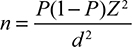Back to Journals » Journal of Multidisciplinary Healthcare » Volume 9
The Iranian physicians attitude toward the do not resuscitate order
Authors Falahi M, Bana Derakhshan H, Abdi A , Borhani F, Kavyannejad R, Karimpour H
Received 25 January 2016
Accepted for publication 22 March 2016
Published 29 June 2016 Volume 2016:9 Pages 279—284
DOI https://doi.org/10.2147/JMDH.S105002
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Masood Fallahi,1 Homayion Banaderakhshan,1 Alireza Abdi,1 Fariba Borhani,2 Rasool Kaviannezhad,3 Hassan Ali Karimpour4
1School of Nursing and Midwifery, 2Medical Ethics and Law Research Center, Medical Surgical Nursing Department, School of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Tehran, 3Department of Anesthesia, Paramedical School, Kermanshah University of Medical Sciences, 4Critical Care, School of Medicine, Imam Reza Hospital, Kermanshah University of Medical Sciences, Kermanshah, Iran
Background: Physicians are responsible for making decisions about the do not resuscitate (DNR) order of patients; however, most of them are faced with some uncertainty in decision making and ethical aspects. Moreover, there are differences on decision making related to the DNR order among physicians, which may be related to the different attitudes toward this issue. Considering the lack of information, this study was performed to investigate doctors’ attitude about DNR order for patients in their final phases of life.
Methods: In a descriptive–analytical study, 152 physicians were enrolled as quota sampling subjects from educational hospitals affiliated to the Kermanshah University of Medical Sciences. The tool used was a researcher-developed questionnaire. Data were analyzed using SPSS 16 software by descriptive and inferential statistics.
Results: The mean of attitude toward DNR was 3.22, for which the univariate t-test showed a significant positive attitude toward DNR (P=0.002); the mean of attitude number toward DNR was higher in physicians with higher education level (P=0.002). But this difference was not found in terms of age group, sex, and experiences in participating in DNR decisions.
Conclusion: Due to the positive attitude of doctors toward DNR orders and lack of identified guidance, clear guidelines that comply with the Iranian Islamic culture are necessary to be established. Implementing this directive requires comprehensive training to various groups, including patients, doctors, nurses, administrators, and policy makers of the health system.
Keywords: cardiopulmonary resuscitation, physicians, attitude
Introduction
Cardiopulmonary resuscitation (CPR) is an emergency medical procedure that is performed on patients with respiratory and cardiac arrest, but it is not fully successful in all the cases. In fact, the prognosis of the patient has the main role to play in the effectiveness of CPR; hence, there is a belief that this approach should just be performed for patients who have a high chance of survival.1–4
Researchers have demonstrated that only 20% of patients survive after CPR until discharge.5 Other findings in USA have also verified that only 10%–15% of patients who survive after CPR would stay revived until discharge; these statistics have not changed during the past 30 years.4 In addition, the chance of survival for patients with diseases such as cancer is lower; moreover, those who undergo successful resuscitation often are subjected to aggressive treatments in intensive care units; consequently, this is accompanied by some complications such as rib fractures, permanent neurological problems, and impaired physical condition.4
Therefore, there are concerns regarding the misuse of CPR and delay of mortality. In this context, due to the lack of recovery or ineffectiveness of CPR, the excessive costs, increased suffering and death without dignity for some patients, the “do not resuscitate (DNR) order” was presented in USA in 1970.1,6–8
DNR involves the decision to ignore CPR and it was officially introduced as an alternative for end-of-life care in the early 1970s.7 The DNR order is carried out only to decide to withhold resuscitation, when cardiopulmonary arrest occurs. This should not affect other aspects of patient care. However, many health care providers inappropriately change the treatment programs for patients with DNR order without discussion with the patient or surrogate.4 Although the DNR order has been reviewed in some communities for decades and has been debated comprehensively, it has faced some controversies; in addition, there are many differences in terms of performance, morality, legal issues, and appropriateness of medical instructions in the application of DNR.9,10 The process of deciding on DNR is an exclusive measure allotted to the physicians. However, based on research findings, doctors face many problems during the decision-making process for DNR, as well as its ethical dilemma,9 so that there are significant differences among doctors in the development, registration, issuance, and implementation of a DNR order.11 These differences may be justified by the diversity of their attitudes. In fact, research has revealed that issuance and implementation of a DNR order are influenced by the attitudes and desires of the health care providers.12,13 Various factors affect the attitude of physicians toward a DNR order, such as culture, religion, race, and geographical location features. Thus, implementation of the DNR order in Asian and Muslim countries is much lower than in European countries.10,13
In fact, although the DNR order is used in Muslim nations, it is not allowed legally. The King Faisal Specialist and the King Khaled hospitals in Saudi Arabia are two of the centers wherein guidance for the DNR order is provided to patients in the end stage of life.14 In Iran, where most of the people are Muslims,15 despite the illegality of the DNR order, it would be ordered upon personal desire, without any established guidance, due to which physicians encounter more sophisticated issues related to the legality of this action.16,17 The distress caused by the situations is in contrast with the beliefs and internal moral values; as a result of these conditions, physicians are forced to take action against their values.18 The Islamic culture has valued and respected the life of the patients and respects every second of their lives; so, it is essential to develop a guidance to reach a clear decision regarding the DNR order to reduce the interference of personal and nonprofessional factors; however, there is lack of information in the Muslim world and Iran about DNR order.8,15,17 Ghajarzadeh et al2 concluded there is a positive attitude toward the DNR order in medical students of the Tehran University of Medical Sciences; however, we could not find other research reports on the attitudes of general practitioners and specialists toward DNR orders in Iran. Considering the important role of the doctor’s attitude toward issuing and executing a DNR order, as well as the shortage of information in this field in Iran, this study was aimed at evaluating the attitudes of specialty doctors, residents, and general practitioners in educational hospitals affiliated to Kermanshah University of Medical Sciences (KUMS) toward the issuance of DNR order to patients.
Methods
This study was conducted as a descriptive–analytical analysis. The population studied included general practitioners, residents, and specialists working in the hospitals of KUMS. The participants were recruited from the Imam Reza (89 participants), Imam Ali (45 participants), and Imam Khomeini (27 participants) hospitals. The sample size was determined by assuming the agreement of 50% of DNR orders by the physicians; using estimation of the 95% confidence interval, test power 90%, and following formula (Equation 1) with n=sample size, P=proportion, Zα/2= 1.96, d= margin of error, a sample size of 152 was calculated. The sampling method was stratified quota.
|
|
Instrument
The tool was a researcher-tailored questionnaire that included two parts, consisting of the demographic information and the attitude toward DNR order. The demographic characteristics included age, sex, job experience, education degree, experience in CPR, and experience in executing DNR. The attitude questions consisted of eleven items that were designed as responses on a five-point Likert scale. The scores of the questions 1–10 ranged from 1–5 and were scored as follows: strongly agree =5, agree =4, no idea =3, disagree =2, and strongly disagree =1; however, this scoring was vice versa for question 11. The higher scores indicate more positive attitudes toward the DNR. Accordingly, average scores between 1 and 2, 2 and 3, 3 and 4, and 4 and 5, indicated highly negative, negative, positive, and highly positive attitudes, respectively, toward the DNR order.
This instrument was created by the researcher based on the literature review.1,10,19–22 The content validity was carried out by consulting with ten faculty members affiliated to the Shahid Beheshti University of Medical Sciences and KUMS, who were experts in nursing, medicine, critical care, and clinical ethics. The reliability was met by calculating the Cronbach’s alpha coefficient, which was equal to 0.88.
Data collection
For data collection, the project was approved by ethics committees of Shahid Beheshti University of Medical Sciences and KUMS, then data were gathered by referring to the workplace of the participants; first the aim and objective of the study were explained to them, written informed consent was taken from the participants and then they were assured of the anonymity and confidentiality of their personal information, after which they completed the questionnaires.
Data analysis
Data were entered into the Statistical Program for the Social Sciences (SPSS)-16 software (SPSS Inc, Chicago, IL, USA) and analyzed by descriptive (mean, percentage, and SD) and inferential (independent t-test and analysis of variance [ANOVA]) statistics. Independent t-test was used to assess the relationship between attitude toward DNR order with job, sex, death viewing experience, working experience in CPR, and DNR order application. To determine the relationship between attitudes toward DNR order and age, experience, education level, hospitals, ward hospital, field of specialization, and participation in the CPR, ANOVA test was used. Kolmogorov–Smirnov test was applied for determining the normality of quantitative variables such as attitudes toward DNR order and age.
Results
Of the 222 physicians contributing to the study, 168 (75%) completed the questionnaires; 16 (7.2%) of the questionnaires had incomplete information, which were excluded from the study. As a result, 152 (68%) questionnaires were assessed; 57.8% of the participants (88 individuals) were male, with mean age of 36.57 years. The majority of the participants had between 1–10 years of job experience, 71 participants (46.6%) were residents, >91% had participated in CPR, 96.8% had dealt with the death of a patient, and 67.8% had experienced executing DNR (Table 1).
  | Table 1 Demographic characteristics of the participants Abbreviation: CPR, cardiopulmonary resuscitation. |
According to the results of the study, the mean score of the doctor’s attitude toward DNR was higher than the value hypothesized by the univariate t-test, which was significant (P=0.002). This indicates that the physicians had a positive attitude toward DNR (Table 2). The mean and SD of each item are presented in Table 3, which demonstrated that items such as “If CPR is ineffective, the patient should not be resuscitated” and “DNR order protects the patient from suffering needlessly” had higher points.
  | Table 2 Univariate t-test on the average score of doctors with respect to do not resuscitate order Abbreviations: df, degree of freedom; t, one-sample t-test. |
  | Table 3 Results of t-test comparing the attitudes of physicians regarding the items Abbreviations: CPR, cardiopulmonary resuscitation; DNR, do not resuscitate. |
The results showed that there are no significant differences in the mean score of physicians’ attitudes toward DNR order in terms of sex (t=0.824; P=0.411), age group (F=1.57; P=0.197), work experience (F=2.15; P=0.096), and their expertise (F=1.069; P=0.394). However, there was a significant difference in the education level (F=5.31; P=0.0002), according to which the general physicians had a mean rate of 2.78, lower than those for residents (3.30) and specialists (3.22). Moreover, the physician professors had the highest rate of attitude toward the DNR (mean=3.82).
Discussion
Based on the results, the doctors have a positive attitude toward DNR order. Accordingly, the results of the items showed that they believed that this order protects patients from unnecessary suffering, and it is essential for patients in the last stages of their lives, as well as showing that the order is morally correct because it is an aid to human dignity. The results also show that there is no significant relationship between physicians’ attitudes toward the DNR order, sex, work experience, and specialty, but there were significant differences between the attitudes of doctors in terms of their education level. In the study of Hosaka et al,19 >90% of the physicians had a positive attitude toward DNR order. In another study, medical students had significantly more positive attitudes toward DNR order compared to nonmedical students.10 Sulmasy et al21 reported that the majority of nurses, physicians, and residents have a positive attitude toward the DNR order. It is shown that the majority of doctors and nurses have a positive attitude toward DNR order. In fact, studies in the field of DNR order in various countries represents challenges in this regard but have indicated a positive outlook on this relationship.17,19,21–23 The results of the review of each item found that the doctors declared that DNR order is in line with patient dignity and they believed that it is morally correct. Indeed, it can be said that for many patients, dignity and respect are the last and most important things that they may demand of their relatives and caregivers, particularly if their illness is life-threatening and dangerous.24 Hilden et al22 indicated that attitudes toward DNR order may vary depending on the expertise of doctors. In the UK, geriatric medicine specialists are willing to perform CPR more than other doctors and were not opposed to the order. Kelly et al12 have concluded in their study the relationship between attitudes toward DNR order and physician specialty, duration of training, and job experience: intensive care physicians recommend DNR order more than other groups. Sham et al10 also indicated that sex has no significant impact on the choice of the DNR order, but age is considered an important factor; hence, older practitioners have more positive attitude about DNR order.
This study showed that there was a significant difference in the attitudes of physicians based on education level, and that specialist physicians had more favorable attitude toward DNR order and general practitioners took the lowest scores. Consistent with our findings, Granja et al13 demonstrated that there are different attitudes among various health care groups, including doctors, nurses, and technicians, as well as the patients, toward the DNR order and the decision upon it; moreover, they also concluded that the nurses and doctors who had higher levels of education had more positive attitude. Moreover, they noted that, in addition to the educational level of the participants, the extent of their participation in the care of patients was also a significant factor.13
In this study, 67.8% of the physicians had experience in executing the DNR order. In this context, in the study by Hosaka et al,19 >60% of doctors participated in the decision-making process about DNR order, and this rate was 100% in the study by Cardoso et al.23 Anther study in Iran on resident and intern physicians showed that only 30% of interns and 40% of residents participated in the issuance and implementation of a DNR order.2 The difference in the participation in DNR may be attributed to the variety in the target groups.
In fact, we believe, the doctors opinions toward DNR is in line with medical ethics, which means acting in the best interests of the patient, because doctors are committed to providing good-quality care to patients. This idea of the benefit of a DNR order is controversial within the medical community; for some doctors, prolonging the life of patient is in their best interests, while others indicated that a good quality of life is the best interest and suggest that for the treatment of patients who had undergone supportive therapy and whose death was inevitable, the treatments should be banned or discontinued.25–27
In this study, the participants declared that the DNR order is only applicable to patients whose death is imminent and should not be used for patients for whom death is predictable or anticipated within the next 6 months to 1 year. In other words, DNR order is authorized only when the patient is dying and in the final hours of his/her life, not for those who are still alert, which finding is consistent with strict Jewish opinion that states that if the patient dies in the next 72 hours and swallowing reflexes have been lost, the treatment can be withheld. However, culture and traditions, religious beliefs, and general comments on the decision of DNR order agree to apply this to patients who may die within 1 year. In orthodox religion, efforts for resuscitation are conducted on all patients, with greater chances of survival; however, when resuscitation is futile, DNR would be ordered.28,29 In fact, it can be said that most of the cultures, traditions, and religious beliefs are general statements about the decision-making to DNR order of patients.28 In Islam also, the DNR order is not prohibited to patients in their end-stage of life when death is inevitable and when medical resuscitation for the patient is useless and misplaced. In Islamic jurisprudence, the issues of euthanasia and brain death have been considerably discussed and it seems there is no clear rule about DNR order as a medical issue; so, decisions about it have been assigned to doctors and the health care system.29 In Iran, physicians are directly responsible for deciding about the resuscitation of patients; however, despite the informal and nonstandard prevalence of the DNR order, there is no definitive conclusion about the legality of this action and, at the moment, current law does not permit its implementation; this has created many ambiguities for the doctors, which may result in overlooking of the rights of patients and their relatives, as well as causing error in performing the Islamic jurisprudence and religious laws.16,17,29 in Iran, because of our values and religious issues, we cannot follow the guidelines of other nations; so, for reducing the consequences of errors, more precise explanations are required.
Conclusion
Due to the positive attitude of doctors, confusion, and lack of guidelines on ethical and legal standards toward DNR order, precise guidelines should be developed based on Islamic–Iranian culture. The implementation of these guidelines requires a comprehensive training for various groups, including patients, doctors, nurses, other health workers, health care and health system managers, and policy makers.
Because the sampling method was a stratified-quota procedure, the sample may not represent the population of doctors; so, it is recommended to undertake other investigations using a randomization method.
Acknowledgments
This article is the result of an MSc thesis of Nursing approved by the School of Nursing and Midwifery of the Shahid Beheshti University of Medical Sciences (SBMU). We appreciate all the officials of SBMU, as well as the physicians working in hospitals of Imam Reza, Imam Ali, and Imam Khomani hospitals affiliated to the Kermanshah University of Medical Sciences, who contributed to the conduct of the study.
Disclosure
The authors report no conflicts of interest in this work.
References
Mogadasian S, Abdollahzadeh F, Rahmani A, et al. The attitude of Iranian nurses about do not resuscitate orders. Indian J Palliat Care. 2014;20(1):21–25. | ||
Ghajarzadeh M, Habibi R, Amini N, Norouzi-Javidan A, Emami-Razavi SH. Perspective of Iranian medical students about do-not-resuscitate orders. Maedica (Buchar). 2013;8(3):261–264. | ||
Cooper JA, Cooper JD, Cooper JM. Cardiopulmonary resuscitation: history, current practice, and future direction. Circulation. 2006;114(25):2839–2849. | ||
Yuen JK, Reid C, Fetters MD. Hospital do-not-resuscite orders: why they have failed and how to fix them. J Gen Intern Med. 2011;26(7):791–797. | ||
Peberdy MA, Kaye W, Ornato JP, et al. Cardiopulmonary resuscitation of adult in the hospital: a report of 14720 Cardiac arrests from the national registry of cardio pulmonary resuscitation. Resuscitation. 2003;58(3):297–308. | ||
Castledline G. Nurses should be more involved in DNR decisions. Br J Nurs. 2004;13(3):1–3. | ||
Bellini S, Damato EG. Nurses, knowledge, attitudes, beliefs and care practices concerning do not resuscitate status for hospitalized neonates. J Obstet Gynecol Neonatal Nurs. 2008;38(2):195–205. | ||
Saiyad S. Do not resuscitate: a case study from the Islamic viewpoint. J Indian Med Assoc. 2009;41(3):109–113. | ||
Loofmark R. Do-Not-Resusciate Orders: Ethical Aspect on Decision Making and Communication Among Physician, Nurses, Patients and Relatives. Lund: Lund University; 2001:1–50,122. | ||
Sham CO, Cheng YW, Ho KW, et al. Do-not-resuscitate decision: the attitudes of medical and non-medical students. J Med Ethics. 2007;33(5):261–265. | ||
O’hanlon S, O’Connor M, Peters C, O’Connor M. Nurses’ attitudes towards do not attempt resuscitation orders. Clin Nurs Stud. 2013;1(1):43–50. | ||
Kelly WF, Eliasson AH, Stocker DJ, Hnatiuk OW. Do specialists differ on do not resuscitate decisions? Chest. 2002;121(3):957–963. | ||
Granja C, Teixeira-Pinto A, Costa-Pereira A. Attitudes towards do-not-resuscitate decisions: differences among health professionals in a Portuguese hospital. Intensive Care Med. 2001;27(3):555–558. | ||
Takrouri M, Halwani T. An Islamic medical and legal prospective of do not resuscitate order in critical care medicine. Internet J Health. 2008;7(1):12–16. | ||
Borhani F, Hosseini SH, Abbaszadeh A. Commitment to care: a qualitative study of intensive care nurses’ perspectives of end-of-life care in an Islamic context. Int Nurs Rev. 2014;61(1):140–147. | ||
Akazi A. A review of the situation in order not perform resuscitation in patients with cardiac breathing arrest. J Forensic Med. 2014;20(3):103–110. | ||
Payamani M, Zahedi F, Larijani B. Not resuscitation order in communities various communities and the need for a moral guide. Iran J Med Ethics Hist. 2011;5:17–30. | ||
Borhani F, Abbaszadeh A, Nakhaee N, Roshanzadeh M. The relationship between moral distress, professional stress, and intent to stay in the nursing profession. J Med Ethics Hist Med. 2013;7:3. | ||
Hosaka T, Nagano H, Inomata C, et al. Nurses’ perspectives concerning do-not-resuscitate (DNR) orders. Tokai J Exp Clin Med. 1999;24(1):29–34. | ||
Lachman V. Do-not-resuscitate order: nurses’ role requires moral courage. Med Surg Nurs. 2010;19(4):249–251. | ||
Sulmasy DP, He MK, Mcaquley R, Ury WA. Beliefs and attitudes of nurses and physicians about do not resuscitate orders and who should speak to patients and families about them. Crit Care Med. 2008;36(6):1817–1822. | ||
Hilden HM, Louhiala P, Palo J. End of life decisions: attitudes of Finnish physicians. J Med Ethics. 2004;30(4):362–365. | ||
Cardoso T, Fonseca T, Pereira S, Lencastre L. Life-sustaining treatment decisions in Portuguese intensive care units: a national survey of intensive care physicians. Crit Care. 2003;7(6):167–175. | ||
Borhani F, Abbaszadeh A, Moosavi S. Status of human dignity of adult patients admitted to hospitals of Tehran. J Med Ethics Hist Med. 2014;7(19):20. | ||
Thompson IE, Melia KM, Boyd KM. Nursing Ethics. 4th ed. London: Churchill Livingstone; 2000. | ||
Williams LS, Hopper P. Medical Surgical Nursing. 3th ed. Philadelphia: F.A. Davis Company; 2007. | ||
Irwin RS. Intensive Care Medicine. 6th ed. Philadelphia: Lippincott Williams and Wilkins; 2008. | ||
Burns JP, Edwards J, Johnson J, Cassem NH, Truog RD. Do-not-resuscitate order after 25 years. Crit Care Med. 2003;3(5):1543–1550. | ||
Larijani B, Zahedi F, Tavakoli Bazzaz C, Parsa Poor A. Ethical issues in end of life from the perspective of faith. Iran J Diabetes Lipid Disord. 2007;6(7):2. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.