Back to Journals » Clinical Ophthalmology » Volume 15
Tectonic Deep Anterior Lamellar Keratoplasty to Treat Corneal Perforation and Descemetocele from Microbial Keratitis
Authors Nguyen HT , Pham ND, Mai TQ , Do HTT, Nguyen DTN, McCluskey P, Pham TV
Received 13 June 2021
Accepted for publication 11 August 2021
Published 24 August 2021 Volume 2021:15 Pages 3549—3555
DOI https://doi.org/10.2147/OPTH.S324390
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Hong The Nguyen,1,2 Ngoc Dong Pham,3 Tung Quoc Mai,2 Hang Thi Thuy Do,3 Duong Thi Nga Nguyen,3 Peter McCluskey,4 Trong Van Pham2
1Department of Ophthalmology, 108 Military Central Hospital, Hanoi, Vietnam; 2Department of Ophthalmology, Hanoi Medical University, Hanoi, Vietnam; 3Department of Cornea, Vietnam National Eye Hospital, Hanoi, Vietnam; 4Department of Ophthalmology, University of Sydney, Sydney, NSW, Australia
Correspondence: Tung Quoc Mai
Department of Ophthalmology, Hanoi Medical University, 1 Ton That Tung Street, Hanoi, 100000, Vietnam
Tel +84 915644181
Email [email protected]
Purpose: To evaluate the result of tectonic deep anterior lamellar keratoplasty (DALK) for keratitis with perforation and descemetocele.
Patients and Methods: A prospective clinical study of 36 patients (36 eyes) treated with tectonic DALK for corneal perforation or descemetocele from microbial keratitis managed at the Vietnam National Eye Hospital over a two-year period. The surgical technique was manual lamellar dissection. The grafts were harvested from the anterior corneal cap of pre-cut donor tissues used for DSAEK or donor corneas with a low endothelial cell count.
Results: A mean age was 55.36 ± 13.98 years (ranged from 25 to 75 years). Female gender represented 52%. causative agents were herpes simplex virus (58.3%), bacteria (22.2%), fungi (13.9%) and microsporidia (5.6%). There were 24 eyes with descemetocele (66.7%) and 12 with perforation (33.3%). There were 33 successful cases (91.7%) and 3 failed cases (8.3%). Best corrected visual acuity (BCVA) improved in 28 eyes (84.8%). The range of post-operative BCVA was from hand motions to 20/70. Eleven eyes (33.3%) attained vision 20/200 and higher. Clear graft was obtained in 15 eyes (45.5%), while mild or severe graft opacity was observed in 14 eyes (42.4%), and 4 eyes (12.1%), respectively. Surgical complications included descemet rupture (20.8%), pseudo anterior chamber (41.6%), persistent corneal epithelial defects (8.3%), reinfection (11.1%), glaucoma or ocular hypertension (5.6%) and cataract (8.3%).
Conclusion: The study demonstrates that DALK is an effective procedure to treat corneal descemetocele, especially when an urgent penetrating keratoplasty (PKP) cannot be performed.
Keywords: deep anterior lamellar keratoplasty, DALK, descemetocele, corneal perforation, corneal transplantation
Introduction
Corneal perforation or descemetocele from microbial keratitis may lead to severe vision loss and ocular morbidity from secondary glaucoma, cataract, endophthalmitis. Evisceration of the eye may be required.1 Surgical intervention depends on the underlying pathogen, the size and depth of corneal stromal involvement, the location of the corneal defect, and the visual potential. Surgery aims to maintain or restore corneal integrity, eradicate infection, and stabilize or improve visual acuity. Available treatments range from bandage contact lens, use of cyanoacrylate or fibrin glue, amniotic membrane transplant, conjunctival flap, lamellar keratoplasty to penetrating keratoplasty (PKP).2 Corneal grafts offer the prospect of long-term control of the corneal disease, whereas most other treatments are short-term solutions. For many years, PKP has been the standard procedure for a corneal perforation or descemetocele.2,3 More recently, deep anterior lamellar keratoplasty (DALK) has been performed as it may reduce anterior synechiae, expulsive hemorrhage, post-operative inflammation, and endothelial graft rejection.4,5
Furthermore, DALK does not rely on high endothelial cell density or fresh corneal donor tissue. Vietnam is among the Asian developing agricultural countries with its only eye bank serving the population of 90 million, and cultural burial practices that result in low corneal donation rates.6 This study reports the outcome of tectonic DALK using either the anterior corneal cap of pre-cut donor tissue for DSAEK or donor tissue with low endothelial cell count, to treat corneal perforations and descemetoceles due to microbial keratitis.
Methods
A prospective clinical series of 36 patients (36 eyes) treated with a tectonic DALK for corneal perforation or descemetocele from microbial keratitis, managed at the Vietnam National Eye Hospital (VNEH) from January 2018 to March 2020 was collected.
The recipient cornea was marked and partly cut using a hand-held trephine with its diameter 0.5mm larger than that of the lesion. In the case of corneal perforation, corneal lesion was marked by the trephine and marking pen, and then the incision was made with 15° blade (Alcon). Corneal stromal was dissected to the level of the pre-Descemet layer using a dissector blade (DCORT) and a curved corneal scissor (GEUDER), from the periphery into the central lesion. In case the lesion’s diameter less than 7.5 mm, grafts were harvested from the anterior corneal cap of pre-cut donor tissues used for DSAEK (from Cornea Gen eye bank). If the lesion’s diameter from or over 7.5mm, full thickness cornea with the low endothelial cell count (<1000 cells/mm2) (from VNEH eye bank) were used and the endothelium removed prior to donor’s trephination. A donor size 0.50 mm larger than recipient bed was used. The graft was sutured to the recipient bed using interrupted 10–0 nylon.
Patients with bacterial keratitis continued topical Moxifloxacin hydrochloride 4 times daily (Vigamox, Alcon, USA), topical Prednisolone acetate 4 times/day for 3 months, tapered to once daily for 6 months (Pred Forte, Allergan). Topical sodium hyaluronate was instilled as needed (Sanlein, Santen, Japan). Topical and systemic antiviral medication were continued in patients with Herpetic keratitis. Appropriate topical anti-microbial medication was continued in the remaining patients. Topical corticosteroid therapy was individually titrated according to diagnosis and clinical course. Data were collected from routine follow-up at 2 weeks, 1 month, and then every 3 months post-operative. The mean observation time was 13.8 months (from 3 months to 24 months).
Pre-operative data collected included: age, sex, the duration between the infectious onset and surgery. Pathogen was microbiologically confirmed using the Gram stain and culture or real-time PCR (polymerase chain reaction) of removed corneal tissues. Clinical features and best corrected visual acuity (converted to LogMAR) were noted.7 Defect location was categorized as central (involving visual axis, ≤5.0mm diameter of the central cornea), paracentral (zone over 5.0mm up to 8.0mm) or peripheral (≥8.0mm), also including the limbus.8
Post-operative outcomes included: BCVA, surgical outcome, graft transparency and complications. Success was defined as resolution of infection and preservation of ocular integrity. Failure was defined as recurrence of infection or graft failure requiring conversion to PKP, or evisceration. Graft clarity was graded using a VNEH subjective grading scheme (see Table 1).
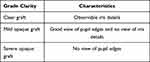 |
Table 1 VNEH Subjective Grading Scheme |
Results
The study included 36 eyes of 36 patients (21 males and 15 females) with a mean age of 55.36 ± 13.98 years (range from 25 to 75 years), a mean pre-operative course was 79.1 ± 82.1 days (range from 16 to 360 days). There were 24 eyes with descemetocele (66.7%) and 12 with a corneal perforation (33.3%). Microbial keratitis was the aetiology in all eyes. And the highest rate was Herpes Simplex Virus (HSV) (21 eyes, 58.3%). The causes are detailed in Table 2. The mean corneal lesions size was 4.3 ± 1.6 mm (range, 2.5 mm to 8.5 mm). The location of the perforation or descemetocele was central in 19 eyes (52.8%), paracentral in 12 eyes (33.3%) and peripheral in 5 eyes (13.9%).
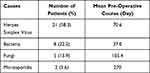 |
Table 2 Pathogens and Preoperative Time |
Twenty-seven of the DALKs were performed using discarded DSAEK anterior corneal caps with a mean size of 6.3 ± 1.7 mm. Nine DALKs were performed using lamellar tissue from donor tissue unsuitable for PKP with a mean size of 8.1 ± 0.3 mm. In the group with descemetocele, 5 eyes (20.8%) were accidentally perforated during the manual dissection. In all cases, the DALK was successfully completed.
The mean preoperative BCVA was 2.03 ± 0.44. The average BCVA at the last follow-up visit was 1.46 ± 0.48. The detailed changes in visual acuity between pre- and post-operation are shown in Table 3. Excluding 3 failed cases, the average BCVA at the last follow-up visit was 1.40 ± 0.48. BCVA improved post-operatively in 28 eyes (84.8%), unchanged in 4 eyes (12.1%) and decreased in one eye (3.1%). A clear graft was seen in 15 eyes (45.5%), mild and severe opaque graft in 14 eyes (42.4%) and 4 eyes (12.1%), respectively.
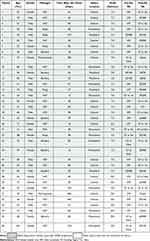 |
Table 3 Pre- and Post-Operative Visual Acuity |
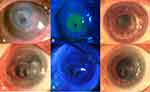
There were 33 successful (91.7%) and 3 failed cases (8.3%). Figure 1 demonstrates two successful cases at 12 months after surgery. The success and failure by pathogen and type of grafts are displayed in Table 4. All 3 failures were due to recurrent infection by microsporidia (2 eyes) and HSV (1 eye). Two eyes with microsporidia keratitis presented the recurrent infection at the host-donor interface at 2- and 3-month follow-up. PKP has been done with preserved structural integrity in one eye, the other underwent endophthalmitis and then enucleation. Recurrent HSV keratitis has also been reported on the graft after 2 months, which required further PKP after anti-viral failure.
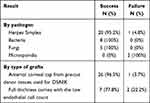 |
Table 4 Surgical Result by and Pathogen and Type of Grafts |
Post-operative graft–host interface haze following DALK was the most common complication (21 eyes, 58.3%), followed by pseudo-anterior chamber in 15 eyes (41.6%), which required further air injection in 3 eyes, while spontaneous resolution occurred over a mean of 6.2 days (from 2 to 14 days) in the remaining eyes. The average duration of re-epithelialization was 6.7 ± 10.3 days (from 2 to 45 days). Persistent corneal defect was noted in 3 eyes (8.3%), up to 14 days. Bandage soft contact lenses and autologous serum eye drops helped the complete re-epithelization in 34 and 45 days. The others were treated with bandage soft contact lenses, autologous serum eye drops and tarsorrhaphy and healed in 28 days. Corneal neovascularization and Descemet membrane folds developed in 12 eyes (33.3%) and 14 eyes (38.8%), respectively. Ocular hypertension occurred post-operatively in 2 eyes (5.6%), with one eye controlled medically and the other requiring trabeculectomy. Cataract developed in 3 eyes (8.3%).
Discussion
Corneal perforation and descemetocele due to microbial keratitis are ocular emergencies. Intensive medical management with appropriate topical anti-microbial drugs is critical and surgical intervention such as corneal patch with tissue adhesives, amniotic membrane graft, and conjunctival flaps is often required to restore anatomic integrity and minimize complications.1,3,9
Keratoplasty techniques are an alternative procedure to preserve globe integrity and include corneal patch grafts, lamellar keratoplasty and PKP. In recent years, DALK has replaced PKP due to a number of advantages, such as the absence of endothelial graft rejection, reduced risk of extension of intraocular infections, the decreased incidence of cataract and glaucoma development.1,3,9,10 Further, DALK does not require donor tissue with a high endothelial cell density donor tissue,11 which is important in countries such as Vietnam where there is a shortage of donor corneal tissue.
The initial indication for DALK, such as keratoconus, stromal scar, or corneal dystrophy, has been recently expanded to include microbial keratitis such as: bacteria, fungal, HSV, microsporidia and Acanthamoeba and obtain potential outcomes.12–15 After recent studies, success rate of DALK was high in patients with severe keratitis, which varied according to bacterial, fungal, viral or protozoan causes.16,17 In the case of microsporidia, DALK has been reported to incompletely eradicate the pathogens.18,19 The big bubble technique has been suggested to completely remove pathological stroma and thus lower recurrent infection rate.15,16
Results in our study also revealed the comparability and difference with other studies.15–18 It can be explained by the difference in lesions and disease stages of each study.16,17 In the current study, the mean duration between onset of infection and surgical performance was 79.1 ± 82.1 days (16–360 days) which implies that patients underwent surgery at the end stage of their infection.
Visual outcome improved in our study, with 33.3% of eyes having 20/200 and higher (Table 3). This outcome was significantly lower than in other studies. Li (2011) has achieved 56.3% of cases with post-operative visual acuity ≥20/40 while 50% of Anshu series (2009) were reported to gain post-operative visual acuity ≥6/9.16,17 My study reported result similar to that of Soong (2000) who explained the defect size, duration and severity of infection to be the leading causes.20
Relating to graft tissues, precut anterior lamellar caps and acellular porcine corneal stroma have been used to treat bacterial, fungal, Acanthamoeba and HSV keratitis.21,22 In this study, 27 grafts were anterior corneal stroma from previous DSAEK corneas (75%), and 9 grafts (25%) were from corneas with low endothelial cell density that did not meet PKP requirement. This practice may optimize the use of tissue donors. Descemet membrane (DM) perforation and pseudo-anterior chamber were reported to be the most common intraoperative complications.4 And the incidence was found lower with Anwar big-bubble technique in comparison to manual DALK with layer-by-layer dissection.4 In the current study, DM perforations were small micro-perforations and did not require conversion to PKP. During post-operative follow-up, 41.7% of patients developed a transient pseudo-anterior chamber which resolved over 2 to 14 days without specific intervention in all but 2 patients. These 2 eyes required injection of air into the anterior chamber. Eyes that required re-bubbling were those with double anterior chamber that did not change or improve during 3 or 5-day follow-up. In our experience, if the size of double anterior chamber progressively decreases during the early post-operative period, it is safe to wait for spontaneous resolution of interface fluid. In this study, spontaneous resolution of interface fluid has been observed in one eye over 14 days.
In addition to optimizing the source of donor cornea tissues, DALK has also a lower rate of complications than PKP, including graft rejection, elevated IOP, and corticosteroid-induced cataract.10 This study has demonstrated 3 eyes with cataract and 2 with ocular hypertension after DALK. Cataract surgery was indicated in 3 eyes and trabeculectomy in 1 eye when the high intraocular pressure was not medically controlled. The limitations of this study include the small sample size and variation of follow-up duration. Therefore, the effect of DALK on post-operative complications was not analyzed in this study.
Conclusion
DALK is an effective surgical procedure for corneal perforation and descemetocele in patients with microbial keratitis. DALK is an extremely useful surgical intervention when there is a shortage of corneal donor material.
Ethical Issue
This study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of Vietnam National Eye Hospital and Hanoi Medical University No. 15 NCS17/HĐĐĐĐHYHN 2018. All the patients participated in this study were informed about the purpose of the study, benefits, and potential risks of the treatment. They all voluntarily signed on the informed written consents. Signed consents to publish data containing identifiable information were also obtained from participants. All tissues were donated voluntarily with written informed consent, and that this was conducted in accordance with the Declaration of Istanbul.
Acknowledgments
The study has been conducted with the assistance and support from Vietnam National Eye Hospital in Hanoi, Vietnam.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis, and interpretation, or in all these areas, took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This study has not financially supported by any organization.
Disclosure
The authors have no conflicts of interest to disclose.
References
1. Jhanji V, Young AL, Mehta JS, Sharma N, Agarwal T, Vajpayee RB. Management of corneal perforation. Surv Ophthalmol. 2011;56(6):522–538. doi:10.1016/j.survophthal.2011.06.003
2. Tuli S, Gray M. Surgical management of corneal infections. Curr Opin Ophthalmol. 2016;27(4):340–347. doi:10.1097/icu.0000000000000274
3. Agarwal R, Nagpal R, Todi V, Sharma N. Descemetocele. Surv Ophthalmol. 2020. doi:10.1016/j.survophthal.2020.10.004
4. Karimian F, Feizi S. Deep anterior lamellar keratoplasty: indications, surgical techniques and complications. Middle East Afr J Ophthalmol. 2010;17(1):28–37. doi:10.4103/0974-9233.61214
5. Nanavaty MA, Vijjan KS, Yvon C. Deep anterior lamellar keratoplasty: a surgeon’s guide. J Current Ophthalmol. 2018;30(4):297–310. doi:10.1016/j.joco.2018.06.004
6. Dong PN, Han TN, Aldave AJ, Chau HT. Indications for and techniques of keratoplasty at Vietnam National Institute of Ophthalmology. Int J Ophthalmol. 2016;9(3):379–383. doi:10.18240/ijo.2016.03.09
7. Lange C, Feltgen N, Junker B, Schulze-Bonsel K, Bach M. Resolving the clinical acuity categories “hand motion” and “counting fingers” using the Freiburg Visual Acuity Test (FrACT). Graefe’s arch clin exp ophthalmol/Albrecht von Graefes Archiv fur klinische und experimentelle Ophthalmologie. 2009;247(1):137–142. doi:10.1007/s00417-008-0926-0
8. Krysik K, Dobrowolski D, Lyssek-Boron A, Jankowska-Szmul J, Wylegala EA. Differences in surgical management of corneal perforations, measured over six years. J Ophthalmol. 2017;2017:1582532. doi:10.1155/2017/1582532
9. Deshmukh R, Stevenson LJ, Vajpayee R. Management of corneal perforations: an update. Indian J Ophthalmol. 2020;68(1):7–14. doi:10.4103/ijo.IJO_1151_19
10. Tan DT, Dart JK, Holland EJ, Kinoshita S. Corneal transplantation. Lancet (London, England). 2012;379(9827):1749–1761. doi:10.1016/s0140-6736(12)60437-1
11. Ke L, Shen D, Wang H, Qiao C, Zeng Q. Lamellar keratoplasty combined with amniotic membrane transplantation for the treatment of corneal perforations: a clinical and in vivo confocal microscopy study. Biomed Res Int. 2020;2020:7403842. doi:10.1155/2020/7403842
12. Xie L, Shi W, Liu Z, Li S. Lamellar keratoplasty for the treatment of fungal keratitis. Cornea. 2002;21(1):33–37. doi:10.1097/00003226-200201000-00008
13. Sarnicola V, Toro P. Deep anterior lamellar keratoplasty in herpes simplex corneal opacities. Cornea. 2010;29(1):60–64. doi:10.1097/ICO.0b013e3181a317d3
14. Sarnicola E, Sarnicola C, Sabatino F, Tosi GM, Perri P, Sarnicola V. Early Deep Anterior Lamellar Keratoplasty (DALK) for acanthamoeba keratitis poorly responsive to medical treatment. Cornea. 2016;35(1):1–5. doi:10.1097/ico.0000000000000681
15. Ang M, Mehta JS, Mantoo S, Tan D. Deep anterior lamellar keratoplasty to treat microsporidial stromal keratitis. Cornea. 2009;28(7):832–835. doi:10.1097/ICO.0b013e3181930ddc
16. Anshu A, Parthasarathy A, Mehta JS, Htoon HM, Tan DT. Outcomes of therapeutic deep lamellar keratoplasty and penetrating keratoplasty for advanced infectious keratitis: a comparative study. Ophthalmology. 2009;116(4):615–623. doi:10.1016/j.ophtha.2008.12.043
17. Li J, Yu L, Deng Z, et al. Deep anterior lamellar keratoplasty using acellular corneal tissue for prevention of allograft rejection in high-risk corneas. Am J Ophthalmol. 2011;152(5):762–70.e3. doi:10.1016/j.ajo.2011.05.002
18. Font RL, Samaha AN, Keener MJ, Chevez-Barrios P, Jd G. Corneal microsporidiosis. Report of case, including electron microscopic observations. Ophthalmology. 2000;107(9):1769–1775. doi:10.1016/S0161-6420(00)00285-2
19. Sabhapandit S, Murthy SI, Garg P, Korwar V, Vemuganti GK, Sharma S. Microsporidial stromal keratitis: clinical features, unique diagnostic criteria, and treatment outcomes in a large case series. Cornea. 2016;35(12):1569–1574. doi:10.1097/ico.0000000000000939
20. Soong HK, Farjo AA, Katz D, Meyer RF, Sugar A. Lamellar corneal patch grafts in the management of corneal melting. Cornea. 2000;19(2):126–134. doi:10.1097/00003226-200003000-00002
21. Li J, Ma H, Zhao Z, et al. Deep anterior lamellar keratoplasty using precut anterior lamellar cap for herpes simplex keratitis: a long-term follow-up study. Br J Ophthalmol. 2014;98(4):448–453. doi:10.1136/bjophthalmol-2013-304199
22. Li S, Li M, Gu L, et al. Risk factors influencing survival of acellular porcine corneal stroma in infectious keratitis: a prospective clinical study. J Transl Med. 2019;17(1):434. doi:10.1186/s12967-019-02192-z
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.