Back to Journals » Therapeutics and Clinical Risk Management » Volume 15
Use Of Regional Anesthesia For Lower Extremity Amputation May Reduce The Need For Perioperative Vasopressors: A Propensity Score-Matched Observational Study
Authors Kim SJ , Kim N , Kim EH , Roh YH , Song J , Park KH , Choi YS
Received 25 April 2019
Accepted for publication 14 September 2019
Published 2 October 2019 Volume 2019:15 Pages 1163—1171
DOI https://doi.org/10.2147/TCRM.S213443
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Garry Walsh
Seon Ju Kim,1 Namo Kim,2,3 Eun Hwa Kim,4 Yun Ho Roh,4 Jeehyun Song,2 Kwang Hwan Park,5,* Yong Seon Choi2,3,*
1Department of Anesthesiology and Pain Medicine, National Health Insurance Service Ilsan Hospital, Goyang 10444, Korea; 2Department of Anesthesiology and Pain Medicine, Anesthesia and Pain Research Institute, Yonsei University College of Medicine, Seoul 03722, Korea; 3Anesthesia and Pain Research Institute, Yonsei University College of Medicine, Seoul 03722, Korea; 4Biostatistics Collaboration Unit, Department of Biomedical Systems Informatics, Yonsei University College of Medicine, Seoul 03722, Korea; 5Department of Orthopaedic Surgery, Yonsei University College of Medicine, Seoul 03722, Korea
*These authors contributed equally to this work
Correspondence: Yong Seon Choi
Department of Anesthesiology and Pain Medicine, Anesthesia and Pain Research Institute, Yonsei University College of Medicine, 50-1, Yonsei-ro, Seodaemun-gu, Seoul 03722, Korea
Tel +82 2 2228 2412
Fax +82 2 2228 7897
Email [email protected]
Kwang Hwan Park
Department of Orthopaedic Surgery, Yonsei University College of Medicine, 50-1, Yonsei-ro, Seodaemun-gu, Seoul 03722, Korea
Tel +82 2 2228 2185
Fax +82 2 2228 7897
Email [email protected]
Purpose: Lower extremity amputation (LEA) is associated with a high risk of postoperative mortality. The effect of type of anesthesia on postoperative mortality has been studied in various surgeries. However, data for guiding the selection of optimal anesthesia for LEA are limited. This study aimed to determine the effect of anesthesia type on perioperative outcomes in patients with diabetes and/or peripheral vascular disease undergoing LEA.
Patients and methods: We reviewed the medical records of patients who underwent LEA at our center between September 2007 and August 2017, who were grouped according to use of general anesthesia (GA) or regional anesthesia (RA). Primary outcomes were 30-day and 90-day mortality. Secondary outcomes were postoperative morbidity, intraoperative events, postoperative intensive care unit admission, and postoperative length of stay. Propensity score-matched cohort design was used to control for potentially confounding factors, including patient demographics, comorbidities, medications, and type of surgery.
Results: Five hundred and nineteen patients (75% male, mean age 65 years) were identified to have received GA (n=227) or RA (n=292) for above-knee amputation (1.5%), below-knee amputation (16%), or more minor amputation (82.5%). Before propensity score matching, there was an association of GA with coronary artery disease (44% [GA] vs 34.5% [RA], p=0.028), peripheral arterial disease (73.1% vs 60.2%, p=0.002), and preoperative treatment with aspirin and clopidogrel (68.7% vs 55.1%, p=0.001; 63% vs 41.8%, p<0.001, respectively). Propensity score matching produced a cohort of 342 patients equally divided between GA and RA. There was no significant between-group difference in 30-day (3.5% vs 2.9%, p=0.737) or 90-day (6.4% vs 4.6%, p=0.474) mortality or postoperative morbidity. However, postoperative ICU admission (14.6% vs 7%, p=0.032), intraoperative hypotension (61.4% vs 14.6%, p<0.001), and vasopressor use (52% vs 14%, p<0.001) were more common with GA than with RA.
Conclusion: Type of anesthesia did not significantly affect mortality or morbidity after LEA. However, intraoperative hypotension, vasopressor use, and postoperative ICU admission rates were lower with RA.
Keywords: lower extremity amputation, diabetes, peripheral vascular disease, type of anesthesia, mortality, morbidity
Introduction
Diabetes and peripheral vascular disease are the leading causes of lower extremity amputation (LEA). LEA is a commonly performed procedure that is indicated in patients with failed attempts at revascularization, comorbidity or anatomic factors precluding revascularization efforts, and extensive tissue loss or infection.1 Patients who undergo LEA usually have comorbidities, including hypertension, heart failure, and end-stage renal disease, and are likely to be in an older age group. Furthermore, these patients have advanced systemic atherosclerotic disease involving not only the peripheral limbs but also the coronary, cerebral, and renal circulations.2 The incidence of coronary artery disease in patients with peripheral artery disease who require LEA is estimated to be as high as 80%,3 and some receive interventional treatment before surgery and ongoing dual antiplatelet therapy. These patients are at high perioperative risk, so the anesthesiologist needs to choose the appropriate anesthetic method carefully.
Theoretically, regional anesthesia (RA) offers several advantages over general anesthesia (GA). A previous study has demonstrated advantages of RA in procedures involving a lower extremity, including fewer pulmonary complications, a decreased risk of arterial or venous thrombosis, avoidance of mechanical ventilation, and a reduced requirement for blood transfusion.4 Compared with GA, neuraxial anesthesia, in particular, has been associated with lower 30-day mortality and decreased morbidity, less blood loss, fewer surgical site infections, and a decreased rate of admission to critical care services after elective total hip or knee arthroplasty.5
It is well established that LEA secondary to diabetes and/or peripheral vascular disease has a high perioperative mortality rate.6 Postoperative 30-day mortality rates after LEA have been reported to be between 7% and 22%.7 According to previous studies,8–11 advanced age, dependent functional status, proximal (eg, above-knee) amputation, a history of cardiac disease, chronic renal disease, preoperative sepsis, and use of steroids are associated with postoperative mortality. However, although there have been several recent reports on the effect of anesthetic methods on postoperative outcome in patients with LEA, no clear consensus has been established.
The purpose of this retrospective, propensity score-matched cohort study was to analyze the effect of type of anesthesia on postoperative mortality and morbidity in patients undergoing LEA because of diabetes and/or peripheral vascular disease.
Materials And Methods
Study Population
The study protocol was approved by the institutional review board (IRB) of Severance Hospital, Yonsei University Health System (IRB No. 4-2017-0979) and carried out in accordance with the rules of the Declaration of Helsinki of 1975. The patient records and information were anonymized before analysis, so the requirement for written informed consent to access medical records was waived. We retrospectively identified all patients who underwent LEA because of diabetic foot or peripheral vascular disease at Severance Hospital between September 30, 2007 and August 31, 2017. The LEAs included both major (above-knee and below-knee) and minor (distal to below-knee) amputations. The exclusion criteria were age under 20 years at the time of surgery, amputation secondary to trauma or malignancy, and LEA performed with concomitant surgery. Patients with incomplete medical records, those who were lost to follow-up, and those undergoing RA that was converted to GA were excluded.
The study population was divided into 2 groups based on anesthesia modality, ie, a GA group and an RA group. GA consisted of endotracheal intubation or use of a laryngeal mask airway with a combination of inhalational anesthetics and intravenous narcotics for maintenance of anesthesia. RA was defined as spinal anesthesia or peripheral nerve block with or without sedation.
Study Objectives
The primary study outcome was 30-day and 90-day mortality. The secondary outcomes were postoperative length of stay, need for admission to the postoperative intensive care unit (ICU), 90-day morbidity, and intraoperative events.
Patient Demographics And Perioperative Variables
Standard demographic data, including age, sex, and body mass index, as well as American Society of Anesthesiologists physical status classification were obtained for all patients. Data on comorbidities were also collected, including history of diabetes, hypertension, coronary artery disease, peripheral artery disease, congestive heart failure, cerebrovascular accident, chronic kidney disease, chronic obstructive pulmonary disease, and smoking history. Preoperative use of aspirin, clopidogrel, steroids, insulin, and statins was also recorded. Preoperative laboratory data included hemoglobin, platelets, prothrombin time, activated partial thromboplastin time, glucose, glycated hemoglobin, creatinine, estimated glomerular filtration rate, albumin, and C-reactive protein. The type of surgery (ie, amputation level), operating time, and anesthesia time were recorded. Information on intraoperative events, such as presence of hypoxia or hypotension, use of a vasopressor (ie, ephedrine, phenylephrine, norepinephrine, or vasopressin), and transfusion of blood products, were obtained. The postoperative variables included death, cardiovascular, pulmonary, renal, and neurologic complications, sepsis, and wound healing complications. Postoperative admission to the ICU and postoperative length of stay were also assessed.
Statistical Analysis
We used a propensity score-matched cohort design to control for potentially confounding factors. This type of design is intended to mimic a randomized trial by selecting comparison cohorts that are similar in regard to the probability, or “propensity,” of receiving the intervention (GA or RA) under study.12 In this model, the type of anesthesia was used as the dependent variable. The independent variables were those identified in earlier studies as being significant in terms of study outcomes as well as those that might, in the opinion of the authors, make a contribution. Propensity scoring was based on the model and included patient demographics (age, sex, and body mass index), comorbidities (diabetes, hypertension, coronary artery disease, peripheral artery disease, congestive heart failure, cerebrovascular accident, chronic kidney disease, chronic obstructive pulmonary disease, and smoking history), medications (aspirin, clopidogrel, steroid, insulin, and statin), and type of surgery. We then matched each case with GA to a case with RA that had a similar propensity score; 1:1 propensity score matching was performed to match patients with RA to controls within a caliper of 0.01. In our matching algorithm, we performed 1:1 nearest neighbor matching.
For unmatched data, the Student’s t-test or Mann–Whitney U-test were used for continuous variables and the Pearson’s chi-squared test or Fisher’s exact test for categorical variables. After matching, the Mann–Whitney U-test was used to analyze the continuous variables and McNemar’s test to assess the categorical variables. We used stratified Cox proportional hazards modeling to compare the risk of postoperative mortality in the different anesthetic groups. The risk was expressed by hazard ratios (HRs) with corresponding 95% confidence intervals (CIs). Conditional logistic regression models were used to compare secondary outcomes within each group. The effect was expressed by odds ratios (ORs) with corresponding 95% CIs.
The statistical analyses were performed using SAS (version 9.4; SAS Institute Inc., Cary, NC, USA) and IBM SPSS Statistics for Windows (version 23; IBM Corp., Armonk, NY, USA). A p-value <0.05 was considered statistically significant.
Results
In total, 1152 patients underwent LEA at Severance Hospital between September 30, 2007 and August 31, 2017. After application of the exclusion criteria, data for 519 patients were available for inclusion in the final analysis. The mean age at the time of surgery was 65 years, and 72% of the patients were male. Eight patients (1.5%) underwent above-knee amputation, 83 (16%) underwent below-knee amputation, and 428 (82.5%) underwent more minor amputation. There were 227 patients in the GA group and 292 in the RA group. In the RA group, 239 patients received spinal anesthesia and 53 received a peripheral nerve block. The study flow chart is shown in Figure 1.
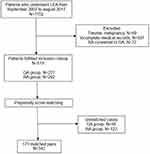 |
Figure 1 Consort diagram. Abbreviations: LEA, lower extremity amputation; GA, general anesthesia; RA, regional anesthesia. |
The baseline patient characteristics, comorbidities, use of medication, surgical details, and preoperative laboratory data are presented in Table 1. Patients with coronary or peripheral artery disease were more likely to receive GA than RA (44.1% vs 34.6%, p=0.028 and 73.1% vs 60.3%, p=0.002, respectively). There were no statistically significant between-group differences in the proportions of patients with diabetes, hypertension, congestive heart failure, cerebrovascular accident, chronic kidney disease, or chronic obstructive pulmonary disease, or according to smoking history. Patients who were receiving antiplatelet therapy, such as aspirin and clopidogrel, preoperatively were more likely to receive GA than RA (68.7% vs 55.1%, p=0.001 and 63% vs 41.8%, p<0.001, respectively). The GA group had lower preoperative hemoglobin and albumin values and higher preoperative platelet, prothrombin time, and C-reactive protein values. Major (ie, above-knee or below-knee) amputation was significantly more common in the GA group than in the RA group (23.8% vs 12.7%, p=0.001) and the operating and anesthesia times were longer in the GA group (72 mins vs 54.1 mins, p<0.001 and 115.7 mins vs 88.2 mins, p<0.001, respectively). Appropriate propensity score matching produced 171 matched pairs (342 patients, comprising 65.9% of the total study population) with exclusion of 177 cases (56 with GA and 122 with RA). There was no significant difference in baseline characteristics, comorbidities, use of medication, or type of operation in the matched study population (Table 2). However, the operating and anesthesia times were significantly longer in the GA group than in the RA group (69.5 mins vs 58.5 mins, p=0.019 and 112.3 mins vs 93.1 mins, p<0.001, respectively). The preoperative platelet and C-reactive protein values were significantly higher in the GA group than in the RA group (344 vs 312.6, p=0.038 and 104 vs 68.6, p<0.001, respectively).
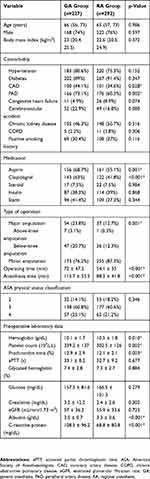 |
Table 1 Baseline Demographic And Clinical Characteristics Of Patients Undergoing Lower Limb Amputation According To Type Of Anesthesia |
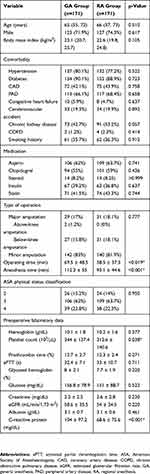 |
Table 2 Baseline Patient Demographic And Clinical Characteristics After Propensity Score Matching |
In the propensity-score matched cohort, there was no statistically significant difference in the primary outcome of 30-day and 90-day mortality between the two groups (3.5% for GA vs 2.9% for RA, HR 0.83, 95% CI 0.28–2.46, p=0.73, 7 and 6.4% for GA vs 4.6% for RA, HR 0.724, 95% CI 0.3–1.75, p=0.474; Figure 2, Table 3). There was also no statistically significant difference in 90-day postoperative morbidity, ie, myocardial infarction, cardiac arrest, pneumonia, sepsis, renal failure, stroke, or wound healing complications. There was no significant between-group difference in the postoperative length of stay (10 days vs 10 days, p=0.24). However, when compared with the GA group, the RA group had significantly lower rates of postoperative ICU admission (14.6% vs 7%, OR 0.458, 95% CI 0.225–0.936, p=0.032), intraoperative hypotension (61.4% vs 14.6%, OR 0.101, 95% CI 0.051–0.201, p<0.001), and use of vasopressors (52% vs 14%, OR 0.145, 95% CI 0.077–0.272, p<0.001; Tables 4 and 5).
 |
Table 3 Cox Regression Results For The Study Groups After Propensity Score Matching |
 |
Table 4 Outcomes Data |
 |
Table 5 Results Of Logistic Regression Analysis Of Between-Group Differences After Propensity Score Matching |
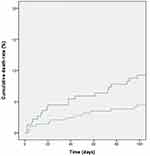 |
Figure 2 Kaplan–Meier 90-day mortality curve. Note: The cumulative death rate in patients undergoing lower extremity amputation under general anesthesia (blue) or regional anesthesia (green). |
Discussion
In this retrospective propensity-matched cohort study of 342 patients undergoing LEA because of diabetic foot and/or peripheral vascular disease, we found no significant difference in 30-day or 90-day mortality between the patients who received RA and those who received GA. Furthermore, the method of anesthesia used did not affect the likelihood of postoperative morbidity or the postoperative length of stay. However, we found that patients who underwent LEA under GA were significantly more likely to develop intraoperative hypotension, require a vasopressor, and be admitted to the ICU postoperatively.
RA, such as a neuraxial or peripheral nerve block, has a number of theoretical advantages when compared with GA. These include attenuation of the normal physiologic response to stress with lower levels of circulating catecholamines and cortisol, sympathetic blockade with resulting peripheral vasodilation and increased blood flow, decreased hypercoagulability with a potentially lower incidence of arterial and venous thrombosis, and the ability to avoid endotracheal intubation and mechanical ventilation.13,14
The results of this study also showed that patients undergoing LEA under RA were more hemodynamically stable during surgery. Generally, changes in intraoperative hemodynamics under GA are a response to cardiovascular suppression and peripheral vasodilation by inhalation or intravenous anesthetic agents. Patients who undergo LEA may have cardiovascular comorbidity, such as coronary artery disease, and may be more vulnerable to the systemic effects of GA because of their decreased cardiopulmonary reserve.15 Although there was no significant difference in the postoperative length of stay between the study groups, patients who underwent GA were significantly more likely to be admitted to the ICU after surgery. This finding may be explained by the greater likelihood of intraoperative hemodynamic instability in patients undergoing GA and their need for intensive monitoring after surgery.
However, the between-group differences in intraoperative hemodynamics did not affect mortality or morbidity after surgery. Although intraoperative hypotension was more common in the GA group, there was no significant difference in postoperative cardiovascular morbidity, such as cardiac arrest or myocardial infarction, between the two study groups. Patients receiving RA avoided intubation or mechanical ventilation during surgery, but without any significant increase in the risk of pulmonary morbidity, such as pneumonia, postoperative intubation, or prolonged mechanical ventilation. Furthermore, there was no significant difference in any of the other postoperative morbidities, such as stroke, renal failure, sepsis, or wound healing complications, according to anesthesia modality.
Many studies have been published on the effect of anesthesia modality on the postoperative prognosis, complication rate, and risk of mortality.16 Several studies in total knee or hip arthroplasty and hip surgery have reported that RA is more advantageous than GA in terms of postoperative mortality and morbidity.5,17–20
Several retrospective studies have been published on the effect of anesthesia technique on the postoperative outcome of LEA, although their findings have been inconsistent.13,15,21 However, there was no difference in postoperative mortality and morbidity in a recently published study that used a propensity score matching cohort.4,22,23 According to Moreira et al, there was no difference in 30-day mortality or postoperative morbidity according to anesthesia modality in a functionally impaired geriatric population receiving major LEA.22 In a retrospective study of 9999 patients who underwent above-knee amputation, Pisansky et al reported no difference in 30-day mortality or cardiovascular, pulmonary, infectious, and bleeding complications according to the method of anesthesia used.23 More recently, Malik et al reported a retrospective propensity score-matched review that included 12,723 patients who underwent below-knee amputation, in which there was no statistically significant difference in 30-day mortality or major morbidity according to type of anesthesia used.4 According to Malik et al, the incidence of perioperative blood transfusion was low in the RA group.
It is not clear why there is no significant difference in postoperative mortality or morbidity in the LEA population according to the anesthetic method used. However, the anesthesia modality selected for LEA has less of an impact when compared with other surgical procedures, and most patients who undergo LEA are high-risk patients with multiple comorbidities.
This retrospective study included 519 patients who underwent LEA performed by any of three orthopedic surgeons over one decade at a single center. Therefore, the perioperative management was consistent and the relevant medical records were preserved in detail.
The 30-day mortality in this study was 3.5% in the GA group, 2.9% in the RA group, and 3.2% overall. In a study by Gurney et al, the 30-day mortality after minor amputation was 3%.24 We included patients who underwent major or minor amputation, unlike previously reported studies that only included patients who underwent major amputation. Therefore, the 30-day mortality rate in this study can be considered relatively lower than the rate of 7–22% in previous reports.7
This study has several limitations. First, it is a retrospective review of a large database, which has inherent limitations. Second, although propensity score matching was used to exclude the effects of variables other than anesthesia modality as far as possible, the preoperative CRP values were not consistent across the 2 cohorts, which could have influenced our results. Furthermore, the operating and anesthesia times and the preoperative platelet values were not controlled; however, any differences were unlikely to be clinically significant. Third, other important clinical factors that may influence the mode of anesthesia chosen, such as severe aortic stenosis, presence of surgical site infection, and patient preference, were not assessed. Finally, the high minor amputation rate of 82.5% needs to be taken into consideration when interpreting the results of this study.
Conclusion
Our present findings suggest that anesthesia modality is not an independent contributor to postoperative mortality or morbidity in patients who undergo LEA. However, more intraoperative hemodynamic changes may occur in patients who undergo minor amputations under GA. Therefore, the choice of anesthesia method should be determined by the overall health status of the patient and the type of surgical procedure and be selected carefully after communication between the surgeon, anesthesiologist, and patient. It is also important to identify and prepare for the patient’s comorbidities and risk factors.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Aulivola B, Hile CN, Hamdan AD, et al. Major lower extremity amputation: outcome of a modern series. Arch Surg. 2004;139:395–399. doi:10.1001/archsurg.139.4.395
2. Anton JM, McHesnry ML. Perioperative management of lower extremity revascularization. Anesthesiol Clin. 2014;32:661–676. doi:10.1016/j.anclin.2014.05.004
3. Abou-Zamzam AM
4. Malik O, Brovman EY, Urman RD. The use of regional or neuraxial anesthesia for below-knee amputations may reduce the need for perioperative blood transfusions. Reg Anesth Pain Med. 2018;43:25–35. doi:10.1097/AAP.0000000000000687
5. Perlas A, Chan VWS, Beattie S. Anesthesia technique and mortality after total hip or knee arthroplasty: a retrospective, propensity score-matched cohort study. Anesthesiology. 2016;125:724–731. doi:10.1097/ALN.0000000000001248
6. Stern JR, Wong CK, Yerovinkina M, et al. A meta-analysis of long-term mortality and associated risk factors following lower extremity amputation. Ann Vasc Surg. 2017;42:322–327. doi:10.1016/j.avsg.2016.12.015
7. van Netten JJ, Fortington LV, Hinchliffe RJ, Hijmans JM. Early post-operative mortality after major lower limb amputation: a systematic review of population and regional based studies. Eur J Vasc Endovasc Surg. 2016;51:248–258. doi:10.1016/j.ejvs.2015.10.001
8. Yamada K, Yasunaga H, Kadono Y, et al. Postoperative outcomes of major lower extremity amputations in patients with diabetes and peripheral artery disease: analysis using the diagnosis procedure combination database in Japan. Am J Surg. 2016;212:446–450. doi:10.1016/j.amjsurg.2015.08.039
9. Thorud JC, Plemmons B, Buckley CJ, Shibuya N, Jupiter DC. Mortality after nontraumatic major amputation among patients with diabetes and peripheral vascular disease: a systematic review. J Foot Ankle Surg. 2016;55:591–599. doi:10.1053/j.jfas.2016.01.012
10. Easterlin MC, Chang DC, Wilson SE. A practical index to predict 30-day mortality after major amputation. Ann Vasc Surg. 2013;27:909–917. doi:10.1016/j.avsg.2012.06.030
11. Belmont PJ, Davey S, Orr JD, Ochoa LM, Bader JO, Schoenfeld AJ. Risk factors for 30-day postoperative complications and mortality after below-knee amputation: a study of 2,911 patients from the national surgical quality improvement program. J Am Coll Surg. 2011;213:370–378. doi:10.1016/j.jamcollsurg.2011.05.019
12. Bulka CM, Shotwell MS, Gupta RK, Sandberg WS, Ehrenfeld JM. Regional anesthesia, time to hospital discharge, and in-hospital mortality: a propensity score matched analysis. Reg Anesth Pain Med. 2014;39:381–386. doi:10.1097/AAP.0000000000000121
13. Chery J, Semaan E, Darji S, Briggs WT, Yarmush J, D’Ayala M. Impact of regional versus general anesthesia on the clinical outcomes of patients undergoing major lower extremity amputation. Ann Vasc Surg. 2014;28:1149–1156. doi:10.1016/j.avsg.2013.07.033
14. Rodgers A, Walker N, Schung S, et al. Reduction of postoperative mortality and morbidity with epidural or spinal anaesthesia: results from overview of randomized trials. BMJ. 2000;321:1–12. doi:10.1136/bmj.321.7252.1
15. Lin R, Hingorani A, Marks N, et al. Effects of anesthesia versus regional nerve block on major leg amputation mortality rate. Vascular. 2013;21(2):83–86. doi:10.1177/1708538113478718
16. Smith LM, Cozowicz C, Uda Y, Memtsoudis SG, Barrington MJ. Neuraxial and combined neuraxial/general anesthesia compared to general anesthesia for major truncal and lower limb surgery: a systematic review and meta-analysis. Anesth Analg. 2017;125:1931–1945. doi:10.1213/ANE.0000000000002069
17. Urwin SC, Parker MJ, Griffiths R. General versus regional anaesthesia for hip fracture surgery: a meta-analysis of randomized trials. BJA. 2000;84(4):450–455. doi:10.1093/oxfordjournals.bja.a013468
18. Neuman MD, Silber JH, Elkassabany NM, Ludwig JM, Fleisher LA. Comparative effectiveness of regional versus general anesthesia for hip fracture surgery in adults. Anesthesiology. 2012;117(1):72–92. doi:10.1097/ALN.0b013e3182545e7c
19. Memtsoudis SG, Sun X, Chiu Y-L, et al. Perioperative comparative effectiveness of anesthetic technique in orthopedic patients. Anesthesiology. 2013;118:1046–1058. doi:10.1097/ALN.0b013e318286061d
20. Helwani MA, Avidan MS, Abdallah AB, et al. Effects of regional versus general anesthesia on outcomes after total hip arthroplasty. J Bone Joint Surg Am. 2015;97:186–193. doi:10.2106/JBJS.N.00612
21. Khan SA, Qianyi RL, Liu C, Ng EL, Fook-Chong S, Tan MGE. Effect of anaesthetic technique on mortality following major lower extremity amputation: a propensity score-matched observational study. Anaesthesia. 2013;68:612–620. doi:10.1111/anae.12182
22. Moreira CC, Farber A, Kalish JA, et al. The effect of anesthesia type on major lower extremity amputation in functionally impaired elderly patients. J Vasc Surg. 2016;63:696–701. doi:10.1016/j.jvs.2015.09.050
23. Pisansky AJB, Brovman EY, Kuo C, Kaye AD, Urman RD. Perioperative outcomes after regional versus general anesthesia for above the knee amputations. Ann Vasc Surg. 2018;48:53–66. doi:10.1016/j.avsg.2017.10.014
24. Gurney JK, Stanley J, Rumball-Smith J, York S, Sarfati D. Postoperative death after lower-limb amputation in a national prevalent cohort of patients with diabetes. Diabetes Care. 2018;41:1204–1211. doi:10.2337/dc17-2557
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
