Back to Archived Journals » Smart Homecare Technology and TeleHealth » Volume 7
Telemedicine in the Management of Inflammatory Bowel Disease: An Update
Authors Bhattacharya S , Wong U, Cross RK
Received 2 October 2019
Accepted for publication 24 January 2020
Published 5 March 2020 Volume 2020:7 Pages 9—17
DOI https://doi.org/10.2147/SHTT.S195566
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Aryya Gangopadhyay
Sumona Bhattacharya,1 Uni Wong,2 Raymond K Cross2
1Digestive Disease Branch, National Institute of Diabetes and Digestive and Kidney Diseases, National Institutes of Health, Bethesda, MD, USA; 2University of Maryland School of Medicine, Department of Medicine, Division of Gastroenterology and Hepatology, Baltimore, MD, USA
Correspondence: Raymond K Cross
University of Maryland School of Medicine, Department of Medicine, Division of Gastroenterology and Hepatology, 685 West Baltimore Street, Suite 8-00, Baltimore, MD 21201, USA
Tel +1 410-706-3387
Fax +1 410-706-4330
Email [email protected]
Abstract: Crohn’s disease and ulcerative colitis are the two most common subtypes of inflammatory bowel disease. Most studies show that this patient population is increasing in incidence. Patients with these diseases require lifelong care by experienced practitioners however the traditional medical model is not ideal for patients who require continuous close monitoring and whose symptoms may dramatically worsen between regularly scheduled visits. Patients with uncontrolled disease may experience abdominal pain, diarrhea, and rectal bleeding and such patients are at increased risk for complications that may necessitate hospitalization and emergency surgery. Traditional medical care can be supplemented by telemedicine, which is the delivery of health care through remote electronic communication, for example, through web-based computer or smartphone applications. Here we describe several studies that highlight the many ways in which telemedicine can augment and improve patient care through telemonitoring, telemanagement, televisit, and teleconsultation.
Keywords: inflammatory bowel disease, crohn’s disease, ulcerative colitis, telemedicine, telehealth, telemonitoring, telemanagement, televisit, teleconsultation
Introduction
Inflammatory bowel disease (IBD) is a lifelong disease that affects patients in every region around the world.1 It consists of two subtypes: Crohn’s disease (CD) and ulcerative colitis (UC). The hallmark symptoms of these diseases consist of diarrhea, rectal bleeding, and abdominal pain. These symptoms may negatively affect a patient’s everyday quality of life. The natural history of these diseases is such that patients may experience exacerbations that often necessitate corticosteroid use or hospitalization. Exacerbations and their complications, including strictures, fistulae, and abscess, may require surgery if not remedied by medical management.2 While studies are mixed on mortality in patients with IBD, a recent study of 23,000 patients in the Netherlands demonstrated increased mortality with an all-cause mortality hazard ratio of 2.4 compared to the general population.2 While there is variation regarding the prevalence of this disease in different regions, it is no longer accepted as a disease only affecting the Western hemisphere.1 Furthermore, studies suggest that the incidence of these conditions is rising.1,3
Several areas have been identified in the traditional healthcare system for potential improvement in addressing the needs of chronically ill patients suffering from diseases such as IBD.4 For example, patient’s symptoms often do not correlate with regularly scheduled follow-up appointments; flares or medication side effects can occur at any time between visits and delays can occur while attempting to schedule “urgent” or “quick sick” visits. The burden on patients to travel to providers for appointments and diagnostic tests can be significant, particularly for patients living in rural areas. Furthermore, access to a gastroenterologist with expertise in IBD or even a general gastroenterologist may be limited, forcing patients with a more complex disease living in rural areas to travel even further for the specialty care that they require. If the number of patients with IBD does increase over time as predicted,1,3 the healthcare system will need to develop new strategies to provide effective and efficient care. Telemedicine is one potential solution to improve monitoring and to provide greater access to IBD specialty care.
Telemedicine is the use of electronic communications between patients and providers, or between providers, to augment patient care. Types of communications include text messaging, electronic mail (email), videoconferencing, patient portals, and remote monitoring programs. Numerous studies have been conducted with telemedicine systems in IBD to assess the feasibility, patient acceptance, effectiveness, impact on health care utilization, and ability to improve patient knowledge. Here, we seek to give an overview of the gap that telemedicine has sought to fill in the traditional model of healthcare in caring for patients with IBD.
Epidemiology of Inflammatory Bowel Disease
In the Western hemisphere, the diagnosis of IBD occurs typically in the younger decades of life and the disease has relatively low mortality.1 This leads to a population that continues to increase over time, as individuals are added to the population faster than they are removed. Worldwide, as patients in developing countries increasingly gain access to healthcare and these health care systems increasingly gain access to endoscopy, it is predicted that the prevalence of UC and CD will rise at an accelerated rate, further contributing to the global burden of disease.1
A recent systematic review evaluated 167 population-based studies on the incidence and prevalence of UC and CD.3 Overall, the areas with the highest prevalence of IBD were in Europe (UC 505 per 100,000; CD 322 per 100,000) and North America (UC 249 per 100,000; CD 319 per 100,000). In time trend analyses, 75% of CD and 60% of UC studies demonstrated increasing incidence that was statistically significant. These findings suggest that an increasing number of patients with IBD will require management by practitioners experienced in IBD.
Even now, IBD places a significant economic burden on the healthcare system in the United States. A recent report from the Crohn’s and Colitis Foundation evaluated direct and indirect health care costs during 2007–2016 from over 52,000 patients with IBD, compared to a cohort of non-IBD patients.5 IBD patients had three times the costs per year compared to non-IBD patients (approximately $22,000 vs $7,000 per year) with the highest costs occurring in the first year after diagnosis (over $25,000). Furthermore, these patients were estimated to pay high out-of-pocket costs, regardless of insurance premium costs. Of note, costs increased over time during the study period. The authors estimated that many variables are associated with increased costs of IBD care including biologic medications, emergency room visits and subsequent hospitalizations, and significant comorbidities (for example, psychiatric diseases and anemia). Given these high and rising costs, providing high-value and cost-conscious care is a priority for many providers as well as their patients.
Introduction to Telemedicine
Telemedicine is defined as the use of electronic communications to provide patient care.6 Other loosely defined but related terms include telehealth and telecare.7 Telemedicine can utilize diverse methods of communication including text messages and other mobile applications, phone calls, email, video, and patient portals to improve or obtain access to care or communicate with health care providers (see Figure 1).8 Remote patient monitoring can be a useful tool to increase the data used by providers to make patient care decisions. Domains of telemedicine include telemonitoring, telemanagement, teleconsultation, and tele-education.6 The concept of telemedicine is not novel.9
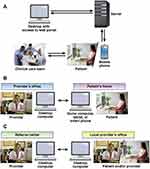 |
Figure 1 Different models of telemedicine. (A) Communication between the patient and clinical care team using electronic technology, for example, mobile phone. (B) Telehealth visit with both the patient and provider using computers to interact. (C) Tele-consultation with providers utilizing electronic technology to communicate. Reprinted from Clin Gastroenterol Hepatol, 15, Cross RK, Kane S, Integration of telemedicine into clinical gastroenterology and hepatology practice, pages no:175–181, copyright (2017), with permission from Elsevier.8 |
Prior to the advent of modern technologies, patients were required to travel, often great distances, to gain consultation by healers (physicians, shamans, etc.) although providers often did make house calls.9 The advent of hospitals sequestered medical care to certain regions and the proportion of medicine that was delivered via house-call decreased to less than 1% by 1980.
Over time, technology evolved and the transmission of medical information, for example, chest x-rays, was common by the 1960s.9 In the 1960s to the 1970s, the National Aeronautics and Space Administration (NASA) developed a telemedicine program for its astronauts using satellites. Telemedicine over time became more widespread and by the 1990s, states developed programs with aims to serve the health care needs of unique patient populations such as prisoners and those in difficult-to-access rural areas (for example, in Alaska and Native Americans in Arizona).
Today, various types of telemedicine are used in all 50 states in a wide variety of settings to achieve diverse goals.9 The American Telemedicine Association (ATA) was founded in 1993 as a non-profit organization that advocates for the use of telemedicine.10 The Balanced Budget Act of 1997 allowed Medicare reimbursements for telemedicine and funding for projects. Other recent federal bills and offices such as the American Recovery and Reinvestment Act of 2009 and Office for the Advancement of Telehealth have helped increase the funding and clarify policies regarding telemedicine.
Many studies have looked at the use of telemedicine as a diagnostic, monitoring, educational, and management tool. Telemedicine in the treatment of IBD has been shown to be both acceptable and feasible by patients.11,12 Here we will summarize the most notable and recent studies on this subject.
Summary of Telemedicine Trials in Patients with Inflammatory Bowel Disease
Telemedicine as a Diagnostic Tool
Diagnosing CD or UC requires physical exam as well as endoscopic and radiographic evaluation therefore telemedicine is unable to contribute in this aspect. However, telemedicine can be used in other ways, for example, remote symptom monitoring and collecting diagnostic information (such as body weight and home point of care testing for diagnostics such as fecal calprotectin). Telemedicine can also be used to review pathology (termed telepathology) and diagnostic imaging. Remote symptom monitoring will be discussed in a subsequent section.
One study conducted in the Netherlands compared smartphone-based analysis of stool specimens with laboratory analysis for longitudinal tracking of children with IBD.13 Fecal calprotectin is a stool test that reflects intestinal inflammation; because the test is non-invasive, it is often used for disease monitoring. The study utilized a lateral flow-based calprotectin test performed on stool samples collected at home. These stool samples were processed by the patient or family member and the final step was to take a picture of the test cassette with a smartphone. The result of the analysis was available immediately and sent to the research team who could then incorporate this result into the assessment of the patient and subsequently adjust management as indicated. A comparison of the home analysis with professional laboratory analysis using ELISA showed that 64–81% of the measurements were in agreement of predetermined ranges for higher and lower fecal calprotectin ranges. Similarly, 71–94% of test results were within range comparing the Quantum Blue laboratory analysis with the home analysis.
Telepathology utilizes the electronic transmission of pathology slide images.14 This is particularly relevant in confirming dysplasia from surveillance biopsies in patients with chronic colitis. In one study published in 2006, images were remotely viewed and interpreted by expert pathologists and compared with a reference pathologist. There was a low interobserver agreement (K=0.32) between the expert and reference pathologist with the lowest levels of agreement among the indefinite and low-grade dysplasia categories; slides evaluated as negative for dysplasia or with high-grade dysplasia showed higher levels of interobserver agreement. Given that gastrointestinal pathologists are less common, the use of telepathology to augment findings by a general pathologist may be useful.
Telemonitoring and Telemanagement
As with other chronic illnesses, patient engagement is essential in the management of IBD as an agency over one’s illness can improve patient outcomes. Patients with CD and UC who gain a better understanding of their chronic condition are more likely to play an active role in their healthcare and decision-making.15 Online and mobile applications allow patients to stay attuned to their chronic condition and collaborate with their care team between visits. Project Sonar is a care management solution developed by Kosinski et al that facilitated self-monitoring of disease activity.16 The real-time data provided by patients allowed providers an opportunity to intervene before disease progression. These support tools have been shown to decrease readmission rates and health care utilization among high-risk patients.16,17
Effective care for chronic diseases such as IBD requires ongoing monitoring between routine office visits. Various online and mobile applications have been developed over the years tracking patients’ clinical progress, with or without communication of these data to the care team. “GI Buddy” was a mobile application developed by the Crohn’s and Colitis Foundation that allowed patients to document personal health records, as well as their symptoms, diet, physical activity, and medication adherence.18 In addition, the application provided medication reminders to promote adherence. “GI Buddy” did not, however, provide direct data transfer to the care team. As a result, health care providers could not provide feedback to patients through this system except at the time of routine office visits. The application did provide patients with a mechanism to better track and organize symptoms between visits.
Feedback from providers and other members of the care team is important for patient’s self-care and for adherence to telemedicine applications. HealthPROMISE is a cloud-based patient-reported outcome and remote patient monitoring platform developed by AppLab, Icahn School of Medicine at Mount Sinai.19 Patients receive automated reminders to complete self-testing, report quality of life and medication adherence, and receive patient education. Through this application, providers can obtain real-time data bridging the gap of care between office visits. Adherence to remote monitoring was good, with 75% of patients continuing to use the application and over 90% of patients recommending the application to others. Improvement in quality of life was noted amongst HealthPROMISE patients with over 1 year of follow-up.
Cross and Finkelstein studied a home telemanagement system, consisting of a laptop computer and an electronic scale.12 Patients logged into the provided computers and complete short questionnaires on symptoms and medication side effects on a weekly basis for 6 months. Alerts were developed based on responses that were reviewed by the health care team. Adherence to self-testing was 91% over the 6-month study. Eight-six percent of the enrolled patients stated that the testing did not interfere with their activities and 91% thought that the testing was not complicated and that it took little time. Secondary analyses also demonstrated trends toward improved control of disease activity and quality of life and significant improvement in patient knowledge.
Cross et al then conducted a small randomized controlled trial of remote monitoring with a home automated telemanagement system for patients with UC.20 Patients were randomly assigned 1:1 to either the control arm or the weekly remote monitoring arm. Monitoring included symptom reporting as well as an electronic weight scale to measure body weight with results automatically forwarded to the research team. Action plans were subsequently created that were automatically delivered to the patients after testing. The goal of the action plan was for patients to initiate self-care. The remote monitoring arm continued to receive standard monitoring identical to the control arm (i.e. routine follow-up visits and telephone calls with more urgent problems). Attrition was high in the telemanagement group during the one-year study (44% compared to 23% in standard care). However, patients in the experimental arm experienced a non-significant decrease in disease activity over time and a significant and clinically meaningful increase in disease-specific quality of life compared to the control arm over 1 year.
Constant Care was a website-based remote monitoring system that created action plans based on patients' self-reported symptoms. The group first demonstrated the feasibility of the system to provide education and for patients to initiate self-management. The investigators then evaluated the system in a year-long randomized, controlled trial in patients with UC.21 Similar to the study by our group, attrition was high during the study (59%). Overall, adherence to acute treatment, knowledge, and quality of life were improved. Additionally, relapses were shorter in the experimental arm compared to the control arm. Routine and urgent office visits were decreased in the web group with estimated costs savings of 189 Euro per year. Conversely, the number of electronic messages and telephone calls were significantly greater in the web group. The same research group later demonstrated that remote monitoring with the addition of home collection and analysis of calprotectin could be used to individualize the dosing of infliximab.22
To address the high attrition rates reported in prior studies, our group conducted a large, multicenter, randomized, controlled trial of a revised system that provided remote monitoring via text messaging.23 Three hundred forty-eight patients were enrolled in the TELEmedicine for Patients with Inflammatory Bowel Disease (TELE-IBD) study. Patients were randomized 1:1:1 to standard care, remote monitoring every other week, or remote monitoring every week. The improved delivery system was associated with much lower rates of attrition than in prior studies (19% in the weekly group) and nearly 75% of patients completed the 1-year follow-up. Overall, remote monitoring was not associated with an improvement in disease activity or disease-specific quality of life. However, it should be noted that all three groups improved in these areas over time. Remote monitoring was associated with a decreased rate of both IBD-related and non-IBD-related hospitalizations. Conversely, remote monitoring patients were significantly more likely to undergo diagnostic testing, electronic communications, and telephone calls than control patients.
Another remote monitoring system, myIBDcoach, was examined in a clinical trial in the Netherlands where patients were randomized to receive telemedicine intervention or standard care in two academic and two non-academic outpatient settings.24 Patients enrolled in this study used remote monitoring as a replacement for standard care. Patients regularly registered disease activity online where the health care team could review the results and intervene if necessary (see Figure 2). The mean number of outpatient visits at 12 months was significantly lower in the intervention arm compared to the standard care arm (1.55 vs. 2.34; p<0.0001). The mean number of hospital admissions was also lower in the intervention arm (0.05 vs. 0.10; p=0.046). Mean number of emergency visits, corticosteroid courses, and surgeries did not differ between the groups.
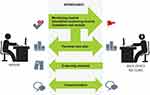 |
Figure 2 Representation of myIBDcoach depicting monitoring, personal care plan, e-learning modules, and communication between the patient and provider. de Jong M, van der Meulen-de Jong A, Romberg-Camps M, et al. Development and feasibility study of a telemedicine tool for all patients with IBD: myIBDcoach. Inflamm Bowel Dis. 2017;23:485–493, by permission of Oxford University Press.28 |
Telehealth Visits
Disparities between care for patients from urban vs. rural communities can unfortunately affect disease outcomes in IBD. Benchimol and colleagues found that IBD patients who live in rural areas of Canada had fewer gastroenterologist visits, more hospitalizations and greater rates of emergency department visits.26 For patients with IBD in general, finding a gastroenterologist sufficiently experienced in IBD management may necessitate time-consuming and costly travel. This can be even worse for patients with more complex diseases who may require care by multiple specialists. Televisits with online video conferencing can be a cost-effective and an efficient alternative to routine office visits in the management of IBD that may alleviate these disparities.
Krier et al conducted a prospective, randomized, controlled study in a Veterans Affairs population which randomized 34 Veterans to an experimental arm where trainees underwent remote supervision of patient care with a highly experienced gastroenterologist located 40 miles away.11 They found that the number of Veterans seen per session, length of visit, and satisfaction with visits was equal between the two groups.
In a study conducted at Dartmouth-Hitchcock Medical Center consisting of 48 IBD patients who participated in telehealth visits, a large proportion of patients (81%) lived more than 25 miles away from their provider.27 When compared to standard clinic visits, patients reporting saving a half day to a full day of time by participating in televisits. Furthermore, replacing standard clinic visits with a telehealth visit saved them an average cost of $62 (range: less than $50 to more than $200). Ninety-one percent of the patients in this study felt that their providers understood their disease state after the telehealth visit and 78% reported a clear understanding of their provider’s recommendations. There were no significant differences in quality measures including current steroid use, current biologic therapy, narcotic use, or health care utilization before and after televisits.
Likewise, the majority of patients undergoing telehealth visits at the University of Maryland felt that conducting visits was not complicated and shorter in duration to routine visits. Nearly 90% felt that all their concerns were addressed at the telehealth visit with reported time savings of 1–3 hrs in 53% of patients and more than 3 hrs in 41% of patients.8 Thus, telehealth visits may help to close the gaps in accessibility and affordability of IBD care, especially for those living in remote areas.27,28 Additionally, multidisciplinary care addressing nutrition, stress, and smoking can also be integrated in IBD telehealth visits.25
Teleconsultation
Technological advancement has not only improved access to care for patients but has also enhanced physician interactions through teleconsultation. The IBD Live interinstitutional and interdisciplinary videoconference education (IBD LIVE) series is a case conference platform for health care providers from multiple institutions and specialties to convene and discuss complex IBD management.29 At each 1 hr conference, two complex IBD cases are presented and providers review evidence-based data, exchange ideas and provide input on management strategies. Technology is provided by an information technology specialist and Chorus Call, Inc., an international teleconferencing service provider. Many of the attendees of this conference have given positive responses on how the conference has changed their practice. The Continuing Medical Education scores (1 = worst to 5 = best) have a high median overall score of 4.6 (range 3.2–5.0). IBD LIVE began in 2009 with 3 sites and has grown to over 20 sites.
Conclusion
Telemedicine can serve an important role in the management and treatment of chronic diseases such as IBD. It can serve as a unique adjunct in the long-term care of patients with UC and CD in the domains of monitoring, management, and consultation. Through the use of technologies associated with phones, tablets, laptops, and other electronic tools, improvement in communication between patients and their medical providers can be achieved. These technologies have been increasing in use over time; however, there are several limitations to telemedicine existing in its current form (see Table 1).
 |
Table 1 Pros and Cons of Telemedicine in the Management of Inflammatory Bowel Disease |
In this review article, we summarized key literature regarding telemedicine in the management of patients with inflammatory bowel disease (Table 2). Telemedicine has a limited role in the initial diagnosis of diseases such as UC or CD. Furthermore, patients with new alarming symptoms such as fever, intractable pain, nausea/vomiting, and symptoms concerning for perianal abscess or intra-abdominal sepsis warrant physical exam and should be evaluated in person rather than through telehealth visits. Providers participating in telemedicine should advise patients in advance of the symptoms that would warrant an in-person evaluation rather than a telehealth visit.
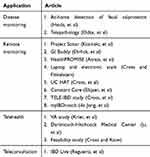 |
Table 2 Main Applications of Telemedicine in Inflammatory Bowel Disease |
It is also important to note that legal and regulatory oversights vary from state to state. The American Telemedicine Association has published an analysis with policies of each of the fifty states.30 Some states require that patients have an in-person visit prior to a telehealth visit. Informed consent is often required as well. Location of service is usually defined as location where the patient is situated. Providers providing interstate telehealth will often need licensure at the respective state(s) and are under the jurisdiction of that state. The Federation of State Medical Boards developed an Interstate Licensure Compact that now includes 29 states, the District of Columbia and the Territory of Guam.31
In general, patients are receptive of technology involved with telehealth and telemonitoring but malfunctioning of hardware or software can disrupt a visit.8 Cybersecurity is a crucial component of telemedicine, and it requires continuous efforts to ensure the protection of patient privacy and to prevent hackers from gaining access to personal health information.
Many providers are reticent to utilize remote monitoring or to conduct telehealth visits. One of the fears that providers have is the increased, non-reimbursed work created by remote monitoring. Improving access and monitoring is important but payers and health system will need to realize the increased new type of work created by these systems. Many payers do not reimburse for telehealth services; additionally, some payers require patients to go to local providers' offices to communicate with a distant provider. These barriers need to be relaxed to fully realize the benefits of telehealth.
Additionally, remote monitoring systems that are not linked to electronic medical records systems are less useful. Providers and the care team need to be able to seamlessly synthesize testing results to other diagnostics with the EMR. Another issue related to telehealth and teleconsultation is the requirement for significant investment to provide services.
We believe that telemedicine has the potential to revolutionize the way we practice medicine in a positive and significant way. Given the evolution of electronics and electronic communications and their roles in our day-to-day lives, it seems likely that telemedicine will also continue to develop and eventually overcome its current barriers, particularly those relating to cybersecurity and provider reimbursements. In the author’s opinion, telemedicine is truly the way of the future and is likely to play a substantial role in the management of patients going forward. Overall, telemedicine has the potential to improve care by increasing communications between patients and providers, reduce the need for patient visits to the clinic or laboratory, and overall increase the efficiency and efficacy of health management. Certainly, further studies are needed to better delineate the optimal role of telemedicine in the treatment of patients with IBD. Despite the barriers that currently exist, we believe that telemedicine has an important role to play in the future of care of patients with IBD.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Kaplan GG. The global burden of IBD: from 2015 to 2025. Nat Rev Gastroenterol Hepatol. 2015;12:720–727. doi:10.1038/nrgastro.2015.150
2. Opstelten JL, Vaartjes I, Bots ML, et al. Mortality after first hospital admission for inflammatory bowel disease: a nationwide registry linkage study. Inflamm Bowel Dis. 2019;25:1692–1699. doi:10.1093/ibd/izz055
3. Molodecky NA, Soon IS, Rabi DM, et al. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology. 2012;142:
4. Dulai PS, Singh S, Ohno-Machado L, et al. Population health management for inflammatory bowel disease. Gastroenterology. 2018;154:37–45. doi:10.1053/j.gastro.2017.09.052
5. Park KT, Ehrlich OG, Allen JI, et al. The cost of inflammatory bowel disease: an initiative from the crohn’s & colitis foundation. Inflamm Bowel Dis. 2020;26:1–10. doi:10.1093/ibd/izz104
6. Aguas M, Del Hoyo J, Faubel R, et al. Telemedicine in the treatment of patients with inflammatory bowel disease. Gastroenterol Hepatol. 2017;40:641–647. doi:10.1016/j.gastrohep.2017.07.001
7. Stanberry B. Telemedicine: barriers and opportunities in the 21st century. J Intern Med. 2000;247:615–628. doi:10.1046/j.1365-2796.2000.00699.x
8. Cross RK, Kane S. Integration of telemedicine into clinical gastroenterology and hepatology practice. Clin Gastroenterol Hepatol. 2017;15:175–181. doi:10.1016/j.cgh.2016.09.011
9. Nesbitt TS, Katz-Bell J. History of Telehealth. In: Schulder Rheuban K, Krupinski EA, editors. Understanding Telehealth. New York: McGraw-Hill Education; 2018. Available from: http://accessmedicine.mhmedical.com/content.aspx?bookid=2217§ionid=187794434.
10. About us. American telemedicine association. Available from: https://www.americantelemed.org/about-us/.
11. Krier M, Kaltenbach T, McQuaid K, et al. Potential use of telemedicine to provide outpatient care for inflammatory bowel disease. Am J Gastroenterol. 2011;106:2063–2067. doi:10.1038/ajg.2011.329
12. Cross RK, Finkelstein J. Feasibility and acceptance of a home telemanagement system in patients with inflammatory bowel disease: a 6-month pilot study. Dig Dis Sci. 2007;52:357–364. doi:10.1007/s10620-006-9523-4
13. Heida A, Knol M, Kobold AM, et al. Agreement between home-based measurement of stool calprotectin and ELISA results for monitoring inflammatory bowel disease activity. Clin Gastroenterol Hepatol. 2017;15:1742–1749.e2. doi:10.1016/j.cgh.2017.06.007
14. Odze RD, Tomaszewski JE, Furth EE, et al. Variability in the diagnosis of dysplasia in ulcerative colitis by dynamic telepathology. Oncol Rep. 2006;16:1123–1129.
15. Baars JE, Markus T, Kuipers EJ, et al. Patients’ preferences regarding shared decision-making in the treatment of inflammatory bowel disease: results from a patient-empowerment study. Digestion. 2010;81:113–119. doi:10.1159/000253862
16. Kosinski LR, Brill J, Regueiro M. Making a medical home for IBD patients. Curr Gastroenterol Rep. 2017;19:20. doi:10.1007/s11894-017-0561-1
17. Kosinski LBJ, Sorensen M, Baum C, Turpin R, Landsman-Blumberg P. Project sonar: reduction in cost of care in an attributed cohort of patients with Crohn’s disease. Gastroenterology. 2016;150:S173. doi:10.1016/S0016-5085(16)30668-0
18. Ehrlich O, Atreja A, Markus-Kennell S, Frederick K. CCFA GI buddy provides patient reported outcomes and IBD symptoms evaluation. Inflamm Bowel Dis. 2012;18:S35–S36. doi:10.1097/00054725-201212001-00083
19. Atreja A, Khan S, Rogers JD, et al. Impact of the mobile healthPROMISE platform on the quality of care and quality of life in patients with inflammatory bowel disease: study protocol of a pragmatic randomized controlled trial. JMIR Res Protoc. 2015;4:e23. doi:10.2196/resprot.4042
20. Cross RK, Cheevers N, Rustgi A, et al. Randomized, controlled trial of home telemanagement in patients with ulcerative colitis (UC HAT). Inflamm Bowel Dis. 2012;18:1018–1025. doi:10.1002/ibd.21795
21. Elkjaer M, Shuhaibar M, Burisch J, et al. E-health empowers patients with ulcerative colitis: a randomised controlled trial of the web-guided ‘constant-care’ approach. Gut. 2010;59:1652–1661. doi:10.1136/gut.2010.220160
22. Pedersen N, Elkjaer M, Duricova D, et al. eHealth: individualisation of infliximab treatment and disease course via a self-managed web-based solution in Crohn’s disease. Aliment Pharmacol Ther. 2012;36:840–849. doi:10.1111/apt.12043
23. Cross RK, Langenberg P, Regueiro M, et al. A randomized controlled trial of TELEmedicine for patients with Inflammatory Bowel Disease (TELE-IBD). Am J Gastroenterol. 2019;114:472–482. doi:10.1038/s41395-018-0272-8
24. de Jong MJ, van der Meulen-de Jong AE, Romberg-Camps MJ, et al. Telemedicine for management of inflammatory bowel disease (myIBDcoach): a pragmatic, multicentre, randomised controlled trial. Lancet. 2017;390:959–968. doi:10.1016/S0140-6736(17)31327-2
25. Benchimol EI, Kuenzig ME, Bernstein CN, et al. Rural and urban disparities in the care of Canadian patients with inflammatory bowel disease: a population-based study. Clin Epidemiol. 2018;10:1613–1626. doi:10.2147/CLEP.S178056
26. Li SX, Thompson KD, Peterson T, et al. Delivering high value inflammatory bowel disease care through telemedicine visits. Inflamm Bowel Dis. 2017;23:1678–1681. doi:10.1097/MIB.0000000000001210
27. Ruf B, Jenkinson P, Armour D, et al. Videoconference clinics improve efficiency of inflammatory bowel disease care in a remote and rural setting. J Telemed Telecare. 2019;1357633x19849280.
28. de Jong M, van der Meulen-de Jong A, Romberg-Camps M, et al. Development and feasibility study of a telemedicine tool for all patients with IBD: myIBDcoach. Inflamm Bowel Dis. 2017;23:485–493. doi:10.1097/MIB.0000000000001034
29. Regueiro MD, Greer JB, Binion DG, et al. The inflammatory bowel disease live interinstitutional and interdisciplinary videoconference education (IBD LIVE) series. Inflamm Bowel Dis. 2014;20:1687–1695. doi:10.1097/MIB.0000000000000187
30. Thomas LCG 50 state telemedicine gaps analysis: physician practice standards & licensure. Volume 2019; 2014. Available from: http://www.americantelemed.org/docs/default-source/policy/50-state-tele-medicine-gaps-analysis–physician-practice-standards-licensure.pdf.
31. American Academy of Dermatology. FSMB interstate medical licensure compact. Website. Available from: https://www.aad.org/advocacy/state-policy/fsmb-interstate-compact.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
