Back to Journals » Neuropsychiatric Disease and Treatment » Volume 17
Serum miR-128 Serves as a Potential Diagnostic Biomarker for Alzheimer’s Disease
Authors Zhang M, Han W, Xu Y, Li D, Xue Q
Received 7 November 2020
Accepted for publication 8 January 2021
Published 29 January 2021 Volume 2021:17 Pages 269—275
DOI https://doi.org/10.2147/NDT.S290925
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Taro Kishi
Ming Zhang, 1– 3 Wei Han, 3, 4 Yuhao Xu, 3, 4 Dapeng Li, 3 Qun Xue 1
1Department of Neurology, The First Affiliated Hospital of Soochow University, Suzhou, Jiangsu 215006, People’s Republic of China; 2Department of Geriatric Psychiatry, Changzhou Dean Hospital, Changzhou, Jiangsu 213000, People’s Republic of China; 3Department of Central Laboratory, The Affiliated Hospital of Jiangsu University, Zhenjiang, Jiangsu 212001, People’s Republic of China; 4Department of Neurology, The Affiliated Hospital of Jiangsu University, Zhenjiang, Jiangsu 212001, People’s Republic of China
Correspondence: Qun Xue
Department of Neurology, The First Affiliated Hospital of Soochow University, Suzhou, Jiangsu 215006, People’s Republic of China
Tel + 86- 13013813620
Email [email protected]
Background: Although numerous microRNAs (miRNAs) have been discovered to participate in the progression of Alzheimer’s disease (AD), they are still difficult to apply in clinical work. Thus, the identification of novel miRNAs and clarification of their clinical significance are importing for improving the diagnosis and treatment of AD. The purpose of this study was to analyze the expression of miR-128 and its diagnostic value in patients with AD.
Patients and Methods: In this study, 117 AD patients and 106 controls were enrolled, and the demographic data, biochemical parameters and serum miR-128 levels were collected. These data were then used to build a logistic regression model, and receiver operating characteristic (ROC) curves were drawn to evaluate the diagnostic value of miR-128. The relationships between miR-128 and inflammatory factors (IL-1β/TNF-α) were also analyzed from clinical serum data.
Results: Our study found that miR-128 was significantly upregulated in the serum samples of AD patients compared with controls, and that this upregulation was negatively correlated with Mini-Mental State Examination (MMSE) scores (r = − 0.687, P< 0.01). ROC curve showed that the area under the curve of miR-128 was 0.831. Logistic regression analyses showed that glycosylated hemoglobin (HbA1c) levels, low-density lipoprotein (LDL) levels, MMSE scores and serum miR-128 levels were statistically significant (P< 0.01), and the ROC curve of the combined detection of these variables was 0.906. The serum miR-128 levels in AD patients were positively correlated with the serum IL-1β (r=0.798, P< 0.01) and serum TNF-α levels (r=0.733, P< 0.01).
Conclusion: Serum miR-128 is a candidate diagnostic biomarker in AD patients who achieved good diagnostic performance when used alone or in combination with other factors and may have the potential to be a novel therapeutic target for neuroinflammation.
Keywords: Alzheimer’s disease, miR-128, logistic regression, ROC curve
Corrigendum for this paper has been published
Introduction
Alzheimer’s disease (AD) is a progressive and irreversible neurodegenerative disease characterized by multiple cognitive anomalies, memory loss, and dysgnosia that accounts for 70–80% of all cases of dementia.1,2 Clinically, an AD diagnosis is comprehensive and based on diagnostic criteria that are combined with brain imaging, neuropsychological testing and medical history. Due to the lack of pathological evidence, doctors need extensive experience to diagnose AD in the current medical setting.3 Thus, it has been proposed that diagnostic methods for AD could be improved by the application of biomarkers that are easily measurable by noninvasive means.
MicroRNAs (miRNAs) are a group of small noncoding RNAs with vital regulatory roles in gene expression.4 Recently, aberrant changes in miRNAs have been discovered to participate in AD progression, and are considered candidate blood-based biomarkers of AD, as they have been found to guide the clinical diagnosis of AD.5,6 Wang et al7 reported that the expression levels of miR-433 were reduced in AD patients and that this miRNA has the potential to be a therapeutic target through improving Aβ-induced neurotoxicity. Yang et al8 provided evidence for miR-133b to serve as a diagnostic biomarker of AD and revealed its neuroprotective role, which is exerted through maintenance of neuronal viability. Although increasing numbers of miRNAs have been discovered, their practical applications in the diagnosis of AD are still limited.9,10 Thus, the identification of novel miRNAs and clarification of their clinical significance are of great importance for improving the diagnosis and treatment of AD.
Previous studies11 showed that miR-128 expression was abnormal in the brains of AD patients and that it is associated with the nosogenesis of AD. Accordingly, a large number of experimental studies have been carried out and have confirmed that miR-128 can downregulate PPAR-γ expression to aggravate Aβ-induced impaired neuronal viability in AD cells and animal models,12,13 which suggests a significant role of miR-128 in AD progression. However, the clinical significance of miR-128 in AD has not been investigated. In this study, we sought to analyze the expression of miR-128 in the serum of AD patients and to determine its diagnostic value; we also sought to tentatively explore the regulatory effect of miR-128 on IL-1β and TNF-α using clinical serum data to provide additional clinical evidence for the early diagnosis and treatment of AD as well as to further reveal possible mechanisms of AD.
Patients and Methods
Participants
A total of 117 AD patients were recruited and diagnosed at the Affiliated Hospital of Jiangsu University from 2017 to 2020. The diagnosis of AD was performed according to the criteria of the National Institute of Neurological and Communication Disorders and Stroke/Alzheimer’s Disease and Related Disorders Association.14 In addition, 106 age- and sex-matched neurologically healthy volunteers were enrolled as controls. The Mini-Mental State Examination (MMSE) score of all participants was assessed to evaluate their cognitive function. None of the participants met the following exclusion criteria: 1) patients with stroke, central nervous system infections, epilepsy and other central nervous system diseases; 2) patients with cardiovascular, liver, kidney and other serious primary diseases; 3) patients with tumors, autoimmune diseases, and anemia; 4) patients with psychiatric disorders or history of familial psychiatric disorders; and 5) patients with a history of a fever, a cold or an infectious venereal disease within the past 2 weeks. The Institutional Review Board of the Affiliated Hospital of Jiangsu University approved the research protocol (JDFY2017098), and a written signed consent, strictly abiding by the Declaration of Helsinki, was obtained from all the participants.
Clinical Examinations of Biochemical Parameters
After fasting for 1 night, 5 milliliters of venous blood from each participant was collected between 6 a.m. and 8 a.m. The blood samples were stored at room temperature for 1 hour, after which the serum was separated by centrifugation at 3000 rpm for 20 minutes at 4°C. An XE-5000 automatic hematology system (Sysmex Corporation, Japan) was used to measure peripheral blood variables. Serum samples were preserved at −80°C until further analysis. Biochemical parameters included levels of fasting plasma glucose (FPG), glycosylated hemoglobin (HbA1c), total cholesterol (TC), triglyceride (TG), high-density lipoprotein (HDL), low-density lipoprotein (LDL), blood urea nitrogen (BUN) and creatinine (CRE) levels.
Extraction and Determination of Serum miR-128
Total miRNA was extracted according to the instructions of the miRcute miRNA extraction and separation kit (DP501, Tiangen, China), and the concentration and purity of RNA were determined by ultraviolet spectrophotometry. According to the miRcute miRNA cDNA first-strand synthesis kit (FP411, Tiangen, China), the corresponding cDNA was reverse transcribed according to the miR-128 primer (5ʹ-GGT CCG AGG TAT TCG CAC TG G ATA CGA CTG CAA T-3ʹ). The reaction conditions of reverse transcription were 42°C for 15 minutes and 95°C for 3 minutes. After reverse transcription, 2 μL of cDNA was obtained. According to the instructions of the miRcute miRNA fluorescence quantitative detection kit (FP411, Tiangen, China), 5 μL of miRcute Plus miRNA PreMix, 0.2 μL of upstream primer (5ʹ-GCG GCG GTC GTC ACA GTG AAC CGG TC-3ʹ). Then, 0.2 μL of downstream primer (5ʹ-ATC CAG TGC AGG GTC CGA GG-3ʹ) and 2.6 μL of ddH2O were added on ice. The expression of miR-128 was determined by real-time fluorescence quantitative PCR. U6 was used as an internal control. The relative level of miR-128 expression was analyzed using the 2-ΔΔCT method and the data were recorded.
Determinations of the Serum IL-1β and TNF-α Levels
The serum levels of IL-1β and TNF-α were examined using ELISA kits (Blue gene, Shanghai, China). One milliliter of serum was collected from each AD patients, and the serum IL-1β and TNF-α levels were determined in each AD patients according to the manufacturer’s instructions.
Statistical Analysis
SPSS 19.0 statistical software (SPSS, Inc., Chicago, IL, USA) and GraphPad Prism 5 (GraphPad Software, Inc., La Jolla, CA) were used to analyze significant differences in the data. Chi-square tests or independent sample t-tests were used to compare the baseline characteristics and the serum miR-128 levels between AD patients and controls. Then, forward logistic stepwise regression analysis was used to build the diagnostic model, and receiver operating characteristic (ROC) curves were drawn to evaluate the diagnostic value of miR-128 for AD patients. Correlation tests were performed using Pearson analysis. The results were considered significant at P <0.05.
Results
Baseline Characteristics of the Research Population
As shown in Table 1, multiple variables were different between the AD patients and controls. Smoking status, diabetes, and FPG, HbA1c, and LDL levels as well as MMSE scores were higher in AD patients than in the controls (P<0.05). Age, sex, and hypertension as well as TC, TG, HDL, BUN, and CRE levels were not significantly different between the two groups (P>0.05).
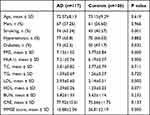 |
Table 1 Analysis of Baseline Characteristics in the Two Groups |
Changes in Serum miR-128 Levels in AD Patients
The AD patients presented significantly higher serum miR-128 levels than controls at baseline [6.37±1.07 vs 5.52±1.01, t=6.256, P<0.01], as shown in Figure 1A. Then, to further assess the relationship between miR-128 and AD, a correlation analysis between miR-128 levels and MMSE scores was performed and analyzed. The results showed that serum miR-128 levels were negatively correlated with MMSE scores (r = −0.687, P< 0.01) (Figure 1B).
Logistic Regression Analysis of the Differences in Baseline Characteristics and miR-128 Levels
Baseline characteristics (smoking status, diabetes, and FPG, HbA1c, and LDL levels, as well as MMSE scores) and serum miR-128 levels were simultaneously included in a multivariate logistic regression analysis using stepwise forward regression, the results of which are shown in Table 2. Only four independent variables, the HbA1c level, LDL level, MMSE score and miR-128 level were entered into the logistic regression equation. The partial regression coefficients were 0.582, 0.774, −0.265 and 0.755, respectively, and their corresponding P-values were 0.001, 0.005, 0.010 and 0.009, respectively. The corresponding regression equation based on these four serum biomarkers was 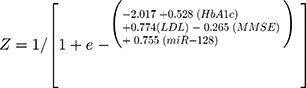
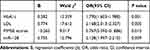 |
Table 2 Logistic Regression Analysis of HbA1c, LDL, MMSE Scores and miR-128 |
ROC Curve Analysis of Serum miR-128 Levels
To further evaluate the diagnostic efficacy of miR-128 in AD, the ROC curve of miR-128 was drawn. The area under the curve was 0.831, the sensitivity was 86.9%, and the specificity was 82.1%, as shown in Figure 2A. Afterwards, the ROC curve obtained by combining the HbA1c level, LDL level, MMSE score and serum miR-128 level was analyzed. The area under the curve of the combined detection of these variables was 0.906, the sensitivity was 93.9%, and the specificity was 87.5%, as shown in Figure 2B. These data suggest that the combined detection of these variables had a better diagnostic rate than the detection of miR-128 alone.
 |
Figure 2 The results of ROC curves. (A) ROC curve of miR-128. (B) ROC curve of combined detection (combining the serum levels of miR-128, HbA1c and LDL and the MMSE score). |
Correlation Analysis of the Serum miR-128, IL-1β and TNF-α Levels
As shown in Figure 3A and B, the correlation analysis indicated that the serum miR-128 levels were positively correlated with the serum IL-1β levels (r=0.798, P<0.01) and the TNF-α levels (r=0.733, P<0.01) in AD patients.
Discussion
The pathogenesis of AD is highly complicated and involves multiple pathophysiological processes, including β-amyloid protein deposition,15 phosphorylation of tau,16 chronic inflammation,17 neurotrophic disorder,18 and oxidative stress,19 among others. The combination of multiple factors leads to the occurrence of AD. Recently, miRNAs and AD has become the focus of research in the field.20 MiR-128, is an important member of the miRNA, but previous studies have mainly focused on the role of miR-128 in central nervous system tumors.21 With the increase in related studies, Lukiw et al,11 first found an increase in miR-128 expression in the hippocampus of AD patients at autopsies. Furthermore, a study by Geng et al,12 found that the inhibition of miR-128 could relieve the Aβ-induced impaired neuronal viability via upregulation of PPAR-γ. Then, Liu et al,13 demonstrated that knockout of miR-128 in AD mice significantly alleviated AD-like performances, and reduced the production of Aβ and the inflammatory response by targeting and reducing PPARγ expression, thereby implying a critical role of miR-128 in AD. Here, with the theoretical support of previous basic research, we studied the changes in serum miR-128 in AD patients and demonstrated, for the first time, that the level of serum miR-128 is increased in AD patient and that it can be used as a biomarker for AD diagnosis.
Substantial research has been devoted to the demographic data of AD patients and has confirmed that age, smoking status, diabetes, and a high LDL level were risk factors for AD.22–24 In this study, after excluding the interference of age and sex, differences in the smoking status, diabetes, FPG level, HbA1c level, LDL level and MMSE score were observed in the baseline data between AD patients and the controls. These results were consistent with those of previous studies and further proved the complexity of AD onset. Then, using logistic regression analysis, we found that the HbA1c level, LDL level, MMSE score and serum miR-128 level were statistically significant and that the miR-128 level could also be an independent risk factor for AD. The area under the ROC curve of miR-128 is 0.831, which demonstrates a high sensitivity and specificity and suggests that serum miR-128 levels can be independently applied to the auxiliary diagnosis of AD. In addition, we jointly analyzed the biomarkers screened by logistic regression and showed that the logistic model based on multiple biomarkers (HbA1c level, LDL level, MMSE score, serum miR-128 level) can improve the diagnostic efficacy of AD according to the comparison of ROC curve parameters. The values of the HbA1c level, LDL level and MMSE score are easy to collect from AD patients, and when analyzed together with the serum miR-128 level, are more conducive to the early diagnosis and treatment of AD.
In addition, a large amount of evidence indicates that neuroinflammation plays a vital role in the pathogenesis of AD with harmful or protective consequences.25,26 As an important member of miRNAs, miR-128 has been reported to be involved in abnormal metabolism of IL-1β and TNF-α in other diseases.27,28 It has also been found that miR-128 may affect the metabolism of inflammatory factors in AD cell and animal experiments. However, the related clinical studies of miR-128 and inflammatory factors in AD patients are still rare. Thus, we tested the serum IL-1β and TNF-α levels in AD patients and analyzed their correlation with serum miR-128 levels, and the results from a clinical perspective also highly suggest that miR-128 may participate in the occurrence of AD by affecting the metabolism of IL-1β and TNF-α; however, this correlation needs to be further explored in cell and animal experiments.
In conclusion, our research is a preliminary clinical study, and some limitations of this study should be noted. First, the baseline data collection in this study is not comprehensive, and many other AD risk factors were not included. Moreover, due to the NINCDS-ADRDA criteria, it is difficult to diagnose AD at an early stage; thus, we did not enroll early-stage patients, and the causal relationship between miR-128 and the progression of the disease may not be conclusive. Additionally, the diagnostic model based on the serum miR-128 level, HbA1c level, LDL level, and MMSE score should be validated in a much larger cohort, and more accurate diagnostic models must exist to further explore this diagnostic model. Despite these restrictions, this study revealed that miR-128 is increased in the serum of AD patients and that its upregulated expression may serve as a promising diagnostic biomarker of AD.
Acknowledgments
This work was supported by the Jiangsu Provincial Key Research and Development Plan (BE2019666).
Disclosure
No conflicts of interest for this work, financial or otherwise, are declared by the authors.
References
1. Pini L, Pievani M, Bocchetta M, et al. Brain atrophy in Alzheimer’s disease and aging. Ageing Res Rev. 2016;30:25–48. doi:10.1016/j.arr.2016.01.002
2. Wahl D, Solon-Biet SM, Cogger VC, et al. Aging, lifestyle and dementia. Neurobiol Dis. 2019;130:104481. doi:10.1016/j.nbd.2019.104481
3. DeTure MA, Dickson DW. The neuropathological diagnosis of Alzheimer’s disease. Mol Neurodegener. 2020;12(1):32. doi:10.3389/fnagi.2020.00005
4. Kou X, Chen D, Chen N. The regulation of microRNAs in Alzheimer’s disease. Front Neurol. 2020;11:288. doi:10.3389/fneur.2020.00288
5. Dong H, Li J, Huang L, et al. Serum microRNA profiles serve as novel biomarkers for the diagnosis of Alzheimer’s Disease. Dis Markers. 2015;2015:625659. doi:10.1155/2015/625659
6. Wei W, Wang ZY, Ma LN, Zhang TT, Cao Y, Li H. MicroRNAs in Alzheimer’s disease: function and potential applications as diagnostic biomarkers. Front Mol Neurosci. 2020;13:160. doi:10.3389/fnmol.2020.00160
7. Wang R, Zhang J. Clinical significance of miR-433 in the diagnosis of Alzheimer’s disease and its effect on Abeta-induced neurotoxicity by regulating JAK2. Exp Gerontol. 2020;141:111080. doi:10.1016/j.exger.2020.111080
8. Yang Q, Zhao Q, Yin Y. miR-133b is a potential diagnostic biomarker for Alzheimer’s disease and has a neuroprotective role. Exp Ther Med. 2019;18(4):2711–2718. doi:10.3892/etm.2019.7855
9. Angelucci F, Cechova K, Valis M, Kuca K, Zhang B, Hort J. MicroRNAs in Alzheimer’s disease: diagnostic markers or therapeutic agents? Front Pharmacol. 2019;10:665. doi:10.3389/fphar.2019.00665
10. Martinez B, Peplow PV. MicroRNAs as diagnostic and therapeutic tools for Alzheimer’s disease: advances and limitations. Neural Regen Res. 2019;14(2):242–255. doi:10.4103/1673-5374.244784
11. Lukiw WJ. Micro-RNA speciation in fetal, adult and Alzheimer’s disease hippocampus. Neuroreport. 2007;18(3):297–300. doi:10.1097/WNR.0b013e3280148e8b
12. Geng L, Zhang T, Liu W, Chen Y. Inhibition of miR-128 abates abeta-mediated cytotoxicity by targeting PPAR-gamma via NF-kappaB inactivation in primary mouse cortical neurons and neuro2a cells. Yonsei Med J. 2018;59(9):1096–1106. doi:10.3349/ymj.2018.59.9.1096
13. Liu Y, Zhang Y, Liu P, et al. MicroRNA-128 knockout inhibits the development of Alzheimer’s disease by targeting PPARgamma in mouse models. Eur J Pharmacol. 2019;843:134–144. doi:10.1016/j.ejphar.2018.11.004
14. McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM. Clinical diagnosis of Alzheimer’s disease: report of the NINCDS-ADRDA Work Group under the auspices of Department of Health and Human Services Task Force on Alzheimer’s Disease. Neurology. 1984;34(7):939–944. doi:10.1212/wnl.34.7.939
15. van der Kant R, Goldstein LSB, Ossenkoppele R. Amyloid-beta-independent regulators of tau pathology in Alzheimer disease. Nat Rev Neurosci. 2020;21(1):21–35. doi:10.1038/s41583-019-0240-3
16. Wei S, Peng W, Mai Y, et al. Outer membrane vesicles enhance tau phosphorylation and contribute to cognitive impairment. J Cell Physiol. 2020;235(5):4843–4855. doi:10.1002/jcp.29362
17. Yoo SM, Park J, Kim SH, Jung YK. Emerging perspectives on mitochondrial dysfunction and inflammation in Alzheimer’s disease. BMB Rep. 2020;53(1):35–46. doi:10.5483/BMBRep.2020.53.1.274
18. Amidfar M, de Oliveira J, Kucharska E, Budni J, Kim YK. The role of CREB and BDNF in neurobiology and treatment of Alzheimer’s disease. Life Sci. 2020;257:118020. doi:10.1016/j.lfs.2020.118020
19. Bello-Medina PC, Gonzalez-Franco DA, Vargas-Rodriguez I, Diaz-Cintra S. Oxidative stress, the immune response, synaptic plasticity, and cognition in transgenic models of Alzheimer disease. Neurologia. 2019. doi:10.1016/j.nrl.2019.06.002
20. Fransquet PD, Ryan J. Micro RNA as a potential blood-based epigenetic biomarker for Alzheimer’s disease. Clin Biochem. 2018;58:5–14. doi:10.1016/j.clinbiochem.2018.05.020
21. Qu C, Yan C, Cao W, et al. miR-128-3p contributes to mitochondrial dysfunction and induces apoptosis in glioma cells via targeting pyruvate dehydrogenase kinase 1. IUBMB Life. 2020;72(3):465–475. doi:10.1002/iub.2212
22. Durazzo TC, Mattsson N, Weiner MW. Alzheimer’s Disease Neuroimaging Initiative. Smoking and increased Alzheimer’s disease risk: a review of potential mechanisms. Alzheimers Dement. 2014;10(3 Suppl):S122–145. doi:10.1016/j.jalz.2014.04.009
23. Lee WJ, Liao YC, Wang YF, Lin YS, Wang SJ, Fuh JL. Summative effects of vascular risk factors on the progression of alzheimer disease. J Am Geriatr Soc. 2020;68(1):129–136. doi:10.1111/jgs.16181
24. Zhou Z, Liang Y, Zhang X, et al. Low-density lipoprotein cholesterol and Alzheimer’s disease: a systematic review and meta-analysis. Front Aging Neurosci. 2020;12:5. doi:10.3389/fnagi.2020.00005
25. Pereira CF, Santos AE, Moreira PI, et al. Is Alzheimer’s disease an inflammasomopathy? Ageing Res Rev. 2019;56:100966. doi:10.1016/j.arr.2019.100966
26. Sinyor B, Mineo J, Ochner C. Alzheimer’s disease, inflammation, and the role of antioxidants. J Alzheimers Dis Rep. 2020;4(1):175–183. doi:10.3233/ADR-200171
27. Wang L, Wang K, Tian Z. miR-128-3p inhibits NRP1 expression and promotes inflammatory response to acute kidney injury in sepsis. Inflammation. 2020;43(5):1772–1779. doi:10.1007/s10753-020-01251-8
28. Wu L, Zhang G, Guo C, Zhao X, Shen D, Yang N. MiR-128-3p mediates TNF-α-induced inflammatory responses by regulating Sirt1 expression in bone marrow mesenchymal stem cell. Biochem Biophys Res Commun. 2020;521(1):98–105. doi:10.1016/j.bbrc.2019.10.083
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


