Back to Journals » Open Access Journal of Contraception » Volume 5
Study on the patterns and trend in contraceptive use in South-South and North-Western zones of Nigeria: 2003–2011
Authors Ezire O, Idogho O, Theophilus A, Ikani S, Oluigbo O
Received 13 November 2013
Accepted for publication 18 January 2014
Published 26 August 2014 Volume 2014:5 Pages 65—72
DOI https://doi.org/10.2147/OAJC.S49541
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Onoriode Ezire,1 Omokhudu Idogho,2 Ajibade Theophilus,3 Samuel Ikani,4 Obi Oluigbo1
1Research and Evaluation Division, Society for Family Health, Nigeria; 2Enhancing Nigeria’s Response to HIV and AIDS Programme, Abuja, Nigeria; 3Population Council, Abuja, Nigeria; 4Strengthening HIV Prevention Services for Most-At-Risk Populations, Abuja, Nigeria
Background: Nigeria is ranked 13th among countries with the highest fertility rates in the world – 5.7 births per woman on average. Age specific fertility rates are as high as 121 and 225 per 1,000 for ages 15–19 and 20–24 years, respectively. Only 9.7% of currently married women in Nigeria use modern methods of family planning (FP). This figure, however, does not reveal important age, geographical, or educational differences in Nigeria. The overall purpose of the study is to establish hidden demographic factors that enhance usage of modern methods of FP.
Methods: Data for this study were obtained from four waves of the National and State Specific HIV and AIDS, Reproductive and Child Health Survey – NARHS/SARHS (2003, 2005, 2007, and 2011). Data were collected among men and women of reproductive age in the 36 states of Nigeria including Federal Capital Territory (FCT). For the analysis, the study was however limited to North West and South-South zones of Nigeria. Bivariate and multiple logistic regression was performed using SPSS version 20.
Results: Use of modern methods of FP has increased over time with an average annual increase of 0.47%. Different age groups, zones, and educational attainment prefer different modern methods of FP. Of all users of modern methods of FP, long lasting methods account for just 3% while condoms account for as high as 58%. Eighty-six percent of sexually active never married women use condoms for FP. Women in South-South Nigeria are over three times and five times more likely to use a modern method of FP and a condom, respectively.
Conclusion: Demographic characteristics significantly determine the patterns, trend, and use of modern methods of FP in the studied states. Bearing in mind identified challenges associated with short term methods, innovative ways should be identified to scale up use of long lasting methods. The study corroborates recommendations of previous studies promoting female child education as a way to improve use of modern methods of contraception.
Keywords: family planning, contraceptive use, Nigeria, condom, injectables
Introduction
Nigeria is ranked 13th among countries with the highest fertility rates in the world with 5.7 births per woman.1 Age specific fertility rates are as high as 121 and 225 per 1,000 for ages 15–19 and 20–24 years, respectively.1 With a fertility rate of 121 per 1,000 among adolescents aged 15–19 years, this places Nigeria as the 15th country with the highest fertility rate among this age group. This is very high when compared to that of other developing and developed countries.2 One of the factors underlying high maternal mortality rates is the low use of modern methods of family planning (FP). Only 9.7% of currently married women in Nigeria use modern methods of FP.1 This figure, however, does not reveal important age, geographical, and educational differences in Nigeria.
FP helps save lives of women and children and preserves their health by preventing untimely and unwanted pregnancies. FP reduces a woman’s exposure to the health risks of childbirth and abortion and gives women, who are often the sole caregivers, more time to care for their children and themselves. All couples and individuals have the right to responsibly decide freely on the number and spacing of their children, as well as the right to access information, education, and the means to do so. Several FP methods predate the emergence of modern birth control. Before the advent of condoms and hormone altering drugs, men and women utilized primitive methods for preventing conception. Although some of these techniques are surprisingly effective, they require diligence and careful planning. Some of these methods include abstinence, withdrawal method, rhythm method, and cervical mucus method among others.2 On the other hand, modern methods of FP refers to safe, effective, and legal methods to prevent pregnancy such as the use of pills, intra-uterine devices (IUD), injectables, use of condoms (male and female), ligation, vasectomy, etc.
North-Western and South-South Nigeria is home to about 15.3 million women of reproductive age (15–49 years). This constitutes 39.5% of all women of reproductive age in Nigeria. Of this 15.3 million, 9.1 million are from North-Western Nigeria while the other 6.2 million are from South-South Nigeria.3
This study focused on these two geopolitical zones of the country with one from the southern part of the country and the other from the north (Figure 1). Of the three geopolitical zones in the south, South-South has the worst health indices, while of the three zones in northern Nigeria, North-Western has the worst health indices.4 Nigeria remains one of the countries with the lowest contraceptive prevalence rates despite efforts by the government and partners. Although awareness of methods of modern FP is as high as 70%, this has not translated into usage. A key factor for this is the low contribution of health workers to providing information.5–7 Studies have shown that the main sources of information about contraception in Nigeria are friends or siblings, media, formal education, and health workers.6–9 Other factors inhibiting the use of modern methods of FP that have been highlighted include fear of side effects, objection from partners, conflict with religious beliefs, objections from family members, not thinking about using contraceptives, and unplanned early sexual debut.5–7
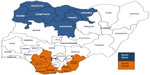  | Figure 1 Map of Nigeria showing the 36 states and North-Western and South-South geopolitical zones of the country. |
Caldwell et al reported that unmarried women in Ibadan, south-west Nigeria, were twice more likely to practice contraception as married women, despite the refusal of hospitals and FP clinics at that time to provide services for single sexually active unmarried females.10 The majority of those practicing contraception wished to prevent premarital pregnancy, which they linked to the desire for continued education or getting a job in the modern sector of the economy.11 In an analysis of the early data sets of the Demographic and Health Surveys in west Africa, Caldwell et al found that levels of contraceptive practice were much higher among never married than among currently married women in Nigeria and Cameroon, and almost as high as in Ghana.10 This pattern of contraceptive usage has a major implication for Africa’s fertility transition. A greater part of the decline would be accounted for by young women under the age of 25 years, a situation that is different from what is obtainable in Asia and Europe, where fertility declines are usually nonexistent or very limited below the age of 25 years.
Considering the prevailing pattern and low usage of modern contraceptive methods in Nigeria, it is imperative to analyze the trend, level, and geographical variation of use of modern FP methods in the country. This will enable hidden demographic processes that enhance usage to be established. Most health indicators in Nigeria have been found to vary substantially according to geographical location.4,12
Objectives of the study
The objectives of the study are: 1) to examine contraceptive use over time to establish whether there has been improvement in the use of modern contraceptives over time in the selected study location; 2) to examine whether there has been a shift in the use of contraceptives over time; and 3) to examine if there are significant differences in the use of modern contraceptives related to demographic characteristics.
Methods
Data for the study was sourced from the National and State Specific HIV and AIDS, Reproductive and Child Health Survey – NARHS/SARHS. NARHS is a population based study aimed at assessing and monitoring levels of, and trends in, various indicators of reproductive health issues in Nigeria. Three waves of NARHS have been conducted: 2003, 2005, and 2007 each with a sample size of 9,250 (250 respondents per state). The need for state level analysis led to the conduct of SARHS in 2011 with a sample size of 960 per state conducted in 18 Nigerian states (Akwa Ibom, Bauchi, Benue, Cross River, Delta, Edo, Jigawa, Kaduna, Kano, Katsina, Kebbi, Lagos, Nasarawa, Ogun, Oyo, Rivers, Sokoto, and Zamfara) using the same methodology. Data were weighted to accommodate differences in population size. Ethical approvals were sought and obtained from the Nigerian Institute of Medical Research, one of the Institutional Review Boards in Nigeria. A consent form was administered to the respondent before each interview was conducted.
Eligible respondents for these surveys were women aged 15–49 years and men aged 15–64 years. Selection is through a stratified probability sampling technique based on locality. Individual respondents were selected within households in various enumeration areas across the country. Enumeration area is a small area in a community composed of one or more neighboring blocks. In Nigeria, Enumeration Areas (EAs) were created by the National Population Commission for the 2006 Census.3 EAs are the basic units for enumeration. Within a state, all eligible persons, irrespective of their place of residence (rural or urban), were given an equal chance of being included in the final sample. Using an appropriate formula that allows for comparison between the baseline and subsequent follow-up studies, sample sizes were calculated based on a 5% level of significance and 80% power of the test. Questionnaires were pretested and administered by trained interviewers under the supervision of seasoned researchers.
Data
The database was created from the four waves of the study (NARHS 2003, 2005, and 2007, and SARHS 2011). In total, the database consists of responses from 20,938 respondents.
Analysis
Data was entered and cleaned using Census and Survey Processing System (CsPro) software (available from: http://www.census.gov/population/international/software/cspro/). Analysis was done using SPSS version 20 (IBM, Armonk, NY, USA). Chi square-test was used to test the significance of relationship between selected demographic variables and use of modern contraceptives. Binary logistic regression was used to determine factors that predict use of different contraceptives.
Variables in the analysis
Dependent variable
Modern method of FP is the dependent variable in this study. The variable is coded 1 if a modern method of FP is used and 0 if not.
Independent variables
Independent variables used in the study include: 1) age of the respondents; 2) place (locality of residence); 3) educational attainment; 4) geographical zones; 5) marital status; and 6) year of study.
For the age of respondents, the current age of the respondent was measured in years, and this ranged between 15 and 49 years. Age was included as a categorical variable in all models and subdivided into 15–19, 20–24, 25–29, 30–39, and 40–49 years. In the multivariate analysis, age was recategorized with age 15–24 years coded as 1 and age 25 years and above coded as 0 (referent group).
For place (locality) of residence, the place of residence was measured based on whether the respondent resided in an urban or rural area at the time of the survey. This was coded as 1 if the respondent resided in an urban area and 0 if the respondent resided in a rural area.
Two dummy variables were created for educational attainment: attained at least a secondary school education or not. Attained at least a secondary school education is coded 1 and not coded 0. The second dummy created is never attended a formal school or have some level of formal education with some level of formal education coded 1 and never attended formal school coded 0 (referent group).
Two geographical zones (South-South and North-Western) were used in this study with South-South coded 1 and North-Western coded 0 (referent group).
Marital status was grouped into three categorical variables: married or cohabitating, formally married (divorced, separated, or widowed), and never married. In the multivariate analysis married or cohabitating and formally married were grouped and coded 1 while never married was coded 0 (referent group). Years 2003, 2005, 2007, and 2011 were used in this study. The year 2011 was coded 1 while pre 2010 was coded 0 (referent group) in the multivariate analysis.
Results
Demographic characteristics of respondents
In the four waves of the study, almost one quarter of the respondents were age 30–39 years; 71.7% were either married or cohabitating while just 7.9% were formally married. Almost half of the respondents never attended school in 2003. This dropped to 31.6% in 2005 and increased to 35% in 2011. Of those who attended school, most had secondary school education (27.8%) while just 5.2% had higher education. Details are in Table 1.
  | Table 1 Demographic characteristics of respondents by year of study |
Use of modern methods of FP 2003 to 2011
Use of modern methods of FP increased from 7.0% in 2003 to 10.2% in 2011. Analysis by modern methods of family planning showed that the use of a condom contributes about 59% to the overall figure of use of modern methods of FP. This is followed by injectables (18.0%) and use of daily pills (14.6%). The most unpopular methods are vaginal foaming tablets and permanent methods (<0.001%). Just 0.3% of the study population used long lasting methods such as IUD and implants for FP. As at 2003, the proportion was 0.3% but dropped to 0.1% in 2011 (Table 2).
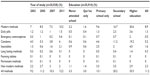  | Table 2 Contraceptive use by year of study and educational attainment |
Use of modern methods of FP and education
Overall, the use of modern methods of FP increased with the respondent’s level of education. It was lowest among those with Qur’nic education (1.6%) and highest among those with higher levels of education (30.6%). All the modern methods of FP follow the same trend (higher proportion as educational level increases). Increase in condom use was observed at over 6% as education level increased by one level. Details are in Table 2.
Use of modern methods of FP by age
The use of modern methods of FP increased with age and peaked at 25–29 years (Table 3). Use of modern methods of FP was lowest among those aged 15–19 years (5.5%). Different age groups appeared to prefer different methods. Use of daily pills was higher among respondents aged 30–39 years while use of emergency contraceptives was higher among those aged 25–29 years. Use of condoms was higher among persons aged 20–24 years, injectables higher among persons 30–39 years, while long lasting methods such as IUD and implants was higher among persons aged 40–49 years.
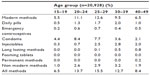  | Table 3 Contraceptive use by age categories |
Use of modern method methods of FP by locality, marital status, and zones
While among urban residents the use of modern methods of FP was as high as 14.2%, among rural residents it was just 7.1%. Use of modern methods of FP is higher among the never married (15.0%) followed by those who are either married or cohabitating (7.2%), and lowest among the formerly married (5.4%). There appears to be a very wide difference in use of modern methods of FP between the South-South (18.1%) and the North-Western zones (3.5%). Details are in Table 4.
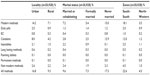  | Table 4 Contraceptive use by locality, marital status, and geographical zones |
Test of significance (chi-squared test and odds ratio [OR])
At 5% level of significance, year of study (P<0.0001), educational attainment (P<0.0001), age (P<0.0001), locality (urban and rural) (P<0.0001), marital status (P<0.0001), and geographical zones (P<0.0001) are significant variables that determined the use of modern methods of FP (Table 5). There is a strong positive correlation between use of modern contraceptives and year of study, education, and locality.
  | Table 5 Logistic regression table |
Multivariate analysis was conducted using logistic regression in an attempt to establish the strength of the relationship. Women with at least a secondary education were found to be almost three times more likely to use a modern FP method (P<0.0001, OR: 2.4; 95% confidence interval [CI]: 2.099 and 2.740). Women in the South-South geopolitical zone were three times more likely to use a modern FP method compared with those in the North-Western zone (P<0.001; OR: 3.2; 95% CI: 2.817 and 3.626). Of those in urban locations, women who were never married and women in 2011 were almost twice more likely to use a modern FP method. It is important to also note that women aged 15–24 years are less likely to use a modern FP method. While the never married and women with at least a primary education were 2.5 and 2.6 times more likely to use condoms for FP, women in South-South were 5.2 times more likely to use a condom compared with women in North-Western Nigeria. At 5% level of significance, never married and geographical zones were not significant determinants of the use of daily pills for FP. Education was found not to be a significant determinant of the use of injectables for FP.
Discussion
This study attempted to look at the patterns and trend in use of contraceptives in Nigeria from 2003 to 2011. The data analyzed suggests that the use of modern FP methods has increased over the study period from 7.0% to 10.2% (average annual increase of less than 0.5%). With the current average annual increase of less than 0.5%, more concerted efforts will be needed if the target of achieving universal access to reproductive health (Millennium Development Goal 5b) is to be achieved.14
Analysis by type of modern method shows that the use of short term methods of FP (daily pills, emergency contraceptives, condoms, and injectables) increased over the study period while the use of long lasting methods (implant and IUD) was constant and rare (<1%). Compliance with appointments and use remains a major challenge with the use of short term methods of FP.15,16 It is with this recognition that long lasting methods are currently being promoted in Uganda and some other countries. Considering the low and the constant proportion of women using long lasting methods in these zones, efforts are needed to scale up their use. Male or female sterilization is most suitable for those who do not want any more children or any at all. Vasectomy keeps sperm cells out of a man’s semen while tubal ligation cuts or blocks a woman’s fallopian tubes so her egg cells stay apart from any sperm. Numbers for the use of both methods dropped within the study period. This may be associated with the irreversibility of these methods. Further education and research on this is required.
From the results of the analysis, the use of condoms accounts for almost 60% of all users of modern methods of FP. Considering this preference for condoms, a considerable opportunity exists for scaling up the use of modern methods of FP as condom use in marital and cohabitating sexual relations is still very low. As reported in NARHS 2007, some of the reasons for preference for condoms include that the condom has less side effects, and that it is easy and convenient to use. It should be pointed out that condoms have relatively high failure rates compared to other modern methods, possibly due to breakage as a result of storage, opening of the condom, and wearing of the condom.
The results of this study suggest a positive association between the use of modern FP methods and education, implying that the higher an individual’s education is, the higher their probability of using a modern method of FP. This corroborates the result in earlier work by Adebayo et al.17 Creative intervention approaches should be identified targeting the uneducated and less educated women to introduce and promote the use of modern FP methods.
It should be noted that the use of traditional methods of FP also increases with education from 1.1% to 3.5%. This may suggest that women are beginning to appreciate the benefits of FP. It is however important to note that the increase in the proportion of women using non modern methods is a possible opening for scaling up use of modern methods of FP in Nigeria.
Analysis by age shows that uptake of FP is highest among women aged 25–29 years for all methods. This result is different from the result in a similar study in Tanzania and Ghana where contraceptive use was found to be highest among women aged 35 years and above.18 The association between age groups and use of modern methods of FP was significant suggesting that the age of women contributes to predicting the trend and use of modern FP methods.
Different age groups seemed to prefer different modern methods of FP. Use of condoms was higher among women aged 20–24 followed by 25–29 years, and lowest among women aged 40–49 years. While the use of condoms decreases with age, the use of daily pills and injectables increased with age up to age 40 years and above where there was a shift to more long lasting methods.
A higher proportion of women in urban locations used modern methods of FP compared with those in rural locations. Similar results were found in Zambia where urban residents are almost two times more likely to use a modern method of FP. This may be connected with education as educational level is higher among urban residents than rural. With rural locations in Nigeria having higher fertility rates, targeting women in rural locations with targeted reproductive health interventions may contribute to increasing the contraceptive prevalence rate in Nigeria.
In terms of marital status, use of a modern FP method was highest among the never married followed by the married or cohabitating, and lowest among those who were formally married. This may be explained by the fact that most women who were formally married (widowed, separated, or divorced) already have children. Being formally married has its own labeling within most African communities. Sexual activities are likely to be on the low side coupled with the fact that most women already have children they are struggling to care for.
The never married sexually active women recorded higher use of emergency contraceptives and condoms. This trend suggests that married persons prefer more “stable” long lasting FP methods whereas unmarried people tend to be inclined towards those methods you use immediately before or after sex, such as condoms, emergency contraceptives etc. This may not be unconnected with the fact that most African societies expect the never married to abstain from sex. As noted earlier, such short term methods have their limitations in terms of compliance. All females, irrespective of their marital status, should have access to a FP method of their choice.
Huge zonal disparity exists between the North-Western and South-South. It is important to note that there are a larger number of educated persons in the South-South than in North-Western Nigeria. Cultural and religious tolerance also tends to be more in the South-South than in the North-West. These are possible reasons for the huge difference.
As in most other behavioral and cross-sectional surveys, these data are based on self-reported sexual practices, and may suffer from the problem of underreporting of behaviors among the respondents. The study is limited to analysis of trend in contraceptive use in selected states in Nigeria between 2003 and 2011. Patterns of use were limited to preferred choices of FP methods by demographic characteristics.
Despite the religious and cultural barriers associated with condoms, it is still the most preferred method of FP. Considering that the use of condoms offers dual protection, scaling up the use of condoms as an FP option, especially among the never married, may contribute to reducing unmet FP needs among this group.
Use of modern methods of FP in North-Western Nigeria is lower than the national average (9.7%). There is a very wide difference between both groups. Considering the lower health indices in this zone of the country (higher infant mortality rate, higher maternal mortality rate, lower life expectancy, etc1) promotion of modern FP methods may be useful. Targeting young ones in school or out of school with FP messages may increase awareness and possible demand for FP services when they are ready for FP services.
Educational attainment appears to have a positive correlation with the use of modern FP methods. It is important to promote female child education. Early marriage also needs to be addressed as it reduces the chances of females getting the education required for making informed decision about the use of FP services.
Acknowledgments
We thank the Federal Ministry of Health, Nigeria for granting permission to use NARHS data. We are also grateful to all authors whose works were referenced in this study.
Disclosure
The authors have no conflicts of interest in this study.
References
National Population Commission and ICF Macro. (2009) Nigeria Demographic and Health Survey 2008. Nigeria: National Population Commission and ICF Macro; 2009. Available from: http://nigeria.unfpa.org/pdf/nigeriadhs2008.pdf. Accessed June 19, 2014. | |
Adolescent fertility rate (births per 1,000 women ages 15–19) [webpage on the Internet]. Washington: The World Bank Group; 2014. Available from: http://data.worldbank.org/indicator/SP.ADO.TFRT. Accessed January 13, 2014. | |
NPC (2006) Nigeria National Population Census 2006. National Population Commission, Abuja, Nigeria. Available from: http://population.gov.ng/index.php/publications/list-of-publications. Accessed July 15, 2014. | |
Otoide VO, Oronsaye F, Okonofua FE. Why Nigerian adolescents seek abortion rather than contraceptives: evidence from focus group discussions. International Family Planning Perspective. 2001;27(2):77–81. | |
Abiodun OM, Balogun OR. Sexual activity and contraceptive use among young female students of tertiary educational institution in Ilorin, Nigeria. Contraception. 2009;79:146–149. | |
Monjok E, Smesny A, Ekabua JE, Essien EJ. Contraceptive practices in Nigeria: literature review and recommendation for future policy decisions. Open Access Journal of Contraception. 2010;1:9–22. | |
Okpani AOU, Okpani JU. Sexual activity and contraceptive use among female adolescent: a report from Port Harcourt. Afr J Reprod Health. 2000;4:40–47. | |
Ankomah A, Anyanti JZ, Oladosu M. Myths, misinformation and communication about family planning and contraceptive use in Nigeria. Open Access Journal of Contraception. 2011;2:95–105. | |
Caldwell JC, Orubuloye IO, Caldwell P. Fertility decline in Africa: a new type of transition? Population and Developmental Review. 1992;18(2):211–242. | |
Caldwell JC, Caldwell P. (2002). The fertility transition in sub-Saharan Africa. In: Fertility and the Current South Africa Issues of Poverty, HIV/AIDS and Youth; 2002; Pretoria, South Africa. | |
Federal Ministry of Health. National HIV/AIDS and Reproductive Health Survey, 2007. Nigeria: Federal Ministry of Health; 2008. Available from: http://www.nepwhan.net/assets/NigeriaNARHSPlus2007.pdf. Accessed June 19, 2014. | |
National Population Commission and ICF Macro. Nigeria Demographic and Health Survey 2008. Nigeria: National Population Commission and ICF Macro; 2009. Available from: http://dhsprogram.com/pubs/pdf/FR222/FR222.pdf. Accessed June 19, 2014. | |
United States Census [webpage on Internet]. International Programs. Census and Survey Processing System (CSPro). Available from: http://www.census.gov/population/international/software/cspro/. Accessed July 15, 2014. | |
United Nations [webpage on Internet]. We can End Poverty. Millennium Development Goal and Beyond 2015. Available from: http://www.un.org/millenniumgoals/maternal.shtml. Accessed July 15, 2014. | |
Kulas M. Analytical methods of family planning [webpage on the Internet]. Santa Monica: Livestrong.com [updated January 28, 2014] Available from: http://www.livestrong.com/article/205455-methods-for-family-planning/#ixzz2VcHR1uDk. Accessed June 19, 2014. | |
Adebayo SB, Gayawan E, Ujuju C, Ankomah A. Modelling geographical variations and determinants of use of modern family planning methods among women of reproductive age in Nigeria. J Biosoc Sci. 2013;45(1):57–77. | |
Tengia-Kessy A, Rwabudongo N. Utilization of modern family planning methods among women of reproductive age in a rural setting: the case of Shinyanga rural district, Tanzania. East Afr J Public Health. 2006;3(2):26–30. | |
White JS, Speizer IS. Can family planning outreach bridge the urban-rural divide in Zambia? BMC Health Serv Res. 2007;7:143. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
