1, 4, or 6 infection: a randomized trial. Ann Intern Med. 2015;163(1):1–13. doi:10.7326/M15-0785
12. Benítez-Gutiérrez L, Barreiro P, Labarga P, et al. Prevention and management of treatment failure to new oral hepatitis C drugs. Expert Opin Pharmacother. 2016;17(9):1215–1223. doi:10.1080/14656566.2016.1182156
13. Pawlotsky JM, Feld JJ, Zeuzem S, Hoofnagle JH. From non-A, non-B hepatitis to hepatitis C virus cure. J Hepatol. 2015;62(Suppl 1):S87–S99. doi:10.1016/j.jhep.2014.09.033
14. Kwo PY, Poordad F, Asatryan A, et al. Glecaprevir and pibrentasvir yield high response rates in patients with HCV genotype 1-6 without cirrhosis. J Hepatol. 2017;67(2):263–271. doi:10.1016/j.jhep.2017.03.039
15. Puoti M, Foster GR, Wang S, et al. High SVR12 with 8-week and 12-week Glecaprevir/Pibrentasvir: integrated analysis of HCV genotype 1-6 patients without cirrhosis. J Hepatol. 2018;69(2):293–300. doi:10.1016/j.jhep.2018.03.007
16. Pol S, Parlati L. Treatment of hepatitis C: the use of the new pangenotypic direct-acting antivirals in “special populations”. Liver Int. 2018;38(Suppl 1):28–33. doi:10.1111/liv.13626
17. European Association for Study of Liver. EASL recommendations on treatment of hepatitis C 2016. J Hepatol. 2017;66(1):153–194. doi:10.1016/j.jhep.2016.09.001
18. Sarrazin C. The importance of resistance to direct antiviral drugs in HCV infection in clinical practice. J Hepatol. 2016;64(2):486–504. doi:10.1016/j.jhep.2015.09.011
19. Pawlotsky JM. Hepatitis C virus resistance to direct-acting antiviral drugs in interferon-free regimens. Gastroenterology. 2016;151(1):70–86. doi:10.1053/j.gastro.2016.04.003
20. AASLD-IDSA. Recommendations for testing, managing, and treating hepatitis C; 2018. Available from: https://www.hcvguidelines.org/. Accessed June 17, 2019.
21. Komatsu TE, Boyd S, Sherwat A, et al. Regulatory analysis of effects of hepatitis C virus NS5A polymorphisms on efficacy of elbasvir and grazoprevir. Gastroenterology. 2017;152(3):586–597. doi:10.1053/j.gastro.2016.10.017
22. Zeuzem S, Mizokami M, Pianko S, et al. NS5A resistance-associated substitutions in patients with genotype 1 hepatitis C virus: prevalence and effect on treatment outcome. J Hepatol. 2017;66(5):910–918. doi:10.1016/j.jhep.2017.01.007
23. Harrington PR, Komatsu TE, Deming DJ, Donaldson EF, O’Rear JJ, Naeger LK. Impact of hepatitis C virus polymorphisms on direct-acting antiviral treatment efficacy: regulatory analyses and perspectives. Hepatology. 2018;67(6):2430–2448. doi:10.1002/hep.29693
24. Paolucci S, Premoli M, Novati S, et al. Baseline and breakthrough resistance mutations in HCV patients failing DAAs. Sci Rep. 2017;7(1):16017. doi:10.1038/s41598-017-15987-1
25. Lontok E, Harrington P, Howe A, et al. Hepatitis C virus drug resistance-associated substitutions: state of the art summary. Hepatology. 2015;62(5):1623–1632. doi:10.1002/hep.27934
26. Sorbo MC, Cento V, Di Maio VC, et al. Hepatitis C virus drug resistance associated substitutions andtheir clinical relevance: update2018. Drug Resist Update. 2018;37:17–39. doi:10.1016/j.drup.2018.01.004
27. Sidharthan S, Kohli A, Sims Z, et al. Utility of hepatitis C viral load monitoring on direct-acting antiviral therapy. Clin Infect Dis. 2015;60(12):1743–1751. doi:10.1093/cid/civ170
28. Ferenci P, Laferl H, Scherzer TM, et al. Austrian hepatitis study group. Peginterferon alfa-2a and ribavirin for 24 weeks in hepatitis C type 1 and 4 patients with rapid virological response. Gastroenterology. 2008;135(2):451–458. doi:10.1053/j.gastro.2008.04.015
29. Harrington PR, Zeng W, Naeger LK. Clinical relevance of detectable but not quantifiable hepatitis C virus RNA during boceprevir or telaprevir treatment. Hepatology. 2012;55(4):1048–1057. doi:10.1002/hep.24791
30. Manns M, Marcellin P, Poordad F, et al. Simeprevir with pegylated interferon alfa 2a or 2b plus ribavirin in treatment-naive patients with chronic hepatitis C virus genotype 1 infection (QUEST-2): a randomised, double-blind, placebo-controlled phase 3 trial. Lancet. 2014;384(9941):414–426. doi:10.1016/S0140-6736(14)60538-9
31. Ferenci P, Asselah T, Foster GR, et al. STARTVerso1: A randomized trial of faldaprevir plus pegylated interferon/ribavirin for chronic HCV genotype-1 infection. J Hepatol. 2015;62(6):1246–1255. doi:10.1016/j.jhep.2014.12.024
32. Tabernilla A, Grandal M, Pernas B, et al. Viral dynamics among hepatitis C virus chronic infected patients during direct-acting antiviral agents therapy: impact for monitoring and optimizing treatment duration. Eur J Gastroenterol Hepatol. 2017;29(7):781–785. doi:10.1097/MEG.0000000000000882
33. Zeuzem S, Foster GR, Wang S, et al. Glecaprevir-pibrentasvir for 8 or 12 weeks in HCV genotype 1 or 3 infection. N Engl J Med. 2018;378(4):354–369. doi:10.1056/NEJMoa1702417
34. Sarrazin C, Wedemeyer H, Cloherty G, et al. Importance of very early HCV RNA kinetics for prediction of treatment outcome of highly effective all oral direct acting antiviral combination therapy. J Virol Methods. 2015;214:29–32. doi:10.1016/j.jviromet.2014.11.027
35. Chatterjee A, Guedj J, Perelson AS. Mathematical modelling of HCV infection: what can it teach us in the era of direct-acting antiviral agents? Antivir Ther. 2012;17(6Pt B):1171–1182. doi:10.3851/IMP2428
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.