Back to Journals » Clinical Ophthalmology » Volume 9
Serial bevacizumab injections and laser photocoagulation for macular edema associated with a retinal artery macroaneurysm
Authors Leung E, Reddy A, Vedula A, Flynn Jr H ![]()
Received 7 January 2015
Accepted for publication 10 February 2015
Published 4 April 2015 Volume 2015:9 Pages 601—609
DOI https://doi.org/10.2147/OPTH.S80504
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Ella H Leung,1 Ashvini K Reddy,2 Anil S Vedula,1 Harry W Flynn Jr1
1Department of Ophthalmology, Bascom Palmer Eye Institute, University of Miami, Miami, FL, 2Department of Ophthalmology, University of Virginia, Charlottesville, VA, USA
Abstract: An 84-year-old female with a history of hypertension and dyslipidemia was referred for a retinal artery macroaneurysm with exudation that had extended into the macula. She underwent a total of six injections of bevacizumab, with some improvement in visual acuity and retinal thickness. Due to persistent macular edema, focal laser photocoagulation was performed around the macroaneurysm. The vision remained at 20/30 during 20 months of follow up. Although anti-vascular endothelial growth factor therapy may improve vision and decrease retinal thickness in retinal artery macroaneurysm, recalcitrant cases may be treated with laser photocoagulation to seal the leaking vessel.
Keywords: bevacizumab, laser, retinal artery macroaneurysm
Introduction
Retinal artery macroaneurysms (RAMs) are rare, acquired dilatations of the retinal arterial vasculature, usually within the first three branches of the arteriolar tree.1 The incidence is estimated to be approximately 1 in 4,500 people over the age of 40.2 Hypertension and older age lead to hyaline degeneration of the vascular walls, loss of autoregulatory tone and elastic recoil, and arterial dilatation.3
Approximately 8%–25% of RAMs will undergo spontaneous involution. Even with submacular hemorrhage, up to 37% of patients will have better than 20/40 visual acuity without treatment.4 However one third of patients will develop vascular leakage and retinal edema and may need treatment.5
Case report
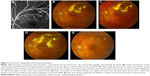
An 84-year-old female with a past medical history of hypertension and dyslipidemia was referred for progressively decreasing visual acuity in the left eye. She had no history of diabetes. On initial examination, her visual acuity was 20/30 in both eyes. Dilated fundus examination and fluorescein angiography of the left eye revealed a superotemporal retinal arterial macroaneurysm, with surrounding circinate exudates involving the fovea (Figures 1 and 2). The right eye was normal.
The patient was observed initially, but the edema increased and her vision deteriorated to 20/60. An intravitreal injection of 1.25 mg of bevacizumab improved the vision to 20/30. The patient was observed for 3 months, but the vision worsened again to 20/60, with increased edema and exudates on optical coherence tomography. She was observed for 3 months, but due to recurrent leakage, she ultimately received a total of six injections of intravitreal bevacizumab every 1 month to 3 months. Her vision gradually improved back to 20/30.
Fourteen months after initial presentation, her vision deteriorated again to 20/60. The decision was made to perform laser photocoagulation around the macroaneurysm. Argon laser at a setting of 400 mW and 200 μm spot size was applied around the RAM. The RAM occluded, and on follow-up examination 6 months later, the patient’s vision has remained at 20/30.
Discussion
The first report of laser photocoagulation to treat exudative retinal artery macroaneurysm was published in 1976 by Dr Donald Gass and colleagues.6 In a study of 27 patients with symptomatic RAM, half of the patients underwent argon laser therapy and the remaining half was observed. The vision in both groups improved, but the laser group experienced a greater gain.7 Approximately 16%–27% of RAMs occlude with lasers, but there is a risk of vascular occlusion, early increase in exudates from selective reabsorption of fluid, arteriovenous shunts, macular pucker, and scotomas.7,8 Other treatment options for RAMs include yellow dye laser and indocyanine green dye-enhanced photocoagulation.9,10
Anti-vascular endothelial growth factor (VEGF) therapy has recently been reported in the treatment of patients with exudative or hemorrhagic RAMs. Chanana and Azad11 published the first case report in 2009, and subsequent case reports have shown encouraging results (Table 1).12–19 Cho et al18 described 23 patients with RAMs who were either observed or received intravitreal bevacizumab. Both groups experienced statistically significant improvements in visual acuity and central macular thickness, but the bevacizumab group regained vision faster. A larger, prospective study of 38 eyes with hemorrhagic and exudative RAMs underwent three monthly injections of bevacizumab, with the vision and retinal thickness improving in both groups.19
  | Table 1 Literature review of anti-VEGF use in the treatment of retinal artery macroaneurysms |
The role of VEGF and the mechanism of action of anti-VEGF therapy in RAMs are not fully understood. In a study that compared the VEGF levels in 500 μL vitreous samples from patients with vitreous hemorrhage from nondiabetic etiologies (including four patients with RAM) with those from patients with proliferative diabetic retinopathy, the VEGF levels were significantly lower in the former than in the latter groups (2.75 pg/mL vs 821 pg/mL, respectively).20 However, these were small vitreous samples obtained up to 3 weeks after the initial hemorrhage and may not have been representative of the vitreous and microenvironment around the RAM.
The role of VEGF in intracranial aneurysms and other biological systems has been more clearly elucidated. In intracranial aneurysms, VEGF levels were found to be significantly higher than the levels in controls.20 In particular, patients with intracranial aneurysms had higher expressions of VEGF receptor 2 (VEGFR2) and lower levels of VEGF receptor 1 (VEGFR1). VEGFR1 is associated with angiogenesis, while VEGFR2 is associated with thrombosis.21 Bevacizumab has been shown to decrease VEGFR1 levels and to increase VEGFR2 levels to normal levels in cancer cells.22 In the circulatory system, platelets produce VEGF, which stimulates nitrous oxide production, resulting in vasodilation.21 Inhibition of VEGF may decrease leakage of fluid and exudates through the endothelium. In mice studies, bevacizumab decreases bleeding time and increases coagulation.23 Thus, VEGF inhibition may block angiogenesis, decrease binding of the prothrombotic VEGFR2, and decrease vascular permeability.
In conclusion, the majority of RAMs can be observed, but intervention may be necessary in cases of persistent or recurrent macular edema from exudative or hemorrhagic RAMs. Our patient’s RAM was initially observed, but continued leakage prompted further therapy.
Anti-VEGF injections have shown promise in improving visual acuity and hastening resolution of macular edema in RAM;5 however, most of the previously published cases had relatively short follow-up. Our case has one of the longest follow-ups with the most number of anti-VEGF treatments, but the patient continued to have leakage into the macula. The potential benefits of anti-VEGF treatment must be carefully weighed against the potential risk of infection from serial injections. Laser photocoagulation remains a viable treatment option in cases of macular edema secondary to RAM.
Disclosure
The authors report no conflicts of interest in this work.
References
Lavin MJ, Marsh RJ, Peart S, Rehman A. Retinal arterial macroaneurysms: a retrospective study of 40 patients. Br J Ophthalmol. 1987;71(11):817–825. | ||
Xu L, Wang Y, Jonas JB. Frequency of retinal macroaneurysms in adult Chinese: the Beijing eye study. Br J Ophthalmol. 2007;91(6):840–841. | ||
Fichte C, Streeten BW, Friedman AH. A histopathologic study of retinal arterial aneurysms. Am J Ophthalmol. 1978;85(4):509–518. | ||
McCabe CM, Flynn HW Jr, McLean WC, et al. Nonsurgical management of macular hemorrhage secondary to retinal artery macroaneurysms. Arch Ophthaolmol. 2000;118(6):780–785. | ||
Rabb MF, Galiano DA, Tske MP. Retinal arterial macroaneurysms. Surv Ophthalmol. 1988;33(2):73–96. | ||
Lewis RA, Norton EW, Gass JD. Acquired arterial macroaneurysms of the retina. Br J Ophthalmol. 1976;60(1):21–30. | ||
Meyer JC, Ahmad BU, Blinder KJ, Shah GK. Laser therapy versus observation for symptomatic retinal artery macroaneurysms. Graefes Arch Clin Exp Ophthalmol. Epub 2014 Jul 13. | ||
Brown DM, Sobol WM, Folk JC, Weingeist TA. Retinal arterial macroaneurysm: long term visual outcome. Br J Ophthalmol. 1994;78:534–538. | ||
Russell SR, Folk JC. Branch retinal artery occlusion after dye yellow photocoagulation of an arterial macroaneurysm. Am J Ophthalmol. 1987;104(2):186–187. | ||
Steigerwalt RD Jr, Pascarella A, Arrico L, et al. Idiopathic juxtafoveal retinal telangiectasis and retinal macroaneurysm treated with indocyanine green dye-enhanced photocoagulation. Panminerva Med. 2012;54(1 suppl 4):93–96. | ||
Chanana B, Azad RV. Intravitreal bevacizumab for macular edema secondary to retinal arterial macroaneurysm. Eye (Lond). 2009;23(2):493–494. | ||
Jonas JB, Schmidbauer M. Intravitreal bevacizumab for retinal macroaneurysm. Acta Ophthalmol. 2010;88(7):e284. | ||
Javey G, Moshfeghi AN, Moshfeghi AA. Management of ruptured retinal arterial macroaneurysm with intravitreal bevacizumab. Ophthalmic Surg Lasers Imaging. 2010;41(4):1–5. | ||
Wenkstern AR, Petersen H. Intravitreal ranibizumab in retinal macroaneurysm. Graefes Arch Clin Exp Ophthalmol. 2010;248(11):1667–1670. | ||
Golan S, Golderberg D, Goldstein M. Long-term follow-up of intravitreal bevacizumab in retinal arterial macroaneurysm: a case report. Case Rep Ophthalmol. 2011;2(3):387–391. | ||
Tsakpinis D, Nasr MB, Tranos P, et al. The use of bevacizumab in a multilevel retinal hemorrhage secondary to retinal macroaneurysm: a 39-month follow-up case report. Clin Ophthalmol. 2011;5:1475–1477. | ||
Zweifel SA, Tonz MS, Pfenninger L, Becker M, Michels S. Intravitreal anti-VEGF therapy for retinal macroaneurysm. Klin Monbl Augenheilkd. 2013;230(4):392–395. | ||
Cho HJ, Rhee TK, Kim HS, et al. Intravitreal bevacizumab for symptomatic retinal arterial macroaneurysm. Am J Ophthalmol. 2013;155(5):898–904. | ||
Pichi F, Morara M, Torrazza C, et al. Intravitreal bevacizumab for macular complications from retinal arterial macroaneurysms. Am J Ophthalmol. 2013;155(2):287.e–294.e. | ||
Shirasawa M, Arimura N, Otsuka H, Sonoda S, Hashiguchi T, Sakamoto T. Intravitreous VEGF-A in eyes with massive vitreous hemorrhage. Graefes Arch Clin Exp Ophthalmol. 2011;249(12):1805–1810. | ||
Maderna E, Corsini E, Franzini A, et al. Expression of vascular endothelial growth factor receptor-1/-2 and nitric oxide in unruptured intracranial aneurysms. Neurol Sci. 2010;31(5):617–623. | ||
Zhang Z, Neiva KG, Lingen MW, Ellis LM, Nor JE. VEGF-dependent tumor angiogenesis requires inverse and reciprocal regulation of VEGFR1 and VEGFR2. Cell Death Differ. 2010;17(3):499–512. | ||
Liu X, Hao L, Zhang S, et al. Genetic repression of mouse VEGF expression regulates coagulation cascade. IUBMB Life. 2010;62(11):819–824. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.