Back to Journals » OncoTargets and Therapy » Volume 8
Single-port versus conventional multiport access prophylactic laparoscopic bilateral salpingo-oophorectomy in high-risk patients for ovarian cancer: a comparison of surgical outcomes
Authors Angioni S , Pontis A, Sedda F, Zampetoglou T, Cela V, Mereu L, Litta P
Received 10 February 2015
Accepted for publication 16 April 2015
Published 25 June 2015 Volume 2015:8 Pages 1575—1580
DOI https://doi.org/10.2147/OTT.S82570
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 5
Editor who approved publication: Dr Faris Farassati
Stefano Angioni,1 Alessandro Pontis,1 Federica Sedda,1 Theodoros Zampetoglou,2 Vito Cela,3 Liliana Mereu,4 Pietro Litta5
1Department of Surgical Sciences, University of Cagliari, Cagliari, Italy; 2Obstetrics and Gynecology, Iaso Thessalia Hospital, Larissa, Greece; 3Department of Obstetrics and Gynecology, University of Pisa, Pisa, 4Ospedale S Chiara, Trento, 5Department of Obstetrics and Gynecology, University of Padua, Padua, Italy
Abstract: Bilateral salpingo-oophorectomy (BSO) in carriers of BRCA1 and BRCA2 mutations is widely recommended as part of a risk-reduction strategy for ovarian or breast cancer due to an underlying genetic predisposition. BSO is also performed as a therapeutic intervention for patients with hormone-positive premenopausal breast cancer. BSO may be performed via a minimally invasive approach with the use of three to four 5 mm and/or 12 mm ports inserted through a skin incision. To further reduce the morbidity associated with the placement of multiple port sites and to improve cosmetic outcomes, single-port laparoscopy has been developed with a single access point from the umbilicus. The purpose of this study was to evaluate the surgical outcomes associated with reducing the risks of salpingo-oophorectomy performed in a single port, while comparing multiport laparoscopy in women with a high risk for ovarian cancer. Single-port laparoscopy–BSO is feasible and safe, with favorable surgical and cosmetic outcomes when compared to conventional laparoscopy.
Keywords: prophylactic salpingectomy, single-port access laparoscopy, BRCA carriers
Introduction
Women with BRCA1 or BRCA2 mutations have a 60%–80% cumulative lifetime risk (to 70 years of age) of developing invasive breast cancer and a 15%–65% cumulative lifetime risk of invasive epithelial ovarian cancer.1 Bilateral salpingo-oophorectomy (BSO) in carriers of BRCA1 and BRCA2 mutations is widely recommended to help reduce the risk of ovarian or breast cancer due to an underlying genetic predisposition. BSO is also performed as a therapeutic intervention for patients with hormone-positive premenopausal breast cancer. Preventive oophorectomy has been associated with an 80% reduction in the risk of ovarian, fallopian tube, or peritoneal cancer in BRCA1 or BRCA2 carriers, and a 77% reduction in all-cause mortality.2 Increased knowledge and availability of genetic testing has increased the number of women who are able to identify their risk for the eventual development of breast cancer or ovarian and/or endometrial cancer. This has led many women to consider asking for surgical prophylactic treatment to decrease the potential risk of developing a malignant disease.
The risks and benefits of salpingo-oophorectomy should be weighed, including the degree of protection against cancer and the consequences of induced surgical menopause on health and quality of life.3,4 BSO may be performed via a minimally invasive approach with the use of three to four 5 mm and/or 12 mm ports inserted through skin incisions. To further reduce the morbidity associated with the placement of multiple port sites, and to improve the cosmetic outcomes, single-port access laparoscopy (SPAL) has played an increasing role in gynecology.5,6 Although the feasibility of this procedure has been established, it is still unclear if real advantages exist in performing SPAL versus conventional multiport laparoscopy (MPL).7–9 The purpose of this study was to evaluate the surgical outcomes of prophylactic single-port salpingo-oophorectomy compared to conventional MPL in women with a high risk for ovarian cancer.
Materials and methods
This was a prospective, multicentric, case–control study of patients with a high risk for ovarian cancer undergoing a BSO. BSOs were performed between June 2008 and March 2014 in the Division of Obstetrics and Gynecology of Cagliari (a university hospital in Cagliari, Italy), the Division of Gynecology and Obstetrics of Pisa (University of Pisa, Pisa, Italy), the Division of Obstetrics and Gynecology, Ospedale S Chiara (Trento, Italy), and the Division of Obstetrics and Gynecology of Padua (University of Padova, Padua, Italy).
The inclusion criteria were gene-status BRCA1 and BRCA2 carriers and women with hormone-positive premenopausal breast cancer. Cervix cytology and transvaginal sonography evaluations were performed to confirm any suspicion of malignancy, and even the possibility of deep endometriosis.10 An office diagnostic hysteroscopy with a biopsy ruled out any potential intrauterine diseases.11 Other exclusion criteria were anesthetic contraindication or a desire of the patient to maintain the ovaries.12 The study was approved by the local ethics committees (Department of Surgical Sciences, Cagliari; University of Pisa; University of Padua; Ospedale S. Chiara Trento), and before entering the study, all eligible patients received oral and written information about the trial by the clinicians and gave their consent.
Ninety-nine out of 115 patients met the inclusion criteria and entered the study. In each center, the patients were informed about the two types of surgeries and were alternatively assigned to undergo an SPAL-BSO performed by four surgeons (SA, PL, VC, and LM) with optimal laparoscopic experience and at least 1 year of training for this procedure, or an MPL-BSO performed by skilled laparoscopic surgeons without SPAL experience. They were also informed that additional incisions might be necessary during the surgical procedure for the single-port laparoscopy.
Upon agreeing to participate in the study, patients were asked to complete baseline questionnaires that included their sociodemographic data and medical history. Prospective data of these patients were collected until March 2014. These data included patient characteristics (age and body mass index [BMI] [kg/m2]), comorbidity, type and duration of surgery, estimated blood loss, postoperative pain score, perioperative complications, length of hospital stay, use of analgesics, and cosmetic satisfaction. At the end of each procedure, intraoperative data – trocar introducing time, operative time, estimated blood loss, intra- and perioperative complications, and conversion to standard multiaccess laparoscopy or laparotomy – were registered.
Operative time was defined as the time from umbilical skin incision to completion of skin closure. Postoperative pain intensity was rated at rest using the visual analog scale (VAS). The scale was presented as a 10 cm line, with a verbal descriptor anchored with “no pain” and “worst imaginable pain”. Patients were asked to rate their pain intensity at 6 hours, 12 hours, and 24 hours after surgery.
Patient cosmetic satisfaction was assessed using the Body Image Questionnaire (BIQ) at baseline, 1 week, 4 weeks, and 24 weeks postsurgery. Subjects were asked to complete the BIQ at each visit before seeing their clinician. The BIQ consisted of eight questionnaires in two domains: the Body Image Scale (BIS) and the Cosmetic Scale (CS). Cronbach’s alpha for body image and cosmetic satisfaction were 0.81 and 0.70, respectively. The maximum scores for BIS and CS were 20 and 24, respectively.13
A regression modeling analysis was preliminary performed to evidence any significant difference in outcomes among the surgeons of the two groups. The Kolmogorov–Smirnov test was used to evaluate whether values had a Gaussian distribution in order to choose between parametric and nonparametric statistical tests. Comparisons of the proportions and means between groups were done by using the χ2 test and independent t-tests, respectively. Statistical differences between repeated measurements were computed using the paired t-test or the Wilcoxon matched pairs test for nonparametric values, both in the case of two comparisons. The analysis of variance for repeated measures and the Friedman test were used for parametric and nonparametric data, respectively. Statistical significance was set at P<0.05.
Surgery
All patients included in the study were admitted to the hospital 1 day before surgery. Standard bowel preparation was indicated, and prophylactic antibiotic therapy (2 g of cefazolin) was administrated 30 minutes preoperatively and again postoperatively. Both SPAL-BSO and MPL-BSO were performed under general endotracheal anesthesia with the patient in the dorsal lithotomy position. A Foley catheter was inserted into the bladder, and then a uterine manipulator was applied. In both procedures, a pelvic washing and an abdominal exploration were performed. The right infundibulopelvic ligament was skeletonized and transected at least 2 cm below the ovarian tissue proper using a 5 mm ENSEAL® Trio Device (Ethicon, Inc., Somerville, NJ, USA). The right fallopian tube and mesosalpinx were dissected, and the utero–ovarian ligament was transected. The same procedure was repeated on the contralateral side. The adnexae were placed in a 10 mm specimen retrieval bag (ENDOPOUCH®; Ethicon, Inc.), and the specimens were removed. To prevent or decrease the occurrence of postsurgical adhesions, 500 mL of warm lactated Ringer’s solution was instilled in the pelvis at the end of the procedures.14 The extracted specimens were sent for histologic examination, and a Foley vesical catheter was maintained until the morning after surgery.
Hemoglobin concentration was determined in all patients 6 hours after surgery. All patients were permitted sips of water starting 6 hours after surgery, and a clear liquid diet was offered as the first meal after passing flatus. If pain control was needed, 30 mg of ketorolac was administered intravenously. The patients were encouraged to ambulate starting the first postoperative day.
All surgical specimens were sent for pathologic evaluation. The ovaries were sectioned along the major axis in order to produce 2 mm thick sections. The tubes were analyzed completely and were cut into sections of 2 mm or 3 mm in transversal thickness. The fimbria, which is known to be the preferential seat of occurrence of tubal carcinoma, was cut into longitudinal sections.
Single-port technique
A 2 cm intraumbilical vertical skin incision and a 2–2.5 cm rectus fasciotomy were performed to enter the peritoneal cavity, as previously described.15 A reusable single-port trocar (S-Portal X-Cone; KARL STORZ GmbH & Co. KG, Tuttlingen, Germany) was inserted into the abdominal cavity, and the abdomen was insufflated to 12 mmHg. The single-port trocar device allows the simultaneous passage of various laparoscopic instruments through one small opening and has the added advantage of being reusable. A rigid, 30°, 5 mm diameter, 50 cm length, Hopkins high-definition three-chip camera (KARL STORZ GmbH & Co. KG) was routinely used.
At the end of the procedures, specimens were removed through the umbilicus after first removing the port device.
Multiport access technique
For conventional laparoscopy, we used a closed technique, preinflating the peritoneal cavity with CO2 through a hollow insufflation needle (Veress needle) via a midline infraumbilical incision. Following pneumoperitoneum, an umbilical 10 mm trocar for a 0° telescope was made. Three additional trocars (5–10 mm) were then inserted in the lower abdominal quadrants under direct laparoscopic vision, as previously described.16 Specimens were removed through a sovrapubic incision.
Results
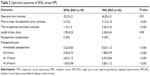
Patient characteristics are shown in Table 1. The surgical treatment allocation did not determine any withdrawals from the study. In total, we performed 99 surgical procedures: 49 SPAL-BSO (group A) and 50 MPL-BSO (group B). There were no differences in the demographic and preoperative data between the two groups.
Port placement was successful in all patients, and there were no vascular or visceral injuries, loss of pneumoperitoneum, or intraoperative port site bleeding. None of the patients were converted to a laparotomy. There was no conversion to MPL or the need for additional ports. No postoperative complications were observed in either group. The preliminary regression modeling analysis that was performed did not yield evidence of any significant difference in the outcomes among the surgeons in the two groups.
The SPAL-BSO mean operative time was statistically significantly lower than that of the MPL (35.32±13 minutes versus 40.02±10 minutes, respectively; P=0.02). The time of entry into the abdominal cavity was significantly lower in group A (4.15±2 minutes versus 9.12±3.10 minutes, respectively; P<0.001), as was the extraction time of the specimens (1.15±1.5 minutes versus 5.30±3.10 minutes, respectively; P<0.001) (Table 2). Moreover, the SPAL group had a shorter postoperative hospital stay compared to the conventional MPL group, but without significance (1.95±0.35 days versus 2.38±0.43 days, respectively; P=0.08).
Pain measured immediately after surgery in the recovery unit was lower in the SPAL-BSO group than in the MPL-BSO group. Moreover, postoperative pain scores after 6 hours, 12 hours, and 24 hours were lower in the SPAL-BSO group compared with the MPL-BSO group (Table 2).
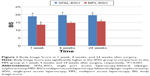
The BIS and CS scores at 1 week, 4 weeks, and 24 weeks in the two groups are shown in Figures 1 and 2. At 1 week and 4 weeks after surgery, the mean (± standard deviation) BIS score in the SPAL-BSO group was significantly higher (18.90±0.69 and 19.65±0.54, respectively; P<0.001). At 24 weeks after surgery, the BIS score was still higher in the SPAL-SH group compared with the MPL-BSO group (P<0.001). The CS scores at 1 week and 4 weeks after surgery were also higher in the SPAL-BSO group than in the MPL-BSO group (P<0.001) and the result was maintained at 48 weeks (23.65±1.06 versus 15.71±0.78, respectively; P<0.001).
Discussion
Women with mutations in the BRCA1 and BRCA2 gene have a higher risk of developing ovarian cancer, but there are currently no screening protocols for ovarian cancer. Adhesion to strict observation protocols can determine a diagnosis at the earliest stages of the tumor, but it does not affect mortality. The cell of origin of ovarian cancer and the mechanisms by which cancer develops have long been debated. There is mounting evidence that type I and type II ovarian tumors develop independently along different molecular pathways, and that both types develop in the fallopian tube and involve it secondarily.17 For this reason, patients who are carriers of BRCA mutations are candidates for BSO. The timing for performing BSO is crucial; it should be proposed to women of childbearing age, 35–40 years, who already had or do not wish to have children. Bilateral salpingectomy and delaying ovariectomy after pregnancy could also be proposed in selected patients.18 The decision to undergo surgery is difficult. On the one hand, there is the possibility of neoplastic disease, while on the other hand, patients are faced with the psychological burden of surgical menopause, as well as the risks and cosmetic damage related to the surgery itself. Therapeutic BSO is even frequently proposed in patients previously treated for hormonal-dependent breast carcinoma.19
Open surgery facilitates the intervention by the surgeon; however, recent progress and development in the laparoscopic technique do not indicate its use for this type of surgery. Numerous studies have demonstrated that laparoscopic approaches to various gynecologic oncology conditions, including early-stage endometrial cancer, cervical cancer, and selected pelvic masses, are feasible and result in shorter hospital stays and improved quality of life.20,21
The SPAL is an important development as a new laparoscopic technique.5–9 This technique, which is based on reducing the invasiveness and increasing the acceptability and esthetic results of the classic laparoscopic technique, consists of the introduction of a single-port access system through a natural scar, the umbilicus. This access system accommodates both the instruments and the camera, eliminating the need for multiple separate trocars required by traditional laparoscopic surgery.
One of the major benefits of the SPAL surgery is purportedly the best esthetic outcome. To date, however, there has been no conclusive evidence supporting this,22–24 and some studies have not shown any superiority of the single-port access over conventional laparoscopic procedures. Lee et al25 demonstrated that SPAL adnexal surgery had comparable operative outcomes to conventional laparoscopic adnexal surgery. In a randomized controlled trial, Song et al24 compared cosmetic satisfaction from laparoendoscopic single-site hysterectomy with multiport surgery. The SPAL group reported significantly higher cosmetic satisfaction at 1 week, 4 weeks, and 24 weeks after surgery. Moreover, a recent study evidenced the benefit in relation to body image and cosmesis in SPAL subtotal hysterectomy.26 Our study also showed that cosmetic results were significantly higher in the SPAL group compared to the MPL group.
Regarding postoperative pain, Kim et al27,28 showed a reduction in postoperative pain scores, but with similar perioperative outcomes with SPAL surgery compared to traditional laparoscopy in adnexal pathology and LAVH. Another randomized controlled trial showed that single-site access provides an advantage over conventional multiaccess laparoscopy in terms of postoperative pain and the need for rescue analgesia, with similar perioperative outcomes.29 A meta-analysis by Song et al30 that included 331 participants evaluated postoperative pain using a VAS at different time points from the first postoperative day to the day of discharge. The VAS score at 6 hours, 24 hours, and 48 hours postoperatively showed no significant differences between the two techniques.30 In our study, we recorded postoperative pain that was significantly lower in the SPAL group than that experienced in the MPL group, as evidenced by lower mean scores on the VAS. The Song et al30 meta-analysis showed that the operative time was longer in the SPAL group than in the MPL group, but this difference was not considered to be statistically significant. In our study, we obtained lower operative times with SPAL-BSO compared to MPL. We clearly demonstrated that single-port entry is significantly more rapid than the creation of a pneumoperitoneum and the insertion of an umbilical trocar and 2–3 suprapubic ancillary trocars. Finally, we showed that SPAL surgery offers the advantage of faster and easier extraction of the surgical specimens. In fact, the single access localized at the level of the umbilicus is broader in comparison to those that are performed for traditional laparoscopic surgery. This allows for more rapid and easier extraction, without the need for fragmentation of the surgical specimen and enlargement of the sites of insertion of the trocar; this results in a significantly shorter time than conventional laparoscopy for this phase of the surgery.
Conclusion
SPAL-BSO is feasible and safe with favorable surgical and cosmetic outcomes compared to conventional MPL. The SPAL approach may be ideal for BRCA mutation carriers and breast cancer patients because of its short convalescence, minimal interruption in any ongoing cancer treatment, and the benefits from improved cosmetics and pain. Prospective randomized controlled trials are needed in the future to assess the benefits of SPAL compared to MPL.
Author contributions
All authors contributed toward the data analysis, as well as drafting and revising the paper, and they have agreed to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Lancaster JM, Powell CB, Kauff ND, et al; Society of Gynecologic Oncologists Education Committee. Society of Gynecologic Oncologists Education Committee statement on risk assessment for inherited gynecologic cancer predispositions. Gynecol Oncol. 2007;107(2):159–162. | ||
Finch AP, Lubinski J, Møller P, et al. Impact of oophorectomy on cancer incidence and mortality in women with a BRCA1 or BRCA2 mutation. J Clin Oncol. 2014;32(15):1547–1553. | ||
Finch A, Evans G, Narod SA. BRCA carriers, prophylactic salpingo-oophorectomy and menopause: clinical management considerations and recommendations. Womens Health (Lond Engl). 2012;8(5):543–555. | ||
Arai M, Taki K, Iwase H, Takizawa K, Nishimura S, Iwase T. [Present status and tasks for genetic testing and risk-reducing surgery in patients with hereditary breast and ovarian cancer]. Gan To Kagaku Ryoho. 2012;39(4):525–531. Japanese. | ||
Angioni S, Mereu L, Maricosu G, Mencaglia L, Melis GB. Single port access laparoscopy (SPAL) for endometrioma excision. J Endometr. 2010;2(2):95–98. | ||
Angioni S, Maricosu G, Mereu L, Mencaglia L, Melis GB. Single-port access laparoscopic assisted vaginal hysterectomy in a case of uterine ventrofixation using a new reusable device. J Obstet Gynaecol Res. 2011;37(7):933–936. | ||
Angioni S, Pontis A, Sorrentino F, Nappi L. Bilateral salpingo-oophorectomy and adhesiolysis with single port access laparoscopy (SPAL) and use of diode laser in a BRCA carrier. Eur J Gynaecol Oncol. In press 2015. | ||
Angioni S, Pontis A, Cela V, et al. Single-port access laparoscopic hysterectomy: a literature review. J Gynecol Surg. 2014;30(6):329–337. | ||
Mereu L, Angioni S, Pontis A, Carri G, Mencaglia L. Single port access laparoscopic myomectomy with X-Cone. Gynecol Surg. 2011;8(3):337–340. | ||
Guerriero S, Ajossa S, Gerada M, Virgilio B, Angioni S, Melis GB. Diagnostic value of transvaginal ‘tenderness-guided’ ultrasonography for the prediction of location of deep endometriosis. Hum Reprod. 2008;23(11):2452–2457. | ||
Di Spiezio Sardo A, Bettocchi S, Spinelli M, et al. Review of new office-based hysteroscopic procedures 2003–2009. J Minim Invasive Gynecol. 2010;17(4):436–448. | ||
Angioni S, Mais V, Pontis A, Peiretti M, Nappi L. First case of prophylactic salpingectomy with single port access laparoscopy and a new diode laser in a woman with BRCA mutation. Gynecol Oncol Case Rep. 2014;9:21–23. | ||
Song T, Kim TJ, Cho J, et al. Cosmesis and body image after single-port access surgery for gynaecologic disease. Aust N Z J Obstet Gynaecol. 2012;52(5):465–469. | ||
Rizzo A, Spedicato M, Mutinati M, et al. Peritoneal adhesions in human and veterinary medicine: from pathogenesis to therapy. A review. Immunopharmacol Immunotoxicol. 2010;32(3):481–494. | ||
Mereu L, Angioni S, Melis GB, Mencaglia L. Single access laparoscopy for adnexal pathologies using a novel reusable port and curved instruments. Int J Gynaecol Obstet. 2010;109(1):78–80. | ||
Pluchino N, Litta P, Freschi L, et al. Comparison of the initial surgical experience with robotic and laparoscopic myomectomy. Int J Med Robot. 2014;10(2):208–212. | ||
Kurman RJ, Shih IeM. The origin and pathogenesis of epithelial ovarian cancer: a proposed unifying theory. Am J Surg Pathol. 2010;34(3):433–443. | ||
Hirasawa A, Masuda K, Akahane T, et al. Experience of risk-reducing salpingo-oophorectomy for a BRCA1 mutation carrier and establishment of a system performing a preventive surgery for hereditary breast and ovarian cancer syndrome in Japan: our challenges for the future. Jpn J Clin Oncol. 2013;43(5):515–519. | ||
Angioni S, Pontis A, Dessole M, Surico D, De Cicco Nardone C, Melis I. Pain control and quality of life after laparoscopic en-block resection of deep infiltrating endometriosis (DIE) vs. incomplete surgical treatment with or without GnRHa administration after surgery. Arch Gynecol Obstet. 2015;291(2):363–370. | ||
Tinelli R, Litta P, Meir Y, et al. Advantages of laparoscopy versus laparotomy in extremely obese women (BMI >35) with early-stage endometrial cancer: a multicenter study. Anticancer Res. 2014;34(5):2497–2502. | ||
Cho JE, Liu C, Gossner G, Nezhat FR. Laparoscopy and gynecologic oncology. Clin Obstet Gynecol. 2009;52(3):313–326. | ||
Mencaglia L, Mereu L, Carri G, et al. Single port entry – are there any advantages? Best Pract Res Clin Obstet Gynaecol. 2013;27(3):441–455. | ||
Angioni S, Pontis A, Cela V, et al. Surgical technique of endometrioma excision impacts on the ovarian reserve. Single-port access laparoscopy versus multiport access laparoscopy: a case control study. Gynecol Endocrinol. In press 2015. | ||
Song T, Cho J, Kim TJ, et al. Cosmetic outcomes of laparoendoscopic single-site hysterectomy compared with multi-port surgery: randomized controlled trial. J Minim Invasive Gynecol. 2013;20(4):460–467. | ||
Lee YY, Kim TJ, Kim CJ, et al. Single port access laparoscopic adnexal surgery versus conventional laparoscopic adnexal surgery: a comparison of peri-operative outcomes. Eur J Obstet Gynecol Reprod Biol. 2010;151(2):181–184. | ||
Angioni S, Pontis A, Pisanu A, Mereu L, Roman H. Single-port access subtotal laparoscopic hysterectomy: a prospective case-control study. J Minim Invasive Gynecol. Epub 2015 Mar 18. | ||
Kim TJ, Lee YY, An JJ, et al. Does single-port access (SPA) laparoscopy mean reduced pain? A retrospective cohort analysis between SPA and conventional laparoscopy. Eur J Obstet Gynecol Reprod Biol. 2012;162(1):71–74. | ||
Kim TJ, Lee YY, Cha HH, et al. Single-port-access laparoscopic-assisted vaginal hysterectomy versus conventional laparoscopic-assisted vaginal hysterectomy: a comparison of perioperative outcomes. Surg Endosc. 2010;24(9):2248–2252. | ||
Fagotti A, Bottoni C, Vizzielli G, et al. Postoperative pain after conventional laparoscopy and laparoendoscopic single site surgery (LESS) for benign adnexal disease: a randomized trial. Fertil Steril. 2011;96(1):255–259.e2. | ||
Song T, Kim ML, Jung YW, Yoon BS, Joo WD, Seong SJ. Laparoendoscopic single-site versus conventional laparoscopic gynecologic surgery: a metaanalysis of randomized controlled trials. Am J Obstet Gynecol. 2013;209(4):317.e1–e9. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.