Back to Journals » Clinical, Cosmetic and Investigational Dermatology » Volume 13
Unique Skin Metastasis from Recurrent Cancer. Case Report
Authors Papadopoulos I
Received 21 April 2020
Accepted for publication 8 June 2020
Published 18 June 2020 Volume 2020:13 Pages 415—417
DOI https://doi.org/10.2147/CCID.S259244
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Jeffrey Weinberg
Iordanis Papadopoulos
Department of Aesthetics and Cosmetology, Alexander Technological Educational Foundation, Thessaloniki, Greece
Correspondence: Iordanis Papadopoulos Email [email protected]
Introduction: Cutaneous metastasis is defined as the dissemination of malignant cells from a primary tumor to the skin. Skin may be affected by tumors, either through direct invasion from an adjacent organ or by cutaneous metastasis from an internal organ malignancy. We report a case of a 75-year-old female patient with skin metastasis 8 years after the initial treatment of primary breast cancer.
Patient Concern: The patient presented only with papules and nodular skin lesions in the left lateral abdominal area, without any other clinical manifestations.
Diagnosis: All laboratory tests were normal. Histological examinati revealed the infiltration of the dermis by tumor cells.
Interventions/Outcome: After the diagnosis of skin metastasis, she was treated with chemotherapy with complete remission of skin lesions.
Conclusion: Skin metastasis from internal organs is rarely the first sign. In this case, skin metastasis was the only clinical sign and the only diagnostic tool to drive to the correct diagnosis of a recurrent cancer after 8 years. Dermatologists might be the first doctors to facilitate the diagnosis of skin metastasis.
Keywords: skin metastases, breast cancer, neoplasm metastases
Introduction
Skin metastases are more common in breast, lung, colon, stomach, uterus and kidney tumors.1 Metastatic skin lesions may be the first clinical finding, a sign of recurrence or end-stage disease. Misdiagnosis of such lesions is therefore critical for the life of the patient. Internal organ tumors tend to metastasize in the skin by a percentage ranging from 0.7% to 10%, through blood or lymphatic dispersion. In women, about 70% of skin metastases are due to breast malignancy.2
Case Report
A 75-year-old woman presented with a rash in the left lateral abdominal area without itching since 1 month (Figure 1). According to her medical history, she had had a total mastectomy of her left breast with concurrent chemotherapy 8 years before. The skin lesions presented on the same side with the breast cancer (Figure 2). Since then, she was asymptomatic without any medical problems. With the thought that the skin lesions were parasite bites, the patient had used topical steroid treatment for 1 month without improvement.
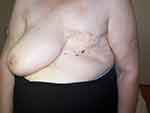 |
Figure 1 Front picture of the mastectomy. |
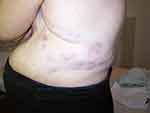 |
Figure 2 Left side of the body. |
The rash consisted of multiple non-pruritic erythematous plaques located only in the left lateral abdomen. The sizes of the plaques were between 2 and 3 centimeters. During palpation, one plaque was elevated with higher peripheral borders without central ulceration (Figure 3). Due to her medical history, there was no differential diagnosis issue, although the granuloma annulare was a possible alternative diagnosis. Histological examination of the skin biopsy, performed on the abdominal lesion, revealed an intact epidermis and a diffuse infiltration of the dermis by tumor cells. The immunohistochemical test was positive for cytokeratin 7 and cerb-2, indicating a breast adenocarcinoma. Three phase bone scintigraphy and Computed Tomography scans (abdominal and retroperitoneal) showed no pathological findings. Blood test examinations were also normal. Carcinoembryonic antigen and antigen 15–3 were both normal.
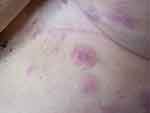 |
Figure 3 Plaques of the skin. |
After the histological examination, letrozole was given as a chemotherapeutic agent. Letrozole blocks the action of the enzyme-aromatase which reduces estrogen production and therefore prevents the development of estrogen-induced breast cancer. In this way, tumor growth and dissemination to other parts of the body are impeded. It was administered at a dosage of 2.5mg once daily for 2 months. After chemotherapy, cutaneous metastases remission was complete. The patient is under periodic follow-up laboratory tests (blood tests, Computed Tomography scans) and is symptom free until today.
Discussion
It is well known that skin is a common metastatic organ from internal malignancy, though it is usually not the first organ to be affected. Usually other organs such as brain, liver, bones, lungs, kidneys are preceded. So when metastasis occurs to the skin, the prognosis is usually poor because it usually means that metastasis has already occurred in other vital organs.3 The most common cancers that metastasize to the skin are melanoma (45%), breast cancer (30%) cancer of the nasal sinuses (20%), laryngeal cancer (16%) and oral cancer (12%).4 The incidence of cutaneous metastasis from internal organs varies from 3% to 10%.5 Breast cancer is the second most common cancer in women. Skin is a common expression of metastases of breast cancer and approximately one in four women with breast cancer may experience metastasis to the skin.6 Skin metastasis of breast cancer can have various clinical forms and great varieties. The most common manifestation is the presence of nodules mainly in the chest wall or other parts of the body such as the neck and the head. They are usually harsh in composition and their size varies from 1 to 3 cm. They manifest as a single or multiple lesions located mostly in the dermis. They are usually not painful and have the skin color. They can also be ulcerated. Other clinical forms of the metastatic breast cancer in the skin may be erythematous rash, erysipeloid and neoplastic alopecia in the scalp. The most frequent histopathological pattern in cutaneous metastases is a nodule in the deeper dermis, adjacent to the subcutaneous tissue. The tumor presents as neoplastic cells surrounded by fibrosis. There is often a little or even non-existent inflammatory reaction.7
Usually, when metastasis occurs to the skin from breast cancer, other organs may already have been affected.8 Rarely, however, as in this case, it may be the first and only sign of cancer recurrence even after 8 years. It is very important to quickly identify the first metastasis because the prognosis in these cases is very good.9 The role of the dermatologist for a patient with skin metastases of an unknown internal cancer is very important, since he might be the first doctor to facilitate the diagnosis of the primary tumor.
Consent Statement
Written informed consent was provided by the patient to have the case details and any accompanying images published.
Disclosure
The author reports no conflicts of interest in this work.
References
1. Papadopoulos Ι, Ioannides D, Lefaki I. Cutaneous metastases from primary internal malignancies: a retrospective study from a tertiary dermatological center in Northern Greece. Hippokratia. 2014;18(2):187.
2. Saeed S, Keehn CA, Morgan MB. Cutaneous metastasis: a clinical, pathological, and immunohistochemical appraisal. J Cutan Pathol. 2004;31:419–430.
3. Sittart JA, Senise M. Cutaneous metastasis from internal carcinomas: a review of 45 years. An Bras Dermatol. 2013;88:541–544. doi:10.1590/abd1806-4841.20131165
4. Oliveira GM, Zachetti DB, Barros HR, Tiengo A, Romiti N. Breast carcinoma en Cuirasse–case report. An Bras Dermatol. 2013;88:608–610. doi:10.1590/abd1806-4841.20131926
5. Alcaraz I, Cerroni L, Rütten A, Kutzner H, Requena L. Cutaneous metastases from internal malignancies: a clinicopathologic and immunohistochemical review. Am J Dermatopathol. 2012;34:347–393. doi:10.1097/DAD.0b013e31823069cf
6. Lookingbill DP, Spangler N, Helm KF. Cutaneous metastases in patients with metastatic carcinoma: a retrospective study of 4020 patients. J Am Acad Dermatol. 1993;29:228–236. doi:10.1016/0190-9622(93)70173-Q
7. Bittencourt MDJS, Carvalho AH, Nascimento BAMD, Freitas LKM, de Parijos AM. Cutaneous metastasis of a breast cancer diagnosed 13 years before. An Bras Dermatol. 2015;90(3 Suppl 1):134–137. doi:10.1590/abd1806-4841.20153842
8. Hussein MR. Skin metastasis: a pathologist’s perspective. J Cutan Pathol. 2010;37:e1–e20. doi:10.1111/j.1600-0560.2009.01469.x
9. Schoenlaub P, Sarraux A, Grosshans E, Heid E, Cribier B. Survival after cutaneous metastasis: a study of 200 cases. Ann Dermatol Venereol. 2001;128:1310–1315.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
