Back to Journals » Clinical Ophthalmology » Volume 13
Straylight As The Result Of Refractive Correction
Authors Gaurisankar ZS , van Rijn GA , Luyten GPM , van den Berg TJTP
Received 27 July 2019
Accepted for publication 16 September 2019
Published 12 November 2019 Volume 2019:13 Pages 2195—2201
DOI https://doi.org/10.2147/OPTH.S224970
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Zoraida S Gaurisankar,1 Gwyneth A van Rijn,1 Gregorius PM Luyten,1 Thomas JTP van den Berg2
1Department of Ophthalmology, Leiden University Medical Center, Leiden, the Netherlands; 2Institute for Neuroscience, Royal Netherlands Academy of Arts and Sciences, Amsterdam, the Netherlands
Correspondence: Zoraida S Gaurisankar
Department of Ophthalmology, LUMC, Albinusdreef 2, 2333 ZA, Leiden, the Netherlands
Tel +31 71 526 9111
Fax +31 71 526 6576
Email [email protected]
Purpose: To investigate the effect of refractive correction on straylight.
Patients and methods: Straylight values were measured with the C-Quant (Oculus Optikgeräte, GmbH, Wetzlar, Germany) in 1) near-emmetropic eyes (n=30) with various negative powered refractive lenses and in 2) myopic eyes (n=30) corrected with prescribed eyeglasses and contact lenses. The straylight measurements in each group were compared in the different conditions.
Results: In the near-emmetropic group, a significant effect (p<0.001) of each added negative diopter was found to increase straylight values with 0.006 log-units. In the second group, no significant correlation with type of correcting lens was found on straylight values.
Conclusion: Refractive correction with high minus power (contact) lenses result in subtle increase of straylight values. These changes are relatively small and do not lead to visual disability in a clinical setting.
Keywords: straylight, contact lenses, eyeglasses, glare, light scatter, refractive error
Introduction
The prevalence of refractive errors, in particular myopia, is increasing worldwide.1–4 Patients with (high) refractive errors, who have inadequate vision with spectacles and are contact lens intolerant, may choose for refractive correction by laser surgery or intraocular lens (IOL) implantation. But correction of refractive errors, even when leading to excellent visual acuity, may, however, not necessarily lead to complete patient satisfaction if vision is tinged by troublesome glare. Since the beginning of the twentieth century, it is known that straylight has great effect on the quality of vision.5–7 The International committee on illumination (CIE) has defined disability glare as “the effect of straylight in the eye whereby visibility and visual performance are reduced.”7
Straylight is the result of forward intraocular light scatter on the retina. For each beam of light that reaches the eye, the light is scattered to some extent by imperfections of optical media, before it reaches the retina.5,8,9 In every eye, this mechanism is responsible for an amount of straylight in the presence of a (bright) light source. Normal values of straylight will induce limited visual disability effects, but an increase in straylight can lead to symptoms that affect the quality of vision seriously. These symptoms include halos and loss of contrast, but also blurred vision, decreased color vision, and difficulty in face recognition.5
Many clinical studies have evaluated the pre- and post-operative effect on straylight after refractive surgery. The results were consistent: post-operative straylight values in myopes after laser-assisted in situ keratomileusis (LASIK)/ laser-assisted epithelial keratomileusis (LASEK)10–14 or after phakic intraocular lens (pIOL) implantation15,16 were on average slightly lower than pre-operative straylight measurements. Assumptions were made that these improvements are the result of ill-tolerated contact lenses pre-operatively.13,15,16 Another factor that might have played a role in these findings is the effect of change in retinal image size due to correction of the refractive error. For example, after pIOL implantation in high myopic eyes, visual acuity may increase 1 or more lines due to image magnification effects.15,17,18 Labuz et al19 demonstrated differences in elevated straylight as the result of multifocal contact lens wearers. Van der Meulen et al20 showed increased straylight during rigid contact lens wear, possibly as a result of deposits on the contact lens, but the degree of refractive error was not taken into account.
The effect of different degrees of refractive correction on retinal straylight, with its concomitant effect on retinal image size, has not yet been investigated and remains unclear. We therefore want to examine if different refractive corrections, resulting in different retinal image sizes, have an effect on straylight values.
Materials And Methods
Subjects
This study involves two study groups with an age range of 18–35 years: 1) a near-emmetropic group (n=30 eyes of 15 subjects), defined as having a spherical refractive error between −1.00 and +1.00 dioptres (D) and a cylindrical refractive error not exceeding −2.00 D. 2) A myopic group (n=30 eyes of 15 subjects) with a spherical refractive error of at least −6.00 D and a cylindrical refractive error not exceeding −2.00 D. Subjects with a history of ocular pathology, cataract, corneal opacities, visual acuity of <0.2 Snellen or epilepsy, were excluded. The participants were recruited and assessed at the Leiden University Medical Center (LUMC) in the Netherlands between May 2013 and October 2014. The study was conducted in accordance with the Declaration of Helsinki and approved by the medical ethical committee of the LUMC. All participants provided written informed consent.
Straylight Measurements
Straylight values were measured using the compensation comparison-based Oculus C-Quant (Oculus Optikgeräte, GmbH, Wetzlar, Germany). This method for assessing straylight has been described in detail in the literature and has been thoroughly validated.6,17,18,21,22 The amount of straylight is quantified by means of the straylight parameter s, given logarithmically as log(s). All measurements were performed in identical light conditions. The test was repeated to obtain 2 reliable measurements for each condition. The mean of the 2 measurements was used for analysis. The reliability outputs of the measurement were chosen as follows: an estimated standard deviation of ≤0.08 and a shape factor Q of ≥0.5.17,21
Study Design
For each study group, we used a different approach to change refractive correction. In the first group, 1) the near-emmetropic group, straylight values were measured under 5 conditions: with a trial lens (provided by the manufacturer of the C-Quant) with a spherical power of (a) −14.00 D, (b) −10.00 D, (c) −6.00 D, (d) −4.00 D and (e) without any correction. Right and left eye were tested alternately. Between every measurement a pause of 30 s was given. Relative magnification of the different retinal image sizes was calculated with the standard spectacle magnification formula (1) for values for spectacle magnification.23
(1)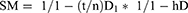
Where: SM = Spectacle magnification; t = thickness of the lens in meters; n = refractive index of the lens material; D1 = the base curve or front surface power of the lens in diopters; h = the vertex distance +3 mm, converted to meters; and D = actual power of the lens in diopters.
In the second group, 2) the myopic group, straylight values were measured under 3 conditions: with correction by (a) trial lens, (b) spectacles and (c) contact lens. The same standard formula (1) was used to determine the image magnification resulting from different vertex distance a under the various test conditions: (a) a=0.026 m (trial lenses), (b) a=0.016 m (spectacles) and (c) a=0.003 m (contact lenses). In Figure 1, the lens magnification factor is plotted as a function of different refractive lens powers. Prior to straylight measurements, autorefraction (Topcon KR 8900 Ref, Tokyo, Japan), corneal topography (Oculus Pentacam HR, Wetzlar, Germany), axial length (Lenstar LS 900 Haag-Streit, Koeniz, Switzerland) and slitlamp examination were performed. Best-corrected visual acuity (BCVA), own-spectacle-corrected visual acuity and contact-lens-corrected visual acuity (if applicable) were determined by ETDRS assessment (logMAR units). Trial lenses and prescribed spectacles were thoroughly cleaned before examination and new contact lenses were used. Only non-tinted spectacles with no macroscopic scratches and refractive index of 1.67 were used. In case spectacles were worn, a vertex distance of 16 mm was maintained.
Statistical Analysis
Statistical analysis was performed using SPSS statistics software version 23 (IBM). Descriptive statistics, including means, standard deviations, proportions, and frequency distributions, were generated for subject characteristics. Bland–Altman analysis was performed and 95% limits of agreement (LoA) were estimated by mean difference±1.95×standard deviation (SD) of the difference. Data are expressed as the mean±SD. The normality of data was checked with the Kolmogorov–Smirnov test. Means, standard deviations and boxplots were used to visualize the data. A linear mixed model with random intercept was used to examine the relationship between straylight values and the different test conditions. We chose this statistical model in order to deal with the potential correlation of repeated measures of right and left eye. The correlation between straylight and the various test conditions was tested with a linear as well as a quadratic function. Our primary variable and all the possible variables were implemented in a model. We compared all the possible combinations by removing the variables with the highest p-value >0.05 once at a time to create the best fit model (backward selection). In addition, each variable was tested individually in separate models on having an effect on straylight measurements. The model with the minimum value for Akaike’s information criterion (AIC) was identified as the optimal model for the specific outcome measure. To evaluate the normal distribution of the final models, residual scatter plots and histograms were used. Statistical significance was defined as a p-value of less than 0.05.
Power calculations were made to determine the sample size. A significance level (adjusted for sidedness) of 0.025, a power of 90% and a standard deviation of the difference of 0.1 provided a minimum sample size of 13 patients for each group to satisfy valid conclusions. We included 15 patients in each group to meet the required sample size, allowing for dropouts.
Results
Characteristics Of The Participants
The characteristics of the study groups are shown in Table 1.
 |
Table 1 Characteristics Of The Near-Emmetropic (A) And Myopic Study Group (B) |
Straylight Results
The repeatability of the straylight measurements was very good in both groups and comparable with previous reports,17,18,22,24 with repeated measures standard deviations of 0.068 and 0.056 log-units for the near-emmetropic and myopic groups, respectively, also shown in Bland–Altman plots (Figure 2).
The measured straylight values are shown in Table 2 and with boxplot analysis (Figure 3). The mean baseline straylight value of the near-emmetropic group (measurements without trial lens, therefore no altering of retinal image size) is 0.91 log-units. In the myopic group, the mean baseline straylight value (measurements with contact lens, therefore minimal altering of retinal image size) is 0.97 log-units. Comparison of baseline straylight values between the near-emmetropic and myopic group shows no significant difference (Mann–Whitney significance 0.133/Independent sample T-test p=0.062).
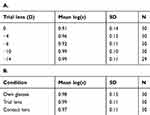 |
Table 2 Measured Straylight Values At Different Conditions Of Retinal Image Size For The Near-Emmetropic (A) And Myopic (B) Eyes |
1) In the near-emmetropic group the refractive correction, with its concomitant image size altering effect, had a significant effect (p<0.001) on the log(s) straylight value. None of the other parameters tested (eye, age, SE and iris pigmentation) had significant effect on straylight. For more details see Table 3A.
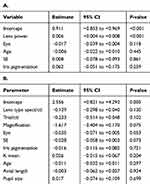 |
Table 3 Associations Of Mean Straylight Values And Possible Predictor Variables Generated By Linear Mixed Models In The Near-Emmetropic Study Group (A) And The Myopic Study Group (B) |
2) In the myopic group the different refractive corrections had no significant effect on retinal straylight values (p=0.150). There was no significant difference between the different test conditions, ie, trial lenses, soft contact lenses and spectacles. None of the other parameters (eye, age, SE, keratometry, iris pigmentation, AL, pupil size) had significant effect on straylight. For more details see Table 3B.
 |
Figure 3 Boxplot of the straylight values measured by C-Quant in log-units (log(s)) for the 30 near-emmetropic eyes (white) and the 30 myopic eyes (gray) under the different test conditions. |
Discussion
The main conclusion is that the effects of glasses and soft contact lenses, including the degree of refractive error it corrects, on straylight are modest and all the measurements were below 1.47 log(s) which is the threshold for serious hindrance. In the first (near-emmetropic) group, a significant effect was found of the different powers of lenses, which must partly be attributed to the known effects of scatter angle (image size), but our hypothesis is that accommodation might also play a role in this finding. During accommodation the crystalline lens takes on a more spherical shape, and lens thickness increases with 0.045 mm for every diopter of added accommodation stimulus.24
To our knowledge, we are the first to describe the effects of glasses on straylight. The effect of contact lenses on straylight, however, has been described by van der Meulen et al.20 They demonstrated straylight values of 0.934 log(s) during soft contact lens wear in a study population with normal eyes, comparable to 0.938 log(s) after removal of the lens. The straylight values of our myopic study population are slightly higher, probably due to the refractive power of the lens. Rigid contact lenses20 and multifocal contact lenses19 have also shown some slightly elevated straylight values, possibly as the result of other underlying mechanisms, such as deposits on the contact lens or diffractive effects, respectively. Therefore, these results cannot be compared with our findings, as we only used soft contact lenses in our study.
Although some studies have shown that age and iris pigmentation9,17,18,25–28 can have significant effect on straylight values, in the present study, age, iris pigmentation, and all the other tested parameters were not significant. Probably, the fact that age is not significant in our study population is caused by a selection effect because we only selected subjects between 18 and 35 years of age. May be the pigmentation spread was not sufficient either in our small cohort.
What might explain the differences between the near-emmetropic and myopic study group? The first thing we should consider is the accommodation effect as described earlier. Second, a possible effect of the contact lenses used in the study as myopic participants’ own contact lenses were used for visual correction and contact lenses have previously been shown to influence straylight values.20,29,30
Another factor that may be considered is that data of the near-emmetropic eyes group may have resulted in better statistical power due to more straylight measurements and greater range of magnification factor. However, if we exclude the data generated by test conditions with trial lenses of powers −14 D and −4 D, resulting in a similar number of observations as in the myopic group, a clearly statistic significant effect remained (p<0.001).
Conclusions
The effect of the degree and the method of correction, including eyeglasses and soft contact lenses, of refractive correction on straylight are modest and clinically irrelevant. The small effects found, might partly be attributed to known effects of scatter angle (image size), but accommodation might also play a role in this finding. Further, in-depth studies in this issue need to be pursued.
Acknowledgments
Our appreciation goes out to Dr R. Wolterbeek (Leiden University Medical Center, the Netherlands) and Dr R. Holman (VU Amsterdam, the Netherlands) for help with the statistical analysis. Also to Dr E.A. Hermans (VU Amsterdam, the Netherlands) for sharing his knowledge on accommodation, and Theo Blom for his help with spectacle magnification effects.
Disclosure
Dr van den Berg developed the method to assess straylight. This is licensed by the Royal Academy to Oculus for the C-Quant instrument. Dr van Rijn was supported by Opthec b.v., Stichting Blindenhulp, and by the ANVVB and LSBS foundations through UitZicht. The funding organisations provided unrestricted grants and had no role in the design or conduct of this research. The authors report no other conflicts of interest in this work.
References
1. Holden BA, Fricke TR, Wilson DA, et al. Global prevalence of myopia and high myopia and temporal trends from 2000 through 2050. Ophthalmology. 2016;123(5):1036–1042. doi:10.1016/j.ophtha.2016.01.006
2. Jones D, Luensmann D. The prevalence and impact of high myopia. Eye Contact Lens. 2012;38(3):188–196. doi:10.1097/ICL.0b013e31824ccbc3
3. Kempen JH, Mitchell P, Lee KE, et al. The prevalence of refractive errors among adults in the United States, Western Europe, and Australia. Arch Ophthalmol. 2004;122(4):495–505.
4. Vitale S, Sperduto RD, Ferris FL
5. van den Berg TJ. Importance of pathological intraocular light scatter for visual disability. Doc Ophthalmol. 1986;61(3–4):327–333. doi:10.1007/BF00142360
6. van den Berg TJ, Franssen L, Kruijt B, Coppens JE. History of ocular straylight measurement: A review. Z Med Phys. 2013;23(1):6–20. doi:10.1016/j.zemedi.2012.10.009
7. Vos JJ. Disability Glare: A State of the Art Report. CIE Journal. 1984;3:39–53.
8. Thomson D. The assessment of vision. In: James B, Benjamin L. Ophthalmology: Investigative Techniques and Ocular Investigation. Oxford: Butterworth-Heinemann; 2006:2–5.
9. IJspeert JK, de Waard PWT, van den Berg TJ, de Jong PT. The intraocular straylight function in 129 healthy volunteers; dependence on angle, age and pigmentation. Vision Res. 1990;30(5):699–707. doi:10.1016/0042-6989(90)90096-4
10. Jin Y, Wang Y, Xu L, et al. Comparison of the optical quality between small incision lenticule extraction and femtosecond laser LASIK. J Ophthalmol. 2016;2016:2507973. doi:10.1155/2016/2507973
11. Lapid-Gortzak R, van der Linden JW, van der Meulen I, Nieuwendaal C, van den Berg T. Straylight measurements in laser in situ keratomileusis and laser-assisted subepithelial keratectomy for myopia. J Cataract Refract Surg. 2010;36(3):465–471. doi:10.1016/j.jcrs.2009.10.029
12. Rozema JJ, Coeckelbergh T, Van den Berg TJ, et al. Straylight before and after LASEK in myopia: changes in retinal straylight. Invest Ophthalmol Vis Sci. 2010;51(5):2800–2804. doi:10.1167/iovs.09-4679
13. Rozema JJ, Trau R, Verbruggen KH, Tassignon MJ. Backscattered light from the cornea before and after laser-assisted subepithelial keratectomy for myopia. J Cataract Refract Surg. 2011;37(9):1648–1654. doi:10.1016/j.jcrs.2011.03.043
14. Xu L, Wang Y, Li J, et al. Comparison of forward light scatter changes between SMILE, femtosecond laser-assisted LASIK, and Epipolis LASIK: results of a 1-year prospective study. J Refract Surg. 2015;31(11):752–758. doi:10.3928/1081597X-20151021-04
15. Garcia M, Gonzalez C, Pascual I, Fimia A. Magnification and visual acuity in highly myopic phakic eyes corrected with an anterior chamber intraocular lens versus by other methods. J Cataract Refract Surg. 1996;22(10):1416–1422. doi:10.1016/S0886-3350(96)80140-4
16. Paarlberg JC, Doors M, Webers CA, Berendschot TT, van den Berg TJ, Nuijts RM. The effect of iris-fixated foldable phakic intraocular lenses on retinal straylight. Am J Ophthalmol. 2011;152(6):969–975.e962. doi:10.1016/j.ajo.2011.05.024
17. Coppens JE, Franssen L, van Rijn LJ, van den Berg TJ. Reliability of the compensation comparison stray-light measurement method. J Biomed Opt. 2006;11(3):34027. doi:10.1117/1.2209555
18. Franssen L, Coppens JE, van den Berg TJ. Compensation comparison method for assessment of retinal straylight. Invest Ophthalmol Vis Sci. 2006;47(2):768–776. doi:10.1167/iovs.05-0690
19. Labuz G, Lopez-Gil N, van den Berg TJ, Vargas-Martin F. Ocular straylight with different multifocal contact lenses. Optom Vis Sci. 2017;94(4):496–504. doi:10.1097/OPX.0000000000001043
20. van der Meulen IJ, Engelbrecht LA, van Vliet JM, et al. Straylight measurements in contact lens wear. Cornea. 2010;29(5):516–522. doi:10.1097/ICO.0b013e3181c11e29
21. Guber I, Bachmann LM, Guber J, Bochmann F, Lange AP, Thiel MA. Reproducibility of straylight measurement by C-Quant for assessment of retinal straylight using the compensation comparison method. Graefes Arch Clin Exp Ophthalmol. 2011;249(9):1367–1371. doi:10.1007/s00417-011-1704-y
22. Montenegro GA, Michael R, van den Berg TJ. Variation of straylight between contra lateral eyes - results from 1017 healthy subjects. Acta Ophthalmol (Copenh). 2012;90(4):e332–e333. doi:10.1111/j.1755-3768.2011.02252.x
23. Stoner EDPP. Optical Formulas Tutorial.
24. Cervino A, Montes-Mico R, Hosking SL. Performance of the compensation comparison method for retinal straylight measurement: effect of patient’s age on repeatability. Br J Ophthalmol. 2008;92(6):788–791. doi:10.1136/bjo.2007.131078
25. Gholami S, Reus NJ, van den Berg T. Changes in intraocular straylight and visual acuity with age in cataracts of different morphologies. J Ophthalmol. 2017;2017:5649532. doi:10.1155/2017/5649532
26. Rozema JJ, Van den Berg TJ, Tassignon MJ. Retinal straylight as a function of age and ocular biometry in healthy eyes. Invest Ophthalmol Vis Sci. 2010;51(5):2795–2799. doi:10.1167/iovs.09-4056
27. van den Berg TJ. Analysis of intraocular straylight, especially in relation to age. Optom Vis Sci. 1995;72(2):52–59. doi:10.1097/00006324-199502000-00003
28. Vos JJ. On the cause of disability glare and its dependence on glare angle, age and ocular pigmentation. Clin Exp Optometry. 2003;86(6):363–370. doi:10.1111/cxo.2003.86.issue-6
29. Elliott DB, Mitchell S, Whitaker D. Factors affecting light scatter in contact lens wearers. Optom Vis Sci. 1991;68(8):629–633. doi:10.1097/00006324-199108000-00009
30. Fonn D, du Toit R, Simpson TL, Vega JA, Situ P, Chalmers RL. Sympathetic swelling response of the control eye to soft lenses in the other eye. Invest Ophthalmol Vis Sci. 1999;40(13):3116–3121.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


