Back to Journals » International Journal of General Medicine » Volume 14
Social Determinants of Health Correlating with Mechanical Ventilation of COVID-19 Patients: A Multi-Center Observational Study
Authors Giovanatti A, Elassar H, Karabon P, Wunderlich-Barillas T, Halalau A
Received 19 August 2021
Accepted for publication 29 October 2021
Published 20 November 2021 Volume 2021:14 Pages 8521—8526
DOI https://doi.org/10.2147/IJGM.S334593
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Alexa Giovanatti,1 Heba Elassar,2 Patrick Karabon,3 Tracy Wunderlich-Barillas,3 Alexandra Halalau2
1Internal Medicine Department, Beaumont Health, Royal Oak, MI, USA; 2Internal Medicine Department, Oakland University William Beaumont School of Medicine, Rochester, MI, USA; 3Office of Research, Oakland University William Beaumont School of Medicine, Rochester, MI, USA
Correspondence: Alexa Giovanatti
Beaumont Health, 3601 W 13 Mile Road, Royal Oak, MI, 48073, USA
Tel +1 248-898-5000
Email [email protected]
Importance: Several studies have relayed the disproportionate impact of COVID-19 on marginalized communities; however, few have specifically examined the association between social determinants of health and mechanical ventilation (MV).
Objective: To determine which demographics impact MV rates among COVID-19 patients.
Design: This observational study included COVID-19 patient data from eight hospitals’ electronic medical records (EMR) between February 25, 2020, to December 31, 2020. Associations between demographic data and MV rates were evaluated using uni- and multivariate analyses.
Setting: Multicenter (eight hospitals), largest health system in Southeast Michigan.
Participants: Inpatients with a positive RT-PCR for SARS-CoV-2 on nasopharyngeal swab. Exclusion criteria were missing demographic data or non-permanent Michigan residents.
Exposure: Patients were divided into two groups: MV and non-MV.
Main Outcome and Measures: The primary outcome was MV rate per demographic. A multivariate model then predicted the odds of MV per demographic descriptor. Hypotheses were formulated prior to data collection.
Results: Among 11,304 COVID-19 inpatients investigated, 1621 (14.34%) were MV, and 49.96% were male with a mean age of 63.37 years (17.79). Significant social determinants for MV included Black race (40.19% MV vs 31.31% non-MV, p< 0.01), poverty (14.60% vs. 13.21%, p< 0.01), and disability (12.65% vs 9.14%; p< 0.01). Black race (AOR 1.61 (CI 1.41– 1.83; p< 0.01)), median income (AOR 0.99 (CI 0.99– 0.99; p< 0.01)), disability (AOR 1.55 (CI 1.26, 1.90; p< 0.01)), and non-English-speaking status (AOR 1.26 (CI 1.05, 1.53)) had significantly higher odds of MV.
Conclusions and Relevance: Black race, low socioeconomic status, disability, and non-English-speaking status were significant risk factors for MV from COVID-19. An urgent need remains for a pandemic response program that strategizes care for marginalized communities.
Keywords: COVID-19, disparities, mechanical ventilation, race, socioeconomic
Plain Language Summary
Social determinants of health are associated with an increased risk of COVID-19 morbidity and mortality.1–3 In this retrospective observational study, we further illustrate how low socioeconomic status, Black race, disability, and non-English-speaking status were associated with an increased rate of mechanical ventilation from COVID-19. These demographic descriptors can be used to help stratify COVID-19 risk and treatment by health-care providers in the emergency room (ER) and inpatient setting.
Introduction
Background/Rationale
The COVID-19 pandemic has illuminated the disparities within our healthcare system. Obesity, diabetes, race, and poverty have emerged as risk factors for the hospitalization of COVID-19 patients.1,2 For instance, Black and Hispanic patients are more likely to test positive for COVID-193. However, findings related to mechanical ventilation (MV) of COVID-19 patients have not been well-defined.4 Recent studies suggest race5 and poverty2 are associated with increased risk for ICU admission from COVID-19, though other studies find this correlation to be inconsistent.1 MV of COVID-19 patients is associated with a high mortality rate,6 so identifying demographic risk factors for MV will help stratify and optimize treatment for patients at risk.
Objectives
Our study aims to identify social determinants of health that predispose COVID-19 patients to MV within a multicenter Michigan hospital system.
Methods
Study Design
We conducted a retrospective observational study at the largest healthcare system (eight hospitals) in southeast Michigan from February 25, 2020, to December 31, 2020. The study was approved under expedited review by the Beaumont Health Institutional Review Board (IRB), #2020-209. Patient consent was waived as the study design was retrospective. Data confidentiality and compliance with the Declaration of Helsinki was maintained. We included all inpatients who were diagnosed with SARS-CoV2 infection by a positive RT-PCR on nasopharyngeal swab. Patients for whom any demographic data were missing or who were not permanent Michigan residents were excluded from analysis. Zip code level data from the United States Census Bureau such as rate of unemployment/use of public transportation/percentage of food stamp use were used as proxies for economic and employment status as individual-level data was not available from the electronic medical record (EMR). The zip code level data was eventually matched with the individual patient level data. Examined variables include age, ethnicity, marital status, education level, employment, zip code, primary language, disabilities, type of insurance, body mass index (BMI), and established primary care provider (PCP). Univariate and multivariate analyses were run using SAS 9.4 software to determine any MV correlates. P values of less than 0.05 were considered statistically significant.
Results
Participants
A total of 11,304 patient records were admitted with a diagnosis of COVID-19. Of these, 1621 (14.34%) were MV.
Descriptive Data
Of the total sample population, 58.8% identified as White or Caucasian, 32.6% as Black or African American, 10% as Arab or Middle Eastern, and 3.1% as Hispanic or Latino. Males represented 49.96% of the sample. Patients with disabilities comprised 9.7% of the sample population.
Outcome Data
Table 1 illustrates the characteristics of the study participants, grouped by need for MV. The mean age in years for patients who were MV was 65.73 (SD 13.73), and for those who were not MV 63.4 (SD 18.33). On average, patients requiring MV were older (p<0.01) and had a significantly higher BMI (33.27 versus 31.12; p<0.01). Males had 47% greater odds of MV than females (OR 1.47, p<0.01). Black patients had 47% greater odds of MV than White patients (OR 1.47, p<0.01). Disabled patients had 73% greater odds of MV than full-time working patients (OR 1.73, p=0.001). Patients with Medicare had 25% greater odds of MV than patients with private insurance (OR 1.25, p<0.01), and those without a PCP had 14% greater odds of MV than patients with a PCP (OR 1.14, p=0.03). Patients needing MV were identified as living in zip codes associated with higher unemployment rates (p<0.01), public transportation to work (p<0.01), working in service professions (p<0.01), lower median income (p<0.01), and poverty (p<0.01).
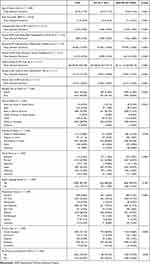 |
Table 1 Descriptive Variables, Stratified by MV |
Main Results
Table 2 illustrates a multivariate model to predict MV. For each additional year of age, odds of MV increased by 2% (p<0.01). For each decrease of $1000 in median income in a ZIP code, the adjusted odds of MV increased by 1% (p<0.01). Male gender (AOR 1.43, p<0.01), Black race (AOR 1.61, p<0.01), low median income (AOR 0.99, p<0.01), non-English speakers (AOR 1.26, p=0.015), and disability (AOR 1.55, p<0.01) correlated with higher odds of mechanical MV.
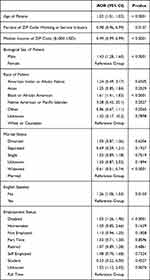 |
Table 2 Multivariate Model to Predict MV |
Discussion
Key Results
Our results suggest that several demographic factors are associated with an increased risk of MV in COVID-19 patients. Beginning with socioeconomic status, MV patients were more likely to live in zip codes with higher rates of unemployment, poverty, public transportation, food stamp use, and essential service jobs. COVID-19 burden has been similarly observed in regions scoring high on the Distressed Communities Index, including Detroit.7,8 Zhang et al further demonstrated that NYC neighborhoods with disadvantaged social conditions (low socioeconomic status, non-white, elderly) had higher mortality rates from COVID-19.9 Under conditions of crowded living, public transport, and frontline work, transmission is more likely.9 Financial insecurity and lack of insurance may also delay seeking medical care until advanced stages of infection.10 Accordingly, we were surprised to find that patients under the “Not employed” category did not have a higher risk of MV. This could be a limitation of the EMR if employment history is not updated.
In terms of race, we found that Black patients were at 47% greater odds of being MV than White patients. In Michigan, Black residents constitute 14.1% of the population,11 7% of COVID-19 cases, yet 20.1% of COVID-19 deaths as of May 26, 2021.12 Similar observations between Black race and COVID-19 burden have been found after controlling for pre-existing comorbidities.10 It is possible that Black patients delay seeking medical attention as quickly as their White counterparts.10 Distrust in medical providers or financial barriers as previously discussed may play a role.10 Black Americans also comprise a disproportionate percentage of frontline jobs where risk of exposure is high, including nursing homes or skilled care facilities, courier services, and urban transportation.13
Patients with disabilities were also more likely to be MV from COVID-19. Intellectual and developmental disability (IDD) has previously been shown to be at greater risk for COVID-19 infection, however these results may be confounded by population density as samples resided in group homes or urban settings where transmission is greater.14 More research to illuminate morbidity/mortality outcomes in disabled patients with COVID-19 is needed. Our results are limited as “disability” in the EMR does not delineate physical, intellectual, or professional definition.
In the univariate analysis, no significant difference was found between MV and non-MV patients regarding non-English speaking status (p=0.1061). However, when adjusted for all other variables in the multivariate analysis, the odds of intubation were significantly increased in non-English speaking patients (p=0.015). Indeed, language barriers, even with the help of translation services, have been associated with less frequent COVID-19 testing and thus higher burden of infection.15
Application of the aforementioned findings could be considered when stratifying patient risk in an emergency room or inpatient setting. Prognostic calculators, such as COVID-Nolab,16 help predict patient outcomes in resource limited settings where diagnostic labs are delayed or unavailable, and adding a demographic component to these calculations could improve their accuracy. Social determinants of health, particularly elderly and socioeconomically vulnerable patients, have even been associated with COVID-19 subphenotypes that yield higher mortality rates.17 Our findings further support the need for health policy to protect these more vulnerable communities.17
Our study focuses on a southeast Michigan population with a primarily urban and suburban demographic, though results can be generalized to the population as similar findings have been observed nationally and internationally. Limitations of this study include retrospective nature as well as potential inaccuracies and missing data in the medical record.
Conclusion
Health-care disparities have negatively impacted patient outcomes during the COVID-19 pandemic. Our study shows how Black race, low socioeconomic status, non-English-speaking status, and disability were all predictors for MV from COVID-19. These demographic predictors should help health providers stratify patient risk and disposition in the ER or inpatient setting. What remains is an urgent need to create a pandemic response program that strategizes prevention and care for communities historically oppressed by structural inequalities.
Data Sharing Statement
The data used to support the findings of this study are available from the corresponding author upon request.
Ethics Approval
The study was approved by the Beaumont Health Institutional Review Board. The study was approved under expedited review and the patient consent was waived as the study design was retrospective. Data confidentiality and compliance with the Declaration of Helsinki were maintained.
Funding
This research did not receive any specific funding.
Disclosure
The authors have no conflicts of interest regarding the publication of this paper.
References
1. Gu T, Mack JA, Salvatore M, et al. Characteristics Associated With Racial/Ethnic Disparities in COVID-19 Outcomes in an Academic Health Care System. JAMA Netw Open. 2020;3(10):e2025197. doi:10.1001/jamanetworkopen.2020.25197
2. Muñoz-Price LS, Nattinger AB, Rivera F, et al. Racial disparities in incidence and outcomes among patients with COVID-19. JAMA Netw Open. 2020;3(9):e2021892. doi:10.1001/jamanetworkopen.2020.21892
3. Ogedegbe G, Ravenell J, Adhikari S, et al. Assessment of Racial/Ethnic Disparities in Hospitalization and Mortality in Patients With COVID-19 in New York City. JAMA Netw Open. 2020;3(12):e2026881. doi:10.1001/jamanetworkopen.2020.26881
4. Yu L, Halalau A, Dalal B, et al. Machine learning methods to predict mechanical ventilation and mortality in patients with COVID-19. PLoS One. 2021;16(4):e0249285. doi:10.1371/journal.pone.0249285. PMID: 33793600; PMCID: PMC8016242.
5. Poulson M, Geary A, Annesi C, et al. National Disparities in COVID-19 Outcomes between Black and White Americans. J Natl Med Assoc. 2021;113(2):125–132. doi:10.1016/j.jnma.2020.07.009
6. Auld SC, Caridi-Scheible M, Blum JM, et al. The Emory COVID-19 Quality and Clinical Research Collaborative. ICU and Ventilator Mortality Among Critically Ill Adults With Coronavirus Disease 2019. Crit Care Med. 2020;48(9):e799–e804. doi:10.1097/CCM.0000000000004457. PMID: 32452888; PMCID: PMC7255393.
7. Hawkins RB, Charles EJ, Mehaffey JH. Socio-economic status and COVID-19-related cases and fatalities. Public Health. 2020;189:129–134. doi:10.1016/j.puhe.2020.09.016. Epub 2020 Oct 17. PMID: 33227595; PMCID: PMC7568122.
8. Sandhu A, Korzeniewski SJ, Polistico J, et al. Elevated COVID19 mortality risk in Detroit area hospitals among patients from census tracts with extreme socioeconomic vulnerability. EClinicalMedicine. 2021;34:100814. doi:10.1016/j.eclinm.2021.100814
9. Zhang Y, Khullar D, Wang F, et al. Socioeconomic variation in characteristics, outcomes, and healthcare utilization of COVID-19 patients in New York City. PLoS One. 2021;16(7):e0255171. doi:10.1371/journal.pone.0255171. PMID: 34324574; PMCID: PMC8321227.
10. Parpia AS, Martinez I, El-Sayed AM, et al. Racial disparities in COVID-19 mortality across Michigan, United States. EClinicalMedicine. 2021;33:100761. doi:10.1016/j.eclinm.2021.100761
11. Census Bureau US. QuickFacts: Michigan. Census Bureau QuickFacts; 2021. Available form: https://www.census.gov/quickfacts/Mi.
12. Coronavirus - Michigan Data. Michigan.gov; 2021. Available form: https://www.michigan.gov/coronavirus/0,9753,7–406–98163_98173–––,00.html.
13. Labor Force Statistics from the Current Population Survey. U.S. Bureau of Labor Statistics. Available form: https://www.bls.gov/cps/cpsaat18.htm.
14. Landes SD, Turk MA. COVID-19 outcomes among people with intellectual and developmental disability in California: the importance of type of residence and skilled nursing care needs. Disabil Health J. 2021;14(2):101051. doi:10.1016/j.dhjo.2020.101051. Epub 2020 Dec 5. PMID: 33309535; PMCID: PMC7719000.
15. Kim HN, Lan KF, Nkyekyer E, et al. Assessment of Disparities in COVID-19 Testing and Infection Across Language Groups in Seattle, Washington. JAMA Netw Open. 2020;3(9):e2021213. doi:10.1001/jamanetworkopen.2020.21213
16. Ebell MH, Cai X, Lennon R, et al. Development and Validation of the COVID-NoLab and COVID-SimpleLab Risk Scores for Prognosis in 6 US Health Systems. J Am Board Fam Med. 2021;34(Suppl):S127–S135. doi:10.3122/jabfm.2021.S1.200464. PMID: 33622827; PMCID: PMC8343954.
17. Su C, Zhang Y, Flory JH, et al. Clinical subphenotypes in COVID-19: derivation, validation, prediction, temporal patterns, and interaction with social determinants of health. NPJ Digit Med. 2021;4(1):110. doi:10.1038/s41746-021-00481-w. PMID: 34262117; PMCID: PMC8280198.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
