Back to Journals » Therapeutics and Clinical Risk Management » Volume 15
Usefulness of bounce-back admission in monitoring the quality of practice in the emergency department
Authors Tarumi Y , Harada T, Saito T , Hiroshige J , Dohi K
Received 8 November 2018
Accepted for publication 19 March 2019
Published 6 May 2019 Volume 2019:15 Pages 647—658
DOI https://doi.org/10.2147/TCRM.S193863
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Garry Walsh
Yoko Tarumi,1 Taku Harada,1 Tsukasa Saito,1 Juichi Hiroshige,1 Kenji Dohi2
1Department of General Medicine, Showa University, Tokyo 142-8555, Japan; 2Department of Emergency, Disaster and Critical Care Medicine, Showa University, Tokyo 142-8555, Japan
Background: Recently, unscheduled readmissions after discharge from the emergency department (ED) (bounce-back admissions, BBAs) have been monitored as a hospital performance measure in countries other than Japan. It has been suggested that BBAs may be caused by errors in diagnoses or treatments.
Purpose: This retrospective cohort study aimed to evaluate BBAs and improve the quality of medical care in the ED of Showa University Hospital by analyzing the data of adult patients (≥18 years) with index visits to the ED of Showa University Hospital between June 2011 and May 2013 (n=15,069).
Patients and methods: Patients were registered and followed up for unscheduled admissions to this hospital within 7 days. In order to understand the reasons for BBAs, individual diagnoses upon BBA were compared to the corresponding diagnoses upon discharge.
Results: Among the 11,669 discharged patients, 180 patients were admitted within 3 days after discharge (3-day BBAs), and 257 were admitted within 7 days after discharge (7-day BBAs). The main diagnoses upon admission (BBA) were pneumonia or exacerbation of chronic obstructive pulmonary disease (COPD) or asthma (n=40, 16%), cholecystitis or cholangitis (n=21, 8.2%), and urinary tract infection (n=16, 6.2%). Among the 7-day BBA cases, 117 patients had similar and 110 patients had different diagnoses upon discharge and admission; in the remaining 30 cases, the results could not be ascertained owing to incomplete diagnostic data. In the cases of pneumonia, exacerbation of COPD or asthma, and colitis or enterocolitis, there was a significantly higher “similar” diagnoses than “different”, while the reverse was true for cases of stroke, ileus or bowel obstruction, and meningitis. These results were shared with the ED staff, and similar surveillances were periodically conducted. The frequency of admission within 7 days after discharge continuously declined from 2013 to 2016.
Conclusion: Analyzing the discharge and admission diagnoses may help ED staff to understand the reasons for common errors in order to follow the plan-do-check-act cycle of medical care in the ED.
Keywords: unscheduled admission after ED discharge, analysis of diagnosis, improvement of emergency care quality
Introduction
In the emergency department (ED), it can be difficult for physicians to effectively determine which patients might benefit from admittance, and which patients should be discharged.1 Most emergency patients are discharged from the ED without additional complications in overcoming their diseases and/or injuries.2 Nonetheless, there are cases where patients may need to be readmitted after discharge, making management errors a risk to patient health and wellbeing.1
In recent years, there has been an effort to evaluate the quality of emergency practices in a few countries other than Japan using some indicators such as revisits shortly after discharge,3–9 unplanned revisits10,11 unplanned readmissions,12 and admissions to the intensive care unit.13 Those studies reported that readmissions rather than revisits shortly after discharge may reflect errors of medical practice in the index ED visit.6 In contrast, one study reported that patients who were discharged during their first ED visits and admitted during a return visit to the ED had lower in-hospital mortality, lower ICU admission rates, and lower in-hospital costs than patients hospitalized during the initial index visit.8
ED practice is characterized by various complaints and different levels of urgency and severity in patients. There are typically no difficulties in the management of patients with obviously severe disease at their first ED visit. On the other hand, trying to reach a diagnosis rapidly with minimal paraclinical evaluation may sometimes lead to difficult decisions regarding patient discharge.
It is not easy to understand the causal relations associated with unexpected death or deterioration of the patient’s status upon the initial ED visit. Gabayan et al reported that bounce-back admissions (BBA), in the absence of non-medical factors, may be an indicator of inadequate ED or follow-up care.6 Emergency patients and their families expect accurate diagnoses and proper management and care, and so, they will feel dissatisfied with admissions shortly after discharge. In Japan, it is important to make efforts to reduce the cases of BBA as patients may access any hospital they choose, and the choice of the hospital on their next visit may be affected by their satisfaction with the initial ED care.
To date, evaluation of the emergency medical practice and comparison of its quality in multiple medical institutions have not been performed in Japan. The differences in emergency, severity, and proportion of diseases or injuries among patients who visit the ED in different countries could make comparisons between studies in other countries and those in Japan difficult. We planned this study to determine the suitability of 7-day BBA (7d-BBA) in the evaluation of emergency medical practice, with the ultimate goal of improving the quality of emergency medicine.
Materials and methods
Study design and setting
We conducted a retrospective cohort study of ED patients older than 18 years who visited the Emergency Department of Showa University Hospital between June 2011 and May 2013. The hospital is a tertiary and educational hospital for advanced care and has 853 beds. In the entire ED of this hospital, there were a total of 22,981 visits in 2011 and 20,502 in 2012. The study protocol was approved by the ethical committee on human studies of Showa University (Approval number: 2224). As this study was retrospective and made no intervention, upon advisement from the ethics committee, the requirement for informed consent was satisfied by allowing subjects to opt-out, either through our web-page or by following the instructions on a poster. The data were de-identified to maintain the confidentiality of private information of the patients.
Following the ED protocol of Showa University Hospital at the time of study initiation, emergency patients who were critical were referred by his/her primary care physician or were in emergencies related to specialized fields (ie, obstetrics, gynecology. ophthalmology, dermatology, and otorhinolaryngology) did not visit the ED because they were provided medical care in a specific department such as a critical care center and were thus excluded from the present study. During the time of the study, a total of 54 physicians with 3–29 years of experience (median 10 years) worked at the ED, specializing in general medicine, internal medicine, digestive surgery, orthopedics, plastic surgery, neurosurgery, and urology. Three or 4 physicians (including residents) and 4 nurses work the daytime shift and 4 or 5 doctors and 4 nurses the night shift. Acceptance of emergency patients was decided by physicians, and triage was performed by nurses. Trauma patients were not accepted if surgeons were not working their shift. There were no uniform criteria for patient management, but all were patients were attended by physicians with more than 3 years of experience, and they were free to consult with a specialist as needed.
The data in this study span a time period corresponding to a change in the acceptance protocol at Showa University Hospital ED. From 2014, acceptance of emergency “walk-in’ patients has been decided by nurses rather than doctors. In addition, many specialists have abolished night shifts, beginning from April 2017, which has made it difficult for ED doctors to consult with them during the night. In this study, we aimed to analyze the standard frequency of BBAs in Showa University Hospital, the effect of removing physicians from the decision to accept patients, and the effect of a backup system.
Main outcomes and measures
The main outcomes were unscheduled admission to Showa University hospital or death within 3 days and/or 7 days after ED discharge instructed by physicians (3d-BBA and 7d-BBA). Cases of cardiopulmonary arrest upon arrival were included in the death cases, and those cases where the dates of death were unknown were excluded. The diagnoses on the index ED visits and on admissions were investigated to identify any errors in diagnosis or management. The dates of discharge were also checked to compare the cases of 7d-BBA and those admitted at the index visit for the length of hospitalization and the time from initial visit to discharge.
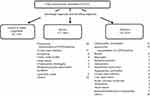
We registered each patient who visited the Emergency Department of Showa University hospital upon entering the ED. We checked the registered patients one month after their index visits to identify any patients who were admitted to Showa University hospital within 7 days after ED discharge. In those cases where patients were admitted within 24 hrs of visiting the ED, we first checked the medical record to determine if the discharge was instructed by a physician. We also identified cases of cardiopulmonary arrest upon arrival and cases who were readmitted to other hospitals during the revisit. The following information was sought from the medical records, referral letters to the specialists, and admission summaries: (1) any difference in the diagnoses on the first visit and on the revisit and (2) unexpected deterioration of the patients’ conditions. Cases of scheduled admission and admission for nonurgent examination, elective surgeries, and social reasons were excluded from this study. We also excluded cases of exacerbation of known malignancy because their admissions were determined both clinically and upon request, in consultation with the attending doctor (Figure 1).
Statistical analysis
Wilcoxon’s rank-sum tests were used to explore differences across the length of hospitalization and period from index visit to discharge in the cases of admission on index visit and 7d-BBA for the same diseases.
When the number of cases was five or more, chi-square tests were used, and when case numbers were less than five, Fisher’s exact tests were used to assess the distribution of admission reasons (diagnosis or management errors) for the same disease.
The Spearman rank method was used to explore the correlation between monthly frequency of 7d-BBA and periods of employment in ED physicians. The periods of employment were calculated on a group basis, according to the number of months from the changes that were implemented. The correlation coefficients were then calculated for the number of months employed and the frequency of 7d-BBA.
Statistical analyses were performed using JMP pro13 statistics program (SAS Institute Inc.; North Carolina, USA).
Results
A total of 15,069 adult patients visited the department during the study period (24% of the patients were transferred by ambulance, median age 57, interquartile range; IQR 36–75), with 11,669 (77%) discharged patients being registered (median age 51, IQR 38–72).
The most frequent diagnoses on the index visit were colitis and enterocolitis (n=1,213), pneumonia, exacerbation of chronic obstructive pulmonary disease (COPD) or asthma attack (n=833), and acute upper respiratory infection (n=617). The most frequent causes of admission on index visit were pneumonia, exacerbation of COPD or asthma attack (n=318), stroke or TIA (n=238), gastrointestinal bleeding (n=161), heart failure (n=149), and ileus or bowel obstruction (n=148).
Three hundred and forty-six patients (3.0% of the discharged patients) were admitted within 7 days after the index visit. Of these, 257 patients (2.2% of the discharged patients) were determined to be 7d-BBAs, with a median period of discharge to admission of 2 days (IQR 1–4 days). One hundred and eighty patients (1.5% of the discharged patients, 70% of the 7d-BBA patients) were admitted within 3 days after discharge (Figure 2). There was one patient who presented with cardiopulmonary arrest upon arrival, but none were readmitted to other hospitals during the revisit.
The main diagnoses upon discharge in the 7d-BBAs were pneumonia or exacerbation of COPD or asthma (n=38, 15%), acute upper respiratory infection (n=20, 7.9%), and acute colitis or enterocolitis (n=19, 7.4%). The main diagnoses upon BBA were pneumonia or exacerbation of COPD or asthma (n=40, 16%), cholecystitis or cholangitis (n=21, 8.2%), and urinary tract infection (n=16, 6.2%) (Table 1).
 | Table 1 Detailed list of diagnoses in 7-day bounce-back admission cases (n=257) |
The main diagnoses upon discharge in the patients who were not 7d-BBAs (n=11,412) were acute colitis enterocolitis (n=1,116, 9.8%), acute upper respiratory infection (n=581, 5.1%), psychosomatic symptoms (n=517, 4.5%), pneumonia or exacerbation of COPD or asthma (n=492, 4.3%), and peripheral vertigo (n=418, 4.3%).
When comparing admitted cases with the same diagnosis on index visit, there was no significant difference in the length of hospitalization and the period from index visit to discharge in the 7d-BBAs for different diseases except for “pneumonia or exacerbation of COPD/asthma” (Figure 3). However, as there were significant differences in age between 7d-BBAs and “admission on index visit” patients for meningitis and appendicitis, diverticulitis, or perforation, we stratified and compared four age groups (18–39, 40–59, 60–79, over 80) for each disease. In the 7d-BBA age groups of 18–39 and 40–59-year-olds with pneumonia, exacerbation of COPD or asthma, the period from index visit to discharge was significantly longer than those of “admission on index visit” (Table 2).
Upon cross-checking the diagnoses from the initial ED visits and the admissions, 115 (45%) patients had similar and 112 (44%) patients had different diagnoses upon discharge and admission; in the remaining 30 (12%) cases, the results could not be ascertained owing to incomplete diagnostic data. The main diagnoses in the “similar” group were pneumonia, exacerbation of COPD or asthma, urinary tract infection, and colitis, and those in the “different” group were cholecystitis or cholangitis, pneumonia, exacerbation of COPD or asthma, and stroke (Figure 4). In the cases of pneumonia, exacerbation of COPD or asthma, and the case of colitis or enterocolitis, there was a significantly higher “similar” diagnosis than “different”, while the reverse was true for cases of stroke, ileus or bowel obstruction, and meningitis (Table 3).
 | Table 3 Comparison of BBA distributions when admission and discharge diagnoses were known (n=227) |
We observed no significant correlation between monthly frequency of 7d-BBA (median 2.25%, IQR 1.77–2.47%) and periods of employment in ED physicians (Spearman’s rank-correlation coefficient −0.1530, p=0.4755) (Figure 5).
Discussion
The acceptable number of BBAs has not been determined to date.15 However previous studies in other countries3,5,6,8,11,13,14 have reported the incidence of 7d-BBAs from 1.2%8 to 2.6%,6 up to 6.7%,16 and for 3d-BBAs from 0.53,14 to 1.5%.5,11,15 The results from this study were close to these reported incidences. The variability of 7d-BBAs in previous studies did not seem to be caused by the difference in the country, study duration, or the number of participants. However, our results might not be generalizable to other hospitals in Japan. In addition, we investigated only BBAs revisiting our hospital, which is a limitation of this study.
There are some challenges in determining the acceptable number of 7d-BBAs, such as the inherent differences in the emergency and insurance medical systems in different countries, the scale of facilities, and the number of staff in the ED. In addition, there are inherent challenges in Japan, namely, ED systems are not standard nationwide; there are no laws or regulations on non-acceptance of patients, and so physicians are allowed to refuse admittance to patients who require specialty services not available in the hospital, and patients can visit any hospital. In many cases, they visit tertiary hospitals at their discretion after visiting primary or secondary hospitals. As patients can visit any hospital and the definitions of “emergency patients” are different depending on the hospital, it is very difficult to investigate BBAs using national databases (such as the receipt information provided by the Ministry of Health, Labour and Welfare).
Hence, it is more practical to determine a range for the number of 7d-BBAs in a particular facility than it is to compare the number of 7d-BBAs in a hospital with a standard acceptable number.
Studies on factors influencing readmissions shortly after discharge from the ED are in process. Studies on the association between diagnoses and patient readmissions have reported that many of the readmissions were for exacerbation of chronic diseases such as chronic kidney disease, congestive heart failure, blood diseases, neoplasms, and mental illness6 or recurrences of chronic diseases such as urolithiasis, functional headache, vertigo, or coronary diseases.15 In this study, the main diseases of 7d-BBAs were recurrent or acute diseases of the respiratory, abdominal, and genitourinary systems such as pneumonia or exacerbation of COPD/asthma, cholecystitis/cholangitis, urinary tract infection, colitis/enterocolitis, and ileus. These findings were somewhat similar to those reported in previous studies.
In this study, patients in the 7d-BBA group had a shorter period of recovery and hospitalization than those admitted for the same disease on the index visit. As a consequence, the calculated costs for treatment did not increase; hence, 7d-BBAs might not necessarily be labeled as clinically or economically adverse results. However, we believe that 7d-BBA is considered an error in diagnosis when the discharge diagnosis and the admission diagnosis are different, and an error in management when both diagnoses are similar. Cheng et al reported that there were 12.1% diagnostic errors in cases returning to the ED within 72 hrs after discharge.5 Our results showed a higher proportion of diagnostic errors. Overall, most errors in this study could be attributed to ED visits at the early stages of the disease because most 7d-BBA patients were admitted within 2 days after index visit, and the periods from index visit to discharge did not significantly differ from the length of hospitalization except for pneumonia or COPD/asthma.
Diagnostic errors might have been made because of the absence of disease-specific symptoms leading the clinician to the specific examinations required for a definitive diagnosis (eg, in cases of cholecystitis or meningitis) or the presence of atypical symptoms (eg, in cases of stroke). Management errors might have been due to the improper prediction of the exacerbation of disease or the influence of the underlying disease on the course of the current problem (eg, respiratory infection and enterocolitis). In cases of similar diagnosis, apart from the potential for management error, patient-related factors such as drug non-compliance and problems in home care might also have played a role.
The results of this study were shared with the ED staff of Showa University Hospital. The guidelines on basic treatment strategies, indications for admission to the hospital, and follow-up duration in the ED were updated following this assessment. The effect of this intervention is unknown at present. However, positive effects may be expected because learning about rare cases occurs more efficiently in a group setting.
We have conducted similar surveillance periodically to test the outcome of these guidelines. For the period from 2013 to 2015, we counted only the cases of admission within 7days after discharge because determining which cases met the exclusion criteria was time-consuming. The frequencies of admission within 7 days after discharge were 3.33–3.64%. The frequency of 7d-BBA in the fiscal period 2016 was 2.48% (153/6165) (Figure 6). In this period, the protocol for patient acceptance had changed, and the proportion of trauma patients had markedly increased (from 1.5% to 20%). These situations may have increased cases of scheduled admissions for elective surgery and cases of 7d-BBAs caused by time constraints. Hence, this data might not necessarily reflect the deteriorating quality of medical care. At least, a continuous decline from 2013 to 2016 might be the effect of the intervention.
We think that periodic monitoring of BBA in a single facility can result in an improvement in the quality of ED practice, by focusing on the plan-do-check-act cycle.
Limitations
Our study has several limitations. First, we investigated only BBAs revisiting our hospital. Hence, we might have underestimated the true frequency of BBAs. Second, accurate information on comorbidities in patients are lacking; hence, we could not always accurately classify diagnoses and could not consider the influence of his/her comorbidities on the hospitalization period. Third, we did not investigate the possibility that the admitted diagnoses had changed in cases of admission on index visits. Hence, we did not compare the frequency of errors in cases of 7d-BBA and cases of “admission on index visit”. Fourth, medical records were managed in writing and were not written in a fixed format. Hence, we could not identify an accurate diagnosis in multiple cases. Fifth, the number of individual disease cases was insufficient; hence, additional factors that may have influenced 7d-BBAs could not be considered adequately.
Conclusion
The incidence of BBA is a useful indicator of the quality of ED practice. Comparing discharge and admission diagnoses to assess the rate of error, improving the procedures in ED practice, and reinvestigating BBAs may be helpful in improving the quality of the ED practice. Further multicentric studies are necessary to determine the standard and target levels of BBAs in Japan and to compare these with the results of previous studies.
Data availability
The availability of data used in this study is restricted by the ethical committee on human studies of Showa University in order to protect patient privacy. Data are available from Yoko Tarumi ([email protected]) for researchers who meet criteria for access to confidential data and upon reasonable request.
Acknowledgments
We would like to thank Editage (
Disclosure
The authors report no conflicts of interest in this work.
References
1. Calder LA, Arnason T, Vaillancourt C, Perry JJ, Stiell IG, Forster AJ. How do emergency physicians make discharge? Emerg Med J. 2015;32(1):9–14. doi:10.1136/emermed-2013-203527
2.
3. Martin-Gill C, Reiser RC. Risk factors for 72 hr admission to the ED. Am J Emerg Med. 2004;22(6):448–453. doi:10.1016/j.ajem.2004.07.023
4. Wu CL, Wang FT, Chiang YC, et al. Unplanned emergency department revisits within 72 hrs to a Secondary Teaching Referral Hospital in Taiwan. J Emerg Med. 2010;38(4):512–517. doi:10.1016/j.jemermed.2008.03.039
5. Cheng SY, Wang HT, Lee CW, Tsai TC, Hung CW, Wu KH. The characteristics and prognostic predictors of unplanned hospital admission within 72 hrs after ED discharge. Am J Emerg Med. 2013;31(10):1490–1494. doi:10.1016/j.ajem.2013.08.004
6. Gabayan GZ, Asch SM, Hsia RY, et al. Factors associated with short-term bounce-back admissions after emergency department discharge. Ann Emerg Med. 2013;62(2):136–144.e1. doi:10.1016/j.annemergmed.2013.01.017
7. Hsia RY, Asch SM, Weiss RE, et al. Is emergency department crowding associated with increased “bounceback” admissions? Med Care. 2013;51(11):1008–1014. doi:10.1097/MLR.0b013e318270baf2
8. Sabbatini AK, Kocher KE, Basu A, Hsia RY. In-hospital outcomes and costs among patients hospitalized during a return visit to the emergency department. JAMA. 2016;315(7):663–671. doi:10.1001/jama.2016.0649
9. Fabbian F, Boccafogli A, De Giorgi A, et al. The crucial factor of hospital readmissions: a retrospective cohort study of patients evaluated in the emergency department and admitted to the department of medicine of a general hospital in Italy. Eur J Med Res. 2015;20:6. doi:10.1186/s40001-014-0081-5
10. van der Linden MC, Lindeboom R, de Haan R, et al. Unscheduled return visits to Dutch inner-city emergency department. Int J Emerg Med. 2014;7:23. doi:10.1186/s12245-014-0023-6
11. Hu KW, Lu YH, Lin HJ, Guo HR, Foo NP. Unscheduled return visits with and without admission post emergency department discharge. J Emerg Med. 2012;43(6):1110–1118. doi:10.1016/j.jemermed.2012.01.062
12. Meldon SW, Mion LC, Palmer RM, et al. A brief risk-stratification tool to predict repeat emergency department visits and hospitalizations in older patients discharged from the emergency department. Acad Emerg Med. 2003;10(3):224–232. doi:10.1197/aemj.10.3.224
13. Fan JS, Kao WF, Yen DH, Wang LM, Huang CI, Lee CH. Risk factors and prognostic predictors of unexpected intensive care unit admission within 3 days after ED discharge. Am J Emerg Med. 2007;25(9):1009–1014. doi:10.1016/j.ajem.2007.03.005
14. Abualenain J, Frohna WJ, Smith M, et al. The prevalence of quality issue and adverse outcomes among 72 hr return admissions in the emergency department. J Emerg Med. 2013;45(2):281–288. doi:10.1016/j.jemermed.2012.11.012
15. Hocagil AC, Bildik F, Kilicaslan I, et al. Evaluating unscheduled readmission to emergency department in the early period. Balkan Med J. 2016;33(1):72–79. doi:10.5152/balkanmedj.2015.15917
16. Greenberg SA, Halpern P, Ziv-Baran T, Gamzu R. Reduced hospitalization rate are not associated with increased mortality or readmission rates in an emergency department in Israel. Isr J Health Policy Res. 2018;7(1):69. doi:10.1186/s13584-018-0265-5
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.