Back to Journals » Clinical Interventions in Aging » Volume 15
Vestibular Rehabilitation Using Posturographic System in Elderly Patients with Postural Instability: Can the Number of Sessions Be Reduced?
Authors Soto-Varela A , Rossi-Izquierdo M, del-Río-Valeiras M, Vaamonde-Sánchez-Andrade I , Faraldo-García A , Lirola-Delgado A, Santos-Pérez S
Received 19 May 2020
Accepted for publication 10 June 2020
Published 26 June 2020 Volume 2020:15 Pages 991—1001
DOI https://doi.org/10.2147/CIA.S263302
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Richard Walker
Andrés Soto-Varela,1,2 Marcos Rossi-Izquierdo,3 María del-Río-Valeiras,4 Isabel Vaamonde-Sánchez-Andrade,4 Ana Faraldo-García,4 Antonio Lirola-Delgado,4 Sofía Santos-Pérez1,2
1Division of Neurotology, Department of Otorhinolaryngology, Complexo Hospitalario Universitario, Santiago de Compostela, Spain; 2Department of Surgery and Medical-Surgical Specialities, University of Santiago de Compostela, Santiago de Compostela, Spain; 3Department of Otorhinolaryngology, University Hospital Lucus Augusti, Lugo, Spain; 4Department of Otorhinolaryngology, Complexo Hospitalario Universitario, Santiago de Compostela, Spain
Correspondence: Andrés Soto-Varela
Division of Neurotology, Department of Otorhinolaryngology, Complexo Hospitalario Universitario de Santiago, Travesía da Choupana, s/n, Santiago de Compostela 15706, Spain
Tel +34981951155
Email [email protected]
Purpose: Vestibular rehabilitation (VR) using posturography systems has proved useful in improving balance among elderly patients with postural instability. However, its high cost hinders its use. The objective of this study is to assess whether two different protocols of VR with posturography, one of them longer (ten sessions) and the other shorter (five sessions), show significant differences in the improvement of balance among old patients with instability.
Patients and Methods: This is a prospective, experimental, single-center (Department of Otorhinolaryngology of a tertiary referral hospital), randomized (into balanced patient blocks) study with two parallel arms, in 40 people over 65 years of age, with instability and at a high risk of falling. The percentage of the average balance (composite) in the sensory organization test (SOT) of the CDP (main outcome measure), other CDP scores, time and steps in the “timed up and go” test, scores of Dizziness Handicap Inventory (DHI), short Falls Efficacy Scale – International (short FES-I), and Vertiguard were compared before and 3 weeks after VR between both intervention groups.
Results: The two treatment groups (20 patients per group) were comparable in age, sex, and pre-VR balance evaluation. In both groups, we observed a significant improvement in global balance (composite) after VR (49± 11.34 vs 57± 13.48, p=0.007, in the group undergoing 10 sessions; 51± 12.55 vs 60± 12.99, p=0.002, 5 sessions). In both groups, we also observed improvements in other posturographic parameters (in the SOT and limits of stability) but not in the timed up and go scores or in the questionnaires. Comparison of the improvement level achieved in both groups revealed no significant differences between them.
Conclusion: The protocols of vestibular rehabilitation by posturography of 5 sessions in elderly patients with postural instability are as effective as those of 10 sessions for improving balance among elderly patients with postural instability.
Trial Registration: ClinicalTrials.gov identifier: NCT03034655. Registered on 25 January 2017.
Keywords: instability, balance, old people, computerized dynamic posturography, mobile posturography, vertiguard
Plain Language Summary
Balance disturbances cause falls in the elderly. Balance can be improved by specific training exercises (vestibular rehabilitation). More specifically, vestibular rehabilitation performed using posturography devices (which measure the balance of a patient and make it possible to design training exercises adapted to the specific needs of each person) has proved highly effective in improving balance. However, these devices are very expensive, thereby preventing its application in large groups of the elderly population. Nevertheless, a way to lower the cost of rehabilitation is to specify the minimum number of sessions necessary for its effectiveness. Thus, in this study, we compare two protocols (of ten and five sessions) and show that they are both effective in improving balance among elderly patients with postural instability. Furthermore, we have not found significant difference in results between them. Therefore, the results from the 5 sessions are similar to those from 10. These findings are crucial as they will permit treatment of twice as many patients with the same resources.
Introduction
Vestibular rehabilitation using posturography systems is useful for improving balance among elderly patients with postural instability.1,2 The causes of balance disturbances in elderly people are multiple and sometimes overlap with one another (neurological and/or vestibular disorders, loss of strength and flexibility, decreased reflexes and aging itself, among others).3,4
Although there is no definitive consensus, postural stability in elderly people is thought to be more effectively improved when using exercises of different types, including posturography exercises.5 The most appropriate approach, especially for elderly people living in the community and at risk of falls, should include exercises aimed at improving strength and balance.4,6,7 Furthermore, the improvement in balance in this particular population segment should translate into a reduced number of falls,8 which is a key strategic issue in terms of public health. Reducing the number of falls also means reducing the number of fractures and therefore, the number of hospital admissions. Ultimately, it implies a significant reduction in morbidity and mortality among elderly people.9,10
The duration of protocols of vestibular rehabilitation using posturography systems is not clearly defined. In general, the number of sessions should be tailored according to the requirements of each patient as just a few sessions can suffice to reasonably restore the balance in some patients, while others require more training time and dedication. Nevertheless, a reasonable alternative is to establish a desirable numerical range of sessions (considering that, for example, one or two sessions should be insufficient, whereas more than twenty would be excessive). At least in our setting, the average number of protocolized sessions is 10.
There are doubts on the appropriate number of sessions required, even more so, when referring to elderly people. Elderly should require more sessions than younger people due to their reduced brain plasticity and decreased learning speed, and cognitive difficulties overlap with balance disturbance. However, elderly patients usually require aid from a third person to take them to the hospital, which implies a disruption (often, even work and economic) for the patient and their family. In fact, these difficulties can decrease the adherence to the rehabilitation treatment in patients of this age group.11 Based on the above, specifying the number of sessions capable of improving performance is crucial.
In addition, the main limitation to the widespread development of vestibular rehabilitation using posturography systems is its high cost (both for equipment and human resources in that only highly qualified professionals can conduct these sessions). A way to lower this cost is to reduce the number of sessions, as long as the reduced number of sessions is sufficient to reach levels of improvement similar to those achieved with the recommended 10 sessions. This has been demonstrated in patients with postural instability secondary to unilateral vestibular deficit (in whom five-session protocols provided results similar to those achieved with 10-session protocols).12 However, to the best of our knowledge, the effectiveness of protocols with a reduced number of sessions in improving postural instability caused by aging has not been investigated.
Accordingly, the objective of this study is to assess whether two different protocols of vestibular rehabilitation by posturography, one of them longer (ten sessions) and the other shorter (five sessions), show significant differences in the improvement of balance among elderly patients with postural instability.
Patients and Methods
This manuscript presents the partial results from a clinical trial funded by the project PI1500329, integrated into the Spanish State Plan for R + D + I and funded by the Instituto de Investigación en Salud Carlos III – ISCIII – Subdirección general de Evaluación y Fomento de la Investigación and the Fondo Europeo de Desarrollo regional (FEDER). This clinical trial, whose protocol has already been published,13 aimed to evaluate the utility of vestibular rehabilitation in the elderly with postural instability for improving balance and reducing the number of falls.
Study Design
An experimental, prospective, single-center (a tertiary hospital), open-label, randomized study (balanced patient blocks) was conducted in 2 groups of elderly patients (at least 65 years of age) with a high risk of falling and a 3-week follow-up period.
Study Population: Inclusion and Exclusion Criteria
This study included patients aged ≥65 years who had instability and met at least 2 of the following inclusion criteria:
- Had fallen at least once in the last 12 months.
- Took >15 seconds or needed support in the timed up and go (TUG) test.
- Obtained a mean sensory organization test (SOT) of dynamic computerized posturography (CDP-SOT) balance score of <68%.
- Had fallen at least once in the CDP-SOT.
- Obtained a score of >60% in the Vertiguard geriatric Standard Balance Deficit Test (gSBDT).
The following were the exclusion criteria:
- Cognitive decline or reduced cultural level that prevents the patient from understanding the assessment, vestibular rehabilitation exercises, and granting informed consent.
- Organic conditions that prevent standing on 2 feet, which is necessary for assessment of balance and performance of VR exercises.
- Balance disorders caused by conditions other than aging (neurological, vestibular, etc.).
- Current treatment with drugs that potentially affect balance.
Sample Size Estimation
The sample size was estimated using a reference of the mean value of balance in the sensory organization test by computerized dynamic posturography. From a previous study performed using a similar methodology,12 the standard deviation estimated for this value was 6. We considered relevant a difference in the score between the two study groups of 7 percentage points. With a 95% confidence level (1-ά) and a type II error probability (β) of 0.5, for a bilateral hypothesis test, a total of 19 subjects were deemed the number necessary in each of the two arms. Considering the above, the estimated sample size was 38 individuals, which was increased to 40 (20 in each group) in anticipation of some loss due to follow-up.
Sample
The study included 40 patients (20 in each group) who met the inclusion criteria and were examined for presenting balance alterations in the otoneurologic unit of a tertiary hospital. The mean age was 78.44 ± 6.31 years, with a maximum of 88.13 years. Regarding the sex distribution, 28 patients were female (70%) and 12 were male (30%), with a female-to-male ratio of 2.3:1.
In reference to the inclusion criteria, 18 patients met the criterion 1) (fell at least once in the previous 12 months), 27 met the criterion; 2) (used more than 15 seconds or needed support during the TUG Test), 38 met the criterion; 3) (obtained a mean CDP-SOT balance score <68%), 38 met the criterion; 4) (fell at least once in the CDP-SOT) and 5 met the criterion; 5) (had a score >60% in Vertiguard’s geriatric Standard Balance Deficit Test). Eleven patients were included with two inclusion criteria, 12 with three, 14 with four, and 3 with five.
Methodology
To exclude causes other than advanced age that would account for the instability, we performed a complete otoneurological clinical history for all patients. This included a complete neurological examination and confirmation of the absence of nystagmus (spontaneous or caused by cephalic agitation), saccades in the head impulse test, and nystagmus in the Dix-Hallpike positional test. If necessary, we performed videonystagmography with caloric tests, video head impulse test, vestibular evoked potential test, and/or head magnetic resonance imaging.
To assess balance, the patients were evaluated using the inclusion criteria and their baseline equilibriometric patterns by performing the following tests before starting the vestibular rehabilitation:
- Modified TUG test:14,15 Seated, the subject must stand up without aid, walk 3 meters, turn around, and sit down again. The time needed and numbers of steps were determined.
- CDP-SOT (Neurocom Smart Equitest platform): The SOT included quantitation of the patient’s COG displacements in 6 different sensorial information conditions as follows: fixed surface and visual surround, with eyes open; fixed surface, with eyes closed; fixed surface and moving visual surround, with eyes open; moving surface and fixed visual surround, with eyes open; moving surface, with eyes closed; moving surface and visual surround, with eyes open. Each of the 6 conditions was repeated 3 consecutive times, with the patients completing a total of 18 tests per record. The time set for each of these tests was 20 seconds.
- CDP LOS: After visual feedback (movement of a pictogram representing the subject’s COG on a television monitor), the patients had to voluntarily move their COG, without moving their feet, on the platform to reach 8 points that represent 100% of the displacement limit of each subject’s COG according to height and age.
- Balance record study using the mobile Vertiguard system: The following 14 tests were performed, and the analysis of the results represented the gSBDT:
- Standing still (SS), with eyes open, on a normal surface (NS).
- SS, with eyes closed, on a NS.
- SS, one leg, eyes open, NS
- Making 8 steps in tandem, with eyes open, on a NS.
- SS, with eyes open, on a foam surface (FS).
- SS, with eyes closed, on a FS.
- Making 8 steps in tandem, with eyes open, on a FS.
- Walking 3 m, with eyes open.
- Walking 3 m, with eyes open, while turning the head from side to side.
- Walking 3 m, with eyes open, while moving the head up and down.
- Walking 3 m, with eyes closed.
- Walking over 4 barriers (height: 26 cm; distance between barriers: 1 m).
- Sitting down on a chair.
- Getting up from a chair.
- Questionnaires that measure disability due to imbalance and risk of falling:
- A question assessing the number of falls in the last 12 months.
- The Dizziness Handicap Inventory (DHI), validated in Spanish,16 assesses disability perceived by the patient in relation to instability. It consists of 25 items divided into 3 groups (9 on the functional scale, 9 on the emotional scale and 7 on the physical scale), with 3 possible answers scored as follows: “yes” (4 points), “sometimes” (2 points), and “no” (0 points). The highest perception of disability is 100, and the lowest is 0.
- A shortened version of the Falls Efficacy Scale – International to assess fear of falling (Short FES-I)17 evaluates fear of falling while performing 7 everyday activities. Each question has 4 possible answers scored as follows: “not at all concerned” (0 points), “somewhat concerned” (1 point), “quite concerned” (2 points), and “very concerned” (3 points). The highest score (greatest fear of falling) is 21, and the lowest is 0.
Intervention
After the first screening visit, the patients who provide consent were included in the study and randomized to one of the study arms. Randomization was performed by the clinical epidemiology and biostatistics unit of our hospital. Once the patient signed the informed consent form, the investigator contacted the unit, which provided the code of the arm to which the patient was assigned. A block balanced randomization sequence was used. The investigator established the applicable intervention schedule with the patient.
The two study arms were:
- Ten sessions of vestibular rehabilitation by posturography (20 patients), using two different interventions:
- Intervention with dynamic posturography exercises (9 patients). The Smart Equitest program was used with a protocol of 10 exercises per session, which were customized depending on the patient´s deficit (as observed in the earlier postural study). The exercises involved visual biofeedback together with sensitive, real-time monitoring of movement. In some exercises, the patients must maintain their COG over the base of support, whereas in others, the COG must be moved to a series of targets. In addition, the support surface and/or visual surround may move in response to the patient’s own movement. The exercise difficulty was progressively increased throughout the rehabilitation sessions by increasing the LOS, transition rate, or movement of the posturography platform). The duration of each session was approximately 15 minutes. The distribution of the sessions was 1 per day and 5 per week (two weeks).
- Intervention with mobile device Vertiguard exercises (11 patients). Up to 6 tasks with the most prominent deviations from the normative control values were included in the training program. Individual feedbacks based on body sway analysis were calculated and stored in the device for each patient. Training was performed using the training function of the Vertiguard1-RT device. This neurofeedback system contains a battery-driven main unit fixed on a belt at the center of body mass (hip) and one vibration stimulator on the front, back, left, and right sides, respectively. Vibration stimulators are mounted on the same belt as the main unit. They were adjustable by sliding over the belt to the correct position in the individual patient. The main unit continuously determines the coriolis force during body movements in pitch and roll by the built-in gyroscope and compares those values with the individual preset thresholds for stimulator activation in specific directions. The patients performed training daily under the supervision of a physician over 2 weeks, excluding weekends. Each training session consisted of 5 repetitions of the 6 selected training tasks described earlier (each repetition lasting 20 s or until the movement was finished). The patient received a vibrotactile feedback signal during training in the directions that showed a higher body sway than the preset thresholds. Vibration was reinforced with increasing sway; that is, the higher it exceeded the preset values, the stronger the vibration was at the corresponding site. The duration of each session was approximately 15 minutes. No vibrotactile feedback was applied if the patient’s sway was below the preset thresholds. The difficulty of the exercises was progressively increased throughout the rehabilitation sessions by pressing the sensitivity buttons (up/down) on the main unit. During this procedure, the individual preset thresholds were similarly decreased for all sway directions of the specific training condition until the patient perceived a vibration while performing the training task.
- Five sessions of vestibular rehabilitation by posturography (20 patients), using the two interventions described in group A, carried out over two weeks (Monday to Friday, every other day). Vestibular rehabilitation was performed in ten patients using the dynamic posturography device and in another ten using the Vertiguard device.
Analyzed Variables
The equilibriometric evaluation conducted prior to the vestibular rehabilitation was repeated 3 weeks after the end of the rehabilitation. The following variables were collected and analyzed:
- Age and sex.
- TUG test (time spent and number of steps).
- CDP sensory organization test:
- The percentage score obtained for each condition (considered as the arithmetic mean of the 3 records obtained for each condition)
- The global mean balance, which is obtained by calculating the weighted mean of the scores obtained in the 18 records of each sensory organization test.
- The number of falls that occurred during the completion of the 18 SOT records.
- The use of somatosensory information, which is a percentage value resulting from the following formula: (mean score for condition 2/mean score for condition 1)/100.
- The efficacy of processing visual information, which is calculated using the following formula: (mean score for condition 4/mean score for condition 1)/100.
- The use of vestibular information, which is calculated using the following formula: (mean score for condition 5/mean score for condition 1)/100.
- The ability to assume erroneous visual information, which has a score resulting from the following formula using the values obtained for the corresponding conditions: [(2 + 5)/(3 + 6)]/100.
- CDP limits of stability:
- Reaction time: time from onset of visual signal showing movement to its actual beginning. (in seconds)
- Speed of the movement: mean speed of displacement from COP, as º/sec.
- Maximum displacement point: measure of the maximum displacement reached by the COG with respect to the theoretical 100% of the LOS (in percentage)
- End point of displacement: measure of the point reached at the end of the displacement of the COP, relative to the theoretical 100% of limit of stability. (as a percentage)
- Directional control: comparison between movement in the direction of the target versus movement away from that direction, as a percentage.
- Vertiguard gSBDT score
- Questionnaires:
- DHI score, total and for each scale (physical, emotional, and functional)
- Short FES-I score
Statistical Analyses
We used the Kolmogorov–Smirnoff test to assess whether the different continuous variables followed a normal distribution. The Fisher exact test was used to determine any association between two nominal variables, always in 2 x 2 tables, presenting the odds ratios and 95% confidence intervals when the results are statistically significant. We used the Student’s t-test to compare the continuous and nominal variables when the continuous variables followed a normal distribution. The non-parametric Mann–Whitney test was used when the distribution was not normal. We used the Wilcoxon test to compare the continuous variables in the same patient at 2 different time points (before and after vestibular rehabilitation). The level of statistical significance in all the tests was set at p < 0.05.
We used SPSS 15.0 software for Windows for the statistical analyses.
Ethical Aspects
The protocol was approved by the Independent Ethics Committee of Galicia (protocol No. 2014/411). The study will be conducted in accordance with the ICH Good Clinical Practices, the Declaration of Helsinki, and Law 14/2007 of 3 July on Biomedical Research. All patients signed a written informed consent form to participate in the study.
Results
The two groups were comparable in age (p=0.130, Student’s t-test) and sex (p=0.366, Fisher’s exact test). There were also no significant differences in the balance evaluation prior to vestibular rehabilitation, or in the questionnaires, as shown in Table 1; only the number of steps taken to complete the timed up and go test was higher in the group of patients who performed five sessions (p=0.035). The number of patients undergoing rehabilitation using the dynamic posturography device and the mobile posturography device Vertiguard were similar in both groups (Table 2); no significant differences were found between the two groups (p=0.5, Fisher’s exact test).
 |
Table 1 Mean Scores of Balance Tests and Questionnaires, Prior to Vestibular Rehabilitation |
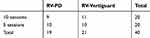 |
Table 2 Type of Rehabilitation by Posturography Conducted in the Two Study Groups |
Analyzing the sample as a whole, vestibular rehabilitation improved many posturographic parameters. Importantly, in the sensory organization test, the scores for the global balance of conditions 3, 4, 5 and 6, and the use of visual and, especially, vestibular information increased; in turn, the number of falls during the test decreased, as shown in Figure 1. Several parameters of the limits of stability also improved: speed of movement (2.55 ± 0.75 vs 2.85 ± 1.04, p=0.010), endpoint of displacement (52.48 ± 12.98 vs 56.74 ± 16.27, p=0.001), maximum displacement point (71.43 ± 13.21 vs 75.67 ± 16.574, p=0.004) and directional control (69.10 ± 12.87 vs 72.03 ± 16.36, p=0.036). We have not found improvement in the gSBDT, although the decrease in the score was almost significant (47.65 ± 10.07 vs 45.16 ± 7.61, p=0.062), in the timed up and go test (neither in the time nor in the steps necessary to complete the test) or in the questionnaires (neither in the DHI nor in the short FES-I).
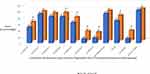 |
Figure 1 Scores for the sensory organization test of dynamic posturography, before and after vestibular rehabilitation (full group). *Significant differences. |
When analyzing each of the two groups separately, the same pattern of improvement is maintained as that observed in the total sample of the patients, albeit with less significance (by halving the sample size). With 10 sessions, some of the parameters of the sensory organization test (Figure 2) and the maximum displacement point in the limits of stability (71.90 ± 13.19 vs 74.15 ± 21.60, p=0.025) improved. We did not observe improvement in the gSBDT, in the timed up and go test, or in the questionnaires. Conversely, in the group that performed only 5 sessions, several parameters of the sensory organization test also improved (Figure 3), and the number of falls during the SOT significantly decreased (4.30 ± 2.41 vs 2.60 ± 2.30, p=0.005). The limits of stability also significantly improved: speed of movement (2.56 ± 0.76 vs 2.82 ± 0.94, p=0.048), endpoint of displacement (50.65 ± 11.44 vs 56.80 ± 11.58, p=0.001) and maximum displacement point (70.95 ± 13.56 vs 76.35 ± 9.37, p=0.048). As in the group of ten sessions, no changes occur in the gSBDT, in the timed up and go test, or in the questionnaires.
 |
Figure 2 Scores for the sensory organization test of dynamic posturography, before and after vestibular rehabilitation (group of ten sessions). *Significant differences. |
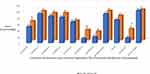 |
Figure 3 Scores for the sensory organization test of dynamic posturography, before and after vestibular rehabilitation (group of five sessions). *Significant differences. |
Lastly, when comparing the response to vestibular rehabilitation between the two treatment groups, we did not detect significant difference in any study parameter (neither in those that improved after vestibular rehabilitation nor in those in which rehabilitation produced no relevant changes). Pre- and post-rehabilitation differences in different parameters are outlined in Table 3.
 |
Table 3 Mean Differences in Balance Test Scores and Questionnaires Scores, Before and After Vestibular Rehabilitation, Between the Two Study Groups |
Discussion
Falls in the elderly are a key issue in the western societies. Their repercussions (fractures, hospital admissions and need for caregivers, among others) affect both the health-care systems and social services and families.9,10 All the strategies that contribute to reducing these repercussions must be promoted, considering the savings that they entail in both economic and morbidity and mortality terms. Vestibular rehabilitation (and, more specifically, vestibular rehabilitation by posturography) has proved effective in not only improving the balance of elderly patients but also reducing at least in the medium term the number of falls they suffer.8 Its main limitation is its high cost, which hinders its widespread use.
Several strategies can be applied to reduce the costs of vestibular rehabilitation by posturography. One of them is to use less expensive devices (more specifically, mobile posturography devices) than the computerized dynamic posturography device. In fact, in our study, we used both vestibular rehabilitation systems as another aim of our research project13 will be to assess whether the results from both systems are comparable. To avoid bias in the use of these two different rehabilitation strategies, the patients were distributed homogeneously between the two study groups. Moreover, they are similar techniques, since both use a biofeedback (in one visual and in the other vibratory) for rehabilitation exercises, they have a similar duration, and previous studies of our group (still pending publication) demonstrated similar benefits. Nevertheless, this is one of the limitations of this study. Conversely, the post-rehabilitation balance evaluation was performed at three weeks and not immediately after rehabilitation, to avoid learning bias that has been described in young adults after repeated sensory organization tests.18
A further option to reduce costs is to optimize the number of sessions required by each patient. Evidently, we must always individualize this decision according to the needs of each patient, in addition to establishing approximately the number of sessions that a priori are necessary to treat each disease. In postural instabilities of other origins (for example, secondary to a unilateral vestibular deficit), the number of sessions has already been optimized in a study which showed that the results from 5 sessions are virtually the same as those from protocols with 10 sessions.12 Indeed, when the evolution of the CDP-SOT was analyzed session by session in patients with postural instability of different causes undergoing vestibular rehabilitation by posturography, the mean value of the composite fundamentally increased throughout the first 5 rehabilitation sessions, whereas the improvement was only slight in the following 5 sessions.19 This decrease from 10 to 5 sessions results in halving the treatment costs (with the same resources, we can treat twice as many patients). If the results in elderly people with postural instability and at risk of falls were similar, the savings for health-care systems (and for families, since elderly patients usually need to go to the hospital accompanied by a relative or caregiver) would be significant, also increasing patient adherence to treatment, as we found in our study: we confirmed that vestibular rehabilitation by posturography (using both the dynamic posturography and the Vertiguard mobile posturography devices) improves short-term balance in elderly people with postural instability, with no significant differences between protocols of 10 and 5 sessions.
A surprising result was the lack of improvement in the questionnaires or in the timed up and go test, when comparing the results before and after vestibular rehabilitation. An increase in postural stability should lead to greater patient agility in movements and to lower perception of disability, along with a reduction in the fear of falling. A possible explanation for our findings is the fact that only 3 weeks have elapsed from the end of vestibular rehabilitation to evaluation. The improvement in balance observed in the posturographic tests may not yet have generated sufficient confidence in the patient to improve their agility in performing the timed up and go test, or to reverse the feeling of insecurity caused by postural instability. If the posturographic improvement is maintained over time, it should also entail improved scores in the timed up and go test and in the questionnaires.
The main limitation of our study is the short follow-up period (3 weeks). Longer follow-up periods are necessary to confirm that the improvement detected at three weeks persists in the medium and long term. Furthermore, a long-term follow-up will allow us to assess whether the improvement in balance translates into a decrease in the number of falls, as previously published.8 However, we consider the balance evaluation at three weeks relevant in this age group, especially if we confirm that the improvement is not maintained over time. In this case, a protocol for “memory” vestibular rehabilitation sessions will have to be established to consolidate good balance and to reduce the risk of falls.
Conclusion
In conclusion, in light of the results from our study, 5-session protocols of vestibular rehabilitation by posturography in elderly patients with postural instability are as effective as 10-session protocols in improving balance. Although these figures may serve as a reference, the specific number of sessions should be nevertheless decided individually for each patient, based on their progress and their conditions (comorbidities, distance to their home, and need or not for a companion, among others).
Data Sharing Statement
The datasets used in the present study, anonymized, are available from the corresponding author on reasonable request.
Acknowledgments
This study has been funded by the project PI1500329, integrated into the Spanish State Plan for R + D + I and funded by the Instituto de Investigación en Salud Carlos III – ISCIII – Subdirección general de Evaluación y Fomento de la Investigación and the Fondo Europeo de Desarrollo regional (FEDER).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Rossi-Izquierdo M, Gayoso-Diz P, Santos-Pérez S, et al. Short-term effectiveness of vestibular rehabilitation in elderly patients with postural instability: a randomized clinical trial. Eur Arch Otorhinolaryngol. 2017;274(6):2395–2403. doi:10.1007/s00405-017-4472-4
2. Basta D, Rossi-Izquierdo M, Soto-Varela A, et al. Efficacy of a vibrotactile neurofeedback training in stance and gait conditions for the treatment of balance deficits: a double-blind, placebo-controlled multicenter study. Otol Neurotol. 2011;32(9):1492–1499. doi:10.1097/MAO.0b013e31823827ec
3. Public Health England with the National Falls Prevention Coordination Group member organisations. Falls and fracture consensus statement. Supporting commissioning for prevention. 2017. Available from: https://assets.publishing.service.gov.uk/government/.
4. Updated American Geriatrics Society/British Geriatrics Society Clinical Practice Guideline for Prevention of Falls in Older Persons and Recommendations: Prevention of Falls in Older Persons AGS BGS Clinical Practice Guideline 2010. 2010. Available from: https://geriatricscareonline.org/ContentAbstract/practice_guideline_for_preventionof_falls/CL014/CL014_BOOK003.
5. National Institute for Health and Care Excellence. 2019 surveillance of falls in older people: assessing risk and prevention (NICE guideline CG161). 2019. Available from: https://www.nice.org.uk/guidance/cg161/resources/2019-surveillance-of-falls-in-older.
6. Blain H, Masud T, Dargent-Molina P, et al. A comprehensive fracture prevention strategy in older adults: the European Union Geriatric Medicine Society (EUGMS) statement. J Nutr Heal Aging. 2016;20(6):647–652. doi:10.1007/s12603-016-0741-y
7. Sherrington C, Michaleff ZA, Fairhall N, et al. Exercise to prevent falls in older adults: an updated systematic review and meta-analysis. Br J Sports Med. 2017;51(24):1750–1758. doi:10.1136/bjsports-2016-096547
8. Rossi-Izquierdo M, Gayoso-Diz P, Santos-Pérez S, et al. Vestibular rehabilitation in elderly patients with postural instability: reducing the number of falls—a randomized clinical trial. Aging Clin Exp Res. 2018;30(11):1353–1361. doi:10.1007/s40520-018-1003-0
9. Gillespie LD, Robertson MC, Gillespie WJ, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2012;9:CD007146.
10. Ungar A, Rafanelli M, Iacomelli I, et al. Fall prevention in the elderly. Clin Cases Miner Bone Metab. 2013;10(2):91–95.
11. Soto-Varela A, Faraldo-García A, Del-Río-Valeiras M, et al. Adherence of older people with instability in vestibular rehabilitation programmes: prediction criteria. J Laryngol Otol. 2017;131(3):232–238. doi:10.1017/S0022215116009932
12. Rossi-Izquierdo M, Santos-Pérez S, Rubio-Rodríguez JP, et al. What is the optimal number of treatment sessions of vestibular rehabilitation? Eur Arch Otorhinolaryngol. 2014;271(2):275–280. doi:10.1007/s00405-013-2423-2
13. Soto-Varela A, Gayoso-Diz P, Faraldo-García A, et al. Optimising costs in reducing rate of falls in older people with the improvement of balance by means of vestibular rehabilitation (ReFOVeRe study): a randomized controlled trial comparing computerised dynamic posturography vs mobile vibrotactile posturogra. BMC Geriatr. 2019;19(1):1. doi:10.1186/s12877-018-1019-5
14. Podsiadlo D, Richardson S. The timed “up & go”: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc. 1991;39(2):142–148. doi:10.1111/j.1532-5415.1991.tb01616.x
15. Vaillant J, Martigné P, Vuillerme N, et al. Modification des performances au Timed « Up and Go » test et à l’appui monopodal par l’addition d’une charge cognitive: valeur discriminative des résultats. Ann Réadaptation Médecine Phys. 2006;49(1):1–7. doi:10.1016/j.annrmp.2005.07.002
16. Pérez N, Garmendia I, Martín E, et al. Adaptación cultural de dos cuestionarios de medida de la salud en pacientes con vértigo. Acta Otorrinolaringol Esp. 2000;51(7):572–580.
17. Kempen GIJM, Yardley L, JCM VH, et al. The short FES-I: a shortened version of the falls efficacy scale-international to assess fear of falling. Age Ageing. 2008;37(1):45–50. doi:10.1093/ageing/afm157
18. Wrisley DM, Stephens MJ, Mosley S, et al. Learning effects of repetitive administrations of the sensory organization test in healthy young adults. Arch Phys Med Rehabil. 2007;88(8):1049–1054. doi:10.1016/j.apmr.2007.05.003
19. Rossi Izquierdo M, Soto-Varela A, Santos-Pérez S, et al. Análise prospectivo dos resultados da reabilitaçao vestibular mediante posturografía dinâmica computorizada em pacientes com instabilidade. Clin Inves Otorri. 2008;2(1):12–16.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
