Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 12
Sarcopenia and type 2 diabetes mellitus: a bidirectional relationship
Authors Mesinovic J , Zengin A , De Courten B, Ebeling PR, Scott D
Received 8 March 2019
Accepted for publication 7 May 2019
Published 8 July 2019 Volume 2019:12 Pages 1057—1072
DOI https://doi.org/10.2147/DMSO.S186600
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Antonio Brunetti
Jakub Mesinovic,1 Ayse Zengin,1 Barbora De Courten,2 Peter R Ebeling,1,3 David Scott,1,3
1Department of Medicine, School of Clinical Sciences at Monash Health, Faculty of Medicine, Nursing and Health Sciences, Monash University, Clayton, Melbourne, VIC, Australia; 2Monash Centre for Health Research and Implementation, School of Public Health and Preventive Medicine, Monash University, Clayton, Melbourne, VIC, Australia; 3Australian Institute for Musculoskeletal Science (AIMSS), Department of Medicine - Western Health, Melbourne Medical School, The University of Melbourne, St Albans, Melbourne, VIC, Australia
Abstract: The incidence and prevalence of metabolic and musculoskeletal diseases are increasing. Type 2 diabetes mellitus (T2DM) is characterized by insulin resistance, inflammation, advanced glycation end-product accumulation and increased oxidative stress. These characteristics can negatively affect various aspects of muscle health, including muscle mass, strength, quality and function through impairments in protein metabolism, vascular and mitochondrial dysfunction, and cell death. Sarcopenia is a term used to describe the age-related loss in skeletal muscle mass and function and has been implicated as both a cause and consequence of T2DM. Sarcopenia may contribute to the development and progression of T2DM through altered glucose disposal due to low muscle mass, and also increased localized inflammation, which can arise through inter- and intramuscular adipose tissue accumulation. Lifestyle modifications are important for improving and maintaining mobility and metabolic health in individuals with T2DM and sarcopenia. However, evidence for the most effective and feasible exercise and dietary interventions in this population is lacking. In this review, we discuss the current literature highlighting the bidirectional relationship between T2DM and sarcopenia, highlight current research gaps and treatments, and provide recommendations for future research.
Keywords: type 2 diabetes mellitus, sarcopenia, metabolic health, muscle health, obesity
Introduction
In 2017, it was estimated that 451 million adults globally had diabetes.1 Approximately 90% of these individuals have type 2 diabetes mellitus (T2DM),2 with the highest prevalence observed in older adults.3 As populations age, incidence and prevalence of metabolic and musculoskeletal diseases increase.1,4 Body composition changes during aging, resulting in significant losses of skeletal muscle mass and increased body fat percentage.5 Collectively and independently, low muscle mass and adiposity are associated with higher incidence of metabolic disorders, including T2DM.6,7 “Sarcopenia” describes age-related declines in muscle mass and function8–12 and has been implicated as both a cause and consequence of T2DM.13 T2DM is characterized by insulin resistance, increased advanced glycation end-products (AGEs), a proinflammatory phenotype and oxidative stress, which can lead to micro- and macro-vascular complications. These characteristics can interfere with normal cellular functioning and cause cell death14, which may lead to losses in skeletal muscle mass, strength, and function, potentially leading to the development of sarcopenia. Conversely, low muscle mass and function in sarcopenia can lead to poorer glucose disposal and decreased metabolic rate and physical activity, all of which may place older adults with sarcopenia at increased risk for developing T2DM.
Type 2 diabetes mellitus and sarcopenia
Currently, there is no consensus definition of sarcopenia; however, several definitions and criteria for diagnosis have been proposed, some of which are presented in Table 1. The most commonly used multi-component operational definition since 2010 is the European Working Group on Sarcopenia in Older People (EWGSOP) definition,8 which has recently been revised.9 The Asian Working Group for Sarcopenia (AWGS) definition12 was derived from the EWGSOP definition but provides appropriate criteria for Asian populations. The International Working Group on Sarcopenia (IWGS)11 definition is similar to the EWGSOP definition, but includes only low muscle mass and physical performance, not low strength. The only group to use statistical procedures to identify criteria for sarcopenia (low lean mass and handgrip strength), rather than expert consensus, is the Foundation for the National Institutes of Health Biomarkers Consortium Sarcopenia Project (FNIH).10 Unsurprisingly, the different approaches taken to develop sarcopenia definitions results in poor agreement between them.
 |
Table 1 Comparison of current definitions of sarcopenia |
Recent meta-analyses indicate sarcopenia prevalence ranges from 10% to 40% in healthy men and women aged ≥60, and this variability is influenced by the operational definition applied and population assessed.15,16 Our understanding of associations between sarcopenia and T2DM is similarly limited by lack of consistency in definitions applied. However, older adults with T2DM do appear to have an increased risk for sarcopenia. The prevalence of sarcopenia in Japanese and Chinese adults (aged ≥65 and >60 years, respectively) with T2DM is 15% using the AWGS definition.17,18 In the Korean Sarcopenic Obesity Study, individuals with T2DM had threefold higher odds of having low skeletal muscle mass relative to weight compared with non-diabetic controls after adjusting for multiple confounders.19 In the Health ABC Study (n=2,675), older women with undiagnosed and confirmed T2DM demonstrated greater losses in thigh muscle cross-sectional area over five years compared with non-diabetic controls (−10.6±1.5 and −9.3±1.2 versus −5.2±0.4 cm2, respectively).20 Interestingly, the English Longitudinal Study of Ageing including 3,404 older adults recently demonstrated that diabetes predicted low handgrip strength eight years later in men (OR: 2.43 [95%CI: 1.5–3.95]), but not women (OR: 1.49 [95%CI: 0.83–2.68]), based on FNIH cut-points.21
In addition to the risk of sarcopenia being increased in T2DM patients, older adults with sarcopenia may have increased risk of developing T2DM. In 113,913 Korean men and 89,854 women (mean age of 40 years), individuals in the lowest skeletal muscle mass relative to body weight quartiles had a twofold greater risk of developing T2DM compared with individuals in the highest quartile.6 Additionally, the Korean Genome Epidemiology Study in 6,895 adults (mean age of 52 years) showed that individuals in the lowest muscle mass index tertile (defined by weight-adjusted appendicular lean mass [ALM]) had twofold higher odds of incident T2DM after adjusting for confounders.22 Furthermore, comorbid presence of obesity and low muscle mass conferred even greater risk of incident T2DM in this population.22 Lower hand grip strength normalized to body weight was also predictive of elevated fasting glucose (>5.56 mmol/L or treatment with glucose-lowering drugs) in 17,703 Chinese men and women aged over 40 years.23
Muscle deficits may affect metabolic health through altered glucose disposal, as skeletal muscle accounts for ~80% of glucose clearance during euglycemic and hyperinsulinemic conditions.24 Therefore, greater quantities of muscle increase glucose disposal and potentially delay the onset of T2DM. Once established, however, T2DM leads to various pathophysiological manifestations that have bidirectional relationships with components of sarcopenia.
Insulin resistance
Insulin resistance is a hallmark of T2DM that results in poor glycemic control, which potentially affects components of sarcopenia. In the MrOS study, men aged ≥65 years without T2DM but in the highest quartile for insulin resistance had two-fold higher odds of losing ≥5% total lean mass over approximately five years.25 In the NHANES study, gait speed decreased across increasing quartiles of insulin resistance in non-diabetic older men, but not women.26 Conversely, in 968 Italian men and women with a mean age of 67 and 68 years, respectively, insulin resistance was negatively associated with handgrip strength normalized to BMI in women, but not men.27 Thus, insulin resistance may be a predictor of poor muscle health, irrespective of diabetes status, although further research is required to clarify sex-specific associations of insulin resistance and components of sarcopenia.
Glycated hemoglobin (HbA1c) is a measure of long-term glycemic control.28 In older Korean men aged ≥65 years with T2DM, poor glycemic control (HbA1c ≥8.5%) was associated with poor lower-limb muscle quality and physical performance.29 Similar associations have been reported for Caucasian and Black individuals; in the Baltimore Longitudinal Study of Ageing, knee extensor strength was lower across increasing quartiles of HbA1c.30 Interestingly, total body and leg lean mass remained the same across all quartiles of HbA1c in adjusted models that included body weight as a covariate. However, this is a potential over-adjustment and could explain the lack of association between HbA1c and lean mass, despite the relationship with muscle strength.30 Loss of muscle strength and mass in individuals with poor glycemic control likely occurs due to increased protein degradation31 and decreased protein synthesis32 Impaired protein metabolism is therefore exacerbated in individuals with T2DM, and particularly in individuals with undiagnosed T2DM, who typically have greater glucose variability. The negative effects of poor glycemic control on muscle health are compounded as it often occurs alongside other adverse characteristics of T2DM, including inflammation.
Inflammation
T2DM is associated with chronic, low-grade systemic inflammation which may negatively affect glucose and muscle homeostasis.33–35 Inflammatory markers including interleukin-6 (IL-6), tumor necrosis factor-alpha (TNF-α) and C-reactive protein (CRP) are often elevated in individuals with T2DM.36,37 These inflammatory markers are associated with adiposity and insulin resistance38 and are elevated in obese and non-obese individuals with T2DM36 Visceral adipose tissue (VAT) secretes IL-6 and TNF-α,39 and it is therefore likely to be a major contributor to inflammation in T2DM. We recently demonstrated that waist circumference (an indirect measure of VAT) was negatively associated with muscle strength, quality, and performance in 84 overweight and obese older adults.40 However, it is unclear whether these negative associations were driven in part by increased inflammation.
Interestingly, IL-6 is also produced by myocytes during exercise, and transient increases in IL-6 assist in nutrient mobilization and muscle hypertrophy.41–43 Contrary to this, IL-6 has been reported to cause muscle atrophy when localized to the tibialis anterior of Sprague-Dawley rats, independent of systemic inflammation.35 In the Framingham Heart Study consisting of 558 older adults aged 72–92 years, IL-6 predicted two-year lean mass losses in women, but not men.44 In 115 older adults aged >60 years, ALM loss over five years was fivefold and fourfold greater in individuals with IL-6 and CRP concentrations in the top tertile of the cohort, respectively.45 Park et al demonstrated that older adults with T2DM had greater losses in leg muscle mass and strength over three years compared with non-diabetic controls, and these associations were partially attenuated after adjusting for cytokines including IL-6 and TNF-α.46
In addition to being negatively associated with muscle mass, inflammatory markers are also negatively associated with muscle strength, which is now considered the principal component of sarcopenia.9 Visser et al reported that in 2,746 generally well-functioning Black and Caucasian men and women from the USA aged 70–79 years, handgrip strength was between 1.1 and 2.4 kg lower per standard deviation increase in IL-6 concentration.47 TNF-α was negatively associated with grip strength in Black and Caucasian women, but not men.47 In the English Longitudinal Study of Ageing, CRP was negatively associated with handgrip strength in women, and chair stand time in both sexes.48 Taken together, inflammation associated with T2DM may independently affect muscle mass and strength.
Oxidative stress
Aging is associated with reduced antioxidant capacity, which has been implicated in the pathogenesis of sarcopenia.49 T2DM is also associated with increased oxidative stress,50 which can lead to myopathy. Oxidative stress in T2DM can occur through dyslipidemia and altered lipid metabolism, insulin resistance, increased AGEs and mitochondrial dysfunction.50 In diabetic rats, increased oxidative stress impairs muscle repair.51 In 107 pre- and post-menopausal women increased oxidative stress(measured by lipid peroxide concentrations) was negatively associated with skeletal muscle mass adjusted for height (SMI).52 Given that oxidative stress also has the capacity to impair satellite cell differentiation and damage DNA,53 it is evident that myopathy in T2DM is caused by the disruption of numerous cellular pathways, and further research is required to clarify how they work, and determine whether they are perhaps suitable targets for interventions.
Another age- and T2DM-related factor implicated in the progression of metabolic and muscle health deterioration through oxidative stress is mitochondrial dysfunction.54,55 Older individuals have up to 50% lower oxidative capacity per unit of muscle56 and increased mitochondrial DNA mutations57 compared with younger adults. Interestingly, when compared with BMI-matched controls, individuals with T2DM had a 45% lower phosphocreatine recovery half-time (a measure of mitochondrial function) immediately after exercise.58 Furthermore, this study also reported that fasting plasma glucose and HbA1c were positively associated with phosphocreatine recovery half-time (r=0.42 and r=0.48, respectively).58 Impairments in oxidative capacity lead to decreased metabolism of macronutrients, and, more importantly, poorer physical performance. Interestingly, T2DM has intergenerational effects on mitochondria; young, lean offspring of individuals with T2DM had 38% lower skeletal muscle mitochondrial density compared with insulin-sensitive offspring from non-diabetic parents.59 Additional studies investigating links between T2DM, sarcopenia and mitochondrial dysfunction in humans are required given the important role of mitochondria in muscle function and metabolism.
Advanced glycation end-products
Non-enzymatic reactions between glucose and amino groups in proteins, lipids, and nucleic acids can lead to the formation of AGEs.60 AGEs are positivity associated with insulin resistance, obesity, and age.61,62 Currently it is unclear how AGEs contribute to poor muscle health; however, it has been proposed that AGE-associated muscle weakness arises through increased protein cross-linking within muscle, thereby interfering with contractility, and also increasing inflammation and oxidative stress.14,6161 Indeed, AGE concentrations within skeletal muscle increase across the lifespan.61 Skin autofluorescence is a common, surrogate measure of AGEs, which is representative of long-term glycemic control.63 Skin autofluorescence was higher (indicating higher AGEs) in a cross-sectional study of 166 Japanese adults (mean age of 63 years) with T2DM and sarcopenia when compared with non-sarcopenic T2DM controls, and was associated with low muscle strength and total body lean mass.64 Another study in 232 Japanese adult men reported that higher skin autofluorescence was associated with lower hand grip strength and leg extension power.65 In 9,203 Japanese men and women with a mean age of 58 years, SMI was inversely correlated with skin autofluorescence.66 Furthermore, in a subpopulation of this study consisting of 1,934 participants aged >60 years, skin autofluorescence was negatively associated with grip and hip flexion and abduction strength.66 Currently, reliability of skin autofluorescence as a proxy for AGE concentrations is questionable due to measurement variability associated with factors including skin pigmentation, presence of body creams and changes in blood flow.67,68 Nevertheless, skin autofluorescence is a quick, non-invasive measurement, and there is some evidence of a link between poor metabolic and muscle health through AGE accumulation within skeletal muscle. However, longitudinal studies assessing the effect of AGEs on components of sarcopenia using more robust measures of AGE concentrations (tissue biopsy and serum/urinary samples) are required.
Vascular complications
Micro- and macrovascular complications of T2DM result from chronic hyperglycemia, AGE accumulation, inflammation, and oxidative stress and have the capacity in their own right to affect skeletal muscle.69,70 Healthy vasculature is crucial for the transfer of nutrients, removal of waste products and oxygenation of tissues, including skeletal muscle. Micro- and macrovascular complications are strongly interconnected in T2DM.
Microvascular complications
Neuropathy, retinopathy, and nephropathy are common microvascular complications in T2DM. Damaged nerve cells innervating skeletal muscle can impair muscle contractility, resulting in reduced muscle strength. A recent study reported that in men and women aged >50 years with T2DM, individuals with neuropathy had lower knee extension strength relative to body weight compared to individuals without neuropathy.71 In addition to impairing muscle strength, nerve damage also causes muscle atrophy.72 Both of these muscle impairments contribute to poor physical performance. In support, a cross-sectional analysis of the Health ABC study including 2,364 older adults (aged 73–82 years) demonstrated that poor peripheral nerve function was independently associated with poor physical performance outcomes including Short Physical Performance Battery (SPPB) scores, gait speed and standing balance ratio.73 In the same study, individuals with T2DM also had poorer physical performance when compared with controls, and although adjusting for peripheral nerve function attenuated the relationship between T2DM and physical performance measures, it still remained significant.73 Thus, neuropathy is one of the various T2DM complications that contributes to poor muscle health and ultimately, sarcopenia.
Although diabetic retinopathy does not appear to inherently affect muscle function, it can affect vision, which is a key component of balance. Balance is important for both locomotion and physical performance. Unsurprisingly, impaired vision in T2DM contributes to increased falls risk.74 In a cross-sectional analysis of the Singapore Epidemiology of Eye Diseases Study (n=9,481, aged 40–80 years), adults with T2DM and diabetic retinopathy had higher odds (OR:1.31 [95%CI:1.07–1.60]) of falling compared to individuals without diabetes in a fully adjusted model.74 Additionally, individuals with diabetes and mild (OR:1.81 [95%CI:1.23–2.67]) and moderate (OR:1.89 [95%CI:1.16–3.07]) non-proliferative diabetic retinopathy had increased falls risk when compared to individuals that had diabetes without diabetic retinopathy.74 Falls have an enormous economic burden75 and they contribute to a large proportion of global injury-related deaths.76 There are very few studies that have explored the relationship between diabetic retinopathy and sarcopenia; however, a small cross-sectional study in 316 Japanese adults with T2DM (aged >20 years) reported that diabetic retinopathy increased odds for prevalent sarcopenia (OR:7.78 [95%CI:1.52–39.81]) and low muscle strength (OR:6.25 [95%CI:1.15–33.96]) and was negatively associated with muscle quality defined by hand grip strength relative to SMI (ß=−0.136; P=0.005).77 Due to the small sample size of this study, there is insufficient evidence to conclude that there is a definitive relationship between diabetic retinopathy and sarcopenia. Further studies in large T2DM and sarcopenic populations that include measures of diabetic retinopathy are required.
Diabetic nephropathy causes chronic kidney disease (CKD),78 which contributes to muscle wasting.79 In 387 older Asians (mean age 68 years) with T2DM, diabetic nephropathy was associated with 2.5-fold (95%CI:1.35–5.13) higher odds of prevalent sarcopenia defined by AWGS criteria.80 Sarcopenia prevalence has been reported to increase with CKD severity81 and depending on the definition utilized, also predicts mortality in CKD patients.82 Pathophysiological mechanisms that are thought to contribute to sarcopenia in CKD include increased inflammation and protein loss, reduced vitamin D synthesis, mitochondrial dysfunction, and metabolic acidosis.79 In 100 CKD patients not on dialysis, high sensitivity CRP was associated with ALM/BMI (r=−0.268).81 In another study of 148 adult CKD patients (aged ≥18 years) not on dialysis, glomerular filtration rate was positively associated with lean mass, appendicular SMI and ALM.83 In addition to losses in muscle mass, respiratory capacity of muscle also appears to be lower in CKD, which could further contribute to development and/or progression of sarcopenia. Muscle biopsies taken in a cohort of adults with stage 5 CKD patients demonstrated that mitochondrial volume density is lower in individuals with CKD compared with non-CKD controls.84 Targeting muscle mass and mitochondrial biogenesis may improve mortality rates in this population.
Macrovascular complications
A key macrovascular complication in T2DM is atherosclerosis. Atherosclerosis appears to progress faster in individuals with T2DM, as it is exacerbated by poor metabolic health.85 Additionally, chronic hyperglycemia inhibits nitric oxide-mediated vasodilation through increased oxidative stress, AGE accumulation, and direct actions on endothelial nitric oxide synthase.86 Both of these complications increase the risk for hypertension, which can lead to end organ damage.87 In 365 hypertensive Turkish adults aged >18 years without T2DM, skeletal muscle mass was negatively associated with hypertensive retinopathy, a measure of end organ damage, in both adults and older adults.88 However, in this same study, SMI was not associated with hypertensive end organ damage. It is plausible that hypertension can damage myocytes; however, there is also evidence that suggests muscle mass can influence blood pressure. A recent study demonstrated that increased muscle mass induced via myostatin knockout leads to reduced systolic and diastolic blood pressure and mean arterial pressure in an obese mouse model (db/db), independent of adiposity and body weight.89 The positive effects of increased muscle mass on blood pressure were thought to be due to improved renal function resulting from metabolic improvements attributed to increased muscle mass. It is possible that increased muscle mass would confer similar vascular benefits in humans; however, this is difficult to determine given that muscle mass is currently increased in humans primarily through exercise. Hence, it is unclear whether increases in muscle mass, or other beneficial effects of exercise are improving vascular health, although both are likely to contribute. Nevertheless, interventions targeting muscle hypertrophy may have the additional benefit of improving vascular health.
Peripheral artery disease (PAD) is another macrovascular complication associated with T2DM that affects up to a quarter of diabetes patients.90 PAD measured using ankle-brachial index (an indirect, non-invasive measure of PAD) has been associated with lower hip extension and knee and hip flexion strength in older adults.70 It has also been reported that older adults with PAD have slower gait speed compared to controls without PAD.91 Reduced blood flow in PAD can result in ischemia, leading to poorer muscle strength, mass and performance outcomes.92 Also, PAD can lead to reduced physical activity and exercise due to the pain associated with this complication, which may further contribute to poor muscle health outcomes. Further studies investigating the relationship between micro- and macrovascular complications and sarcopenia outcomes including muscle composition and function are required in T2DM populations.
IMAT and T2DM
Muscle quality is an underappreciated component of sarcopenia.9 Parallel to muscle loss with aging, numerous neuromuscular changes contribute significantly to reduced force-production capacity, including inter- and intra-muscular adipose tissue (IMAT). IMAT is an ectopic fat depot associated with poor metabolic93 and muscle health outcomes.94,95 Obese and T2DM individuals have greater amounts of thigh IMAT compared with lean controls, and IMAT is associated with insulin sensitivity.96 In overweight and obese non-diabetic adults, calf IMAT was negatively associated with insulin sensitivity in both men (r = −0.40) and women (r = −0.43) using gold-standard MRI and glucose clamp techniques.93 In comparison, subcutaneous adipose tissue, a considerably larger fat depot, does not appear to predict insulin sensitivity.96 In a cross-sectional analysis of the Look AHEAD study (n=183), overweight and obese men and women with T2DM had greater IMAT at higher levels of total-body adiposity when compared with non-diabetic overweight and obese controls.97 In addition to influencing insulin sensitivity, various studies have reported that IMAT is an independent predictor of physical function94,95 and falls risk.98,99 In fact, IMAT is a stronger predictor of mobility function in older adults than lean mass.95 In a cross-sectional study (n=79), obese adults with T2DM and peripheral neuropathy had higher amounts of calf muscle IMAT and lower subcutaneous fat when compared with obese age-matched controls both with and without T2DM.100 The authors suggested that IMAT may exacerbate peripheral neuropathy through increased concentrations of localized cytokines, including TNF-α and IL-6,100 which have been implicated in disrupted nerve cell homeostasis and neuropathy.101 IL-6 is associated with an increased loss of muscle mass and strength in T2DM,46,47 and this is likely due to direct effects on myocytes, alongside indirect effects on neurons and vasculature. Given that IMAT consists of non-contractile tissue, fat infiltration into skeletal muscle affects elastic properties of skeletal muscle.102 It is clear that IMAT makes an important contribution to the relationship between sarcopenia and T2DM in older individuals, and should be considered as a key outcome measure in future interventional studies.
Impaired muscle function may contribute to high levels of sedentary behavior in T2DM patients and contribute to a positive feedback loop where functional impairments lead to metabolic impairments, and vice versa. This positive feedback loop can be broken using lifestyle interventions with proven effectiveness for improving metabolic and musculoskeletal health.
Treatment and prevention of T2DM and sarcopenia
T2DM is commonly treated using glucose-lowering medications. Some of these may influence muscle mass (Table 2), but for the majority, their effects on sarcopenia components are unclear. Metformin increases AMP-activated protein kinase activity,103 which inhibits the mechanistic target of rapamycin (mTOR), a key factor in muscle growth.104 However, metformin is being investigated as an adjunct therapy to resistance training in older adults,105 as it may assist in the mobilization of M2 macrophages, which could have anti-inflammatory properties in skeletal muscle.105 In the MrOS study, men with diabetes treated with metformin alone and metformin plus thiazolidinediones (insulin sensitizers) over 3.5±0.7 years follow-up had an attenuated loss of total lean mass and ALM compared to men with diabetes that were not treated with insulin sensitizers, and men with untreated diabetes.106 Thus, it is unclear whether metformin has positive, negative, or negligible effects on muscle mass and strength in humans. Insulin has anabolic effects on muscle mass and protein metabolism in young and non-insulin resistant men and women;32,107 however, this does not seem to occur for individuals with T2DM.32,108 Indirectly, insulin therapy may improve muscle health by reducing blood glucose concentrations, which, as described above, can have negative effects on muscle through inflammation, oxidative stress and increased AGEs if chronically elevated. Sulfonylureas have been reported to cause muscle atrophy in a very small proportion of users;109 however, to the best of our knowledge there are no clinical trials investigating this relationship in a controlled setting. Overall, there is a paucity of data pertaining to the relationship between glucose-lowering medication and muscle health in humans, but purported effects on body weight and muscle mass in T2DM are described in Table 2.
 |
Table 2 Direct effect of glucose-lowering medications on body weight and muscle mass in type 2 diabetes |
There are no approved pharmacological treatments for sarcopenia. Possible therapeutic targets include hormonal interventions such as a transdermal testosterone gel116 and selective androgen receptor modulators.117,118 Transdermal testosterone gels increase serum concentrations of androgens, which have well-documented anabolic effects on skeletal muscle.119 However, these have undesirable side effects in regions such as the prostate gland and seminal vesicles, and have virializing side effects in women.120 Thus, selective androgen receptor modulators (SARMs) that only bind with androgen receptors within skeletal muscle are an attractive therapeutic.121 SARMs have acceptable safety profiles, and positive effects on body composition and physical function in clinical trials.117,118 Other novel treatments for sarcopenia undergoing clinical trials in humans include activin type IIB receptor antagonists121 and myostatin blockades (NCT01963598), which inhibit myostatin action. Myostatin is a negative regulator of myogenesis, and its inhibition significantly increases skeletal muscle mass in various animal knockouts.89,122 Improving muscle mass, quality and function using these treatments could also lead to indirect improvements in metabolic health; however, further studies are required to establish their safety and efficacy. Even if pharmacological agents are approved for the treatment of sarcopenia in the future, lifestyle modification will likely remain the primary therapy for the management of T2DM and sarcopenia.
Physical activity and exercise
Higher levels of physical activity are protective against the development of T2DM and sarcopenia. In the US Diabetes Prevention Program which included 3,234 non-diabetic adults, a lifestyle modification program (low-calorie, diet-induced weight loss of 7% of initial body weight and ≥150 min moderate-intensity physical activity per week) resulted in 58% reduced incidence of T2DM over three years, which was significantly more effective than metformin, a first-line glucose-lowering drug.123 In addition to reducing the incidence of T2DM, lifestyle interventions also achieve remission of T2DM.124 In the Look AHEAD study, approximately 12% of individuals completing a lifestyle intervention (aerobic activity for ≥50 min/week in the first month and ≥175 min/week after 6 months, alongside a weight loss goal of ≥10%) experienced partial or complete remission of T2DM compared with diabetes support and education (control).124 Similarly, a meta-analysis has reported that any engagement in physical activity reduces the likelihood of incident sarcopenia (OR:0.45 [95%CI:0.37–0.55]) in adults older than 40 years.125 Recent findings from the Look AHEAD study demonstrated that the lifestyle intervention resulted in better lower-limb performance, and lower likelihood (adjusted OR: 0.84 [95%CI:0.71–0.99]) of having poor gait speed (<0.8 m/s) in individuals with T2DM after 11 years. However, lifestyle intervention did not improve hand grip strength when compared with controls.126 This is unsurprising given aerobic exercise is generally not effective for improving muscle strength, despite its ability to improve metabolic health.127
Indeed, a recent network meta-analysis including 2,208 individuals ≥18 years of age with T2DM reported that supervised aerobic and strength training were both effective at reducing HbA1c compared with no exercise.127 However, the greatest reductions in HbA1c were experienced by individuals undertaking combined resistance and aerobic exercise.127 Furthermore, a recent randomized control trial (RCT) in 137 pre-diabetic adults (mean age 59 years) reported that two-year supervised resistance training alone (HR:0.35 [95%CI:0.15‐0.79]) and in combination with aerobic training (HR:0.26 [95%CI:0.11‐0.62]) were as effective as aerobic training alone (HR:0.28 [95%CI:0.13‐0.64]) in preventing progression to T2DM.128 Resistance training is the most effective strategy for improving both muscle mass and function in sarcopenic individuals,129 and is similarly effective for improving muscle strength, size, and quality and metabolic health in older adults with T2DM.130 Resistance training may therefore reduce the risk of developing sarcopenia in T2DM patients.
Combining resistance and aerobic training with diet-induced weight loss may be the most effective strategy for improving metabolic and musculoskeletal health in obese older adults. Resistance training may prevent or minimize muscle mass losses commonly associated with diet-induced weight loss,131 which needs to be avoided in older adults at risk of sarcopenia, including those with T2DM. In dieting obese older adults, combined resistance and aerobic training led to a 21% improvement in physical performance,132 and improved strength and preserved muscle mass more than aerobic training alone.132 Similarly, in obese older adults intentionally losing weight over 18 months, resistance training combined with caloric restriction resulted in less loss of lean mass (−1.5%) than caloric restriction combined with aerobic training (−3.1%) and caloric restriction alone (−2.0%).133 Nevertheless, the effect of exercise and diet-induced weight loss interventions on metabolic and muscle health in older adults with T2DM and sarcopenia is largely unexplored.
Diet
Caloric restriction is an effective strategy for weight loss in overweight and obese individuals.134 While weight loss can lead to remission of T2DM,135 as described above, it can lead to significant losses in muscle mass.131 To an extent, muscle mass losses may be commensurate to decreased loading as a result of losses in fat mass; however, muscle mass losses during caloric restriction may also result from inadequate protein intake.
Protein is important for the maintenance and growth of skeletal muscle. In older adults, there is evidence to suggest that recommended daily intake (RDI) of protein should be between ~1.2–1.6 g/kg/day,136 despite the RDI in many countries being ~0.8 g/kg/day.137,138 In the Health ABC study, older adults in the highest quintile of energy-adjusted protein intake (1.2±0.4 g/kg/day) lost approximately 40% less ALM and total lean mass over three years when compared with individuals in the lowest quintile for protein intake (0.8±0.3 g/kg/day).139 Different protein sources may also affect the risk for incident T2DM. Findings from the Melbourne Collaborative Cohort Study (MCCS) and a meta-analysis showed that individuals in the highest animal and total protein intake category had increased pooled risk ratios for incident T2DM (RR:1.19 [95%CI:1.11–1.28] and RR:1.09 [95%CI:1.06–1.13], respectively), compared with the lowest intake category. Interestingly, individuals in the highest plant protein intake category had reduced, albeit not significantly, risk for incident T2DM (RR:0.95 [95%CI:0.89–1.02]) compared with individuals in the lowest intake category.140 It was also reported that in the MCCS cohort alone (n=21,523), plant protein was negatively associated with incident T2DM in women (OR:0.60 [95%CI:0.37–0.99]), but not men (OR:1.26 [95%CI:0.75–2.13]). Thus, to ensure older adults with, or at risk of, T2DM are meeting protein requirements, increases in protein intake from primarily plant sources may be most appropriate. Plant protein appears to have a lower skeletal muscle anabolic response when compared with animal protein; however, proposed strategies to augment the anabolic properties of plant protein include fortification of plant-based protein sources with amino acids, selective breeding of plants to improve amino acid profiles, and consuming a combination of plant protein sources.141
The efficacy of combining protein supplementation with resistance training to enhance exercise-related muscle outcomes in older adults with and without sarcopenia is still unclear. A recent meta-analysis by Morton et al demonstrated that protein supplementation was effective for improving lean mass in resistance-trained adults, but appears to have very little effect on muscle outcomes in older adults.142 This meta-analysis also reported that protein intake beyond ~1.6 g/kg/day did not further increase changes in lean mass.142 Interestingly, Beaudart et al recently reported that an additional effect of protein supplementation combined with exercise on muscle mass and strength in older adults with sarcopenia was only evident in 3/12 RCTs included in their systematic review.143 Nevertheless, ensuring adequate protein intake is important for muscle maintenance and, potentially, growth, which in turn is beneficial for metabolic health.
Vitamin D may also affect metabolic and muscle health. Low vitamin D has been linked to poor physical function144 and glycemic control.145 Vitamin D receptors are located within the pancreas and skeletal muscle, suggesting a role in both glucose and muscle homeostasis. A recent randomized controlled trial in older adults with low vitamin D concentrations (≥8 and ≤20 ng/mL) reported that vitamin D supplementation (800 IU/d) for 12 months did not affect lower-extremity power, strength or lean mass.146 On the contrary, meta-analyses by Stockton et al147 and Rabenda et al148 suggest that vitamin D supplementation can improve muscle strength, but only in individuals with baseline 25-hydroxyvitamin D [25(OH)D] <25 and <30 nmol/L, respectively. Interestingly, vitamin D also shows potential as an adjunct therapy during exercise. In a meta-analysis by Antoniak and Greig, minor improvements in lower limb muscle strength (standard mean difference: 0.98 [95%CI: 0.73–1.24]) were evident with combined vitamin D and exercise versus exercise alone; however, for the timed up and go test (TUG), there were no additive effects of vitamin D combined with exercise compared with exercise alone.149 Only three studies were included in the analysis of lower limb muscle strength, and two studies were included in the analysis of TUG, highlighting the need for further research into the effects of combined vitamin D supplementation and exercise. There is also a need for more RCTs investigating the effect of vitamin D on muscle in vitamin D deficient populations, both with and without T2DM and sarcopenia.
Regarding direct effects of vitamin D on metabolic health, a recent RCT utilizing gold-standard measures of insulin sensitivity and high-dose vitamin D supplementation (100,000 IU initial bolus; 4,000 IU/d) reported no effects on insulin sensitivity in 54 non-diabetic, vitamin D deficient ([25(OH)D] ≤50 nmol/L) overweight and obese adults.150 Furthermore, a subgroup analysis (n=23) was performed in this study in participants with baseline 25(OH)D concentrations <30 nmol/L; however, there was no effect of vitamin D supplementation on insulin sensitivity.150 It should be noted that this sub-analysis was likely underpowered. Also, vitamin D supplementation has been reported to have no effect on insulin sensitivity in vitamin D deficient individuals ([25(OH)D] ≤50 nmol/L) with T2DM.151 Meta-analyses have reported conflicting findings; with vitamin D supplementation influencing glucose regulation in prediabetes and diabetes145,152–154 but not in other populations.155 Future studies in larger T2DM and non-T2DM populations with moderate to severe vitamin D deficiency ([25(OH)D] <30 or 25 nmol/L) may help establish whether there is an effect of vitamin D supplementation on various aspects of glucose metabolism, and whether this effect is limited to individuals with poorer metabolic health.
Lastly, omega-3 supplementation alone and in combination with exercise may improve metabolic and muscle health. Omega-3 supplementation can affect muscle directly by increasing muscle protein synthesis156 and indirectly by decreasing systemic inflammation.157 In 118 postmenopausal women, 6 months of fish oil-based supplementation (rich in omega-3 fatty acids) was associated with improved gait speed compared with placebo (3±16 vs -3.5±14%.158 Furthermore, in 60 healthy older adults (aged 60–85 years), 6 months of fish oil-based omega-3 supplementation increased thigh muscle volume (mean change: 3.6% [95%CI:0.2–7.0%]), handgrip strength (mean change: 2.3 kg [95%CI:0.8–3.7 kg]) and composite 1 repetition maximum muscle strength scores (mean change: 4.0% [95%CI:0.8–7.3%]).159 However, RCTs have also reported that omega-3 supplementation alone has no effect on muscle health in older populations.160,161 Similar to vitamin D supplementation, omega-3 supplementation has shown some potential as an adjunct therapy during exercise. In 51 older adults (mean age 64 years) that completed a 12-week resistance training program combined with flaxseed oil-derived alpha-linolenic acid (ALA) supplementation (rich in omega-3 fatty acids) or placebo, ALA supplementation resulted in a small increase in knee flexor muscle thickness, and a decrease in IL-6 concentrations in men.162 Although, it is still unclear what type and dosage of omega-3 supplement is most effective for preventing and treating sarcopenia. Regarding the effect of omega-3 supplementation on metabolic health, studies assessing the effect of omega-3 supplementation on fasting glucose,159 insulin resistance,163 and T2DM164 have reported little, or no effect. There are also limited data on nutritional interventions in individuals with comorbid T2DM and sarcopenia. Further studies in well-defined populations, particularly those with nutritional deficiencies, will help clarify the effect of the aforementioned nutritional interventions on metabolic and muscle health.
Conclusion
There are numerous bidirectional links between T2DM and sarcopenia, and the existence of one condition may increase the risk of developing the other. Factors such as insulin resistance, inflammation, AGE accumulation, increased oxidative stress and vascular complications can all affect various components of muscle health; and impaired muscle health can also contribute to development and progression of T2DM. The use of different operational definitions of sarcopenia clouds our understanding of this relationship, and therefore, development of a consensus definition is paramount. Evidence suggests that several lifestyle interventions (identified in Figure 1) can improve and maintain functional and metabolic health in individuals with T2DM and sarcopenia, but evidence for the most effective and feasible interventions in those with both conditions is lacking. Further research is needed to better understand, treat and prevent comorbid sarcopenia and T2DM, the beneficial outcomes of which would include increased independence and quality of life in these individuals.
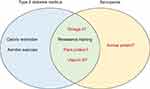 |
Figure 1 Lifestyle interventions for type 2 diabetes mellitus and sarcopenia. |
Author contributions
All authors contributed to conception and design, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
JM is supported by a Research Training Program Scholarship. BDC is supported by a National Heart Foundation Future Leader Fellowship (100864). DS is supported by a National Health and Medical Research Council R.D. Wright Biomedical Career Development Fellowship (GNT1123014). The authors report no other conflicts of interest in this work.
References
1. Cho NH, Shaw JE, Karuranga S, et al. IDF diabetes atlas: global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res Clin Pract. 2018;138:271–281. doi:10.1016/j.diabres.2018.02.023
2. American Diabetes A. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2009;32 Suppl 1(Suppl1):S62–S67. doi:10.2337/dc09-S062
3. Harreiter J, Kautzky-Willer A, Pacini G. Sex and gender differences in risk, pathophysiology and complications of type 2 diabetes mellitus. Endocr Rev. 2016;37(3):278–316. doi:10.1210/er.2015-1137
4. Briggs AM, Woolf AD, Dreinhöfer K, et al. Reducing the global burden of musculoskeletal conditions. Bull World Health Organ. 2018;96(5):366–368. doi:10.2471/BLT.17.204891
5. St-Onge M-P, Gallagher D. Body composition changes with aging: the cause or the result of alterations in metabolic rate and macronutrient oxidation? Nutrition. 2010;26(2):152–155. doi:10.1016/j.nut.2009.07.004
6. Hong S, Chang Y, Jung HS, Yun KE, Shin H, Ryu S. Relative muscle mass and the risk of incident type 2 diabetes: a cohort study. PLoS One. 2017;12(11):e0188650. doi:10.1371/journal.pone.0188650
7. Wang Y, Rimm EB, Stampfer MJ, Willett WC, Hu FB. Comparison of abdominal adiposity and overall obesity in predicting risk of type 2 diabetes among men. Am J Clin Nutr. 2005;81(3):555–563.
8. Cruz-Jentoft AJ, Baeyens JP, Bauer JM, et al. Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010;39(4):412–423.
9. Cruz-Jentoft AJ, Bahat G, Bauer J, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing. 2018;48(1):16–31. doi:10.1093/ageing/afy169
10. Studenski SA, Peters KW, Alley DE, et al. The FNIH sarcopenia project: rationale, study description, conference recommendations, and final estimates. J Gerontol A Biol Sci Med Sci. 2014;69(5):547–558. doi:10.1093/gerona/glu010
11. Fielding RA, Vellas B, Evans WJ, et al. Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc. 2011;12(4):249–256. doi:10.1016/j.jamda.2011.01.003
12. Chen LK, Liu LK, Woo J, et al. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc. 2014;15(2):95–101. doi:10.1016/j.jamda.2013.11.025
13. Scott D, de Courten B, Ebeling PR. Sarcopenia: a potential cause and consequence of type 2 diabetes in Australia’s ageing population? Med J Aust. 2016;205(7):329–333.
14. Nowotny K, Jung T, Höhn A, Weber D, Grune T. Advanced glycation end products and oxidative stress in type 2 diabetes mellitus. Biomolecules. 2015;5:194–222. doi:10.3390/biom5010194
15. Amog K, Raina P, Mayhew AJ, et al. The prevalence of sarcopenia in community-dwelling older adults, an exploration of differences between studies and within definitions: a systematic review and meta-analyses. Age Ageing. 2018;48(1):48–56.
16. Shafiee G, Keshtkar A, Soltani A, Ahadi Z, Larijani B, Heshmat R. Prevalence of sarcopenia in the world: a systematic review and meta- analysis of general population studies. J Diabetes Metab Disord. 2017;16:21. doi:10.1186/s40200-017-0302-x
17. Murata Y, Kadoya Y, Yamada S, Sanke T. Sarcopenia in elderly patients with type 2 diabetes mellitus: prevalence and related clinical factors. Diabetol Int. 2018;9(2):136–142. doi:10.1007/s13340-017-0339-6
18. Wang T, Feng X, Zhou J, et al. Type 2 diabetes mellitus is associated with increased risks of sarcopenia and pre-sarcopenia in Chinese elderly. Sci Rep. 2016;6:38937. doi:10.1038/srep38937
19. Kim TN, Park MS, Yang SJ, et al. Prevalence and determinant factors of sarcopenia in patients with type 2 diabetes. Diabetes Care. 2010;33(7):1497. doi:10.2337/dc09-2310
20. Park SW, Goodpaster BH, Lee JS, et al. Excessive loss of skeletal muscle mass in older adults with type 2 diabetes. Diabetes Care. 2009;32(11):1993–1997. doi:10.2337/dc09-0264
21. Yang L, Smith L, Hamer M. Gender-specific risk factors for incident sarcopenia: 8-year follow-up of the English longitudinal study of ageing. J Epidemiol Community Health. 2019;73(1):86. doi:10.1136/jech-2018-211258
22. Son JW, Lee SS, Kim SR, et al. Low muscle mass and risk of type 2 diabetes in middle-aged and older adults: findings from the KoGES. Diabetologia. 2017;60(5):865–872. doi:10.1007/s00125-016-4196-9
23. Wu H, Liu M, Chi VTQ, et al. Handgrip strength is inversely associated with metabolic syndrome and its separate components in middle aged and older adults: a large-scale population-based study. Metabolism. 2019;93:61–67. doi:10.1016/j.metabol.2019.01.011
24. Thiebaud D, Jacot E, DeFronzo RA, Maeder E, Jequier E, Felber JP. The effect of graded doses of insulin on total glucose uptake, glucose oxidation, and glucose storage in man. Diabetes. 1982;31(11):957–963.
25. Lee CG, Boyko EJ, Strotmeyer ES, et al. Association between insulin resistance and lean mass loss and fat mass gain in older men without diabetes mellitus. J Am Geriatr Soc. 2011;59(7):1217–1224. doi:10.1111/j.1532-5415.2011.03472.x
26. Kuo CK, Lin LY, Yu YH, Wu KH, Kuo HK. Inverse association between insulin resistance and gait speed in nondiabetic older men: results from the U.S. National Health and Nutrition Examination Survey (NHANES) 1999-2002. BMC Geriatr. 2009;9:49. doi:10.1186/1471-2318-9-49
27. Abbatecola AM, Ferrucci L, Ceda G, et al. Insulin resistance and muscle strength in older persons. J Gerontol A Biol Sci Med Sci. 2005;60(10):1278–1282.
28. Sherwani SI, Khan HA, Ekhzaimy A, Masood A, Sakharkar MK. Significance of HbA1c test in diagnosis and prognosis of diabetic patients. Biomark Insights. 2016;11:95–104. doi:10.4137/BMI.S38440
29. Yoon JW, Ha Y-C, Kim KM, et al. Hyperglycemia is associated with impaired muscle quality in older men with diabetes: the Korean Longitudinal Study on Health and Aging. Diabetes Metab J. 2016;40(2):140–146. doi:10.4093/dmj.2016.40.2.140
30. Kalyani RR, Metter EJ, Egan J, Golden SH, Ferrucci L. Hyperglycemia predicts persistently lower muscle strength with aging. Diabetes Care. 2015;38(1):82–90. doi:10.2337/dc14-1166
31. Russell ST, Rajani S, Dhadda RS, Tisdale MJ. Mechanism of induction of muscle protein loss by hyperglycaemia. Exp Cell Res. 2009;315(1):16–25. doi:10.1016/j.yexcr.2008.10.002
32. Pereira S, Marliss EB, Morais JA, Chevalier S, Gougeon R. Insulin resistance of protein metabolism in type 2 diabetes. Diabetes. 2008;57(1):56. doi:10.2337/db07-0887
33. de Rekeneire N, Peila R, Ding J, et al. Diabetes, hyperglycemia, and inflammation in older individuals. Diabetes Care. 2006;29(8):1902. doi:10.2337/dc05-2327
34. Vozarova B, Weyer C, Lindsay RS, Pratley RE, Bogardus C, Tataranni PA. High white blood cell count is associated with a worsening of insulin sensitivity and predicts the development of type 2 diabetes. Diabetes. 2002;51(2):455. doi:10.2337/diabetes.51.2.455
35. Haddad F, Zaldivar F, Cooper DM, Adams GR. IL-6-induced skeletal muscle atrophy. J Appl Physiol. 2005;98(3):911–917. doi:10.1152/japplphysiol.01026.2004
36. Goyal R, Faizy AF, Siddiqui SS, Singhai M. Evaluation of TNF-α and IL-6 levels in obese and non-obese diabetics: pre- and postinsulin effects. N Am J Med Sci. 2012;4(4):180–184. doi:10.4103/1947-2714.94944
37. King DE, Mainous AG, Buchanan TA, Pearson WS. C-reactive protein and glycemic control in adults with diabetes. Diabetes Care. 2003;26(5):1535. doi:10.2337/diacare.26.5.1535
38. Vozarova B, Weyer C, Hanson K, Tataranni PA, Bogardus C, Pratley RE. Circulating interleukin-6 in relation to adiposity, insulin action, and insulin secretion. Obes Res. 2001;9(7):414–417. doi:10.1038/oby.2001.54
39. Makki K, Froguel P, Wolowczuk I. Adipose tissue in obesity-related inflammation and insulin resistance: cells, cytokines, and chemokines. ISRN Inflamm. 2013;2013:139239. doi:10.1155/2013/139239
40. Mesinovic J, McMillan BL, Shore-Lorenti C, De Courten B, Ebeling RP, Scott D. Metabolic syndrome and its associations with components of sarcopenia in overweight and obese older adults. J Clin Med. 2019;8:2. doi:10.3390/jcm8020145
41. Bach E, Nielsen RR, Vendelbo MH, et al. Direct effects of TNF-α on local fuel metabolism and cytokine levels in the placebo-controlled, bilaterally infused human leg. Diabetes. 2013;62(12):4023. doi:10.2337/db12-0863
42. Carey AL, Steinberg GR, Macaulay SL, et al. Interleukin-6 increases insulin-stimulated glucose disposal in humans and glucose uptake and fatty acid oxidation in vitro via AMP-activated protein kinase. Diabetes. 2006;55(10):2688–2697. doi:10.2337/db05-1404
43. Serrano AL, Baeza-Raja B, Perdiguero E, Jardi M, Munoz-Canoves P. Interleukin-6 is an essential regulator of satellite cell-mediated skeletal muscle hypertrophy. Cell Metab. 2008;7(1):33–44. doi:10.1016/j.cmet.2007.11.011
44. Payette H, Roubenoff R, Jacques PF, et al. Insulin-like growth factor-1 and interleukin 6 predict sarcopenia in very old community-living men and women: the Framingham Heart Study. J Am Geriatr Soc. 2003;51(9):1237–1243.
45. Alemán H, Esparza J, Ramirez FA, Astiazaran H, Payette H. Longitudinal evidence on the association between interleukin-6 and C-reactive protein with the loss of total appendicular skeletal muscle in free-living older men and women. Age Ageing. 2011;40(4):469–475. doi:10.1093/ageing/afr040
46. Park SW, Goodpaster BH, Strotmeyer ES, et al. Accelerated loss of skeletal muscle strength in older adults with type 2 diabetes: the health, aging, and body composition study. Diabetes Care. 2007;30(6):1507–1512. doi:10.2337/dc06-2537
47. Visser M, Pahor M, Taaffe DR, et al. Relationship of interleukin-6 and tumor necrosis factor-alpha with muscle mass and muscle strength in elderly men and women: the Health ABC Study. J Gerontol A Biol Sci Med Sci. 2002;57(5):M326–M332.
48. Hamer M, Molloy GJ. Association of C-reactive protein and muscle strength in the English Longitudinal Study of Ageing. Age (Dordr). 2009;31(3):171–177. doi:10.1007/s11357-009-9097-0
49. Gomes MJ, Martinez PF, Pagan LU, et al. Skeletal muscle aging: influence of oxidative stress and physical exercise. Oncotarget. 2017;8(12):20428–20440. doi:10.18632/oncotarget.14670
50. Asmat U, Abad K, Ismail K. Diabetes mellitus and oxidative stress—A concise review. Saudi Pharm J. 2016;24(5):547–553. doi:10.1016/j.jsps.2015.03.013
51. Aragno M, Mastrocola R, Catalano MG, Brignardello E, Danni O, Boccuzzi G. Oxidative stress impairs skeletal muscle repair in diabetic rats. Diabetes. 2004;53(4):1082.
52. Zacarias-Flores M, Sanchez-Rodriguez MA, Garcia-Anaya OD, Correa-Munoz E, Mendoza-Nunez VM. Relationship between oxidative stress and muscle mass loss in early postmenopause: an exploratory study. Endocrinol Diabetes Nutr. 2018;65(6):328–334. doi:10.1016/j.endinu.2018.01.009
53. Scicchitano BM, Pelosi L, Sica G, Musarò A. The physiopathologic role of oxidative stress in skeletal muscle. Mech Ageing Dev. 2018;170:37–44. doi:10.1016/j.mad.2017.08.009
54. Short KR, Bigelow ML, Kahl J, et al. Decline in skeletal muscle mitochondrial function with aging in humans. Proc Natl Acad Sci U S A. 2005;102(15):5618–5623. doi:10.1073/pnas.0501559102
55. Abbatecola AM, Paolisso G, Fattoretti P, et al. Discovering pathways of sarcopenia in older adults: a role for insulin resistance on mitochondria dysfunction. J Nutr Health Aging. 2011;15(10):890–895. doi:10.1007/s12603-011-0366-0
56. Conley KE, Jubrias SA, Esselman PC. Oxidative capacity and ageing in human muscle. J Physiol. 2000;526 Pt 1(Pt1):203–210.
57. Bua E, Johnson J, Herbst A, et al. Mitochondrial DNA-deletion mutations accumulate intracellularly to detrimental levels in aged human skeletal muscle fibers. Am J Hum Genet. 2006;79(3):469–480. doi:10.1086/507132
58. Schrauwen-Hinderling VB, Kooi ME, Hesselink MK, et al. Impaired in vivo mitochondrial function but similar intramyocellular lipid content in patients with type 2 diabetes mellitus and BMI-matched control subjects. Diabetologia. 2007;50(1):113–120. doi:10.1007/s00125-006-0475-1
59. Morino K, Petersen KF, Dufour S, et al. Reduced mitochondrial density and increased IRS-1 serine phosphorylation in muscle of insulin-resistant offspring of type 2 diabetic parents. J Clin Invest. 2005;115(12):3587–3593. doi:10.1172/JCI25151
60. Singh R, Barden A, Mori T, Beilin L. Advanced glycation end-products: a review. Diabetologia. 2001;44(2):129–146. doi:10.1007/s001250051591
61. Haus JM, Carrithers JA, Trappe SW, Trappe TA. Collagen, cross-linking, and advanced glycation end products in aging human skeletal muscle. J Appl Physiol. 2007;103(6):2068–2076. doi:10.1152/japplphysiol.00670.2007
62. Forbes JM, Sourris KC, de Courten MPJ, et al. Advanced glycation end products (AGEs) are cross-sectionally associated with insulin secretion in healthy subjects. Amino Acids. 2014;46(2):321–326. doi:10.1007/s00726-013-1542-9
63. Mulder DJ, Water TV, Lutgers HL, et al. Skin autofluorescence, a novel marker for glycemic and oxidative stress-derived advanced glycation endproducts: an overview of current clinical studies, evidence, and limitations. Diabetes Technol Ther. 2006;8(5):523–535. doi:10.1089/dia.2006.8.523
64. Mori H, Kuroda A, Ishizu M, et al. Association of accumulated advanced glycation end products with a high prevalence of sarcopenia and dynapenia in patients with type 2 diabetes. J Diabetes Investig. 2019;35:731–737. doi:10.1111/jdi.13014
65. Momma H, Niu K, Kobayashi Y, et al. Skin advanced glycation end product accumulation and muscle strength among adult men. Eur J Appl Physiol. 2011;111(7):1545–1552. doi:10.1007/s00421-010-1779-x
66. Tabara Y, Ikezoe T, Yamanaka M, et al. Advanced Glycation End Product Accumulation Is Associated with Low Skeletal Muscle Mass, Weak Muscle Strength, and Reduced Bone Density: The Nagahama Study. J Gerontol A Biol Sci Med Sci. 2018. doi:10.1093/gerona/gly233
67. Chaudhri S, Fan S, Davenport A. Pitfalls in the measurement of skin autofluorescence to determine tissue advanced glycosylation content in haemodialysis patients. Nephrology. 2013;18(10):671–675. doi:10.1111/nep.12118
68. Noordzij MJ, Lefrandt JD, Graaff R, Smit AJ. Dermal factors influencing measurement of skin autofluorescence. Diabetes Technol Ther. 2011;13(2):165–170.
69. Fowler MJ. Microvascular and macrovascular complications of diabetes. Clin Diabetes. 2008;26(2):77.
70. McDermott MM, Criqui MH, Greenland P, et al. Leg strength in peripheral arterial disease: associations with disease severity and lower-extremity performance. J Vasc Surg. 2004;39(3):523–530.
71. Nomura T, Ishiguro T, Ohira M, Ikeda Y. Diabetic polyneuropathy is a risk factor for decline of lower extremity strength in patients with type 2 diabetes. J Diabetes Investig. 2018;9(1):186–192.
72. Andersen H, Gjerstad MD, Jakobsen J. Atrophy of foot muscles. Diabetes Care. 2004;27(10):2382.
73. Strotmeyer ES, de Rekeneire N, Schwartz AV, et al. The relationship of reduced peripheral nerve function and diabetes with physical performance in older white and black adults. Diabetes Care. 2008;31(9):1767.
74. Gupta P, Aravindhan A, Gand ATL, et al. Association between the severity of diabetic retinopathy and falls in an asian population with diabetes: the Singapore Epidemiology of Eye Diseases Study. JAMA Ophthalmol. 2017;135(12):1410–1416.
75. Haddad YK, Bergen G, Florence CS. Estimating the economic burden related to older adult falls by state. J Public Health Manag Pract. 2019;25(2):E17–E24.
76. Haagsma JA, Graetz N, Bolliger I, et al. The global burden of injury: incidence, mortality, disability-adjusted life years and time trends from the Global Burden of Disease study 2013. Injury Prevention. 2016;22(1):3.
77. Fukuda T, Bouchi R, Takeuchi T, et al. Association of diabetic retinopathy with both sarcopenia and muscle quality in patients with type 2 diabetes: a cross-sectional study. BMJ Open Diabetes Res Care. 2017;5(1):e000404.
78. Collins AJ, Foley RN, Gilbertson DT, Chen S-C. United States renal data system public health surveillance of chronic kidney disease and end-stage renal disease. Kidney Int Suppl. 2015;5(1):2–7.
79. Wang XH, Mitch WE. Mechanisms of muscle wasting in chronic kidney disease. Nat Rev Nephrol. 2014;10(9):504–516.
80. Fung FY, Koh YLE, Malhotra R, et al. Prevalence of and factors associated with sarcopenia among multi-ethnic ambulatory older Asians with type 2 diabetes mellitus in a primary care setting. BMC Geriatr. 2019;19(1):122.
81. VAd S, Oliveira D, Barbosa SR, et al. Sarcopenia in patients with chronic kidney disease not yet on dialysis: analysis of the prevalence and associated factors. PLoS One. 2017;12(4):e0176230–e0176230.
82. Pereira RA, Cordeiro AC, Avesani CM, et al. Sarcopenia in chronic kidney disease on conservative therapy: prevalence and association with mortality. Nephrol Dial Transplant. 2015;30(10):1718–1725.
83. Zhou Y, Hellberg M, Svensson P, Hoglund P, Clyne N. Sarcopenia and relationships between muscle mass, measured glomerular filtration rate and physical function in patients with chronic kidney disease stages 3-5. Nephrol Dial Transplant. 2018;33(2):342–348.
84. Gamboa JL, Billings F, Bojanowski MT, et al. Mitochondrial dysfunction and oxidative stress in patients with chronic kidney disease. Physiol Rep. 2016;4(9):e12780.
85. Martín-Timón I, Sevillano-Collantes C, Segura-Galindo A, Del Cañizo-Gómez FJ. Type 2 diabetes and cardiovascular disease: have all risk factors the same strength? World J Diabetes. 2014;5(4):444–470.
86. Singleton JR, Smith AG, Russell JW, Feldman EL. Microvascular complications of impaired glucose tolerance. Diabetes. 2003;52(12):2867.
87. McMaster William G, Kirabo A, Madhur Meena S, Harrison David G. Inflammation, immunity, and hypertensive end-organ damage. Circ Res. 2015;116(6):1022–1033.
88. Doğan MH, Karadag B, Ozyigit T, Kayaoglu S, Ozturk AO, Altuntas Y. Correlations between sarcopenia and hypertensive target organ damage in a Turkish cohort. Acta Clin Belg. 2012;67(5):328–332.
89. Butcher Joshua T, Mintz James D, Larion S, et al. Increased muscle mass protects against hypertension and renal injury in obesity. J Am Heart Assoc. 2018;7(16):e009358.
90. Lange S, Diehm C, Darius H, et al. High prevalence of peripheral arterial disease and low treatment rates in elderly primary care patients with diabetes. Exp Clin Endocrinol Diabetes. 2004;112(10):566–573.
91. Dziubek W, Bulińska K, Stefańska M, et al. Peripheral arterial disease decreases muscle torque and functional walking capacity in elderly. Maturitas. 2015;81(4):480–486.
92. McDermott Mary M. Lower extremity manifestations of peripheral artery disease. Circ Res. 2015;116(9):1540–1550.
93. Boettcher M, Machann J, Stefan N, et al. Intermuscular adipose tissue (IMAT): association with other adipose tissue compartments and insulin sensitivity. J Magn Reson Imaging. 2009;29(6):1340–1345.
94. Scott D, Shore-Lorenti C, McMillan LB, et al. Calf muscle density is independently associated with physical function in overweight and obese older adults. J Musculoskelet Neuronal Interact. 2018;18(1):9–17.
95. Marcus RL, Addison O, Dibble LE, Foreman KB, Morrell G, LaStayo P. Intramuscular adipose tissue, sarcopenia, and mobility function in older individuals. J Aging Res. 2012. doi:10.1155/2012/629637
96. Goodpaster BH, Thaete FL, Kelley DE. Thigh adipose tissue distribution is associated with insulin resistance in obesity and in type 2 diabetes mellitus. Am J Clin Nutr. 2000;71(4):885–892.
97. Gallagher D, Kelley DE, Yim J-E, et al. Adipose tissue distribution is different in type 2 diabetes. Am J Clin Nutr. 2009;89(3):807–814.
98. Scott D, Johansson J, McMillan LB, Ebeling PR, Nordstrom A, Nordstrom P. Mid-calf skeletal muscle density and its associations with physical activity, bone health and incident 12-month falls in older adults: the Healthy Ageing Initiative. Bone. 2018;120:446–451. doi:10.1016/j.bone.2018.12.004
99. Frank-Wilson AW, Farthing JP, Chilibeck PD, et al. Lower leg muscle density is independently associated with fall status in community-dwelling older adults. Osteoporos Int. 2016;27(7):2231–2240.
100. Bittel DC, Bittel AJ, Tuttle LJ, et al. Adipose tissue content, muscle performance and physical function in obese adults with type 2 diabetes mellitus and peripheral neuropathy. J Diabetes Complications. 2015;29(2):250–257. doi:10.1016/j.jdiacomp.2014.11.003
101. Skundric DS, Lisak RP. Role of neuropoietic cytokines in development and progression of diabetic polyneuropathy: from glucose metabolism to neurodegeneration. Exp Diabesity Res. 2003;4(4):303–312. doi:10.1155/EDR.2003.303
102. Csapo R, Malis V, Sinha U, Du J, Sinha S. Age-associated differences in triceps surae muscle composition and strength – an MRI-based cross-sectional comparison of contractile, adipose and connective tissue. BMC Musculoskelet Disord. 2014;15(1):209. doi:10.1186/1471-2474-15-209
103. Musi N, Hirshman MF, Nygren J, et al. Metformin increases AMP-activated protein kinase activity in skeletal muscle of subjects with type 2 diabetes. Diabetes. 2002;51(7):2074–2081. doi:10.2337/diabetes.51.7.2074
104. Mihaylova MM, Shaw RJ. The AMPK signalling pathway coordinates cell growth, autophagy and metabolism. Nat Cell Biol. 2011;13(9):1016–1023. doi:10.1038/ncb2329
105. Long DE, Peck BD, Martz JL, et al. Metformin to Augment Strength Training Effective Response in Seniors (MASTERS): study protocol for a randomized controlled trial. Trials. 2017;18(1):192. doi:10.1186/s13063-017-1932-5
106. Lee CG, Boyko EJ, Barrett-Connor E, et al. Insulin sensitizers may attenuate lean mass loss in older men with diabetes. Diabetes Care. 2011;34(11):2381. doi:10.2337/dc11-1032
107. Cetrone M, Mele A, Tricarico D. Effects of the antidiabetic drugs on the age-related atrophy and sarcopenia associated with diabetes type II. Curr Diabetes Rev. 2014;10(4):231–237.
108. Fanzani A, Conraads VM, Penna F, Martinet W. Molecular and cellular mechanisms of skeletal muscle atrophy: an update. J Cachexia Sarcopenia Muscle. 2012;3(3):163–179. doi:10.1007/s13539-012-0074-6
109. Mele A, Calzolaro S, Cannone G, Cetrone M, Conte D, Tricarico D. Database search of spontaneous reports and pharmacological investigations on the sulfonylureas and glinides-induced atrophy in skeletal muscle. Pharmacol Res Perspect. 2014;2(1):e00028–e00028. doi:10.1002/prp2.28
110. Diabetes Prevention Program Research G. Long-term safety, tolerability, and weight loss associated with metformin in the Diabetes Prevention Program Outcomes Study. Diabetes Care. 2012;35(4):731–737. doi:10.2337/dc11-1299
111. van Dieren S, Czernichow S, Chalmers J, et al. Weight changes and their predictors amongst 11 140 patients with type 2 diabetes in the ADVANCE trial. Diabetes Obes Metab. 2012;14(5):464–469. doi:10.1111/j.1463-1326.2012.01556.x
112. Fujita S, Rasmussen BB, Cadenas JG, Grady JJ, Volpi E. Effect of insulin on human skeletal muscle protein synthesis is modulated by insulin-induced changes in muscle blood flow and amino acid availability. Am J Physiol Endocrinol Metab. 2006;291(4):E745–E754. doi:10.1152/ajpendo.00271.2005
113. Raz I, Chen Y, Wu M, et al. Efficacy and safety of sitagliptin added to ongoing metformin therapy in patients with type 2 diabetes. Curr Med Res Opin. 2008;24(2):537–550. doi:10.1185/030079908X260925
114. Scheen AJ. Pharmacodynamics, efficacy and Safety of Sodium–glucose Co-Transporter Type 2 (SGLT2) inhibitors for the treatment of type 2 diabetes mellitus. Drugs. 2015;75(1):33–59. doi:10.1007/s40265-014-0337-y
115. Zinman B, Hoogwerf BJ, Duran Garcia S, et al. The effect of adding exenatide to a thiazolidinedione in suboptimally controlled type 2 diabetes: a randomized trial. Ann Intern Med. 2007;146(7):477–485.
116. Atkinson RA, Srinivas-Shankar U, Roberts SA, et al. Effects of testosterone on skeletal muscle architecture in intermediate-frail and frail elderly men. J Gerontol A Biol Sci Med Sci. 2010;65(11):1215–1219. doi:10.1093/gerona/glq118
117. Dalton JT, Barnette KG, Bohl CE, et al. The selective androgen receptor modulator GTx-024 (enobosarm) improves lean body mass and physical function in healthy elderly men and postmenopausal women: results of a double-blind, placebo-controlled phase II trial. J Cachexia Sarcopenia Muscle. 2011;2(3):153–161. doi:10.1007/s13539-011-0034-6
118. Papanicolaou DA, Ather SN, Zhu H, et al. A phase IIA randomized, placebo-controlled clinical trial to study the efficacy and safety of the selective androgen receptor modulator (SARM), MK-0773 in female participants with sarcopenia. J Nutr Health Aging. 2013;17(6):533–543. doi:10.1007/s12603-013-0335-x
119. Neto WK, Gama EF, Rocha LY, et al. Effects of testosterone on lean mass gain in elderly men: systematic review with meta-analysis of controlled and randomized studies. Age (Dordr). 2015;37(1):9742. doi:10.1007/s11357-014-9742-0
120. Narayanan R, Coss CC, Dalton JT. Development of selective androgen receptor modulators (SARMs). Mol Cell Endocrinol. 2018;465:134–142. doi:10.1016/j.mce.2017.06.013
121. Becker C, Lord SR, Studenski SA, et al. Myostatin antibody (LY2495655) in older weak fallers: a proof-of-concept, randomised, phase 2 trial. Lancet Diabetes Endocrinol. 2015;3(12):948–957. doi:10.1016/S2213-8587(15)00298-3
122. Lv Q, Yuan L, Deng J, et al. Efficient generation of myostatin gene mutated rabbit by CRISPR/Cas9. Sci Rep. 2016;6:25029. doi:10.1038/srep25029
123. Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393–403. doi:10.1056/NEJMoa012512
124. Gregg EW, Chen H, Wagenknecht LE, et al. Association of an intensive lifestyle intervention with remission of type 2 diabetes. JAMA. 2012;308(23):2489–2496. doi:10.1001/jama.2012.67929
125. Steffl M, Bohannon RW, Sontakova L, Tufano JJ, Shiells K, Holmerova I. Relationship between sarcopenia and physical activity in older people: a systematic review and meta-analysis. Clin Interv Aging. 2017;12:835–845. doi:10.2147/CIA.S132940
126. Houston DK, Neiberg RH, Miller ME, et al. Physical function following a long-term lifestyle intervention among middle aged and older adults with type 2 diabetes: the look AHEAD study. J Gerontol Series A. 2018;73(11):1552–1559. doi:10.1093/gerona/glx204
127. Pan B, Ge L, Xun Y-Q, et al. Exercise training modalities in patients with type 2 diabetes mellitus: a systematic review and network meta-analysis. Int J Behav Nutr Phys Act. 2018;15(1):72. doi:10.1186/s12966-018-0703-3
128. Dai X, Zhai L, Chen Q, et al. Two-year-supervised resistance training prevented diabetes incidence in people with prediabetes: a randomised control trial. Diabetes Metab Res Rev. 2019;e3143. doi:10.1002/dmrr.3143
129. Vlietstra L, Hendrickx W, Waters DL. Exercise interventions in healthy older adults with sarcopenia: a systematic review and meta-analysis. Australas J Ageing. 2018;37(3):169–183. doi:10.1111/ajag.12521
130. Hovanec N, Sawant A, Overend TJ, Petrella RJ, Vandervoort AA. Resistance training and older adults with type 2 diabetes mellitus: strength of the evidence. J Aging Res. 2012;2012:284635. doi:10.1155/2012/284635
131. Sardeli A, Komatsu T, Mori M, Gáspari A, Chacon-Mikahil M. Resistance training prevents muscle loss induced by caloric restriction in obese elderly individuals: a systematic review and meta-analysis. Nutrients. 2018;10(4):423. doi:10.3390/nu10040423
132. Villareal DT, Aguirre L, Gurney AB, et al. Aerobic or resistance exercise, or both, in dieting obese older adults. N Engl J Med. 2017;376(20):1943–1955. doi:10.1056/NEJMoa1616338
133. Beavers KM, Ambrosius WT, Rejeski WJ, et al. Effect of exercise type during intentional weight loss on body composition in older adults with obesity. Obesity (Silver Spring). 2017;25(11):1823–1829. doi:10.1002/oby.21977
134. Greco M, Chiefari E, Montalcini T, et al. Early effects of a hypocaloric, mediterranean diet on laboratory parameters in obese individuals. Mediators Inflamm. 2014;2014:750860. doi:10.1155/2014/750860
135. Taylor R, Al-Mrabeh A, Zhyzhneuskaya S, et al. Remission of human type 2 diabetes requires decrease in liver and pancreas fat content but is dependent upon capacity for β cell recovery. Cell Metab. 2018;28(4):547–556. doi:10.1016/j.cmet.2018.07.003
136. Phillips S, Chevalier S, Leidy H. Protein “Requirements” beyond the RDA: Implications for Optimizing Health. Appl Physiol Nutr Metab. 2016;41(5): 565–572. doi:10.1139/apnm-2015-0550
137. Trumbo P, Schlicker S, Yates AA, Poos M. Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein and amino acids. J Am Diet Assoc. 2002;102(11):1621–1630.
138. Nowson C, O’Connell S. Protein requirements and recommendations for older people: a review. Nutrients. 2015;7(8):6874–6899. doi:10.3390/nu7085311
139. Health ABCS, Newman AB, Nicklas BJ, et al. Dietary protein intake is associated with lean mass change in older, community-dwelling adults: the Health, Aging, and Body Composition (Health ABC) Study. Am J Clin Nutr. 2008;87(1):150–155. doi:10.1093/ajcn/87.1.150
140. Shang X, Scott D, Sanders KM, et al. Dietary protein intake and risk of type 2 diabetes: results from the Melbourne Collaborative Cohort Study and a meta-analysis of prospective studies. Am J Clin Nutr. 2016;104(5):1352–1365. doi:10.3945/ajcn.116.140954
141. van Vliet S, Burd NA, van Loon LJC. The skeletal muscle anabolic response to plant- versus animal-based protein consumption. J Nutr. 2015;145(9):1981–1991. doi:10.3945/jn.114.204305
142. Morton RW, Murphy KT, McKellar SR, et al. A systematic review, meta-analysis and meta-regression of the effect of protein supplementation on resistance training-induced gains in muscle mass and strength in healthy adults. Br J Sports Med. 2018;52(6):376.
143. Beaudart C, Dawson A, Shaw SC, et al. Nutrition and physical activity in the prevention and treatment of sarcopenia: systematic review. Osteoporos Int. 2017;28(6):1817–1833. doi:10.1007/s00198-017-3980-9
144. Dang M, Shore-Lorenti C, McMillan BL, et al. Associations of serum 25-hydroxyvitamin D with physical performance and bone health in overweight and obese older adults. Int J Environ Res Public Health. 2019;16(3). doi:10.3390/ijerph16030509.
145. Mirhosseini N, Vatanparast H, Mazidi M, Kimball SM. Vitamin D supplementation, glycemic control, and insulin resistance in prediabetics: a meta-analysis. J Endocr Soc. 2018;2(7):687–709. doi:10.1210/js.2017-00472
146. Shea MK, Fielding RA, Dawson-Hughes B. The effect of vitamin D supplementation on lower-extremity power and function in older adults: a randomized controlled trial. Am J Clin Nutr. 2019;109(2):369–379. doi:10.1093/ajcn/nqy290
147. Stockton KA, Mengersen K, Paratz JD, Kandiah D, Bennell KL. Effect of vitamin D supplementation on muscle strength: a systematic review and meta-analysis. Osteoporos Int. 2011;22(3):859–871. doi:10.1007/s00198-010-1407-y
148. Rabenda V, Buckinx F, Slomian J, et al. The effects of vitamin D on skeletal muscle strength, muscle mass, and muscle power: a systematic review and meta-analysis of randomized controlled trials. J Clin Endocrinol Metab. 2014;99(11):4336–4345. doi:10.1210/jc.2014-1742
149. Antoniak AE, Greig CA. The effect of combined resistance exercise training and vitamin D(3) supplementation on musculoskeletal health and function in older adults: a systematic review and meta-analysis. BMJ Open. 2017;7(7):e014619–e014619. doi:10.1136/bmjopen-2016-014619
150. Mousa A, Naderpoor N, de Courten MP, et al. Vitamin D supplementation has no effect on insulin sensitivity or secretion in vitamin D-deficient, overweight or obese adults: a randomized placebo-controlled trial. Am J Clin Nutr. 2017;105(6):1372–1381. doi:10.3945/ajcn.117.152736
151. Gulseth HL, Wium C, Angel K, Eriksen EF, Birkeland KI. Effects of vitamin D supplementation on insulin sensitivity and insulin secretion in subjects with type 2 diabetes and vitamin D deficiency: a randomized controlled trial. Diabetes Care. 2017;40(7):872–878. doi:10.2337/dc16-2302
152. Lee CJ, Iyer G, Liu Y, et al. The effect of vitamin D supplementation on glucose metabolism in type 2 diabetes mellitus: a systematic review and meta-analysis of intervention studies. J Diabetes Complications. 2017;31(7):1115–1126. doi:10.1016/j.jdiacomp.2017.04.019
153. Wu C, Qiu S, Zhu X, Li L. Vitamin D supplementation and glycemic control in type 2 diabetes patients: a systematic review and meta-analysis. Metabolism. 2017;73:67–76. doi:10.1016/j.metabol.2017.05.006
154. Hu Z, Chen J, Sun X, Wang L, Wang A. Efficacy of vitamin D supplementation on glycemic control in type 2 diabetes patients: a meta-analysis of interventional studies. Medicine (Baltimore). 2019;98(14):e14970. doi:10.1097/MD.0000000000014970
155. Jamka M, Woźniewicz M, Jeszka J, Mardas M, Bogdański P, Stelmach-Mardas M. The effect of vitamin D supplementation on insulin and glucose metabolism in overweight and obese individuals: systematic review with meta-analysis. Sci Rep. 2015;5:16142. doi:10.1038/srep16142
156. Smith GI, Atherton P, Reeds DN, et al. Dietary omega-3 fatty acid supplementation increases the rate of muscle protein synthesis in older adults: a randomized controlled trial. Am J Clin Nutr. 2011;93(2):402–412. doi:10.3945/ajcn.110.005611
157. Kiecolt-Glaser JK, Belury MA, Andridge R, Malarkey WB, Hwang BS, Glaser R. Omega-3 supplementation lowers inflammation in healthy middle-aged and older adults: A randomized controlled trial. Brain Behav Immun. 2012;26(6):988–995. doi:10.1016/j.bbi.2012.05.011
158. Hutchins-Wiese HL, Kleppinger A, Annis K, et al. The impact of supplemental n-3 long chain polyunsaturated fatty acids and dietary antioxidants on physical performance in postmenopausal women. J Nutr Health Aging. 2013;17(1):76–80. doi:10.1007/s12603-012-0415-3
159. Smith GI, Julliand S, Reeds DN, Sinacore DR, Klein S, Mittendorfer B. Fish oil-derived n-3 PUFA therapy increases muscle mass and function in healthy older adults. Am J Clin Nutr. 2015;102(1):115–122. doi:10.3945/ajcn.114.105833
160. Krzyminska-Siemaszko R, Czepulis N, Lewandowicz M, et al. The effect of a 12-week omega-3 supplementation on body composition, muscle strength and physical performance in elderly individuals with decreased muscle mass. Int J Environ Res Public Health. 2015;12(9):10558–10574. doi:10.3390/ijerph120910558
161. Sneddon AA, Tsofliou F, Fyfe CL, et al. Effect of a conjugated linoleic acid and omega-3 fatty acid mixture on body composition and adiponectin. Obesity (Silver Spring). 2008;16(5):1019–1024. doi:10.1038/oby.2008.41
162. Cornish SM, Chilibeck PD. Alpha-linolenic acid supplementation and resistance training in older adults. Appl Physiol Nutr Metab. 2009;34(1):49–59. doi:10.1139/H08-136
163. Gharekhani A, Dashti-Khavidaki S, Lessan-Pezeshki M, Khatami MR. Potential effects of omega-3 fatty acids on insulin resistance and lipid profile in maintenance hemodialysis patients: a randomized placebo-controlled trial. Iran J Kidney Dis. 2016;10(5):310–318.
164. Wu JHY, Micha R, Imamura F, et al. Omega-3 fatty acids and incident type 2 diabetes: a systematic review and meta-analysis. Br J Nutr. 2012;107 Suppl 2(0 2):S214–S227. doi:10.1017/S0007114512001602
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
